Prevention strategies have focused on early-onset GBS infection. Maternal
immunization is an attractive strategy because maternal IgG is transferred
across the placenta and appears to offer the neonate protection
from GBS.24,25,37 The main defense against GBS is antibody-dependent phagocytosis. Vaccines
that produce antibodies against the capsule of GBS have been made.41 Unfortunately vaccination to prevent GBS neonatal sepsis needs to overcome
several obstacles to have a place in clinical practice. Antibody
levels can be achieved in the majority of vaccines, but some vaccines
do not induce antibody development.42 Important genetic determinants of the antibody response may limit the
effectiveness of these polysaccharide vaccines. In a study of allotype
frequencies in Sweden, some women were found to have a genetic deficiency
in their ability to produce IgG antibodies against many bacterial
polysaccharides.43 A large vaccination trial is needed to resolve this issue. In addition, the
impact of protective antibody may be limited for premature infants
because transport of antibody across the placenta is reduced before 32 weeks' gestation. Conversely, immunoprophylaxis appears to offer a
rational approach to control GBS disease without the need for antibiotic
prophylaxis. Antibiotics given several weeks before labor has not reduced the maternal
GBS colonization rate when labor begins,10,44 probably because the genital tract becomes recolonized with GBS from the
rectal reservoir. Postnatal penicillin given to infants at birth has
limitations because 70% of the neonates with early-onset infection are
infected before birth.22 Preterm neonates are particularly likely to be infected before birth, and
postnatal penicillin given to preterm infants did not reduce early-onset
GBS infection.45 In another study, penicillin given at birth significantly reduced the
rate of GBS sepsis, but the overall sepsis rate was not reduced in neonates
who received penicillin because they had an increased rate of infection
from penicillin-resistant bacteria.46,47 Thus, the focus in preventing early-onset GBS infection has been on giving
intrapartum antibiotics after the onset of labor or ROM. Two randomized
studies found that antibiotics significantly reduced early-onset
GBS sepsis in high-risk groups with GBS48 and in heavily colonized neonates.49 Three other nonrandomized antibiotic trials also found a significant reduction
in early-onset infection when intravenous ampicillin was given
to GBS-colonized women with preterm labor or ROM lasting more than 12 hours.48,50,51 In the largest randomized trial, early-onset GBS neonatal infection was
reduced in the treated compared to the control group (0% versus 6%, p < 0.02).48 Neonates given intrapartum ampicillin were continued on ampicillin after
birth. It was estimated that at least 50% of early-onset GBS infection
could be prevented by this strategy. For effective intrapartum antibiotic
prophylaxis, however, the following steps are necessary: GBS identification, risk
identification, and protocol institution. In 1992, two strategies to help prevent neonatal GBS sepsis were published
by the American College of Obstetrics and Gynecology (ACOG)52 and the American Academy of Pediatrics (AAP).53 The AAP strategy has not been widely accepted because cultures recommended
at 26 to 28 weeks' gestation were poor predictors of exposure to
GBS at term. Recently, a strategy was published by the Centers for Disease
Control (CDC) that includes a culture at 35 to 37 weeks' gestation.4 These strategies are compared in Table 4. TABLE 4. Comparison of Antibiotic Prophylaxis Strategies and Estimated
Prevention of Early—Onset Neonatal GBS Sepsis
High—Risk Groups |
| | | | | Prior | | Weeks | Pregnancies | Early |
| Labor | ROM | ROM | Temperature | Pregnancy | GBS | Screen | Receiving | GBS |
Strategy | <37 wk | <37 wk | at Term | in Labor | with GBS | Bacteriuria | for GBS | Antibiotics* | Prevented* |
CDC4 | + | + |  18 h 18 h
|  38ºC 38ºC
| + | + | 35–37 | 27% | 86% |
ACOG53 56 57 | + | + |  18 h 18 h
|  38ºC 38ºC
| + | + | None | 18% | 69% |
AAP54 | + | + | >12 h |  37.6ºC 37.6ºC
| + | No (twins) | 26–28 | 3% | 51% |
*Estimated in Rouse et al.55
CDC = Centers for Disease Control; ACOG = American College of Obstetricians
and Gynecologists;
AAP = Association of American Physicians; ROM = rupture of membranes; GBS = group
B streptococcus.
