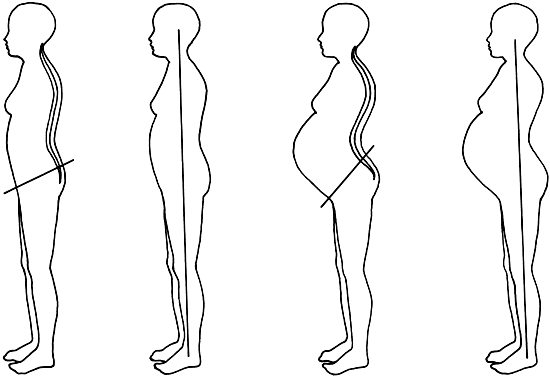
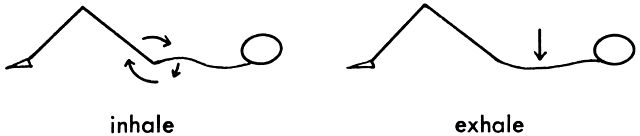A regimen of regulated exercises, done slowly and deliberately and without
strain or to the point of fatigue, includes all areas of the body
and assists with the postural correction described previously. These exercises
improve tone and elasticity of slackened or stretched muscles (abdominals, rhomboids, upper back and neck muscles); stretch shortened
muscles (lower back and pectorals); reduce tension in joints of the
pelvis, shoulders, hips, and knees; support breasts by strengthening
pectorals; and improve posture and increase vital capacity of the lungs. Although
in many childbirth preparation classes a variety of exercises
are taught,13,17,18,19,57,58 the following basic examples can be easily explained by the physician
or midwife at the prenatal visits. Guidelines for Exercise During Pregnancy/Postpartum - Regular exercise (3 times/week) is preferable to intermittent activity.20
- All exercises are done slowly and deliberately. Jerking or bouncing movements
that strain joints should be avoided. Wooden or securely carpeted
surfaces will reduce body shock and provide sure footing.
- Activities requiring jumping, jarring motions or rapid change of direction
should be avoided because of joint instability, and competitive activities
and contact sports should be discouraged
- Vigorous exercise should be avoided in very hot, humid weather (unless
in an air-conditioned environment) and during periods of febrile illness.
- It is vitally important to begin any exercise session with a period of
warm-up exercises such as arm circling, shoulder and neck rotations, trunk
flexion, and gentle knee bends.57 This should be followed by stretching of the various muscle groups in
the arms, legs, and trunk to prevent damage of muscle fibers and joint
strain; these may include gentle yoga stretches17 that are not taken to the point of maximum resistance.20
- Similarly, each session ends with muscle and joint stretches58 done slowly, without bouncing or jerky movements. “Cooling down” should
be accompanied by slow and comfortable breathing and followed
by a relaxation period.
- Heart rate should be measured before the exercise session and at time of
peak activity, and the target level of 140 beats per minute should not
be exceeded except in strong athletes who have consulted and established
their own target rates with their physicians.
- Strenuous exercise should not exceed 15 minutes in duration, and exercises
that employ or produce the Valsalva maneuver should be avoided.
- Caloric intake should be adequate to meet the extra energy needs of pregnancy
and lactation as well as the exercise performed. Liquids should
be imbibed liberally before, during, and after exercise to prevent dehydration.
