Authors
INTRODUCTION
With the chapters in this volume that address specific contraceptive methods and issues, this introductory chapter provides an overview of the overall benefits of birth control, details contraceptive practices (particularly among US women), and concludes by comparing the efficacy, costs, and benefits of existing as well as emerging reversible contraceptives.
By reducing unintended pregnancies and abortions, and facilitating family planning/spacing of births, effective contraception provides both health and social benefits to mothers and their children. According to worldwide estimates, some 600,000 women die each year of pregnancy-related causes, and 75,000 die following unsafe abortions.1 At least 200,000 of these maternal deaths are attributable to the failure or lack of contraceptive services.2 In addition to preventing mortality, effective contraception improves maternal health. Data from the well-controlled Intergenerational Panel Study of Mothers and Children, a 31-year longitudinal survey of 1113 mother-child pairs, indicate that unwanted births can lead to nonpsychotic major depression (postpartum depression), feelings of powerlessness, increased time pressures, and a reduction in overall physical health.3 Finally, effective contraception improves the social and economic role of women and enables them to participate in society fully.4, 5
Infants and children also derive benefits from effective contraception. As modern contraceptive methods have become more widely available throughout the world, infant mortality has decreased from approximately 150 deaths per 1000 live births in the 1950s to 80 deaths per 1000 live births in the 1990s.4 In developing countries, 53% of married women plan family size, and 90% of them use modern birth control methods such as female sterilization, oral contraceptives (OCs), and intrauterine devices (IUDs).4 According to Population Action International, infant mortality in developing countries could be decreased by one third by increasing the spacing between births to 2–4 years.1 The health status of infants and children is also improved as the result of effective contraception. In the 31-year mother-child survey, unwanted children had more health problems, such as lower birth weight and higher mortality, than those who had been wanted.3 Mothers who had an unwanted birth also had a poorer quality relationship with all their children, tending to spank them more and spend less leisure time with them.3 In addition, evidence indicates that children from large families generally receive less education.1
| Major Events in Birth Control In The United States | ||||||||||||||||||||||||||||||||
| Key events in the availability of modern contraceptive in the United States are summarized in Table 1.4, 6 Although many refer to these events as the contraceptive revolution, Diczfalusy recently observed that "many scientists wonder whether or not contraception is still a revolution or rather a normal way of life—with significantly improved quality of life—for a billion couples".7 Condoms have been available for hundreds of years, yet most major advances in contraception have occurred since the 1960s and 1970s.6 OCs and IUDs were introduced in the early 1960s, and both had become highly popular methods of contraception by the 1970s, as use of the diaphragm and male condom waned.6, 8 However, the 1980s saw a dramatic decrease in IUD use as the result of concerns about intrauterine infections.4, 8 Today, only 0.8% of US women use IUDs compared with nearly 100 million women worldwide.6 Major changes occurred during the 1990s as condom use among adolescents increased, probably because of public health efforts to increase awareness about the risks of human immunodeficiency virus infection and other sexually transmitted diseases (STDs), and OC use decreased slightly.4, 9 Additionally, approval of levonorgestrel implants and the depot medroxyprogesterone acetate (DMPA) contraceptive injection provided methods that offered excellent protection in less user-dependent forms.6 In fact, the decline in teen pregnancies seen in the last decade has been attributed largely to increased use of DMPA.10 Table 1. Key events in availability of modern contraceptive methods in the United States
|
COMPARISON OF CONTRACEPTIVE EFFICACY, COSTS, AND BENEFITS
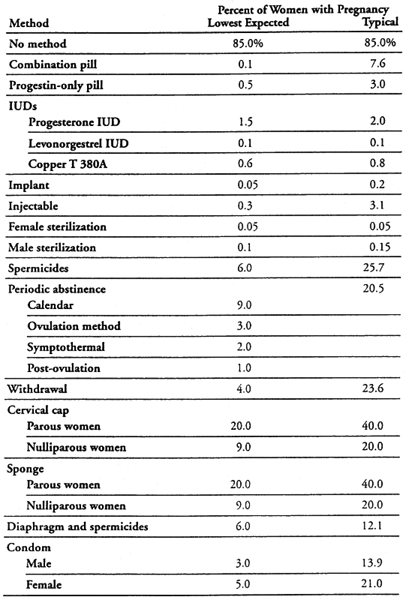
As shown in Fig. 1, contraceptive methods with high first-year failure rates during typical use are periodic abstinence, withdrawal, male condoms, diaphragms, and spermicides.11, 12 Highly effective methods with low first-year failure rates during typical use include copper or progesterone-bearing IUDs, OCs, implants, injectables, and sterilization.
