Admission to Labor and Delivery
A patient who presents to a labor and delivery unit with symptoms of labor should have a thorough and systematic evaluation. The evaluating clinician should first make a rapid assessment of the clinical situation. If there are no signs of an obstetric emergency (e.g., vaginal bleeding, severe hypertension, shock), the clinician should continue with a careful history and physical examination. A complete history should be obtained, including past obstetric, gynecologic, medical, and surgical problems. Allergies should be noted clearly. The social history should be evaluated for the presence of toxic habits. The family history may suggest hereditary or multifactorial problems that could have an impact on the present pregnancy. Any current medications and their indications must be recorded. All of these components of the history should be obtained, even if they already were obtained and documented during the prenatal period. If the patient had prenatal care, careful attention should be given to any complications that may have developed (e.g., gestational diabetes, anemia). It is customary to document any prenatal laboratory results or testing. This provides the clinician with additional tools to evaluate the patient at the moment of admission. Any problems identified during the history should be evaluated for any possible impact on the course of labor, the delivery, and the neonate.
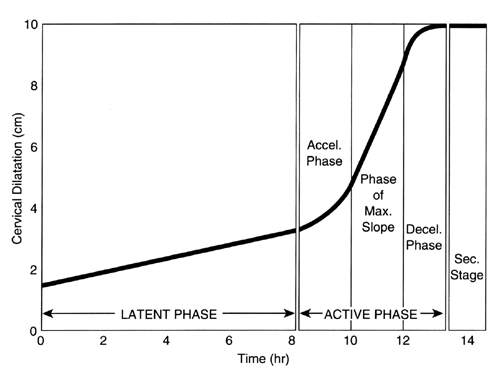
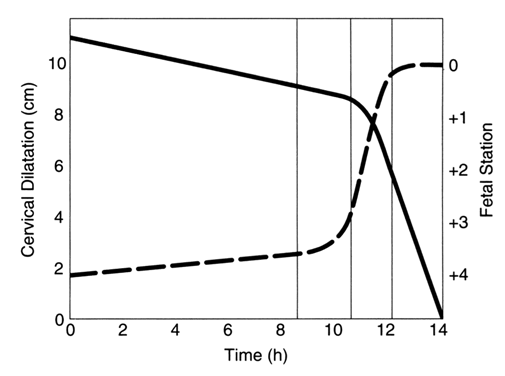
The physical examination for a patient being admitted to a labor and delivery unit should be as thorough as that for any patient being admitted to any other acute-care ward. After the vital signs are obtained, a systematic examination is rendered, the pelvic examination being reserved for last. During the abdominal examination, the clinician performs Leopold's maneuvers. This, in conjunction with the pelvic examination, allows the clinician to assess the fetal lie, presentation, and position. Careful attention should be given to the identification of any abnormalities, such as uterine tenderness, fibroids, or possible malpresentations. During the abdominal examination, the clinician should assess the fetal heart tones, using either a DeLee fetoscope or a Doppler device. If there are any difficulties obtaining the fetal heart tones, an ultrasound examination must be performed immediately. During the pelvic examination, the clinician assesses the type of pelvis. The cervix is palpated for the presence of dilation and effacement. During the pelvic examination, the station of the presenting part can be determined. The cervical examination should be plotted on graph paper (i.e., a partogram) for serial evaluation of the progress of labor. The cervical dilation is plotted on the vertical axis. The longitudinal axis is used to record time in hours (Fig. 1). Some partograms include a double vertical axis, so that dilation and fetal station can be plotted simultaneously over time (Fig. 2). By the end of the examination, the clinician should be confident of his assessment of the fetal presentation. If not, or if any other clinical indications are present, an ultrasound examination should be performed.
|
Occasionally, a patient presents in advanced labor. There might not be enough time to do a complete history and physical examination before the delivery. The clinician must make judgments based on the clinical situation and defer parts of the admission examination to after the delivery. No patient should be permitted to leave the labor and delivery unit without a complete examination.
