Traditional Amniocentesis: Gestation of 15 Weeks or Longer
Amniocentesis, the aspiration of amniotic fluid, has traditionally been performed at and after 15 to 17 weeks of gestation. At this stage of gestation, the volume of amniotic fluid is about 200 mL. The ratio of viable to nonviable cells in the amniotic fluid is relatively high,1 thus allowing timely culture and diagnosis of fetal cytogenetic abnormalities and providing women the option of pregnancy termination should an abnormality be determined.
Amniocentesis is routinely performed in an outpatient facility. An ultrasound examination should be done immediately before the procedure to evaluate fetal number and viability, perform fetal biometric measurements to confirm gestational age, establish placental location, and estimate amniotic fluid volume. In our hospitals, a fetal anatomic survey to screen for major anomalies is standard practice. In addition, ultrasonography may be useful in discovering maternal gynecologic conditions (e.g., leiomyomata) that could influence the technique and timing of the amniocentesis.
After the preoperative ultrasound examination has been completed, a needle insertion site is chosen. We prefer to insert the needle in the midline fundal area of the uterus, but this is not always the site at which the optimal pocket of amniotic fluid is located. Not infrequently, a lower uterine segment or lateral approach is required. If possible, we avoid the placenta; however, transplacental amniocentesis has not been shown to reduce the safety of amniocentesis.2–4 If tapping the optimal pocket of fluid requires traversing the placenta, we select the thinnest portion of the placenta possible through which the needle can be directed. The umbilical cord insertion site should be identified and avoided. The maternal bowel and bladder should also be located, because these should likewise be avoided. A local subcutaneous anesthetic (e.g., 2 to 3 mL of 1% lidocaine) may be used, but we usually find this unnecessary. After the maternal skin is cleaned with an iodine-based solution, sterile drapes are placed around the needle insertion site to help maintain an aseptic field. We prefer a 22-gauge spinal needle and recommend no larger than a 20-gauge needle.
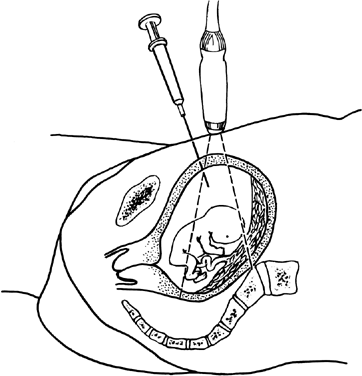
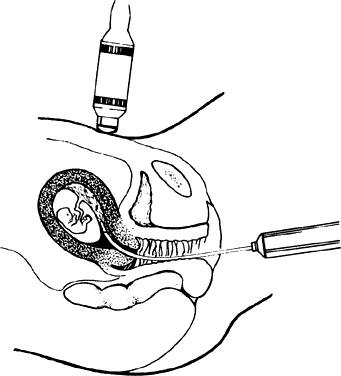
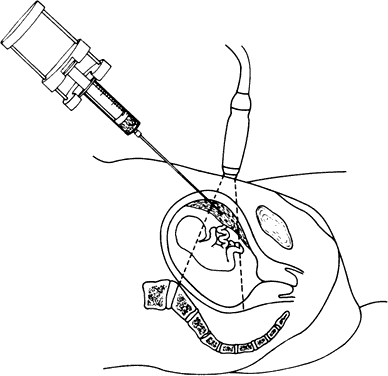
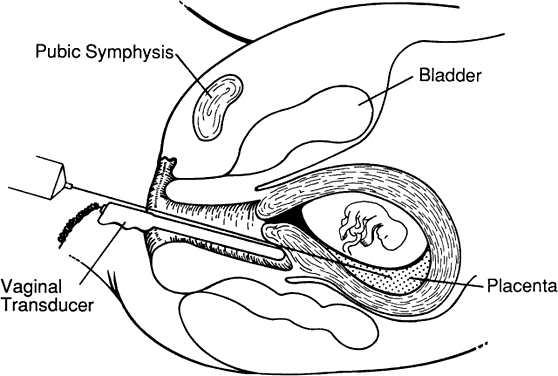
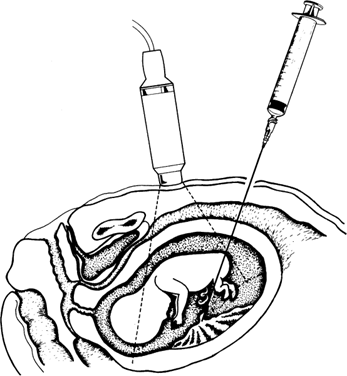
Ultrasonographic monitoring with continuous visualization of the needle should be used throughout the procedure. Ultrasound gel is applied adjacent to the insertion site, and a real-time ultrasound transducer is held in position such that the ultrasound beam is directed parallel to the planned needle track. Needle insertion should be performed with one smooth continuous motion until the needle tip is within the amniotic cavity (Fig. 1). Some practitioners locate the needle tip within the subcutaneous fat and assess the distance from tip to amniotic cavity as well as the appropriate needle angle required to successfully enter the amnion and avoid maternal structures and the fetus.
