The Use of Gonadotropin-Releasing Hormone to Induce Ovulation
Authors
INTRODUCTION
Gonadotropin-releasing hormone (GnRH) was first isolated, characterized, and synthesized by Schally and Guillemin in 1971.1, 2, 3 However, it was the classic work by Knobil and co-workers demonstrating (1) that the pulsatile secretion of GnRH by the hypothalamus is the primary process controlling the menstrual cycle,4 and (2) that tonic GnRH stimulation causes downregulation of the pituitary GnRH receptor, that led to the widespread investigation of the therapeutic potentials of GnRH. Since that time, long-acting synthetic analogues of endogenous GnRH have gained widespread use in clinical gynecology for the treatment of pelvic pathology such as leiomyomas and endometriosis and as adjunctive therapy for use in ovulation induction with gonadotropins.
Since 1980, pulsatile GnRH has also been used with considerable success to stimulate the release of follicle-stimulating hormone (FSH) and luteinizing hormone (LH) from the pituitary gland for clinical ovulation induction.5, 6 This chapter reviews the physiology and rationale of ovulation induction with pulsatile GnRH, as well as patient selection and indications, therapy protocols, potential pitfalls, and expected outcomes.
PHYSIOLOGY
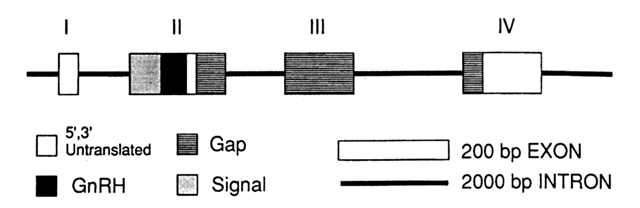
GnRH is a decapeptide that has been found in a number of mammals, including humans (Fig. 1). In postpubertal primates, GnRH is synthesized in the arcuate nucleus of the hypothalamus and is released in a pulsatile fashion and transported via the portal circulation to the anterior pituitary, where it stimulates the release of FSH and LH from gonadotropes. Immunohistochemical studies suggest that GnRH cells have an origin in the olfactory pit7 and migrate during early development to their final destination in the hypothalamus by approximately 11 weeks' gestation.8 The GnRH gene sequences were first isolated in 1984,9 and the human gene was localized to the short arm of chromosome 8 (Fig. 2).10 The GnRH decapeptide results from the post-translational processing of a larger 92 amino acid polypeptide and is frequently released in tandem with the GnRH-associated peptide (GAP). GAP may play a role in prolactin regulation. GnRH is rapidly degraded in the peripheral circulation, with a half-life of 2–8 minutes.11
|
A major advance in our understanding of GnRH physiology came in 1978, when Knobil and co-workers4 demonstrated that monkeys with lesions localized to the arcuate region had no detectable endogenous GnRH or gonadotropin release. Continuous replacement of exogenous GnRH in these monkeys led to gonadotropic desensitization resulting from a loss of GnRH receptors on the surface of the gonadotropes. However, exogenous replacement of GnRH in a pulsatile pattern, without varying the frequency or amplitude of administration, resulted in reinitiation of normal menstrual cycles characterized by orderly follicular development and a spontaneous midcycle LH surge. The findings that pulsatile administration of fixed doses of exogenous GnRH in the follicular phase of the primate menstrual cycle could lead to ovulation (and that overstimulation causes pituitary downregulation and unresponsiveness) form the basis for the clinical applications of GnRH use today.
Several features unique to the GnRH system make its pulsatile administration for ovulation induction theoretically advantageous compared to stimulation with either clomiphene citrate or exogenous gonadotropins. First, the GnRH receptors on pituitary gonadotropes increase in response to episodic GnRH stimulation. This 'self-priming' function allows an enhanced LH and FSH response to a steady dose of GnRH.12 Second, the feedback communication between the ovary and the pituitary remains intact, thereby allowing physiologic modulation of the cycle response and decreasing the risk of ovarian hyperstimulation or multiple pregnancy. Finally, for patients in whom fertility is a concern, GnRH has no antiestrogenic effects on the endometrium, thus providing a more receptive environment for implantation.
INDICATIONS AND PATIENT SELECTION
Given the aforementioned physiologic considerations, it follows reasonably that the women most likely to benefit from ovulation induction with pulsatile GnRH are those with an ovulatory defect resulting from deficient GnRH secretion. Thus, patients with hypogonadotropic hypogonadism will have the highest response rates. This group includes women with primary GnRH deficiency (e.g. Kallmann syndrome) as well as those with an intact hypothalamus but decreased GnRH release (e.g. hypothalamic amenorrhea). The success of GnRH stimulation in these patients led the Food and Drug Administration (FDA) to approve the use of intravenous (IV) pulsatile GnRH for ovulation induction in women with primary hypothalamic amenorrhea.
Ovaluation induction with pulsatile GnRH has also been used in many other settings. It has been used as a therapeutic modality in women with disordered endogenous GnRH secretion, such as polycystic ovary syndrome (PCOS), hyperandrogenic anovulation, and late-onset congenital adrenal hyperplasia, who are resistant to ovulation induction with clomiphene citrate. As will be discussed below, however, ovulation and pregnancy success rates in these groups are much lower than in women with hypogonadotrophic hypogonadism. Women with anovulation secondary to hyperprolactinemia respond similarly to those with GnRH deficiency, but the relative ease of administration and efficacy of the specific dopamine agonists make hyperprolactinemia a relatively rare indication for pulsatile GnRH. More logically, GnRH has also been used with success for ovulation induction in unusual causes of hypogonadotropic hypogonadism, such as the sequelae of treatment for cranial tumors13, 14 or amenorrheic lactating postpartum women.15
Depending on an infertile couple's history, documentation of tubal patency, normal uterine anatomy, and normal sperm parameters may be indicated before embarking on a course of pulsatile GnRH therapy. For women with anovulation resulting from conditions other than hypogonadotropic hypogonadism, a trial of clomiphene citrate is usually warranted before attempted ovulation induction with GnRH.
