Exploration of the Abdomen
Exploration of the abdomen is an important part of any abdominal operation, and it should be done during a hysterectomy or other gynecologic operative procedure that permits such exploration. Systematic exploration of the abdominal cavity should include examination of the liver and its surfaces for possible metastatic or inflammatory disease. In doing so, it is important to handle tissues gently and to remove any powder from gloves, so as to minimize the formation of adhesions. In young to middle-aged women who have been on oral contraceptives, it is important to examine the liver for possible liver-cell neoplasms. Next, the gallbladder should be examined, if at all possible, since gallstones are prevalent in women. Next, if possible, the pancreas, esophageal hiatus, spleen, and kidneys should be palpated. At this point, adhesions involving the small bowel may be lysed, since it is difficult to explore well in the face of adhesions. When adhesions are dense, however, and freeing these adhesions is not a necessary part of the operation, exploration of the area involved is not appropriate. It is generally difficult to examine the colon thoroughly, but a brief examination of the ascending, transverse, and descending colon can be performed if indicated. In the vicinity of the sigmoid, one may find adhesions in patients who have had a history of diverticulitis. If one is using a previous abdominal incision, it is not at all unusual to have small bowel or even colon adherent to the incision: Consequently, in performing such an incision, one must take special care to avoid inadvertent enterotomy. Probably the best technique to avoid entering intestine that is adherent to the incision is to place the posterior rectus sheath and peritoneum on traction with Kocher or Allis clamps. This makes the adhesions between the small bowel or colon and the peritoneum fairly taut and also allows the surgeon to divide these adhesions under better vision. An alternative is to select an incision that is at a distance from previous incisions, if possible.
Intestinal Complications
ADHESIONS.
One of the most common complications that can occur during an operation such as abdominal hysterectomy is an enterotomy involving small bowel or the colon, usually the sigmoid because of its proximity to pelvic structures. This injury occurs principally during the lysis of adhesions, and although sometimes unavoidable, it usually is a preventable complication. When enterotomy occurs during the division of adhesions, it usually results from tearing the serosa when using blunt dissection or cutting directly into the lumen of the bowel during sharp dissection. There is no single best method of dividing adhesions, in spite of dogma to the contrary. In some situations, particularly when the adhesions are flimsy and are torn apart easily, gentle blunt dissection is the safest method. In other situations, when adhesions are dense and, especially, when important adjacent structures such as the urinary bladder are involved, blunt dissection or pulling on the small intestine results in tears of the bowel or adherent viscus. This happens primarily because the tensile strength of the adhesions exceeds that required to maintain bowel or other visceral seromuscular layer intact. Consequently, when adhesions are dense, it is generally safer to use a sharp method of dissection. The immediate recognition of enterotomy is important because if the operation is terminated without closing the defect, peritonitis will occur in the immediate postoperative period.
INJURIES TO THE SMALL INTESTINE.
Injuries to the small intestine can result during gynecologic procedures ranging from dilatation and curettage to total abdominal hysterectomy. Newly introduced laparoscopic and hysteroscopic procedures (such as laser-assisted endometrial ablation) can also result in intestinal injuries. For example, trochars, cautery, or lasers used in these procedures can produce intestinal injuries, and sometimes these injuries are not immediately apparent at the time of operation. A patient with such injuries may present with postoperative ileus, compounded by signs of peritoneal irritation, elevated temperature, and leukocytosis. Early re-exploration in these situations can be life-saving.
