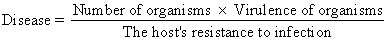Host resistance, or host defense, refers to the sum of all host attributes
mitigating the infectious properties of microorganisms. Therefore, host
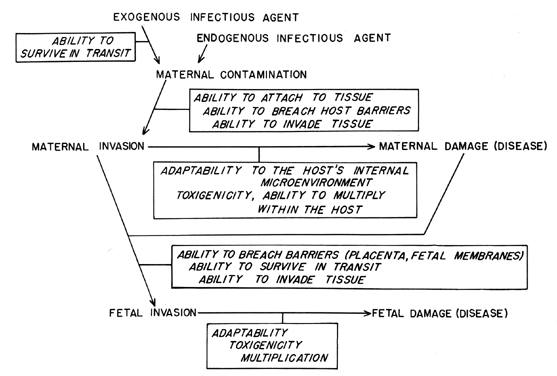
resistance to infection encompasses a variety of components (Fig. 4). Characteristically, an invading microorganism first encounters some
barrier during its entry into the host; next, it comes in contact with
nonspecific defenses; and finally, it activates the host's immune
system. 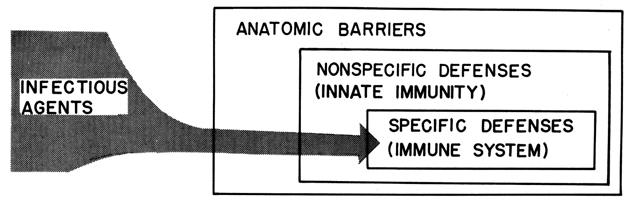 Fig. 4. Resistance to infection: sequential involvement of various aspects of host
defense in protection against infectious challenge. Fig. 4. Resistance to infection: sequential involvement of various aspects of host
defense in protection against infectious challenge.
|
The past 2 decades have been characterized by such an astounding proliferation
of knowledge in the field of immunology that the significance
of the nonspecific defenses is often in eclipse. The nonspecific defense
system is important for two reasons: First, before active immunity
becomes effective, the immune system requires both a sufficiently large
antigenic exposure to become activated and adequate time for lymphoid
proliferation to take place; thus, the nonspecific defenses protect
the host from being overwhelmed by an infectious process prior to activation
or specific immunity. Second, the nonspecific defense system is
more frequently iatrogenically compromised in the pregnant patient than
the specific defense system. Nonspecific Defenses (Innate Immunity) PHYSICAL BARRIERS. The skin and mucous membranes provide the primary barriers to entry of
microorganisms into the host. The adequacy of these barriers is enhanced
by a variety of adjunctive antimicrobial factors. The skin, in addition
to its physical barrier function, is hostile to microbial invasion
because of its dryness and perhaps because of the presence of antibacterial
lipids. The mucosal surfaces of the body also possess adjunctive
antimicrobial properties that complement their barrier function. It
is becoming increasingly apparent that tissues which have a characteristic
microbial flora may be protected from microbial invasion by that
resident flora. Alteration of the indigenous microflora may be a prerequisite
for some infectious disease processes involving the upper respiratory
tract, gut, or vaginal epithelium. Phagocytic cells may also
be present in or on mucosal surfaces, and lysozyme and immunoglobul'm
A are also usually present. CELLULAR DEFENSES. The cellular defenses involve phagocytic cells with various functions. When
tissue injury occurs and microorganisms are implanted in the tissue, they
may be phagocytized by local “wandering” macrophages. Eosinophils
are abundant in skin, gut, vagina, and respiratory mucosa
and may fulfill a similar protective role. Elimination of organisms
from the tissue does not depend solely on resident phagocytes. Following
injury, an inflammatory response occurs in which circulating polymorphonuclear
leukocytes egress from the bloodstream and enter the site
of injury. If the organisms persist in the tissue for more than approximately 24 hours, tissue macrophages infiltrate the lesion and become
the predominant phagocytic cell type in the lesion. If the infectious
process extends to the bloodstream or is primarily blood borne, phagocytic
cells of the reticuloendothelial system (fixed macrophages) in
the liver and spleen are responsible for removal of microbial contamination. Three stages in the phagocytic process may be influenced by the host's
physiology or exogenous factors. First, the chemotactic phase is
characterized by the attraction of phagocytic cells, moving along a chemical
gradient of chemotactic factors, to the infectious agent. Chemotactic
factors include tissue components released when tissue is damaged, bacterial
components, and breakdown products of complement. The chemotactic
response is altered in uncontrolled diabetic states which can
occur during pregnancy. The second stage of the phagocytic event is
ingestion of the microorganisms. This step is aided by opsonic antibodies
and basic peptides released from damaged tissues. The third major
step in phagocytic defense is intracellular killing of the ingested microorganisms. A