The first several milliliters of amniotic fluid are aspirated into a syringe. These first few milliliters are theoretically most likely to contain maternal cells; therefore, this initial sample is usually discarded or set aside for an AFP assay. For a second-trimester amniocentesis performed at 14 to 20 weeks inclusive, 20 to 30 mL of amniotic fluid is usually aspirated. After obtaining the amniotic fluid, the specimen should be clearly labeled and transported at ambient temperature to the laboratory.
The amniotic fluid aspirated is bloody in approximately 1% to 2% of amniocenteses. The blood, which is almost always maternal in origin, does not adversely affect amniotic cell growth. Indeed, the performance of a transplacental amniocentesis may increase the risk for a bloody tap; this has not been shown to have an adverse affect on the safety or accuracy of the amniocentesis. By contrast, brown or dark red or wine-colored amniotic fluid is associated with an increased likelihood of adverse pregnancy outcome. This color indicates earlier intra-amniotic bleeding, with hemoglobin breakdown products accounting for the pigment. Pregnancy loss eventually occurs in about one third of such cases.5 If the abnormally colored fluid is also characterized by an elevated AFP level, the risk for adverse perinatal outcome (fetal death, anencephaly, spontaneous abortion, or fetal abnormality) is usually further increased. Green amniotic fluid, presumably due to meconium staining, is apparently not associated with poor pregnancy outcome.6–8 By contrast, brown amniotic fluid has been associated with an increased risk of fetal aneuploidy.8
The propriety of administering Rh immunoglobulin (RhIG) to prevent Rh immunization in unsensitized women with Rh-positive fetuses remains controversial although widely done. Fetomaternal transfusion by disruption of the fetoplacental circulation logically might have an immunizing effect; however, the magnitude of the risk has not been determined. The task is difficult because one must consider such variables as ABD compatibility, number of needle insertions, placental location, and the amount of fetal blood transfused into the maternal circulation. Early investigators considered that prophylactic RhIG should not be administered following genetic amniocentesis,9 but almost all now advocate its routine use.10–13 The dose to be administered is controversial. The American College of Obstetricians and Gynecologists recommends that 300 μg of RhIG be administered for an exposure of 30 mL of fetal blood.14 In the United Kingdom, the recommended dose of RhIG is 50 μg before 20 weeks of gestation and 100 μg thereafter.15 We routinely administer 300 μg of RhIG following genetic amniocentesis, regardless of whether the needle may have traversed the placenta.
Following amniocentesis, fetal heart motion should be documented by ultrasonographic visualization. The patient is observed briefly following the procedure and is instructed to report any vaginal fluid loss or bleeding, uterine cramping, or fever. Reasonably normal activities may be resumed following the procedure; however, we recommend that strenuous exercise (e.g., jogging or aerobic exercises) and coitus be avoided for 1 day.
