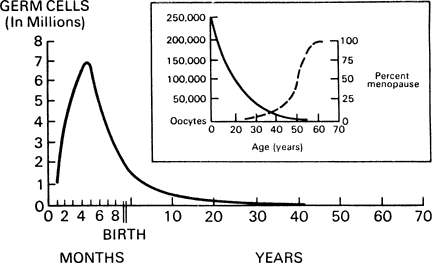
It is well-known that radiation can have a profound effect on both normal
and tumor cells. However, effects do not depend solely on the physical
characteristics of radiation, but also on various environmental conditions. Type and quantity of radiation are obviously significant. For example, the
distribution of x-rays will be relatively uniform in exposed embryos, whereas
radioactive isotopes will not necessarily be uniformly distributed.2 Compared with an acute dose administered at the period of maximum sensitivity, fractionation
of the dose reduces its effect.2,3,4 Similarly, lowering the dose rate increases the number of surviving oocytes, at least in the female mouse, suggesting
that there may be repair processes in oocytes.2,5 Among important environmental and host factors are ambient temperature
and oxygen levels, the lowering of which mitigates radiation effects.6 Concurrent drug or hormone regimen, genetic predisposition, age, reproductive
history, pathologic condition, germ cell stage, and species2,3,7 also influence the effects of radiation on individuals, even when type, dose, and
delivery rate are fixed. For example, primordial oocytes in
juvenile mice are exquisitely radiosensitive in contrast to oocytes
of macaques and human females.8 One explanation for the difference in species sensitivity is difference
in chromosome organization within oocytes; dense chromosomes are more
resistant to radiation than is diffuse chromatin.9 Another hypothesis is that it is the plasma membrane rather than the deoxyribonucleic
acid (DNA) that is the target of ionization, at least
in mouse oocytes.8 Presumably, the human oocyte membrane is less sensitive. Because so many variables exist, generalizations are hazardous. Nonetheless, the
effects of high-dose and low-dose ionizing radiation, radionuclides, and
nonionizing radiation are discussed and conclusions attempted. High-Dose External Ionizing Radiation High doses to the ovaries of external ionizing radiation cause permanent
amenorrhea. Indeed, x-rays were used for this purpose 50 years ago. In 1939, Jacox10 reported that 500 rads to the ovaries was sufficient to cause permanent
castration in most patients, although an occasional patient required
significantly more. Peck and colleagues11 later clarified one of the reasons for this variation: observing that
older patients were more sensitive than younger ones. Nearly 90% of patients
older than 40 years of age required only 375 to 499 radiographs
to ensure permanent castration, whereas younger patients usually required 625 to 749 radiographs. Although large doses are sufficient to cause permanent loss of ovarian
function, there appears to be a threshold below which fertility is not
significantly affected. Blot and Sawada12 studied 2345 Japanese women in Hiroshima and Nagasaki 18 years after the
atomic bomb explosions. They observed no significant difference in
fertility among groups exposed to no radiation, 0 to 9 rads, 10 to 99 rads, and 100 rads
or more. Seigel's findings were similar.13 Tabuchi14 also studied women exposed to the atomic bombs and claimed an increase in fertility in young women for 1 year after exposure, with no evidence
of subsequent decreased fertility. No change in the age at menarche
among exposed girls and no change in the age at menopause in exposed women
were noted. Exposure doses and number of women studied were not stated
in the latter study nor, apparently, were other variables controlled. Exposure to high levels of external ionising radiation currently is essentially
limited to women undergoing treatment for malignant diseases (e.g., Hodgkin's
disease). Before the development of oophoropexy, women
treated with pelvic irradiation for Hodgkin's disease (approximately 4000 rads) invariably had ovarian failure develop. To prevent
castration, Ray and coworkers15 devised the technique of oophoropexy. At staging laparotomy, both ovaries
and their attached vascular pedicles are moved to the middle of the
true pelvis and sutured to either the anterior or the posterior surface
of the uterus; metallic clips mark ovarian placement. A lead shield
is placed over the central portion of the true pelvis before irradiation. Ray's
group treated 22 patients (13 to 23 years of age) with
oophoropexy and pelvic irradiation (mean follow-up interval, 10 months).15 In 13 (59%) of the 22, normal ovarian function was maintained, although
in four of these 13, menses temporarily ceased. The remaining nine patients (41%) manifested
permanent amenorrhea. The investigators were
unable to relate differential maintenance of ovarian function to patient's
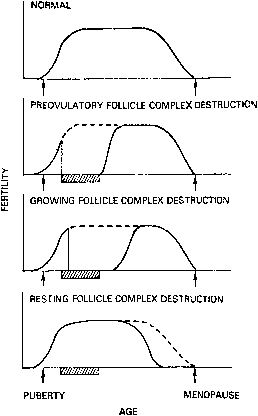
age, ovarian dose, dose/fraction, or total treatment time. Radiation-induced amenorrhea will sometimes be followed by spontaneous
resumption of menses. This may be because of the destruction of preovulatory
follicle complexes but not of resting follicle complexes. The resting
follicles would, subsequently, still be available for recruitment
to the growing and preovulatory follicle populations. Of four patients
receiving 150 rads to the ovaries following oophoropexy, Thomas and
colleagues found three initially showed menstrual disturbances that
