Diagnosis Findings suggestive of multiple gestation include discrepancy between size
and date, elevated α-fetoprotein (AFP) levels, and the auscultation
of fetal heart tone at two locations. Before ultrasonography was
available, a diagnosis of higher-order gestation commonly was made by
obtaining a radiograph of the abdomen. As late as 1980,36 diagnosis at the moment of the delivery was not uncommon. Fortunately, such
events are now rare because most cases follow treatment for infertility
or ART, and the possibility of a higher-order gestation is never
in question. The use of ultrasonography virtually ensures early and accurate diagnosis
of all higher-order gestations. Careful documentation of placental
location and the number of sacs is essential (Fig. 5). Regardless of the number of sacs, it is necessary to search for evidence
of monoamniotic placentation. According to Landy and colleagues,74,75 a significant number of twin pregnancies spontaneously disappear, giving
rise to the so-called vanishing twin syndrome; it also is possible
that some naturally occurring higher-order gestations undergo a similar
process of reduction, especially in pregnancies that have an odd number (i.e., 3 or 5). Although Allen76 has postulated a variety of additive mechanisms by which triplets or quintuplets
might occur, his analysis was made in the years before the
knowledge of “vanishing,” and he considered only variations
of the splitting process. 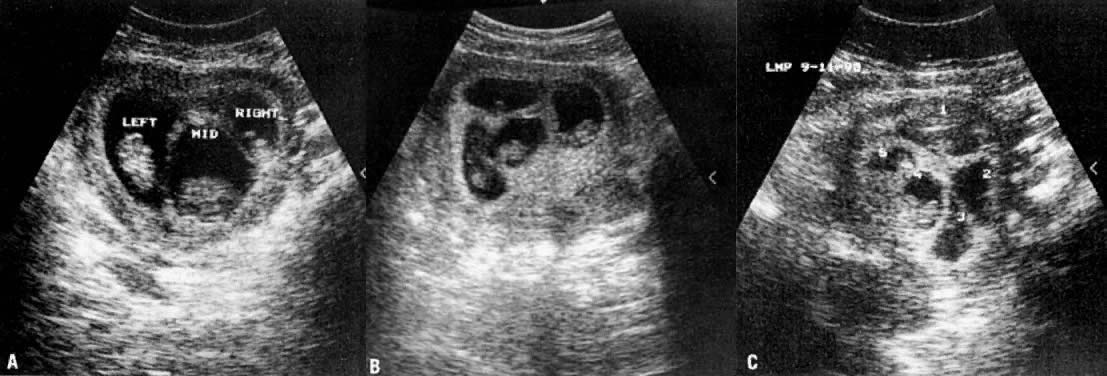 Fig. 5. Ultrasound images of twin ( A ), triplet ( B ), and quadruplet ( C) gestation. These early ultrasound images were obtained using real-time
ultrasonography with an abdominal transducer at about 9 to 11 weeks' gestation.(Courtesy of Dr. Rudy Sabbagha) Fig. 5. Ultrasound images of twin ( A ), triplet ( B ), and quadruplet ( C) gestation. These early ultrasound images were obtained using real-time
ultrasonography with an abdominal transducer at about 9 to 11 weeks' gestation.(Courtesy of Dr. Rudy Sabbagha)
|
The phenomenon of a vanishing sac also has been reported in higher-order
gestations conceived by IVF.77 Higher-order gestations, like twins, have an increased incidence of congenital
malformations. It is possible that some of these anomalies originate
from the splitting of monovular twins. A detailed ultrasound anatomic
survey should be attempted at 18 to 20 weeks' gestation. As a result
of technical difficulties involved in such types of scanning, however, the
need for this investigation may represent an indication for
consultation with a maternal—fetal medicine subspecialist or an
expert in obstetric ultrasound. If one of the fetuses is diagnosed with
a malformation, the patient should be advised about the availability
of selective termination. Management DIET. No doubt remains about the increased nutritional demands of higher-order
gestations. A weight gain of 44 pounds has been suggested for twins78; in higher-order gestations, the appropriate weight gain remains to be
established. Few data are available for the establishment of objective
guidelines; reports on triplet gestations describe only the maternal
weight gain. Syrop and Varner34 reported on 20 triplet gestations with a mean maternal weight gain of 34.1 lb (range, 18.9 to 69.7 lb). Michlewitz and co-workers79 reported on 15 triplet gestations in which maternal weight gain ranged
from 6 to 44 lb; average gain was not reported. Both of these reports, however, encompassed
several decades of patient delivery. During that
time, not only did recommendations provided by physicians regarding
weight gain change considerably but also social factors that influenced
body image and prepregnant weights changed. The most recent report on weight gain in triplet gestation was by Luke
and co-workers.80 This pilot study comprised a cohort of women who brought their triplet
children to the Multiple Births Foundation Clinic in London and who had
given birth since 1983. The study design was a retrospective, anonymous, pilot
telephone survey of demographic, anthropometric, and perinatal
data. Telephone interviews were conducted by a research nurse. Specific
details about weight gain were obtained from the Cooperation Card
retained by the patient during and after her pregnancy, which contained
data on prenatal weights at each visit. This study focused not only
on total maternal weight gain but also on birth weight. Of interest, better
intrauterine growth was achieved when maternal weight gains were
equal to or greater than 1.5 pounds per week before 24 weeks' gestation. Collins and Blyel21 reported on the maternal weight gain in 70 quadruplet pregnancies; the
mean maternal weight gain was 45.8 lb (range, 11 to 100 lb). Even though
these gains are similar to those reported for twins, the periods during
which the gain was recorded are dissimilar because quadruplets are
delivered up to 4 to 6 weeks earlier than twins, who are delivered, on
average, at 36 to 37 weeks. If matched for gestational age, even large
gains undoubtedly would be recorded for higher-order gestations. It
