In young girls, abnormal ovarian function manifests clinically as the lack of, or the delayed appearance of, secondary sexual characteristics or delayed menarche.10 For most young girls, menarche occurs between the ages of 9 and 16, with thelarche and pubarche preceding the onset of menses by about 1 year. Absence of signs of puberty by age 14 suggests delayed puberty or abnormal ovarian function and warrants medical consultation.
Etiology
In general, primary amenorrhea may be caused by gonadal or extragonadal malfunction. A detailed description of the various genetic and developmental aberrations is given in the appropriate chapters. Here, such aberrations will be described only in general terms sufficient for a diagnosis. The etiologic classification of primary amenorrhea is summarized as follows:
- Gonadal abnormalities
- Gonadal dysgenesis (Turner's syndrome)
- Pure gonadal dysgenesis
- XY gonadal dysgenesis (Swyer's syndrome)
- Mixed gonadal dysgenesis
- Ovarian insensitivity syndrome (Savage's syndrome)
- 17 α-hydroxylase deficiency
- Chronic functional anovulation of pubertal onset
- Gonadal dysgenesis (Turner's syndrome)
- Extragonadal anomalies
- Congenital absence of the uterus and vagina
- Male pseudohermaphroditism
- Female pseudohermaphroditism
- Abnormal hypothalamic-pituitary function
- Congenital absence of the uterus and vagina
GONADAL ABNORMALITIES.
In about 60% of patients with primary amenorrhea, the cause is failure of gonadal differentiation or inappropriate gonadal function during early fetal and neonatal development.11 As a result, the external genitalia fail to mature, or they are inappropriate for the genetic sex of the patient. In about 40% of women with primary amenorrhea, the cause is either gonadal dysgenesis or gonadal failure in phenotypic females who are actually genetic males.11 The following is a brief review of the clinical conditions in this category.
Gonadal Dysgenesis (Turner's Syndrome).
Gonadal dysgenesis designates the most common error in fetal gonadal differentiation, with an incidence of about 1 in 2,700 newborn phenotypic females.11
A spectrum of sex chromosome karyotypes ranging from 45,X to 45,X/46,XX and 45,X/46,XY has been described in these patients. Short stature (less than 150 cm tall) is the principal clinical finding. Such anomalies as webbed neck, shield chest, a high arched palate, a low hairline on the neck, and cubitus valgus may or may not accompany the diminished stature. Other anomalies seen include cardiovascular and renal malformations. The gonads are replaced by tenuous streaks of fibrous stroma lacking either follicles or tubules containing germ cells. In most instances, sex chromosomal aberrations are found in karyotypes prepared from cultures of somatic cells from such patients. Because of the possible presence of a Y-chromosome component12 and the risk of malignant degeneration of the streak containing the Y chromosome, it is important to screen all patients with gonadal dysgenesis. Use of currently available fluorescent techniques to identify the Y body and immunologic determination of H-Y antigen may help identify patients at risk for dysgenetic gonadal tumors.13
Pure Gonadal Dysgenesis.
This term is used to distinguish sexually immature girls who appear normal and who are taller than 150 cm from those with typical Turner's syndrome. It encompasses a more heterogeneous group of patients, with different etiologies implicated in ovarian failure. Many of these patients have a 46,XX or 46,XY karyotype. Patients with a normal chromosomal component tend to be tall, because the epiphyses stay open in the absence of ovarian steroids. The gonads are similar to the rudimentary streak gonad seen in Turner's syndrome. The distinction between the two is clinically important, because patients with pure gonadal dysgenesis have a higher incidence of presence of a Y chromosome. The syndrome also occurs more frequently in siblings than does classic Turner's syndrome.14
XY Gonadal Dysgenesis (Swyer's Syndrome).
Affected persons have an XY chromosomal component, but phenotypically they are feminine, with normal female internal and external genitalia and streak ovaries. Because of the high frequency of malignant degeneration, persons with XY forms of gonadal dysgenesis should undergo prophylactic excision of the rudimentary gonads.
Mixed Gonadal Dysgenesis.
This term refers to the rare anomaly of asymmetrical gonadal development, with a germ cell tumor or testis on one side and a streak or no gonad on the other side.15 Such persons usually are mosaics with X/XY karyotypes. They have anomalous external genitalia and exhibit virilization at or after puberty. The Y-containing gonad should be removed as soon as possible.