CLINICAL USE AND PROTOCOLS
Protocols using pulsatile GnRH and resulting in successful ovulatory responses and clinical pregnancies have been reported with varied doses, frequencies, and routes of administration; these will each be discussed later in more detail. All the clinical methods share in common the delivery of the pulsatile GnRH via a small, portable, programmable infusion pump. Several pumps are available in the United States, and all store a reservoir of GnRH solution and deliver a fixed or variable volume at specified intervals (e.g. Zyklomat, Ferring Laboratories, Ridgewood, New Jersey, USA; Auto Syringe, Auto Syringe Inc, Hooksett, New Hampshire, USA; Lutrepulse, Ortho Pharmaceutical, Raritan, New Jersey, USA). These pumps are similar to those used for insulin or tocolytic therapy, and most deliver the pulse over a 1-minute period.
Route of administration
Multiple routes of GnRH administration are available. Absorption occurs after IV, subcutaneous (SC), intramuscular (IM), nasal, and sublingual administration.16, 17, 18 Considerable debate exists over the preferred route of pulsatile GnRH administration for ovulation induction. Several centers have reported successful pregnancies using the SC administration of pulsatile GnRH.5, 19, 20, 21, 22 Most centers, however, have reported superior ovulation and pregnancy rates, as well as lower spontaneous abortion rates with IV administration.23, 24, 25, 26, 27, 28
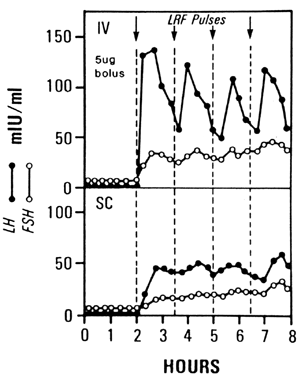
The pharmacokinetic data clearly suggest the superiority of the IV route.23, 29 IV administration of pulsatile GnRH results in a well-defined episodic release of LH and FSH, whereas SC administration of identical GnRH pulses can result in prolonged absorption with a slower sustained rise in LH and FSH without a normal pulsatile pattern and a slower return to baseline (Fig. 3). Advocates of SC administration stress the relative convenience and safety of this route and save IV administration only for those subjects who fail SC therapy. Subsequent to the higher ovulatory rates, however, the FDA has approved only the IV route for pulsatile GnRH administration.
At our institution, we favor the IV route of administration. Using sterile technique, a 22-gauge, 1 1/4-inch Teflon catheter is inserted into a vein in the nondominant forearm. Microbore plastic extension tubing (with a dead space less than 1 mL) is used to connect the catheter to the pump reservoir. Setups will vary depending on the pump and reservoir system chosen. A three-way stopcock between the reservoir and the extension tubing is often useful for refilling the reservoir or removing air from the line in certain setups. In our experience, patients tolerate the IV setup very well, and initial lines are often left in place for an entire cycle. A few programs leave the same peripheral IV in for several cycles,27 whereas others recommend changing the IV site every 3–7 days.30 Infection rates are generally low (see Complications section), and patient acceptance has been quite high in our experience.
Pulse frequency
The pulse frequency of endogenous GnRH in normal women during regular ovulatory menstrual cycles ranges from approximately 95 minutes in the early follicular phase to approximately 60–70 minutes in the periovulatory period.31, 32, 33 Luteal-phase pulses are of decreasing frequency but higher amplitude.
Based on Knobil's work in the monkey, original pulsatile GnRH ovulation induction in humans was largely performed with a fixed pulse frequency.5, 24 Excellent rates of ovulation (90–100%) and pregnancy have been reported with the use of fixed follicular-phase pulse frequencies of every 90 minutes26 and every 60 minutes,34 with little difference in steroid response, ovulation rates, or pregnancy rates being demonstrated between these two regimens.35 When pulse frequency was extended to 120 minutes, ovulation rates fell to approximately 70%.36 A 60-minute follicular-phase frequency has been shown more effective than a 120-minute frequency at inducing a spontaneous LH surge and ovulation in women with hypothalamic amenorrhea.37
In an effort to mimic the physiologic pulsations of GnRH in the normal menstrual cycle, some centers use a varying pulse frequency. A regimen using a 90-minute pulse frequency in the first week of folliculogenesis, followed by an increase in frequency to every 60 minutes in the midfollicular phase of the induced cycle, followed by a return to slower pulse frequency in the luteal phase, has been well described.27 The literature to date supports a follicular-phase pulse frequency of 90 minutes or less to achieve maximum spontaneous ovulation rates, and further studies need to be performed to determine whether there is an added benefit to cycle-specific, nonfixed frequency regimens.
