Fetal Neural Tube Defects: Diagnosis, Management, and Treatment
Authors
INTRODUCTION
Despite recognition that periconceptional folic acid supplementation in reproductive age women decreases the risk of fetal neural tube defects (NTDs), these malformations remain the second most common serious fetal birth defect in the United States, surpassed only by congenital heart defects. Screening methods used to identify neural tube defects are now a component of routine obstetrical care, and include both second trimester maternal serum alpha-fetoprotein (MSAFP) levels and fetal ultrasonographic evaluations. Once an NTD is identified, various management options are available for families, including consideration of pregnancy termination, in utero fetal surgery, as well as referral to a tertiary care center for management and delivery. Therefore, it is useful for the practicing obstetricians to be aware of these complex diagnostic and management options for optimal care of the obstetric patient and fetus.1 In this chapter, the etiologies, antenatal diagnosis, and management, as well as information regarding prevention are reviewed.
ETIOLOGY: GENETICS AND EMBRYOLOGY
Neurulation is defined as the embryonic process that leads to the ultimate development of the neural tube, the precursor to the brain and spinal cord. There are two distinct phases of neurulation. In the primary phase (weeks 3–4) the brain and the neural tube form from the caudal region to the upper sacral level. Secondary neurulation (weeks 5–6) completes the distal sacral and coccygeal regions. The molecular events during neural tube development are complex and are still incompletely understood. In brief, current theories of neural tube development are related to the principle of convergent extension (CE), which is thought to direct the lengthening of cells to make the embryonic axis. This process is likely controlled by PCP (planar cell polarity), the process in which cells align and become polarized within epithelium. Multiple genes regulate these complex cellular pathways.2, 3
The failure of neurulation at any stage leads to the formation of a neural tube defect. Identification of human genes predisposing to NTDs using positional cloning is difficult due to the complex etiologies of these lesions, as well as the limited numbers of large families with multiple affected family members. The genetic basis of NTDs has focused on genes related to the folic acid pathway as well as candidates genes from animal studies. Although many genes have been associated with NTD development, no major causative gene has been identified. To date, genes in the PCP pathway implicated in CE development and neural tube formation are the most strongly implicated in NTD development.
Embryology
NTDs are a heterogeneous group of malformations resulting from failure of neural tube closure between the third and fourth week of embryologic development. Approximately 18 days after conception, the neural plate folds inward to form a central neural groove and bilateral neural folds. The cranial end of the neural tube becomes the forebrain, midbrain, and hindbrain, and a failure of closure results in anencephaly. The caudal end of the neural tube becomes the spinal cord, and a failure of posterior neuropore closure results in spina bifida. Van Allen and colleagues, using reviews of previous published clinical reports, have shown evidence of multisite neural tube closure based on five common sites for NTD lesions.4 Each closure site may be modified by unique genetic or environmental factors during development. Furthermore, certain closure sites are associated with particular fetal insults or genetic abnormalities. For example, the NTD associated with Meckel-Gruber syndrome is associated with site 4; valproic acid is associated with site 5. Martinez-Frias and colleagues5 evaluated 774 live born infants with NTDs following the multi-site classification proposed by Van Allen’s group. They classified every case by the multi-site closure model, lending support to this theory of localized cellular disruption. They could therefore estimate the prevalence of each site of closure failure; not all sites were affected with similar frequency.
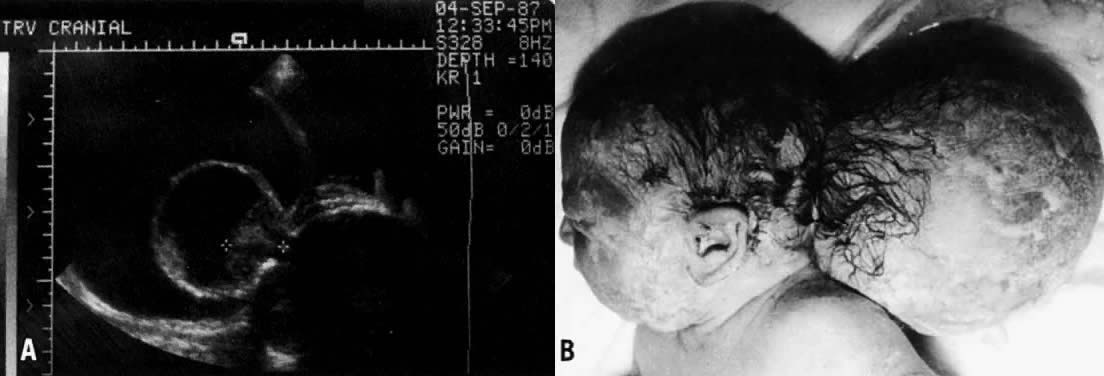
Anencephaly, encephalocele, and spina bifida are the three most common forms of NTDs. Anencephaly is the most severe of these lesions. With failure of brain development, the cranium does not form (called acrania), and the remaining neural elements are covered by a thin membrane. Encephaloceles (Fig. 1) are much less common than anencephaly or spina bifida. They are cystic extensions of the brain through an overlying scalp and skull defect, somewhat analogous to a spina bifida.
|
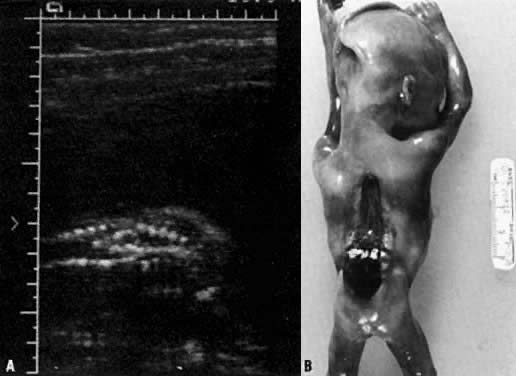
A disruption of the vertebral arches often accompanied by underlying spinal cord defects is collectively called spinal dysraphism or spina bifida (Fig. 2). It is classified as spina bifida occulta if the disruption involves only bony structures and spina bifida cystica if there is a saccular defect involving neural elements. Meningomyeloceles constitute 90% of spina bifida and are composed of neural tissue covered by meninges that extrude through the vertebral column. Alternatively, a fluid filled sac (not containing neural elements) covered by meninges that protrudes through the bony defect is called a meningocele. Although spinal dysraphism can occur at any region of the vertebral column, the most common site for these defects is the lumbosacral area.
Spina bifida is frequently accompanied by the Arnold-Chiari malformation. This anomaly results from a downward displacement of the medulla, fourth ventricle, and cerebellum through the foramen magna into the region of the cervical spine. This downward displacement of the hindbrain can hinder the egress of cerebrospinal fluid from the brain, causing an enlargement of the ventricles. This accounts for the 70–90% incidence of hydrocephalus associated with spina bifida.6
Other, less common defects include exencephaly (i.e., exteriorization of an abnormally formed brain) and iniencephaly (i.e., defect of the skull base, cervical spine, and underlying neural tissue). Myeloschisis, usually seen as an early fetal defect, describes an open flat neural plate that may be extensive.7 Myelodysplasia, or occult spinal dysraphism, describes less obvious malformations of the cord resulting from maldevelopment of the caudal region of the neural tube. These defects are often associated with lipomas or cutaneous changes overlying the region such as dimpling, sinus tracts, or hairy patches. These probably result from an embryologic mechanism similar to NTDs and may be associated with neurologic or orthopedic disabilities. Schut and coworkers have extensively reviewed the clinical aspects and variations of these defects.8
INCIDENCE AND RECURRENCE RISKS
The incidence of NTDs varies with race, geographic location, and various other predisposing factors. In the United States, the incidence is approximately one to two cases per 1000 live births, whereas the incidence in the UK is about four times greater. Since the introduction of the fortification of grain products in 1996, the incidence of NTDs has decreased about 25%.9 Families who have had a child with an NTD have a 10-fold increase in their recurrence risk. In the United States, a family with an affected child has a 2% recurrence risk of another child with an NTD. If the defect in the first affected pregnancy was anencephaly, the family has a higher risk for recurrence of anencephaly than for recurrence of spina bifida. The risks for other affected US populations are listed in Table 1.10 Between 90% and 95% of NTDs occur in families without a prior family history of an NTD.