Multiple Gestations
In multiple gestations, amniocentesis can usually be performed on all fetuses, provided amniotic fluid volume is adequate.16 Following aspiration of amniotic fluid from the first sac, 2 to 3 mL of indigo carmine, diluted 1:10 in bacteriostatic water, is injected before the needle is taken out. A second amniocentesis is then performed. The second needle is then inserted into the sac of the second fetus, preferably determined after visualizing the membranes separating the two sacs. Aspiration of clear fluid confirms that the second sac has truly been entered. In experienced hands, amniocentesis is performed successfully in more than 95% of twin pregnancies with ostensibly no increased risks over that of amniocentesis in singleton pregnancies.16,17 Anderson and Goldberg17 observed a postprocedure twin-loss rate of 3.57% up to 28 weeks, a rate interpreted as not increased over the sum of background twin-loss rate plus the loss rate associated with singleton amniocentesis. Triplets and higher-order multiple gestations can be managed similarly by sequentially injecting dye into successive sacs. If the aspirated fluid remains clear, the clinician can be reassured that a new amniotic sac has been entered. However, the overall safety of amniocentesis in triplets and higher-order multiple gestations have not yet been formally determined.
Other techniques for sampling multiple gestations have been reported, including a single puncture technique and an air bubble infusion procedure. Despite advances in ultrasonography, we have concerns that single-puncture techniques could lead to cross-contamination between sacs, resulting in diagnostic inaccuracies. In addition, we believe it unwise to instill any substance into the amniotic cavity unless the instillation is performed in a strict, aseptic fashion and serves to improve safety or accuracy considerably and consistently. More recently, some operators have not used dye instillation to distinguish separate sacs, instead relying on ultrasonographic visualization alone.18–20 In view of the considerable positive experience with dye instillation techniques during the past 20 years with regard to safety and accuracy, we still use the dye instillation procedure.
Safety
Any procedure that involves passing a device into an organ, especially the pregnant uterus, entails risk; amniocentesis is no exception. Indeed, amniocentesis carries potential danger to both mother and fetus. Maternal risks are quite low, with symptomatic amnionitis occurring only rarely. Minor maternal complications such as transient vaginal spotting and minimal amniotic fluid leakage occur in 1% or fewer cases, but these are almost always self-limited. Other very rare complications include intra-abdominal organic injury or hemorrhage.
The safety of traditional amniocentesis has been addressed by several large collaborative studies. The US National Institute of Child Health and Human Development21 conducted the first major prospective study of genetic amniocentesis that comprised 1,040 study subjects and 992 matched controls. Of the 1,040 women undergoing amniocentesis, 950 (91.3%) had the procedure performed for cytogenetic analysis and 90 (8.7%) to evaluate for the possible presence of an inborn error of metabolism. Of all women who underwent amniocentesis, 3.5% experienced fetal loss between the time of the procedure and delivery compared with 3.2% of controls; the slight difference was not statistically significant and disappeared completely when corrected for maternal age. In Canada, a collaborative group conducted a cohort study but did not include a concurrent control group.22,23 Analysis was based on 1,223 amniocenteses performed during 1,020 pregnancies in 900 women. The pregnancy loss rate was 3.2%, a frequency similar to that reported in the US collaborative study.
