As of 1996, approximately 28 million noninstitutionalized, American women older than 15 had some type of disabling condition.1 Many other women suffer from chronic conditions that, despite significantly impairing functional capabilities, fail to meet classic definitions of “disability.” The medical community frequently overlooks clinical issues important to this very large population, including many unique gynecologic and obstetric problems.
Basic Screening and the Pelvic Examination
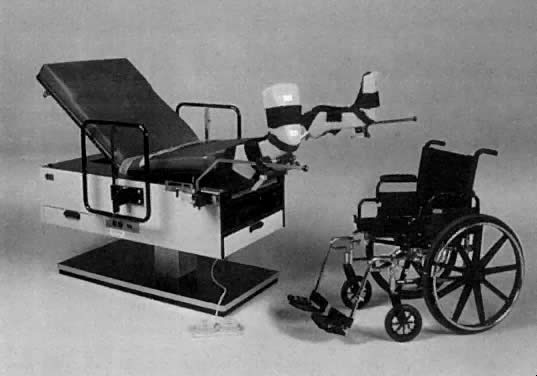
Physicians caring for disabled women must perform pelvic examinations in a way that assures patient access, safety, and comfort. Adjustable tables that lower to the standard wheelchair height of 19 or 20 inches facilitate access for the examination. Handrails on either side of the table enhance safety and allow independent movement up or down the table. Alternative stirrups, particularly padded boot stirrups, increase comfort for women with limited range of motion of the lower extremities (Fig. 1) (Welner Universally Accessible Examination Table, patent issued 4–96, no. 507050). An assistant should attend each examination and when necessary, manually support lower extremities, individually adjusting adduction/abduction, flexion/extension positioning for patients with spinal cord injury (SCI), stroke, cerebral palsy (CP), orthopedic injury, multiple sclerosis (MS), and even obesity. When padded boots are available, the need for extra personnel is minimized, as boots can stabilize spastic limbs and those with limited range of motion. In patients with CP, who often have very severe flexion contractures, it may be preferable to use knee-chest, side lying, or heel-to-heel positions. Above all, physicians must allow more time to examine a disabled patient.2
Spinal cord-injured women with lesions above T6 pose a particular problem during a pelvic examination because these patients are at increased risk for having an episode of autonomic dysreflexia (AD) during this type of examination (see section titled Autonomic Dysreflexia). Before obtaining a pelvic examination, physicians should advise these patients to empty their bladders and to perform standard bowel programs the night before to minimize the risk of triggering AD and bowel accidents during examination.
Rapid pulling movements to adjust leg positioning should be avoided as this can cause increased muscle spasticity. Liberal application of lidocaine gel to the perineum before insertion of the speculum can lessen the likelihood of developing AD. Topically applied lidocaine gel can also be useful to decrease discomfort when examining disabled nulliparous women or those that are elderly.3 Despite all precautions, AD can still occur in a predisposed patient. Care givers should have rapid-acting antihypertensive agents available and should monitor blood pressure periodically during the pelvic examination.
Breast Cancer Screening
Breast cancer is the most common gynecologic malignancy. Not only are women with disabilities at increased risk for underdetection of breast disease but they also may harbor an increased risk for developing such malignancies. Women with disabilities are statistically more likely to be overweight than non-disabled women. Women with disabilities may be at increased risk for underdetection of breast pathology as a result of a variety of factors. Some clinicians and patients wrongly believe that mammography can be performed only when a woman is standing, neglecting to offer this essential screening tool to women in wheelchairs. Some women with disabilities have restrictions in upper body movements, making it difficult for them to perform breast self-examination. Physical limitations may impact the quality of the mammography image, limiting views to the anteroposterior dimension and restricting the ability to obtain lateral views. Unfortunately, access barriers such as high examination tables may limit a woman's ability to obtain regular clinical breast examination. Clinicians need to work closely with these women to overcome these obstacles in breast health care. In addition to delayed diagnosis because of access barriers, women with disabilities may harbor an increased risk for developing breast cancer. These women, because of decreased physical activity and limited food choices are statistically heavier than other women, with obesity being one of the risk factors linked with breast cancer (National Center for Health Statistics. Healthy People 2000 Review, 1997) Early exposure to ionizing radiation to the spine, a common occurrence in girls with cerebral palsy, scoliosis, and other conditions has also been linked to an increased risk for the development of breast cancer.3a
Menstrual Cycle
For many disabled women, regular menstruation signifies normalcy as well as the opportunity for childbearing. Other disabled women discover that normal and particularly abnormal menstruation causes hygiene problems and increases the need for attendant care. Physicians evaluating disabled women must therefore know the effects of various disabilities on the menstrual cycle while remembering that disabled women often experience the same menstrual disorders that trouble the nondisabled.