Table 1. Estimated incidence of neural tube defects based on specific risk factors in the United States
Population | Incidence/1000 Live Births |
Mother as reference |
|
General incidence | 1.4–1.6 |
Women undergoing amniocentesis for advanced maternal age | 1.5–3.0 |
Women with diabetes mellitus | 20 |
Women on valproic acid in first trimester | 10–20 |
Fetus as reference |
|
One sibling with NTD | 15–30 |
Two siblings with NTD* | 57 |
Parent with NTD | 11 |
Half sibling with NTD | 8 |
First cousin (mother's sister's child) | 10 |
Other first cousins | 3 |
Sibling with severe scoliosis secondary to multiple vertebral defects | 15–30 |
Sibling with occult spinal dysraphism | 15–30 |
Sibling with sacrococcygeal teratoma or hamartoma |
|
NTD, neural tube defect.
*Risk is higher in UK studies. Risk increases further for three or more siblings or combinations of other close relatives.
Main DM, Mennuti MT: Neural tube defects: Issues in prenatal diagnosis and counseling. Obstet Gynecology 67:1–15, 1986.
Eighty-five per cent of NTDs occur by multifactorial inheritance, a genetic predisposition from an interaction between various genes and environmental factors. The etiologic heterogeneity of NTDs was best illustrated by Holmes and coworkers, who reported that, of 106 liveborn or stillborn infants with an NTD, about 12% had identifiable causes.11 A small proportion of NTDs occur because of single-gene disorders, chromosomal aneuploidy, and teratogen exposure. Meckel syndrome is the most common of the single-gene disorders associated with an NTD. This autosomal recessive syndrome includes posterior encephalocele, polydactyly, cleft palate, and cystic dysplasia of the kidneys. Because the recurrence risk for such a defect is 25%, it underscores the need for careful evaluation of all infant with NTDs, because recurrence risks depend on the cause of the malformation.
Chromosomal aneuploidy also accounts for a small percentage of NTDs. Of the various types of NTDs, encephaloceles and spina bifida are more likely to be associated with triploidy; with trisomies 13, 18, and 21; and with various unbalanced translocations. The recurrence risk for these disorders varies with the mechanism responsible for the aneuploidy. For example, the recurrence risk for a trisomy is approximately 1% and triploidy is thought to be a sporadic event with a negligible recurrence risk. Recurrence estimates for translocations depend on the specific nature of the translocation and whether they are maternally or paternally transmitted. Significant controversy remains as to whether patients in whom a fetus appears to have an isolated spina bifida should undergo karyotype analysis. Recurrence risk, reproductive decisions, and obstetrical management may be altered if a fetus has a demonstrated chromosomal aneuploidy. Babcook and coworkers retrospectively reviewed sonograms for 63 fetuses with sonographically detected spina bifida and correlated the results with subsequent autopsy or clinical findings. Of fetuses with sonographically isolated spina bifida, 22% had chromosomal aneuploidy. Although this is a small cohort, cytogenetic analysis remains a justifiable method by which to fully evaluate an affected fetus for appropriate recurrence risk counseling.12
Several teratogens have been implicated in the cause of NTDs. Two anticonvulsant medications in current use, carbamazepine and valproic acid, have been demonstrated to cause these defects. Robert and Guibaud13 originally reported an association between valproic acid and NTDs, noting a 1% risk for NTDs in patients taking this medication. This observation has been substantiated in several animal models.14, 15, 16 Carbamazepine also is associated with a 1% risk of spina bifida.17 Isotretinoin, an FDA approved oral vitamin an isomer used in the treatment of severe, recalcitrant nodular and cystic acne is associated with a high incidence of spontaneous abortion and major malformations. Congenital defects include hemifacial microsomia, central nervous system malformations including neural tube defects and hydrocephalus, and severe cardiovascular anomalies.18 The critical period of exposure is believed to be 14–35 days postconception with approximately a 25% incidence of a major malformation with exposure to the drug during the first 20 weeks of gestation.19 Although there is no debate regarding its teratogenicity, its unique efficacy and relatively short treatment course of about 15–20 weeks warrants its continued use as dermatologic therapy in specific situations. Therefore, the FDA now regulates the use of oral isotretinoin by a computer based risk management program to ensure restricted distribution and usage.20 The use of topical isotretinoin preparations is not associated with congenital malformations.21
Children of mothers with insulin-dependent diabetes mellitus have a 1–2% risk of NTD and a twofold to threefold (4–9%) increased incidence of congenital malformations compared with the general population.22 Although glycemic control may not be the sole etiologic factor in malformations in infants of diabetic women, careful preconceptional control is believed to decrease the prevalence of NTDs and other anomalies in these patients. The most common causes of NTDs are listed in Table 2.
Table 2. Causes of neural tube defects
Multifactorial inheritance
Single-gene (autosomal recessive) disorders
Meckel syndrome (most common)
Robert syndrome
Jarcho-Levin syndrome
Median facial cleft syndrome
HARDE (Walker-Warburg) syndrome
Oculo-auriculo-vertebral (Goldenhar) syndrome
Chromosomal aneuploidy
Trisomy 18
Trisomy 13
Trisomy 21
Triploidy
Unbalanced translocations, markers, ring chromosomes
Teratogens
Valproic acid
Carbamazepine
Aminopterin
Thalidomide
Oral isotretinoin
Amniotic band sequence
Cloacal extrophy
Sacrococcygeal teratoma
Maternal insulin-dependent diabetes mellitus
PERICONCEPTIONAL FOLIC ACID SUPPLEMENTATION
Epidemiologic observations such as geographic and seasonal variation, as well as an association with socioeconomic status, supported a hypothesis that dietary factors might play a role in the occurrence of NTDs. As early as 1965 work of Hibbard and Smithells suggested that folate might be an important dietary factor in the occurrence of NTDs.23 By the 1980s observational trials and one double-blind randomized controlled trial using high dose folic acid (4 mg daily) appeared to confirm this hypothesis. In 1991 Wald and colleagues published results of the British Medical Research Council (MRC) Vitamin Study, a randomized controlled trial showing that administration of 4 mg daily of folic acid for 3 months prior to conception and during early fetal development resulted in a 72% reduction of NTDs in women with a prior NTD pregnancy.24 This landmark study used four arms to demonstrate the effect of folic acid and excluded an effect of the concomitant administration of multivitamins or placebo. The relatively high dose of folic acid was selected because of the earlier experience and the desire to avoid a negative result with a lower dose. The lowest effective dose and the shortest duration of treatment prior to conception have not been defined and it is unlikely that definitive studies to determine these limits will ever be conducted. It was subsequently demonstrated by others that a multivitamin with trace elements plus 0.8 mg folic acid compared to a supplement containing trace elements and vitamin C prevented a significant portion of first occurrence of NTDs.25
Folic acid is important in transfer and exchange of methyl groups. As such, it is a substrate for the methionine synthase reaction which converts homocysteine to methionine. The production of methionine is important for protein synthesis. One-carbon transfer is also essential to a number of intracellular processes including the synthesis of the purine and pyrimidine building blocks of DNA and RNA. Thus, the relationship of folic acid deficiency to embryopathy is quite plausible. Deficiency of folic acid is marked by microcytic anemia and mild elevation of homocysteine. An elevation of homocysteine has been implicated in thrombogenesis and atherogenesis, and treatment with folic acid reduces the homocysteine elevation. While some portion of the prevention of NTDs by folic acid may relate to dietary deficiency, it is believed that an important effect is compensation for a genetically determined metabolic defect in homocysteine metabolism, e.g., due to MTHFR mutation. These observations are consistent with the epidemiologic observations as well as the familial recurrence patterns. Thus, approximately 70% of isolated open neural tube defects are considered “folate dependent” while the remaining 30% remain unexplained.
