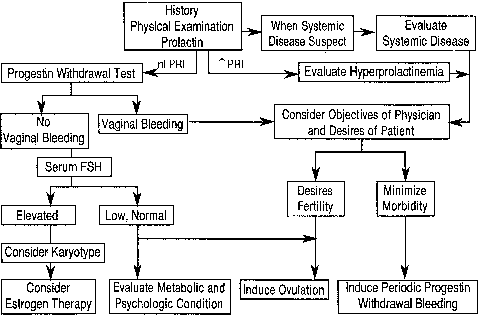
Classification of the many entities that may result in failure of ovulation
can take numerous forms, depending on the perspective of the clinician
or research investigator. Attempts at classification are based either
on a primary entity's effect on the normal physiologic mechanism
of ovulation or on the entity's relationship to a series of
diagnostic tests framed by a specific protocol. On the basis of the physiologic
mechanisms described elsewhere in these volumes, etiologic
factors can be grouped into five major categories: hypothalamic anovulation, pituitary
anovulation, ovarian anovulation, integrative anovulation, and
systemic anovulation. The use of such categories and the placement
of specific disease states within them should not be considered
immutable. As our understanding of the complex interrelationships that
lead to ovulation improves, these categories and their constituents
will change. Hypothalamic Anovulation Active participation of the hypothalamus in the initiation and maintenance
of ovulation has been amply shown through animal studies involving
traumatic ablation of specific nuclei and the histochemical localization
of GnRH-secreting neurons in the diencephalon. The extent to which
other cell types and portions of the hypothalamus interact with GnRH- secreting
cells and these nuclei is only partially understood. Histologic
studies have shown that GnRH-secreting neurons are in close proximity
to axons of a number of synaptic transmitter-type cells. Moreover, there
is pharmacologic evidence that these neurotransmitters are involved
in the control of GnRH release.6 Serotonin, dopamine, and norepinephrine levels in the rat hypothalamus
vary with the estrous cycle, and they also vary in the peripheral circulation
of women during the menstrual cycle.7 These data suggest that catecholamines are involved in the control of
GnRH release and may be the link between higher centers and the hypothalamic
cycling centers to which estrogen feeds back. Disease in these
hypothalamic centers, in higher centers, or along the course of the efferent
neurons from these centers can alter the normal cycling mechanism
and cause anovulation. In addition, the hypothalamus may fail to respond
to changes, in serum steroid concentrations, as a result of intrinsic
or higher center defects. Those etiologic factors that affect the
hypothalamus directly or indirectly through their influence on other
portions of the brain are collectively categorized as the hypothalamic
causes of anovulation. PSYCHOGENIC TRAUMA. It has long been recognized that subtle environmental influences may alter
the menstrual cycle (e.g., the tendency toward synchronization of
cycles among women living in close quarters).8 It is not surprising, then, that minor alterations in place or activity
may lead to anovulation, as in the syndrome of schoolgirl or summer
camp amenorrhea. Most likely, these conditions are caused by the influence
of higher centers on the hypothalamus. More severe forms of psychic
trauma are also apt to result in anovulation, with a frequency approaching 54%, as
in the concentration camps of World War II9 ;little documentation of the hormonal status in such cases is available. In
women with outright emotional disturbances that temporarily relate
to their amenorrhea, normal concentrations of pituitary gonadotropins
and normal prolactin levels have been found, serum estrogen levels
have been in the low-to-normal range, and both cortisol and growth hormone
levels have been elevated.10 The anterior pituitary responds in a generally normal fashion to releasing
factors, and the ovary is capable of responding to pituitary gonadotropins. Pituitary
pulsatile secretion of LH is, however, diminished, reflecting
a decrease in GnRH neuronal activity. Mounting evidence suggests
that elevated corticotropin-releasing factor (CRF) output is the
suppressor of GnRH pacemaker activity, which, in turn, prevents pituitary
stimulation of folliculogenesis.11,12 Exceptions to the general rule of hypogonadotropism in psychogenic amenorrhea
have been reported. Patients with a history of temporally related
hypergonadotropic anovulation, vasomotor symptoms, and acute stress
have subsequently returned to cyclic menstruation and even pregnancy.13 ANOREXIA NERVOSA. Anorexia nervosa, a psychiatric-endocrine disease, presents as extreme
weight loss, amenorrhea, and abnormal ideation concerning body image
and food intake. Women with this condition consider themselves to be overweight
and instigate drastic efforts at weight reduction.14 Amenorrhea often begins at the same time that weight reduction starts
and occasionally precedes attempts at dieting. The entity may affect as
many as 5% of adolescent women.15 When severe, the disease has a significant mortality rate. It is separated
categorically from other traumatic forms of psychogenic anovulation
because it is not ordinarily initiated by a specific temporal event
and because its characteristic picture can be directly related to the