Identification As mentioned, GBS colonization during pregnancy is not stable. The closer
to delivery the GBS culture is performed, the more predictive it will
be as to the risk of neonatal exposure at delivery. The culture result, however, needs
to be available by the time of labor. Thus, 35 to 37 weeks
is advised to perform cultures to identify patients with GBS
at term. This approach leaves unscreened those pregnancies that deliver
prematurely. The appropriate site to culture is the rectum and vaginal introitus because
these sites are most likely to contain GBS.4 The vaginal introital sample should be obtained without a speculum examination, and
the same swab can be introduced into the rectum and sent
as a single culture. Commercially available selective broth media (SBM
broth or Lim broth) should be used. The CDC has provided in detail the
technique of culture and the laboratory methods to use.4 High-Risk Group Identification and Strategy The AAP recommended that the following risk factors be identified because
of results from the only randomized treatment trial that used risk
factors48: labor or ROM occurring at less than 37 weeks' gestation, ROM occurring
more than 12 hours before delivery, and maternal temperature greater
than 37.5°C.53 In addition, intrapartum antibiotics were advocated for women with GBS-positive
pregnancies with a prior neonate with GBS infection and for
those with multiple gestations. The ACOG guidelines were slightly different than those developed by the
AAP. ACOG did not recommend routine GBS screening at any time during
pregnancy. Intrapartum antibiotics were recommended for the following: preterm
labor or ROM at less than 37 weeks, ROM lasting 18 hours or longer, fever
equal to or greater than 38°C during labor, and a previous
neonate with symptomatic GBS infection (Fig. 2).52 This strategy has not been tested for efficacy, and it does not include
low-risk pregnancies with GBS at term. 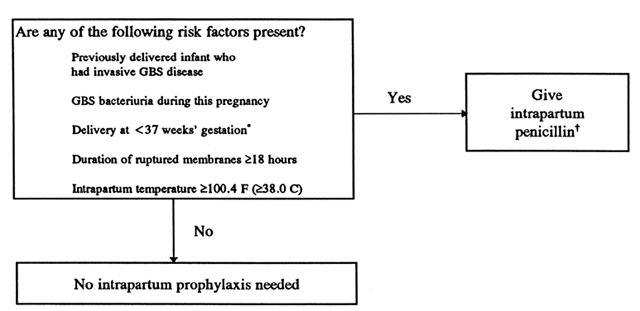 Fig. 2. Algorithm for prevention of early-onset of group B streptococcal (GBS) disease
in neonates, using risk factors. *If membranes ruptured at less
than 37 weeks' gestation, and the mother has not begun labor, collect
GBS culture and either (1) administer antibiotics until cultures are
completed and the results are negative; or (2) begin antibiotics only
when positive cultures are available. †Broader spectrum antibiotics
may be considered at the physician's discretion, depending
on clinical indications.(Schuchat A, Whitney C, Zangwell K: Prevention of perinatal group B streptococcal
disease: A public health perspective. MMWR 45:1, 1996) Fig. 2. Algorithm for prevention of early-onset of group B streptococcal (GBS) disease
in neonates, using risk factors. *If membranes ruptured at less
than 37 weeks' gestation, and the mother has not begun labor, collect
GBS culture and either (1) administer antibiotics until cultures are
completed and the results are negative; or (2) begin antibiotics only
when positive cultures are available. †Broader spectrum antibiotics
may be considered at the physician's discretion, depending
on clinical indications.(Schuchat A, Whitney C, Zangwell K: Prevention of perinatal group B streptococcal
disease: A public health perspective. MMWR 45:1, 1996)
|
GBS-positive pregnancies at term without risk factors are expected to represent
approximately 30% of cases of neonatal GBS infection.54 A nonrandomized trial suggested the efficacy of treating all women screened
and found positive for GBS.50 Thus, a CDC-appointed committee recommended a combined strategy of (1) treating
all unscreened, preterm, high-risk pregnancies (preterm labor
or ROM at less than 37 weeks, prior pregnancy with GBS infection, GBS
bacteria in the current pregnancy); (2) screening at 35 to 37 weeks; and (3) treating