variety of intracellular factors are reported to be involved
in intracellular inactivation of microorganisms within the phagocyte, but
of particular importance is the increased oxidative metabolism
of the phagocytic cell which accompanies the phagocytic event. The
hormonal status of the host may influence this metabolic response to
phagocytosis. HUMORAL DEFENSES. The phagocytic defenses described above take place in a milieu which contains
soluble antimicrobial factors. Transferrin, which is responsible for serum iron transport, also functions
as an antimicrobial factor by binding iron and thus making the host's
serum iron supplies unavailable for microbial growth. An analogous
iron-binding protein, lactoferrin, is present in milk. Lysozyme is an enzyme present in most body fluids and secretions. It depolymerizes
the peptidoglycan of the cell walls of Gram-positive bacteria, but
its activity is not strictly limited to Gram-positive bacteria. It
may cooperate with other antibacterial factors, expanding its inhibitory
role. β-Lysin, a heat stable antimicrobial factor, is active primarily against
a limited number of Gram-positive organisms. It is released from
platelets when they rupture and is therefore found in greater abundance
following trauma. The cationic or basic peptides are a diverse, poorly
characterized group of peptides with similar antibacterial activity. They
are generally of low molecular weight, are heat stable, and bind
to anionic bacterial cells. They are reported to diminish bacterial
respiration and to facilitate phagocytosis. Viral infection and endotoxemia cause elaboration of interferon, which
protects uninfected cells from vital infection. Interferon is species-specific
but not virus-specific and appears to be a glycoprotein with
a molecular weight of approximately 25,000 daltons. It is extremely potent
in small quantities. A zinc-polypeptide antimicrobial system has been identified in amniotic
fluid, but its role in host defense is not clear 7. Other nonspecific defense mechanisms probably exist but have not yet been
adequately studied. The involvement of ascorbic acid in antibacterial
defenses of the host has been proposed, and its cooperative effects
with hydrogen peroxide or copper ion in low concentrations have been
reported in in vitro studies. Additionally, it is now known that during
infection the body dramatically redistributes its zinc and copper for
reasons which are unknown. This will be an important area for future
research, paticularly in view of the recognized association between infection
and undernutrition. Specific Defenses (Immune System) CELLULAR IMMUNITY. The immune response is classified as cellular or humoral, depending on
the effector mechanism. Common to both humoral and cellular immune response
is recognition of an antigenic stimulus, blastogenesis, and proliferation
of a specific population of lymphocytes. For both cellular
and humoral immunity, macrophages may trap, process, and present the antigen
or some soluble message to the lymphocyte. In cellular immunity
the lymphocyte population stimulated is the T-cell population. The effector
cell may be the T lymphocyte itself. Although many of the activated
T-cells' activities are directed against mammalian cells (ie, tumor
or graft-cells), T-cells are important in defense against intracellular
bacterial infection and viral infection. The activated T-cell may
also produce an array of soluble factors such as interferon. Other soluble
factors summon macrophages to the site of antigen stimulation and
cause their activation. The activated macrophage is the principal effector
in cell-mediated antimicrobial immunity. HUMORAL IMMUNITY. Antibody. Humoral immunity results from the production of antibodies by plasma cells
derived from B lymphocytes. Antibodies belong to one of five classes
of immunoglobulins which possess different physical, chemical, and
functional properties. Of the five classes, however, only three have
any apparent role in antimicrobial immunity. IgG is quantitatively the
most abundant of the immunoglobulins and is active in the serum and interstitial
fluid and crosses the placenta. IgM is a larger molecule which
will not pass into the extravascular fluid or cross the placenta
