Difficult Dilation With early pregnancies, especially in the young primigravida, the cervical
canal may be quite narrow, tortuous, and resistant to dilation. The
exocervix may be small, with little space for the tenaculum or stabilizer
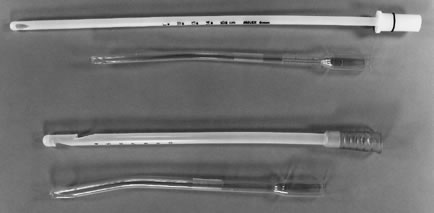
to be applied. Flexible cannulas of the Karman design may be advantageous; sometimes
the 4-mm cannula can be inserted as a flexible sound, and
this can be followed with a 5-mm and then a 6-mm cannula to evacuate
the uterus. Rigid instruments are avoided altogether with this
approach, but on occasion the curve on a rigid cannula may pass more
easily. If the pregnancy is beyond 8 menstrual weeks, the 6-mm cannula
may not consistently evacuate all of the gestational tissue. Therefore, the
operator could use rigid dilators after first probing the cervical
canal with the smaller cannula. Another option is to insert a laminaria
tent and perform the abortion the next day. Misoprostol would produce
cervical softening and dilation in several hours. A less desirable
option is to delay the abortion a week to await greater cervical softening. Vasovagal Reaction In some women, manipulation of the cervix induces a marked vagal response
with bradycardia, hypotension, and possibly syncope. If the patient
loses consciousness, a tonic-clonic movement may be seen that can be
confused with a convulsion. This syndrome has been seen with insertion
of intrauterine contraceptive devices and may also be seen with venipuncture
and other procedures in susceptible men as well as women. When
it occurs during cervical dilation, vasovagal reaction must be distinguished
from local anesthetic toxicity. With a vasovagal response the
pulse is initially quite slow but rapidly returns to normal as the patient
regains consciousness, a very different picture from the loss of
consciousness, convulsions, and cardiovascular collapse of local anesthetic
toxicity. If the patient begins to lose consciousness during cervical
manipulation, the surgeon should immediately stop the painful stimulus, give
atropine 0.4 to 1.0 mg intravenously or subcutaneously, turn
the patient to a more comfortable position, and then monitor vital
signs while the patient recovers. When the patient has fully recovered, the
abortion procedure may be safely resumed. Inability to Evacuate the Pregnancy and Failed Abortion Failed abortion is a continuing pregnancy, whether recognized immediately
or recognized on another day. Before attempting a second procedure, the
operator should consider the possibility of a uterine anomaly, multiple
gestation, ectopic pregnancy, or gestation larger than expected.64,67,68,69,70 Usually a repeat ultrasound is indicated. In a very retroverted or very anteverted uterus the pregnancy may be difficult
to reach with the usual instruments. If the pregnancy is located
at the fundus, the posterior wall of a retroverted uterus, or the anterior
wall of an anteverted uterus, it may not be reached by the minimal
curve of the cannula. Using a shorter speculum and straightening
the cervix is helpful, as is ultrasound guidance. A polyp forceps or curette
bent into an appropriate curve may loosen the pregnancy, and suction
can then remove the remainder. Contracting the uterus with a prostaglandin
or oxytocic may straighten the axis of the uterus. Intraoperative
ultrasound to ensue complete removal may be helpful. When the uterus is distorted by fibroids, septa, or other anomalies, the
pregnancy may be difficult to feel or to reach with any instrument. Ultrasound
guidance is essential in this situation. If the uterine cavity
is elongated, a flexible cannula, which is longer than a rigid cannula, may
reach the pregnancy. Pregnancy More Advanced Than Anticipated When a more advanced gestation is encountered, the outcome depends on several
circumstances: the point in the procedure at which discovery of
the more advanced gestation occurs, the operator's skill and experience, the
available instruments, and staff support. If the advanced
gestational age is diagnosed because the cannula is inserted to its full
length and the fetal membranes remain intact, it is best to stop the
procedure and reconsider. The use of ultrasound in borderline situations
is strongly recommended. Where the procedure is already begun, the
membranes are ruptured, and the tissue is partly removed, the decision
is more difficult. An operator skilled in first-trimester abortion
should be able to complete a 13- to 15-week abortion using the 12-mm
vacuum cannula and standard ring forceps (Foerster) under local anesthesia
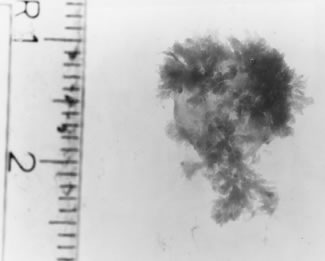
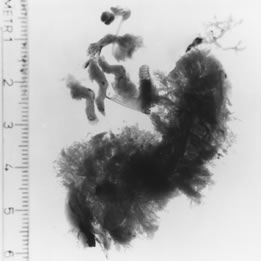
in a freestanding clinic. If the error in sizing is not appreciated
until some fetal parts have been extracted, measurement of the fetal
