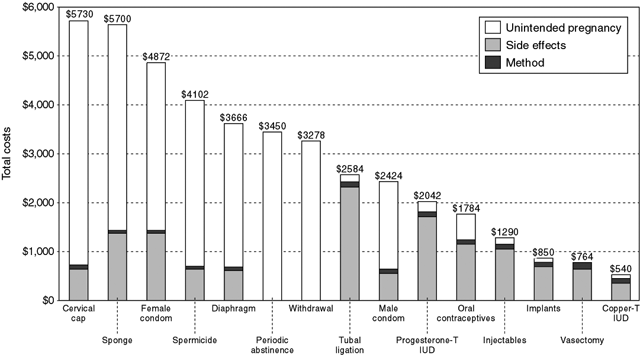
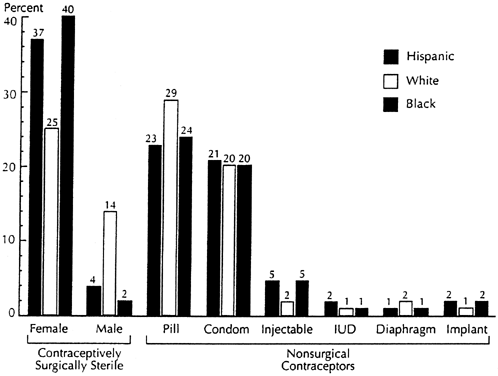
The 1995 National Survey of Family Growth (NSFG) provides the most current definitive data on the contraceptive methods used by US women aged 15 to 44 years. As shown in Figure 1, female and male sterilization and OCs account for 65% of contraceptive usage.9 DMPA, levonorgestrel (Norplant), and IUDs account for another 5% of contraceptive use. Therefore, 30% of US women are not using effective contraceptive methods.
In both Canada and the United States, a substantial percentage of those desiring contraception rely on male or female sterilization, whereas in France, only 3% of women use female sterilization and male sterilization is virtually nonexistent (Table 2).9,11,12 The percentage of US women who rely on the male condom as their contraceptive method is twice that in either Canada or France. Fewer than 30% of US women and fewer than 20% of Canadian women use OCs as their contraceptive method. France is unique among these developed countries, with its fairly high level of OC use, even among older women, and of IUD use, and its low use of female sterilization. Access to female sterilization is limited in France and in many developing nations.12 In less developed countries, the IUD is the most popular modern reversible contraceptive method, followed by the male condom.2 However, in more developed regions, the OC is the most popular method of birth control, followed by the male condom and then by the IUD.2
TABLE 2. Comparison of Contraceptive Methods Used in
Developed Countries: 1994---1994
|
Country |
Ages |
Method (Percentage of Reproductive-Age Women Using) |
|||
|
|
|
OC |
IUD |
Male Condom |
Male/Female Sterilization |
|
United States |
15---44 |
26.9 |
0.8 |
20.4 |
38.6 (female 27.7) |
|
Canada |
15---49 |
16.9 |
2.6 |
9.5 |
27.9 (female 17.3) |
|
France |
20---44 |
40.2 |
15.8 |
7.8 |
3.0 (female only) |
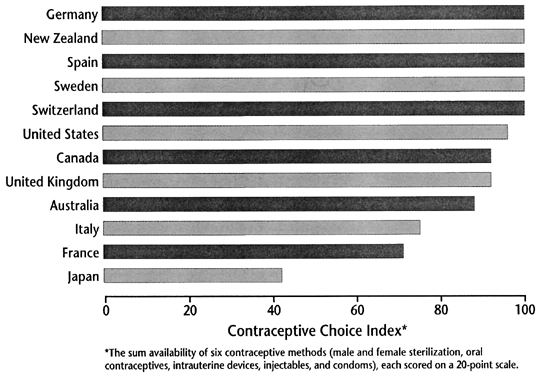
Despite the many advances made in contraception, access to a wide range of method choices is limited, even in developed countries. When nations were ranked according to the availability of six contraceptive methods (male sterilization, female sterilization, OCs, IUDs, injectables, and condoms) in 1996, the United States ranked sixth as a result of low availability of the IUD (Fig. 2).1
|
|
Likewise, Italy and France ranked tenth and eleventh because of limited access to sterilization, and Japan ranked last because at that time OCs were not available. Lack of an adequate variety of contraceptive choices has a direct impact on the percentage of couples who use any method. Data from 36 developing countries indicate that when only one or two methods are available, the prevalence of contraceptive use is lower than 30%, whereas when five or six methods are available, use increases to more than 60%.2