Food folate, in contrast to folic acid, is inconsistently absorbed due to attachment of polyglutamated side chains of variable length. Due to greater bioavailability and ease of compliance with recommended intake, supplementation with the synthetic form of folic acid rather than dietary intervention is a more efficacious approach for prevention neural tube defects. As a result, the US Public Health Service recommended in 1992 that all women of child-bearing age consume at least 400 μg of synthetic folic acid daily in addition to eating a folate-rich diet.26 In spite of efforts to educate women and the providers who care for them about these recommendations, fewer than half of the women of reproductive age adhere to the recommendations. Attempts to specifically target women who will become pregnant are hampered by the high rate of unintended pregnancies in the United States.
In 1996 the US FDA considered folic acid enrichment of all cereal and grain products in the United States. This generated substantial debate as potential risks of such a broad sweeping program were considered. A major concern was the impact on elderly patients, particularly those with vitamin B12 deficiency. Ultimately, the FDA mandated fortification by January 1998 at a level of 140 μg/100 g of flour.27 This is a level of fortification below what is needed to maximize prevention of neural tube defects in the majority of reproductive aged women. Since the implementation of the fortification at the level of 140 μ/100g , the prevalence of neural tube defects has decreased by 27%.28 A greater reduction in neural tube defects has been observed in several other countries, e.g., Chile, which fortified at a higher level and where women consume more fortified grain products.29 Thus, there is reason for renewed debate about increasing the level of fortification. It has been estimated that a 50% reduction in prevalence is obtainable with additional supplementation. Despite hypothetical risks of fortification no adverse effects have been observed and a comprehensive critical review favors increasing the level of fortification to achieve more effective prevention.30
Issues such as the potential benefit of additional vitamin B12 supplementation particularly in women who are strict vegetarians and a reduction in other birth defects continue to be studied. Likewise, the benefits of folic acid with regard to reduction of adult cardiovascular disease and prevention and treatment of the elderly with and without dementia are areas of interest.31 In the mean time, the recommendation in the United States remains unchanged, i.e., that during the reproductive years, women should take 400 μg (0.4 mg) of synthetic folic acid daily and consume a diet rich in folate. Women in high risk categories should take 4 mg of synthetic folic acid daily for 3 months prior to conception and during early fetal development. The effective use of folic acid for the prevention of a large portion of neural tube defects has been a major advance in the health care of women and children.
SCREENING AND DIAGNOSIS OF NEURAL TUBE DEFECTS
Both ultrasound and MSAFP screening can identify neural tube defects. Ultrasound can visualize the lesion, while MSAFP levels, if elevated, will place the patient in a high risk group to justify a detailed fetal ultrasound survey and/or amniocentesis to confirm the diagnosis. Screening decreases morbidity and mortality by promoting access to earlier diagnosis, enabling families to make informed reproductive choices, and designing appropriate strategies for prenatal care and delivery.
Screening and diagnostic testing
Since its introduction into obstetric practice, MSAFP during the early second trimester remains the most important biochemical marker for open fetal defects. MSAFP is also a component in the biochemical screening for fetal aneuploidy as well as adverse gestational outcome. It is important to note that not all screening or diagnostic strategies for aneuploidy include second trimester measurement of MSAFP. Any screening protocol that includes second trimester blood testing, such as a quad screen, integrated screen, or sequential screen, includes measurement of MSAFP and a risk assessment for open fetal defects. On the other hand, patients who decline aneuploidy screening or who choose only to undergo first trimester screening or who opt for chorioic villus sampling (CVS) do not have biochemical screening for open fetal defects unless a second trimester MSAFP is also performed. Since second trimester MSAFP and ultrasound are independent screening methods, both can be used to assess an individual patient's risk. The combination of these two independent screening methods, each with high sensitivity, result in a powerful approach to screening. Given the high sensitivity of second trimester ultrasound of intracranial and spinal anatomy for detection of spina bifida some physicians forego offering second trimester MSAFP to patients who do not have this performed as part of the aneuploidy risk assessment or diagnsosis. The rationale for such an approach is that when the defect cannot be seen with ultrasound the clinical implications are more difficult to estimate. The decision to forego offering second trimester MSAFP to these patients is generally based on experience of the sonographer, and the quality of the ultrasound evaluation of the individual patient.
ALPHA-FETOPROTEIN: BIOLOGIC PROPERTIES
Normal production of alpha-fetoprotein (AFP) is unique to fetal development, making it an ideal marker for early fetal evaluation. AFP was first isolated in 1956 by Bergstrand and Czar.32 Its name reflects its location on protein electrophoresis (in the a1 region between albumin and a1-globulin) and its fetal origin. It is structurally and functionally related to albumin. Genes for both proteins originate on chromosome 4,33 and both proteins have a molecular mass of 69,000 daltons.
Several functions have been postulated for AFP. Like albumin, it may be an intravascular transport protein and may play a role in maintaining oncotic pressure. An immunosuppressive effect of AFP has also been suggested as a mechanism for protecting paternally derived antigens in the fetus against maternal antibodies. However, because there are reported cases of congenital deficiency of AFP resulting in normal newborns34 the actual function of AFP remains speculative.
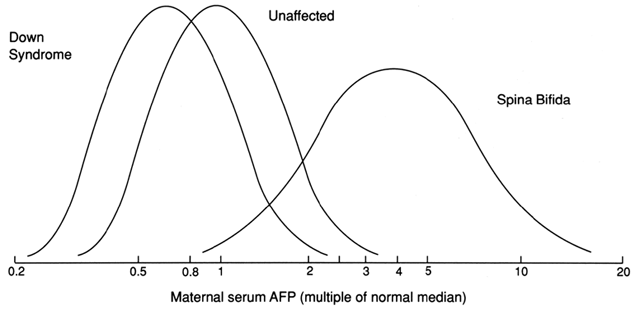
AFP is produced sequentially by the fetal yolk sac, gastrointestinal tract, and liver. It reaches a peak concentration in fetal serum of approximately 300 mg/dl by the end of the first trimester.35 The fetal liver produces a constant amount of AFP through the 30th week of gestation, although levels in the fetal blood decrease as the pregnancy advances. This is best explained by a dilutional effect in the enlarging fetal intravascular compartment. After 30 weeks' gestation, fetal AFP production declines precipitously. The log gaussian distribution of MSAFP levels for fetuses with spina bifida and fetal Down syndrome is noted in Figure 3.