foot will reveal the true gestational age (Table 2). Management of gestations beyond 15 weeks varies depending on the availability
of proper instruments and a surgeon skilled with more advanced
procedures. Surgical abortion in the middle trimester, intentionally performed
by experienced operators, has been shown to be a safe procedure. However, gestational
age beyond 12 weeks is a predictor of uterine
perforation, excessive blood loss, and incomplete abortion.9,10 The difference may be in preparation: a procedure with adequate dilation, instrumentation, and
operator experience may have a better outcome
than aborting a midtrimester pregnancy by accident. If no one experienced
in later procedures is available, transfer of the patient to a hospital
or other facility, either for prostaglandin induction or cervical
dilation and uterine evacuation, is indicated. Bleeding During and After Abortion Most women have minimal bleeding during first timester abortion, and bleeding
in excess of 100 mL is uncommon with abortion under paracervical
block.3,9 Uterine atony is the most likely cause of heavy and prolonged bleeding.72 Intracervical or intravenous ergonovine (0.2 mg) or oxytocin (10 to 20 units) should
be used to contract the uterus. An alternative is buccal
or oral misoprostol, 400 μg; doses as high as 1000 μg have been used rectally for postpartum atony.72 Prostaglandin F (Hemabate) can be given intramuscularly or into the uterus. In
the absence of an obvious cervical or uterine injury, the operator
should complete the abortion, evacuating the uterus rapidly but
gently. The uterus is then massaged between two hands. The aspirated tissue
is examined to confirm gestational age and to confirm that all fetal
parts have been removed. If the bleeding does not stop, the cervix
should be rechecked for a laceration or for bleeding from the tenaculum
site. Next, the uterus is gently explored with a sharp curette, possibly
under ultrasound, checking for uterine shape and size, retained
tissue, and uterine wall irregularities or defects. Repeat suction may
remove clots and retained tissue and allow the uterus to contract. Bleeding in the postabortion period may indicate a hematometra or postabortal
syndrome, this can occur immediately or up to several days later. This
is a variant of uterine atony in which the uterus is distended
with clots that are not expelled.71 Treatment is repeat uterine evacuation and uterotonic drugs. More serious causes of bleeding include uterine injury, arteriovenous malformation, and
coagulopathy. These situations are rare but may not respond
to uterine contraction. Other treatments include reversal of coagulopathy
if possible, pelvic artery embolization, open ligation of bleeding
points, and hysterectomy as a last resort. The rate of hysterectomy
for abortion-related hemorrhage, including second-trimester procedures, is 1 in 10,000;73 rates in first-trimester procedures would be expected to be lower than
second-trimester procedures. Suspected Perforation Uterine perforation during the performance of abortion is a potentially
serious complication that can result in hemorrhage or visceral injury. Reported
rates of perforation rage from less than 1 to 3 per thousand
abortions11,12,15,74,75,76,77,78,79,80 and become more frequent with increasing gestational age.15 However, Kaali and associates77 reported a rate of 15 per thousand in a setting where laparoscopic sterilization
was performed immediately after abortion; they concluded that
perforations are frequently unrecognized and frequently benign. Many
perforations are thought to occur during sounding or dilation because
the most common site of perforations is the junction of the cervix and
the lower uterine segment.77 Lateral perforation at this location may be particularly hazardous for
the patient in that branches of the uterine artery can be lacerated with
resultant hemorrhage,77 whereas midline perforations may be benign unless other organs are injured. Perforation can be suspected when no tissue is obtained, when instruments
are inserted deeper than expected, when ultrasound shows instruments
outside the uterus, when hemorrhage occurs, or when obviously maternal
tissues such as omentum are obtained. Treatment of perforation depends
on the expected location, the woman's vital signs and condition, and
whether the abortion is complete. Some authors have reported rates
of operative evaluation and treatment as high as 80% to 100%;15,74,75 other authors do not advocate routine laparoscopy or even hospitalization.76,78 In our practice, when the uterus is already empty before a perforation
is first suspected and the perforation is thought to be midline, then
bleeding is unlikely and hospitalization may not be necessary. The woman
can be observed for several hours. If the pain and bleeding continue