later spontaneously resolved.16,17 Of 12 patients who received 500 to 3500 rads to the ovaries, all initially
became amenorrheic. However, three of the 12 (exposure, 600 to 700 rads; ages 24, 25, 32) resumed menses after 6 to 24 months of amenorrhea. Finally, Horning
and associates18 observed that 13 of 19 patients (13 to 28 years of age) treated with oophoropexy
and total lymphoid irradiation were temporarily amenorrheic. However, at
follow-up (median interval after treatment, 87 months), 18 of 19 patients
were menstruating. Not surprisingly, several authors have found that the age of the patient
at treatment is inversely related to the likelihood of continuation
or resumption of regular menses.18,19 That is, younger women are more likely to retain ovarian function after
treatment than are older women. Younger women have larger pools of oocytes
before therapy than do older women. Logically, after therapy, younger
women are more likely to have some functional oocytes persisting. Children
seem especially resistant to ovarian failure caused by abdominal
irradiation.19 However, at high doses (2000 to 3000 rads), even children will suffer
ovarian failure.20,21 Because so few data are available, it is difficult to generalize about
the response of the human fetal ovary to x-rays. As is true of other potential teratogens, the effects
of radiation on the fetus are influenced by the specific type of agent, the
dose, the time in gestation when the fetus is exposed, and the
genetic susceptibility of mother and fetus. Fetal mice exposed to 120 to 200 rads
on day 15 (total gestation, 18 to 20 days) show decreased
fertility during their adult life.14 Similarly, rats exposed to 100 rads on day 15.5 in utero (total gestation, 21 to 22 days) show markedly decreased oocyte number.2 However, significant species' difference in fetal susceptibility may exist.2,7 Human fetal germ cells appear more resistant in vitro than do rat or monkey germ cells.22 For example, Tabuchi14 did observe delayed menarche in women exposed to 500 rads or more in utero at Hiroshima and Nagasaki at 1 to 3 months of fetal age. Among Japanese
women exposed in utero to either 10 to 50 rads or 50 to 459 rads, Burrow and coworkers23 found no significant difference in age at menarche. Similarly, in Japanese
women exposed prenatally, Blot and associates24 showed no difference in the number of childless marriages, the number
of births, or the interval between marriages and first births. To summarize the effects of high-dose external ionizing radiation, ovarian
doses of 150 rads or less usually have no deleterious effects on young
women; however, an occasional woman older than 40 years will be sterilized
by this dose (Table 1). Four hundred rads will cause permanent amenorrhea in almost all women
older than 40 years. A variable percentage of younger women will be
rendered temporarily, or permanently, amenorrheic at doses of 250 to 800 rads. Acute
or fractionated doses of greater than 800 rads will render
virtually all women permanently sterile. Children show greater resistance
to radiation castration than do adult women. Table 1. Effect of Ionizing Radiation on Ovarian Function
Minimum Ovarian | | | |
Dose | Dose Rate | Effect | Evidence |
150 | 150 in fractions over | No deleterious effect in most young | No permanent change in menstrual |
| 28 days | women; some risk of sterilization in | cycle in three patients aged 20–31 |
| | women more than 40 years of age. | years.16,17 |
250–500 | 263–500 fractionated | Variable. Among women 15–40 years, | Of 14 patients 15–24 years old, 4 |
| over 12–41 days | about 30% are permanently sterilized; | showed permanent amenorrhea |
| | some of the others may suffer | and 10 had normal menstrual cycles |
| | temporary amenorrhea. | (some had temporary amenorrhea |
| | | 1 eventually became pregnant).15 |
| 400–700 in 1–4 fractions | Among women older than 40 years, almost | Artificial menopause was induced |
| | 100% are permanently sterilized. | with 400 rads in women older than |
| | | 40 years.11 |
500–800 | 530–660 fractionated | Variable. About 60% of women | Of seven patients 13–32 years of age, |
| over 30–55 days | 15–40 years are permanently sterilized; | four showed permanent |
| | of the others, some may suffer | amenorrhea and three had normal |
| | temporary amenorrhea. | menstrual cycles.15 |
| 500–800 fractionated | Variable. About 70% of women | Of seven patients 19–36 years, five |
| over 28 days | 15–40 years are permanently sterilized; | showed permanent amenorrhea |
| | others may suffer temporary | and two suffered temporary |
| | amenorrhea. | amenorrhea; one of these |
| | | eventually became pregnant.16 |
>800 | 900–3500 fractionated | 100% permanently sterilized | Four patients 18–32 years showed |
| over 28 days | | permanent amenorrhea.16 |
| 700–1500 | 100% permanently sterilized | Artificial menopause was induced in |
| | | women of all ages.4 | (Adapted from Ash P: The influence of radiation on fertility in man. Br
J Radiol 53:271, 1980.)Low-Dose External Ionizing Radiation To extrapolate the effects of high-dose irradiation to low-dose short-term
or long-term (occupational) exposure would not necessarily be correct. In