is important that such gains not be viewed as abnormal. Only the rapid
weight gain associated with various stigmata of preeclampsia should
be of concern. Early in pregnancy, consultation with a registered dietitian should be
requested to maintain a well-balanced diet and to ensure the adequate
and early weight gain that is necessary to assist the early developmental
stages of gestation. In addition, prenatal vitamins are recommended. The
expected high incidence of anemia associated with higher-order
gestations dictates that iron supplementation be started at the initial
prenatal visit, even if the hemoglobin level is normal at that time. We
suggest 300 to 600 mg/d of oral ferrous sulfate. Red meat is the best
and most palatable form of dietary iron supplementation because it
provides iron in a bioavailable form without gastrointestinal side effects
otherwise associated with iron supplementation. One-half pound of
red meat per day should be the minimum for women with higher-order gestations. ULTRASOUND. Ultrasonography is essential for the early diagnosis of higher-order gestations; it
also is an essential part of antenatal management for these
pregnancies. Only with the use of serial ultrasonography is it possible
to detect fetal growth abnormalities or fetus-to-fetus transfusion
if monochorionic placentation is present. The use of triplet-specific ultrasound growth tables is not without controversy. There
are few reports on this issue81 because of the difficulty of obtaining data on large numbers of higher-order
gestations for the creation of such tables. Weissman and colleagues81 performed serial ultrasonography in 24 triplet gestations between 1978 and 1987 and
documented slowing of the biparietal diameter, head circumference, and
abdominal circumference starting at 28 weeks. However, the
head circumference/abdominal circumference ratio remained normal, possibly
suggesting a pattern of symmetric growth retardation. Nevertheless, femur
growth was assessed to be parallel to that seen in singletons. The
authors suggested the use of their triplet-specific growth tables
for the detection of IUGR. In contrast, Jones and co-workers82 reviewed 196 sets of triplets (from the same database as Newman and colleagues18) and were not able to detect any distinct slowing of the birth-weight
growth curves. They plotted a linear curve of growth between 22 and 38 weeks. Using the Rossavik growth models, Hata and associates83 compared the fetal growth of 7 triplet, 13 twin, and 20 singleton gestations. Their
findings demonstrated growth potential realization in the
values for triplets that were similar to those for singletons and twins. These
authors concluded that individual assessment of growth in triplets
can be performed with the same methods generally used for both
singletons and twins. In contrast, Yuval and colleagues84 reported on the intrauterine growth of triplets as estimated from live-born
birth-weight data. Their study was based on 109 sets of triplets. The
estimated intrauterine growth of triplets, in contrast to that of
singletons, exhibited neither an acceleration phase during the third
trimester nor a flattening of the growth curve during the last few weeks
of the third trimester. The mean birth weight of the triplets in this
study was slightly below the 10th percentile for singletons at 38 weeks' gestation
or later. The authors concluded that the growth of triplets
as estimated from live-born birth weights is slower that of singletons. They
further recommended that the diagnosis of intrauterine growth
in triplet pregnancies should be based on triplet gestation-specific
growth curves. Only one report has been published on the accuracy of the estimation of
fetal weight in multiple gestations. Lynch and co-workers85 evaluated 1832 singleton, 518 twin, and 51 triplet fetuses. Their analysis
concluded that ultrasound estimation of fetal weight is as accurate
in twins and triplets as it is in singletons. Ultrasonographic determination of chorionicity is of great importance because
it helps assess the likelihood of morbidity and mortality in multiple
gestations. Using transvaginal ultrasonography before 14 weeks' gestation, Monteagudo
and colleagues86 reported on 43 gestations (40 twin and 3 triplet) with confirmatory placental
pathologic evaluation. In all cases, transvaginal ultrasonography
correctly predicted the chorionic and amniotic type that subsequently
was confirmed by placental pathology. The ultrasonographic findings
of interest were the following: if a wedge-shaped junction was seen, it
was considered to be the fusion of two chorionic membranes; if a T-shaped
junction was seen, it was considered to be the fusion of the two
amnions. All higher-order multiple gestations should be evaluated by targeted ultrasonography
at an appropriate age. Pryde and co-workers87 stated that the likelihood of having at least one malformed fetus in triplet
gestation is about 9%, whereas the incidence of two or three simultaneously