CP, spina bifida, and other congenital disabilities usually do not affect the onset or pattern of menarche. Young girls who suffer traumatic brain injury (TBI) or SCI may experience delayed menarche or even precocious puberty.4
Women with previously normal menstruation may experience transient menstrual disorders after becoming disabled. Women with chronic disease states, such as diabetes mellitus or obesity, may experience menstrual irregularity. Patients with rheumatoid arthritis retrospectively report later onset of menarche and increased rates of ovulatory dysfunction.5 Women with SCI, TBI, and MS have an increased frequency of hyperprolactinemia.6,7,8 If no structural abnormalities of the pituitary are discovered and menstrual cycles are regular, no further therapy is warranted. Disabled women with hyperprolactenemia may have significant hygienic problems due to related menstrual irregularities. Moreover, many have low levels of 17-b-estradiol, which intensifies their risk for osteoporosis. Patients with hyperprolactinemia and menstrual irregularities require pharmacologic therapy.
Contraception
Although disabled women require safe and effective contraception, they lack comprehensive data to guide their choices.
Women with impaired mobility face particularly difficult issues given their increased risk for the development of deep vein thrombosis due to lower extremity venous stasis. Although spasticity may diminish venous stasis, it is unknown how greatly spasticity decreases overall risk of deep vein thrombosis. Because estrogen-containing contraceptives increase the risk of thrombosis, physicians may wish to avoid prescribing them in this population, substituting progestin-only pills (“minipills”), medroxyprogesterone (Depo-Provera) injections, or levonorgestrel (Norplant) subdermal implants. The mini pill is somewhat reduced in effectiveness compared to combination oral contraceptives and should be combined with a barrier method for improved efficacy.9 Because of the high prevalence of latex allergy in women with spina bifida, only spermicidal nonlatex methods may be appropriate in these patients.10 Nonlatex condoms are being developed, which will greatly benefit this population.11 Unfortunately, progestin-only methods pose other, troublesome side effects. Patients may experience irregular bleeding with associated hygiene problems. Depo-Provera can cause prolonged amenorrhea with a related drop in estrogen levels, thereby heightening the risk of osteoporosis in patients already at risk because of chronically impaired mobility.12 Although the Norplant system is not associated with such decreases in estrogen level, physicians may find insertion and removal of Norplant problematic in women with upper extremity contractures and spasticity. Barrier methods of contraception, though safe, may be difficult for many disabled patients to insert or use properly.
Women with chronic disease states face a variety of problems frequently limiting their choice of contraception. Patients with chronic, debilitating cardiac disease should avoid estrogen-containing contraceptives because they increase the risk of thrombosis. Physicians may prescribe progestin-only methods, or they might consider the use of intrauterine devices in women wishing to avoid hormonal agents. Women with pelvic sensory impairment or a history of endocarditis or valvular heart disease should not use an IUD because they are at increased risk for infection, especially during insertion.13 Although women with rheumatoid arthritis may experience decreased severity of symptoms while using combined oral contraceptives, women with other autoimmune conditions, such as systemic lupus erythematosus (SLE), may experience adverse side effects.14 SLE patients experience a significantly increased frequency of thrombotic events.15 Thus, they should use IUDs, progestin-only methods, or barrier methods. Depo-Provera is highly effective and safe, and it reduces seizure frequency. Paradoxically, Norplant has been linked with an increased risk of contraceptive failure in women with epilepsy and should be avoided in this population.16
Sexually Transmitted Disease
Unfortunately, many health-care providers and family members still view disabled women as asexual. Although the disabled woman may therefore find it uncomfortable sharing intimate needs with health-care providers and family, she may also be less likely to self-detect signs of sexually transmitted disease (STD). In many cases, an STD may be the only sign of an abusive relationship (see section titled Abuse). Thus, anyone caring for the disabled patient must become knowledgeable about the particular problems that STDs pose within this population.
Signs and symptoms of STDs used by physicians to diagnose infection reliably in nondisabled patients may prove less reliable in disabled women. Women with pelvic sensory impairment may not feel pain or cramping as do nondisabled women with chlamydia, gonorrhea, or pelvic inflammatory disease.17 Malaise or increased spasticity may be the only warning signs voiced during the examination. Visually impaired women may not detect or accurately describe a lesion that could represent syphilis, herpes, or human papillomavirus infection. Although a complete discussion of all STDs exceeds the scope of this chapter, several infections warrant particular discussion.
SYPHILIS.