- Maternal core temperature should not exceed 38.5°C.48,54
Each patient progresses at her own rate, starting by doing each exercise
for three or four repetitions and slowly building up to ten repetitions. Some
exercises include specific breathing techniques in conjunction
with the required movement (e.g. pelvic tilt with exhalation and release with inhalation; inhalation with
two-arm stretching to the sides to expand the chest and exhalation
with return to midline). Holding the breath on exertion of any exercise
is not helpful; continuous breathing is to be encouraged. No exercise
must be performed to the point of fatigue; rest and relaxation should
be interspersed during the session.37,57 Adding music to the exercise session enhances enjoyment and encourages
rhythmic movements. At no time should the the toes pointed, because this
often predisposes to calf cramps. Sit-ups or double leg raises should
not be done during pregnancy nor attempted until after the 6-week
postpartum checkup, because they put too much strain on the abdominals
and encourage diastasis.18,27,57 Positions that increase lumbar lor-dosis should be avoided to reduce possibility
of backache.59 Patients used to be discouraged from lying flat on her back for extended
periods of time to minimize the possibility of slowing circulation to
the uterus and prevent supine hypotension. However, there is no harm
in lying recumbent for short periods while doing exercises,20 and newest research46,55 shows that in healthy pregnancies, it is not necessary for the patient
to “never lie on her back after the fourth month,” as formerly
advocated by ACOG.21 There are some exercises (e.g. abdominal curls) that are most effectively done while lying on the back, and
the patient can change to alternate positions after each set. Exercises
that increase circulation in and around the pelvis should be
encouraged (e.g. pelvic tilt, abdominal exercises). Standing or side-lying positions can
be substituted for executing hip and leg movements normally performed
while recumbent. Time should be set aside each day for some exercise and, where feasible, exercise
should be incorporated into daily activities. ACOG guidelines
suggest exercising 3 times per week.1,21 Breathing Exercises Because of the difficulties pregnant women may have with respiration during
the second and third trimesters and the tendency to hold the breath
during exercising, deliberate attention to continuous breathing is
encouraged. This ensures a steady intake of oxygen as well as prepares
the woman for the need to maintain uniform and rhythmic breathing during
labor. Focused and relaxed abdominal and low chest breathing skills
improve ventilation and enhance relaxation during pregnancy, through
labor, and postpartum.11 Pelvic Tilt The pelvic tilt movement, which is slight, strengthens and tones the abdominal
muscles and stretches the lower back muscles. It is most helpful
for decreasing the lumbar lordosis, realigning posture, and reducing
low back pain. The patient lies on her back with both knees bent and feet on the floor
or examination table about 45 cm (18 inches) apart. She breathes in through
her nose, and as she breathes out through her relaxed mouth she
presses the small of her back against the floor and notices the upward
tilting movement of her pelvis and tightening in the abdominals. To
make sure she is doing this exercise correctly, the physician can place