and which, along with IgG, represents the main intravascular antibody
defense. IgA is the dominant antibody in secretions of the body's
internal and external surfaces. The antibacterial effects of antibodies depend on their combination with
the microbial agent. This binding to the infectious agent may inactivate
the microorganism or may promote phagocytosis of the agent by leukocytes. The
reaction of antigen with its antibody may also precipitate
a reaction with complement, resulting ultimately in damage to the infectious
agent's membrane and subsequent lysis of the microorganism. Complement. Complement is a group of nine separate proteins (C1 to C9) which act sequentially
in cascade fashion, analogous to the clotting sequence, to
produce a biologic effect. The classic pathway of complement activation
is initiated by combination of antibody with its antigen. The subsequent
orderly reaction of complement components C1q, C1r, C1s, and C2 to
C9 results in damage to the cell membrane. Other biologic activities
are generated during reaction of some of the components of the complement
system. Anaphylatoxin activity is generated by two reaction steps
and results in increased capillary permeability. Chemotaxis of polymorphonuclear
leukocytes is also promoted by complement components. Complement
bound to a microorganism may cause adherence of the organism to
host phagocytes, facilitating the removal of the organism. Viruses and
many bacteria are not lysed by effects depend on its associated opsonic
and chemotactic activities. Activation of the complement system is not limited to the classic pathway
involving all nine components. An alternate pathway which bypasses
C1q, C1r, C1s, C2, and C4 has been described. Initiators, including bacterial
endotoxin (lipopolysaccharide), zymosan, IgA, and subclass 4 of
IgG, react with components of the properdin system to activate C3 activator
and trigger the rest of the complement sequence (C3, C5 to C9). While
the lytic activity of this system is minimal, antimicrobial effects
are possible through generation of chemotactic and opsonic principles. COOPERATIVE EFFECTS OF ANTIMICROBIAL SYSTEMS. As indicated in the preceding paragraphs, the host defenses are many, and
some are ostensibly redundant. However, systems which seem distinct
may operate in concert, producing greater antimicrobial effects than
are produced by a single system. For example, phagocytosis occurs slowly
in the absence of opsonins; however, opsonizing entities are not derived
primarily from phagocytic cells but from the immune system or from
complement. Likewise, the lytic activity of complement is enhanced
by lysozyme. Lysozyme also operates synergistically with IgA to produce
a bactericidal effect on Gram-negative organisms which neither factor
produces alone. Such synergistic effects emphasize the importance of
the uncompromised host defense system, since cooperative effects may
amplify the effect of a single deficiency. Maternal Defenses Because of the profound changes in maternal physiology resulting from pregnancy, it
is appropriate to consider what effects these may have on
her resistance to infectious challenge. NONSPECIFIC DEFENSES. Pneumonia and, to some extent, influenza appear to affect the pregnant
woman more severely than the nonpregnant woman of the same age, suggesting
a defect in some intrinsic defense mechanism in pregnancy. The reason
for this is unknown, although diminished vital lung capacity and
the progesterone-induced hyperventilation may aggravate respiratory infections. Anatomic changes in the urinary tract occur during pregnancy and may predispose
to infection. The hormones of pregnancy cause a relaxation of
the ureter, which allows it to distend, resulting in the complement; in
these infections, its antimicrobial physiologic hydroureter and hydronephrosis
of pregnancy. Whether this is responsible for the susceptibility
of women with bacteriuria to upper urinary tract involvement is
not clear. Other reasons have been proposed. Bacteriuria has been associated
with a urine-concentrating defect. It has been suggested that
the normally high concentration of urea in the urine inhibits bacterial
growth. It is possible that dilute urine may predispose to infection. Finally, a
phagocytic defect may be involved in urinary tract infection