|
ALPHA-FETOPROTEIN LEVELS
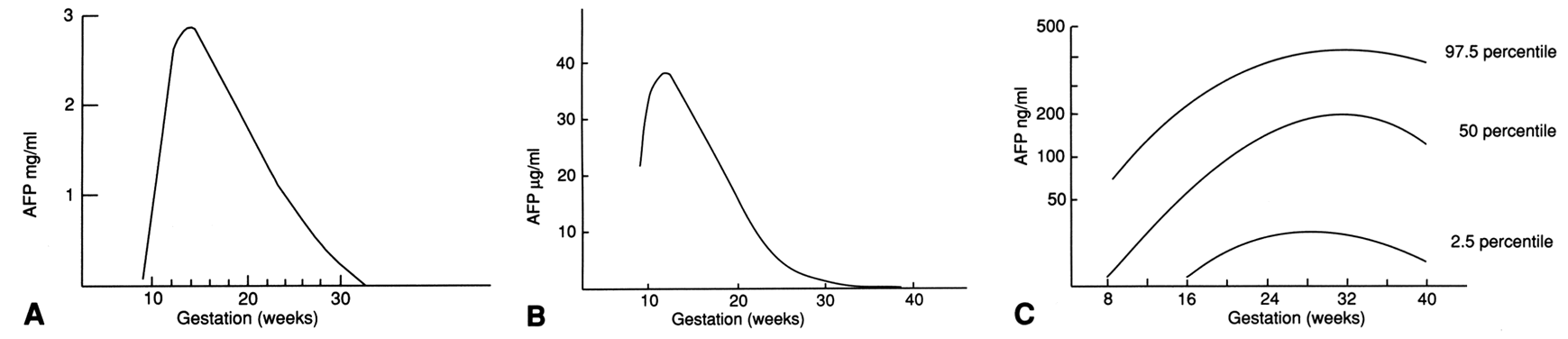
In the maternal circulation, AFP levels rise until the 30th gestational week. Thereafter, levels decline until term and drop precipitously after delivery. During the second trimester, maternal serum AFP levels increase, while fetal serum levels decline. This paradox is not completely understood, but it may result from the enlarging placenta allowing a greater capacity for diffusion of AFP or changes in the permeability of the placenta to AFP. The mechanism for transfer of AFP to the maternal circulation is transplacental (two thirds) and transamniotic (one third).36 A comparison of AFP levels in the maternal and fetal compartments is shown in Figure 4.37
AFP is also found in high concentrations in amniotic fluid. The decrease in amniotic fluid AFP through the second and third trimester closely parallels the decrease in AFP in fetal blood. A small proportion of AFP enters the amniotic fluid after filtration of the fetal blood through the kidney. As the fetus swallows amniotic fluid, AFP is destroyed by gastrointestinal proteolytic enzymes. AFP concentration in amniotic fluid is approproximately 150 times less than that in fetal serum.
In 1972, Brock and Sutcliffe measured AFP in the amniotic fluid of 31 pregnancies with anencephaly and six pregnancies with spina bifida, hydrocephaly, or both conditions.38 All of the cases of anencephaly and most of the spina bifida cases before 30 weeks' gestation demonstrated amniotic fluid AFP levels that were markedly elevated during pregnancy. When the fetus has an open (not skin covered) NTD, AFP leaks from the fetal circulation into the amniotic fluid. In 1974, Wald and coworkers performed a case-controlled study comparing maternal serum AFP levels in seven pregnancies with open NTDs with 14 control pregnancies matched for maternal age, parity, and gestational age.38 Maternal serum AFP levels in the affected pregnancies were significantly higher than those of the control population. This led to the hypothesis that there would be a role for measuring MSAFP in screening for NTDs. The UK Collaborative study demonstrated the utility of this test for prospective open NTD screening in 1977.39
In anencephaly, the malformed skull is not completely covered by overlying skin, and it is therefore the lesion most accurately detected with MSAFP screening. More than 90% of anencephaly cases can be detected by MSAFP screening, and 99% can be detected by ultrasound examination. Approximately 99% of anencephaly cases can also be detected by amniotic fluid AFP and acetylcholinesterase (AChE) testing. In contrast, most encephaloceles are skin covered and therefore are less likely to be identified by MSAFP screening or amniocentesis and are most often detected by ultrasound. Spina bifida and anencephaly occur with equal frequency. Approximately 80% of spinal cord defects are open – the tissue overlying the defect is not skin covered. The remainder of spinal cord defects are covered by skin or by a thick membrane and are not detectable by screening.
In general, MSAFP screening programs detect approximately 85% of open fetal NTDs: 80% of open spina bifida and 90% of anencephaly. Almost all of these open lesions can then be diagnosed by amniotic fluid testing. The object of any screening program is to maximize detection at an acceptable false-positive rate. A screening test cutoff point is a balance between these two factors. The correct MoM value for MSAFP can only be calculated after all the appropriate information regarding the patient is taken into account. This includes weight (at the time the blood sample was obtained), gestational age, and race, and considers whether the patient has insulin-dependent diabetes mellitus. An MSAFP level is considered elevated if the value is greater than 2.0 or 2.5 times the median value (2.0 or 2.5 MoMs) for normal controls at the same week of gestation.
Consider the hypothetical example given with the protocol in Figure 5. A cohort of 10,000 consecutive women present for MSAFP screening with a level of risk comparable to that of the US population. About 10–15 of these pregnancies would be affected with an NTD. MSAFP screening would detect 8–10 of these defects. At a cutoff of 2.0 MoMs, the false positive rate for this test of 4%, but a screen positive test result would only imply a 3% risk of having a child affected with an open NTD. A positive screening test result increases these patients' risk from 1.5 per 1000 to 3 per 100. Conversely, 97% of pregnancies with a postive screening test result are unaffected. If a screening cutoff of 2.5 MoM is used, the false positive rate is about 2%.40
|
MSAFP screening is most accurate when performed between 16 and 18 weeks' gestation, but testing can be performed between 15 and 22 weeks. Screening earlier or later than the optimal gestational age decreases the sensitivity of the test. Screening should be voluntary and should be performed after the patient has been fully informed regarding the benefits and limitations of the test. The patient should understand that a normal MSAFP result does not ensure a child without an abnormality (including an NTD), and that an elevated MSAFP level does not specifically diagnose an abnormality. Instead, an elevated value places the patient in a high-risk group that necessitates further evaluation. The most common causes of false-positive and false-negative MSAFP results are listed in Table 3.
Table 3. Common causes of false-positive and false-negative maternal serum alpha-fetoprotein levels
False-Positive Levels
Inaccurate gestational dating (patient has a more advanced gestation than estimated)
Multiple gestation
Race (black patients have higher levels than white patients)
Underweight patients (less than 90 pounds)
Spontaneous fetal to maternal bleeding
False-Negative Levels
Inaccurate gestational dating (patient has less advanced gestation than estimated)
Maternal insulin-dependent diabetes mellitus
Obesity
AMNIOTIC FLUID ALPHAFETOPROTEIN AND ACETYLCHOLINESTERASE
Amniocentesis is often used to differentiate the disorders responsible for a maternal serum AFP elevation. If there is an amniotic fluid AFP elevation, a secondary test for the presence or absence of the acetylcholinesterase (AChE) enzyme by gel electrophoresis is performed on the fluid. AChE is not normally identified in amniotic fluid. Tissues containing AChE are red blood cells, muscle, and neural tissue. Concentrations of AChE are much higher in fetal cerebrospinal fluid than in fetal serum. If the fetus has an open NTD, amniotic fluid AFP and AChE are usually both elevated and the high concentration of AChE in cerebrospinal fluid transudates across the defect into the amniotic fluid. AChE is a sensitive test for confirming an open NTD.
Fetal blood contamination is the most common source of falsely elevated AFP levels in amniotic fluid, and the amniocentesis performed to obtain the sample is the most common cause of fetal blood in the fluid. In such cases, amniotic fluid AFP is usually in the 3–5 standard deviation range. AChE is not detected in 90% of cases because of the relatively low AChE concentrations in the fetal blood. In congenital (Finnish) nephrosis, a rare autosomal recessive disorder, amniotic fluid AFP levels may be very high, and AChE is not identified.