The results of a recent 60-week, US multicenter, controlled, nonrandomized, parallel study in which 1103 women used either a monthly contraceptive injection containing MPA and estradiol cypionate (E2) (Lunelle, n = 782) or an OC-containing triphasic norethindrone (NET) and ethinyl estradiol (Ortho-Novum 7/7/7, n = 321) demonstrate the high effectiveness that can be achieved with reversible contraceptives.13 In this trial, one unintended pregnancy was reported at the third visit in a patient receiving the OC and no pregnancies occurred during 13 cycles of 28 days in study subjects receiving monthly injections. Pregnancy rate estimates using Pearl index and life-table methods were 0.0 and 0.0, respectively, with the monthly injection and 0.3 and 0.4, respectively, with the OC. Thus, both the monthly injections and the OC provided a high degree of contraceptive efficacy. Because this was a clinical trial, participants were highly motivated (and monitored). Accordingly, higher failure rates are observed in routine clinical practice. Increased use of these and other highly effective methods of contraception by US women would decrease rates of unintended pregnancy and induced abortion.
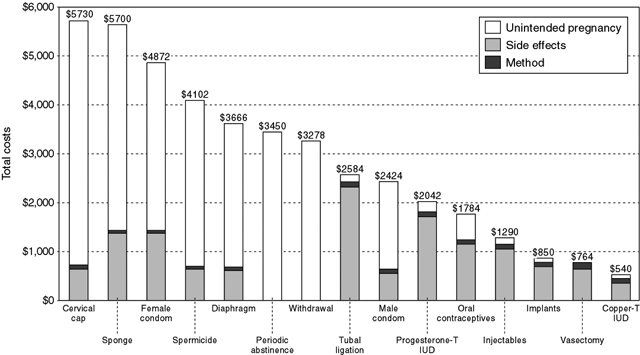
Effective methods of contraception are also highly cost-effective (Fig. 2).14 In an analysis in the managed care payment model, 5-year costs associated with reversible methods increase as the effectiveness of the method decreases; nearly all cost with less effective methods is related to unintended pregnancy rather than method acquisition.14 With the highest cost-effective reversible methods—copper-T IUD, implants, and injectables—method acquisition accounts for most of the cost. Costs of barrier methods are increased by unintended pregnancy. Among permanent methods of contraception, female sterilization is less cost effective than vasectomy as the result of the greater cost of tubal sterilization, including operating room and anesthesia requirements.
Characteristics of highly effective, reversible contraceptive methods are compared in Table 2. Several comments are warranted with regard to differences in benefits and risks associated with these methods. In terms of major risks, OCs are known to have procoagulant effects related to the estrogen component. Such procoagulant changes increase users' risk of deep vein thrombosis. Although procoagulant effects were most pronounced with high estrogen-dose OC formulations, mild procoagulant effects within the normal range have been reported with formulations containing 35 μg or less of estrogen.15 Unlike OCs, DMPA does not increase globulin production in the liver and is not associated with increases in procoagulant factors.16 No procoagulant changes are seen with either levonorgestrel implants or the copper IUD.16
Table 2. Comparison of highly effective, reversible contraceptive methods
Parameter | OC | DMPA | Implants | Copper Ultrauterine Device |
Efficacy | User dependent | High | High | High |
Length of protection | Continuous if taken daily | 3 months | 5 years | 10 years |
Rapid return of fertility | Yes | No | Yes | Yes |
Regular cycles | Yes | No | Variable | Yes |
Amenorrhea | Uncommon | Common | Variable | No |
Appropriate in nursing mothers | Suboptimal | Yes | Yes | Yes |
Procoagulant | Yes | No | No | No |
Noncontraceptive benefits | Established | Established | Unknown | No |
Provider required to initiate | Yes (Rx) | Yes | Yes | Yes |
Provider required to discontinue | No | No | Yes | Yes |
Privacy | Requires pill pack | Yes | Seen or felt by some users | Usually (string may be felt by partner) |
OC, oral contraceptives; DMPA, depot medroxyprogesterone acetate.
