Incidence and Origin Oligohydramnios is defined as a decrease in the volume of amniotic fluid, relative
to the gestational age. The incidence in an unselected population
without membrane rupture ranges from 0.4% to 19%, depending on
the criteria used for diagnosis and the study population.33,39,40 Oligohydramnios onset may be either acute or chronic. Acute onset is most
commonly the result of membrane rupture, whereas chronic oligohydramnios
may reflect a structural abnormality of the fetal urinary tract
or a pathophysiologic response to chronic or intermittent fetal hypoxemia. Risk
factors for oligohydramnios are shown in Table 2. TABLE 2. Risk Factors for Oligohydramnios
Chronic and/or intermittent fetal hypoxemia Intrauterine growth retardation
Postterm pregnancy
Repetitive cord compression
Fetal anomalies Renal agenesis
Renal anomalies (e.g., multicystic dysplastic kidneys, polycystic kidneys)
Posterior urethral valves
Bilateral ureteropelvic junction obstruction
Twin-to-twin transfusion
Premature rupture of membranes
Pathogenesis Spontaneous premature rupture of membranes (PROM) is the most common cause
of acute oligo-hydramnios. The incidence of rupture of membranes before
term is approximately 1% to 2%. Vintzileos and colleagues found
that 35% of patients with PROM did not demonstrate a vertical amniotic
fluid pocket greater than 2 cm, and this figure did not vary with gestational
age.41 Chronic oligohydramnios may be the product of major fetal anomalies or
prenatal hypoxia. The importance of the contribution of fetal urine to
amniotic fluid volume is demonstrated by several fetal anomalies in which
there is either obstruction of the urinary tract or renal agenesis/dysfunction. These
anomalies are associated with decreased amniotic
fluid formation. Chronic or intermittent fetal hypoxia may also result in reduced amniotic
fluid volume. Chronic low-grade fetal hypoxia may be a consequence
of long-standing uteroplacental insufficiency or maternal hypoxia, whereas
prenatal cord compression may lead to either prolonged or repetitive
episodes of acute hypoxia of varying intensity and duration. Corroborative
evidence for this pathophysiologic process leading to oligohydramnios
exists in both animal and human models. ANIMAL MODEL. A redistribution of fetal cardiac output has been noted in pregnant ewes
made hypoxic, but controlled for carbon dioxide tension.42 An increased proportion of cardiac output was shunted to the brain, myocardium, and
adrenal glands (high-priority organs), with a decrease in
blood flow to the gut, musculature, spleen, lungs, and kidneys (low-priority
organs). Under ordinary circumstances, this decreased renal perfusion
would ultimately result in reduction of fetal urine production
and oligohydramnios. HUMAN MODEL. Support for redistribution of cardiac output away from the fetal kidneys
as the operative mechanism is also provided by several human observations. Wladimiroff
and Campbell measured hourly human fetal urine production
rate (HFUPR) by measuring bladder volume on two occasions 1 hour
apart.5 The increase in bladder volume was equated with the hourly production
rate. A normal curve of HFUPR versus gestational age in 92 normal pregnancies
from 30 to 41 weeks was established. Subsequently, 62 pregnancies
at risk for chronic uteroplacental insufficiency were studied; 47% had
HFUPRs below the fifth percentlie limit. Of the 29 fetuses with decreased
HFUPR, 18 (62%) had a birth weight less than the tenth percentile
for gestational age. Additionally, all nine subjects that delivered
infants whose weights were less than the fifth percentlie had HFUPRs
below the normal range. Oligohydramnios has been demonstrated in 3% to 54% of prolonged pregnancies, reflecting
differences in sonography criteria used.43,44,45,46,47 The pathogenesis is presumably similar to the mechanism causing a growth-retarded
fetus, because it is clinically recognized that prolonged
pregnancy is associated with uteroplacental insufficiency in approximately 10% of
cases. However attractive the theory of redistribution of flow is, there may be