Pulse dosage
Ovulation can be effectively induced over a range of GnRH doses. The optimal dose depends somewhat on the route of administration, because the SC route requires higher doses than the IV route. Studies have shown that a 1-μg pulse of IV GnRH will result in peak concentrations of GnRH within 4 minutes with levels between 200 and 260 pg/mL.38 These values correspond to the lower range of normal reported for pituitary portal blood concentrations (40–2000 pg/mL) in humans.39
Martin and associates27 elegantly defined the hormonal effects of varying IV pulse dosage at optimal pulse intervals. At a dosage of 25 ng/kg (1.25 μg/pulse for a 50-kg patient), the mean peak estradiol level was lower than in normal spontaneous cycles, corpus luteum function (as defined by integrated progesterone levels) was lower than normal, and ovulatory rates were only 80%. At 75 ng/kg (3.75 μg/pulse for a 50-kg patient), midcycle estradiol and progesterone levels were indistinguishable from normal cycles, and the ovulatory rate was 95%. At 100 ng/kg (5 μg/pulse for a 50-kg patient), high ovulatory rates were maintained (93%), but peak estradiol and integrated progesterone levels were exaggerated compared to normal cycles (Fig. 4).
Thus, we recommend a starting dose for IV therapy of 75 ng/kg/pulse (approximately 3.5–5.0 μg/pulse). For women who do not respond to this pulse dose, the dose can be incrementally increased up to 10–20 μg/pulse. We administer our pulses in a 0.9% sodium chloride solution containing 10 μg/mL GnRH and 30 units of heparin/mL. When tailoring optimal dosage regimens, allowances should be made for considerable individual differences in GnRH requirements. Obese patients and those with PCOS may require much higher doses than average.
Clinical monitoring and luteal-phase support
The clinical monitoring of induced cycles varies with the setting in which therapy takes place, available clinical resources, and the comfort level of the practitioner and patient. Many centers combine serum estradiol and transvaginal ultrasound monitoring with urine ovulation prediction kits for timing of intercourse. A presumptive diagnosis of ovulation is made by clinical or ultrasonographic findings (e.g. disappearance of a dominant follicle with free pelvic fluid on ultrasound, LH surge determined by urine monitoring, elevated progesterone, clear rise in basal body temperature). Others take a more simple approach and use only cycle length and basal body temperature charting as an index of ovulation.
Most patients ovulate within 10–20 days of initiation of IV pulsatile GnRH therapy. Cycle variance results largely from the length of the early follicular phase. Women with absolute GnRH deficiencies tend to have longer follicular phases, because the pituitary must be primed for several days before active secretion of FSH and LH.
At our center, for the first treatment cycle, we prefer a combination of ultrasound and urine LH monitoring. During subsequent cycles, usually only LH monitoring is necessary. Serial ultrasound examinations are performed starting about day 10, and urine LH testing is initiated when the mean ultrasound diameter of the lead follicle is 15 mm. Sexual intercourse, or intrauterine insemination in couples with male-factor infertility, is timed by the urinary LH surge. In our experience, the lack of a spontaneous LH surge is rare. This is an important advantage of GnRH-stimulated cycles because it is the administration of human chorionic gonadotropin (hCG) that may play a critical role in the development of ovarian hyperstimulation syndrome in patients undergoing stimulation with gonadotropins. However, in patients with a lead follicle of 23 mm or greater and no spontaneous surge, ovulation may be induced by the IM injection of 5000 units of hCG.
Luteal-phase support of the corpus luteum is essential to the outcome of a GnRH-induced cycle. Three methods are frequently used in clinical practice, but no prospective data exist to suggest the superiority of one method over the other. If the cycle stimulation resulted in the ovulation of a healthy follicle, successful cycle support can be achieved by continuing pulsatile GnRH administration at the same dose and frequency used in the first part of the cycle.40 Other groups have reported achieving successful clinical pregnancies by slowing the pulse frequency to every 4 hours in the luteal phase, with no apparent shortening of the cycle.41 Similar clinical results can be achieved by discontinuing the GnRH pump after ovulation and administering 1500–2000 U of exogenous hCG every 3 days for four doses starting 2 days after presumed ovulation. This method is more convenient than continuation of the pump, but it does not allow for multiple monthly cycles using the same catheter, an option that some centers offer.
Pulsatile gonadotropin-releasing hormone and polycystic ovary syndrome
Patients with PCOS or other variants of hyperandrogenic oligo-ovulation present a special challenge for ovulation induction with GnRH. The disordered release of endogenous GnRH and LH in this subpopulation is often exaggerated by pulsatile GnRH therapy. Ovulatory rates in women with PCOS treated with pulsatile GnRH alone are as low as 40–60% per cycle.42 However, the addition of GnRH agonist (GnRHa) therapy to downregulate the pituitary and reduce ambient testosterone levels before initiating pulsatile GnRH therapy dramatically improves the outcome in these patients. Filicori and colleagues,43 in a small study, initially showed an increase in ovulatory cycles from 38 to 90% in PCOS patients pretreated with GnRHa. Subsequently, they published the results of 228 GnRH-induced cycles in women with multifollicular ovary, PCOS, and other forms of hyperandrogenic anovulation.34 Seventy-four per cent of post-GnRHa cycles were ovulatory compared to 59% of 104 cycles in the same groups of patients without GnRHa pretreatment. In PCOS patients alone, pretreatment with GnRHa improved ovulatory rates from 49% to 71%.