(Adapted from Kaunitz AM: Injectable contraception: New and existing options. Obstet Gynecol Clin North Am 27:741–780, 2000.)
Another concern with hormonal methods of contraception is their impact on bone mineral density (BMD). Several studies of OCs, DMPA, and levonorgestrel implants have examined changes in BMD. A history of OC use was found to be protective against low BMD in a US cross-sectional study.17 In a large Swedish case-control study, OC use by women age 40 and older was associated with a 25% reduction in postmenopausal hip fracture risk.18 Studies have found the OC use has a protective effect against osteopenia in young, reproductive-age women with hypoestrogenic conditions (e.g. hypothalamic amenorrhea or anorexia nervosa), and helps maintain BMD in older reproductive-age women with declining ovarian function.19 Available data suggest that use of levonorgestrel implants may have a neutral or beneficial effect on BMD.20
The impact of current or past use of DMPA on BMD has been addressed by 13 studies.16 Overall, current use of DMPA appears to be associated with a decrease in BMD that is reversible following cessation of use and therefore unlikely to have clinical importance. A New Zealand study found that postmenopausal bone mineral density in former DMPA users was not significantly different from that of never-users at any site.21 In this regard, the impact of DMPA on bone density resembles that of lactation in that both lower ovarian production of estradiol, leading to reversible declines in BMD.16
In contrast to implants and the copper IUD, both OCs and DMPA have many well-established noncontraceptive benefits. Both OCs and DMPA prevent iron-deficiency anemia, ectopic pregnancy, pelvic inflammatory disease, and endometrial cancer.22, 23 Additional noncontraceptive benefits of OCs include protection from dysmenorrhea and menorrhagia, ovarian cysts, benign breast disease, and ovarian cancers, emerging benefits such as the treatment of acne and dysfunctional uterine bleeding, and the prevention of osteopenia and osteoporotic fractures.18, 22, 24 An additional noncontraceptive benefit of DMPA is a reduced need for hysterectomy in women with uterine leiomyomata.23
Protection against STDs represents a critical issue for reproductive-age women. Because the trend toward initiating sexual activity at a younger age and postponing marriage until an older age places women at increased risk for both unintended pregnancy and STDs, clinicians should try to encourage use of contraceptive options that achieve both goals. However, as shown in Table 3, the most effective reversible contraceptive methods (DMPA, implants, IUDs, and OCs) do not protect users against STDs, whereas a method with relatively low contraceptive efficacy—the male condom—provides the greatest STD protection.25
Table 3. Protection against sexually transmitted diseases (STDs) with different contraceptive methods
Contraceptive Method | Effects on Bacterial STDs | Effects on Viral STDs |
Diaphragm, cervical cap, sponge | Some protection against cervical infection; increases organisms associated with bacterial vaginosis | No protection against vaginal infection or external genitalia transmission; prevention of HPV controversial |
Female condom | In vivo protection against recurrent trichomonal infection suggests possible protection against other STDs | In vitro impermeability to cytomegalovirus, HIV |
IUD | No protection | No protection |
Latex male condom | Protection against most pathogens in genital fluids | Less protection against organisms such as HSV and HPV transmitted from external genitalia |
Combination oral contraceptive | No protection against bacterial STDs | Data on HIV transmission risks conflicting; role regarding risk of HPV infection and cervical dysplasia unclear |
DMPA implants | Assume no protection | May promote HIV transmission |
Spermicide with nonoxynol-9 | Modest protection against cervical gonorrhea and chlamydia | Data conflicting on HIV transmission risks |
Tubal ligation | No protection | No protection |
HPV, human papillomavirus; HIV, human immune deficiency virus; IUD, intrauterine device. HSV, herpes simplex virus; DMPA, depot medroxyprogesterone acetate.
(Adapted from Cates W Jr, Sulak PJ: Contraceptives and STDs: Alternative approaches to providing dual protection. Dialog Contracept 6:1–4, 9, 2000.)