additional operative mechanisms. In an animal model subjected to hypoxemia, glomerular
filtration was maintained despite decreased renal blood
flow.48 It was also observed that one or more episodes of fetal stress could result
in secretion of vasopressin as well as catecholamines.48,49 Secretion of vasopressin could result in significant antidiuresis and
reduction of fetal lung secretion, resulting in further diminution of
amniotic fluid.50 A final, hypothesized cause of unexplained oligohydramnios is amniotic
rupture with an intact chorion.51 The amniotic fluid could potentially be reabsorbed in the extra-amniotic
space, resulting in no loss of fluid per vaginam. Corroborative evidence for this process exists in amniotic band syndrome, in
which it is theorized that the fetus is partially extruded into
the extra-amniotic space. To date, no experimental confirmation of this
pathway for oligohydramnios has been provided. Regardless of the precise mechanism, the presence of oligohydramnios in
the absence of structural anomalies or membrane rupture suggests past
and possibly ongoing stress significant enough to have altered normal
physiological processes. Its presence also increases the risk for prenatal
cord compression. Unfortunately, it is not known what prognostic
significance one should attribute to the observation, particularly in
a pre-term fetus. Clinical Presentation and Diagnosis Before more widespread use of real-time ultrasonography, the diagnosis
of oligohydramnios was occasionally suspected on the basis of “soft” clinical
signs, including easily palpated fetal parts, inadequate
fundal height growth, and difficulty in ballottement of the fetal
head. Absence of amniotic fluid at the time of artificial rupture of
the membranes is also strongly suggestive of oligohydramnios and, in
the absence of a sonographic diagnosis, may be the first indication of
its presence. Although ultrasonography has provided a means of assessing the volume of
amniotic fluid, a consensus of criteria for sonographic diagnosis of
oligohydramnios has not been achieved. In early reports, amniotic fluid
volume was assessed subjectively, allowing for differences according
to gestational age. Subsequent investigators attempted to quantify amniotic
fluid volume by various techniques. Data presented in these studies
are listed in Table 3 and summarized below. TABLE 3. Ultrasonographic Assessment of Oligohydramnios
| | | | | | | Positive | Negative |
| | Largest Pocket | Oligohy- | Abnormal End | Sensitivity | Specificity | Predictive | Predictive |
Author | Population | Criteria | dramnios (%) | Point | (%) | (%) | Value (%) | Value (%) |
Crowley47 | >42 weeks | Subjective | 35 | Cesarean for | 100 | 68 | 12 | 100 |
(1980) | | | | “fetal distress”- | | | | |
Manning53 | Suspected | <1 cm | 24 | SGA | 84 | 97 | 90 | 95 |
(1981) | IUGR | | | | | | | |
Philipson40 | Unselected | Subjective | 4 | SGA | 16 | 97 | 40 | 91 |
(1983) | | | | | | | | |
Bottoms33 | Unselected | Subjective | 19 | SGA | 32 | 83 | 23 | 89 |
(1986) | | | | | | | | |
Hill39 | Unselected | <1 cm | 0 | SGA | 0 | 100 | - | 98 |
(1983) | | Subjective | 1 | SGA | 50 | 100 | 100 | 99 |
Haddick54 | Retrospective | <1 cm | 4 | SGA | 4 | - | - | - |
(1984) | SGA preg- | | | | | | | |
| nancy | | | | | | | |
Mercer68 | Retrospective | <1 cm | 3 | Apgar 5 <7 | - | - | 8 | - |
(1984) | unselected | | | | | | | |
Chamberlain55 | Referred for | Vertical | 3 | SGA | 13 | 98 | 25 | 95 |
(1984) | biophysical | 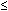 2 cm 2 cm | | | | | | |
| profile | | | | | | | |
Phelan46 | >41 weeks | <1 cm | 3 | Apgar 5 <7 | 25 | 98 | 29 | 97 |
(1985) | | | | Postmaturity | 3 | 97 | 17 | 83 |
Bastide69 | Referred for | Vertical | .7 | SGA | - | - | 37 | - |
(1986) | biophysical | <1 cm | | | | | | |
| profile | | | | | | | |
Patterson56 | Risk for malnu- | Average | 15 | SGA | 40 | 91 | 50 | 86 |
(1987) | trition | <3.2 cm | | | | | | |
Hashimoto44 | >42 weeks | “Volume” | 46 | Postmature | 90 | 64 | 36 | 97 |
(1987) | | <60 | | | | | | |
Rutherford57 | “High risk” | Sum of 4 | 8 | Cesarean for | 30 | 93 | 11 | 98 |
(1987) | pregnancy | vertical | | “fetal dis- | | | | |