metabolic alterations accompanying severe weight loss rather than to
initiation of the abnormal behavior patterns. More than one third of the
women experiencing anorexia manifest signs of an affective disorder
later in their adult lives.16 Patients with anorexia nervosa have low serum gonadotropin levels, with
an increase in the FSH/LH ratio. Serum estrogen levels are low, and prolactin
levels are low to normal. The decreased estrogens prevent withdrawal
bleeding after a progestin challenge and contribute to the development
of osteoporosis. Thyroxine levels are normal, but diminished
conversion of this hormone to triiodothyronine can result in the development
of hypothyroid signs (e.g., bradychardia, dry skin, hypercarotenemia, slow
relaxation reflexes). Growth hormone levels are frequently
elevated during periods of inanition. Pituitary gonadotropin release
patterns regress from the characteristic adult pulsations through the
pubertal pattern and become identical to that seen in childhood.17 The pituitary response after a bolus of GnRH is variable, depending on
the seriousness of the disease.18 Pulsatile administration of GnRH stimulates pituitary gonadotropin secretion
and ovulation, suggesting that the major hormonal defect in anorexia, as
in other psychological stress-induced states, lies above the
pituitary gland. Pathologic hypothalamic function is also seen by loss
of the normal paradoxic response to heat and cold and by the frequent
development of diabetes insipidus.16 Coincidentally, CRF levels are elevated in this state.12 Thus, the degree to which anovulation is caused by CRF suppression of
GnRH pulsatility or mechanisms related to body fat content may vary.19 Bulimic women with weight loss may present a pathophysiologic picture
similar to that of anorexia nervosa. However, many maintain a normal weight
while experiencing anovulation and amenorrhea. Provocative testing
suggests that their cyclic dysfunction is at the level of the hypothalamus
or pituitary.20 PSEUDOCYESIS. Amenorrhea, galactorrhea, and abdominal distention mimicking pregnancy
can be induced by nonfactitious, psychogenic means. These simulated pregnancies
are sometimes accompanied by a persistent corpus luteum. Contradictory
hormonal pictures have been described in these patients, including
both elevated and depressed serum LH concentrations.21 An exaggerated LH response to GnRH and an abnormal dexamethasone suppression
test have also been found.22 Prolactin levels are usually elevated, and FSH levels are within the normal
range.23 Estrogen and progesterone levels resemble those found during the early
luteal phase or in Halban's syndrome (persistent corpus luteum). The
endometrium may have a secretory histologic appearance. Psychogenic stress can be manifest through several seemingly different
pathways, and the resultant anovulatory state may be associated with either
active or quiescent ovaries and a spectrum of gonadotropin levels.13 Most likely, the underlying neuropharmacology is similar in each of the
states described here.21,24 The derangement in hypothalamic-pituitary function manifest in pseudocyesis
may be the result of an impairment in dopaminergic activity with
malfunction at a hypothalamic or higher level. Resolution of the underlying
psychological conflict is usually necessary for the resumption
of ovulation. When resolution occurs, hypothalamic-pituitary stimulation
test responses rapidly return to normal. PHARMACOLOGIC AGENTS. Because the dynamic relation between various diencephalic centers and
between the hypothalamus and the pituitary is partially governed by the
biogenic amines, it is reasonable to expect that drugs affecting their
metabolism might alter the ovulatory process.25 Agents such as phenothiazines (e.g., chlorpromazine, perphenazine, thioridazine), tricyclic
antidepressants (e.g., imipramine, amitriptyline), reserpine, morphine, cimetidine, metoclopramide, dextroamphetamine, α-methyldopa, and
verapamil can cause anovulation. Serum LH and
prolactin levels are usually elevated, and FSH levels are normal in patients
receiving long-term drug therapy. Discontinuation of an offending
agent results in a rapid return of prolactin to normal levels and
resumption of ovulatory cycles.26 Inhibitors of prostaglandin synthesis, such as indomethacin, may also
affect ovulation. These inhibitors have a direct effect on the central
nervous system as well as on the ovary. ANATOMIC DEFECTS. Tumors and inflammatory or degenerative lesions in or adjacent to the hypothalamus
can alter its functional capacity. These defects tend to affect
gonadotropin secretion more frequently and at an earlier time than
they do the other pituitary hormones. Both hypogonadotropic and normogonadotropic
states can result. Craniopharyngiomas are the most common tumor at this site, but gliomas, dermoid
cysts, meningiomas, and germinomas have been found. Inflammatory
lesions, including the reticuloendothelioses and tuberculosis, have
also been found in the hypothalamus. In children, such lesions have
