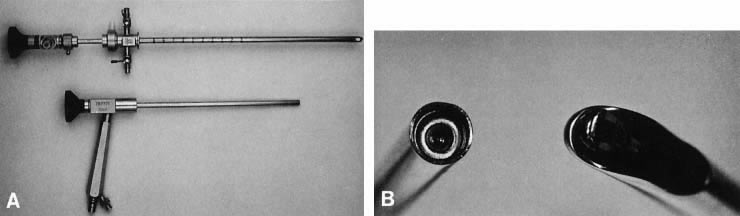
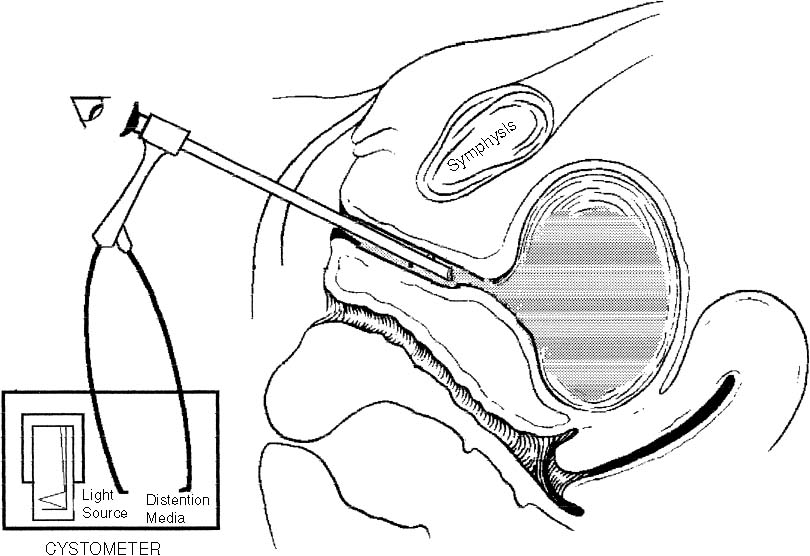
Normal Urethra The normal urethral mucosa has epithelial folds that form a symmetric, stellate
configuration. The color is lush and pink owing to the generous
vascularity and thin epithelium. The urethrovesical junction is likewise
pink, with more developed folds. The color and appearance are uniform
throughout its length. The trigone and both ureteral orifices should
be visualized with the urethroscope. Acute Urethritis In acute urethritis, the epithelium develops a fiery red color. Most commonly
seen is an associated purulent exudate. Frequently there are friable
polypoid projections or fronds from both the urethra and the urethrovesical
junction. Often there is concomitant trigonitis with a shaggy, flocculent
exudate. Atrophic Urethritis/Trigonitis Atrophic changes of the urethra and trigone are generated by a relative
lack of estrogen. Estrogen maintains the uroepithelium, promotes adequate
vascular supply, and stimulates the connective tissue support of
the urethra and trigone. With a deficiency of estrogen comes epithelial
thinning and decreased vascular perfusion, which results in a profound
paleness. In addition, the urethrovesical junction fails to function
well in its sphincteric capacity, resulting in urine loss. A frequent
finding associated with this condition is urethral caruncles. These
reddish blue projections of urethral mucosa emanate from the meatus usually
at the 6-o’clock position. Caruncles are benign and require
no treatment unless bleeding or pain ensues as a result of irritation. Treatment
usually consists of topical estrogens, which work well. Rarely
is excision required. Urethral Diverticulum A urethral diverticulum is a cystic outpouching of the urethral lumen usually
formed by chronic infection of the periurethral glands. It is best
identified in conjunction with palpation. This allows easier identification
of the orifice, particularly when exudate is flowing from it. Compression
of the proximal urethra with the urethroscope in place will
permit distention of the urethra and diverticulum, thereby increasing
emanation of the exudate.3 The urethral diverticulum is most commonly seen in patients with a long
history of chronic infections as well as a history of dyspareunia. It
is most commonly found in the midurethra on the posterior wall. Often
the diverticulum is palpable over the urethroscope with a finger inserted
into the vagina. The treatment is surgical excision. Urethral fistulas are tracts of communication between the urethra and the
vagina. They often result as a complication of surgery for diverticula. Less
commonly, they may develop as a result of a chronic infection
of the periurethral glands. The fistula resembles a diverticular orifice
when viewed with the urethroscope. It is best diagnosed radiographically. Ectopic Ureter Ectopic ureters are an extremely rare finding. They are identified by the
presence of a ureteral orifice opening into the urethra, from which
urine is seen to be emanating. The presence of an ectopic ureter should
be suspected when incontinence exists in the face of an otherwise normal
examination. Urethral Condylomata In the patient with known perineal condylomata and lower urinary tract
symptoms, urethral condylomata may be seen. They appear as dense, white
papillary projections into the urethral lumen. Biopsy should precede
any treatment regimens. Cryotherapy has been used with good success and
is generally well tolerated. Urethral condylomata are a rare finding
and virtually are never seen in the absence of perineal lesions. Urethral Neoplasms Urethral neoplasms are rare findings and are most commonly malignant.3 Associated symptomatology includes urgency, frequency, dysuria, hematuria, urinary
retention or incontinence, and occasionally purulent urethral
discharge with tumor necrosis. They may be either primary or metastatic. Primary
lesions are usually of the epidermoid or transitional
cell type. Metastases arise from transitional cell carcinoma of the bladder, adenocarcinoma
of the endometrium, and squamous cell carcinoma
of the vulva and vagina. Visually they appear as fleshy growths impinging
on the urethral lumen. They may be found in association with a diverticulum. Urethroscopy
can identify these lesions, but it cannot differentiate
between benign and malignant processes, and therefore biopsy
is mandatory. |