Anatomy
The uterus is still enlarged and raised out of the pelvis for several days to 3 weeks after delivery, making the tubes more accessible to abdominal surgical techniques and less attainable by vaginal routes. Therefore, almost all sterilization procedures in the early postpartum period are performed through abdominal incisions.
The fallopian tubes may be larger and more edematous, and the mesosalpinx, as well as the broad ligament, often contains enlarged, tortuous blood vessels in the early postpartum period. These conditions may make surgical procedures on the tubes more difficult and provide a greater opportunity for bleeding problems to occur. It is extremely important to identify the tubes throughout their entire length before any intervention to ensure that the proper structure is being occluded or divided. Both adnexal regions should be thoroughly inspected for any abnormalities. Likewise, the uterus should be evaluated for any significant or unexpected gynecologic disease.
Patient Preparation
When a patient inquires about sterilization, the procedure should be thoroughly discussed during the antenatal course. Topics covered should include timing, techniques, side-effects, complications, long-term effects, sexual ramifications, and the potential for reversibility and failure of reversibility. The patient's husband or partner should be included in the discussion, if practical, or at least the wife should be asked to impart the information to him. For completeness, the alternatives to female sterilization (i.e. contraception, male sterilization) should also be mentioned to the couple.2,3
Tubal sterilization procedures are among the most frequent sources of litigation. Adequate informed consent with chart documentation of the points mentioned earlier, especially failure rate and the most usual complications, is essential.4 Some physicians and hospitals may require the patient and her husband to sign a sterilization permit as well as the usual consent for surgery.
Preoperative laboratory studies should include evaluation of hemoglobin, hematocrit, and white blood cell count with differential. These studies may be obtained during labor in those patients who are to have immediate postpartum sterilization. Hospital regulations may require a recent electrocardiogram and/or blood chemistry profile, especially in those women with special medical situations or in those taking certain medications (e.g. steroids, diuretics).
A patient's bladder should always be emptied just before the sterilization procedure to minimize the risk of entering the bladder. An indwelling catheter is not necessary unless one is already in place or is advisable for other reasons (e.g., cesarean section, traumatic delivery). Other standard preoperative preparatory conditions must be met if sterilization is being performed as a separate procedure at a time other than immediately after delivery.
Timing of the Procedure
Tubal sterilization may be done immediately following the completion of the vaginal delivery or after the bladder peritoneum is restored over the uterine incision during cesarean section. Otherwise, the procedure is usually delayed to within the first 48 hours after delivery. There are advantages to both immediate and delayed procedures, and factors in the choice include patient and physician preferences, and issues involving anesthesia, and hospital routines. The advantage of performing the tubal procedure at the time of cesarean section needs no further comment.
If there are any significant complications or potential problems at or immediately after delivery, the tubal procedure should be delayed, sometimes indefinitely. Concurrent medical, psychological, or neonatal conditions may also warrant deferment. Additionally, if any uncertainty regarding permanent sterilization is expressed by the patient or her spouse during or after labor and delivery, it is best to delay the procedure.
Discussing with the patient the options of immediate versus delayed procedures is helpful. Some patients or couples prefer to wait for 12 to 48 hours to be as certain as possible that the baby is healthy. Others want no future pregnancy under any foreseeable circumstance, and the procedure may be done at any time.
A single anesthetic procedure, avoidance of a second operative protocol and procedure, and shorter hospital stay all favor doing the tubal surgery in the delivery room at the conclusion of the usual delivery procedure. Postoperative morbidity seems to be about the same regardless of the timing of the tubal surgery. It is important to remember that postpartum sterilization is an elective procedure and one should not proceed unless conditions are safe.5
Methods
The abdominal approach is used because of increased vascularity and because the size and location of the uterus permit easier access to the tubes via this method. Most physicians use an small, open laparotomy type of incision rather than laparoscopy unless the procedure has been delayed for more than several days and the uterus has decreased too much in size. There has been little enthusiasm or advantage shown for using the laparoscopic approach within the first 2 or 3 days after delivery. If laparoscopy is chosen as the postpartum technique, it should be performed only by physicians who have expertise in the method, because of uterine size and broad ligament vascularity.6,7
A periumbilical transverse incision is often used when the tubal procedure is done soon after delivery and the level of the uterine fundus is near the umbilicus. It is cosmetically more appealing, and there is less bleeding and less postoperative discomfort. The procedure may take slightly longer if this type of incision is used, and the exposure for inspecting the uterus and adnexa is more limited.
The other approach is through a longitudinal midline incision somewhere between the umbilicus and the symphysis pubis. The height of the fundus determines the specific location, as well as the possibility of using a preexisting lower abdominal incision. Choice of anesthetic is usually to redose an existing epidural if the catheter is still in place and functioning.8 Local infiltration into the abdominal wall and then into the mesosalpinx is a less common alternative.