been associated with precocious puberty; in the adult female, they are
more often associated with hypogonadotropic anovulation.27 As in women with psychogenic anovulation, women with such lesions may
also have deficits in pituitary function, which can be defined by their
response to GnRH stimulation.28 These defects, however, have been found in patients who have already undergone
conservative surgery and may be the result of the surgery and
not of the primary lesion. CONGENITAL DEFECTS. Familial hypogonadism that results from a hypothalamic defect has traditionally
been linked with two syndromes: Kallmann's and Laurence-Moon-Biedl. In
the former, a heterogeneous group of inheritance patterns
have been implicated in a complex involving hypogonadotropic hypogonadism
and anosmia.29 In addition to low circulating levels of LH and FSH, these patients have
low levels of human pituitary prolactin (PRL) that fail to rise significantly
after thyroid-releasing factor injection. An anatomic defect
of the olfactory lobes in these patients is associated with migratory
failure to the GnRH-secreting cells, with a subsequent lack of stimulation
to the gonadotropin-producing cells within the pituitary gland. In
males, the deletion of a gene (KAL) on the X chromosome that encodes
for a neuronal migratory protein (anosmin) has been implicated in this
defect.30 Although the syndrome has been described in and ascribed primarily to
males, anosmia with hypogonadotropic hypogonadism also exists in females.31 Both the histology of the ovaries (follicles are all at the primary stage
of development) and their response to exogenous gonadotropins indicate
that the primary defect is above the ovarian level. The response
to GnRH in women with Kallmann's syndrome has been variable, with
successful ovulation induction occurring most often when menotropin therapy
has been used.32 Laurence-Moon syndrome (polydactyly, obesity, mental retardation, retinitis
pigmentosa, and hypogonadism) has been described most frequently
in males and has an autosomal-recessive inheritance pattern. Patients
have been described as having either hypogonadotropic hypogonadism, presumably
because of hypothalamic malfunction, or primary hypogonadism.33 In women with the very similar Bardet-Biedl syndrome, reproductive dysfunction
is common, although hypogonadism is infrequent.34 More recently, the application of molecular biologic techniques has identified
a cluster of genetic defects among women who experience hypogonadotropic
hypogonadism. This group exhibits delayed pubertal development, infertility, and
low or absent serum levels of pituitary gonadotropins. Mutations
in the FSH-β subunit, PROP-1, GnRH receptor, congenital adrenal hypoplasia, leptin, and
leptin receptor genes, in addition to that of KAL, have been implicated.35 In each case, the defect is manifest by a failure to instigate sufficient
gonadal activity to produce pubertal development and subsequent reproductive
competence. FUNCTIONAL. Anovulatory women who fail to shed endometrium after progestin stimulation
and are without a recognizable cause of their condition are categorized
as having functional hypothalamic amenorrhea. Although this is one
of the most common forms of anovulation, its diagnosis is made by exclusion. When
optimally evaluated, a significant proportion of such individuals
show a subclinical eating disorder characterized by low fat
and eucaloric intake.36 As a group, they are hypoestrogenic and mildly hypercortisolemic, with
low or normal circulating levels of pituitary gonadotropins. When given
GnRH, they usually respond normally. However, their LH secretory pulse
frequency is prolonged, suggesting an abnormality in hypothalamic
GnRH output.37 This presentation is essentially identical to that seen in women with
non-anorexic weight reduction. Minor abnormalities in the control and
secretion of other pituitary hormones(prolactin, growth hormone, thyroid
hormone) have also been documented, leading to the suggestion that
this clinical presentation is an adaptive contraceptive mechanism in response
to an unfavorable psychic or physical environment.38 A high percentage of these women eventually undergo spontaneous return
of ovulatory function. Pituitary Anovulation The anterior hypophysis, once considered the “master gland,” now
appears to be an intermediary between the brain and peripheral endocrine
organs. It secretes a number of proteins, including FSH and LH, the
primary hormonal stimuli to follicular maturation. Control in the
output of these hormones appears to reside in the hypothalamus and
ovary. Steroid feedback to the anterior pituitary acts as a modifier for
the primary effects of GnRH. The ability of the anterior hypophysis
to respond to GnRH may be altered or prevented by various diseases that
affect the gland directly. Steroid hormones may alter the biologic
activity of LH secreted by the gland. In addition, the gland may be altered
by inherent defects that impair its capacity to secrete biologically