In a small study, pretreatment with GnRHa was shown to be superior to pretreatment with an estrogen-gestagen compound in terms of resultant ovulatory GnRH-induced cycles.44 Pretreatment with GnRHa also reduces the risk of multiple pregnancy in patients with PCOS undergoing ovulation induction with pulsatile GnRH.28
Despite GnRHa pretreatment, luteal-phase steroid secretion remains abnormal after GnRH-induced ovulation in women with PCOS, and elevated spontaneous abortion rates have been reported in those cycles resulting in pregnancy.28 Continuous pulsatile GnRH therapy in women with PCOS has been suggested to improve the endocrine milieu. In women with PCOS treated with 100 ng/kg of IV pulsatile GnRH during consecutive cycles, first cycles were characterized by elevated levels of LH and luteal-phase estradiol compared to second cycles, which better approximated levels found in normal, eumenorrheic women.45 In another study, however, a suboptimal endocrine pattern and a lower ovulatory rate were found when a second post-GnRHa cycle occurred without an initial repeat of analog suppression.43 Table 1 summarizes selected series studying ovulation induction with GnRH in women with PCOS.19, 26, 43, 46, 47, 48, 49, 50, 51, 52
Table 1. Outcomes with pulsatile GnRH therapy in women with PCOS in selected studies
Study | No. of cycles | GnRH dose (μg) | Frequency (min) | Route | Ovulatory cycles (%) | Pregnancy rate (%) |
Saffan19 | 5 | 20 | 120 | SC | 40 | 0 |
Eshel52 | 108 | 15 | 90 | SC | 48 | 21 |
Hurwitz46 | 12 | 20–40 | 120–400 | SC | 17 | 0 |
Coelingh-Bennick47 | 42 | 10–20 | 90 | IV | 69 | 28 |
Ory48 | 6 | 90 | IV | 83 | 0 |
|
Burger49 | 85 | 5–40 | 60–120 | IV | 87 | 6 |
Wilson50 | 9 | 5–40 | 90 | IV | 0 | 0 |
Surrey51 | 9 | 5 | 90 | IV | 22 | 0 |
Post-GnRHa | 7 |
|
|
| 28 | 0 |
Filicori43 | 24 | 5 | 60 | IV | 38 | 8 |
Post-GnRHa | 21 |
|
|
| 90 | 38 |
Jansen26 | 14 | 2.5–5 | 60–120 | IV | 50 | 7 |
GnRH, gonadotropin-releasing hormone; GnRHa, GnRH agonist; PCOS, polycystic ovary syndrome; SC, subcutaneous; IV, intravenous.
(Modified from Santoro N, Elzahr D: Pulsatile gonadotropin-releasing hormone therapy for ovulatory disorders. Clin Obstet Gynecol 27:975,1984.)
In summary, women with PCOS constitute a more challenging population than those with hypothalamic amenorrhea for induction of ovulation with GnRH. For clomiphene-resistant women, however, pulsatile GnRH still represents a safe and relatively effective option that the clinician should consider before pursuing gonadotropin therapy. Pretreatment with GnRHa maximizes cycle potential in women with PCOS.
EXPECTED OUTCOMES
For women with hypogonadotropic hypogonadism, ovulation can be expected to occur in more than 90% of cycles (Table 2). Rates as low as 80% are reported from the earliest studies, but many of these stimulated cycles were performed with SC therapy and suboptimal pulse frequencies. In fact, ovulatory rates are so high in women with hypogonadotropic hypogonadism, that a failure in the delivery system should be considered in those women who do not ovulate. As discussed above, ovulatory rates are much lower in women with PCOS. In a review of 600 GnRH-induced cycles, decreased success was noted in overweight patients as well as those with elevated baseline LH, testosterone, and insulin levels.34
Table 2. Outcome with pulsatile GnRH therapy for ovulation induction in selected studies
Study | Indications | No. of patients | No. of cycles | GnRH dose (μg) | Frequency (min) | Route | Ovulatory cycles (%) | Pregnancy rate per ovulatory cycle (%) |
Filicori34 | HH, HA, | 292 | 600 | 1.25–20 | 60–120 | IV | 75 | 23 |
| PCOS, others |
|
|
|
|
|
|
|
Liu41 | HH, HA | 17 | 45 | 1–10 | 60–240 | IV | 82 | 30 |
| PCOS, others |
|
|
|
|
|
|
|
Martin53 | HA | 41 | 118 |
| 60–240 | IV | 93 | 31 |
Filicori28 | HH, HA, PCOS | 114 | 187 | 2.5–5 | 60 | IV | 76 | 32 |
Santoro35 | HA | 7 | 20 |
| 60–240 | IV | 100 | 30 |
Jansen26 | HH, HA | 26 | 79 | 2.5 | 60 | IV | 97 | 34 |
Braat54 | HH, HA | 49 | 272 | 2–100 | 60–120 | IV | 90 | 23 |
Skarin22 | HA | 24 | 67 | 1–40 | 60 | SC | 96 | 28 |
HH, hypogonadotropic hypogonadism; HA, hypothalamic amenorrhea; PCOS, polycystic ovary syndrome; SC, subcutaneously; IV, intravenously
Pregnancy rates per GnRH-induced cycle for hypogonadotropic patients range from 18 to 32%, with slightly higher rates per ovulatory cycle (see Table 2). Life-table analysis has been performed in a number of studies. Martin and colleagues27 reported the cumulative conception rate using life-table analysis for 21 patients with idiopathic hypogonadotropic hypogonadism and hypothalamic amenorrhea. The cumulative chance of conceiving over six GnRH-induced cycles was 94%. Braat and co-workers54 reported a cumulative conception rate of 93% after 12 cycles, with a mean conception rate of 22.5% per cycle. Homburg and colleagues55 reported cumulative pregnancy rates of 93–100% at 6 months in women with idiopathic hypogonadotropic hypogonadism, amenorrhea related to low weight, and organic pituitary disease. In women with PCOS, the cumulative pregnancy rates fell to 74% at 6 months. All of these reported pregnancy rates compare favorably to the 73% 6-month cumulative pregnancy rate seen in normal, fertile women.56, 57
One retrospective study compared exogenous gonadotropin stimulation (30 patients and 111 cycles) to pulsatile GnRH therapy (41 patients and 118 cycles) for ovulation induction in hypogonadotropic amenorrhea.53 Overall ovulatory rates (93% vs. 97%) and pregnancy rates per cycle (29% vs. 25%) were not significantly different between the two groups. Life-table analysis, however, revealed a higher cumulative 6-month pregnancy rate for the GnRH group (96%) than the exogenous gonadotropin group (72%). To date, no randomized clinical trial has been performed comparing the two methods of therapy, but the life-table analyses clearly reveal the therapeutic efficacy of pulsatile GnRH therapy in the select group of patients with hypogonadotropic hypogonadism.
