Hospitals and/or obstetric units providing maternity services for twin
deliveries should have a full range of personnel and equipment prepared
to (1) reduce the potential sequelae of preterm delivery; (2) decrease the risk of birth trauma; and (3) optimize the quality of resuscitative efforts provided to newborns. Requisite personnel for a twin delivery should comprise the following: two
qualified birth attendants (i.e., two obstetricians or an obstetrician-midwife team); an anesthesiologist
with an assistant if required; two neonatal resuscitation teams; and, finally, qualified
sonographic assistance. Equipment should include
sufficient clamps for two umbilical cords and sufficient resuscitative
equipment for two infants; ultrasound equipment; maternal and fetal monitoring equipment; a variety of oxytocic agents, including methylergonovine
maleate (Methergine) and prostaglandin analogs; a complete
setup for emergency operative intervention or cesarean section in
the delivery room; and setups for regional and/or general anesthesia. In the event that a hospital has inadequate facilities and/or staff, health
care providers and patients necessarily face the difficult decision
as to whether it is preferable to arrange an antenatal transfer for
delivery, often miles away from family and support systems, or to risk
the possibility of complications that may arise from inadequate facilities. Postpartum
transfer of newborns to neonatal intensive-care units
does not allow the same quality of resuscitation that can be obtained
when mothers are transferred antenatally and delivery takes place in
an optimally equipped facility. Five areas of obstetric practice (fetal monitoring, fetal imaging, anesthesia, cesarean
section and vaginal birth after cesarean section [VBAC], and
immediate neonatal care) impact on labor and delivery
in a twin pregnancy. Fetal Monitoring Monitoring of both fetal heart rates (FHRs) is essential throughout labor
and delivery. Newer technology permits monitoring both twins simultaneously, by
the external and/or internal route. Whereas auscultation
of FHR with a stethoscope or hand-held Doppler is sometimes advocated
in the absence of appropriate technology, such a system cannot detect
subtle postcontraction changes in the heart rates of both fetuses, even
when two examiners are present simultaneously. Moreover, from a cost-effective
point of view, use of the equipment to accomplish electronic
fetal monitoring is probably less labor intensive than intermittent
auscultation. Moreover, in the absence of dual-channel monitoring, it
is possible to elicit heart tones from one fetus for long periods of time, during
which the second fetus is essentially unmonitored. Two caveats are associated with dual-channel monitoring: (1) it is possible
to monitor one twin twice; and (2) it is possible to confuse the
maternal heart rate with bradycardia in one of the twins. The acute onset
of bradycardia in one twin should always alert the caregiver to check
the maternal pulse immediately to determine if the mother's heart
rate differs from the rate of bradycardia: if this latter rate is
identical to the rate of bradycardia, the transducers can then be adjusted
until the two FHRs reappear. In such circumstances, ultrasound can
be helpful in locating the heart and determining the FHR of the twin
suspected of having bradycardia. If this does not solve the problem, immediate
steps must be undertaken to determine the reason for the abrupt
change in the FHR in one twin. After the birth of the first twin, it is essential that the second twin
continue to be monitored. When the second twin enters the pelvis, and
if there is no contraindication to amniorrhexis, a spiral electrode can
be applied to the second twin's scalp or buttock. Before that
time, however, the FHR of the second twin can be assessed with a cardiotransducer
and/or a hand-held Doppler. The continued use of the tocotransducer
after the birth of the first twin permits simultaneous assessment
of the strength and frequency of maternal contractions. A comprehensive
protocol for monitoring twins in labor has been described by Eganhouse (Table 1).1 TABLE 1. Protocol for the Use of Monitors with Twins
- Apply EFM with mother in the lateral position or semi-Flower's.
- Use two different brands of monitors to improve signal quality.
- Synchronize internal clock of both monitors.
- Auscultate twin A and apply the cardiotransducer.
- Apply the tocotransducer.
- Auscultate twin B and discriminate from A's tracing. Apply cardiotransducer
for twin B.
- Adjust belts to old transducers in place. Try to accomplish monitoring
with two or three belts rather than four.
- Observe FHR tracings carefully to ascertain that both fetuses are being
monitored.
Document location of FHRs.
- Apply a spiral electrode to twin A as soon as possible.
- Ascertain that US and spiral electrode produce different tracings. (It
is possible to monitor twin A using two modes.)
- If only one tracing appears, reauscultate and readjust the cardiotransducer
for twin B.
- Observe for nonreassuring FHR patterns, including decreased variablility, late, severe
variable, or prolonged decelerations.
- Watch for nonreassuring patterns.
- Institute appropriate interventions for nonreassuring FHR patterns as needed.
EFM = external fetal monitoring; FHR = fetal heart rate; US = ultrasound.
(Modified from Eganhouse D: Fetal monitoring of twins. J Obstet Gynecol
Nurs 21:17, 1992)Whereas in twin gestations tracings from each infant may be synchronous, absolutely
identical tracings do not present as a clinical problem. When
two monitors record exactly the same signal, either a malfunction
is occurring or both transducers are monitoring the same fetus. No other
possibility exists. Further, the concept that dual-channel monitors
can be used in a manner such as to provide a single, “blended” signal
is erroneous.