| | quadrants | | tress” | | | | |
| | <5 cm | | | | | | |
Silver45 |  41 weeks 41 weeks
| Mean of 3 | 54 | Delivery for | 79 | 55 | 41 | 87 |
(1987) | | vertical | | nonreassuring | | | | |
| | <3.8 cm | | fetal heart rate | | | | |
| | | | trace | | | | |
Varma59 | “At risk” | Vertical | | SGA | - | - | 39 | 92 |
(1988) | pregnancy | <2 cm | 3 | | | | | | Subjective Oltrasonographic Evaluation of Amniotic Fluid Volume Crowley used subjective criteria to evaluate amniotic fluid volume in pregnancies
after 42 weeks, looking for the presence or absence of anechoic
space between fetal limbs and uterine wall, as well as between limbs
and the fetal trunk.47 Philipson and colleagues used the subjective criteria of paucity of amniotic
fluid, crowding of the fetal parts, and “poor fluid/fetal
interspace.”40 Projecting these criteria to a theoretical study population in predicting
small for gestational age (SGA) infants, the sensitivity was 15.5% and
positive predictive value was 39.6%. Bottoms and associates subsequently
compared a five-tiered subjective evaluation (oligohydramnios, decreased, normal, increased, hydramnios) to an objective measurement
of maximum vertical pocket diameter, the latter measured with the transducer
held at right angles to the sagittal plane of the maternal abdomen.33 Using SGA infants as an abnormal end point, the sensitivity and positive
predictive values were similar between the two techniques (32% versus 31%, and 83% versus 82%, respectively). Similarly, Goldstein and Filly
also demonstrated good correlation between subjective and objective
evaluations of amniotic fluid volume.52 Semi-Quantitative Ultrasonographic Assessment of Amniotic Fluid Volume Manning and colleagues were among the first to describe and popularize
semi-quantitative analysis of amniotic fluid volume. In 1981, Manning
determined “qualitative” amniotic fluid volume in a selected
high-risk patient population.33 Subjects included were those with suspected intrauterine growth retardation (IUGR) based
on fundal height measurements. Volume was arbitrarily
classified as decreased if the largest fluid pocket measured less than 1 cm
in broadest dimension. Twenty-four percent of these subjects
were found to have decreased amniotic fluid volume, and 90% of these were
delivered of babies that were found to be SGA. Conversely, 84% of
SGA infants were observed to have had decreased fluid. Although Manning's group deserves much of the credit for suggesting
a clinical value for diminished amniotic fluid volume in the overall
assessment of fetal status, subsequent studies were less optimistic, showing
both a lower prevalence and sensitivity of' oligohydramnios as
a predictor of IUGR.33,39,40,54 Manning's group subsequently re-evaluated the 1 cm rule in 1984.55 Qualitative amniotic fluid volume was recorded in all patients referred
for a biophysical profile by measuring the vertical and transverse dimension
of the largest amniotic fluid pocket, with the transducer oriented
perpendicular to the contour of the uterus. Vertical diameters less
than 1 cm were classified as decreased, 1 to 2 cm as marginal, and
greater than 2 cm to less than 8 cm as normal. Nine-tenths of 1% had
decreased and 2% had marginal amniotic fluid. As a result of improved
sensitivity in detecting IUGR by including the marginal category (5.5% for
decreased, 13.2% for decreased plus marginal groups), it was suggested
that the 1 cm rule might be too stringent. Subsequently, the amniotic
fluid component of the biophysical profile has been modified to
a 2 cm cutoff in two perpendicular planes. In addition to Manning's 2 cm rule, other objective techniques of
amniotic fluid volume have been evaluated. Patterson and colleagues measured
the vertical and two horizontal dimensions of the largest fluid
pocket and calculated a mean value of the three dimensions.56 Only pockets that were free of umbilical cord and extremities were included. By
using a receiver operating characteristic curve, a statistical
tool that is employed to maximize sensitivity and specificity, an average