At the time of amniocentesis for elevated MSAFP, karyotype analysis should also be performed regardless of the amniotic fluid AFP result. Omphaloceles and NTDs are both associated with chromosomal aneuploidy. Even when the amniotic fluid AFP level is normal, the addition of chromosome analysis allows more informative counseling regarding perinatal outcome.
ULTRASOUND
Despite the implementation of newer techniques, such as first trimester endovaginal sonography as well as three dimensional imaging, the diagnostic accuracy of detecting neural tube defects is dependent on the time allotted, the quality of the equipment, the ability to obtain adequate images, and the experience of the sonologist. The detection of anencephaly is reported to be 100% at midgestation.41 With regard to identification of neural tube defects, assessment of the intracranial structures aids the diagnosis of the NTD.
Evaluation of the cranial structures through two images of the transverse sonographic planes yield all relevant anatomic details for the diagnosis of malformations. This includes the superior transventricular plane through the frontal horn, cavum septum pellucidi, and lateral ventricular atria. The second, more inferior view is through the transcerebellar plane, through the thalamus, cerebellum, and cisterna magna.
In almost all cases of neural tube defects, an Arnold-Chiari malformation can be identified, defined as displacement of the cerebellar vermis, fourth ventricle, and medulla through the formen magnum. The term “banana sign” describes the elongated (as opposed to dumbbell) shape of the cerebellum. The “lemon sign” describes in utero frontal bossing, however, the lemon sign can also be identified in 1–2 % of normal fetuses, and sometimes can be caused by significant pressure during scanning (Fig. 6). A variable degree of lateral ventricular atrial enlargement can also be identified in the midtrimester. The sensitivity of cranial signs in detection of spina bifida approaches 99%.42
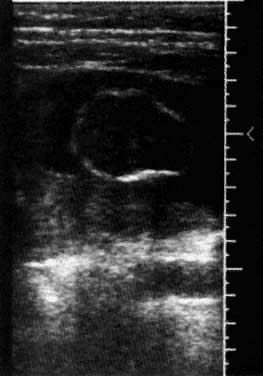 Fig. 6. Biparietal diameter with the lemon sign at 15 weeks' gestation.
Fig. 6. Biparietal diameter with the lemon sign at 15 weeks' gestation.
Budorick and colleagues offer a comprehensive review of the technique of fetal spine imaging.43 In brief, sonography depends on identification of the three ossification centers with the fetal vertebrae. Three imaging planes are used to identify the fetal spine: transverse plane, in which the ossification centers have to be identified, the parasagittal and coronal views. The spine must be imaged completely from the cervical to the sacral region.
Three dimensional imaging can be a powerful complementary adjunct to two dimensional imaging. There may be better localization of the lesion with three dimensional imaging, since both the axial and coronal images can be stored simultaneously and produce a rendered image of the fetal vertebrae. Some current limitations of three dimensional imaging include the additional time it takes to achieve accurate imaging, as well as the amniotic fluid interface necessary to capture and render a three dimensional image.
Current detection of neural tube defects with experienced sonographers and knowledge of MSAFP level should be greater than 90%. In patients at elevated risk for open fetal defects, Lennon and Gray44 reported a detection rate for spina bifida by ultrasound of 97% with 100% neonatal ascertainment. However, these data may be limited to their own site and their improved detection may even be affected by the knowledge that this study was being performed as well as the fact that the patients presented at high risk for this disorder. Caution should be used with regard to interpreting this type of ascertainment in general since equipment and ability are so varied. Further, these data cannot be extrapolated to low risk centers in low risk patients undergoing routine sonographic screening evaluations. In the RADIUS trial, when low risk ultrasound was performed with MSAFP screening, the detection rate was about 80%.45
How should MSAFP screening be used in patients undergoing other forms of screening and diagnostic tests?
Both MSAFP results and ultrasound evaluations in pregnancy are screening tests: that is, they place women in lower or higher risks groups for the detection of open fetal defects. Ultrasound can be diagnostic, but ultrasound examinations have the limitations of the training of the sonographers and quality of the equipment. Therefore, the combination of MSAFP screening with ultrasound is the most powerful combination for detection of neural tube defects: each screens by a different method. As noted above, patients who decline aneuploidy screening, and those who have only first trimester screening or diagnosis with CVS may also be offered second trimester MSAFP screening in addition to second trimester sonographic evaluation. In this situation MSAFP should be ordered as an individual analyte measurement to avoid obtaining unwanted or confusing information.
Given that there is a significant association between neural tube defects and chromosomal aneuploidy, we believe that offering a fetal karyotype to a patient with a fetal NTD is warranted. Approximately 6–16% of isolated appearing NTDs are associated with aneuploidy, these are most often trisomies, triploidy and chromosomal deletions.46, 47, 48 Knowledge of the etiology of the lesion profoundly affects recurrence rates for a family. A fetus with a trisomy will yield a 1% recurrence risk for future conceptions. Further, fetal autopsy, to evaluate the fetus for single gene disorders with a recurrence risk for the family at 25% is essential. Other abnormalities identified by the AFP screening process are shown in Table 4.
Table 4. Other abnormalities identified by the alpha-fetoprotein screening process
Ventral wall defects
Omphalocele
Gastroschisis
Triploidy
Trisomies: 18, 13, 21
Unbalanced translocations
Amniotic band sequence
Pentalogy of Cantrell: omphalocele, lower sternal defect, deficiency of diaphragmatic pericardium, intracardiac abnormality, anterior diaphragm defect
Renal agenesis
Fetal demise
Multiple gestation
Congenital nephrosis (Finnish type)
Sacrococcygeal teratoma
Dermatologic disorders
Epidermolysis bullosa
Congenital icthyosiform erythroderma
Chorioangioma
Maternal hepatoma
Maternal ovarian teratoma
MANAGEMENT COUNSELING REGARDING MORBIDITY AND MORTALITY
Thorough counseling of patients who have an NTD identified in an ongoing pregnancy is essential. Because anencephaly is uniformly fatal, the most important aspect of counseling is identifying the cause for the purpose of accurate recurrence risk counseling and preparation of the parents for the loss of their child at or shortly after birth. In a review of 181 liveborn infants with anencephaly, 40% were alive at 24 hours of age, and 5% lived to 1 week of age.49 Encephalocele, although a closed lesion, is a serious condition with a mortality rate of 60–75% during the first year.
The disabilities among survivors with spina bifida are accounted for by the location and extent of the lesion and the presence or absence of hydrocephaly. In general, because neural function is interrupted distal to the lesion, the higher the lesion, the greater is the neurologic deficit. If a patient survives with an NTD, the major morbidities include developmental delay and the ability to ambulate and maintain continence. Eventual outcome for the child varies with perinatal management and availability of support services.
Althouse and Wald evaluated an unselected series of 213 patients born in the UK with spina bifida (including encephaloceles) between 1965 and 1972.50 Their data reflect the natural history of these lesions before the advent of MSAFP screening. The 5-year survival rate for all patients was 36% for those with open lesions, 60% for those with closed lesions, and 18% for those with lesions that could not be classified. Closed cranial lesions (i.e., occipital meningomyelocele or encephalocele) were more commonly associated with severe handicap (75%) than were closed spinal lesions (23%).