A later British collaborative study found that the rate of fetal loss following amniocentesis was significantly greater than in controls (2.6% versus 1%).24 In the British study, however, one common indication for amniocentesis was elevated maternal serum AFP (MSAFP) now itself recognized as a factor associated with fetal loss and adverse perinatal outcome. Analysis after excluding subjects undergoing amniocentesis for that indication lowered the loss rates between study subject and control groups to less than 1%, albeit still a significant difference.25
None of the collaborative studies cited above was conducted with high-quality ultrasonography as defined by today's standards, nor was concurrent ultrasonography universally applied. More relevant recent data are from a Danish randomized controlled study of amniocentesis that involved 4,606 women aged between 25 and 34 years who were without known risk factors for fetal genetic abnormalities.26 Women with three or more previous spontaneous abortions, diabetes mellitus, multiple gestation, uterine anomalies, or intrauterine contraceptive devices were excluded. Maternal age, social group, smoking history, number of previous induced and spontaneous abortions, stillbirths, livebirths, and low-birthweight infants were comparable in the study and control groups, as was gestational age at time of entry into the study. Amniocentesis was performed under real-time ultrasound guidance with a 20-gauge needle by experienced operators. Followup evaluation was available for all but 3 women. The spontaneous abortion rate after 16 weeks was 1.7% in amniocentesis patients compared with 0.7% in controls (p < .01), with a 2.6-fold relative risk of spontaneously abortion if the placenta was traversed. Transplacental needle passage is a risk factor that has more recently been shown to not increase the risk for postprocedure loss (see previous discussion). The frequency of postural malformations in the infants in the two groups did not differ. However, respiratory distress syndrome was diagnosed more often (relative risk [RR], 2.1) in the study group, and more infants were treated for pneumonia (RR, 2.5). A more recent assessment of the safety of second-trimester amniocentesis can be found in the CEMAT study that compared conventional second-trimester amniocentesis to early amniocentesis.27 In this multicenter trial performed by experienced operators using concurrent ultrasonography, the total loss rate in the second trimester amniocentesis cohort was 5.9%.
In a study from British Columbia, Baird and colleagues28 considered the question of whether children delivered of women who had midtrimester amniocentesis can be identified by a population-based database of congenital anomalies and disabilities at a different rate from that of matched controls (i.e., children of women who had not undergone amniocentesis). The authors studied 1,296 cases (651 boys and 645 girls) and 3,704 matched controls (1,867 boys and 1,837 girls) among live births (1972 to 1983) from the Health Surveillance Registry with data collected to 1990 to allow followup of 7- to 18-years' duration. Cases were children of mothers who had midtrimester amniocentesis for advanced maternal age (35 years or older) and whose examination results were normal for chromosomal disorders and neural tube defects. When possible, three controls per case were matched for age of mother, gender, date of birth, and state of health from provincial birth records. In all 128 (9.9%) of the cases and 308 (8.3%) of the controls were registered (RR, 1.23); this RR was not significantly different from 1. The likelihood of having disabilities was examined for cases compared with controls, and no difference was found except for an increased ABO isoimmunization associated with amniocentesis. Overall, this study provides reassuring data for patients considering midtrimester amniocentesis with respect to long-term outcome.
In conclusion, we believe it wise to continue to counsel that the risk of pregnancy loss secondary to amniocentesis is 0.5% over baseline, or perhaps slightly less at centers with experienced operators. At our centers, serious maternal complications and fetal injuries are stated to be “remote” risks.
Early Amniocentesis: Gestation of 14 Weeks or Less
With the advent of high-resolution ultrasound equipment, some physicians began offering amniocentesis before 15 weeks of gestation. Some programs not offering chorionic villus sampling (CVS) viewed early amniocentesis as an attractive alternative for those women who desired prenatal diagnosis before the time in pregnancy when traditional amniocentesis is performed (i.e., 15 or more weeks of gestation). In other medical centers, early amniocentesis was explored to lessen the inconvenience of patients' having to be rescheduled if they came in for CVS and were determined to be beyond 12 weeks but under 15 weeks of gestation.
Several programs, including those at our own centers, reported experiences suggesting early amniocentesis was a promising technique. In a series of 936 amniocenteses at 12.8 weeks of gestation or less reported by Hanson and colleagues,29 loss rates were 0.7% (7 of 936) within 2 weeks of amniocentesis, with an additional 2.2% before 28 weeks and an additional 0.5% stillbirths or neonatal deaths. Total losses (32 of 936, or 3.4%) were considered comparable with the 2.1% to 3.2% in ultrasonographically normal pregnancies not undergoing a procedure; however, lack of corrections for maternal age and gestational age render comparisons less than exact. Other series reported include those conducted by Elejalde,30 Penso,31 Stripparo,32 Hackett,33 Assel,34 Djalali,35 Henry,36 Yang,37 Eiben,38 and in all cases, by their respective coworkers, and by Kerber and Held.39 Our group, then at the University of Tennessee, Memphis,40 compared our initial experience with 250 early amniocenteses (14 weeks or less) to that of our first 250 cases of transabdominal CVS (9.5 to 12.9 weeks), finding loss rates for early amniocentesis and transabdominal CVS to be 3.8% and 2.1%, respectively. Our group also reported early amniocentesis in 6 twin gestations (mean 11.9 weeks; range 10.5 to 13.6 weeks), using a similar dye injection technique as described for traditional amniocentesis (see earlier discussion).41 We successfully tapped both amniotic sacs in each of 6 cases (5 requiring two needle insertions, 1 requiring three needle insertions); all cultures yielded normal cytogenetic results, and all six pregnancies resulted in the delivery of health infants.