Miscarriage rates approximate 25–30% in GnRH-induced cycles.34, 53, 55 These rates tend to be lower in women with hypothalamic amenorrhea and higher in hyperandrogenic women with elevated body mass index. The miscarriage rate among women with PCOS who conceive during GnRH-induced cycles approximates 45%.34, 52
COMPLICATIONS
The overall incidence of complications with GnRH therapy is low. The risk of multiple gestation with pulsatile GnRH is greater than in the general population, but lower than that seen with exogenous gonadotropin therapy and comparable to that resulting from clomiphene citrate therapy. Rates of multiple gestation resulting from GnRH cycles is in the range of 4–8%.27, 34, 55, 53 Martin and co-workers53 reported more than two dominant follicles on ultrasound in 48% of gonadotropin-treated cycles compared to 19% of pulsatile GnRH-induced cycles, whereas three or more dominant follicles were seen in 17% vs. 5%, respectively. Homburg and associates55 and Filicori and colleagues34 reported a less than 1% incidence of triplets resulting from GnRH-induced cycles.
Mild ovarian hyperstimulation has occasionally been reported with GnRH-induced cycles,58 but resolves quickly upon discontinuation of the therapy, perhaps because the prolonged stimulus of exogenous hCG is rarely present. Moderate or severe ovarian hyperstimulation, however, is extraordinarily rare. This is in contrast to the reported experience with exogenous gonadotropins plus hCG with 23% of cycles resulting in mild to severe, and occasionally life-threatening, hyperstimulation syndrome.27
Infectious complications are also rare, even with prolonged indwelling IV catheter placement. Superficial phlebitis at IV sites and cellulitis at the site of SC catheters have been reported.59, 60 The largest prospective study to date followed 230 catheters for 1958 catheter days.61 Just 11% of all catheter tips cultured positive, and only 2% of 195 blood cultures were positive. All positive blood cultures were obtained from patients with catheters in place for only 4–7 days. No positive blood cultures were obtained from patients with 97 catheters in place for more than seven days. Two of the four positive blood cultures grew Staphylococcus epidermidis and were thought to be possible contaminants. None of the four patients with positive blood cultures were clinically ill, none received antibiotics, and three had follow-up blood cultures within 10 days, all of which were negative.
The data suggest that the use of IV administration is associated with a low incidence of infectious complications. Nevertheless, for women with cardiac valvular disease (e.g. mitral valve prolapse) or any prosthetic device, it may be preferable to use the SC route of administration to minimize the theoretic risk of endocarditis.
The potential of antibody formation with GnRH therapy apparently exists, but has not been extensively studied. A 3% rate of GnRH antibody formation during 3 weeks to 9 months of SC GnRH therapy in 141 men and 22 women has been reported,62 but the clinical significance of these findings remains unclear.
COST
The cost of ovulation induction with GnRH varies from institution to institution and depends largely on the expense of the monitoring performed. Martin and associates27 estimated the range of costs for GnRH cycles compared to exogenous gonadotropin cycles. They estimated that a pulsatile GnRH cycle costs $495–3180, whereas an exogenous gonadotropin cycle costs between $700 and $5795, depending on the cost of the drug and the type of monitoring used. However, because of the relative risks of hyperstimulation and multiple gestation associated with each method, it is reasonable to assume that most treatment cycles would be in the low range of the GnRH scale (with a minimum of clinical monitoring necessary) and the higher end of the gonadotropin scale (with frequent ultrasound and serum estradiol evaluation necessary).
FUTURE CONSIDERATIONS
The success of pulsatile IV GnRH therapy in inducing ovulation has led to consideration of its utility for in vitro fertilization techniques. Supraphysiologic doses of IV pulsatile GnRH (10 μg/pulse) at 60–120-minute intervals has been reported to override successfully the normal estradiol feedback mechanisms and induce multiple follicular development in normal, eumenorrheic women.63 During these stimulated cycles, two to five follicles of mature size on ultrasound were induced in all six subjects. Mean peak estradiol levels were 585 pg/mL. In addition, we have had a successful pregnancy result from in vitro fertilization after oocyte aspiration from a GnRH-stimulated cycle (abstract presented 1998 ASRM Annual Meeting).
Another use for GnRH analogue therapy is the induction of final follicular maturation or ovulation triggering in cycles of controlled ovarian stimulation either for in vitro fertilization or intrauterine insemination. This is usually accomplished as noted above by a trigger shot of hCG that will bind to the shared LH receptor and mimic the LH surge. However, hCG has a much longer half-life and binds to the receptor for considerably longer than LH, thereby increasing the risk of prolonged ovarian stimulation resulting in ovarian hyperstimulation syndrome (OHSS). Several published reports have demonstrated the ability of GnRH agonsists to induce a spontaneous LH surge leading to ovulation in ovulation induction cycles or final follicular maturation in IVF cycles. This can be accomplished with a reduction in the incidence of OHSS compared to hCG-triggering, and may represent another useful role for GnRH analogues in assisted reproduction.64, 65, 66
SUMMARY
From this overview, it is apparent that pulsatile IV GnRH represents a reliable, acceptable, safe, and effective means of physiologically inducing ovulation in anovulatory women. Patients with hypogonadotropic hypogonadism constitute a small subset of the total infertile population. Yet, for this group of women, pulsatile GnRH therapy essentially restores normal ovulatory and cumulative conception rates with extremely low risks of ovarian hyperstimulation and multiple pregnancy. Women with anovulation resulting from other disorders, such as PCOS, may also benefit from ovulation induction with GnRH. However, ovulation and pregnancy rates are lower than those seen with hypogonadotropic hypogonadism, and a trial of clomiphene citrate should be undertaken before attempting ovulation induction with GnRH. Pretreatment with GnRHa improves the outcome for women with PCOS.