High Rates of Sterilization in US Women
In the United States, couples have compensated for the lack of contraceptive choices by increased reliance on voluntary sterilization.13 According to estimates for women from the 1995 NSFG and for men from the 1987–1988 National Survey of Family Households (NSFH), three quarters of all intact marriages rely on sterilization as the contraceptive method.14 Based on data from the National Hospital Discharge Survey for the period from 1970 to 1995, Westhoff and Davis estimate that 11 million US women aged 15 to 44 years rely on tubal sterilization for contraception.15 Each year in the United States, 700,000 sterilization procedures are performed; half these are done as outpatient procedures.15
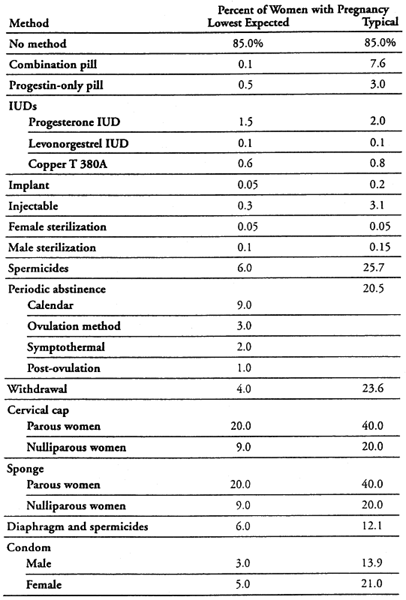
Those who opt for surgical sterilization to prevent pregnancy believe that the method is “foolproof” when, in fact, failure rates across all types of procedures have been underestimated at 0% to 0.4%.16 The US Collaborative Review of Sterilization (CREST), a multicenter, prospective cohort study that included a total of 10,685 women who underwent tubal sterilization between 1978 and 1986 at 16 US medical centers, found 10-year cumulative rates ranging from 7.5 to 1000 for unipolar coagulation and postpartum partial salpingectomy to 36.5 to 1000 with spring clip application17 (Table 3). The risk of pregnancy was highest among women who were sterilized at younger ages (28 to 33 years) compared with those sterilized at age 34 years and older.
TABLE 3. Life-Table Cumulative Probabilities of Pregnancy
Among Women Undergoing Tubal Sterilization by Method (Cumulative Probability
per 1000 Procedures and 95% Confidence Interval)
|
Method (n)* |
Years Since Sterilization |
||
|
|
1 |
5 |
10 |
|
Bipolar coagulation (2267) |
2.3 (0.3---4.2) |
16.5 (10.6---22.4) |
24.8 (16.2---33.3) |
|
Unipolar coagulation (1432) |
0.7 (0.0---2.1) |
2.3 (0.0---4.8) |
7.5 (1.1---13.9) |
|
Silicone rubber band (3329) |
5.9 (3.3---8.5) |
10.0 (6.4---13.5) |
17.7 (10.1---25.3) |
|
Spring clip (1595) |
18.2 (11.5---24.9) |
31.7 (22.6---40.7) |
36.5 (25.3---47.7) |
|
Interval partial salpingectomy (425) |
7.3 (0.0---15.5) |
15.1 (3.1---27.1) |
20.1 (4.7---35.6) |
|
Postpartum partial salpingectomy (1637) |
0.6 (0.0---1.9) |
6.3 (2.2---10.3) |
7.5 (2.7---12.3) |
|
All methods (10,685) |
5.5 (4.1---6.9) |
13.1 (10.8---15.4) |
18.5 (15.1---21.8) |
n, number of women sterilized.
(Adapted from Peterson, HB et al: The risk of pregnancy after tubal sterilization: Findings from the U.S. Collaborative Review of Sterilization. Am J Obstet Gynecol 174:1161---1170, 1996.)