active gonadotropins. PITUITARY TUMORS. The frequent association of anterior pituitary tumors with amenorrhea has
been recognized for more than 50 years. In the past, large tumors (more
than 10 mm in diameter) usually came to attention because of debilitating
symptoms such as a visual field loss or severe headaches. Amenorrhea, which
frequently preceded these symptoms by 2 or more years, was
often ignored. Today, with women seeking assistance for increasingly
subtle symptoms and with the availability of sophisticated diagnostic
aids, the diagnosis of pituitary tumor-induced anovulation is being
made more frequently. Large tumors of the anterior pituitary were originally thought to invoke
amenorrhea through changes brought about during their growth. The limited
space available for expansion within the sella turcica is presumed
to cause pressure atrophy of the nontumorous, normal gland, with loss
of trophic hormone secretion. Involution of the ovaries without simultaneous
thyroid or adrenal atrophy was explained by the existence of
a pattern of hierarchical functional loss within the gland. Evidence
to support such a concept came from experimental pituitary ablation studies
in dogs. These showed that when fractions of the gland were removed
serially, the first secretory product to be lost was growth hormone. Subsequently, with
excision of large fractions, the gonadotropins were
lost. The last secretory products to be found after removal of major
gland segments were thyrotropin and corticotropin. The role played
by small tumors (less than 10 mm in diameter) in the development of anovulatory
states was not resolved through these studies because it was
difficult to conceive of their inducing pressure atrophy or a portal
circulatory disturbance. The existence of small, nonprolactin-secreting
tumors in patients with normal ovulatory function suggests that microadenomas
associated with anovulation act by means other than either pressure
atrophy of the gland or interruption of portal communication with
the hypothalamus.39 When PRL was identified and methods of assay were developed, a new appreciation
evolved for the role played by small tumors in the induction
of anovulation. High circulating levels of PRL were frequently shown to
be associated with anovulation or amenorrhea, and almost all of the
small adenomas found in anovulatory women produced the hormone. The exact mechanism that causes PRL-producing microadenomas to form is
unknown.40 Both an anomalous blood supply and the presence of specific oncogenes
have been suggested as inciting factors in prolactinoma development. Generally, however, it
is thought that high levels of PRL feed back on
the hypothalamus to invoke an increase in dopamine production. High levels
of hypothalamic dopamine then inhibit GnRH production, and anovulation
results. A direct effect of hyperprolactinemia on folliculogenesis
has also been postulated but is less well substantiated by experimental
data. Small adenomas rarely grow into macroadenomas; they seldom
cause debilitation beyond menstrual dysfunction or galactorrhea. Approximately 80% of
large anterior pituitary tumors associated with anovulation
secrete excess amounts of prolactin.41 It is probable that some large tumors actively inhibit pituitary function
by a pressure effect, because a significant minority (20%) of these
lesions do not secrete prolactin. However, many so-called functionless
tumors have been shown to secrete gonadotropins in a nonphysiologic
manner, thereby instigating aberrant folliculogenesis.42 In both forms of pituitary tumor (microadenomas and macroadenomas), the
patient's hypogonadotropic status is what ultimately leads to the
acyclic state. The mass effect that is produced by macroadenomas of
the anterior hypophysis may also result from expansion of sarcoid, tuberculous, cystic, aneurysmal, or other space-occupying lesions. ISCHEMIA. Destruction of the secretory cells within the pituitary gland may also
result from ischemia. Necrosis of this sort, as seen in Sheehan's
syndrome and Simmond's disease, is usually global. Whereas an enlarging
tumor may sequentially inhibit the secretion of growth hormone, gonadotropin, thyrotropin, and adrenocorticotropin by the gland, ischemic
necrosis most often results in near-total loss of secretory capacity. The
same may be said of other forms of pituitary destruction, such
as infection. In the empty-sella syndrome, conversely, dysfunction
is usually partial and anovulation infrequent.43 PITUITARY DEFECTS. The stimulation of primary follicles in preparation for ovulation depends
on adequate amounts of biologically active gonadotropin secretion. Defects
in the pituitary secretory cells that result in gonadotropin
deficiency have been shown to account for anovulation in at least a few
patients. These defects are in one of the subunits of the hormones, usually
the β-subunit. A two-base pair deletion in the FSH-β gene has been found in at least two of these women.44 Thus, in the patient with an FSH-β subunit deficiency, both biologically active LH and FSH-α subunit