Providing the dual benefits of protection against pregnancy and STDs is a particularly vexing challenge among adolescents. Clinicians have noted that long-acting hormonal preparations such as DMPA or levonorgestrel represent better options than OCs for pregnancy prevention in this age-group because they remove need for daily compliance.26 However, a recent study in urban teens found that those using levonorgestrel were less likely to report condom use at last sexual contact or consistent condom use at follow-up 1 or 2 years later than users of OCs or condoms.27 These findings suggest that both the sexual behavior and motivation to use condoms in teens who use implants differ from those of teens who use OCs and condoms. In addition, teens often fail to use OCs or condoms in a fashion sufficiently consistent to prevent either unintended pregnancy or STDs.
EMERGING CONTRACEPTIVES
Contraceptive methods that may be available in the United States in the near future are described in Table 4. These include a monthly injection containing medroxyprogesterone acetate/estradiol cypionate (MPA/E2C, Lunelle, a two-rod levonorgestrel subdermal implant (Norplant-II), a one-rod etonorgestrel implant (Implanon), an IUD that releases levonorgestrel 20 μg/day for up to 7 years (LNG-20 IUD, Mirena), a vaginal ring that releases etonorgestrel and ethinyl estradiol (NuvaRing) and is discarded after 3 weeks to allow menses, and a 1-week transdermal patch that releases 17-desacetylnorgestimate and ethinyl estradiol (EVRA). A US company has also announced its intentions to reintroduce the Today contraceptive sponge impregnated with 1-g nonoxynol-9. Data from clinical trials indicate that the monthly combination injection, the new implants, and the levonorgestrel IUD are highly effective contraceptive methods.1, 13 In an open-label, nonrandomized, parallel, controlled study of the MPA/E2C contraceptive injection, no pregnancies occurred among 782 women during the first year of use (13 cycles of 28 days).13 With the two-rod implant, 5-year failure rates of 0.7% were reported in a large clinical trial,28 and the one-rod implant has been shown to be effective for 3 years with no pregnancies in a large number of women.29 A 7-year cumulative failure rate of 1.1% has been reported with the LNG-20 IUD.1 The vaginal ring appears to have contraceptive effectiveness considerably higher than the diaphragm, approaching that of OCs.30 However, no published data addressing the contraceptive efficacy of the estrogen-progestin vaginal ring or the transdermal patch are currently available.
Table 4. Comparison of available and prospective contraceptive methods
Parameter | Monthly Injection | Implants | LNG-20 IUD | Vaginal Rings | Transdermal Patch | Sponge |
Efficacy | High | High | High | Intermediate, some user dependence | Intermediate, some user dependence | Similar to other barrier methods |
Length of protection | 1 mo | 3–5 yr | 5–7 yr | 1 mo | 7 days | Single use with coitus |
Rapid return of fertility | Yes | Yes | Yes | Yes | Yes | Yes |
Regular cycles | Yes | Variable | Yes, most users | Yes, user controlled | Yes | Yes |
Amenorrhea | Uncommon | Variable | Variable | No | No | No |
Appropriate in nursing mothers | Unknown | Yes | Yes | No | No | Yes |
Procoagulant | No | No | No | May be less so than oral contraceptive | Unknown | No |
Noncontraceptive benefits | Unknown | Unknown | Reduces menorrhagia | Unknown | Unknown | May reduce risk of STDs |
Provider required to initiate | Yes | Yes | Yes | Yes (Rx) | Yes (Rx) | No |
Provider required to discontinue | No | Yes | Yes | No | No | No |
Privacy | Yes | Seen or felt by some users | Usually (string may be felt by partner) | Yes, can be removed before intercourse | No | No |
LNG, levonorgestrel; IUD, intrauterine device, STD, sexually transmitted disease.
(Adapted from Mishell DR, Arias RD, Darney PD et al: Contraception in the US: New methods = wider choices. Contemp Obstet Gynecol Suppl:1–26, 2000.)
These new contraceptive options will be valuable additions to the menu of contraceptive choices that clinicians can offer their patients. With the monthly combination injection, US women will have a shorter-acting alternative to DMPA. Although monthly injections are required, menstrual cycles are regular and there is a rapid return to fertility following cessation of use. Moreover, because estradiol cypionate does not increase hepatic globulin synthesis, no significant procoagulant effects have been seen in users of the monthly combination injection.16 The new second generation implants are much simpler to insert and remove than the first generation six-rod system, and their initial acceptance by patients and clinicians in many European countries has been excellent.30 Amenorrhea rather than irregular bleeding is generally seen with these products, which is acceptable to an increasing number of US women.30 These improvements may lead to a renaissance of interest in contraceptive implants among US clinicians and patients.