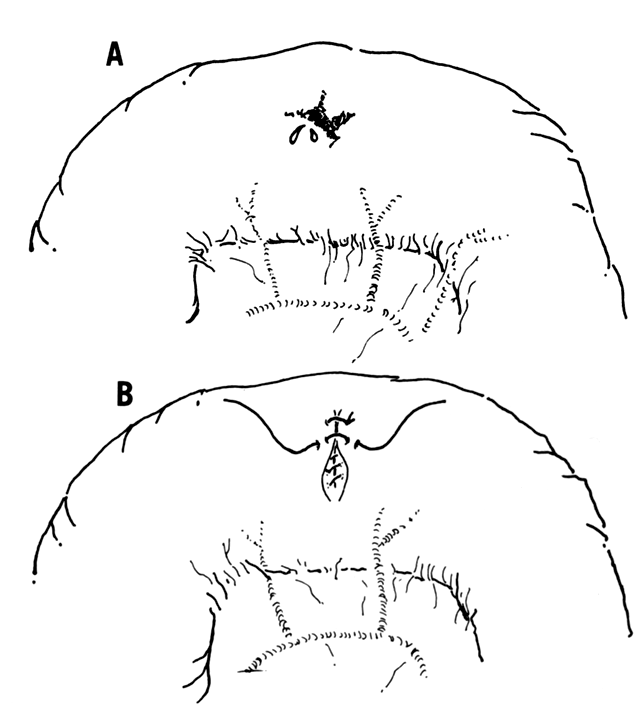
Ordinarily, once recognized, small bowel injuries can be dealt with in a straightforward manner. Serosal tears represent weak points in the small bowel. If obstruction develops postoperatively, these weak spots may perforate, leading to peritonitis or enterocutaneous fistulae. If serosal tears are few in number, they can be oversewn with either an absorbable or fine nonabsorbable 3-0 or 4-0 grade suture. On the other hand, if the serosal tears are numerous, and if one is satisfied after careful inspection of the entire length of small bowel that the tears do not include the mucosa, an alternative is either to leave the small bowel alone or to perform a resection. Through-and-through injuries are best treated by suture repair. These are usually evident in that bilious material can be seen emanating from the area of the small bowel injury. Generally, a single or double-layer closure is satisfactory. A single layer of running absorbable suture followed by an outer layer of interrupted 4-0 silk or teflon/dacron or, alternatively, a single layer of interrupted nonabsorbable sutures is quite effective. It is most prudent to repair the defect in the small bowel in the transverse direction (Fig. 1). If the laceration is long, or if multiple areas are involved, one should consider a small bowel resection. A resection can be done in a number of ways, but first, the two areas to be outlined are clamped to minimize the amount of intestinal contents that spill into the abdomen (Fig. 2A). An additional precaution is to place moist lap pads on either side of the small bowel, so as to further minimize the chance of spillage into the abdomen. A small V-shaped defect is constructed in the mesentery by first incising the peritoneum on both sides. Then the vessels in the V can be clamped, divided, and ligated so as to completely excise this V in the mesentery. When this is accomplished and the two ends of the bowel are freed over a distance of approximately 0.5 cm from the edge of the clamp, the anastomosis is performed. Although the tissue that is enclosed in the clamps can be included in the anastomosis, it is clear that healing of an anastomosis is enhanced by using noncrushed, viable tissue in the anastomosis. Therefore, stay sutures are placed between the mesenteric and antimesenteric segments of the two limbs, which are then pulled together and the tissue excised by sharp dissection just below the level of the clamp on each side (Fig. 2B). Next, either a single- or double-layer anastomosis can be performed.
A single-layer anastomosis of the inverting or approximating type can be performed by using Lembert sutures that encompass the seromuscular layer in its entirety. These sutures are placed circumferentially 5 mm apart. When one side is sutured, the anastomosis can be turned over and the other side can be done. The mesentery is then closed with a running suture so as to eliminate the possibility of an internal hernia.
Similarly, a two-layer anastomosis (Fig. 2C-E) can be done by closing the entire thickness or just the mucosal layer with a running absorbable suture such as chromic catgut or polyglactin and then using an outer layer of interrupted Lembert sutures of material such as 4-0 braided teflon/dacron or silk. As in the single-layer anastomosis, the mesenteric defect is closed by approximating the peritoneal edge of the mesenteric leaves using a running or interrupted suture technique. It is important not to include any mesenteric vessels in the bites taken with the needle, since this can result in a mesenteric hematoma that might compromise the blood supply to the anastomosis and lead to an anastomotic breakdown.