Ovarian Insensitivity Syndrome (Savage's Syndrome).
Patients with ovarian insensitivity syndrome are normally developed but appear to have functional primary ovarian failure.16 On ovarian biopsy, large numbers of primordial follicles are found. It is speculated that because of an ovarian cell membrane gonadotropin-receptor defect or postreceptor protein defect, the ovary cannot respond to the gonadotropic stimulus.17
The resistant ovary syndrome may be an early stage of ovarian failure in which there is maturation arrest of the follicles that will eventually disappear.18
Hypergonadotropic hypogonadism is characterized by decreased gonadal function due to the inability of the gonads to respond to pituitary gonadotropins. Hypergonadotropic hypogonadism in females has many causes, including the gonadal dysgenesis syndromes discussed above and abnormalities of the ovarian receptors for pituitary gonadotropins. Such an abnormality can be associated with a mutation of the luteinizing hormone (LH) receptor gene, leading to LH resistance as a cause of primary amenorrhea.19 On histologic analysis of the ovary, follicles are seen at all developmental stages, suggesting that in humans LH is necessary for ovulation but follicular maturation can occur in the presence of follicle-stimulating hormone (FSH) alone.
17 a-Hydroxylase Deficiency.
Impairment of 17-hydroxylation, an extremely rare cause of primary amenorrhea, results in failure to produce androgens, estrogens, and some adrenal steroids. As a consequence of this abnormality in steroidogenesis, these patients have increased levels of desoxycorticosterone and progesterone. Clinically, these girls exhibit sexual infantilism, primary amenorrhea with elevated gonadotropins, and hypertension with hypokalemic alkalosis.20 The metabolic derangement responds to glucocorticoid replacement therapy, but ovarian function cannot be restored, probably because the joint action of gonadotropins and estrogens is required for normal follicular maturation.21
EXTRAGONADAL ANOMALIES.
Extragonadal anomalies account for about 40% of primary amenorrhea cases.11 The gonads in these patients usually are normal and functioning. If gonads are nonfunctional because of lack of gonadotropic stimulation, ovulation can be induced with exogenous gonadotropins.
Congenital Absence of the Uterus and Vagina.
When pubertal changes occur at the appropriate age and secondary sexual characteristics have developed normally but menses have not appeared, primary consideration should be given to the genital tract as the locus of the problem. For unknown reasons, in some genetic females the anlagen of the müllerian ducts or the urogenital sinus do not develop or develop abnormally. In such persons, the external genitalia are normal, but the fallopian tubes, uterus, and upper third of the vagina are absent. The direct cause of congenital anomalies of the female genital tract is unknown. Studies have suggested an association of an autosomal dominant gene, polygenic, or multifactorial factors with müllerian agenesis. Environmental factors, including radiation, intrauterine infections, and medications, have also been linked to genetic anomalies. The possible presence of müllerian-inhibitory-like substance early in development has been suggested.22 An immune etiology or an association with collagen vascular disease has also been suggested.23 In cases of aplastic urogenital sinus, the internal genitalia are normal but the lower two thirds of the vagina fails to develop. Various intermediate anomalies also occur. Congenital absence of the uterus and vagina (Mayer-Rokitansky-Kuster-Hauser syndrome) is the most common defect, with an estimated frequency at birth of 1 per 4,000 females.24 In about 10% of these cases, vaginal aplasia is associated with a functionally normal uterus and cervix. Congenital absence of the cervix associated with a functional uterus is extremely rare.25 Müllerian duct agenesis is often associated with urinary tract anomalies and musculoskeletal malformations.26
When the uterus is absent, the most common complaint is primary amenorrhea. Because of normal ovarian function, the physical development and appearance of these girls is normal. Conversely, when the uterus is present and the vagina or parts of it are absent, menarche appears at the normal age, but the menstrual effluent is retained, producing endometriosis and cyclic abdominal pain without external evidence of menses.25
Diagnosis of such conditions is made during physical examination. When the defect consists of an imperforate hymen only, a simple hymenotomy will restore normal menstrual function. When the defects are more extensive, however, the treatment may be more complex. Transverse vaginal septum, resulting from failure of canalization of the distal third of the vagina, is not always recognized.27 It leads to proximal hematocolpos and hematometra. The symptoms are cyclic lower abdominal pain and bladder irritability. Examination shows a firm pelvic mass that varies in size and is not always symmetrical in outline. Vaginal inspection reveals a short vagina and no cervix. The upper vagina may be quite distended. Treatment involves excision of the septum and mobilization of the upper vagina so that it can be connected to the lower vagina or perineum. Occasionally, a split-thickness skin graft is required.