The disabled woman with syphilis may present with mild or severe symptoms, either unnoticed by the patient, partner, attendant, or practitioner or mistaken for consequences of her disability.
Women with visual or sensory impairment may not detect the ulcer or chancre of primary syphilis before its spontaneous regression 3 to 12 weeks after infection. As with nondisabled patients, physicians should maintain a high index of suspicion when considering a diagnosis of syphilis, and not hesitate to perform serum screening tests, which generally detect infection 4 to 6 weeks after exposure.
Patients with secondary syphilis most commonly present with flulike symptoms or skin rash. The rash often involves the palms, soles, trunk, and upper extremities. Women whose disabilities require that they take multiple medications may mistake skin rashes for yet another medication reaction, particularly because manifestations vary considerably from patient to patient.
In approximately 30% of patients, tertiary syphilis will develop if the initial infection is not treated. Sequelae of tertiary syphilis include optic atrophy, tabes dorsalis, and even generalized paresis. MS patients also develop this constellation of findings. Thus, a physician treating a woman with MS, who develops visual disturbance and sensory or balance abnormalities, may falsely attribute these findings to MS. Patients with symptoms of neurosyphilis may exhibit a change of mental status or the onset of a new physical disability. Such findings often confuse the patient, the patient's family, and her care givers, who may have overlooked infectious etiologies, such as syphilis, that they might not overlook in nondisabled patients.
HERPES SIMPLEX VIRUS.
Approximately 50% of adults test positive for exposure to herpes simplex virus (HSV), and nearly 60% of these persons remain entirely asymptomatic. Both primary and recurrent lesions present problems for the disabled, infected patient.
Patients with primary HSV typically present with painful genital ulcerations and flulike symptoms. Women with sensory impairment may fail to detect the lesions, but may report malaise or increased spasticity. Although healing of lesions may improve with adequate ventilation of involved areas, immobilized patients may have difficulty attaining or maintaining positions that allow ventilation.
Recurrent genital herpes, though usually milder in severity than primary outbreaks, may also go undetected by the disabled patient. Clinicians and personal care attendants must monitor women with sensory impairment and a known history of HSV infection for skin lesions consistent with HSV and not falsely assume that lesions in the perineum or other weight-bearing areas are simply related to pressure ulcers. Often, women with recurrent HSV become familiar with less traditional prodromes, such as generalized malaise or spasticity, and can help inform their care givers accordingly.
HEPATITIS B VIRUS.
Hepatitis B virus (HBV) is transmitted through sexual contact, transfusion, and intravenous drug use. Many disabled women became physically impaired as a result of risk-taking behavior, or required transfusion after traumatic injury before routine screening of blood for HBV or HIV viruses, and yet never underwent testing during their rehabilitation. Complicating this dilemma, health care providers may confuse constitutional symptoms such as fatigue, malaise, arthritis, and flulike symptoms with exacerbation of certain disabilities, such as MS or rheumatologic diseases, and not screen for hepatitis. Patients who continue to engage in high-risk behavior after the onset of a disability should undergo vaccination, just as is recommended for all nondisabled patients. Vaccination may also be warranted in patients with a history of TBI, who may have impaired judgment.
HUMAN PAPILLOMAVIRUS.
Between 10% and 60% of the population demonstrates DNA evidence of exposure to human papillomavirus (HPV).18 Many HPV infections are asymptomatic, requiring regular screening for diagnosis. HPV lesions are inadequately detected in women with mobility impairments, who often do not undergo regular screening because of access issues, and therefore these women are at increased risk for premalignant and malignant cervical diseases commonly associated with HPV infection. Concurrent autoimmune disease compounds this risk: women with such disorders may have a 10% to 30% increased risk for cervical dysplasia compared to women who do not have autoimmune diseases or are otherwise autoimmune suppressed.19
Many medical practitioners find colposcopic examination of the disabled woman cumbersome and unduly uncomfortable for the patient. Wall-mounted colposcopy units and examination tables that allow support of altered leg adduction will help both patient and physician. Women with SCI lesions above T6 risk development of AD during any cervical manipulation necessary to diagnose or treat dysplastic lesions. These patients require careful monitoring of blood pressure, the immediate availability of antihypertensive agents, and personnel familiar with AD and its treatment to be on hand. Physicians might wish to consider performing colposcopic examination in a monitored setting, such as an outpatient surgical suite in patients with lesions above T6, particularly those with a history of AD.
HUMAN IMMUNODEFICIENCY VIRUS.