Under certain circumstances, it may be necessary to avoid an anastomosis altogether. For example, when the small bowel injury occurs in a patient with massive peritonitis, any intestinal anastomosis is hazardous and construction of such an anastomosis may be followed by suture line infection, with breakdown of the closure and recurrence of peritonitis due to the intestinal fistula. On the other hand, minimal and, especially, localized infections in the peritoneal cavity do not necessarily preclude the use of such an anastomosis or closure. An anastomosis may also be hazardous in the patient with longstanding bowel obstruction. In such a situation the fecal spillage that may result is infectious, especially when gangrenous segments are present, and occasionally, it may be prudent to perform an ileostomy or jejunostomy rather than an anastomosis. In addition, it may be desirable to perform an ostomy rather than anastomosis when an operation has been unduly long and it is important to save time: In the patient who is deteriorating, a simple stoma is more quickly constructed than is an anastomosis.
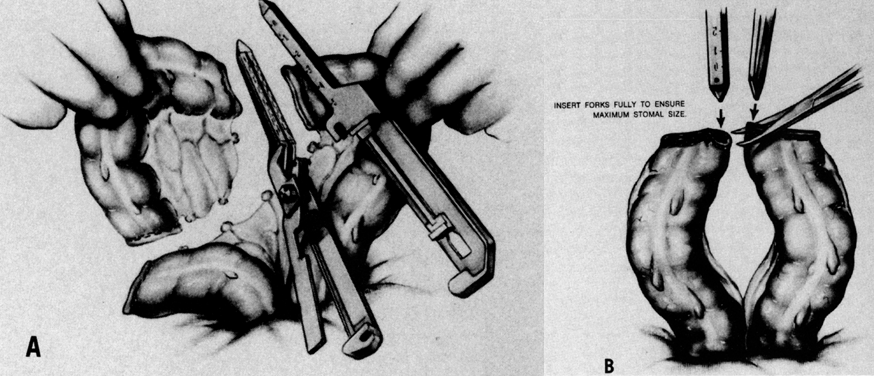
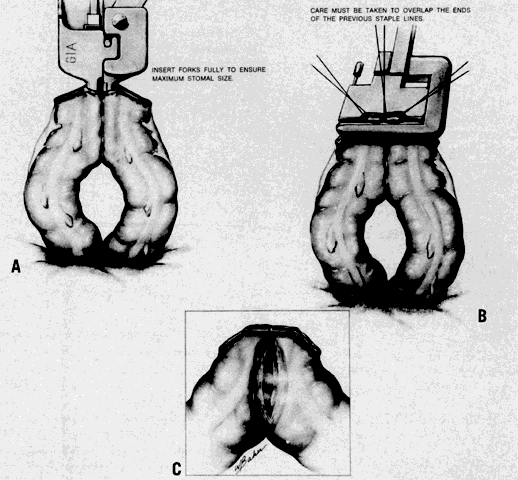
A stapling technique may be used instead of sutures to perform a small bowel resection and anastomosis.6 This is both a rapid and effective technique, once mastered (Fig. 3 and Fig. 4). Both sides of the bowel are divided with a stapling device (GIA ™ for example), which staples and divides the two ends at the same time (Fig. 3A). Next, a small portion of the staple line on the antimesenteric corner is excised on each end of the bowel to be anastomosed (Fig. 3B). Another identical stapler is introduced into both ends and is fired (Fig. 4A). This results in a side-to-side anastomosis, and the final step is to close the hole that results with a TA ®-type stapler, which staples but does not divide any tissue (Fig. 4B). Excess tissue is excised above the stapler before it is released. An additional important point is to make sure to add one or two sutures to reinforce the lower end of the side-to-side anastomosis, since there may be an open spot where the bowel was actually divided but not stapled over a short distance. Mesenteric defects must of course be closed just as in the suture technique. This results in a functional, end-to-end anastomosis, which is reliable and rapidly performed. The only disadvantage is the extra cost involved in using the stapling instruments. Depending on the clinical situation, however, the time saved may well be worth the extra cost.
INJURIES TO THE COLON.