Fetal Imaging Diagnostic real-time ultrasound should be available at all times during
labor and delivery of multiples. The presence of ultrasonography in the
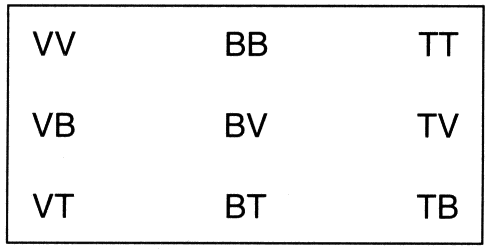
labor and delivery suite allows: (1) documentation of the positions
of both twins at the onset of labor; (2) early detection factors favoring
locked twins; (3) reassurance that the cord is not in front of the
presenting part (especially useful in cases of hydramnios); (4) immediate
detection of any change in the second twin's position during
and after delivery of the first twin; (5) visual guidance if internal
podalic version and/or breech extraction is used; and (6) visual assurance
of the position of the cord of the first twin during the intertwin
delivery interval. Chervenak and colleagues2 noted that ultrasonography is also indispensable for external cephalic
version of the second twin after delivery of the first. Chervenak and
associates3 reported success in 10 of 14 transverse lies and 8 of 11 breech presentations, respectively. In
these two small series, epidural anesthesia
enhanced the likelihood of success. In two of the unsuccessful attempts
at positional change, the weight of twin B exceeded that of twin A by 500 g
or more. In the absence of ultrasonography to continuously monitor
position and FHR, external cephalic version is considered potentially
unsafe by many physicians. Anesthesia Scant data exist comparing general versus regional anesthesia for the delivery
of multiples. Regardless of which modality is contemplated antenatally
or at the onset of labor, a skilled anesthesiologist should be
available throughout labor in the event that immediate operative intervention is required. Several precautions should be observed when the patient is admitted to
labor and delivery, regardless of whether her status is characterized
as preterm or term: - Blood should be obtained and sent for type and screen. The risk of life-threatening
postpartum hemorrhage for mothers of twins or higher order
multiples is real, whereas cross-matching all singleton patients at
the onset of labor is not cost-effective and this practice is no longer
routine.
- Isotonic crystalloid solution should be infused intravenously (IV) to prevent
dehydration that would otherwise decrease uterine perfusion.
- All IV lines should be of sufficient diameter to allow fluid resuscitation
or therapy with blood or blood products.
- Ingestion of solid food is contraindicated. Some obstetric units prefer
a strict nil per os regimen; others permit ingestion of clear liquids. In either case, the
aim is to decrease the likelihood of aspiration of solid or partially
digested stomach contents.
- The mother's lumbothoracic spine should be evaluated in the sitting
position early in labor to facilitate insertion of an epidural needle
if deemed desirable or necessary. At the same time, the patient's
neck and airway should be evaluated in preparation for a rapid induction
of general anesthesia should that be necessary.
Regardless of which type of anesthesia is planned, or even if none is administered, steps
should be taken to prevent gastric acid aspiration
and its sequelae. The most popular combination of medications used to
reduce the risk of gastric acid aspiration is 30 mL of an oral nonparticulate
antacid, such as sodium bicitrate, together with 10 mg of IV metoclopramide
to enhance stomach emptying and increase the tone of the
gastroesophageal sphincter. The administration of an H2 blocker, such as ranitidine (50 mg IV), decreases the acidity of subsequent
gastric secretions. No adverse maternal or neonatal side effects
have been described after the use of these agents. Metoclopramide and
ranitidine may be begun as soon as the patient enters the active phase
of labor, and may be repeated every 6 hours. Before 1975, it was thought that regional analgesia and anesthesia were
contraindicated for multiple gestation. Practitioners were concerned
that regional blocks prolonged the duration of labor as well as increased
the risk of aortocaval compression, with resulting maternal hypotension
and reduced placental perfusion. This opinion changed in subsequent
years: currently, regional anesthesia is considered an excellent method
for pain relief during labor and delivery of twins.4 It allows continuous or near-continuous pain relief for the mother without
direct depression of the fetus, provided that the regional analgesia
is properly administered and complications are avoided. To enhance
patient safety and acceptability, regional blocks should be administered
by those who are experienced in administration of epidural analgesia
for normal deliveries.4 In the case of twins, analgesic blocks should not be started until obstetric
conditions are appropriate (i.e., frequent, strong uterine contractions producing an adequate rate of cervical
dilation).4 Many services place the catheter early on, but delay delivery of the anesthetic
dose until conditions are deemed favorable. Proponents of epidural anesthesia cite four main points to justify its
use4: - The need for maternal narcotics and sedatives is greatly reduced, thus
avoiding the fetal respiratory depressant effect associated with such
drugs.