dimension cutoff of 3.2 cm was established. Using this value, 15% of
a study population “at risk for fetal malnutrition” was
abnormal. The 3.2-cm cutoff was 40% sensitive and 91% specific, with
a 50% positive predictive value and 86% negative predictive value for
detecting SGA infants. Observed differences in average fluid volume
were more likely to be due to true differences between patients and not
due to measurement error; measurement of the average dimension of the
largest amniotic fluid pocket had an interpatient variability that
was fourfold higher than the intraobserver variability. In contrast, use
of maximum vertical diameter had an intraobserver variability that
was higher than the interpatient variability. The authors concluded that
average amniotic fluid volume was more reproducible than the largest
vertical diameter and would be a superior screening test to identify
malnourished fetuses. Phelan and colleagues introduced the four-quadrant technique of amniotic
fluid volume assessment in pregnancies from 36 to 42 weeks.43 With the transducer held in a sagittal plane perpendicular to the floor, the
largest vertical diameter in each quadrant was measured and summed. This
number, in centimeters, was termed the amniotic fluid index (AFI). Between 36 and 40 weeks, the average AFI was 12.4 -+ 4.6 cm. Whereas
two standard deviations below and above the mean would have
resulted in statistical cutoffs of 3.7 and 22.1 cm, respectively, the
authors used threshold values of 5 cm to define decreased amniotic fluid
and 20 cm for excessive fluid. Further investigation by these authors
demonstrated a significant increase in meconium-stained fluid, cesarean
section, and low Apgar scores in subjects with AFI less than 5 cm.57 Moore and Cayle subsequently assessed the amniotic fluid index in 791 normal
pregnancies between 16 and 42 weeks.58 Since significant differences were observed between the preterm, term, and
postdates pregnancies, a finding that is consistent with physiologic
fluid changes that occur throughout gestation, the data was stratified
by week of gestation. The mean AFI value at each week of pregnancy, as
well as the 90% to 95% confidence intervals, was calculated (Table 4). This study demonstrated the importance of establishing gestation-specific
norms for the AFI, rather than a single cutoff value. Interestingly, the 2.5th
percentile AFI value at each gestational age was greater
than the 5 cm threshold established by Phelan.43 Therefore, the use of the 2.5th percentile cutoff would result in a more
frequent diagnosis of oligohydramnios. It remains to be determined
if implementation of either the 2.5th or 5th percentile threshold would
reduce the positive predictive value and increase the number of unnecessary
interventions for oligohydramnios. Additional studies are needed
to assess the clinical significance of Moore and Cayle's data
before widespread clinical usage can be recommended. TABLE 4. Amniotic Fluid Index Values in Normal Pregnancy (in mm)
| Amniotic fluid index percentile values |
Week | 2.5th | 5th | 50th | 95th | 97.5th | n |
16 | 73 | 79 | 121 | 185 | 201 | 32 |
17 | 77 | 83 | 127 | 194 | 211 | 26 |
18 | 80 | 87 | 133 | 202 | 220 | 17 |
19 | 83 | 90 | 137 | 207 | 225 | 14 |
20 | 86 | 93 | 141 | 212 | 230 | 25 |
21 | 88 | 95 | 143 | 214 | 233 | 14 |
22 | 89 | 97 | 145 | 216 | 235 | 14 |
23 | 90 | 98 | 146 | 218 | 237 | 14 |
24 | 90 | 98 | 147 | 219 | 238 | 23 |
25 | 89 | 97 | 147 | 221 | 240 | 12 |
26 | 89 | 97 | 147 | 223 | 242 | 11 |
27 | 85 | 95 | 146 | 226 | 245 | 17 |
28 | 86 | 94 | 146 | 228 | 249 | 25 |
29 | 84 | 92 | 145 | 231 | 254 | 12 |
30 | 82 | 90 | 145 | 234 | 258 | 17 |
31 | 79 | 88 | 144 | 238 | 263 | 26 |
32 | 77 | 86 | 144 | 242 | 269 | 25 |
33 | 74 | 83 | 143 | 245 | 274 | 30 |
34 | 72 | 81 | 142 | 248 | 278 | 31 |
35 | 70 | 79 | 140 | 249 | 279 | 27 |
36 | 68 | 77 | 138 | 249 | 279 | 39 |
37 | 66 | 75 | 135 | 244 | 275 | 36 |
38 | 65 | 73 | 132 | 239 | 269 | 27 |
39 | 64 | 72 | 127 | 226 | 255 | 12 |
40 | 63 | 71 | 123 | 214 | 240 | 64 |
41 | 63 | 70 | 116 | 194 | 216 | 162 |
42 | 63 | 69 | 110 | 175 | 192 | 30 | (Moore TR, Cayle JE: The amniotic fluid index in normal human pregnancy. Am