Once the patient's history and physical are obtained and recorded, an assessment of the patient's risk status and labor situation is made so that the care of the patient can be individualized. Each institution should have a formal designation of what type of forms will be used for this purpose. In the United States, it is customary to obtain intravenous access on most laboring patients, although midwife nurses will frequently abstain from doing so. Some patients may request a heparin lock for more comfortable ambulation during early labor. If this is the case, intravenous solutions should be started at the earliest signs of dehydration or the development of a complication. At the same time intravenous access is obtained, a blood sample can be obtained for a complete blood count and for a type and screen. Besides the blood sample, a urine specimen is obtained for protein and glucose determination. If the laboring patient did not have prenatal care, the complete panel of routine maternal prenatal laboratory tests should be ordered. This panel can vary among institutions and types of patient populations.
During the course of labor, the fetus is monitored by either continuous or intermittent auscultation. In the United States, the majority of hospital births attended by physicians are monitored electronically. Further assessment of the fetus can be obtained from the quality of the amniotic fluid. If it is meconium stained, careful attention should be given to any abnormal fetal heart patterns. The presence of meconium suggests the possibility of a compromised fetus. If circumstances were to allow it, an ultrasound assessment for estimated fetal weight would provide the clinician with helpful information to assess the clinical situation.DeLee suctioning of the fetus at birth is essential in cases of meconium stained amniotic fluid, as is the presence of medical personnel trained to perform neonatal intubation.
Most of the discussion on the stages of labor that follows is based on the scholarly contributions of Friedman, who for the last four decades has documented the normal and abnormal patterns of human labor.
FIRST STAGE.
The first stage of labor is the period of time from the onset of labor to complete cervical dilation. This stage is divided into latent and active phases. The active phase is further subdivided into the acceleration, maximum slope, and deceleration phases of dilation.
Latent Phase.
The latent phase is the longest of all the phases of the first stage (Table 1). It has been determined that there is a negative correlation between the length of this phase and the amount of cervical dilation at the moment of onset of labor.6,7 Although multiparous patients appear to have shorter latent phases than nulliparous ones, this has not been a consistent finding.7
| Latent | Active | Maximum | Second |
| Phase | Phase | Dilatation | Stage |
| (h) | (h) | (cm/h) | (h) |
Nulliparas |
|
|
|
|
Mean | 6.4 | 4.6 | 3 | 1.1 |
Limit* | 20.1 | 11.7 | 1.2 | 2.9 |
Multiparas |
|
|
|
|
Mean | 4.8 | 2.4 | 5.7 | 0.39 |
Limit* | 13.6 | 5.2 | 1.5 | 1.1 |
* 5th or 95th percentile.
(Modified from Friedman EA: Labor: Clinical Evaluation and Management, p23, 2nd ed. New York, Appleton-Century-Crofts, 1978)
Active Phase.
The “transition” from the latent to the active phase is sometimes a very difficult one to identify. Some patients have a transition of labor while manifesting increased levels of pain and discomfort. Not infrequently, some have emesis as the cervix starts dilating at a faster rate. This probably is due to the stimulation of vagal nerve endings present in the cervix. The use of epidural anesthesia also makes this transition more clinically difficult to assess without the performance of a cervical examination. Although the transition from latent to active phase is difficult to identify, a dilation of 3 cm is accepted as the point beyond which the rate of dilation should increase to the rate expected in the active phase7: 1.2 cm/hour in the nulliparous patient and 1.5 cm/hour in the multiparous patient.8
Acceleration Phase.
The acceleration phase is clinically very difficult to document unless the clinician is performing frequent serial vaginal examinations. It encompasses the period shortly before the phase of maximum slope. In the nulliparous patient, this is compatible with a cervical dilation of 3 to 5 cm. In clinical practice, there will be a significant degree of variation in the length of this phase.
Maximum Slope Phase.
This phase has the most rapid rate of cervical dilation during labor. It typically occurs during dilation from 5 to 8 cm. According to Friedman,9 the plotting of the rate of dilation during this phase reveals a linear relationship. Other authors have suggested that the labor curve during this phase is hyperbolic.10,11 This is based on observations that reflected a constantly increasing rate of dilation as dilation progressed. The rate of dilation during the active phase is currently accepted to reflect a linear relationship. It is important for the clinician to be aware that it is during this phase that the descent of the presenting part will begin.12
Deceleration Phase.