in pregnant women. The importance of barriers has been mentioned. In the pregnant woman the
vaginal epithelium and cervix are of particular importance as they relate
to ascending infection. Ascending intrauterine infection may be
caused by vaginal microorganisms. However, it was noted in one study 8 that as pregnancy progressed, changes in the vaginal flora occurred which
may be interpreted as being generally benign. The number of aerobic, Gram-positive
rods increased during pregnancy; most other groups, with
the exception of the yeasts, decreased in number. Bacterial interference
by the normal flora may offer some protection against infection. However, as
is well-known, the mechanisms responsible for colonization
by benign bacterial flora may predispose to yeast vaginitis. The cervical mucus plug is putatively the protective barrier between the
contaminated vagina and the normally sterile uterus. As the cervix becomes
more dilated, the mechanical barrier function of the cervical plug
obviously diminishes. However, certain components of the cervical
mucus may afford some protection against ascending infection. The presence
of lysozyme and IgA in cervical mucus and the presence of an uncharacterized
component that inhibits motility of Proteus have been documented. The fetal membranes represent an additional barrier. The time-dependent
increase in amniotic infection following premature rupture of membranes
attests to their importance. However, as a barrier, the fetal membranes
are not impermeable. Bacterial contamination of the amniotic fluid
can occur with intact membranes, but the contamination appears to be
minimal and probably is controlled by antibacterial factors in the amniotic
fluid. The clinician should keep the function of this barrier in
mind when performing amniocentesis and intrauterine fetal monitoring
and when managing the patient with premature rupture of the membranes. During parturition and thereafter, considerable alteration of these defenses
occurs. The barrier function of the membranes is gone. The uterus
contains blood and adherent clots which may provide a nidus for bacterial
proliferation. Retained secundines likewise may be the site of bacterial
growth. Vaginal or cervical laceration or episiotomy may provide
an additional portal for entry of organisms into the host, as may
sites of administration of paracervical or pudendal blocking agents. Further
threatening the mother in the puerperium is the dramatic change
in bacterial flora of the vagina within the first 3 days post partum 8. Group B streptococcal colonization nearly doubles, Baeteroides fragilis increases from 2.6% to 34.8%; E coli increases from 2.6% to 32%. Other groups of organisms are likewise increased. In addition to altering the nonspecific host defense, pregnancy may alter
the phagocytic defenses of the gravida. First, pregnancy causes a leukocytosis, primarily
of neutrophilic leukocytes. Whether this affords
any added protection to the host is not known. Pregnancy is not known to affect the chemotactic activity of phagocytes, although
it has been reported that hyperglycemia inhibits leukocyte
chemotaxis. Thus, unrecognized gestational diabetes may represent a compromise
of the host's defense. The hormones of pregnancy, particularly estriol, appear to enhance the
phagocytic activity of leukocytes and increase metabolic activities associated
with intracellular killing. In one study, however, it was found
that some pregnant women with bacteriuria failed to display leukocytic
hyperbactericidal activity 9. Soluble host defense factors may also undergo change during pregnancy. Transferrin
concentration increases during pregnancy, and serum iron concentration
declines. This should provide a more hostile environment
for bacteria which gain access to the bloodstream. Other soluble nonspecific
factors have not been adequately studied. SPECIFIC DEFENSES. The status of the immune system during pregnancy has been a topic of intense
interest to immunologists because the fact that the fetus is not
immunologically rejected implies that pregnancy alters the normal immune
responsiveness of the host. The question has not been resolved satisfactorily. Some
animal studies seem to support the concept of an immunosuppression
during pregnancy, but less information is available on