all women in labor who were colonized with GBS at 35 to 37 weeks
irrespective of the risk for GBS infection. This strategy
has not been subjected to an antibiotic trial, but it is estimated to
prevent the greatest number of GBS infections (see Table 4). It also results, however, in the largest percentage of pregnant women
receiving antibiotics (see Table 4). Several nuisances exist in this strategy. All high-risk preterm pregnancies
regardless of knowledge of GBS status, and all term pregnancies
with GBS irrespective of high-risk factors, would be treated. Antibiotic
prophylaxis for pregnancy with ROM at less than 37 weeks' gestation, in
the absence of labor, could be started and continued until the
GBS culture result is known or withheld until the culture result is known
to be positive. This, of course, is also an option with the ACOG and
AAP strategies, because antibiotics would be given to all women with
GBS-positive term pregnancies at greater than 37 weeks who had a fever
equal to or greater than 38°C during labor, or ROM lasting more
than 18 hours. These three strategies are compared in Table 4.54,55,56 Although strategies differ, the adoption of one of these strategies to
prevent early-onset GBS sepsis is advocated,4 preferably the CDC or ACOG strategy because they are estimated to prevent
the greatest percentage of neonatal infections. All of these strategies
are estimated to be cost-effective. A full discussion of these strategies
is provided in the CDC recommendation.4 Women with GBS bacteriuria during pregnancy should be treated at the time
of diagnosis, and because these women are usually heavily colonized
with GBS, they should also be treated during labor without further screening. Likewise, women
who previously delivered an infant with neonatal
GBS infection should not be screened for GBS, but should be treated
in labor (see Fig. 2; Fig. 3). Unscreened pregnancies or known GBS-positive pregnancies with the major
risk factors (see Table 4) should also be treated (see Fig. 2 and Fig. 3). According to the CDC strategy, all pregnancies with a positive GBS culture
at 35 to 37 weeks should also be treated at the onset of delivery, regardless
of risk factors (see Fig. 3). 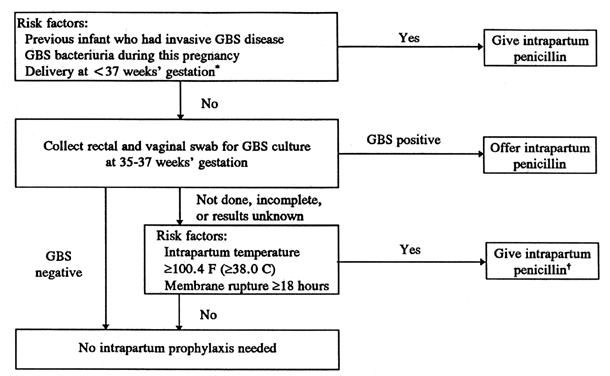 Fig. 3. Algorithm for prevention of early-onset group B streptococcal (GBS) disease
in neonates, using prenatal screening at 35 to 37 weeks' gestation. *If
membranes ruptured at less than 37 weeks' gestation, and the mother
has not begun labor, collect GBS culture and either (1) administer
antibiotics until cultures are completed and the results are negative; or (2) begin
antibiotics only when positive cultures are available. No
prophylaxis is needed if culture obtained at 35 to 37 weeks' gestation
was negative. †Broader spectrum antibiotics may be considered
at the physician's discretion, depending on clinical indications.(Schuchat A, Whitney C, Zangwell K: Prevention of perinatal group B streptococcal
disease: A public health perspective. MMWR 45:1, 1996) Fig. 3. Algorithm for prevention of early-onset group B streptococcal (GBS) disease
in neonates, using prenatal screening at 35 to 37 weeks' gestation. *If
membranes ruptured at less than 37 weeks' gestation, and the mother
has not begun labor, collect GBS culture and either (1) administer
antibiotics until cultures are completed and the results are negative; or (2) begin
antibiotics only when positive cultures are available. No
prophylaxis is needed if culture obtained at 35 to 37 weeks' gestation
was negative. †Broader spectrum antibiotics may be considered
at the physician's discretion, depending on clinical indications.(Schuchat A, Whitney C, Zangwell K: Prevention of perinatal group B streptococcal
