Coital Frequency
As part of their original work, Masters and Johnson3 published the first scientific data on sexual activity during pregnancy (Table 2). A decrease in first-trimester sexual activity was noted, with an increase over prepregnancy levels in the second trimester and the greatest decline in activity during the third trimester. Falicov13 and Bogren5 found a similar decline in sexual activity in the first and third trimesters, with the second trimester similar to prepregnancy sexual activity levels. Kenny14 and Morris15 found less sexual activity only in the third trimester compared with prepregnancy levels.
TABLE 2. Sexuality According to Pregnancy Trimester Compared with Prepregnancy
Level
|
|
| First Trimester | Second Trimester | Third Trimester | ||||||
Study | Sample | Design | C | L | O | C | L | O | C | L | O |
|
Masters and Johnson, 19663 | 101 F, 79 M, US | Prospective | ↓ | ↓ | - |
|
| - | ↓ | ↓ | – |
|
Falicov, 197313 | 19 F, US | Prospective | ↓ | ↓ | - |
|
| - | ↓ | ↓ | – |
|
Kenny, 197314 | 33 F, US | Retrospective |
|
|
|
|
|
| ↓ | ↓ |
|
Solberg et al, 1973 | 260 F, US | Retrospective | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ |
|
Morris, 197515 | 114 F, Thailand | Cross-sectional |
| - | - |
| - | - | ↓ | – | – |
|
Tolor and DiGrazia, 197616 | 216 F, US | Cross-sectional | ↓ | ↓ | - | ↓ | ↓ | - | ↓ | ↓ | – |
|
Robson et al, 198117 | 119 F, GB | Prospective | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ |
|
Ryding, 198418 | 50 F, Sweden | Prospective | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ |
|
Reamy and White, 19858 | 52 F, US | Prospective | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ | ↓ |
|
Elliott and Watson, 198519 | 128 F, 87 M, GB | Prospective | ↓ | ↓ | - | ↓ | ↓ | - | ↓ | ↓ | – |
|
Pepe et al, 198720 | 175 F, Italy | Prospective | ↓ | - | - | ↓ | - | - | ↓ | – | – |
|
Bogren, 19915 | 81 F, 81 M, Sweden | Prospective | ↓ | ↓ | ↓ |
|
|
| ↓ | ↓ | ↓ |
|
Barclay et al, 199422 | 25 F, 25 M, Australia | Prospective | ↓ | ↓ | - | ↓ | ↓ | - | ↓ | ↓ | – |
|
Adinma, 199625 | 440 F, Nigeria | Prospective | ↓ | - | - | ↓ | -- | -- | ↓ | -- | -- |
|
Haines et al, 199621 | 150 F, China | Retrospective | ↓ | - | - | ↓ | - | - | ↓ | – | – |
Oruc, 1999 | 158 F, Turkey | Prospective | ↓ | - | ↓ | ↓ | - | ↓ | ↓ | – | ↓ |
|
Naim and Bhutto 200024 | 150 F, Pakistan | Cross-sectional | ↓ | - | - | ↓ | - | - | ↓ | – | – |
C, coital activity; F, female; GB, Great Britain; L, libido; O, orgasmic function; US, United States;
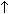 , more than prepregnancy level; ↓, less than prepregnancy level;
, more than prepregnancy level; ↓, less than prepregnancy level; 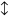 , equal to prepregnancy level; -, not measured.
, equal to prepregnancy level; -, not measured.Twelve other studies have shown a progressive decline in sexual activity during pregnancy. This progressive decline has been reported in the United States,4,7,16 Europe,17,18,19,20 Asia, 21 Australia,22 the Mideast,23,24 and Africa.10,25 Those studies failing to show a linear decline often used small samples,13,14 were cross-sectional in design,15 or used nonrepresentative populations.3
A variety of reasons have been suggested for this decrease in sexual activity. Early in pregnancy, some women report fears that intercourse will cause miscarriage; during the third trimester, both mothers and fathers report fears that intercourse or orgasm may harm the fetus.5 However, there is currently no strong research evidence of increased pregnancy complications associated with sexual activity during pregnancy. Other reasons for decreased coital frequency include physical discomfort associated with intercourse, particularly in the man-on-top position, and loss of interest in sex.