J Obstet Gynecol 162:1168, 1990)Comparison of Ultrasonographic Assessment of Amniotic Fluid Volume To date, no single method to assess amniotic fluid volume has proved to
be the most valuable clinically. Difficulty in comparing fluid assessment
methods arises from differences in the population tested, the abnormal
end point chosen, and the variety of ultrasonographic criteria. Manning's 2 cm
rule appears to be most widely used, predominantly
as a component of the biophysical profile. Recently, however, the amniotic
fluid index has appeared with increasing frequency in the literature
and in clinical practice. The AFI, by measuring all four quadrants, would
appear to more accurately assess serial changes in fluid volume
over time, compared to a single vertical pocket, which might be subject
to greater variation due to fetal positioning. Additionally, by using
gestation-specific norms, the AFI may more accurately reflect abnormalities
in fluid volume compared to the 2 cm rule. However, the AFI
has not been evaluated as extensively in identifying the fetus at risk
for IUGR, cord compression, and abnormal perinatal outcome. By comparison, the
use of subjective criteria, which may be less dependent on
fetal positioning in serial testing, relies more on a gestalt of fluid
volume than on any one measurement value. As a result, the experience
of the examiner may be more critical in determining if the amniotic fluid
is appropriate for the gestational age, as the same subjectively
normal amniotic fluid volume at 42 weeks might be decreased for 34 weeks. Additionally, subjective criteria may vary from individual to individual, making
interobserver communication and statistical comparisons
more difficult to express. Inconsistencies in Ultrasonographic Assessment of Amniotic Fluid Volume Difficulties arise when comparing various criteria for oligohydramnios. One
variable not addressed in the majority of studies is the inclusion
or exclusion of fluid pockets that contain loops of umbilical cord. With
oligohydramnios, the umbilical cord makes up an increased proportion
of fluid pockets. At the Thomas Jefferson University Hospital, amniotic
fluid pockets containing cord are excluded only if there is little
amniotic fluid surrounding the cord. If free fluid can be identified
with occasional loops of cord, these pockets are not excluded. A frequently overlooked but critically important issue is that of transducer
positioning. In some reports, the transducer was held at right angles
to the uterine contour,55,59 whereas in others the plane of the ultrasound was perpendicular to the
floor or sagittal plane of the abdomen.33,43 Many studies did not indicate how the transducer was oriented. Orientation
is critical in evaluating vertical diameter. If the transducer is
held perpendicular to the uterine contour, a view from the lateral aspect
of the uterus might falsely create a vertical pocket on the ultrasonography
screen. For the sake of consistency, it is recommended that
the transducer be oriented longitudinally and perpendicular to the plane
of the floor (the plane in which the fluid has layered), thereby minimizing differences
if the subject is laterally displaced. Clinical Significance of Oligohydramnios The literature suggests that oligohydramnios does increase risk in a fetus
with no major anomalies. However, the clinical significance of oligohydramnios
differs between studies. depending on criteria used and end
points evaluated. Overall, decreased amniotic fluid is associated with
a higher incidence of SGA infants (less than the tenth percentile
for gestational age), postmaturity syndrome, variable and late decelerations
in labor, cesarean section for nonreassuring fetal heart rate tracing, lower
umbilical artery pH, lower Apgar scores, and higher perinatal mortality. Second-trimester
oligohydramnios is especially associated with adverse perinatal outcomes, as
a result of both pulmonary hypoplasia and lethal congenital anomalies .60 The relative degree to which the increased morbidity results from either
the underlying condition producing the oligohydramnios or from a direct