but discordantly malformed fetuses in a multizygotic triplet
gestation is 0.09% and 0.0027%, respectively; these authors reported
the first of such instances. MATERNAL α-FETOPROTEIN AND GENETICS. Few data are available on the normal values of maternal serum AFP in higher-order
gestations. Wald and co-workers88 suggested values in triplets of up to 3.2 times those in singletons at
matched gestational ages and values in quadruplets of up to 5 times those
in singletons. No normative tables have been published for the interpretation
of AFP values in higher-order gestations, and it is not possible
to use this screening test for accurate detection of neural tube
defects in these pregnancies. If this test is performed, consultation
with a perinatologist or a geneticist is advised for the interpretation
of results. The indications for genetic evaluation of a fetus are numerous, the most
frequent being advanced maternal age. This state also is an indication
for amniocentesis in a higher-order gestations. Family history or a
prior infant affected by a chromosomal problem also may be an indication
for amniocentesis. In the event that amniocentesis is performed, indigo-carmine
should be instilled in each sac to prevent multiple sampling
of the same sac. Prevention of Premature Labor CERCLAGE. Elective cerclage has been evaluated in triplet pregnancy17,89 and appears to be without substantial benefit in the management of these
cases. Newman and co-workers18 reported on several patients treated with cerclage. It is not clear from
this report, however, whether these patients had cervical incompetence
or whether suture placement was elective. The outcome of operated
patients was poorer, with an average EGA of 29.2 weeks at delivery, than
the nonoperated EGA of 33.6 weeks at delivery. Understandably, the
indications for cerclage placement may have contributed substantially
to this unsatisfactory outcome. Similar experiences have been reported
by Lipitz and colleagues17 and by Itzkowic.89 A controlled evaluation of 35 women with triplet conceptions hospitalized
in the high-risk pregnancy unit at the Hebrew University Hadassah Medical
School was described by Mordel and co-workers.90 Twelve of the 35 women underwent elective cerclage at 12 to 14 weeks' gestation; 23 served
as controls. None of the study subjects had historical
or physical findings indicative of cervical incompetence. The gestational
age (in weeks) at delivery was 33 ± 5.1 and 34.7 ± 2.8 (mean, ±standard deviation) for the sutured and control
groups, respectively. Birth weights were 1833 ± 524.5 and 1884 ± 455.5 for
the sutured and control groups, respectively. Despite
the retrospective nature of the analysis, the authors believed the
rigid criteria for case inclusion (i.e., absence of history or physical signs of cervical incompetence) strengthened
their conclusion that triplet gestations did not benefit by late
first-trimester or early second-trimester cerclage. TOCOLYTICS. Tocolytic therapy often is required to treat preterm labor. The armamentarium
of tocolytics includes β-mimetics (e.g., ritodrine, terbutaline, salbutamol), magnesium sulfate, and indomethacin. These
agents have been used with varying results. Prophylactic Tocolytics. Ron-El91 compared eight patients who received β-mimetic prophylaxis with six
who did not and could not document improvement in EGA at delivery after
prophylactic use of these agents. Similarly, Newman and co-worker18 reported on 115 (58.1%) of 198 sets of triplets who received prophylactic β-mimetics. No
improvement was apparent in any outcome variables
after therapy. Interpretation of data from these two reports does
not support the efficacy of prophylactic β-mimetic tocolysis in triplet
gestation. The same caution might also apply to other types of
higherorder gestations, but data are limited. Therapeutic Tocolysis. Whereas data on prophylactic tocolysis is severely limited, the impact
of therapeutic tocolysis on higher-order gestations has been reported
more frequently. Itzkowic89 reported an incidence of preterm labor of 78% (46 of 59 triplet sets). Of
these cases, seven patients received salbutamol in an attempt to stop
their labors. Of these seven patients, four delivered within 36 hours, and
three delivered at least 3 weeks later. No mention was made of
any side effects from the treatment. Newman and co-workers18 reported that more than half (66.2%; 131 of 198 triplet sets) of cases
in their series was complicated by preterm labor, with a mean EGA at
diagnosis of 29.9 weeks. No description of the type of tocolytic agent
or the administration regimen was provided. Also, no mention was made
of complications from this therapy. Holcberg and co-workers16 reported an incidence of preterm delivery of 97% (30 of 31 triplets). Five
patients were treated with ritodrine, with an average gain of 2.6 weeks
before delivery. Again, no mention was made of side effects. Keith and associates45 reported on 13 sets of triplets, of whom two thirds required tocolysis
in the form of ritodrine or magnesium sulfate. No significant complications