By the year 2000, human immunodeficiency virus (HIV) will infect approximately 40 million people worldwide. By the end of 1997, over 100,000 women in the United States were diagnosed with acquired immune deficiency syndrome (AIDS), and AIDS had become the fourth leading cause of death in women.20,21 AIDS will likely remain a major health problem for both disabled and nondisabled women well into the 21st century.
As with other infectious diseases, care givers may mistakenly attribute signs and symptoms of HIV infection to other afflictions encountered by disabled patients. Patients using wheelchairs, who are already prone to frequent bouts of candidal vaginitis and vulvitis, may not realize that recalcitrant infection may represent a more serious problem. Mucocutaneous ulcerations due to HIV may masquerade as decubitus ulcers of the perineum and buttocks. Clinicians may less commonly test disabled women for HIV than their nondisabled counterparts, buying into the false notion that HIV is not a disease of women and that disabled women are not sexually active or vulnerable to abuse.
Infertility
Women with a variety of disabilities may be more prone to ovulatory dysfunction. Disabilities such as SCI, TBI, and MS may be associated with hyperprolactinemia. Although many patients exhibit concomitant menstrual irregularity or galactorrhea, others remain asymptomatic. Practitioners should maintain a high index of suspicion when treating these patients, and not neglect to obtain a pituitary evaluation. Similarly, chronic disease states such as diabetes mellitus, Sjögren's syndrome, and myasthenia gravis may—through altered thyroid function or other associated endocrinopathies—result in oligo-ovulation. Drugs commonly used by disabled women, such as corticosteroids, nonsteroidal anti-inflammatory agents, phenytoin, and tricyclic antidepressants may also affect ovulation.22,23,24
Although the evaluation and treatment of infertility is the same in disabled and nondisabled women, women with disabilities may require special consideration in a variety of circumstances. Women with pelvic contractures, such as is caused by CP, may have difficulty attaining adequate positioning for many required procedures. Those with impairment of vision and movement may require assistance interpreting basal body temperature or other ovulation testing. Women with SCI above T6 may exhibit AD in response to endometrial biopsy, hysterosalgpingography, or hyperstimulation caused by ovulation-induction regimens. The majority of women with physical disabilities have unaffected fertility potential and clinicians should avoid assuming that the male partner need not be evaluated.
Menopause
As of the most recent census, there were nearly 16 million women with disabilities over the age of 50.25 Like their nondisabled counterparts, the majority will have sequelae of estrogen deficiency, including osteoporosis, but their disabilities often complicate standard modes of therapy.
Disabled women may respond somewhat differently in symptomatology to decreased estrogen levels in menopause. These include vasomotor instability, which can be especially troublesome in women with high spinal cord lesions or in women with MS who are sensitive to temperature fluctuations. Women with MS may experience worsening of symptoms, but this may improve with estrogen replacement therapy (ERT).26 Urinary symptoms such as incontinence, increased frequency of cystitis, and bladder pain often complicate menopause. SCI patients and others with bladder regimens may need to modify their routines throughout the menopausal years. Cognitive impairment, often linked to estrogen deficiency states, may further complicate ongoing cognitive impairment related to TBI, stroke, or MS. Although virtually no prospective data address the efficacy of ERT in the disabled population, it has been linked to an improvement in insomnia and depression and has been reported to delay the onset and decrease the severity of Alzheimer's disease in the nondisabled.27,28 These benefits may be especially important in the face of cognitive impairments.
Osteoporosis is responsible for significant morbidity and mortality in general, but especially so in menopausal women with disabilities. Chronic immobilization and medications such as corticosteroids increase bone loss. Studies are currently underway that will attempt to confirm what can be inferred from these risk factors (i.e. that women with long-standing disabilities may enter menopause with established osteoporosis). Patients with MS have an increased risk of vitamin D deficiency, potentially resulting in secondary hyperparathyroidism and resultant osteoporosis. Many MS patients, therefore, may benefit from daily supplementation of at least 600 IU of vitamin D.29 Women with SCI, in addition to being at risk for osteoporosis associated with menopause and chronic immobilization, may also show neurogenic osteopenia and heterotopic ossification (development of bone around joints). Such patients often benefit from disphosphonate therapy.30,31
Menopausal women with stroke and resultant unilateral weakness may have impaired balance and may be prone to falling. Many such women are elderly and may have underlying osteoporosis, which may be exacerbated by long-term heparin therapy given to stroke patients.32
Clinical studies have prompted the use of many different serum markers for osteoporosis, including alkaline phosphatase, serum calcium, osteocalcin, 25-hydroxyvitamin D, parathyroid hormone, urinary hydroxyproline, and urinary pyridinolenes.33,34 Furthermore, a variety of radiologic procedures—most notably, dual X-ray aborptiometry—are commonly used to quantify bone mass compared to control populations.35 Unfortunately, there are no control data regarding expected bone mass for women with disabilities.