her or his hand under the lumbar vertebrae and tell the patient to press
down onto the hand. The woman holds this position for a count of
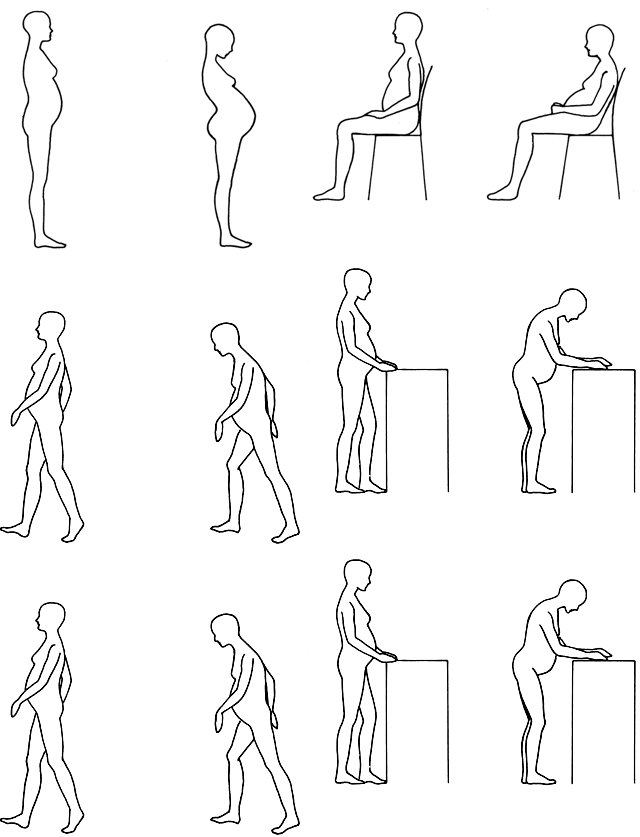
four and then slowly releases as she inhales and exhales (Fig. 3). Once mastered, this exercise can be done while sitting, standing, or
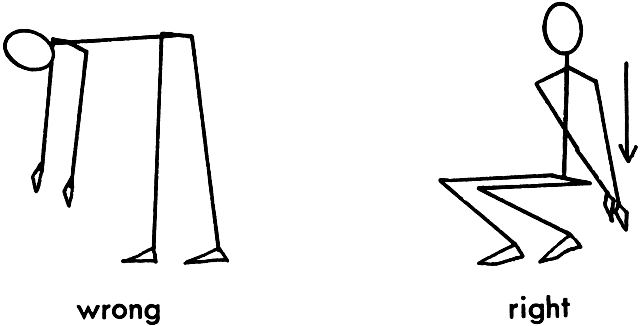
on all fours, with care being taken not to let the spine sag (Fig. 4). When doing the pelvic tilt in the standing position, slight bending
of the knees will ensure that the movement is performed in the pelvic
region and does not strain the hips. The pelvic tilt is particularly helpful
for backache during pregnancy, labor, and the postpartum period23,38,59 and is also useful as an abdominal toner. 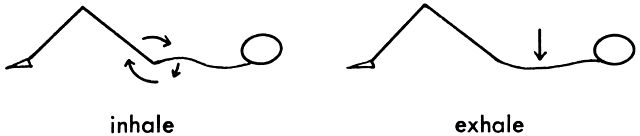 Fig. 3. Pelvic tilt in the supine position. Fig. 3. Pelvic tilt in the supine position.
|
 Fig. 4. Pelvic tilt while on all fours. Fig. 4. Pelvic tilt while on all fours.
|
Abdominal Toners Abdominal toners are progressions of the pelvic tilt exercise and are excellent
for toning and strengthening the rectus, or straight, abdominals
and the oblique abdominals. These muscles are used in second-stage
pushing and for postpartum curl-ups and waistline recovery. RECTUS OR STRAIGHT ABDOMINALS. The position is the same as for the pelvic tilt. A pillow placed under
the head reduces pressure on vena cava. With inhalation, the patient relaxes. As
she exhales, she tilts her pelvis as in the previous exercise, and
then lifts her head and slowly stretches both arms toward her
knees and holds this position for a count of four while breathing normally; she
then relaxes to the starting position (Fig. 5). If a diastasis is diagnosed (i.e. if two fingers can be inserted between the recti), instead of stretching
her arms forward the patient should brace her abdomen by placing both
hands across it, holding on to the opposite sides of the muscle bellies.18  Fig. 5. Abdominal curls with arm raising. Fig. 5. Abdominal curls with arm raising.
|
OBLIQUE ABDOMINALS. The position is the same as described previously. Again, the patient begins
with the pelvic tilt, but this time she lifts her head and both arms
and stretches toward the left knee and holds this position for a count
of four while breathing normally; she then relaxes slowly to the
starting position. The patient inhales and exhales a few times. With the next inhalation, she
relaxes, and on exhalation repeats the pelvic tilt, this time bringing
both arms to the right knee (see Fig. 5). Hip, Knee, and Ankle The starting positions for these exercises are either side-lying or standing. The
body remains relaxed as the patient inhales (Fig. 6A). If patient is lying on her side, both knees are bent. As she exhales, she
bends her knee toward her chest (Fig. 6B). While inhaling, she stretches her right leg forward by extending her
knee and dorsiflexing her foot (Fig. 6C). With exhalation, she brings the straight leg back to midline (Fig. 6D), and with inhalation brings it back to the flexed starting position. This
exercise is then repeated with the left leg while keeping the right
leg flexed after the patient turns to lie on opposite side. 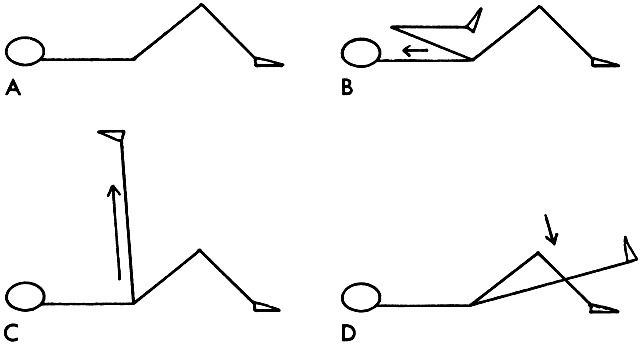 Fig. 6. Hip, knee, and ankle flexibility done in side lying position. Fig. 6. Hip, knee, and ankle flexibility done in side lying position.