from this therapy were reported. Yet another study, by Vervliet
and colleagues,35 reported on 15 triplets and 6 quadruplets who were treated with intravenous
ritodrine. In addition, some patients were treated with rectal indomethacin (Indocin) until 34 weeks' gestation. No mention was made of
oligohydramnios as a sequelae of indomethacin therapy. Elliott and Radin92 reported on 12 triplet and 4 quadruplet gestations. These patients received
magnesium sulfate for tocolysis. Higher serum levels of magnesium
sulfate (7.0 to 7.5 mg/dL) were necessary to achieve adequate cessation
of uterine activity. These authors also concluded that rates of infusion
of magnesium sulfate of 4 to 5 g/h were necessary in triplets and
quadruplets to achieve cessation of uterine activity. These observations, if
confirmed by others, have important clinical implications: namely, that
the present low levels of success in prolonging gestation
in higher-order multiple gestations may be improved with a more aggressive
approach toward medication dosage. Because most medications available
for tocolytic therapy have substantial side effects, controlled studies
are warranted to document the pharmacokinetics of each agent in
higher-order multiple gestations. Although the total number of reported patients who have received therapeutic
tocolysis for preterm labor in higher-order gestations is modest, we
believe that β-mimetics and probably magnesium sulfate have
therapeutic value. The presence of contractions alone is probably an insufficient
indication to start treatment, however. A diagnosis of preterm
labor should include documentation of cervical change. Utter and
co-workers,93 using data from singleton pregnancies, confirmed that the success of tocolytic
therapy is not hampered by waiting for cervical change to strengthen
the diagnosis of preterm labor. We further recommend that if tocolysis
is used, the clinician should be prepared to handle any possible
side effects of the medication, including maternal tachycardia, pulmonary
edema, myocardial ischemia, hyperglycemia, and electrolyte imbalances. Data
from twin gestations suggest a higher incidence of side
effects when compared with singletons.94 A similar assumption can be made with regard to higher-order multiple
gestations. INDUCTION OF PULMONARY MATURITY. Little information exists on this topic with regard to higher-order multiple
gestations. Holcberg and colleagues,16 Ron-El,91 and Newman and co-workers18 all described several patients in their respective series who received
steroids for the induction of surfactant production by the fetuses. The
small numbers of patients treated, however, precludes making a comprehensive
evaluation of the effectiveness of this treatment. Pons and
co-workers54 reported that 10 of their 21 sets of triplets received steroids. None
of the newborns of mothers who received steroids developed respiratory
distress syndrome. Of the group that did not receive steroids, however, 21% of
newborns developed respiratory distress syndrome. No maternal
side effects were noted. The administration of steroids may result in an increase in uterine activity. Elliott
and Radin95 reported on 10 triplet and 5 quadruplet gestations that received at least
one course of steroids for the induction of pulmonary maturity. A
significant increase in contractions, a statistically increased likelihood
of labor with cervical change, and the need for tocolysis were noted
when the basal contraction rate was at least 3.5 contractions per
hour. These investigations concluded that there should be fewer than 3.5 contractions
per hour to minimize the steroid effect on uterine activity. If the clinician caring for a higher-order multiple gestation decides to
use steroids, careful monitoring is urged, especially if the patient
is being treated concomitantly with β-mimetics. An increase in cardiovascular
complications, especially pulmonary edema, has been reported
in singletons and twins. BED REST. During the past several decades, bed rest has been the subject of intense
discussion in terms of its value for the prevention of preterm labor
and the improvement of birth-weight outcomes in multiple gestations. In
the triplet literature, some authors have advocated early hospitalization
for bed rest.16,96,97 Others18 have suggested decreased physical activity with bed rest at home, limiting
hospital admissions to the treatment of premature labor or significant
obstetric or medical complications. One of the few studies that tried to assess the quantity of activity in
triplet gestations34 documented a higher incidence of IUGR and preterm delivery among patients
with “unrestricted” activity compared with patients with “restricted” activity. The EGAs at delivery were 31.3 weeks' gestation
and 34.3 weeks' gestation, respectively. This retrospective
series included patients who were prescribed hospital bed rest as
well as limitation of activity at home (the group with restricted activity). If
no mention was made in the patient's record regarding
