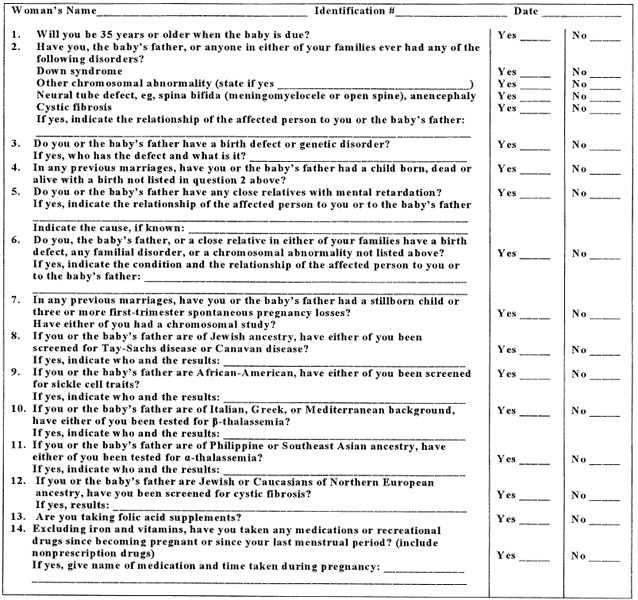
Some obstetricians consider it useful to obtain genetic information through use of questionnaires or checklists, often constructed to requiring action only to positive responses. Figure 1 reproduces a form that was recommended by the American College of Obstetricians and Gynecologists.2 A similar form was used by the authors in a survey.3 It showed that 21.4% of couples in a prenatal clinic gave at least one positive response, with 7.8% of the original sample couples requiring formal genetic counseling. Advanced maternal age was the most common indication.3 For all pregnancies, it is standard practice to determine whether a couple or anyone on either side of their families has a disorder that might prove heritable. The same holds true for gamete donors.4–6
|
One should inquire about the health status of first-degree relatives (siblings, parents, offspring), second-degree relatives (uncles, aunts, nephews, nieces, and grandparents), and third-degree relatives (first cousins). Record abnormal reproductive outcomes such as repetitive spontaneous abortions, stillbirths, and anomalous liveborn infants.4–6
The subsequent counseling may be sufficiently complex to warrant referral to a geneticist, or it may prove sufficiently facile for the informed clinician to handle. If a birth defect is detected in a second- or third-degree relative, the likelihood of that anomaly occurring in a pregnancy rarely proves significantly increased. Identification of a second- or third-degree relative with an autosomal-recessive trait ordinarily places the couple at little increased risk for an affected offspring, the exception being if the couple is consanguineous. Nonetheless, one should inquire about the status of relatives as distant as first cousins (of the fetus) because identification of certain disorders in such relatives may be the only clue that the couple may be at increased risk for autosomal-dominant disorders characterized by decreased penetrance or for X-linked recessive disorders.
In addition to identifying relatives with genetic disorders, one should record drug exposure to the woman and her partner. Identify not only those agents currently received but also noxious agents to which exposure occurred before pregnancy. The latter could be mutagenic.
Parental ages should also be recorded. Indeed, the most common indication for prenatal diagnosis is advanced maternal age, which warrants discussion regardless of a patient's difficulties in achieving pregnancy and regardless of a physician's personal convictions regarding prenatal diagnosis and pregnancy termination. Offspring of fathers in their fifth decade and beyond are at increased risk of new dominant mutations.
Finally, ethnic origin should be recorded. This is relevant to the genetic screening issues discussed later in this chapter. Ashkenazi Jews are at increased risk for offspring with Tay-Sachs disease and, hence, should be screened to determine heterozygote status (frequency is 1 in 27). The same holds true for Canavan disease. In the United States, Jewish people often are uncertain whether they are of Ashkenazi or Sephardic descent; thus, we recommend screening to all Jewish couples, as well as couples in which only one partner is Jewish. It also is advisable to offer routine heterozygote screening for β-thalassemia in Mediterranean people, sickle cell anemia in blacks, and α-thalassemia in Southeast Asians, Chinese, and Filipinos.7 The most recent addition is cystic fibrosis launched in 2000 with considerable foresight and specific recommendations. Table 1 summarizes current recommendations.
TABLE 1. Heterozygote Screening
Ethnic Group | Disorder | Screening Test | Definitive Test |
Ashkenazi Jews | Tay-Sachs disease | Decreased serum hexosamidase-A, possibly molecular analysis | CVS or amniocentesis for enzymatic assays or molecular analysis to detect affected fetus for hexosamidase-A |
| Canavan disease | DNA analysis to detect most common alleles | CVS or amniocentesis for molecular analysis to determine genotype of fetus |
Blacks | Sickle cell anemia | Presence of sickle cell hemoglobin, confirmatory hemoglobin electrophoresis | CVS or amniocentesis for genotype determination (direct molecular analysis) |
Mediterranean people | β-Thalassemia | MCV <80%, followed by hemoglobin electrophoresis | CVS or amniocentesis for genotype determination (direct molecular analysis or linkage analysis) |
Southeast Asians and Chinese (Vietnamese, Laotian, Cambodian, Filipinos | α-Thalassemia | MCV <80%, followed by hemoglobin electrophoresis | CVS or amniocentesis for genotype determination (direct molecular analysis or linkage analysis) |
Ethnic groups(In whites and Ashkenazi Jews should be offered; in other ethnic groups [Asians, Hispanics, blacks] should be made available) | Cystic fibrosis | DNA to detect specified panel of CFTR mutations (those present in | CVS or amniocentesis for fetal genotype determination. Definitive diagnosis on all fetuses is not possible, sensitivity varying by ethnic group. |
CVS, chorionic villus sampling; MCV, mean corpuscular volume.
Some centers offer not just Tay-Sachs and Canavan disorders to Jewish couples but also screening for Gaucher disease, Niemann-Pick disease, and cystic fibrosis. Relatively efficient screening is possible in Ashkenazi Jews by that ethnic group having only a limited number of mutations. Overall, one in seven Ashkenazi Jews is heterozygous for one of the disorders listed above.
 0.1% of general population)
0.1% of general population)