effect of the reduced fluid (i.e., umbilical cord compression) has not been determined. However, there
is some suggestion that part of the risk of cord compression may be reversible, as
indicated by studies in which fluid was removed versus those
in which fluid was replaced (amnioinfusion) to determine clinical
effect. Gabbe and colleagues noted that removal of amniotic fluid from
the amniotic cavity of fetal monkeys resulted in variable decelerations
secondary to cord compression.61 This pattern resolved after amnioinfusion. Confirmation of this finding
in humans has been demonstrated by Miyazaki and associates, who observed
a significant diminution of intrapartum variable decelerations in 5 1% of
patients treated by amnioinfusion through an intrauterine pressure
catheter.62 Nageotte and co-workers observed a significantly lower rate of variable
decelerations and higher cord pH values in patients who had PROM and
underwent prophylactic amnioinfusion.60 Pulmonary hypoplasia, as measured by low wet lung weights, low lung DNA
content, and low radial alveolar counts, can occur after PROM and oligohydramnios
in the very preterm gestation (<24 weeks).64 It may result from limitation of lung expansion secondary to prolonged
external compression, inhibition of fetal respiratory movements, and
lack of fluid circulation into the terminal alveoli, which may require
growth factors contained in amniotic fluid that are critical for alveolar
development.65 In one study of PROM in which pulmonary hypoplasia was observed, the majority
of cases were less than 26 weeks at the time of membrane rupture, suggesting
that the developing terminal air sacs are more susceptible
to the damaging effects of oligohydramnios.66 Further, prolonged oligohydramnios increases the risk of Potter's
syndrome, which, in addition to pulmonary hypoplasia, includes fetal
skeletal and facial deformities due to prolonged external compression .65 Antepartum Management of Spontaneous Oligohydramnios In the absence of membrane rupture or fetal urinary obstruction, there
is no known direct treatment for antepartum oligohydramnios, aside from
general measures to improve uteroplacental blood flow (e.g., left-sided bed rest). Oligohydramnios in the absence of major congenital
anomalies may be a marker for prior fetal adjustment to chronic uteroplacental
insufficiency or partial cord occlusion, as well as a predisposing
factor for cord compression. Therefore, it is generally recommended
that, depending on gestational age, these patients be either
followed closely with serial biophysical testing (nonstress test, biophysical
profile, or contraction stress test) including assessment for
the presence of variable decelerations, or else delivered. However, when
oligohydramnios is present, there is no consensus at this time about
a critical diagnosis-to-delivery interval. In the presence of marked
oligohydramnios at term, delivery should be initiated within 24 to 48 hours
after diagnosis, particularly in the presence of associated findings
such as spontaneous variable decelerations or a positive contraction
stress test. Further study is indicated to determine the benefits
of such an approach on both short- and long-term morbidity. Oligohydramnios resulting from congenital urinary tract obstruction (e.g., posterior urethral valves) may be treated, especially in a preterm gestation, by
sonographically directed procedures that divert urine from
the bladder to the amniotic cavity.67 This procedure may be a useful temporizing measure to decompress the bladder, potentially
preventing further damage to the fetal kidneys, and
to alleviate oligohydramnios, while allowing the fetus to mature in utero. Further experience is necessary to establish the safety and usefulness
of this procedure. Intrapartum Management Oligohydramnios increases the risk of cord compression during labor; consequently, the
fetus should be followed closely for variable decelerations, as
well as late decelerations secondary to uteroplacental insufficiency. | 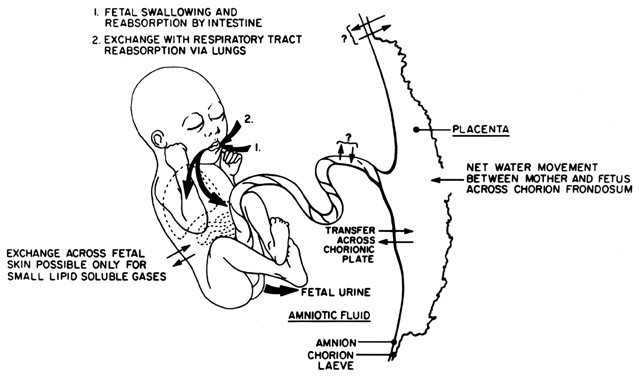
 2 cm
2 cm 41 weeks
41 weeks