However, these studies represented observational reports of amniocentesis with most procedures being performed at or after 13 weeks of gestation. More rigorous comparative studies evaluating the safety and efficacy of early amniocentesis have, in general, failed to corroborate the generally favorable outcomes reported in the observational studies. Nicolaides and colleagues42 reported a comparison of amniocentesis and CVS at 10 to 13 weeks of gestation. Early amniocentesis was performed in 731 patients (493 by choice and 238 by randomization) and CVS in 570 (320 by choice and 250 by randomization). Both procedures were performed by transabdominal ultrasound-guided insertion of a 20-gauge needle. The spontaneous loss (intrauterine or neonatal death) was significantly higher after early amniocentesis (total group mean, 5.3%; 95% confidence interval [CI] 3.8 to 7.2; randomized subgroup mean, 5.9%; CI, 3.3 to 9.7) than after CVS (total group mean, 2.3%, CI 1.2 to 3.9; randomized subgroup, mean, 1.2%; CI, 0.3 to 3.5). Subsequently, Nicolaides and colleagues43 reported further findings of this study. Again, postprocedure loss rates were significantly higher in the total early amniocentesis group (4.9%) and the randomized early amniocentesis subgroup (5.8%) than in the total transabdominal CVS group (2.1%) and the randomized transabdominal CVS subgroup (1.8%). The frequency of talipes equinovarus was higher in the early amniocentesis group, but this difference did not attain statistical significance.
Sundberg and colleagues44 performed a similar type of randomized trial comparing early amniocentesis and CVS. In this study, the rate of talipes equinovarus increased significantly in the early amniocentesis group, even though investigators used a filter system to reduce the amount of fluid removed. This finding led the authors to terminate their study for safety concerns prematurely.
The results of the Canadian Early Amniocentesis versus Mid-Trimester Amniocentesis Trial,27,45 a multicenter, randomized trial of early amniocentesis and conventional second-trimester amniocentesis have been most revealing. This multicenter trial randomized 4,374 women into an early amniocentesis cohort (n = 2,183) and a conventional mid-trimester amniocentesis cohort (n = 2,185). In the early amniocentesis cohort, 1,916 women (87.8%) underwent amniocentesis before 13 weeks of gestation.
Loss rates were 7.6% for the early amniocentesis cohort and 5.9% for the midtrimester cohort (p = .012). Talipes equinovarus occurred in 1.3% of infants delivered of women in the early amniocentesis group compared to 0.1% in the midtrimester cohort (p = .0001). In addition, postprocedure amniotic fluid leakage occurred more frequently in the early amniocentesis group (3.5%) than in the midtrimester group (1.7%; p = .0007). Failed procedures, multiple needle insertions, and culture failures also occurred more frequently in the early amniocentesis group.27,45
In view of these recent studies, the ongoing United States multicenter trial evaluating the safety and efficacy of early amniocentesis with the EATA (Early Amniocentesis-Transabdominal CVS) trial ceased offering early amniocentesis to women who had sustained less than 14 weeks of gestation. These more recent prospective studies strongly suggest that second trimester amniocentesis and first-trimester chorionic villus sampling should remain, for the foreseeable future, as the invasive procedures of choice for the detection of fetal cytogenetic and Mendelian abnormalities.