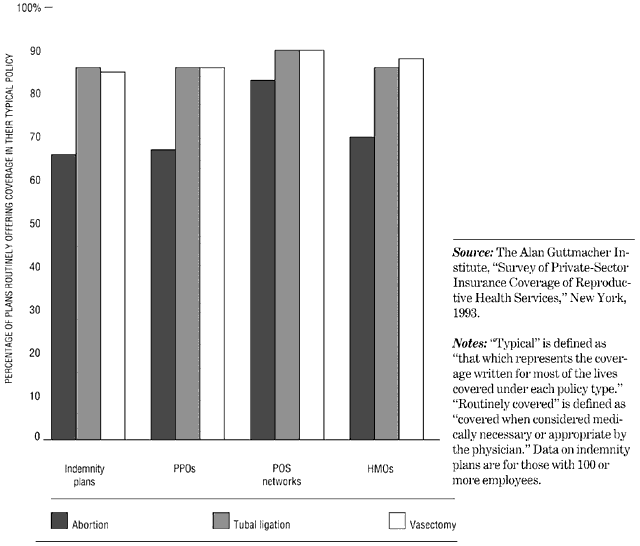
Several factors contribute to the high prevalence of sterilization among US couples. Coverage of costs by health care providers has a major impact on contraceptive choice. A recent survey by the Alan Guttmacher Institute found that 85% to 90% of all managed care plans routinely covered tubal sterilization and vasectomy and at least two thirds covered abortions performed by dilatation and curettage or suction aspiration (Fig. 3).18
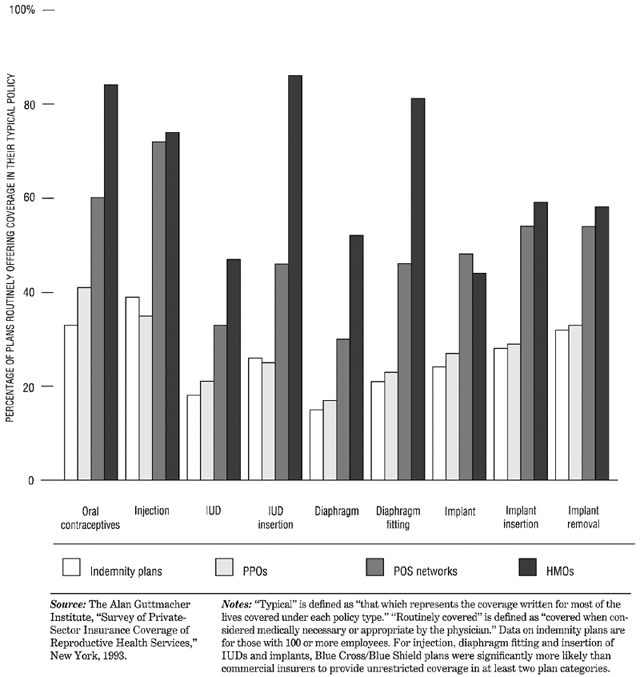
This is in sharp contrast to the coverage provided for reversible contraception by these same health care plans (Fig. 4).18
None of the reversible contraceptive methods is routinely covered by 49% of typical indemnity plans, and only 15% cover provider costs for all five of the most commonly used methods: IUD, diaphragm, contraceptive implant, injection, and OC. Moreover, although most traditional indemnity plans and preferred provider organizations provide coverage for prescription drugs in general, only about 40% routinely cover the cost of OCs.18 In contrast, coverage for OCs is provided by 84% of health maintenance organizations.
The attention given by the news media to negative reports regarding reversible methods of contraception has also contributed to high use of female sterilization in the United States. According to Philip D. Darney in a conversation in April 2000:
The heavy reliance of American couples on sterilization rather than temporary methods is due partly to reimbursement issues and partly to the negative reputation one method after another has acquired as a result of scare stories by the media—beginning with the birth control pill scare in the early 1970s, the Dalkon Shield debacle in the late 1970s, and then the Norplant reaction in the 1990s. Couples have been literally driven toward sterilization. The final irony is evidence showing that sterilization isn't necessarily more effective than the IUD or Norplant or even oral contraceptives.
Education also affects contraceptive practices. Data from the 1995 NSFG showed that among non-Hispanic white and non-Hispanic black women aged 22 to 44, use of female sterilization decreased as the woman's years of education increased.9 Among those with less than 11 years of schooling, 50% used female sterilization and 11% used male sterilization. By contrast, among those with at least 13 years' education, 16% used female sterilization and 14% used male sterilization as the contraceptive method. Combined data from the 1995 NSFG and the 1987–1988 NSFH indicate that among couples who chose sterilization, the likelihood of female sterilization relative to vasectomy decreases as the wife's education increases, which is consistent with the expectation that better-educated husbands are more likely to undergo vasectomy.14
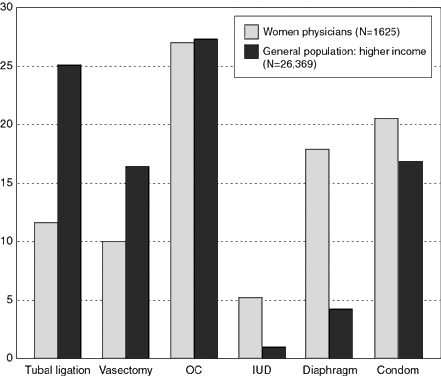
Frank provides further insight into the impact that education can have in improving use of reversible contraceptive methods.19 A comparison of data on contraceptive use from the 1993–1994 Women Physicians' Health Study, which included female physicians aged 30 to 44 and the general population of women aged 15 to 44 (1990 NSFG) showed that overall, female physicians were more likely to use contraception than higher income nonphysicians (73% versus 64%).