limitation of physical activity, she was classified as unrestricted. Of
the restricted activity group, 1 infant of 39 had IUGR. In contrast, 67% of
the infants of the unrestricted activity group had IUGR. In a retrospective study of 105 sets of triplets delivered between 1975 and 1984 in
Zimbabwe, Crowther and Hamilton97 reported on the impact of bed rest. Patients managed with bed rest in
the hospital had less PMR than the group managed as outpatients. A more liberal approach was reported by Newman and co-workers,18 which entailed restricting activity at home and limiting hospital admission
to strict indications. A total of 44% of their patients required
admission for obstetric complications, and 66.2% had preterm labor requiring
admission. The EGA at delivery for this group of 198 sets of triplets
was 33.6 weeks, with a perinatal survival of 95%. The largest published series of quadruplets21 was unable to provide an in-depth analysis of the impact of bed rest, but
it was almost universally applied. We recommend that decreased physical activity be applied universally to
higher-order multiple gestations after 20 to 24 weeks, with hospital
admission indicated only by a complication and not for prophylaxis of
preterm labor. HOME MONITORING OF UTERINE ACTIVITY. The technique of home monitoring of uterine contractions and the concomitant
use of telephone lines to relay the information obtained is being
evaluated for its utility in the diagnosis of preterm labor that may
not be apparent to the patient or her clinical care givers. Because
of the acknowledged risk of preterm labor in higher-order multiple gestations, this
technique might logically be considered as having a key
role in the early recognition of such a complication. In the report by Newman and co-workers,18 all patients were managed with this technology. Outcomes in this study, however, were
not different than those of other recent series in which
this system was not used universally or was not used at all.17 We encourage clinicians to evaluate each case separately. Until additional
studies help define the possible role of home monitoring in the recognition
of preterm labor and the prevention of premature birth, it is
too soon to draw conclusions. Assessment of Fetal Well-Being In addition to serial ultrasonography and the routine prenatal blood tests
that are performed on all gravidas, higher-order multiple gestations
require antenatal surveillance in the form of the nonstress test. The
use of this test in singletons and its predictiveness for well-being
have been well documented.98 The lack of similar data from higher-order gestations undergoing surveillance
makes it difficult to determine accurate sensitivity, specificity, and
negative and positive predictive values in the detection of higher-order
gestation fetal compromise. For example, it is not possible
to state with certainty when surveillance should be started; between 30 and 32 weeks
appears to be reasonable. A nonreactive nonstress test
should be pursued in a similar fashion as in singletons, with the exception
of the contraction stress test, which probably should not be included
as an alternative because of the possibility of triggering premature
labor. The biophysical profile is a reasonable alternative to the
contraction stress test. The results of an abnormal biophysical profile
should be interpreted as for singleton pregnancy. Some clinicians
use the biophysical profile as their routine antenatal surveillance test. The
nonstress test may be impractical in all instances because of
the difficulties of simultaneous assessment in three or more fetuses. Elliott and Finberg99 reported on 18 triplet and 6 quadruplet gestations monitored with biophysical
profiles. There were no stillbirths in this series; however, 25% of
these gestations were delivered because of nonreassuring biophysical
profile testing, all with good outcomes. Four gestations had poor
neonatal outcomes in the presence of normal biophysical testing. All
of these late pregnancies apparently had acute changes in their clinical
status. These investigators concluded that the biophysical profile
is a reliable technique for the assessment of fetal well-being in higher-order
multiple gestations. Umbilical Doppler blood flow analysis has received a great deal of attention. The
use of umbilical Doppler for surveillance has been reported
in three series of triplets. Giles and co-workers100 reported on 20 sets of triplets. Using continuous-wave Doppler, these
authors were able to predict all the cases of SGA as well as all stillborns. Similar
findings were reported by Rafla.101 Gaziano and colleagues reported on 94 twin and 7 triplet gestations.102 Abnormal Doppler findings were associated with delivery 3 to 4 weeks earlier
and increased morbidity and mortality when compared with fetuses
with normal Doppler results. Because of the high incidence of SGA in higher-order gestations, this technique
may play an important role in the surveillance of these patients. |