The problems associated with bleeding myomas are related primarily to anemia, but
the myomas can also create difficulties in maintaining an acceptable
lifestyle because of the problems of pelvic discomfort. The
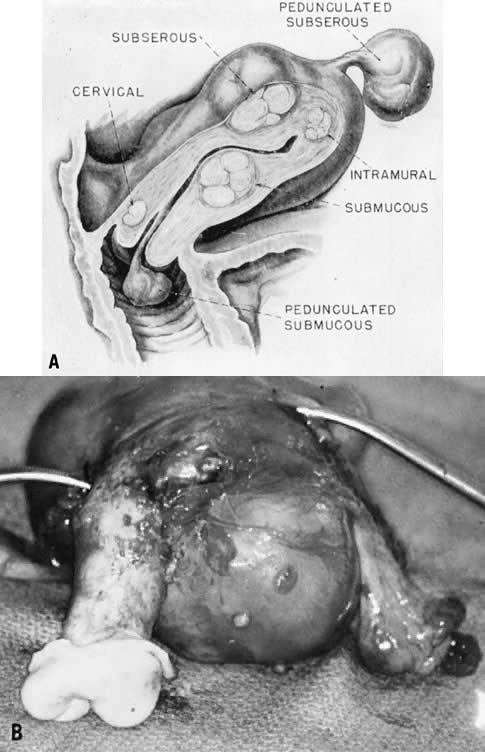
submucous myoma particularly can be the cause of major hemorrhage and
produce emergency situations. Intramural fibroids and a distorted endometrial
cavity can produce a similar picture and force intervention. The clinical problems produced by the mass of the myomatous uterus usually
are not observed until the mass rises out of the pelvis. In nonpregnant
states, the mass may cause ureteral obstruction, bladder and rectal
pressure, pelvic pain, and if the mass extends to the umbilicus or
above, diaphragmatic pressure. Rarely, when the pedunculated subserous
myomas twist and causes acute or chronic symptoms or marked abdominal
protuberance, surgical intervention is warranted. Benign degeneration of the myoma is usually caused by avascular necrosis. It
is principally seen during pregnancy, when it should be treated
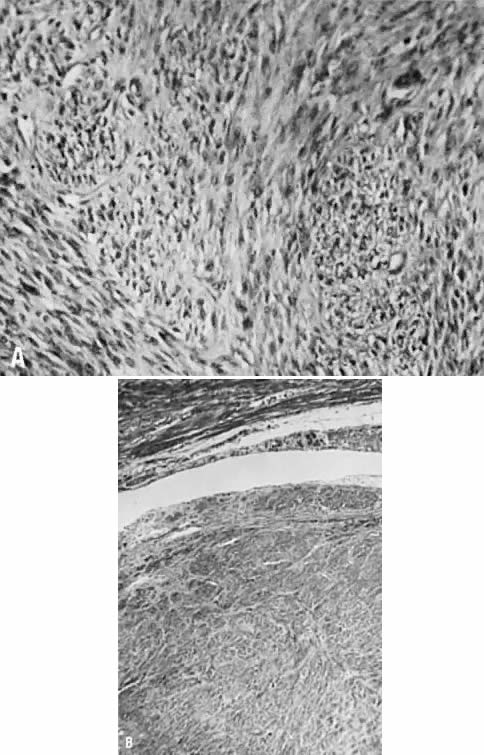
symptomatically. Malignant degeneration results in sarcoma, which occurs
in 0% to 5% of cases. Sarcomas arising de novo in normal uteri usually tend to be more aggressive. Changes in size, especially
those associated with vaginal bleeding a postmenopausal woman, are
signs of possible malignant degeneration. Major advances in the treatment of symptomatic fibroids have created treatment
options. The principal treatments for uterine myomas are control
of the symptoms after a benign diagnosis is established. The options
for treatment of symptomatic fibroids are medical management and surgery. Medical Management The management of symptomatic uterine myomas has traditionally involved
surgery. However, the introduction of GnRH agonists in the 1980s offered
temporary relief to women with myomas who do not desire surgery and
are approaching menopause.18 The use of a GnRH agonist produces a hypoestrogenic state, which leads
to a median reduction in uterine volume of approximately 50%. The maximal
effect is seen after 12 weeks of therapy, with no further reduction
in uterine size observed between 12 and 24 weeks of therapy. Unfortunately, rapid
regrowth of myomas after therapy and side effects related
to the hypoestrogenic state such as bone loss and hot flashes have limited
the usefulness of the GnRH agonists. To overcome the side effects of long-term GnRH therapy and maintain decrease
in uterine size, Friedman and coworkers proposed an “add-back” regimen
of estrogen and progesterone in small doses.19 Early reports with add-back therapy appear promising, but the high cost ($300.00/month) associated with GnRH agonist with estrogen and progesterone
have limited this approach. The ultimate place for GnRH agonist
therapy may be as a presurgical treatment before myomectomy or hysterectomy. The GnRH agonist can cause a cessation of menses, allowing severe anemia
to be corrected before surgery and avoiding preoperative blood transfusions. It
also been shown to reduce operative blood lose. Preoperative
GnRH also opens the possibility for converting some cases of abdominal
hysterectomy into a vaginal hysterectomy through reduction in uterine
mass. Surgical Management The key factors governing the surgical options are the patient's age, fertility
status, and reliability; the impact of fibroids on surrounding
organs; and attendant medical, surgical, or anesthetic risks that
may complicate surgical treatment. If fertility is a consideration
and the patient has major symptoms, myomectomy is the procedure of choice. Myomectomy
should be preceded by a hysterosalpingogram to determine
the location and patency of the fallopian tubes and to screen for submucous
myomas. Extensive and aggressive myomectomy runs the risk of
resulting in emergency hysterectomy. The use of uterine tourniquets and
vasopressin has reduced the amount of blood loss during myomectomy. Dillon
reported that, with the use of vasopressin, 72% of patients undergoing