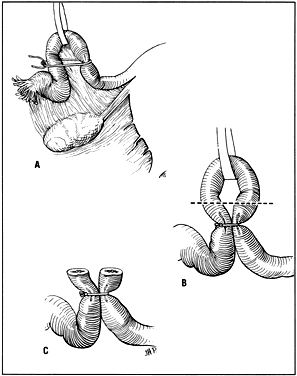
Several procedures for interrupting the passage of the egg through the fallopian tube are popular. Most often, a portion of the ligated tube is removed so that the cut ends will close over and separate. The Pomeroy method9 or its modifications remain the most commonly used tubal ligation procedures. A small loop in the tube is formed near the midportion by picking up the tube with a clamp. The loop is ligated at its base using an absorbable suture (Fig. 1); then a portion of the loop is excised. This is the simplest method, and if the cut ends and the surrounding mesosalpinx are carefully inspected for bleeding, complications are unusual. Some surgeons ligate the cut ends individually to ensure hemostasis. However, more inflammatory reaction and less likelihood of separation of the cut ends when dissolution of the suture occurs are the theoretical disadvantages of using more than a single catgut suture at the base of the loop.
|
A similar but less effective method, that of Madlener, also involves forming a loop of tube, but a portion is not removed. Instead, the tube is crushed at the base of the loop and ligated with a nonabsorbable suture (Fig. 2A). Occlusion but not division of the lumen is achieved. Care must be taken to not make the ligature so tight as to cut through the tube. Failures are attributed mainly to fistula formation at the ligature site.
|
In 1924, Irving described a technique of tubal sterilization at cesarean section.10 More adequate exposure of the uterus allows an easier approach for this method. A revision of this procedure was described in 1950.11 After cutting through the tube at the isthmic portion, the proximal end is buried into the posterior wall of the uterus. Others have modified this technique to include burying the distal end into the leaves of the broad ligament (Fig. 2B). This method takes longer, and there may be greater blood loss; however, the chances of tubal recanalization or pregnancy in the proximal stump are remote. Among these three methods, the least number of pregnancies have been reported with the Irving technique.
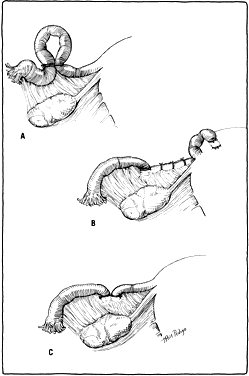
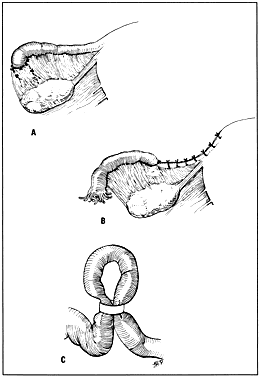
Other variations of tubal sterilization have been tried but never gained much popularity. The Irving method was modified to bury both cut ends into the broad ligament (Fig. 2C). Additionally, merely burying the fimbriated end of the tube in a pocket in the broad ligament (i.e. Aldridge technique) was thought to be a good temporary means of sterilization (Fig. 3A). Reversal by freeing the ends of the tubes was thought to be easily accomplished. Unfortunately, the rate of pregnancy after restoration was not as anticipated, especially if tubal or peritoneal infection occurred after the initial attempt at sterilization.
|
Cornual resection including an adjacent portion of the tube has also been described, but this procedure requires more exposure and results in greater blood loss (Fig. 3B).
The Oxford method of interposing the round ligament between the cut ends of the isthmic portion of the tube has never been prevalent in the United States, nor has the Uchida method of tubal resection at its ampullary portion been popular because of its complexity, potential for bleeding, and greater length of tubal resection.12 Another method of fimbriectomy following distal ligation with silk sutures attributed to Kroener also carries a high failure rate.
More recently, banding of the tube with nonabsorbable materials has gained popularity. Stainless steel clips and Silastic bands can be used to occlude the tubal lumina (Fig. 3C).13 Laparoscopy and open incisional techniques have both been used for application of these clips and bands in the postpartum period. Complications are minor; mild discomfort has been noticed at the site of occlusion. The effectiveness rate has been found to be very acceptable based on follow-up of patients for several years after application. Green and Laros give a complete description of most traditional and newer techniques in their monograph.6
Ancillary Procedures
Appendectomy has been routinely performed by some physicians at the time of postpartum tubal sterilization provided there are no medical or surgical contraindications. To add removal of the appendix to the procedure usually requires a larger incision, extra time, and an increase in blood loss. However, at least one study has indicated that there is no difference in postoperative morbidity.14
Removal of ovarian and paratubal cysts, lysis of adhesions, and resection of endometrial implants and small leiomyomas have also been done in conjunction with the tubal procedure. Again, the limitations of anesthesia and exposure might recommend against the additional intervention, but the surgeon must judge the possible benefits against any additional risks. Each patient must be evaluated on an individual basis.