Injuries to the colon can occur during gynecologic procedures, particularly in those involving left adnexal masses or in patients with previous inflammatory disease due to diverticulitis or previous pelvic inflammatory disease with adhesions involving the sigmoid or right colon. Rarely, the transverse colon can be so redundant as to be adherent to structures in the pelvis. When one is anticipating a possible resection of the colon, such as for ovarian malignancy, a bowel preparation is in order, such as the method previously described using neomycin and erythromycin base (or metronidazole). This combination has been shown to be effective against both gram-negative aerobic and anaerobic fecal organisms. Many surgeons add a parenteral intravenous antibiotic, given just before the operation.
Injury or perforation of the prepared colon can be primarily repaired using suture techniques similar to those used in small bowel repair. Small tears can be repaired with a few interrupted sutures in either one or two layers, but formal resection with anastomosis is required if a segment of colon must be resected along with the neoplasm. This can be done in nearly the same manner as in small bowel resection, by taking a small wedge of mesentery, taking care to preserve blood supply to the two ends, since this is especially critical for colonic surgery. As in the small bowel anastomosis, a two-layer closure using an inner layer of running absorbable suture material and an outer layer of interrupted nonabsorbable Lembert sutures of 4-0 strength, is an accepted method. It is important not to greatly narrow such an anastomosis and to be sure that the bowel ends are viable and have an adequate blood supply. If an adequate length of colon is available at both ends, the stapling technique described for the small bowel anastomosis can also be used.
Injury to the colon that has not been prepared in any way preoperatively presents a special problem; the extent of injury and the speed with which it is recognized and repaired are the key factors in deciding whether or not some type of colostomy is required. A minor injury to the colon (i.e., one that encompasses approximately 1 cm or less) or an injury with minimal fecal spillage that is recognized early can be treated by primary single- or double-layer closure. Nonabsorbable interrupted sutures should be used for the outer layer. Parenteral antibiotic therapy using a combination of drugs effective against both anaerobic and aerobic organisms should be started and maintained for several days postoperatively.
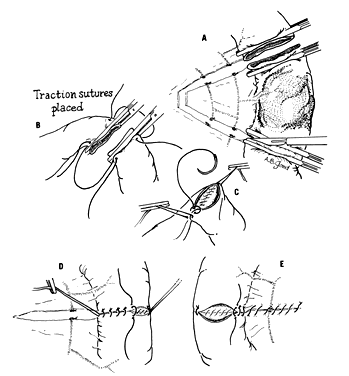
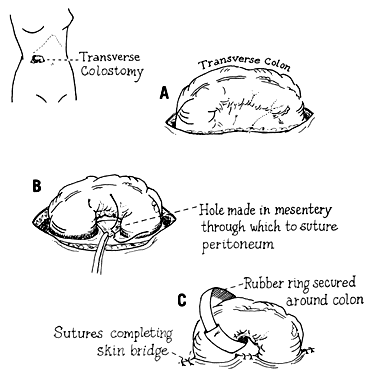
A major injury with extensive fecal spillage is another matter. Generally, a simple repair of such a lesion can be expected to fail, with resultant fecal peritonitis. The only exception to this is if the injury is to the cecum or ascending colon, where the stool is often liquid, and a primary closure may be feasible. If possible, the injured area should be exteriorized as a colostomy. If the area is below the level that can be easily exteriorized, however, there are at least two other options, depending on the extent of injury. Primary repair of the injured colon can be performed along with a proximal colostomy, such as a sigmoid or transverse colostomy (Fig. 5); the area should be drained with a sump drain. An alternative is resection with an end colostomy and a Hartmann procedure (closure of the rectal stump). Consultation with a general surgeon may be helpful in choosing the best approach.
In addition to injuries that occur in the course of vaginal or abdominal hysterectomy, oophorectomy, and other resective abdominal procedures, injuries can result from perforation of the uterus (e.g., in conjunction with dilatation and curettage, colpocentesis, or a laparoscopic or hysteroscopic procedure). Under these conditions, injury to the small bowel may not be directly observed, and it is necessary to watch for the development of signs of peritoneal irritation that may indicate either hemorrhage or actual perforation of viscera: If perforations are found at laparotomy, management depends on the nature of the injury, the presence of infection, and the duration of time from the occurrence of the injury to the time the patient is actually explored.