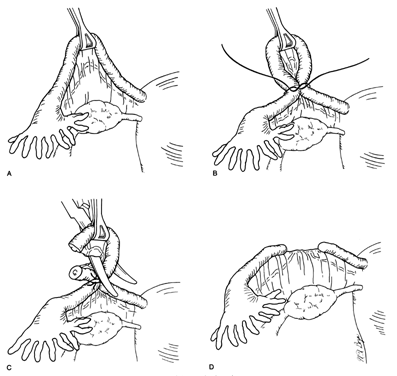
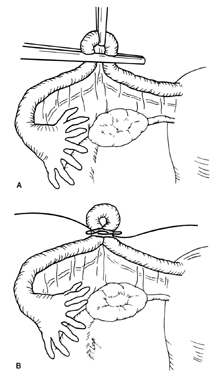
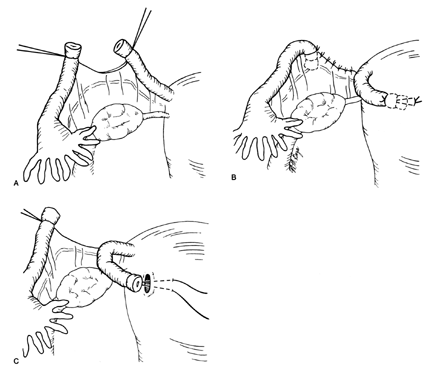
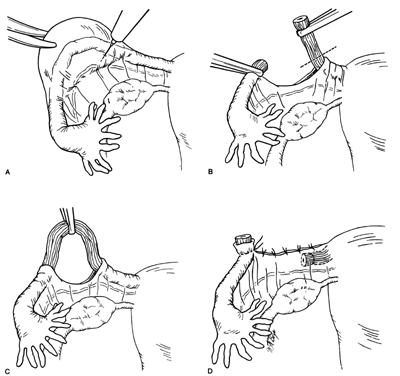
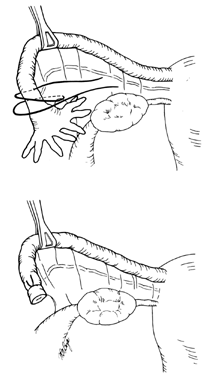
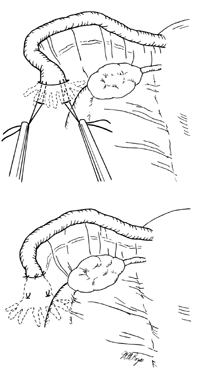
The Pomeroy technique for bilateral partial salpingectomy is the preferred method for interval surgical female sterilization (Fig. 1). The popularity of this technique is based on its inherent simplicity and its long-established efficacy. Following accurate identification of the fallopian tube, a Babcock clamp is placed around the proximal portion of the tubal ampulla and the tube is elevated to reveal the vascular supply of the mesosalpinx (see Fig. 1A). A single strand of absorbable suture material (1-0 plain catgut) is placed around the elevated loop of tube and firmly tied. The fallopian tube is thus ligated and the blood supply is occluded simultaneously (see Fig. 1B). A hemostat may now be placed on the suture strands immediately distal to the knot, and the excess suture may be excised. The hemostat now becomes a useful holder for the next step in the procedure. At this point, a second tie of the same suture material may be applied at the discretion of the surgeon, but this is not usually necessary. While gentle traction is maintained on the elevated section of tube, the open blade of the Metzenbaum scissors is used to pierce the mesosalpinx and approximately 1 cm of tube is excised (see Fig. 1C). The excised tube should be appropriately labeled and sent to the pathology laboratory for documentation. With the contraction of the muscularis, the white avascular endosalpinx appears as an elevated area in the center of each cut segment. The proximal and distal ends of the divided and ligated oviduct are now examined for bleeding and then the tube is returned to the abdominal cavity and the procedure is repeated on the opposite tube.
The end result following dissolution of the absorbable suture material and return of the proximal and distal portions of the tube to their normal anatomic positions is shown in Figure 1D. The use of absorbable suture material allows this separation to occur and is probably a critical factor in the development of the anatomic discontinuity. This factor is undoubtedly related to the low failure rate reported for this procedure. Accordingly, the newer synthetic absorbable suture materials with longer dissolution times are probably less desirable than simple plain catgut.
The major advantages of the Pomeroy technique are that it is easily taught, is simple to perform, and is highly effective. Its acceptance for both puerperal and interval sterilization is quite high. It can be performed either abdominally or vaginally, and the complications are minimal. It has no major disadvantages. The reported pregnancy rate is two to four pregnancies per 1000 procedures.6