When the uterine cervix is absent in a patient with vaginal anomalies, the treatment of choice is total abdominal hysterectomy, because attempts at plastic reconstruction of a functional vagina and a patent outflow tract have met with little success.25 Although there are several reports in which preservation of the uterus in association with partial or complete vaginal agenesis resulted in a successful pregnancy, evaluating the condition of the cervix is critical before making a definitive surgical plan. The uterus should be removed in women with cervical atresia, but the uterus can be conserved if the cervix is stenotic. In this procedure, a modification of the McIndoe split-thickness skin graft operation can be used to create a neovagina in conjunction with cervical and vaginal stents.28
Male Pseudohermaphroditism.
Pseudohermaphroditism resulting from inadequate or inappropriate masculinization of the urogenital sinus and external genitalia may be caused by enzymatic deficiencies in gonadal or adrenal steroidogenesis. In such persons, incomplete masculinization of the urogenital sinus and external genitalia gives rise to incomplete male pseudohermaphroditism, which may present clinically as primary amenorrhea. The most common cause of this condition is the testicular feminization syndrome, characterized by normal female external genitalia, a blind vaginal canal, absent uterus, sparse to absent pubic and axillary hair, and well-developed breasts with immature nipples and hypopigmented areolae.29 On physical examination, gonads may be palpable in the inguinal canal, or frequently there is a history of inguinal herniorrhaphy. Subjects with testicular feminization have normal or only slightly elevated serum gonadotropin levels and normal male testosterone levels, but because the cytosol receptors for testosterone are defective, testosterone is biologically ineffective.30 Such persons are always raised as females and come to the physician because of primary amenorrhea or infertility.
Other forms of male pseudohermaphroditism associated with various degrees of virilization31 are discussed in detail elsewhere in these volumes.
Female Pseudohermaphroditism.
Extraovarian sources of androgen may virilize the external genitalia in genetically normal females with normal internal genitalia. Congenital adrenal hyperplasia is the most common cause. Excessive adrenal androgen secretion is usually associated with defective cortisol synthesis due to 21-hydroxylase or 11 β-hydroxylase deficiency.32 In female fetuses with such deficiencies, the excessive adrenocortical androgens virilize the external genitalia to various degrees during fetal life. Generally, these infants show symptoms of adrenocortical insufficiency and are diagnosed and appropriately treated during the neonatal period. Elevated 17-hydroxyprogesterone levels in the blood or increased pregnanetriol in the urine confirms the diagnosis. It is most important to examine the nuclear chromatin or karyotype before assigning a sex to the infant. Although some of these patients may menstruate and ovulate, most are amenorrheic or oligomenorrheic. However, when adequately treated, they resume normal menstrual function.32 Other rare causes of androgen overproduction are virilizing adrenal and ovarian tumors.
Abnormal Hypothalamic-Pituitary Function.
Central nervous system and pituitary lesions in preadolescents may be a cause of primary amenorrhea. Failure of the pituitary to secrete sufficient amounts of gonadotropins results in failure of follicular development and maturation, lack of gonadal steroids, and therefore delayed sexual development and amenorrhea. Such failure may result from inadequate hypothalamic stimulation or primary pituitary disease. Usually these conditions are associated with low gonadotropin levels and are therefore called hypogonadotropic hypogonadism. Several well-known syndromes are included in this category. Kallmann's syndrome (olfactogenital dysplasia),33 pituitary dysfunction manifested by isolated gonadotropin deficiency,34 and destruction of the anterior pituitary by neoplasms or metastases all result in hypogonadotropic hypogonadism. Nonpituitary intracranial space-occupying mass lesions are uncommon causes of primary amenorrhea or galactorrhea.35 Craniopharyngiomas account for one fourth of neoplasms in the pituitary regions. These tumors arise from epithelial remnants of Rathke's pouch and can be associated with hypopituitarism and hyperprolactinemia. The tumors may be found within the third ventricle, hypothalamus, and sella. Pituitary adenomas are a more common cause of secondary amenorrhea, and there is an increased incidence in the fourth decade.