myomectomy did not need blood products.20 Other complications associated with abdominal myomectomy are pelvic adhesion
and bowel obstruction. In comparing the overall morbidity associated
with myomectomy with that of hysterectomy, Iverson found no difference.21 A patient undergoing myomectomy should understand that the procedure is
a treatment for fibroids, not a cure. There is a 15% recurrence rate
of myomas after myomectomy and a 10% reoperation rate. Dubuisson first reported myomectomy under laparoscopic control.22 Technical innovations such as electric morsulators (Karl Stortz) and simplified
suturing techniques have made this procedure more feasible. Laparoscopic
myomectomy can be offered as an alternative to abdominal
myomectomy in selected cases (i.e. with a single myoma smaller than 6 cm) and should only be attempted by
experienced laparoscopic surgeons. It has been suggested that adequate
closure of the myometrium after laparoscopic myomectomy is difficult
and may account for uterine rupture during pregnancy after undergoing
a laparoscopic myomectomy. The hysteroscope has been employed to establish the diagnosis of submucous
fibroids and, in selected cases, has been used successfully to perform
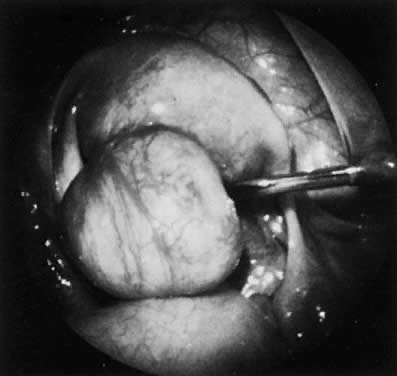
total (Fig. 7) or subtotal (Fig. 8) submucous myomectomy (Fig. 9). Younger women with infertility, recurrent abortion, or menorrhagia have
had successful pregnancies after this procedure and avoided a cesarean
section.23 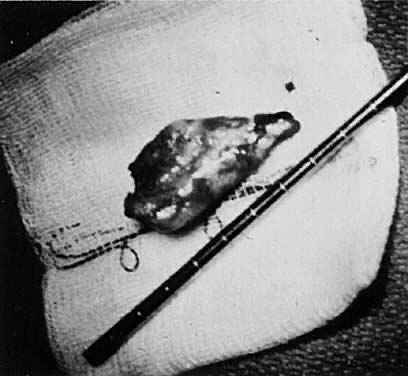 Fig. 7. The pedunculated submucous myomas were removed intact after hysteroscopic
localization, avulsion, and extraction through the dilated cervix. Fig. 7. The pedunculated submucous myomas were removed intact after hysteroscopic
localization, avulsion, and extraction through the dilated cervix.
|
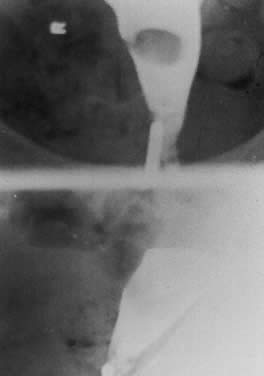
 Fig. 8. The submucous fibroid was confirmed by hysteroscopy and removed by hysteroscopically
controlled resection. Fig. 8. The submucous fibroid was confirmed by hysteroscopy and removed by hysteroscopically
controlled resection.
|
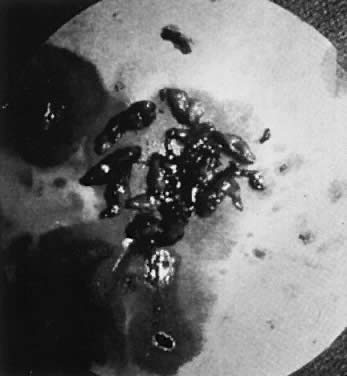 Fig. 9. Resected pieces of a submucous myoma after hystero-scopically controlled
removal. Fig. 9. Resected pieces of a submucous myoma after hystero-scopically controlled
removal.
|
Two other modalities are available for the treatment of symptomatic fibroids: myolysis
and uterine artery embolization. Myolysis was described
by Goldfarb in the United States, and it is performed by penetrating
the fibroid (3 to 10 cm) at multiple sites at a 90-degree angle with
the neodymium-doped yttrium-aluminum-garnet (Nd:YAG) laser or bipolar
needles.24 In response to the treatment, the myoma undergoes thermal necrosis and
frequently atrophies. The complication rate is not established. Transcatheter arterial embolization has been used for postpartum hemorrhage
since 1979. Ravin in Paris reported that bilateral uterine artery
embolization could be used to effect a 39% to 70% decrease in uterine
size and an 85% decrease in patient symptoms.25 Although results of uterine artery embolization for fibroids have been
encouraging, serious complications have occurred, complication rates
are unknown, and long-term follow-up is needed. If fertility is not a factor, hysterectomy remains the traditional therapy. However, for
those patients whose major problem is bleeding and who
wish or need to avoid hysterectomy, hysteroscopic endometrial ablation
of the endometrial cavity has been tried with success in a growing
number of patients. Long-range follow-up has shown these methods to be
effective for up to 8 years, because more than 80% of patients so treated
have not required further surgery in the interval.26 New techniques of nonhysteroscopic endometrial ablation are becoming available. If
the uterine cavity is of normal shape and not larger than 10 cm, Thermachoice, a
thermal balloon ablation technique can be employed
with equal effectiveness to that of hysteroscopic ablation, even
if intramural or subserosal myomas are present. |