|
Neck and Shoulder Muscles The exercise for the neck and shoulder muscles is done in the tailor sitting
position (i.e. sitting like a tailor with knees flexed) or standing17 (Fig. 7). The patient drops her head forward and gently circles it to the left, upward, to
the right, and forward in as large an arc as possible. This
is done slowly and deliberately and is repeated on alternating sides, while
being careful not to place pressure on the cervical vertebrae  Fig. 7. Neck and shoulder exercises. Fig. 7. Neck and shoulder exercises.
|
The shoulders are raised toward the ears, pulled backward, and slowly circled
down and forward. This exercise should be repeated several times; it
can also be done with the woman's fingertips on her shoulders
while lifting and circling the elbows forward, upward, and backward. Care
must be taken to keep the back straight and to keep the chin from
poking forward. These exercises are helpful in releasing tension in
the neck and shoulder muscles and should be followed by postural alignment
of the head, neck, and shoulders. Upper Back and Abdominal Side Flexors With the patient in the tailor sitting position or standing with legs apart
for balance, the arms are bent at the sides, and the fingertips are
placed on the shoulders. The right arm is stretched upward as the woman
inhales (Fig. 8). Keeping the torso erect, the patient stretches her rib cage and upper
back and then slowly lowers her arm to the starting position while exhaling. This
is repeated with the left arm and then with both arms at
once. The patient should progress to stretching her right arm and bending
to the left while keeping her torso in alignment; the patient should
then repeat this exercise by stretching her left arm and slowly bending
to the right (Fig. 9). These exercises allow for greater vital capacity by stretching the rib
cage and upper back and strengthening the abdominal side flexors in
preparation for postpartum recovery. When the patient's posture
demonstrates kyphosis, the pectorals are usually shortened; these stretching
exercises are most beneficial in correction of this problem. 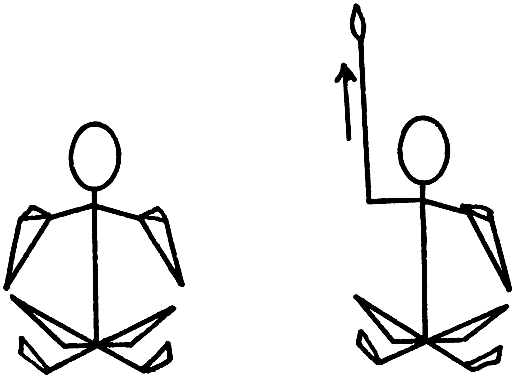 Fig. 8. Upper back and rib cage stretch. Fig. 8. Upper back and rib cage stretch.
|
 Fig. 9. Abdominal side flexors. Fig. 9. Abdominal side flexors.
|
Breast Support In the second and third trimesters, when breasts enlarge and increase in
weight, as well as during the postpartum period, additional support
of the breasts is necessary. Strengthening of the pectoral muscles, which
support the breasts, is achieved through use of an easy exercise. In the sitting position, the patient puts her hands together, as in prayer, with
her elbows flexed at shoulder level. She slowly presses her
hands together (Fig. 10). The position is held to a count of four and slowly released, and the
exercise is repeated several times. Normal, regular breathing should
accompany this exercise. 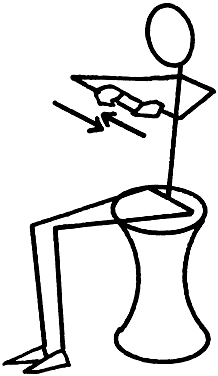 Fig. 10. Pectoral toning. Fig. 10. Pectoral toning.