disease: A public health perspective. MMWR 45:1, 1996)
|
The recommended antibiotics and doses are listed in Table 5. Penicillin is recommended over ampicillin because it may cause less resistance
in other bacteria. Penicillin-allergic patients should receive
clindamycin or erythromycin. Patients with fever during labor with
an unknown GBS status should receive gentamicin to inhibit Enterobacteriaceae, including E. coli, in addition to a penicillin. TABLE 5 Antibiotic Protocol for Intrapartum GBS Prophylaxis
Recommended: penicillin G | 5 million IV load |
| 2.5 million units IV every 4 hours until delivery |
Alternative: ampicillin | 2 g IV load |
| 1 g IV every 4 hours until delivery |
Penicillin allergy: | |
Recommended: clindamycin | 900 mg IV every 8 hours until delivery |
Alternative: erythromycin | 500 mg IV every 6 hours until delivery | (Adapted from Schuchat A, Whitney C, Zangwell K: Prevention of perinatal
group B streptococcal disease: A public health perspective. MMWR 45:1, 1996)An important aspect of early-onset GBS infection prevention is the administration
of antibiotics to premature and symptomatic neonates after
delivery. Asymptomatic infants at 35 weeks' gestation or older whose mothers
received antibiotic prophylaxis 4 hours before delivery can be
observed for 48 hours and not evaluated or treated. If antibiotics were
given to the mother 4 hours before delivery, a limited evaluation with
a blood count and blood culture and observation for 48 hours would
be recommended. Symptomatic neonates with suspected sepsis should receive
a full evaluation (blood count, blood culture, chest x-ray, and perhaps
a spinal tap) and antibiotic therapy (Fig. 4). A word of caution: this algorithm has not been field tested, because
all neonates were treated after delivery in the one randomized antibiotic
trial.48 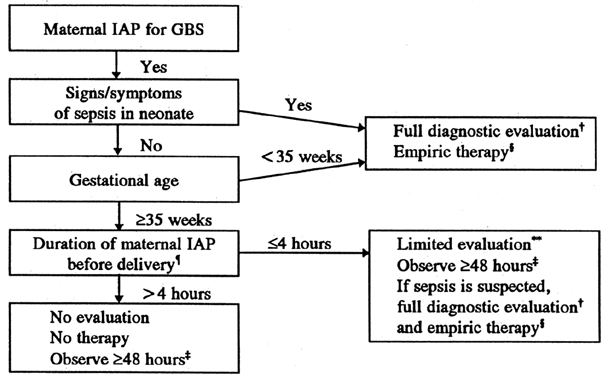 Fig. 4. Algorithm* for management of a neonate born to a mother who received intrapartum
antimicrobial prophylaxis (IAP) for prevention of early-onset
group B streptococcal (GBS) disease. *This algorithm is not an exclusive
course of management. Variations that incorporate individual circumstances
or institutional preferences may be appropriate. †Includes
a complete blood count (CBC) and differential, blood culture, and
chest radiograph if neonate has respiratory symptoms. Lumbar puncture
is performed at the physician's discretion. §Duration of therapy
will vary, depending on blood culture and results and the clinical
course of the infant. If laboratory results and clinical course are
unremarkable, duration of therapy may be as short as 48 to 72 hours. ¶Duration
of penicillin or ampicillin chemoprophylaxis. **CBC and
differential and a blood culture. ‡Does not allow early discharge.(Schuchat A, Whitney C, Zangwell K: Prevention of perinatal group B streptococcal
disease: A public health perspective. MMWR 45:1, 1996) Fig. 4. Algorithm* for management of a neonate born to a mother who received intrapartum
antimicrobial prophylaxis (IAP) for prevention of early-onset
group B streptococcal (GBS) disease. *This algorithm is not an exclusive
course of management. Variations that incorporate individual circumstances
or institutional preferences may be appropriate. †Includes
a complete blood count (CBC) and differential, blood culture, and
chest radiograph if neonate has respiratory symptoms. Lumbar puncture
is performed at the physician's discretion. §Duration of therapy
will vary, depending on blood culture and results and the clinical
course of the infant. If laboratory results and clinical course are
unremarkable, duration of therapy may be as short as 48 to 72 hours. ¶Duration
of penicillin or ampicillin chemoprophylaxis. **CBC and