Clinical Evaluation
HISTORY.
A detailed history is paramount in evaluating the patient with amenorrhea. Particular attention should be paid to family and developmental history, the patient's prenatal history, ingestion of drugs, and exposure to chemicals and radiation. Menstrual histories of mother, aunts, and sisters should be recorded. The chronologic development of pubertal changes should be carefully noted, because anomalies may point to the diagnosis. For example, normal thelarche and pubarche are seen with müllerian duct aplasia, whereas lack of axillary and pubic hair in conjunction with good breast development suggests testicular feminization. Information about dietary habits and changes in body weight should be obtained through careful questioning. Psychosocial history is of considerable importance because excessive stress may cause amenorrhea.
PHYSICAL EXAMINATION.
Complete physical and pelvic examinations are essential. Careful clinical observations can provide information that may eliminate the need for expensive laboratory tests. Special attention should be paid to evidence of sex steroid activity (e.g., adequate development of the breasts and pubic and axillary hair indicates normal ovarian function and points to an extragonadal cause for amenorrhea). A simplified clinical assessment of the etiology of primary amenorrhea is presented in Table 1.
TABLE 1. Clinical Differential Diagnosis of Primary Amenorrhea
Presence |
|
|
of Uterus | Breast Development | No Breast Development |
Present | Similar to secondary amenorrhea | Hypothalamic amenorrhea |
|
| Pituitary amenorrhea |
|
| Gonadal dysgenesis |
|
| 17α-hydroxylase deficiency (46,XX) |
Absent | Müllerian agenesis | Testicular regression |
| Androgen insensitivity syndrome | 17,20-desmolase deficiency |
|
| 17α-hydroxylase deficiency (46,XY) |
In general, attention should be paid to the following: androgen overproduction, cortisol overproduction, hypothyroidism, galactorrhea, acromegaly, weight changes, short stature with or without associated anomalies such as webbed neck and cubitus valgus, and sexual infantilism. Obvious signs of Turner's syndrome are easily detectable, but in cases of mosaicism the diagnosis may be difficult.36 Detailed clinical attention to the quality of the skin (oiliness, acne, dryness, abnormal pigmentation, or bruises), hair distribution, general nutritional status, size and consistency of the thyroid, breast development and presence of galactorrhea, and quality of the vaginal mucosa and cervical mucus can alert the physician to possible problems.
Additional important information is gained during the pelvic examination, when obvious genital malformations and anomalies can be detected. Because many patients with primary amenorrhea are youngsters who have never been examined gynecologically, the examination should be carried out with as little trauma as possible; if necessary, it should be done under anesthesia.
PROGESTERONE WITHDRAWAL TEST.
The progesterone withdrawal test, which indirectly reflects HPO activity, is frequently used to challenge the adequacy of endogenous estrogen production. The progesterone challenge must be performed with a “pure” progesterone devoid of intrinsic estrogenic activity. Usually we use 100 mg of progesterone in oil given intramuscularly, or medroxyprogesterone acetate (Provera), 10 mg/day orally for 5 days. Patients with adequate endogenous estrogens will bleed within 3 to 5 days after medication, indicating adequate endogenous estrogen stimulation of the endometrium. Patients with relatively low levels of endogenous estrogens may have a limited response to the progesterone challenge. If bleeding does not occur, more extensive studies are indicated.
LABORATORY TESTS.