The existence of the deceleration phase has been questioned.11 The debate on its existence is complicated by the short length of this phase, which is shorter than the length of the acceleration phase and easily missed if the cervical examinations are done infrequently. This phase rarely lasts more than 3 hours in a nullipara or 1 hour in a multipara. It usually extends from 8 to 9 cm until cervical dilation is complete. The descent curve reaches its maximum slope concomitant with the deceleration phase.13 The normal rate of descent of the presenting part is at least 1 cm/hour in the nullipara or 2 cm/hour in the multipara.
SECOND STAGE.
The second stage of labor is the period of time from complete cervical effacement to the delivery of the fetus. The presenting part is expected to descend at the same rate as during the deceleration phase.
THIRD STAGE.
The third stage of labor is the period of time from the delivery of the fetus to the delivery of the placenta. There are several signs associated with the separation of the placenta from the wall of the uterus. The uterus becomes globular, and there is a sudden gush of blood. This is followed by the umbilical cord's extending more toward the vagina and introitus. During this process, some clinicians massage the uterus using the Brandt-Andrews maneuver and maintain a steady pull on the umbilical cord. Any excessive tension on the umbilical cord could cause evulsion of the umbilical cord from its placental insertion, requiring manual removal of the placenta. Uterine inversion is another complication derived from overaggressive uterine massage and excessive tension on the umbilical cord. Placenta accreta also has been associated with this problem. If uterine inversion occurs, rapid correction of the inversion is essential. To decrease overall blood loss, the placenta should be removed after the uterus is returned to the abdomen. Subsequent to the correction of the inversion, uterotonic agents should be administered. The agents typically used are methylergonovine or prostaglandins. A more rapid action of these agents is seen if they are administered directly intramyometrially rather than intramuscularly. Many institutions routinely use a diluted intravenous oxytocin solution after the delivery of the placenta. Oxytocin should not, however, be administered as a direct intravenous bolus because it is associated with hypotension.14
The signs of separation of the placenta usually become evident within 5 to 10 minutes after birth. Classically, failure to deliver the placenta after a period of 30 minutes or more is defined as a retained placenta. This would justify a manual removal. If the patient is not having excessive blood loss, it is advised that the clinician wait for adequate sedation before performing the removal. This can be accomplished with a combination of narcotics and benzodiazepines, or under regional anesthesia if it was used for pain control during labor and delivery. In an emergency, however, the removal may have to be performed without analgesia.
During or after the delivery of the placenta, it is important that the patient be examined for any lacerations or hematomas. A first degree laceration involves the vaginal mucosa and perineal skin, leaving intact the muscle and fascia. In a second degree laceration, there is involvement of the perineal muscles but not of the rectal sphincter. A fourth degree laceration includes involvement of the rectal mucosa. Any patient with a significant laceration requires a pelvic examination several hours after the repair to exclude the possibility of a hematoma. In addition, all patients who had an episiotomy or laceration at the moment of delivery, should have a gentle manual examination of the repair and visual examination of the perineum before being discharged from the hospital. The patient should be instructed on the warning signs of episiotomy breakdown or infection. Table 2 describes the advantages and disadvantages of different types of episiotomies.
TABLE 2. Advantages and Disadvantages of Different Types of Episiotomy
| Midline | Mediolateral |
Advantages | Easy to repair | Extension to rectum |
| Better healing | or sphincter uncommon |
| Less painful |
|
| Smaller amount of blood loss |
|
Disadvantages | Higher risk of extension to rectum | Greater amount of blood loss |
|
| More painful |
|
| Difficult to repair |
Active Management of Labor
The active management of labor (AMOL), was first described in 1969 by O'Driscoll and colleagues.2 It was originally conceived as a technique for the prevention of prolonged labor, originally defined by the authors as more than 24 hours of labor, and in later publications as 12 hours. More recently,AMOL has been found to be a highly successful method for the prevention of labor dystocia and operative delivery.2,16,17,18 This technique was first implemented at the National Maternity Hospital in Dublin, Ireland, in 1968. Within the past 27 years, their total cesarean section rate has remained less than 10%.