differential and a blood culture. ‡Does not allow early discharge.(Schuchat A, Whitney C, Zangwell K: Prevention of perinatal group B streptococcal
disease: A public health perspective. MMWR 45:1, 1996)
|
Several issues about antibiotic prophylaxis require comment. First, none
of the antibiotic prophylaxis strategies presented in Table 4 is going to be totally protective against early-onset GBS infection. Approximately 14% of
GBS infection still would be expected with the CDC-recommended
strategy. Some of this would be related to the fact that
the culture method is not 100% effective and that approximately 3% of
women cultured at 35 to 37 weeks are found to have GBS during labor. The
impact of antibiotic prophylaxis in late-onset GBS disease is unknown, but
because late-onset infection is usually acquired from nonmaternal
horizontal GBS transmission, its impact may be small. The institution
of these strategies requires complex communication for successful
implementation. In one report, 37% of more than 2000 pregnancies had at
least one risk factor, but 13% of women with high-risk pregnancies did
not receive intrapartum antibiotics.57 This was similar to 20% of GBS-positive pregnant women who did not receive
intrapartum antibiotics in a university practice setting.58 Patients who do not receive prenatal care or those who deliver rapidly
before antibiotics can be administered are particularly likely to not
receive antibiotics. However, failure to administer antibiotics despite
the presence of risk factors and/or GBS colonization attests to the
difficulty of implementing routine treatment to all eligible pregnant
women. A strategy that uses antepartum cultures requires additional coordination
to ensure that cultures are performed and reported in a timely manner
and that reports are available 24 hours/day.4 It was also found that the availability of culture results before delivery
prompted up to one third of physicians to treat GBS in the genital
tract of the antepartum patient before labor, even though they knew
this treatment to be ineffective.59 This practice must be discouraged. Penicillin would be expected to result in a mild allergic reaction in 10% of
women, anaphylaxis in approximately 1 in 10,000,60 and death from anaphylaxis in 1 in 100,000.61 Although serious penicillin reactions are uncommon, a second direct problem
of antibiotics is the potential for the production of drug-resistant
bacterial strains. Antibiotic resistance would not be expected in
GBS (which is exquisitely sensitive to penicillin), but it would be expected
in other bacteria. The possible administration of even short-term
antibiotics in up to 30% of all pregnancies4 (see Table 4) would be expected to produce resistance to bacteria that could colonize
hospitals and eventually lead to clinically significant problems due
to antibiotic-resistant sepsis. Strategies aimed at GBS infection would have little impact on penicillin-resistant
bacteria.47 In fact, the majority of sepsis cases in newborns are not caused by GBS, but
rather by penicillin-resistant E. coli, other Enterobacteriaceae, Staphylococcus aureus, and anaerobic bacteria. Finally, intrapartum antibiotic administration has a major impact on the
clinical management of the newborn.57 In some instances, additional diagnostic tests or prolonged observation
in the hospital is given to antibiotic-exposed neonates. These additional
measures increase hospital costs. Although a reasonable guide is
provided in the CDC recommendations to follow the neonate (see Fig. 4),4 this algorithm has not been extensively tested. The algorithm is subject
to a variety of management interpretations, and it may take years to
know the impact of these variations on the prevention of neonatal GBS
sepsis. | 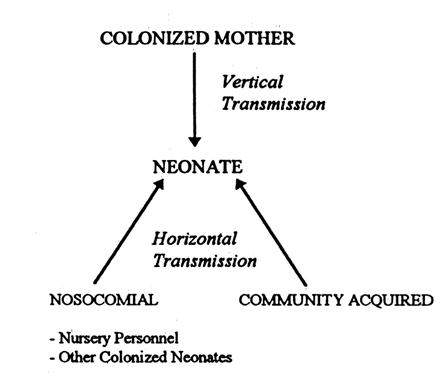
 0.001).
0.001). 7 days
7 days