to be minimal, repeated pelvic examinations are negative, and vital
signs and repeat hematocrit are stable, then the patient may be given
the telephone contact information, scheduled for a repeat examination
the next day, and allowed to go home in the company of a responsible
adult. Under any other circumstance, she should be admitted to a hospital
for observation and possible laparoscopy. If the abortion is not complete
at the time perforation is suspected, it should be completed with
the aid of ultrasound or laparoscopy. Incomplete Abortion Incomplete abortion may occur in 0.5% to 2% of surgical abortions;12 the rate depends on the operator's skill, the gestational age, and
the criteria used to make the diagnosis. Although incomplete procedures
were thought to be more common after abortion performed before 8 weeks, more
recent reports do not support this concept.64 Typically the woman returns several days after the abortion with increased
bleeding and cramping. On examination she may have an enlarged uterus
or tissue visible in the cervical os, but often examination is unrevealing. Serum
HCG levels are not often helpful; they are invariably
positive, and a steep decline does not rule out an incomplete abortion. Ultrasound
is generally not helpful: blood and debris are present in
the uterus, and the amount of retained tissue may be small. Treatment of incomplete abortion may be pharmacologic: uterotonic drugs
such as methylergonovine (Methergine) may contract the uterus and expel
the residual tissue. This method is appropriate when the amount of
retained tissue is small, if the diagnosis is uncertain between incomplete
abortion and retained blood clots, and if there is no sign of infection. If
this route is chosen, the woman should be contacted within
a few days to make sure that her symptoms have resolved. If the uterus is tender, if infection is a possibility, if the amount of
retained tissue is large, or if the woman cannot return for follow-up, then
repeat suction should be done. Repeat suction is usually easy
because the cervix is dilated, and a cannula smaller than used for the
original procedure is adequate. If infection is possible, then antibiotics
should definitely be used, and some operators prefer to use antibiotics
after a repeat curettage for any reason. Endometritis Rates of postabortion endometritis of women undergoing first-trimester
surgical abortion range from less than 0.5% to 5%;9,10,11,12,46,47,48,49,50,51,52,53,54 the incidence depends on the patient population, the incidence of other
genital infections, and characteristics of the abortion, such as the
use of general anesthesia. Typically the woman returns 3 or 4 days after
the procedure with increased cramping and bleeding, sometimes accompanied
by fever or nausea. Such symptoms 1 or 2 days after abortion may
be due to β-hemolytic streptococci. On examination, the uterus is tender and usually
slightly enlarged. Because of the normal or increased bleeding, cervical
discharge usually cannot be evaluated. Endometritis should be treated
immediately to avoid progression of infection, but if it is treated
early, outpatient treatment should be sufficient. Early-onset endometritis (1 or 2 days) should be treated with an antibiotic effective
against β-hemolytic streptococci, such as ampicillin. Other untreated infections, such
as chlamydia or bacterial vaginosis, should be considered in the
treatment plan. At our institution we frequently use the combination
of oral metronidazole and doxycycline; another combination is metronidazole
and ofloxacin. Either of these oral combinations gives serum levels
similar to levels after intravenous administration. If the woman has an incomplete abortion with endometritis, then repeat
aspiration is necessary, preferably after the first dose of antibiotics
has been given. In an outpatient setting, intramuscular ceftriaxone
is often available and provides antibiotic coverage for the aspiration; oral
antibiotics can be started afterward. Repeat aspiration of all
women with endometritis appears to be a common practice; the utility of
this approach has not been shown, however, and excessive curettage in
the face of infection has the potential for endometrial damage. Amenorrhea and Cervical Agglutination Cervical agglutination occurs when the endocervical mucosa heals with obstruction
of the cervical canal, resulting in amenorrhea and possibly
cyclic cramping.81 In our experience this may be associated with vigorous suctioning of the
lower uterine segment and cervix. It is distinguished from cervical
stenosis, such as occasionally follows cone biopsy, in that with cervical
agglutination damage to the underlying stroma is unlikely. Cervical
agglutination is easily treated by passing a small sound through the
cervical canal. In our experience, this is sufficient and rarely needs
repetition. |