With the LNG-20 IUD, progestin is released more slowly and acts locally on the endometrium.30 Thus, there is less bleeding and indeed often amenorrhea occurs, making this a useful contraceptive option to reduce menstrual blood loss in women with menorrhagia, including those with bleeding dyscrasias. This progestin-releasing IUD also provides endometrial protection in menopausal women using estrogen, with few of the side effects related to systemic progestin use. The vaginal ring releases a low dose of hormones continuously when in place. Although designed to be removed for 7 days after 3 weeks of use, it can remain in place for longer periods, enabling a woman to control the timing of menses. The device is smaller than the diaphragm; because it is a one-size-fits-all product, no fitting is required. The ring should be an attractive contraceptive option for a substantial number of women. Like the vaginal ring, the new estrogen/progestin transdermal patch provides efficacy and cycle control similar to that of OCs without the need for daily pill-taking.30
A dedicated formulation became available in the United States in 1998 for emergency contraception. With Preven, the marketed version of the Yuzpe regimen, two tablets of a 50 μg-estrogen/progestin OC are taken 12 hours apart. Recently, a progestin-only method—Plan B—was approved. With Plan B, two 750-mg tablets of levonorgestrel are taken 12 hours apart. Plan B is reported to be 85% effective with a pregnancy rate of less than 2%.30 An advantage of the progestin-only method is that it causes fewer gastrointestinal side effects than the older method. Today, some clinicians provide every patient at risk for pregnancy with an advance prescription for emergency contraception. This strategy increases the likelihood that women will use emergency contraception when they need it and represents an important tool for reducing unintended pregnancies.
CONCLUSIONS
Effective contraception benefits both mothers and children by decreasing morbidity and mortality, improving the social and economic status of women, and improving the relationship of the mother with all her children. Despite the availability of effective, reversible methods of contraception, the United States has rates of unintended pregnancy and abortion more resembling those of a developing country than other industrialized nations. Among US couples, 40% choose male or female sterilization as their method of contraception, whereas in developing nations where access to female sterilization is limited, the IUD is the most popular method. In more developed countries, the OC is the most popular method of birth control, followed by the condom and the IUD.
Heavy reliance on sterilization by US couples reflects the lack of contraceptive choices and the mistaken belief that this surgical method is 'foolproof'. In fact, failure rates with various methods of tubal sterilization have been underestimated; this method is no more effective than injections, IUDs, or implants. The negative media attention focused on problems with reversible methods has also contributed to overuse of sterilization. An additional factor is that most health-care plans cover sterilization whereas only 49% of typical indemnity plans cover the cost of OCs, IUDs, diaphragms, or contraceptive implants and injections. Plans that provide coverage of prescription drugs often do not cover OCs.
New contraceptive methods likely to become available in the US soon will increase the number of effective, reversible contraceptive choices for US couples. Greater access to a wider variety of methods will increase contraceptive use. Much as a good cafeteria offers a wide selection of foods to accommodate a variety of tastes, so too must clinicians be able to offer women safe, effective, convenient options that meet their individual needs and preferences. The availability of a greater number of contraceptive choices will increase the use of more effective methods and thus has the potential to reduce unintended pregnancies and abortions in US women of all ages.