may be found in the circulation.45 The capacity of pituitary cells to vary the biologic activity of their
secretory products is potentially more important to ovulation than isolated
defects in gonadotropin synthesis. Evidence is accumulating to suggest
that the serum LH level measured by immunologic methods does not
vary directly with the serum LH level measured by bioassay. The implications
of these findings could be great, both for the role of LH in
normal ovarian stimulation and for its role in abnormal states such as
polycystic ovarian disease.46 A similar discontinuity has not been observed for FSH.47 Ovarian Anovulation The normal ovary is a relatively inactive structure until stimulated. Advanced
follicular maturation, ovulation, and steroidogenesis do not proceed
in the absence of pituitary gonadotropins. In patients who have
never been exposed to endogenous gonadotropins, follicles rarely develop
beyond the primary stage. Rising titers of FSH and LH stimulate specific
sequential events in the course of follicular maturation. The rapidly
increasing serum estrogen concentrations that result are the signal
responsible for hypothalamic/pituitary induction of the midcycle
LH surge. Hypothetically, then, the ovarian factors responsible for anovulation
might include absence of primordial follicles, resistance to
gonadotropin stimulation, and failure of steroidogenesis, resulting in
inadequate feedback to the pituitary and hypothalamus. In fact, examples
of each of these ovarian causes for anovulation have been documented. Intrinsic
defects compromising ovarian hormone production cause an
increase in serum gonadotropin levels. This is primarily because low
levels of circulating estrogens fail to suppress pituitary FSH and LH
production. However, ovarian inhibin is also involved in the natural
modulation of FSH secretion. Thus, estrogen therapy does not completely
suppress serum gonadotropin levels in women with ovarian failure. OVARIAN DYSGENESIS. Failure to develop or maintain normal numbers of oocytes in a state of
developmental arrest until puberty usually results from a genetic defect. The
major gene loci involved in normal ovarian development are located
on the arms of the X chromosome.48 In addition, case reports provide evidence for the existence of autosomal
loci that contribute to normal ovarian development. The most common karyotypic defect associated with abnormal ovarian development
is the 45,X pattern of Turner's syndrome. Variants, including
mosaics, make up 20% of the syndromic population. In addition, there
are a number of 46,XX females with streak ovaries who do not exhibit
Turner's stigmata. Two thirds of these women have a genetic (autosomal-recessive)basis
for their streak ovaries, whereas the remainder
are thought to result from infarction, infection, or other as-yet undetermined
events.49 Although women in this latter group may not be recognized in childhood, lack
of pubertal development eventually brings them to the attention
of a physician. Patients with ovarian dysgenesis have the capacity for cyclic hypothalamic
and pituitary function. Their menopausal levels of pituitary gonadotropins
in adulthood are presumably the result of a hypothalamic response
to very low levels of serum estrogen and a lack of ovarian inhibin
production. Even in the prepubertal state, however, these women have FSH levels that are elevated for their
chronologic age. PREMATURE OVARIAN FAILURE. Menopause is a natural event having a mean onset at approximately 50 years
of age. It occurs when the ovaries have become depleted of all functionally
competent follicles and is accompanied by high serum levels
of pituitary gonadotropins and low levels of estrogen. In contrast to
menarche, which has begun, over the decades at progressively earlier
ages, its temporal appearance has not changed during the past 200 years. When
menopause occurs before age 40, it is referred to as premature. So
few women (1%) have amenorrhea with hypergonadotropic hypoestrogenism
develop at this relatively young age that the presence of a pathologic
mechanism is suspected.50 The syndrome presents with either of two histologic findings in the ovaries. Most
frequently, follicles are absent. Less often (less than 1%), there
are abundant primordial follicles that show no evidence of maturation
beyond that of primary follicles. Despite the presence of follicles
in only one subset, this clinical presentation is generally referred
to as premature ovarian failure. The history of cyclic menstruation
serves to distinguish this entity from primary ovarian failure, a
clinical presentation that may involve some overlapping etiologies. Although
permanent in most cases, on rare occasions, menopause can reverse
spontaneously, with return of ovulation and even pregnancy. Most women who present with premature ovarian failure have either lost
their complement of follicles through an active process or failed to produce
sufficient numbers during embryogenesis. The relative likelihood
of each of these alternative possibilities is unknown. With the exception