Bamforth and Baird performed a population based study of patients with both spina bifida and hydrocephalus and compared life expectancy between the cases, which was ascertained from 1962 to 1970 and compared with the group from 1970 to 1986.51 At least 60% of patients had serious disabilities. These included a cerebrospinal fluid shunt (28%), neurogenic bladder (23%), congenital hip dislocation (23%), talipes equinovarus (23%), spasticity (15%), urinary obstruction (5%), scoliosis (3%), developmental delay (6%), seizures (2%), and blindness (1%). The group of patients ascertained between 1970 and 1986 had a dramatic improvement in the probability of survival to the first birthday. There was no difference in survival between the two cohorts between the ages of 7 and 16 years.
The best outcomes were reported by Hunt.52 Between 1963 and 1971, 117 consecutive infants with open spina bifida were followed to their 16th birthday. All had surgical repair within 48 hours of life. The overall survival rate was 60%. Fifty per cent of patients could ambulate more than 50 yards, 25% of patients were continent, and 70% of patients had an IQ of more than 80. If the lesion was at L3 or below, 75% of patients survived. Of the survivors, 90% of patients could ambulate more than 50 yards, 45% were continent, and 80% of patients had an IQ higher than 80.
FETAL SURGERY FOR MENINGOMYELOCELE
The survival rate of fetuses with an NTD has increased due to the multidisciplinary team approach with delivery at a tertiary care center.53 However, due to the significant sequelae of these lesions, the mean longevity of these patients is reduced to less than 40 years of age, with significant compromises to their quality of life.54 The standard management of these defects is by neonatal surgical repair, including a primary closure of the defect and often a ventriculoperitoneal shunt placement for hydrocephalus. Approximately 14% of the newborns do not survive beyond age 5 years.54 At least 45% of these children suffer complications from the ventriculoperitoneal shunt placements within the first year of repair.55
Evidence in other species supports the implementation of in utero fetal surgery to repair a meningomyelocele (MMC). Cultured rat spinal cords, when exposed to human amniotic fluid at differing gestational ages, demonstrate that, after 34 weeks' gestation, the amniotic fluid is toxic to the exposed fetal cells.56 Various methods of intrauterine repair of NTDs have been performed in various species, including rat, mice, rabbit, sheep, pig, and monkeys.
Meuli and coworkers surgically created MMC in fetal sheep.57, 58 Three sheep underwent surgical laminectomy at 75 days' gestation. At 100 days' gestation, they underwent in utero surgical repair using a latissmus dorsi flap. At birth, the sheep demonstrated continence, intact sensation, and significant motor improvement over the control subjects who underwent laminectomy without repair. The controls had the predicted motor and sensory dysfunction and incontinence. Paek and colleagues recently demonstrated hindbrain herniation in sheep with surgically created MMC. At 75 days' gestation, 20 sheep underwent surgical creation of MMC. Of the sheep that survived repair at 100 days' gestation, none demonstrated hindbrain herniation, defined as displacement of the cerebellar vermis and medulla through the foramen magnum.59
Concerns about these surgically constructed animal models for MMC are related to the later development of these disorders that is not analogous to congenital fetal development of these lesions. Therefore, outcome for these animal models may not reflect outcome for an in utero repair of a naturally occurring lesion. However, since human spinal cord myelination begins at about 15 weeks' gestation, early closure of an MMC might allow for more spinal cord regeneration, resulting in better long term outcomes.60 Further, observed deficits in offspring with MMC are generally milder if the defect is protected from amniotic fluid with either skin covering or adipose tissue.
In 1997, Bruner and colleagues reported the first endoscopic repair of an MMC by intrauterine approach.61 They performed the first in utero repair in 1994.62 They compared their first four fetoscopic repairs with four open fetal procedures, all performed at a mean gestational age of 28+ weeks. Both groups had complications, and, of the survivors, the level of neurologic impairment was not improved by either technique. In 1998, Adzick and colleagues reported the first open fetal repair of an MMC at the Children’s Hospital of Philadelphia.63 This fetus had an MMC from the eleventh thoracic level to the sacral region. After open repair at 23 weeks' gestation, the neurologic function of the newborn correlated with L5 on the left and L4 on the right, and there was no evidence of an Arnold-Chiari malformation or hydrocephalus.
Further procedures have not yielded such a dramatic improvement in neonatal outcome.64 In order to compare outcomes from in utero procedures with standard neonatal management outcomes, a retrospective review of 297 patients managed at the Children’s Hospital of Philadelphia was undertaken.65 In this series, the overall rate of ventricular shunting was 81%. In 86% of patients, the functional level of the lesion was found to be equal or higher than the radiologic lesion. In a combined series of 104 patients from Vanderbilt and CHOP who underwent intrauterine MMC closure, the overall rate of shunting decreased to 44%.66 With regard to neurologic function, 15 of 34 neonates with in utero repair at CHOP had an improvement in function at least two spinal levels higher than predicted.67 Unfortunately, this improvement in neurologic function is not necessarily maintained.
Further, there are risks to both mother and fetus from fetal surgery. Open fetal surgery is performed by accessing the fetus through an incision at the uterine fundus, essentially causing a premature classical incision on the uterus. To date, no reported maternal deaths have been reported from this type of surgery.
Given the evidence, the NICHD introduced the MoMS trial in 2003 as an unblended, randomized controlled trial at three United States Centers to evaluate outcomes from in utero versus neonatal surgery for spina bifida. Enrollment information can be obtained from the NIH sponsored website: www.spinabifidamoms.com. The goal is enrollment of 200 patients; currently about 140 patients have been enrolled, extending this study about 2 more years (personal communication, Catherine Spong). Patients diagnosed with an MMC between 16 and 26 weeks will be randomized to one of three centers (Children's Hospital of Philadelphia, Vanderbilt University, or the University of California, San Francisco) and will be randomized to one of two management protocols. This includes either intrauterine repair between 18 and 25 weeks with delivery by cesarean section at 37 weeks' gestation, versus management by local maternal fetal medicine team, with referral for a 37 week cesarean delivery at one of the three centers with neonatal repair. The primary study endpoints include need for shunt placement and fetal and infant mortality. Secondary endpoints include neurologic function, cognitive outcome, and maternal morbidity.
In utero fetal surgery requires a multidisciplinary team approach.68 Briefly, the surgical procedure for an in utero spina bifida repair includes an upper segment maternal hysterotomy with care to avoid the placenta. The hysterotomy is stabilized with a uterine stapler to achieve hemostasis. Continuous perfusion of the cavity with Ringers lactate and fetal cardiac sonography often by pulse oximetry. The fetus is not removed from the cavity, but turned to expose the MMC. A dural fascial closure is performed and often dermis graft material may be used to cover the closure. Postpartum management includes multiple tocolytics, with elective delivery by cesarean section at 36 weeks' gestation following amniocentesis for pulmonary maturity. The major risk to this procedure is preterm delivery due to uncontrollable preterm labor.
MODE OF DELIVERY FOR PATIENTS CARRYING FETUSES WITH NEURAL TUBE DEFECTS
There is no conclusive evidence regarding the most appropriate route of delivery for a fetus with an NTD. Cesarean delivery should be considered for appropriate maternal indications, maternal request after counseling, hydrocephalus precluding vaginal delivery, breech presentation, and large fetal lesions. One review of routes of delivery for fetuses with all types of structural anomalies uses the cut off of a lesion measuring 6 cm as a size in which cesarean delivery is justified to decrease the risk of disruption.69 Of note, participants in the MoMs trial undergo cesarean delivery for both the in utero fetal surgery cohort as well as the neonatal surgical group to control for delivery route to better evaluate the timing of the repair.