REFERENCES
Grimes DA (ed): The Contraception Report. 10:1–30, 2000 |
|
Huezo CM: Current reversible contraceptive methods: A global perspective. Int J Gynecol Obstet 62 (Suppl 1): S3– S15, 1998 |
|
Barber JS, Axinn WG, Thornton A: Unwanted childbearing, health, and mother-child relationships. J Health Soc Soc Behav 40: 231– 257, 1999 |
|
US Centers for Disease Control and Prevention: Achievements in Public Health, 1900–1999: Family Planning. MMWR Morb Mortal Wkly Rep 48:1073–1080, 1999 |
|
Baird DT, Glasier AF: Hormonal contraception. N Engl J Med 328: 1543– 1544, 1993 |
|
Speroff L: A quarter century of contraception: Remarkable advances, increasing success. Contemp Ob/Gyn May 15, 1998 |
|
Dicfalusy E: The contraceptive revolution. Contraception 61: 3– 7, 2000 |
|
Parker Jones K: Oral contraception: Current use and attitudes. Contraception 59 (Suppl 1): 17S– 20S, 1999 |
|
Piccinino LJ, Mosher WD: Trends in contraceptive use in the United States: 1982–1995. Fam Plann Perspect 30: 4– 10, 1998 |
|
Kaunitz AM: Long-acting hormonal contraception: Assessing impact on bone density, weight, and mood. Int J Fertil 44: 110– 117, 1999 |
|
Burnhill MSA: Contraceptive use: the U.S. perspective. Int J Gynecol Obstet 62 (Suppl 1): S17– S23, 1998 |
|
Hatcher RA, Trussell J, Stewart F et al: Contraceptive Technology. 17th rev ed. New York: Ardent Media, 1998 |
|
Kaunitz AM, Garceau RJ, Cromie MA et al: Comparative safety, efficacy, and cycle control of Lunelle monthly contraceptive injection (medroxyprogesterone acetate and estradiol cypionate injectable suspension) and Ortho-Novum 7/7/7 oral contraceptive (norethindrone/ethinyl estradiol triphasic). Contraception 60: 179– 187, 1999 |
|
Trussell J, Leveque JA, Koenig JD et al: The economic value of contraception. A comparison of 15 methods. Am J Public Health 85: 494– 503, 1995 |
|
Speroff L, Glass RH, Kase NG: Clinical Gynecologic Endocrinology and Infertility. 6th ed. Baltimore: Lippincott Williams & Wilkins, 1999 |
|
Kaunitz AM: Injectable contraception: New and existing options. Obstet Gynecol Clin North Am 2000 |
|
Kleerekoper M, Brienza RS, Schultz LR et al: Oral contraceptive use may protect against low bone mass. Arch Intern Med 161: 1971– 1976, 1991 |
|
Michäelsson K, Baron JA, Farahmand BY et al: Oral-contraceptive use and risk of hip fracture: A case-control study. Lancet 353: 1481– 1484, 1999 |
|
Sulak PJ, Kaunitz AM: Hormonal contraception and bone mineral density. Dialogues Contraception 6: 1– 4, 1999 |
|
Cromer BA, Blair JM, Mahan JD et al: A prospective comparison of bone density in adolescent girls receiving depot medroxyprogesterone acetate (Depo-Provera), levonorgestrel (Norplant), or oral contraceptives. J Pediatr 129: 671– 676, 1996 |
|
Orr-Walker BJ, Evans MC, Ames RW et al: The effect of past use of the injectable contraceptive depot medroxyprogesterone acetate on bone mineral density in normal post-menopausal women. Clin Endocrinol 49: 615– 618, 1998 |
|
Kaunitz AM: Oral contraceptive health benefits: Perception versus reality. Contraception 59 (Suppl 1): 29S– 33S, 1999 |
|
Kaunitz AM: Injectable depot medroxyprogesterone acetate for contraception: An update for U.S. clinicians. Int J Fertil 43: 73– 83, 1998 |
|
Davis A, Lippman J, Godwin A et al: Triphasic norgestimate/ethinyl estradiol oral contraceptive for the treatment of dysfunctional uterine bleeding. Obstet Gynecol 95 (Suppl 1): S84, 2000 |
|
Cates W Jr, Sulak PJ: Contraceptives and STDs: Alternative approaches to providing dual protection. Dialog Contracept 6: 1, 2000 |
|
Kaunitz AM: Contraception for the adolescent patient. Int J Fertil 42: 30– 38, 1997 |
|
Darney PD, Callegari LS, Swift A et al: Condom practices of urban teens using Norplant contraceptive implants, oral contraceptives, and condoms for contraception. Am J Obstet Gynecol 180: 929– 937, 1999 |
|
Sivin I, Alvarez F, Mishell DR et al: Contraception with two levonorgestrel rod implants: A 5-year study in the United States and Dominican Republic. Contraception 58: 275– 282, 1998 |
|
Zheng S-R, Zheng H-M, Qian S-Z et al: A randomized multicenter study comparing the efficacy and bleeding pattern of a single-rod (Implanon) and a six-capsule (Norplant) hormonal contraceptive implant. Contraception 60: 1– 8, 1999 |
|
Mishell DR Jr, Arias RD, Darney PD et al: Contraception in the US: New methods = wider choice. Contemp Obstet Gynecol Suppl:1–26, 2000 |