of a very few Turner's variant women who have had cyclic menstruation, patients
experiencing premature ovarian failure have a normal 46,XX
karyotype.51 There are only a few documented pedigrees in which multiple members experience
premature ovarian failure and have a normal karyotype. Several
genes residing on the X chromosome have been proposed as causative agents
in such cases but, as yet, none have been compellingly shown to be
a culprit.52 Perhaps the most likely suspect for such a role is the fragile X syndrome
gene: FMR-1. This is because carriers of the fragile X mutation frequently (13% to 25%) experience premature ovarian failure. However, the
mechanism by which ovarian failure is induced remains obscure since
expression of the FMR-1 protein appears to be the same as in unaffected
women with the normal number of X chromosome trinucleotide repeats. An
abnormality of at least one autosomal gene (FOXL2 on chromosome 3) has
also been implicated as a possible inducer of premature ovarian failure.53 The relative infrequency of familial premature ovarian failure suggests
that the syndrome seldom has a primary genetic basis.54 A more solidly founded explanation for the early exhaustion of follicular
activity is an autoimmune reaction. Both systemic autoimmune diseases (e.g., juvenile
rheumatoid arthritis) and those involving specific
organs (e.g., thyroid [Hashimoto's, Graves], adrenal [Addison's], hypoparathyroidism, juvenile-onset diabetes
mellitus, pernicious anemia, idiopathic thrombocytopenic purpura, myasthenia
gravis) have been linked with premature ovarian failure. This
type of association has been noted in 18% of the women experiencing premature
ovarian failure.55 Circulating antibodies to ovarian proteins are sometimes found in patients
with premature ovarian failure.56 More often (up to 92%), a less-specific autoimmune response can be shown
in these women.57 Failure of other endocrine tissues in women with premature menopause is
seen with sufficient frequency to justify a general survey of endocrine
tissue function in each newly diagnosed patient. Adrenal insufficiency
is the most commonly found associated disorder. Attempts to reverse
ovarian dysfunction with glucocorticoids have produced resumption of
menses in a few women, but pregnancy has not been reported after this
form of therapy. Other known causes of afollicular hypergonadotropic hypogonadism include
mumps oophoritis, and β-galactosemia.58 Hypergonadotropic hypogonadism in the presence of unstimulated follicles(Savage
or Gonadotropin-Resistant Ovary Syndrome)has been shown to be
caused by at least two different pathophysiologic conditions: a mutation
in the β-subunit of FSH59 and a mutation in the FSH receptor gene.60 The former defect has been identified in only two homozygous women, so
its incidence remains unknown. In one of these women, conception was
achieved through the administration of FSH. In the latter anomaly, also
autosomal recessive, an incidence of one in 8399 females was found among
a Finnish population. Because the follicles that are present in this
condition fail to respond to the high levels of endogenous FSH and
LH by undergoing maturation, it has been called the resistant ovary syndrome. Both
primary resistance and acquired resistance have been reported.61 The differential diagnosis between this state and that of follicular exhaustion
is an important one when pregnancy is desired, because some
women who have follicles ovulate in response to estrogen or menotropin
administration.62 PSEUDO-OVULATION. Anomalous follicular luteinization may result from a failure of ovulation
followed by luteinization of the unruptured follicle or from ovulation
with inadequate progesterone production. In the luteinized unruptured
follicle (LUF) syndrome, basal body temperatures show an elevation
consistent with ovulation, serum progesterone levels are elevated over
those of the follicular phase, and the endometrium takes on a secretory
histologic appearance. Serial ultrasound examinations show the dominant
follicle to be intact during the early luteal phase, and laparoscopy
fails to show an ovulatory stigma. LUF is thought to occur in 10% of
cycles. In some women, it can be repetitive, causing infertility.63 The underlying cause of this defect is unknown. However, because follicular
rupture requires the activation of collagenase, a prostaglandin-dependent
event, anything that perturbs the cyclo-oxygenase system could
be at fault. It is, therefore, not surprising that intake of nonsteroidal
anti-inflammatory drugs has been associated with LUF.64 Cessation of these agents has resulted in a return to normal ultrasound-appearing
ovulation. In spontaneous LUF, administration of clomiphene
citrate has produced ovulation. The degree to which this syndrome produces
a low serum progesterone level that is not sufficient to develop
a normal secretory endometrium is unknown, and the extent to which the
condition overlaps with the inadequate luteal phase syndrome has not