The basic principles of AMOL involve the education of patients, attention to the accurate diagnosis of labor, close nursing or midwife support during labor, early amniotomy, early use of relatively high doses of oxytocin for the correction of labor abnormalities, and rigorous peer review.
In most of the published trials on AMOL, the criterion for patient enrollment has been as follows: term pregnancy (a minimum of 37 weeks), singleton, vertex presentation, nullipara, and spontaneous onset of labor.16,17,18 To our knowledge, there are no peer-review published reports documenting the use of this technique on multiparas or for induction of labor.
A very concise and clear description of the labor and delivery process is given to the patient during prenatal care visits. She is completely familiarized with all the principles of AMOL, and all of her doubts or concerns will have been answered before she is admitted to the labor and delivery unit. If there are no unexpected events, the patient is expected to have less anxiety regarding her labor, thus allowing her to develop a more comfortable attitude toward her labor process.
When patients are more aware of their labor process, unnecessary visits to labor and delivery for evaluation of possible labor can be prevented. In AMOL protocol, labor is defined as regular painful contractions in a frequency of at least one every 5 minutes. In addition to this, the patient should have at least one of the following three criteria: spontaneous rupture of membranes, complete cervical effacement, or the passage of bloody show. The evaluation of labor is carried out within 1 hour of the arrival of the patient to the unit. Every attempt is made to prevent having a patient walking for a prolonged period of time while still under evaluation for labor. If the patient does not meet the above criteria, she is encouraged to go home and to return when the labor symptoms are more intense.
One of the most important aspects of the AMOL protocol is the close support during labor. AMOL does not imply a more aggressive or interventional attitude toward labor, but an active involvement and awareness of the medical personnel with the events of a laboring patient. At the National Maternity Hospital, the nursing personnel perform duties similar to a midwife. This is done in close collaboration with the obstetrician-gynecologist. The nurse-to-patient ratio is 1:1. Every attempt is made to have a nurse attend a patient at all times. The nurse should be intimately aware of the progress and status of the patient. If there are any signs of an abnormality, she assesses the situation and consults the attending physician. Along with this, the constant presence of the nurse provides the patient with the so-called Dulla effect. “Dulla” refers to a constant companion of a laboring patient. This companion provides psycho-social support, with the goal of decreasing anxiety and stress during labor. The exact mechanism of action of the “Dulla” effect is unknown. This effect by itself has been found to be associated with a decreased incidence of cesarean section.19 The degree of participation of nurses is not limited only to labor management: Nurses also are permitted to deliver low-risk patients under the supervision of the attending obstetrician. These aspects of AMOL have made it difficult to implement in US hospitals. Several US hospitals have adopted the AMOL protocol, but not with the same degree of success as in Ireland. It is possible that if AMOL is implemented in US hospitals in association with midwives, it could achieve even better success.
Once the diagnosis of labor is made, an amniotomy is performed within 1 hour. Obviously, this should not be performed if the vertex is high and unengaged. With careful attention to the station of the vertex, the likelihood of an umbilical cord prolapse is rare.17 There are several reasons to perform early amniotomy. It allows the clinician to assess the quantity and quality of the amniotic fluid. The clinician would have a higher level of suspicion for the presence of a compromised fetus if scanty and thick, meconium-stained amniotic fluid was identified; this would also lead to a different approach to the labor management of the patient. Moreover, although it has been a source of debate in the literature, early amniotomy is generally considered to accelerate the labor process. A recent review20 of the literature on the effects of routine amniotomy on labor reached several important conclusions:
- The length of labor is shortened by an amniotomy, without having a significant
impact on the route of delivery.
- The reduction in the total length of labor consists mostly of a reduction
in the length of the first stage of labor.
- The amniotomy will be more effective in reducing the length of labor if
it is performed during the active phase of the first stage.
- Because of the shorter length of labor, there is a decreased utilization
of oxytocin for the treatment of protracted labors.