|
Adductors and Hamstrings At one time it was thought that pregnant women should become accustomed
to stretching of the adductors and internal rotators of the thighs for
added comfort in expulsion. It was argued that use of stirrups for delivery
put strain on these muscles as well as the hip and pelvic joints, and
that with conscientious practice of some stretching exercises, the
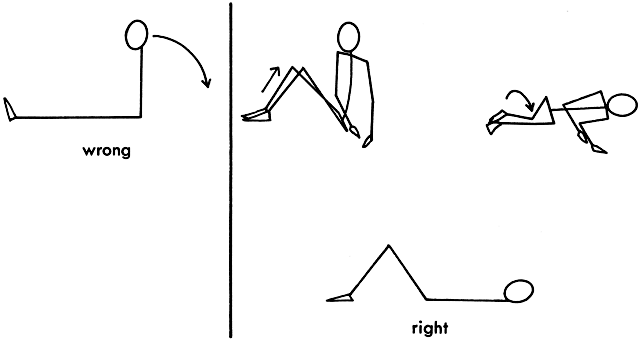
associated discomfort could be decreased. Incorrect teaching or learning of the exercise could lead to subluxation
of the pubic symphysis as a result of too-vigorous pressure on the knees
or a bouncing movement, which initiates the stretch reflex, causing
a rebound with further shortening and protective splinting of the muscles.18 The following exercise not only allows for some stretch of the adductors
but, more importantly, allows for stretch of the tight hamstrings and
low back extensors.17,18,57,60 The patient sits on the floor with her legs extended and separated as
widely as comfortable and her hands stretched forward with her arms kept
at shoulder level. Gently and slowly, she flexes forward from the hips, maintaining
her arms parallel to the floor while stretching them
forward, not toward her toes (Fig. 11).At first this movement may feel uncomfortable, but with practice the
discomfort eases. No jerking or bouncing movements should be done, only
stretching forward slowly, holding for the count of four, and slowly
releasing to the starting position.57 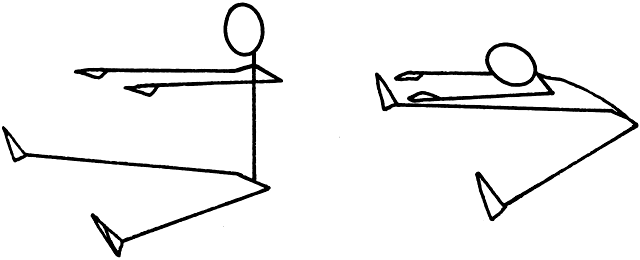 Fig. 11. Hamstring and adductor stretch. Fig. 11. Hamstring and adductor stretch.
|
Exercises Aiding Circulation As discussed in the section on cardiovascular and respiratory changes, pressure
from the enlarged uterus, dependency edema, dilated blood vessels, and
blood stasis cause swelling in the lower extremities, fingers, and
hands. Exercises to reduce swelling and improve blood circulation
decrease patient discomfort and fatigue. To increase circulation in
the legs and reduce edema of the feet, alternate flexion and extension
of the ankles causes pumping action of the calf muscles that promotes
the flow of blood (Fig. 12). These exercises should be repeated six to eight times and done slowly. Pointing
of the toes and extreme plantar flexion may result in leg
cramps and therefore should be avoided. Rotation of the ankles in wide
circles, first in one direction and then the other, is another excellent
exercise (see Fig. 12). The effects of this exercise on circulation can be enhanced if the legs
are supported and raised higher than the hips so that gravity assists
in return blood flow. 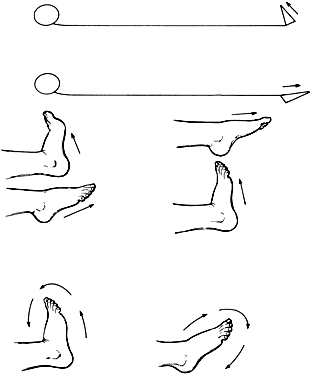 Fig. 12. Alternate flexion and extension of ankles and rotation of ankles in wide
circles enhances circulation. Fig. 12. Alternate flexion and extension of ankles and rotation of ankles in wide
circles enhances circulation.