As shown in Figure 5, compared with the general population of higher income women, female physicians were five times more likely to use IUDs (5% versus 1%), more likely to use diaphragms (18% versus 4%) and condoms (20% versus 17%), and less likely to use tubal sterilization (12% versus 25%) or vasectomy (10% versus 16%). Compared with other female physicians, obstetrician/gynecologists were more likely to use OCs, diaphragms, and IUDs and less likely to rely on male or female sterilization. However, Frank notes that the comparisons may have been biased by the lower fecundity and higher rates of marriage of these female physicians. Sterilization is not an appropriate contraceptive method until careful consideration has been given to irrevocably ending childbearing potential.
Unintended Pregnancy and Abortion
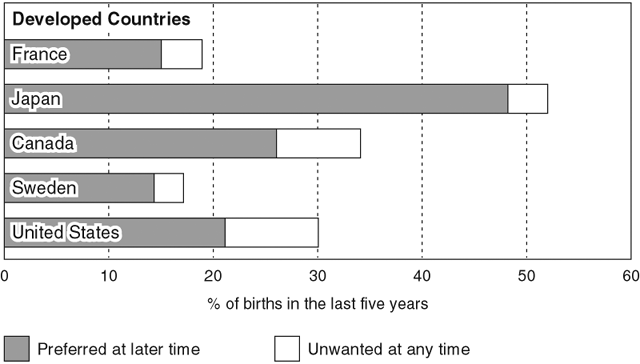
Nearly half of all pregnancies and one third of all births in the United States in 1994 were unintended, and over 50% of unintended pregnancies ended in abortion (Table 4).20
TABLE 4. Unintended Pregnancy by Age Group: United States,
1994
|
|
Age at Outcome (yr) |
||||||
|
|
15---19 |
20---24 |
25---29 |
30---34 |
35---39 |
|
Total |
|
Pregnancies unintended (%) |
78.0 |
58.5 |
39.7 |
33.1 |
40.8 |
50.7 |
49.2 |
|
Births unintended (%) |
66.0 |
38.7 |
22.2 |
18.0 |
23.2 |
26.7 |
30.8 |
|
Unintended pregnancies ended in abortion (%) |
45.3 |
55.2 |
56.7 |
55.7 |
56.3 |
64.7 |
54.0 |
Numerator for rates includes women aged 40 and older; denominator includes women aged 40---44.
(Adapted from Henshaw SK: Unintended pregnancy in the United States. Fam Plan. Perspect 30:24---29 & 46, 1998.)
The highest rates of unintended pregnancies and births occurred in teens (ages 15 to 19) and young women (ages 20 to 24), followed by older reproductive-age women at least 40 years of age (Fig. 6). However, compared with 1987, the rate of unintended pregnancies in 15- to 19-year-olds declined from 79.3 in 1000 women to 71.1 to 1000 women.21 This decline is attributable primarily to increased use of long-acting hormonal contraception by teenagers.4,9
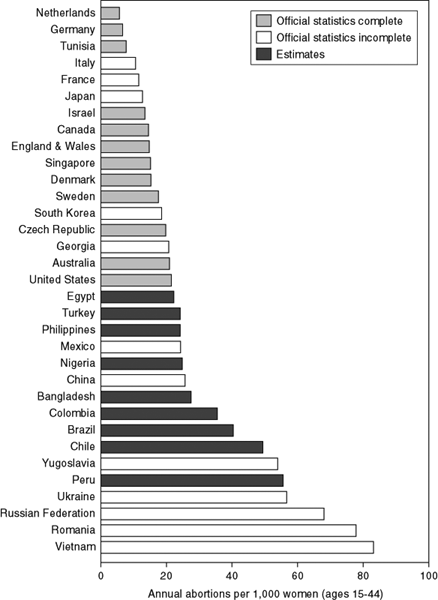
The rate of unintended births in the United States is similar to those in Canada, which has comparable contraceptive access, and higher than that in Sweden where a greater number and variety of contraceptive methods are available (see Fig. 2).1,4,21,22 However, the abortion rate in the United States is higher than that of other developed countries as well as many less-developed nations (Fig. 7).21,22 For example, according to recent statistics, the abortion rate per 1000 women aged 14 to 44 years was 6.5 in the Netherlands and 20 to 22.9 in the United States.23 With its heavy reliance on abortion and sterilization to limit family size, the United States resembles a less developed country more than it does other industrialized nations, such as Germany or Canada.
|
|
 40
40