Effective therapy can be administered by either the SC or IV route, although the pharmacologic data as well as our own experience support the superiority of IV administration. With this route, patient acceptance is high and infectious complications are low. The optimal physiologic dose for initial ovulation induction with pulsatile IV GnRH is 75 ng/kg/pulse administered every 60–90 minutes. Outpatient clinical monitoring (and, therefore, cycle cost) can be kept to a minimum while patient safety is assured. Spontaneous ovulation is the norm, and luteal-phase support with either continued GnRH or exogenous hCG is mandatory.
It is unclear why ovulation induction with pulsatile GnRH has not enjoyed the widespread use in the United States that it has in Europe as an alternative to exogenous gonadotropin therapy in anovulatory women. It is hoped, however, that its worldwide success will lead to increased usage in the United States and will stimulate further research into its use. Specific projects that need to be performed prospectively include a study to determine whether a variable pulse frequency is superior to a fixed frequency, a randomized clinical trial comparing GnRH therapy to exogenous gonadotropins, and a study examining the benefit of supraphysiologic doses of pulsatile GnRH to be used for multiple follicular development for the assisted reproductive technologies.
REFERENCES
Matsuo H, Baba Y, Nair RMG et al: Structure of the porcine LH and FSH releasing factor: I. The proposed amino acid sequence. Biochem Biophys Res Commun 43: 1334, 1971 |
|
Burgus R, Butcher M, Ling N et al: Structure moleculair du facteur hypothalamique (LRF) d'origine ovine controlant la secretion de l'hormone gonadotrope hypophysaire de luteinisation (LH). CR Acad Sci 273: 1611, 1971 |
|
Amoss M, Burgus R, Blackwell R et al: Purification, amino acid composition and N-terminus of the hypothalamic luteinizing hormone releasing factor of ovine origin. Biochem Biophys Res Commun 44: 205, 1971 |
|
Belchetz PE, Plant TM, Nakai Y et al: Hypophysial responses to continuous and intermittent delivery of hypothalamic gonadotropin-releasing hormone. Science 202: 631, 1978 |
|
Crowley WF Jr, McArthur JW: Stimulation of the normal menstrual cycle in Kallman's syndrome by pulsatile administration of luteinizing hormone-releasing hormone (LHRH). J Clin Endocrinol Metab 51: 173, 1980 |
|
Leyendecker G, Wildt L, Hansmann M: Pregnancies following chronic intermittent (pulsatile) administration of Gn-RH by the means of a portable pump (“Zyklomat”): A new approach to the treatment of infertility in hypothalamic amenorrhea. J Clin Endocrinol Metab 51: 1214, 1980 |
|
Schwanzel-Fukuda M, Pfaff DW: Origin of luteinizing hormone-releasing hormone neurons. Nature 338: 161, 1989 |
|
Bloch B, Gaillard RC, Culler MD, Negro-Vilar A: Immunohistochemical detection of proluteinizing hormone-releasing hormone peptides in neurons in the human hypothalamus. J Clin Endocrinol Metab 74: 135, 1992 |
|
Seeburg PH, Adelman JP: Characterization of cDNA for precursor of human luteinizing hormone releasing hormone. Nature 311: 666, 1984 |
|
Yang-Feng TL, Seeburg PH, Francke V: Human luteinizing hormone-releasing hormone gene (LHRH) is located on the short arm of chromosome 8 (region 8p11.2 |
|
Jeffcoate SL, Greenwood RH, Holland DT: Blood and urine clearance of luteinizing hormone releasing hormone in man measured by radioimmunoassay. J Endocrinol 60: 305, 1974 |
|
Clayton RN, Catt KJ: Gonadotropin-releasing hormone receptors: Characterization, physiological regulation, and relationship to reproductive function. Endocr Rev 2: 186, 1981 |
|
Hall JE, Martin KA, Whitney HA et al: Potential for fertility with replacement of hypothalamic gonadotropin-releasing hormone in long term survivors of cranial tumors. J Clin Endocrinol Metab 79: 1166, 1994 |
|
Park KH, Park WI, Lee BS et al: Pulsatile gonadotropin-releasing hormone therapy in patients with pituitary tumors treated by surgery and irradiation. Clin Endocrinol 40: 407, 1994 |
|
Zinaman MJ, Cartledge T, Tomai T et al: Pulsatile GnRH stimulates normal ovarian function in amenorrheic lactating postpartum women. J Clin Endocrinol Metab 80: 2088, 1995 |
|
Gonzalez-Barcena D, Kastin AJ, Schlach DS et al: Synthetic LH-releasing hormone (LH-RH) administered to normal men by different routes. J Clin Endocrinol Metab 37: 481, 1973 |
|
Keller PJ: Treatment of anovulation with synthetic luteinizing hormone-releasing hormone. Am J Obstet Gynecol 116: 698, 1973 |
|
London DR, Butt WR, Lynch SS et al: Hormonal responses to intranasal luteinizing hormone-releasing hormone. J Clin Endocrinol Metab 37: 829, 1973 |
|