Sexual Interest
Masters and Johnson3 reported that “sexual tension and effectiveness of performance” declined in the first trimester of pregnancy in nulliparous women, whereas multiparous women reported little change (see Table 2). They described an improvement in performance and sexual arousal during the second trimester in women studied, with no significant differentiation between nulliparous and multiparous subjects. During the third trimester, most subjects reported a decline in sexual interest. Kenny14 found a decrease in libido during the third trimester only. Others have reported decreases in libido in women during the first and third trimesters, with no change from prepregnancy levels during the second trimester.5,13 All other researchers have found a steady decline in libido during pregnancy, regardless of parity.4,7,16,17,18,19,22 The evidence from the earlier studies is somewhat conflicting, but it seems reasonable to assume that most women experience a decline in sexual interest during the end of pregnancy.
Although inadequately studied, male sexual interest either remains unchanged22 or decreases during the third trimester.3,5 The effect of the partner's pregnancy on the male may vary—some men find their wives increasingly attractive, whereas others are fearful of “hurting them” or feeling that their intrauterine presence renders sex “improper.”12
Although associations between sociodemographic variables and sexual behavior has rarely been significant, sexual interest has been found to decrease more in expectant mothers with a stronger religious affiliation.4,5,19 However, sexual interest before pregnancy appears to be the best predictor of interest during pregnancy, regardless of gender.2,12
Orgasmic Function
Solberg and colleagues4 reported that orgasmic function decreased as pregnancy progressed (see Table 2). The percentage of coital acts leading to orgasm progressively decreased, as did the strength or intensity of orgasm experienced by the patient. In a small percentage of women, however, orgasmic intensity was noted to be increased at all stages of pregnancy. Although most researchers have reported a steady decrease in orgasmic function during pregnancy,7,17,18,23 one author reported decreases during the first and third trimesters but not during the second trimester.5 A small, retrospective study found no change in the frequency or orgasms throughout pregnancy.14 No data on male orgasm have been collected.
The consistent reduction in orgasmic function during pregnancy may be related to changes in physiologic response or to an active repression of orgasm to protect the baby.2
Noncoital Behavior
Solberg and colleagues evaluated noncoital sexual behavior.4 Sixteen percent of women had used masturbation to achieve orgasm before pregnancy. Most of these women did not continue this practice during pregnancy. Of those who practiced orogenital stimulation, approximately half did not use this type of sexual activity during pregnancy. Only 2% of women had recommendations given them by physicians or other healthcare personnel regarding sexual activities that might be used instead of coitus. Of these, hand stimulation was the activity recommended for both partners. As opposed to women, masturbation in men has been shown to remain stable throughout pregnancy.26
Activities that could replace sexual activities yet maintain intimacy of a couple's relationship have been addressed by Tolor and DiGrazia in a questionnaire of 216 women.16 Women indicated a preference for even less coital frequency than was actually occurring. It was noted that the women reported a high need for close physical contact during all stages of pregnancy. As an alternative to sexual intercourse, the most frequent response was simply wanting to be held. The investigators acknowledge that merely informing couples of the possible changes in sexual interest is insufficient and that the increased need for physical contact should be included in prepregnancy counseling.
One sexual activity is a potential danger to a women during pregnancy. An infrequently used type of cunnilingus consists of a partner's forcing air into the vagina. Several deaths to mother and fetus from air embolism have been reported after this activity.27,28
Behavioral Change
Because of anatomic considerations, coital positions differ as pregnancy progresses. Solberg and colleagues' data included an evaluation of coital positions used.4 There was a significant decrease in the male superior position, which had been used by couples approximately 80% of the time before pregnancy. In the last trimester, the side-by-side position was the most frequently used coital position, whereas the rear-entry position, rarely used before pregnancy, also became more popular. No association was found between position used and orgasm rate or coital frequency.
 12
12