- Perineal anesthesia prevents reflex bearing-down by the mother and permits
a more controlled delivery of the infant over a relaxed perineum.
- Operative delivery, common in twins, is facilitated by the presence of
epidural anesthesia.
- When required, postpartum manual removal of the placenta and/or manual
exploration of the uterine cavity are facilitated in the presence of adequate
anesthesia and in the absence of compromised uterine contractility.
Additional arguments in favor of regional anesthesia are as follows: premature
infants fare better, the likelihood of gastric acid aspiration
is decreased, mothers are more alert during recovery, and postoperative
pain can be reduced with appropriate medication and dosage. Continuous
lumbar epidural anesthesia, if used successfully for first-stage pain
relief, may be renewed to provide anesthesia for delivery. In some
circumstances, pudendal block or local infiltration may be used concomitantly. Regardless
of the type of anesthesia selected, however, two
factors are of overriding importance: the fetuses must be monitored throughout
labor and delivery, and the anesthesiologist must be present
and prepared to give general endotracheal anesthesia should circumstances
require it. Systemic narcotics may be administered with safety early in labor if due
regard is given their potential respiratory depressant effect on the
fetuses. Should delivery occur unexpectedly or at any time when drug
activity may still be present, naloxone (Narcan) should be administered
to the mother to reverse the narcotic effects before delivery and, in
an appropriate dose, to the infant to reverse narcotic effects after
delivery. The use of paracervical block is no longer favored because
of its association with fetal bradycardia. Psychoprophylactic methods of pain relief are popular in North America
and can be used as easily with twins as with singletons. They are not
only harmless, as far as obstetric outcome is concerned, but appear to
be a benefit to many patients. Indeed, when premature labor occurs, use
of psychoprophylaxis may minimize analgesic needs, as may the presence
of a trained labor coach or a doula. On occasion, rapid uterine relaxation is required. A small bolus of nitroglycerin (50 to 100 μg) is efficacious and apparently not harmful. In
the double dilution technique, 5 mg of nitroglycerin is diluted in 10 mL
of saline, yielding 500 μg/mL. The dilution procedure is repeated
so that 1 mL of the doubly diluted solution contains 50 μg. This
is an appropriate concentration for the bolus administration of nitroglycerin. When postpartum blood loss is severe, oxytocin should be administered after
the delivery of the fetuses. Some practitioners prefer to delay administration
of oxytocin until after the delivery of the placenta in
order to avoid its entrapment. Because oxytocin is not always effective, prostaglandin
F2 should be available in the delivery room for direct injection into the
uterus (through the abdominal wall) at a concentration of 0.2 mg/mL and
a maximum total dose of 1 mg. Cesarean Section and Vaginal Birth After Cesarean Section Patients with twin gestation should be cared for in an institution capable
of providing an emergency cesarean section should circumstances warrant
this. Institutions that cannot provide the means and personnel to
deliver infants of high-risk mothers by cesarean section in 30 minutes
or less should not attempt to provide care for multiple pregnancy. The vaginal delivery of twins after prior cesarean section was reported
as early as the 1960s, well before the present trend toward VBAC. Although
the 1988 Committee Opinion (No. 64) of the American College of Obstetricians
and Gynecologists stated that data were insufficient to evaluate
the safety of this delivery modality in twins, subsequent reports
support this practice. Nevertheless, the risk for maternal trauma in the form of scar rupture
is always present in association with VBAC. Intrauterine manipulations, such
as total breech extraction or internal podalic version, theoretically
enhance this risk, although data to support this contention are
lacking. Further, in the absence of data from comparative randomized
trials, the risk/benefit ratio of VBAC must be evaluated on a case-by-case
basis. Diverse elements merit consideration, including the patient's
desires and potential fears, the obstetrician's experience, and
the ability of the hospital to provide a safe vaginal delivery
or cesarean section with appropriate intrapartum monitoring by personnel
and technologic equipment 24 hours per day, 365 days per year. Also
to be considered is the indication for the prior cesarean. Permanent
indications (e.g., contracted pelvis) speak against VBAC except in cases of extreme prematurity, whereas
transient indications (e.g., failure to progress) favor VBAC. The use of epidural anesthesia does
not mask the pain of scar dehiscence/rupture, and whereas in the past
fetal heart tone decelerations were thought to be indicative of scar dehiscence/rupture, this
clinical sign is no longer deemed useful by all
knowledgeable parties. Immediate Neonatal Care Twins mirror, and at the same time magnify, the two major problems facing
obstetricians in the United States today: preterm delivery and low
birth weight. Under these circumstances the first few minutes of extrauterine existence
are of paramount importance to twins in terms of their ability to
survive and the degree of subsequent morbidity or lack thereof. Ideally, an
experienced pediatrician or neonatologist should be present at
the delivery. Although it may be acceptable for the obstetrician, anesthesiologist, or
delivery room nurse to provide emergency neonatal stabilization
for the deliveries of low-risk patients, this is less than
ideal for deliveries of twins. |