Saffan D, Seibel MM: Ovulation induction with subcutaneous pulsatile gonadotropin-releasing hormone in various ovulatory disorders. Fertil Steril 45: 475, 1986 |
|
Seibel MM, Kamrava M, McArdle C, Taymor ML: Ovulation induction and conception using subcutaneous pulsatile gonadotropin-releasing hormone. Obstet Gynecol 61: 292, 1983 |
|
Hurley DM, Brian RJ, Burger HG: Ovulation induction with subcutaneous pulsatile gonadotropin-releasing hormone: Singleton pregnancies in patients with previous multiple pregnancies after gonadotropin therapy. Fertil Steril 40: 575, 1983 |
|
Skarin G, Ahlgren M: Pulsatile gonadotropin-releasing hormone (GnRH): Treatment for hypothalamic amenorrhoea causing infertility. Acta Obstet Gynecol Scand 73: 482, 1994 |
|
Reid RL, Leopold GR, Yen SSC: Induction of ovulation and pregnancy with pulsatile luteinizing hormone-releasing factor: Dosage and mode of delivery. Fertil Steril 36: 553, 1981 |
|
Leyendecker G, Struve T, Plotz EJ: Induction of ovulation with chronic intermittent (pulsatile) administration of LH-RH in women with hypothalamic and hyperprolactinemic amenorrhea. Arch Gynecol 229: 177, 1980 |
|
Loucopoulos A, Ferin M, Vande Wiele RL et al: Pulsatile administration of gonadotropin-releasing hormone for induction of ovulation. Am J Obstet Gynecol 148: 895, 1984 |
|
Jansen RPS, Handelsman DJ, Boyland LM et al: Pulsatile gonadotropin-releasing hormone for ovulation-induction in infertile women: I. Safety and effectiveness with outpatient therapy. Fertil Steril 48: 33, 1987 |
|
Martin K, Santoro N, Hall J et al: Clinical Review 15: Management of ovulatory disorders with pulsatile gonadotropin-releasing hormone. J Clin Endocrinol Metab 71 (5): 1081A, 1990 |
|
Filicori M, Flamigni C, Meriggiola MC et al: Endocrine response determines the clinical outcome of pulsatile gonadotropin-releasing hormone ovulation induction in different ovulatory disorders. J Clin Endocrinol Metab 72: 965, 1991 |
|
Handelsman DJ, Jansen RPS, Boylan LM et al: Pharmacokinetics of gonadotropin-releasing hormone: Comparison of subcutaneous and intravenous routes. J Clin Endocrinol Metab 59: 739, 1984 |
|
Blacker CM: Ovulation stimulation and induction. Endocrinol Metab Clin North Am 21: 57, 1992 |
|
Elkind-Hirsch K, Ravnikar V, Tulchinsky D et al: Episodic secretory patterns of immunoreactive luteinizing hormone-releasing hormone (IR-LH-RH) in the systemic circulation of normal women throughout the menstrual cycle. Fertil Steril 41: 56, 1984 |
|
Veldhuis JD, Beitins IZ, Johnson ML et al: Biologically active luteinizing hormone is secreted in episodic pulsations that vary in relation to stage of the menstrual cycle. J Clin Endocrinol Metab 58: 1050, 1984 |
|
Filicori M, Santoro N, Merriam GR, Crowley Jr WF: Characterization of the physiological pattern of episodic gonadotrophin secretion throughout the human menstrual cycle. J Clin Endocrinol Metab 62: 1136, 1986 |
|
Filicori M, Flamigni C, Dellai P et al: Treatment of anovulation with pulsatile gonadotropin-releasing hormone: Prognostic factors and clinical results in 600 cycles. J Clin Endocrinol Metab 79: 1215, 1994 |
|
Santoro N, Wierman ME, Filicori M et al: Intravenous administration of pulsatile gonadotropin-releasing hormone in hypothalamic amenorrhea: Effects of dosage. J Clin Endocrinol Metab 62: 109, 1986 |
|
Braat DDM, Schoemaker J: Endocrinology of gonadotropin-releasing hormone induced cycles in hypothalamic amenorrhea: The role of the pulse dose. Fertil Steril 56: 1054, 1991 |
|
Filicori M, Flamigni C, Campaniello E et al: Evidence for a specific role of GnRH pulse frequency in the control of the human menstrual cycle. Am J Physiol 257: E930, 1989 |
|
Miller DS, Reid RR, Cetel NS et al: Pulsatile administration of low-dose gonadotropin-releasing hormone: Ovulation and pregnancy in women with hypothalamic amenorrhea. JAMA 250: 2937, 1983 |
|
Antunes JL, Carmel PW, Housepian EM, Ferin M: Luteinizing hormone-releasing hormone in human pituitary blood. J Neurosurg 49: 382, 1978 |
|
Filicori M, Valdiserri A, Flamigni C et al: Ovulation induction with pulsatile gonadotropin-releasing hormone: Technical modalities and clinical perspectives. Fertil Steril 56: 1, 1991 |
|
Liu JH, Yen SSC: The use of gonadotropin-releasing hormone for the induction of ovulation. Clin Obstet Gynecol 27: 975, 1984 |
|
Santoro N, Elzahr D: Pulsatile gonadotropin-releasing hormone therapy for ovulatory disorders. Clin Obstet Gynecol 36: 727, 1993 |
|
Filicori M, Flamigni C, Camaniello et al: The abnormal response of polycystic ovarian disease patients to exogenous pulsatile gonadotropin-releasing hormone: Characterization and management. J Clin Endocrinol Metab 69: 825, 1989 |
|