Treatment of osteoporosis in women with disabilities needs to be individualized. Options that have been used include calcitonin, cyclic etidronate disodium, alendronate, and ERT. Intranasal calcitonin helps prevent bone loss during immobilization and may also produce an analgesic effect. However, there are drawbacks, including tachyphylaxis with long-term use and lack of beneficial effect on cortical bone.36 ERT protects both cortical and trabecular bone, and these benefits are enhanced with concomitant administration of calcium, vitamin D, and magnesium.37,37a ERT has beneficial effects on skin and soft tissue strength, urinary tract function, and cardiovascular health.38,39,40 The cardiovascular benefits of ERT on the nondisabled population have been widely discussed, but similar data are not available for the disabled population.41 For example, many patients have subclinical hypercoagulability. Approximately 10% of patients with such states have no prior history of a thrombotic event.42 The additive contribution of immobility to preexisting hypercoagulability remains unclear. Thus, clinicians who might feel comfortable prescribing standard ERT to nondisabled women without prior evaluation for a subclinical hypercoagulable state, might wish to rule it out in the chronically immobilized patient or the patient with preexistent cardiovascular or cerebrovascular disease.43,44 Hypercoagulability parameters commonly available for testing include antithrombin III activity, protein S activity, protein C, anticardiolipin antibody, plasminogen activator inhibitor, fibrinogen, factor V Leiden mutation, and prothrombin fragment 12. Choice of markers needs to be individualized based on clinical history.44a
It is essential to screen all women for breast cancer before initiating ERT therapy. Some women with irregular upper body contours or restricted range of motion, such as those with CP, stroke, MS, and quadriplegia, may find mammography more cumbersome and may require referral to special mammography centers for alternative imaging techniques.
Sexual Response in Women with Disabilities
Physicians and family members often forget that disabled women are sexual beings and experience the same sexual response cycle as their nondisabled counterparts.
Although disabled women experience sexual desire in response to standard erotic stimuli, fatigue or discomfort caused by chronic diseases or disabilities may suppress excitement. Soft touch of areas that have preserved sensation, erotic videos, and sensual music can help stimulate sexual desire. Couples may find gentle touching of all areas arousing, sharing in the knowledge that they are being touched by each other. Patients may wish to alter analgesic regimens to permit sexual activity during periods of maximum pain relief. Women with some chronic conditions experience increasing fatigue at different times of day and it would be prudent to avoid attempting sexual activity during these periods.
Some women with SCI experience spasticity in the lower extremities, causing discomfort and difficulty in adjusting positions. Slow and gentle muscle stretching can help relieve spasticity and can become an important part of foreplay.45 Although some women with SCI will not experience genital vasocongestion as a result of neurologic injury, many experience reflex genital vasocongestion despite a complete lack of subjective arousal. Women with lesions above T6 may even experience AD in response to any phase of the sexual response cycle. Clinicians should discuss these issues with an SCI specialist.
Abuse
“Abuse” is preventable emotional or physical harm that results from intentional human action. Although approximately 20% of the general female population experiences abuse, nearly 50% of women with disabilities suffer this violation. Sadly, half of all cases may go unreported.46,47
Most cases of abuse result from one person's taking advantage of an actual or perceived power differential. Such interactions can occur between parents and children, spouses, personal care attendants and clients, physicians and patients, and caretakers and clients living in long-term care facilities. Women with physical limitations may become accustomed to relinquishing some control to others. This dependency may take the form of needing to hold a person's hand when going downstairs, requiring someone to lift her wheelchair into a car, or needing even more basic support with activities of daily living (e.g., getting out of bed, dressing, toileting, feeding). Moreover, parents, siblings, or others who discount a woman's positive attributes and focus instead on her physical limitations, may help lower a woman's self-esteem, thereby increasing her vulnerability to abuse.
Combating abuse may overwhelm any woman who feels trapped and powerless. Health-care workers should try to identify abused women, looking for subtle signs (e.g., idiopathic chronic pain, headaches, unexplained traumatic injuries, centrally located bruising, emotional disturbance, weight changes). Frequently, the abuser may accompany the woman to visits. Thus, physicians should insist on speaking with the patient privately, whenever possible. After identifying situations of abuse, health-care workers should locate accessible shelters, counseling services, and alternative living situations.48
The psychosocial and sexual needs of women with disabilities have many things in common with those of nondisabled women. Access, education, and empowerment can improve communication between these women and their medical providers, ultimately improving their quality of care.