In 1984, Chervenak and colleagues first advocated the use of cesarean delivery to avoid fetal trauma, maintain an aseptic environment, and have more convenient surgical repair for the newborn.70 While there are multiple small retrospective studies evaluating this issue, the largest series was conducted by Luthy and colleagues.71 Over a 10 year study period, they reviewed the antenatal and neonatal records of 200 cases of isolated MMC, accounting for 95% of the cases identified in Washington State between 1979 and 1988. Of these, 81 had an antenatal diagnosis, and 119 had a diagnosis made at delivery. A total of 160 infants survived for follow up in the neonatal period. Comparison groups included 47 infants delivered by cesarean delivery prior to labor, 35 delivered by cesarean section after labor, and 78 with vaginal delivery. At 2 years of age, the motor level of paralysis was evaluated by physical therapists. When the motor level was subtracted from the level of the anatomic lesion, infants delivered by cesarean section without labor had a mean level of paralysis 3.3 segments below the anatomic lesions, as compared with infants delivered vaginally (at 1.1 segments below the lesion) or 0.9 segments for those undergoing cesarean delivery after labor. The authors concluded that cesarean delivery prior to labor may result in better long term motor function. The results of this retrospective study may, however, be attributed to selection bias, since the patients undergoing cesarean delivery were prenatally identified, compliant, and well evaluated. Patients who underwent vaginal delivery may have been noncompliant or may not have presented for antenatal care, perhaps affecting long term neonatal outcome as well.
In summary, given the lack of consensus regarding improved outcome with regard to mode of delivery, delivery management at this time should be individualized with a multidisplinary team. Consideration should be given to size of the lesion and biparietal diameter at term, maternal indications, and patients' desires after counseling.
CONCLUSION
Although preconceptional folic acid supplementation has decreased the prevalence of neural tube defects, they are still common birth defects for the obstetrician to screen, diagnosis, and manage in the pregnant patient. Counseling regarding folic acid supplementation is essential for all women of reproductive age. However, understanding the etiology of NTDs at the genetic and cellular level is limited by the ability to identify large kindreds with similar disorders to develop effective gene mapping. For the clinician, controversy with regard to the use of in utero fetal surgery to repair these defects should be resolved by the NIH sponsored randomized clinical trial in the next few years. The most appropriate mode of delivery for affected fetuses is also not clearly defined. Therefore, a multidisciplinary approach to management, involving the obstetrician as well as subspecialists, is essential to ensure the best outcome for the neonates and their families.
REFERENCES
Shaer CM, Chescheir, N, Erickson K, and Shulkin J. Obstetrician-Gynecologists’ Practice and Knowledge Regarding Spina Bifida. Am J Perinat 2006; 23(6): 355-362 |
|
Kibar Z, Capra V, Gros P. Toward understanding the genetic basis of neural tube defects. Clin Genet 2007; 71: 295-310 |
|
DeMarco P, Merello E, Macelli S, Capra V. Current perspectives on the genetic causes of neural tube defects. Neurogenetics 2006; 7: 201-221 |
|
Van AllenMI, Kalousek DK, ChernoffGF et al: Evidence for multisite closure of the neural tube in humans. Am J Med Genet 47: 723-743, 1993 |
|
Martinez-Frias ML, Urioste M, Bermejo E et al: Epidemiological analysis of Multi-Site Closure Failure of Neural Tube in Humans. Am J Med Genet; 66: 64-68, 1996 |
|
Leonard CO, Freeman JM: Spina bifida: A new disease. Pediatrics 68: 136, 1981 |
|
Osaka K, Tanimura T, Hirayama A et al: Meningomyelocele before birth. J Neurosurg 49: 711, 1978 |
|
Schut L, Pizza EJ, Bruce DA: Occult spinal dysraphism. In McLaurin RL (ed): Myocele. New York: Grune & Stratton, 1977 |
|
Folic Acid and Prevention of Spina Bifida and Anencephaly 10 Years After the U.S. Public Health Service Recommendation. MMWR September 13, 2002 / 51(RR13);9-11 |
|
Main DM, Mennuti MT: Neural tube defects: Issues in prenatal diagnosis and counselling. Obstet Gynecol 1: 67, 1986 |
|
Holmes LB, Driscoll SG, Atkins L: Etiologic heterogeneity of neural tube defects. N Engl J Med 294: 365, 1976 |
|
Babcook CJ, Goldstein RB, Filly RA. Prenatally detected fetal myelomeingocele: is karyotype analysis warranted? Radiology 1995; 194: 491-494 |
|
Robert E, Guibaud P: Maternal valproic acid and congenital neural tube defects. Lancet 2: 937, 1982 |
|
Bruckner A, Lee YJ, O'Shea KS, Henneberry RC: Teratogenic effects of valproic acid and diphenylhydantoin on mouse embryos in culture. Teratology 27: 29–42, 1983 |
|
Kao J, Brown NA, Schmid B et al: Teratogenicity of valproic acid: In vivo and in vitro investigations. Teratog Carcinog Mutagen 1: 367–376, 1981 |
|
Fabro S, Schull G, Brown NA: The relative teratogenic index and teratogenic potency: Proposed components of developmental toxicity risk assessment. Teratog Carcinog Mutagen 2: 61–76, 1982 |
|
Rosa FW: Spina bifida in infants of women treated with carbamazepine during pregnancy. N Engl J Med 324: 675–677, 1991 |
|
Rothman KJ, Moore LL, Singer MR et al: Teratogenicity of high vitamin A intake. N Engl J Med 1995; 333: 1369-1373. |
|
Lammer EJ, Chen DT, Hoar RM et al: Retinoic acid embryopathy. N Engl J Med 313; 837-841, 1985 |
|
www.ipledgeprogram.com |
|
Rothman KF, Pochi PE: Use of oral and topical agents for acne in pregnancy. J Am Acad Dermatol 19: 431-442, 1988. |
|
Mills JL, Knopp RH, Simpson Jl et al: Lack of relation of increased malformation rates in infants of diabetic mothers to glycemic control during organogenesis. N Engl J Med 318: 671-676, 1988. |
|
Eskes TKAB. From anemia to spina bifida – the story of folic acid. A tribute to Professor Richard Smithells. Eur J Obstet Gynecol Reprod Biol 2000; 90: 119-123 |
|
Wald N, Sneddon J, Densem J, Frost C, Stone R. Prevention of neural tube defects: Results of the Medical Research Council Vitamin Study. Lancet 1991; 338: 131-137 |
|
Czeizel AE, Dudas I. Prevention of the first occurrence of neural-tube defects by periconceptional vitamin supplementation. N Engl J Med 1992; 327: 1832-1835 |
|
Centers for Disease Control: Recommendations for the use of folic acid to reduce the number of cases of spina bifida and other neural tube defects. MMWR Morb Mortal Wkly Rep 1992; 41(no. RR-14):1-7 |
|
US Food and Drug Administration. Food standards: Amendments of standards of identity for enriched grain products to require addition of folic acid. Federal Register 1996; 61: 8781-8797 |
|
Centers for Disease Control and Prevention. Spina bifida and anencephaly before and after folic acid mandate–United States, 1995-1996 and 1999-2000. MMWR Morb Mortal Wkly Rep 2004; 53: 362-365 |
|
