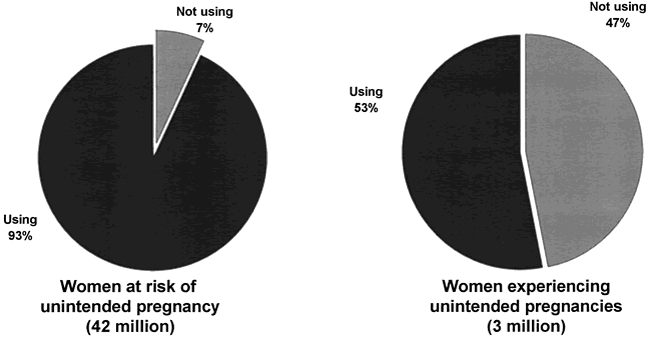
More than nine in 10 women ages 15 to 44 years in 1995 who were at risk of unintended pregnancy were using a contraceptive method (Table 2). Thirty-six percent relied on contraceptive sterilization of themselves or their partner, 52% used reversible medical methods, 5% used nonmedical methods such as withdrawal and periodic abstinence, and 8% were currently using no contraceptive, even though they were at risk of unintended pregnancy.
| Total at Risk |
| Union Status | Race/ethnicity | Poverty status | |||||||||||||
Contraceptive | of Unintended | Age | Current |
| Former | Never | Non-Hispanic |
| 0– | 150– |
| |||||||
Method Used | Pregnancy | 15–19 | 20–24 | 25–29 | 30–34 | 35–39 | 40–44 | Married | Cohabiting | Married | Married | White | Black | Other | Hispanic | 149% | 299% | 300%+ |
Total | 100 | 100 | 100 | 100 | 100 | 100 | 100 | 100 | 100 | 100 | 100 | 100 | 100 | 100 | 100 | 100 | 100 | 100 |
Sterilization | 36 | 0 | 5 | 20 | 38 | 56 | 66 | 46 | 27 | 50 | 8 | 36 | 38 | 29 | 37 | 40 | 37 | 32 |
Female | 26 | 0 | 4 | 16 | 28 | 39 | 47 | 30 | 23 | 47 | 8 | 23 | 36 | 21 | 34 | 37 | 27 | 19 |
Male | 10 | 0 | 1 | 4 | 10 | 18 | 19 | 16 | 4 | 3 | 0 | 13 | 2 | 8 | 4 | 3 | 10 | 14 |
Reversible medical methods | 52 | 76 | 83 | 68 | 51 | 33 | 23 | 43 | 63 | 39 | 74 | 52 | 49 | 57 | 49 | 48 | 50 | 55 |
Oral contraceptives | 25 | 35 | 48 | 37 | 27 | 11 | 6 | 19 | 34 | 19 | 38 | 27 | 21 | 18 | 21 | 22 | 25 | 26 |
Male condom | 19 | 30 | 24 | 23 | 17 | 16 | 12 | 17 | 18 | 14 | 28 | 18 | 18 | 34 | 19 | 16 | 18 | 21 |
Depo Provera injectible | 3 | 8 | 6 | 4 | 2 | 1 | 0 | 2 | 4 | 2 | 5 | 2 | 5 | 2 | 4 | 5 | 3 | 2 |
Barrier methods† | 2 | 0 | 1 | 1 | 3 | 3 | 3 | 3 | 2 | 1 | 1 | 2 | 1 | 1 | 1 | 1 | 2 | 3 |
Norplant (implant) | 1 | 2 | 3 | 2 | 1 | 0 | 0 | 1 | 2 | 1 | 2 | 1 | 2 | 2 | 2 | 3 | 1 | 1 |
Spermicides | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 2 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 |
IUD | 1 | 0 | 0 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 0 | 1 | 1 | 1 | 1 | 1 | 1 | 1 |
Nonmedical methods | 5 | 5 | 4 | 5 | 6 | 6 | 5 | 6 | 5 | 4 | 4 | 5 | 3 | 9 | 5 | 4 | 5 | 6 |
Withdrawal | 3 | 3 | 3 | 4 | 3 | 3 | 2 | 3 | 3 | 3 | 3 | 3 | 1 | 4 | 3 | 3 | 3 | 3 |
Periodic abstinence | 2 | 1 | 1 | 1 | 3 | 3 | 2 | 3 | 2 | 1 | 1 | 2 | 1 | 5 | 2 | 1 | 2 | 3 |
No method | 8 | 19 | 9 | 6 | 6 | 6 | 7 | 5 | 5 | 8 | 14 | 7 | 10 | 5 | 9 | 8 | 8 | 7 |
IUD, intrauterine device.