been determined.65 OVARIAN TUMORS. Tumors of the ovary may disrupt the ovulatory cycle by destruction of
the ovarian parenchyma, stimulation of adjacent ovarian stroma to hormone
production, or direct production of steroid hormones. The stimulation
of stroma by either a primary or a metastatic tumor is the least well
understood of these three mechanisms. A postulate is that the tumor
secretes an inducer substance that, in turn, stimulates the ovarian
stroma to produce androgens. The androgens may then be converted to estrogens
at peripheral tissue sites.66 In at least one case, the tumor secretagogue was shown to be a chorionic-like
gonadotropin.67 The androgens and estrogens that result from ovarian tumor growth disrupt
hypothalamic cycling activity and cause the patient to become anovulatory. Integrative Anovulation Ovulation is the end product of a highly integrated set of events involving
the hypothalamus, pituitary, and ovary. Perturbations of this axis
have not been fully delineated. Events that seem on the surface to be
remote from those of ovulation can have a strong influence on the cyclic
function of the axis. In some of the entities cited below, functional
hypothalamic defects can be shown, but in none of these has a primary
mechanistic defect been identified. They have in common a general
malfunction of the integrative functions between the involved organs. Although
these entities have traditionally been categorized as having
hypothalamic etiology, they are placed in a separate section here to
emphasize the importance of integrative functions in their induction of
anovulation. POLYCYSTIC OVARIAN SYNDROME. An illdefined but seemingly ubiquitous condition, polycystic ovarian syndrome
includes several metabolic defects, hirsutism, and occasionally
obesity in association with anovulation.68 It is sometimes referred to as a disease, but because a means of specific
definition is lacking, the presentation is more often called a syndrome. An
elevation in circulating androgens, an inversion in the ratio
of estrone to estradiol, insulin resistance, a normal-to-elevated serum
LH level, and a normal serum FSH level are the common biochemical
findings of the disorder.69 Obese women with the syndrome frequently have acanthosis nigricans develop
that is concomitant to their insulin resistance. A hallmark of the
syndrome is the presence of polycystic ovaries, which may be identified
clinically by palpation or by ultrasound.70 However, because there are several well-established conditions (e.g., Cushing's
disease, congenital adrenal hyperplasia, and hyperprolactinemic
amenorrhea) that can also produce a polycystic ovarian morphology, a
determination of polycystic ovarian syndrome must be made by exclusion. Polycystic
ovaries are sometimes (7%) found in otherwise healthy
women. More often, this ovarian morphology is seen with anovulation (87%), hirsutism (54%), an abnormal LH/FSH ratio, and an elevated serum
testosterone level (85%).70 Specific criteria for making a diagnosis of polycystic ovarian syndrome
may vary but usually include clinical, ultrasonographic, and biochemical
parameters. The cause or causes of polycystic ovarian syndrome are not positively known.71 In some instances, there is a clear indication that inheritable factors
are involved.72 Kindred studies are consistent with an autosomal-dominant form of inheritance. A
high incidence of associated insulin resistance (50%) suggests
that elevated levels of circulating insulin may stimulate insulin-like
growth factor receptors within the ovary, raising steroidogenic enzyme
activity and thereby effecting an increase in androgen production.73,74 This thesis, together with the determination that both positive and negative
feedback mechanisms are intact, suggests that the syndrome may
have its origins directly within the ovary. Whatever its origin or origins, a relatively effective means of treating
its anovulatory component exists with the use of clomiphene citrate
and insulin sensitizing agents.75 Less satisfactory, and therefore more controversial, are the means for
treating the hirsutism and endometrial hyperplasia that often present
in this syndrome. NONPSYCHOGENIC WEIGHT DISTURBANCES. Weight loss to below the 10th percentile for body height is usually accompanied
by anovulation and amenorrhea. Although the primary defect is
unknown, most of the metabolic and physiologic disturbances found in
such patients resemble those of anorexia nervosa.16 The major differences seem to be in the degree of hypothalamic dysfunction
and the absence of severe psychiatric debilitation. These women usually
have low-to-normal levels of circulating gonadotropins and low
levels of serum estrogens. Pituitary responsiveness to GnRH is normal, but
gonadotropin pulse frequency is depressed, causing some investigators
to categorize this entity as a form of functional hypothalamic amenorrhea.38 A gain in weight to above the 10th percentile usually results in return
of ovulatory function. Decreased total body fat with a concomitant decrease
in aromatization of adrenal androgens has been suggested as the