Hertrampf E. National food fortification program with folic acid in Chile. Technical Consultation on Folate and Vitamin B12 Deficiencies. World Health Organization, Geneva, October 2005 |
|
Johnston RB. Will increasing folic acid in fortified grain products further reduce neural tube defects without causing harm?: consideration of the evidence. Pediatr Res 2008; 63(1): 2-8 |
|
Malouf R, Grimley EJ. Folic acid with or without vitamin B12 for the prevention and treatment of healthy elderly and demented people. Cochrane Database Syst Rev 2008; (4): CD004514 |
|
Bergstrand CG, Czar B: Demonstration of a new protein fraction in serum from the human fetus. Scan J Clin Lab Invest 8: 174, 1956 |
|
Harper ME, Dugaiczyk A: Linkage of evolutionary-related serum albumin and alpha-fetoprotein genes within 911-22 of human chromosome 4. Am J Hum Genet 35: 565, 1983 |
|
Faucett WA, Greenberg F, Rose E et al: Congenital deficiency of alpha-fetoprotein (abstract). Am J Hum Genet 45: 1019A, 1989 |
|
Haddow JE, Palomaki G, Knight GJ et al: Prenatal screening for major fetal disorders. In Haddow JE (ed): Fetal Disorders Associated With Elevated MSAFP Levels, vol 1, p 4. Scarborough, ME: Foundation for Blood Research, 1990 |
|
Los FJ, Debruijn HWA, Van Beek Calkoen-Carpay T et al: AFP transport across the fetal membranes in the human. Prenat Diagn 5: 277, 1985 |
|
Habib A: Maternal serum alpha-fetoprotein: Its value in antenatal diagnosis of genetic disease and in obstetrical-gynecologic care. Acta Obstet Gynecol Scand Suppl 61: 14, 1977 |
|
Brock DJH and Sutcliffe RG: Alpha fetoprotein in the antenatal diagnosis of anencephaly and spina bifida. Lancet 2: 197, 1972 |
|
UK Collaborative Study on Alpha Fetoprotein in Relation to Neural Tube Defects: Maternal serum alpha-fetoprotein measurement in antenatal screening for anencephaly and spina bifida in early pregnancy. Lancet 2: 1323–1332, 1977 |
|
Haddow JE: Screening for spinal defects. Hosp Pract 17: 128–138, 1982 |
|
Pilu G, Perolo A, falco P et al: Ultrasound of the fetal central nervous system. Curr Opin Obstet Gynecol 12:9 3-103, 2000 |
|
Watson WJ, Cheschier NC, Katz VL et al: The role of ultrasound if the evaluation of patients with elevated maternal serum alpha fetoprotein: a review. Obstet Gynecol 1991; 78: 123-128 |
|
Budorick NE, Pretorius D, Nelson TR: Sonography of the Fetal Spine: Technique, Imaging Findings, and Clinical Implications. Am J Radiol 164(2): 421-8, 1995 |
|
Lennon CA,Gray DL. Sensitivity and specificity of ultrasound for the detection of neural tube and ventral wall defects in a high risk population. Obstet Gynecol 1999; 94: 562-566 |
|
Crane JP, Lefevre ML, Winborn RC et al. A randomized trial of prental sonographic screening: impact on the detection, management, and outcomes of anomalous fetuses. The RADIUS study group. Am J Obstet Gynecol 1994; 171: 392-399 |
|
Sepulveda W, Corral E, Ayala C et al. Chromosomal abnormalities in fetuses with open neural tube defects: prenatal identification with ultrasound. Ultrasound Obstet Gynecol 2004; 23: 352-356 |
|
Kennedy D, Chitayat D, Winsor EJT et al. Prenatally diagnosed neural tube defects:ultrasound, chromosome, and autopsy or postnatal findings in 212 cases. Am J Med Genet 1998; 7: 317-321 |
|
Drugan A, Johnson MP, Dvorin E et al. Aneuploidy with neural tube defects: another reason for complete evaluation in patients with suspected ultrasound anomalies or elevated maternal serum alpha fetal protein. Fetal Ther 1989; 4: 88-92. |
|
Baird PA, Sadovnick AD: Survival in infants with anencephaly. Clin Pediatr 23: 268, 1984 |
|
Althouse R, Wald N: Survival and handicap of infants with spina bifida. Arch Dis Child 55: 845–850, 1980 |
|
Bamforth SJ, Baird PA: Spina bifida and hydrocephalus: A population study over a 35 year period. Am J Hum Genet 44: 225–232, 1989 |
|
Hunt GM: Open spina bifida: Outcome for a complete cohort treated unselectively and followed into adulthood. Dev Med Child Neurol 32: 108–118, 1990 |
|
Hogge WA, Dungan JS, Brooks MP et al. Diagnosis and management of prenatally detected meningomyelocele: a preliminary report. Am J Obstet Gynecol 1990; 163: 1061-1064 |
|
Zambelli H, Carelli E, Honorato D et al. Assessment of neurosurgical outcome in children prenatally diagnosed with myelomeningocele and development of a protocol for fetal surgery to prevent hydrocephalus. Child Nerv Syst 2007; 23: 421-425 |
|
Caldarelli M, DiRocco C, LaMarca F. Shunt complications in the first postoperative year in children with myelomeningocele. Childs Nerv Syst 1996; 12: 748-754 |
|
Drewek MJ, Bruner JP, Whelsell WO et al. Quantitative analysis of the toxicity of the human amniotic fluid to cultured rat spinal cord. Pediatr Neurosurg. 1997; 27: 190-193 |
|
Meuli M, Meuli-Simmen C, Hutchins GM et al. In utero fetal Surgery rescues neurological function at birth in sheep with spina bifida. Nat Med 1995; 1: 342-347 |
|
Meuli M, Meuli-Simmon C, Yingling CD et al. In utero repair of experimental myelomeningocele saves neurological function at birth. J Pediatr Surg 1996; 31: 397-402 |
|
Paek BW, Farmer DL, Wilkenson CC et al. Hindbrain herniation develops in surgically created meningomyelocele but is absent after repair in fetal lambs. Am J Obstet Gynecol 2000; 183: 1119-1123 |
|
Wiedenheim KM, Epshteyn I, Rashbaum WK et al. Neuroanatomical localization of melin basic protein in the late first and early second trimester human feotal spinal cord and brainstem. J Neurol 1993; 22: 507-516 |
|
Bruner JP, Tulipan NE, Richards WO. Endoscopic coverage of fetal open minigomyelocele in utero. Am J Obstet Gynecol. 1997; 176: 256-257 |
|
Bruner JP, Tulipan NB, Richards WO et al. In utero repair of meningomyelocele: a comparison of endoscopy and hysteroscopy. Fetal Diagn Ther 2000; 15: 83-88 |
|
Adzick NS, Sutton LN, Crombleholme TM et al. Successful fetal surgery for spina bifida (letter). Lancet 1998; 52: 1675-1676 |
|
Sutton LN, Adzick NS, Bilaniuk LT et al. Improvement in hindbrain herniation demonstrated by serial fetal magnetic resonance imaging gellowing fetal surgery for meningomyelocele. JAMA. 1999; 282: 1819-1825 |
|
Rintoul N. A new look at meningomyleoceles: Functional level, vertebral level, shunting, and implications for fetal intervention. Pediatrics 109; 494-495, 2002 |
|
Tulipan N: The effect of intrauterine meningomyelocele repair on the incidence of shunt-dependent hydrocephalus. Pediatr Neurosurg 38; 27-33, 2003 |
|
Johnson M et al: Fetal meningomyelocele repair: Short term clinical outcomes. Am J Obstet Gynecol 2003; 189:482-487 |
|
Sutton LN. Fetal neurosurgery for myeleomeningocele. Child Nerv Syst 2003; 19: 587-591 |
|
Anteby EY, Yagel S: Route of delivery of fetuses with structural anomalies. Eur J Obstet Gynecol Reprod Biol 2003; 106; 5-9 |
|
Chervenak FA, Duncan C, Ment NR. Perinatal management of meningomyelocele. Obstet Gynecol 1984; 63: 376-80 |
|
Luthy DA, Wardinsky T, Shurtleff, DB et al. Cesarean section before the onset of labor and subsequent motor function in infants with meningomyelocele diagnosed antenatally. N Engl J Med 1991; 324: 662-6 |