|
For swollen fingers and wrists, the patient should sit with her elbows
flexed and supported on a table and her hands in the air. Alternate flexion
and extension of the fist or rotation at the wrists, with gravity's
assistance, reduces swelling and the associated tingling sensation. Postpartum, the risk of thrombophlebitis is increased when patients have
undergone cesarean birth under regional anesthesia with lengthy pressure
on the calf muscles. Foot and ankle exercises in the recovery room
and early ambulation improve circulation and prevent stasis. Pelvic Floor The importance of the pelvic floor (i.e. pubococcygeus or levator ani muscles) has been sadly neglected by obstetricians. These
several-layered muscles, both voluntary and involuntary, form
a figure-eight as they are slung in loops around the vaginal
and urethral sphincters anteriorly and the anus posteriorly. They form
the essential support of the pelvic organs, and their tone and elasticity
are vital during everyday life, pregnancy, and childbirth, especially
during second stage when the pelvic floor muscles must be consciously
released to facilitate delivery. These muscles must then be rehabilitated
immediately after the delivery or repair of the episiotomy, if
performed, and consistently during the postpartum period if this pelvic
organ support is to be maintained. Sphincter control of the bladder and rectum is a vital function provided
by the pelvic floor muscles. Women can be taught by their obstetricians/midwives
to release these muscles voluntarily during pelvic examinations
and during delivery of the infant's head so as to facilitate
its expulsion. Teaching these exercises in prenatal exercise classes, childbirth
education classes, or any exercise classes for all women
of all ages is mandatory and cannot be emphasized enough. Exercise of the pelvic floor, or Kegel's muscles, when frequently
and conscientiously practiced, maintains tone in these muscles, reduces
the possibility of urinary incontinence or difficulty with postpartum
urination, and helps prevent prolapse of the uterus.61 Another important function of the pelvic floor muscles is their active
contraction to enhance enjoyment during coital activity and reflex contraction
during orgasm.62,63 Kegel exercises entail gaining awareness of the muscles of the pelvic floor
and learning how to consciously contract and release them. The patient
is taught to stop and start the flow of urine midstream during urination
by using the sphincters, gently yet firmly, several times; this
exercise makes her aware of the action of these muscles. Once awareness
has been gained, frequent practice is necessary to maintain muscle
tone not associated with urine flow. For the first week, at least 6 repetitions
should be done slowly, maintaining the tension for at least 5 seconds
each time followed by release. Additional sets of contractions
are added to build up to at least 5 sets of 6 repetitions each day. Another effective exercise is to imagine that this hammock of muscles is
an elevator on the first floor that successively rises in a smooth, controlled, progressively
tighter fashion to the second, third, fourth, and
fifth floors, holding at each floor and then, just as smoothly, releasing
tension as the elevator descends to the fourth, third, second, and
first floors.22,35,57 The act of releasing and then “pushing into the basement” prepares
the patient for the release and bulging of the perineum necessary
for expulsion.57 Postpartum exercise of these muscles should be instituted soon after delivery. Conscious
effort should be directed to the contraction rather
than to the release of these muscles. These exercises are included in
preparation classes but can be taught by the physician at a prenatal visit, by
the nurse in the delivery room, and again during the postpartum
period. With early exercising of the pelvic floor, postpartum swelling is reduced, which
in turn reduces discomfort. Frequent contraction of these muscles
enhances circulation, promotes healing of the episiotomy, and strengthens
muscle tone. Incidence and severity of postpartum urinary incontinence
can be reduced by early initiation and frequent practice of
these exercises. As with all these exercises, contraction is done slowly and with concentrated
effort to facilitate toning of the muscles and to increase pelvic
organ support by tensing successively harder, holding for 5 to 6 seconds, and
releasing. Sets of six repetitions should be performed, and
the number of sets should be gradually increased. During muscle contraction, the
edges of the incision are pulled together rather than apart, and, with
this reassurance, frequent practice must be encouraged. Daily
exercise of these muscles, together with practice of the pelvic tilt, relieves
the low, achy feeling experienced by many women during the
postpartum period.63 |