functional defect in this syndrome. An analogous condition is frequently found in competitive athletes and
other women who undertake intense physical training. Ballet dancers, rowers, and
runners who cover more than 35 miles per week often experience
the luteal phase defect or anovulation.76 They have low gonadotropin and estrogen levels and high serum endorphins, and
they show an abnormal adrenocorticotrophic hormone-cortisol response
to CRF.77 Despite high caloric intake, their fractional body fat content is low
and they experience relative hypoglycemia/hypoinsulinemia associated with
glucoregulatory adaptations including hypercortisolemia.37 These alterations may be the underlying reason for their long-observed
hypothalamic- pituitary malfunction.78 When hypoestrogenism is prolonged, osteoporosis becomes a problem. Cessation
of intense physical activity usually results in fairly prompt resumption
of menstruation.79 However, because amenorrhea occurs more frequently in those athletes who
experienced menstrual dysfunction before beginning training, cessation
of intense exercise does not guarantee initiation of regular ovulation. In a converse situation, morbid obesity, anovulation has been related to
high circulating levels of androgens. These women have normal serum
estradiol concentrations. Serum FSH levels are usually depressed and LH
levels are slightly elevated.80 Dietary weight loss has been followed by resumption of cyclic menses. Systemic Anovulation ACUTE AND CHRONIC DISEASE. Acute, critical illness can induce temporary hypogonadotropic hypogonadism. Severe, chronic
debilitating disease of almost any type, such as
renal failure, lymphomas, untreated tuberculosis, and cystic fibrosis, can
also result in anovulation.81 Adrenal and thyroid disease, although usually not so debilitating, frequently
present as anovulation or amenorrhea. In Cushing's syndrome
of primary adrenal origin, the etiology of the anovulation is unknown. In
those patients with bilateral hyperplasia, a primary abnormality
of pituitary or hypothalamic function can usually be shown to accompany
the failure to cycle. Normal serum estrogen and gonadotropin levels
are present in these women. Adrenal failure can also be accompanied
by anovulation. In untreated cases, this is usually of the hypogonadotropic
type that accompanies debilitation, but a number of cases with an
autoimmune etiology are known. These have been accompanied by high levels
of circulating gonadotropins. Congenital adrenal hyperplasia patients with a 21- or 11-hydroxylase deficiency
are frequently anovulatory during adulthood. In part, this is
due to less-than-optimal glucocorticoid therapy. The longer these patients
remain untreated, the more difficult it becomes to induce ovulation. In
the rare instance when congenital adrenal hyperplasia results
from a deficiency of 17-hydroxylase, hypoestrogenism and anovulation will
continue despite optimal gluco- and mineralocorticoid replacement
therapy.82 Ovulation and pregnancy are, nevertheless, possible using GnRH agonists
and menotropins plus estrogen therapy to overcome the physiologic abnormalities
caused by the block in follicular estrogen production.83 Hyperthyroidism is usually accompanied by an elevated serum estrogen concentration, which
is due to altered steroid metabolism and clearance. With
higher levels of estrogen, there is a failure of the hypothalamic
feedback mechanism similar to that seen in polycystic ovarian syndrome, with
normal FSH and elevated LH levels. Because hepatic disease can
impair the metabolism of estrogens and obesity can enhance conversion
of androgens to estrogens, both conditions can induce a similar picture. Hypothyroidism
may be accompanied by elevated serum estrogens and
a feedback problem. Anovulation may also occur as a result of the hyperprolactinemia
that often accompanies primary hypothyroidism and is a
consequence of an increased output of thyroid-releasing factor. POSTPILL ANOVULATION. Anovulation is the rule for women taking combination oral contraceptive
pills. For most users, there is only a slight delay in the return of
ovulation after cessation of therapy and a minimal time lapse between
the initial attempt to conceive and pregnancy. However, 0.2% to 3.4% of
women discontinuing contraceptive pills fail to ovulate. Although this
rate is approximately the same as the rate of secondary amenorrhea
among nonpill users,84 there is a persistent suspicion that oral contraceptives leave a residual
of anovulation. A retrospective study suggests that postpill anovulation
may occur in an epidemiologically different group than does spontaneous
anovulation.85 The demonstration that oral contraceptives are or are not an etiologic
factor in anovulation would not diminish the need for thorough evaluation
of all postpill patients who fail to menstruate, because a number
of these women are found to have mild abnormalities of their hypothalamic
feedback mechanisms86 and others may have a concomitant disease such as a pituitary tumor.87 |