Without a comprehensive labor management plan, such as AMOL,21 the amniotomy may indeed fall short of having the impact of decreasing the incidence of cesarean deliveries. The amniotomy may increase the incidence of intrapartum abnormal fetal heart rate patterns, specifically variable decelerations, but this has not resulted in an increased incidence of low Apgar scores, neonatal acidosis, or morbidity.
After the amniotomy is performed, the patient is examined hourly for 3 hours, and then every 2 hours until delivery. This frequency of examinations has not resulted in an increased incidence of chorioamnionitis or postpartum endometritis. The goal of this close monitoring of the labor progress is to detect any dysfunctional pattern early. It is thought that with early detection and an attempt to correct a dysfunctional pattern of labor, there would be a higher likelihood of successfully correcting the abnormality, thus decreasing the need for operative delivery.
The ideal rate of progress under the AMOL protocol is 1 cm/hour during the first stage. The second stage is expected to last no more than 2 hours. A labor pattern associated with a rate of progress slower than this would require careful evaluation for a cause of such an abnormality. If the etiology is thought to originate from a dysfunctional pattern of uterine contractions, then oxytocin augmentation would be indicated.
The AMOL oxytocin augmentation protocol uses relatively higher doses compared with other protocols currently used in clinical practice.22 The protocol consists of an initial rate of 6 mU/minute, which is increased by increments of 6 mU/minute, to a maximum rate of 36 mU/minute. The optimal frequency of contractions with this augmentation protocol is seven in 15 minutes. The major goal of the use of higher dosages of oxytocin is to correct a dysfunctional pattern of labor before an intractable uterine dystocia becomes established. The oxytocin augmentation is limited to a period of 6 hours. Any patient that requires longer augmentation is thoroughly evaluated for factors other than dysfunctional uterine contractions that could account for the labor dystocia.
The major concerns regarding this augmentation protocol have centered on the issues of possible morbidity and mortality to either the mother or the fetus. Maternal issues include tachysystolic and tetanic uterine contractions, placental abruption, uterine rupture, postpartum uterine atony, and the need for transfusion. Fetal/neonatal issues include intrapartum meconium, fetal distress, acidosis, low Apgar scores, hyperbilirubin levels, admission to the neonatal intensive-care unit, seizures, death, and length of hospitalization. Several investigators have reported on the lack of association between AMOL augmentation and these factors.17,23,24 The use of relatively higher levels of oxytocin for augmentation of labor is not associated with a higher incidence of morbidity when compared with protocols that use oxytocin in a more conservative method. Of interest, the group at the National Maternity Hospital reported on more than 30,000 nulliparous patients who had AMOL according to the outlined protocol.24 There were no cases of uterine rupture secondary to the higher levels of oxytocin.
The use of AMOL has not resulted in a higher utilization of analgesia or anesthesia during labor.17 Patients can have intravenous sedation and regional blocks as judged clinically necessary.
No method of labor management or augmentation can eliminate the problem of labor dystocia. Even with AMOL, the clinician will have to determine when the augmentation is considered unsuccessful and an operative delivery indicated. If there is minimal or no dilation after 1 hour of optimal augmentation during the first stage, the clinician may consider proceeding with a cesarean section. Lack of descent after 1 hour of optimal augmentation during the second stage in the presence of optimal maternal pushing efforts is also an indication to proceed with an operative delivery, either vaginally or abdominally. Obviously if the patient has an arrest of dilation or descent disorder but an adequate pattern of spontaneous uterine contractions, the above indications for operative intervention would still apply. Whether and when to use an intrauterine pressure monitor for assessment of a dysfunctional labor is a clinical decision. The AMOL protocol neither requires nor excludes the use of this type of monitoring.
It has been demonstrated that the AMOL technique results in a shorter length of total labor. As a consequence of this, there is a decrease in the incidence of infectious problems, such as chorioamnionitis or endometritis.17 The incidence of labor dystocia also is diminished, resulting in a lower rate of operative delivery. This is accomplished with no increase in maternal or neonatal morbidity. These benefits also may translate into better utilization of the resources of the labor and delivery unit, as well as potential savings to the patient and society.