Gerhard I, Matthes J, Runnebaum B: The induction of ovulation with pulsatile gonadotropin-releasing hormone (GnRH) administration in hyperandrogenic women after down-regulation with buserelin or suppression with an oral contraceptive. Hum Reprod 8: 2033, 1993 |
|
Corenthal L, Von Hagen S, Larkins D et al: Benefits of continuous physiological pulsatile gonadotropin-releasing hormone therapy in women with polycystic ovarian syndrome. Fertil Steril 61: 1027, 1994 |
|
Hurwitz A, Rosenn B, Palti Z et al: The hormonal response of patients with polycystic ovarian disease to subcutaneous low-frequency pulsatile administration of luteinizing hormone-releasing hormone. Fertil Steril 46: 378, 1986 |
|
Coelingh-Bennick HJT, Weber HW, Alsbach HPJ, Thijssen JHH: Induction of ovulation by pulsatile intravenous administration of GnRH in polycystic ovarian disease. Fertil Steril 41: 34S, 1984 |
|
Ory SJ, London SN, Tyrey L, Hammond CB: Ovulation induction with pulsatile gonadotropin-releasing hormone administration in patients with polycystic ovarian syndrome. Fertil Steril 43: 20, 1985 |
|
Burger CW, Korsen TJ, Hompes PG et al: Ovulation induction with pulsatile luteinizing hormone-releasing hormone in women with clomiphene citrate-resistant polycystic ovary-like disease: Clinical results. Fertil Steril 46: 1045, 1986 |
|
Wilson JM, Traub AI, Sheridan B et al: Conventional dose intravenous pulsatile GnRH therapy does not induce ovulation in polycystic ovarian disease. Acta Endocrinol (Copenh) 117: 289, 1988 |
|
Surrey ES, de Ziegler D, Lu JKH et al: Effects of gonadotropin-releasing hormone (GnRH) agonist on pituitary and ovarian responses to pulsatile GnRH therapy in polycystic ovarian disease. Fertil Steril 52: 547, 1989 |
|
Eshel A, Abdulwahid NA, Armar NA: Pulsatile luteinizing hormone-releasing hormone therapy in women with polycystic ovary syndrome. Fertil Steril 49: 956, 1988 |
|
Martin KA, Hall JE, Adams JM, Crowley WF: Comparison of exogenous gonadotropins and pulsatile gonadotropin-releasing hormone for induction of ovulation in hypogonadotropic amenorrhea. J Clin Endocrinol Metab 77: 125, 1993 |
|
Braat DD, Schoemaker R, Schoemaker J: Life table analysis of fecundity in intravenously gonadotropin-releasing hormone-treated patients with normogonadotropic and hypogonadotropic amenorrhea. Fertil Steril 55: 266, 1991 |
|
Homburg R, Eshel A, Armar NA et al: One hundred pregnancies after treatment with pulsatile luteinising hormone releasing hormone to induce ovulation. Br Med J 298: 809, 1989 |
|
Guttmacher AF: Factors affecting normal expectancy of conception. JAMA 161: 855, 1956 |
|
Tietze C: Fertility after discontinuation of intrauterine and oral contraception. Int J Fertil 13: 385, 1968 |
|
Skarin G, Millius SJ, Wide L: Pulsatile low dose luteinizing hormone-releasing hormone treatment for ovulation induction of follicular maturation and ovulation in women with amenorrhea. Acta Endocrinol (Copenh) 101: 78, 1982 |
|
Hurley DM, Brian R, Outch K et al: Induction of ovulation and fertility in amenorrheic women by pulsatile low dose gonadotropin-releasing hormone. N Engl J Med 310: 1069, 1984 |
|
Molloy BG, Hancock KW, Glass MR: Ovulation induction in clomiphene nonresponsive patients: The place of pulsatile gonadotropin-releasing hormone in clinical practice. Fertil Steril 43: 26, 1985 |
|
Hopkins CC, Hall JE, Santoro NF et al: Closed intravenous administration of gonadotropin-releasing hormone (GnRH): Safety of extended peripheral intravenous catheterization. Obstet Gynecol 74: 267, 1989 |
|
Meakin JL, Keogh EJ, Martin CE: Human anti-luteinizing hormone-releasing hormone antibodies in patients treated with synthetic luteinizing hormone-releasing hormone. Fertil Steril 43: 811, 1985 |
|
Liu JH, Durfee R, Muse K, Yen SSC: Induction of multiple ovulation by pulsatile administration of gonadotropin-releasing hormone. Fertil Steril 40: 18, 1983 |
|
Engmann L, DiLuigi A, Schmidt D et al: The use of gonadotropin-releasing hormone (GnRH) agonist to induce oocyteundergoing in vitro fertilization prevents the risk of ovarian hyperstimulationsyndrome: a prospective randomized controlled study. Fertil Steril. 2008;89:84-91. Epub 2007 Apr 26. |
|
Engmann L, Siano L, Schmidt D et al: GnRH agonist to induce oocyte maturation during IVF in patients at high risk ofOHSS. Reprod Biomed Online. 2006 Nov;13(5):639-44. |
|
Acevedo B, Gomez-Palomares JL, Ricciarelli E et al: Triggering ovulation with gonadotropin-releasing hormone agonists does notcompromise embryo implantation rates. Fertil Steril. 2006 Dec;86(6):1682-7. Epub 2006 Oct 30. |



 3–15
3–15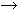 p21). Somat Cell Mol Genet 12: 95, 1986
p21). Somat Cell Mol Genet 12: 95, 1986