humans. It is known that the pregnant woman can rally an immune response, but
whether this response is equivalent to that of the nonpregnant
woman is not clear. Cellular Immunity. Because cellular immune responses are important in protection against
vital infections, the increased morbidity and mortality reported for pregnant
women with influenza, varicella, polio, herpesvirus, and coxsackievirus
infections have been cited as evidence that cellular immunity
is diminished in pregnant women. In addition, lymphocytopenia, thymic
atrophy, decreased tuberculin skin test reactivity, and prolonged skin
graft survival have also been associated with pregnancy and may reflect
depressed cellular immunity. Humoral Immunity. It has been shown that IgG levels diminish during pregnancy; IgA and IgM
levels do not change significantly. An increased rate of IgG catabolism
and transplacental transport is believed to account for the decrease
in IgG levels during gestation. Alterations in the complement system have been noted. Serum C3 levels are
diminished during the first trimester and rise throughout pregnancy, returning
to normal by 6 weeks post partum. However, C3 is abundant
in the serum, and a greater than 90% reduction in C3 is needed to effect
a reduction in total complement activity. Total complement has been
measured during pregnancy. Individual reports vary, and some of the earlier
literature gave conflicting data. However, recent reports, while
showing some difference in the control levels of complement, agree that
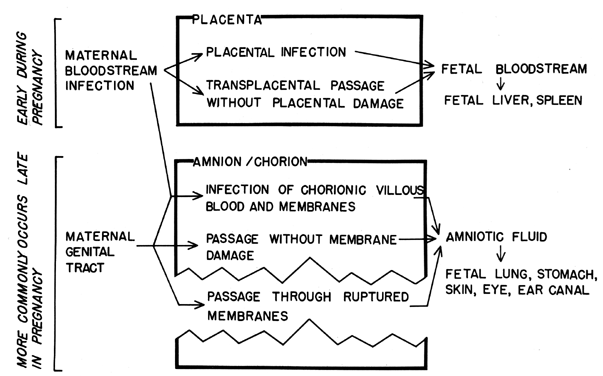
total complement activity increases significantly during pregnancy. Fetal Defenses THE FETUS. Two barriers protect the fetus from infectious assault, viz, the placenta
and the fetal membranes. The placental barrier is not as impenetrable
as was once thought. We have noted several organisms which commonly
cross the placenta, but in addition to those organisms, there is evidence
of the rare transmission of a larger group of organisms. Once an
organism passes the placenta, it is immediately in contact with the blood-borne
defenses of the fetus. Organisms which pass the fetal membranes are in contact with the amniotic
fluid before reaching the fetus. Although there was once controversy
as to whether amniotic fluid inhibited bacterial growth, it is now clear
that at or near term, amniotic fluid from well-nourished, healthy
women inhibits bacterial growth. Such inhibition is primarily due to
a zinc-polypeptide inhibitor, the activity of which is abrogated by added
phosphate ion. The phosphate-sensitive inhibitor is inactive when
large numbers of bacteria are present, suggesting why the minimal contamination
that may occur before membrane rupture may be contained but
the massive contamination occurring with prolonged rupture without labor
often leads to infection. The activity of this inhibitory factor is
variable and frequently is absent before the 30th week of gestation; it
is usually present at term and declines slightly in post-term pregnancies. No
residual inhibition of Gram-negative organisms is ordinarily
present after the addition of phosphate to amniotic fluid, although
occasionally, inhibition may remain for Gram-positive bacteria. This may
be due to any of several other known antibacterial substances in amniotic
fluid, including transferrin, immunoglobulin, lysozyme, fatty acids, β-lysin, spermine, and steroids. Phagocytes may also enter
the amniotic fluid, but their protective role is questionable. Phagocytosis
is inefficient in a fluid environment; surface phagocytosis usually
plays a more important role in protection of the host. The innate defenses of the fetus have not been well defined. It is known
that transferrin is present in cord blood at approximately haft the
concentration of that in adult serum. Phagocytic cells develop early in
pregnancy but may function suboptimally due to opsonic deficiency. Complement
in fetal blood is present in approximately half the concentration
of that in adult blood. Immunocompetence is dependent on the production of stem cells and the maturation
of these cells in the primary lymphoid organs. This occurs for
T-cells and, presumably, B cells at approximately the eighth week of
gestation. Therefore, by the time the fetus is mature, the necessary