those instances in which oocyte killing has been measured directly, there
did not appear to be a clear threshold dose under the observed
conditions.3 However, Mondorf and Faber25 studied 180 women exposed to 1 to 5 rads during infancy. No differences
were found between the control subjects and the exposed patients with
respect to the number of children born and the age distribution of births. There
was no evidence of a decrease in fertility later in life. In
a second study, Meyer and colleagues26 investigated the effects of prenatal x-ray exposure due to pelvimetry
on subsequent reproductive performance and found no decrease in the birth
rate of women exposed as fetuses when compared with control subjects. Summarizing
the effects of radiation in utero, Brent2 concluded that short-term doses of less than 25 rads will not cause sterility
in human female fetuses. The above imply that even if no threshold
exists, the number and proportion of oocytes killed by low-dose radiation
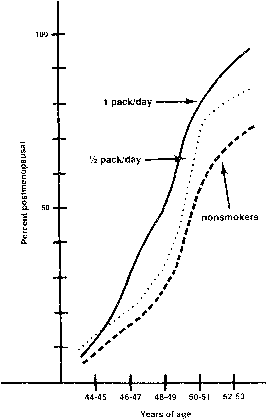
are presumably small enough not to affect fertility. However, depletion
of resting follicle complexes could accelerate ovarian failure
and age at menopause. Radionuclides Radionuclides are internal emitters, radioisotopes that are concentrated
in specific tissues, potentially emitting radioactivity as long as they
remain in the body. The effects of radioisotopes have been less well
studied than the effects of externally administered radiation. Again, it
is difficult to generalize about their effects, because such effects
are dependent on the specific radionuclide, the dose and dose rate, tissue
distribution, genetically controlled susceptibility, and the
pathologic condition of the recipient. In the case of fetal exposure, the
time during gestation in which the agent is administered and its
ability to cross the placenta are also crucial. Although not implicated in ovarian failure after exposure in adulthood, the
effects on the fetus of several internal emitters (radioactive isotopes) should
be considered. Although therapeutic doses of 131I (2 to 10 mCi) to the mother can ablate the fetal thyroid, the effect
of 131I on the human fetal ovary is unknown. Oral administration of 5 mCi 131I delivers only 1 to 2 rads to the adult gonad. Presumably, then, the dose
to the fetal gonad after maternal administration is of similar magnitude
or less and thus unlikely to be significant. Certainly, small doses
of 131I (5 to 50 μ Ci) administered to the mother for diagnostic purposes (thyroid scan) have
not been reported to be harmful to the fetus.2 Tritium (3H) is a potential pollutant from nuclear energy production. Animal
studies have shown that tritiated drinking water (HTO) and tritiated
thymidine have a deleterious effect on the in utero development of the rat, mouse, and monkey oocyte.2,3 Cesium-137 (137Cs), 8.4 rads/day, produces sterility in female mice exposed during gestation
and the early neonatal period.3 Human exposure in this range is unlikely, barring a major nuclear reactor
accident. Nonionizing Radiation Nonionizing radiation is a form of electromagnetic radiation with a longer
wavelength and lower energy than ionizing radiation. Such low-energy
waves produce biologic effects by means of hyperthermia, excitation, and
possibly other mechanisms. This energy could, in theory, be ovotoxic
in humans. Prediction of the biologic effects of nonionizing radiation
depends, again, on many factors. In particular, the wavelength, frequency, and
intensity are important. In general, the higher the frequency, the
lower the tissue-penetrating power and the less likely an
effect occur. Microwaves, shortwaves, and ultraviolet light are forms of nonionizing
irradiation. Ultraviolet light does not penetrate tissue well; therefore, it
cannot affect either adult or fetal gonadal tissue. Shortwaves
are of lower frequency than microwaves and ultraviolet light and have
greater tissue-penetrating power. For example, 27.5 MHz (cycles/second) shortwave
radiation can heat mammalian tissues to a depth of 10 to 12 cm.2 In one set of experiments, pregnant rats exposed to 27 MHz shortwaves
showed an increased rate of embryo resorption.2 In contrast to shortwaves, the frequency of most microwave ovens and diathermy
machines is 2450 MHz. Such waves cannot penetrate human tissue
and produce a significant thermal effect beyond 3 to 4 cm.2 It seems unlikely, then, that 2450-MHz microwaves actually reach the human
fetus in any common clinical situation. Rubin and Erdman reported
four women who were treated with microwave radiation (2450 MHz) for pelvic
inflammatory disease and who, in addition, were pregnant or became
pregnant during therapy.27 Three of the women delivered healthy infants. The fourth patient spontaneously
aborted, but subsequently delivered a healthy baby during a later
pregnancy, in which she also received microwave therapy. In summary, there is no evidence that clinically relevant microwave exposure(2450-MHz
microwave ovens, most diathermy machines) could cause ovarian
failure in either fetuses or adults. Even a microwave oven that
leaked would not cause significant ovarian exposure. The same is true
of ultraviolet light. Short-wave exposure, however, may have deleterious
effects. |