*Alan Guttmacher Institute tabulations of the 1995 National Survey of Family Growth (Cycle V).
† Female barrier methods include the diaphragm, cervical cap, sponge, and female condom.
Patterns of contraceptive use differ by age. Younger women at risk of unintended pregnancy are more likely than older women to use no method of contraception. Nearly one in five teen women at risk uses no method compared to 6% to 7% of women at risk ages 25 and older. The proportion using reversible medical methods declines steeply with age from more than four of five women ages 20 to 24 years to fewer than one quarter of those ages 40 to 44. OCs are the most commonly used method among women younger than 30 years of age, accounting for 35% to 48% of these women. Condoms are second in popularity among this age group, accounting for 23% to 30% of women in this group. Although fewer than 3% of women at risk use Depo Provera injectible contraceptives, this method has grown in popularity since its introduction in the United States, particularly among young women. Eight percent of teens at risk used this method. As women become older and complete their families, male and female contraceptive sterilization becomes increasingly common, rising steeply from 5% of women at risk ages 20 to 24 to one in five women in their late 20s and to two of three women ages 40 to 44. Among women in their 20s, female sterilization is approximately four times more common than vasectomy. The margin narrows among older women to between two and two and a half times more common.
The proportion of women at risk of unintended pregnancy who use no contraceptive method is highest among never-married women, 14% compared to 5% of those who are currently married or cohabiting and 8% of formerly married women. Sterilization is the most frequently used method among women who are currently married (46%) as well as formerly married women (50%). The pill is the most commonly used method among never-married women (38%) and cohabiting women (34%). Condoms are most likely to be used by never-married women (28%).
The growing awareness of the protection that latex condoms give against contracting sexually transmitted diseases, including AIDS, undoubtedly has contributed to the increase in condom use among never-married women using contraception from 12% in 1982, to 15% in 1988, to 30% in 1995. The increase also was steep among formerly married method users: from 2% in 1982, to 6% in 1988, to 15% in 1995. Among currently married women, the proportion rose only from 14% in 1982 and 1988 to 17% in 1995.1,10
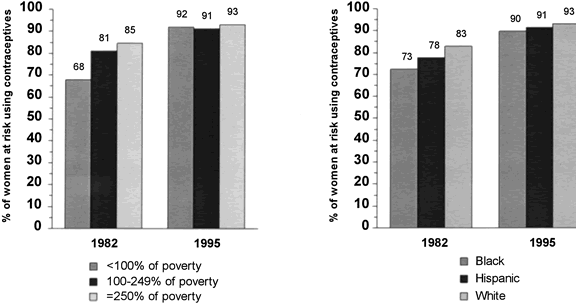
Although poor women and minority women at risk of unintended pregnancy have, in the past, been more likely than higher income and non-Hispanic white women to be using no contraceptive method, these differences have lessened. Compared to the 1980s, in 1995 there were no significant race/ethnicity or poverty differences in the percentages of women at risk of unintended pregnancy who used no method of contraception (Fig. 1). However, there is some variation in the types of methods used according to these subgroups. Low-income women are less likely to rely on reversible methods and more likely to rely on sterilization than higher income women. Forty percent of women at risk of unintended pregnancy who are below 150% of the poverty level use sterilization compared to 32% of women at 300% of poverty and above. Poor women relying on sterilization are more likely than higher income women to have been sterilized themselves rather than have a partner who has a vasectomy. Female sterilization accounts for 92% of all contraceptive sterilization among poor women compared with 58% among those with higher incomes.
|
|
Contraceptive use at first intercourse rose from 50% of women who began having sex before 1980 to 76% of those who first had intercourse from 1990 to 1995. This change resulted from greater condom use, which increased from 18% of those who had intercourse for the first time before 1980, to 54% of those beginning intercourse more recently.11