immunologic equipment for producing an immune response is present, but
paradoxically, because the fetus is sequestered from antigenic challenge
during pregnancy, the neonate faces a hostile environment immunologically
unprepared. If infected in utero, the fetus responds immunologically, producing
IgM and IgG. IgM production by fetal cells in culture
has been detected by the 10th week of gestation, IgG is detected by
the 12th week, and IgA appears at the 30th week. In the absence of infection, the
fetus at birth has an IgG concentration that is greater than
the maternal concentration, an IgM concentration that approximates 10% of
the maternal levels and an IgA concentration that is less than 1% of
the maternal level. MATERNAL CONTRIBUTION TO FETAL DEFENSE. The fetal contribution to humoral immunity is minimal. The fetal levels
of IgG are primarily derived from the maternal serum. IgA and IgM do
not cross the placenta, but IgG appears to be actively appropriated by
the fetus against a concentration gradient. Passive diffusion provides
the fetal circulation with minimal quantities of IgG as early as the 38th
day of gestation. Levels remain low until the 17th to 22nd week. Thereafter, IgG
levels in the fetal serum rise sharply, with the result
that concentrations in maternal and fetal serum are approximately
equal by the 25th week. Subsequently, fetal levels continue to rise gradually, and
at term the fetal blood concentration of IgG is 5% to 10% greater
than the maternal blood concentration. The antibodies thus transferred
to the fetus reflect the maternal antigenic experience. Neonatal Defenses THE NEONATE. The neonate at birth is challenged with a variety of potentially hazardous
organisms, first in the birth canal and then from the environment, as
organisms begin to establish themselves as normal inhabitants of
the body. Little is known about the precise host defense deficiencies
in the newborn. Certainly, the umbilical stump is a likely portal of entry
for many organisms, as is the conjunctiva. At birth the concentrations
of IgM, IgA, serum transferrin, and complement have been found to
be diminished. The rapidity with which certain infectious processes
overwhelm the newborn further emphasizes the fact that the neonate must
be considered a compromised host. Some information is available on how the infant begins to assume responsibility
for his own immunologic defense. The passively transferred antibodies
which are present in his serum at the time of birth may be somewhat
protected from destruction by a diminished catabolic rate. The
half-life of IgG in the neonate is approximately 25 to 30 days as compared
with a 23-day half-life in adults. The rate of antibody synthesis, however, does
not keep pace with this decreased catabolic rate, and
IgG levels decrease. The decrement reported in one study 10 was 560 mg/dl, from 900 mg/dl at birth to 340 rag/ dl by the fourth week. Levels
begin to rise by the third month but are still subnormal at 22 months
of age. Significant quantities of IgA and IgM begin to appear
by the fourth month of life. MATERNAL CONTRIBUTION TO NEONATAL DEFENSE. The neonate is denied passively transferred IgG after birth but has a
ready source of IgA in his mother's milk or colostrum. In addition
to the immunoglobulin acquired in the milk, protection is afforded by
several other antimicrobial systems, including lactoferrin, a milk protein
which inhibits bacterial growth by a mechanism similar to that
of transferrin. Breast milk also contains complement components C3 and
C4, interferon, and unsaturated fatty acids which are inhibitory to staphylococci. Cellular
defensive elements, including T and B lymphocytes
and macrophages, are also present in breast milk. In addition to these antimicrobial factors, certain components, including
high lactose and the bifidus factor, promote the orderly colonization
of the neonatal gut with a benign microflora 11. In support of the concept of the protective activity of the mother's
milk are several reports which indicate that infectious disease problems
of the neonate are more likely if human milk is withheld 12,13,14. The effect may be particularly significant in geographic areas where
sanitation is poor and infectious challenge to the newborn is particularly
great. |