Complications
Tubal sterilization procedures are usually not associated with significant risk or morbidity. Serious complications are reported in about 2% of all types of tubal sterilization procedures.2,15 Bleeding is the most common postoperative problem; it usually occurs as a result of inadequate ligature of the tube or failure to adequately ligate bleeding points in the mesosalpinx or broad ligament. The increased blood supply to these areas with varicosities in pregnancy lends itself to the possibility of hemorrhage and hematoma if meticulous hemostasis is not achieved.
The usual sequelae of intraabdominal surgery (e.g. paralytic ileus, abdominal distention, adhesions, intestinal obstruction) are associated with tubal sterilization procedures. Incisional infections and hematomas are less frequent but occasionally occur, especially in obese patients or in those with a chronic systemic illness.
Injury to the bladder is uncommon but may occur if the abdominal incision is too low or the bladder is distended. As mentioned previously, catheterization to ensure that the bladder is empty should be done immediately before all sterilization procedures.
Anesthesia problems are also uncommon, but inadequate anesthesia may occur, especially with regional techniques used for delivery. Supplementation with local or inhalation techniques may be necessary to complete the tubal procedure in the immediate postpartum period. The use of continuous conduction anesthesia may allow for more prolonged and consistent levels when sterilization is combined with delivery.
Precautions when using general anesthesia from the immediate postpartum period to several days after delivery are essential to minimize the possibility of aspiration and its sequelae.16 Residual gastrointestinal changes due to pregnancy make preoperative preparation especially important.
The Pomeroy method and its modifications have the fewest overall operative complications.
Side-Effects
The short-term puerperal difficulties stem mainly from discomfort at the incision site and at the points where the tubes have actually been ligated or divided. It is unusual for any significant abdominal discomfort to persist beyond 2 weeks.
There are usually no long-term alterations in a patient's menstrual or sexual functions. Irregularity of menses can be anticipated in a small number of patients (<5%). The cause of the menstrual dysfunction is not clear, nor does it always bear a direct relation to the tubal procedure. Thus, the existence of a true post-tubal syndrome remains controversial.17,18
A number of recent studies on patient regret following tubal sterilization emphasize the need for time for adequate, early, and repeated predelivery counseling.2,19,20 Youthfulness (<30 years at sterilization), poststerilization family events, and discovery that the procedure is not protective against sexually transmitted diseases are the most common causes of later regret.
Effectiveness
With various tubal methods, the overall failure rate in large series is less than 1%. Among the procedures discussed, the Irving and Uchida methods are associated with the fewest subsequent pregnancies, and the Madlener and Kroener methods are associated with the highest number. The Pomeroy procedure is not only the safest of the methods mentioned but also has a very acceptable level of effectiveness. The highest failure rates occur with methods causing minimal tubal damage, but these methods provide the maximum potential for reversibility.21
Tubal sterilization at cesarean section was reported to have a two to three times higher failure rate than that following vaginal delivery; however, this belief has not been sustained.6,22,23 Explanations for the increased pregnancy rate include greater congestion in the tube and mesosalpinx and less careful attention at surgery to the portion of the tube chosen for interruption. A portion of the tube with a relatively avascular area in the mesosalpinx beneath it is the ideal area for tubal sterilization.
The three most common causes of failure are luteal phase pregnancy if the procedure is delayed beyond 30 days from delivery; occlusion of the wrong structure, most often the round ligament; and most frequently, recanalization of the severed ends of the tube. Although there is an increased incidence of ectopic pregnancy in failures of tubal sterilization (5% to 12%), no single technique seems to predispose to this condition.24 Some recent reports indicate that the risk of ovarian cancer may decrease in women who have had tubal sterilization procedures.2
Reversibility
The rate of intrauterine pregnancies following reconstructive efforts on fallopian tubes varies with the type of tubal sterilization procedure that was done. Newer microsurgical techniques have improved the pregnancy rate after reversal; however, the prognosis is still guarded. The technique of reconstruction depends on the method of sterilization, the length of the proximal patent tubal segment, and the condition of the infundibulum.
Results have been most successful in those patients who have had an end-to-end anastomosis of the tube after sterilization by the classic Pomeroy method. One group reported a 39% pregnancy rate.25 With the newer assisted reproductive techniques (ART) and procedures, the need for reversibility of tubal occlusion is not as frequent.