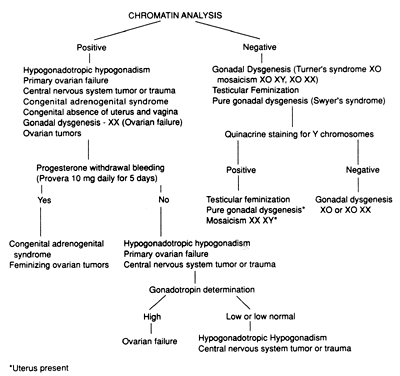
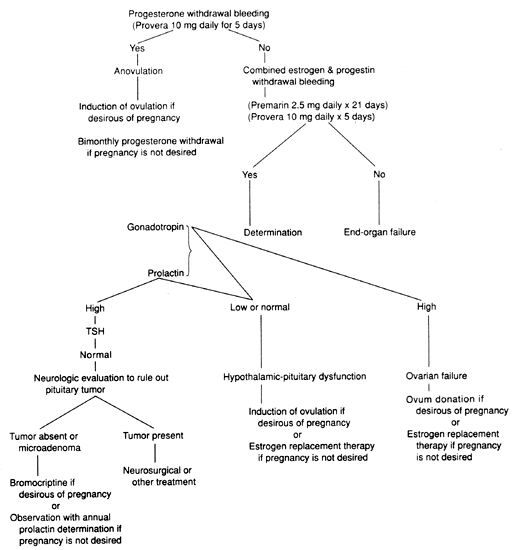
In general, few laboratory tests are needed to establish a diagnosis. Chromatin analysis (buccal smear), karyotyping with quinacrine mustard stain for the presence of a fluorescent chromocenter characteristic of the Y sex chromosome,37 immunologic determination of the H-Y antigen,38 and determination of serum gonadotropins and prolactin by radioimmunoassay are the tests most frequently required. The importance of a karyotype should not be underemphasized. A review of the literature of 33 cytogenetic studies composed of 1,757 phenotypic females with primary amenorrhea revealed a 32% incidence of chromosome abnormalities.22 Figure 1 gives a schematic outline of the laboratory workup.
|
At the initial examination, a buccal smear or blood karyotype is taken, blood is drawn for LH, FSH, and prolactin determination, and the patient is given progesterone intramuscularly or medroxyprogesterone orally for the progesterone challenge test. If bleeding occurs within 3 to 5 days, the diagnosis is probably anovulation, because bleeding indicates adequate endogenous estrogen levels and activity along the HPO axis. If bleeding does not occur and a uterus is present, gonadotropin levels and chromosome analysis will determine the diagnosis. High LH and FSH levels in the menopausal range indicate ovarian failure, whereas low or low-normal levels indicate hypothalamic or pituitary dysfunction. Patients with high levels of prolactin should have the pituitary evaluated by either magnetic resonance imaging or computed tomography.
The buccal smear is positive in genotypic females and negative in females with only one chromosome and in genotypic males. Chromatin-negative patients should be karyotyped and, if possible, their blood should be tested for the presence of H-Y antigen. In young chromatin-positive patients whose gonadotropins are elevated, karyotyping of several tissues (leukocytes, skin, gonads) may be helpful in determining the exact genetic aberration, because a normal karyotype from one tissue does not exclude the possibility of sex chromosome mosaicism or gonadal dysgenesis. In such cases, laparoscopic examination and ovarian biopsy and histologic and cytogenetic studies may be used to confirm the diagnosis.
A relatively small number of patients with primary amenorrhea have ambiguous external genitalia with considerable clitoromegaly. Karyotyping with quinacrine stain for the Y chromosome is essential in these cases. A Y chromosome indicates male pseudohermaphroditism, mixed gonadal dysgenesis, or true hermaphroditism.39 A final diagnosis can be made only by inspection and biopsy of the gonadal tissue.
In rare instances, ambiguous external genitalia are found in genetically normal females with congenital adrenal hyperplasia.40 Determination of urinary 17-ketosteroids, pregnanetriol, plasma testosterone, and 17-hydroxyprogesterone establishes the diagnosis. The finding of significantly elevated levels of plasma 17-hydroxyprogesterone and urinary pregnanetriol, suppressible with dexamethasone, confirms the diagnosis. With adequate adrenal suppression and plastic surgery of the external genitalia, these women can function normally.41,42
Virilizing ovarian or adrenal tumors that develop before menarche can cause primary amenorrhea and clitoromegaly. Although such tumors are extremely rare, they should be considered in the diagnosis of amenorrhea.
Treatment
Treatment of primary amenorrhea depends on its cause. The aims of treatment are two: to help the patient attain normal feminine physical development and to restore the patient's fertility potential. When the cause of amenorrhea is a gonadal or severe genital anomaly, little can be done to restore fertility. Estrogen replacement therapy will stimulate maturation of the secondary sexual characteristics, but correction of ambiguous genitalia and excision of the Y chromosome-containing gonads is required. In cases of testicular feminization, the gonads should be removed after puberty because they carry a 22% chance of malignancy.39 The possibility of virilization in testicular feminization is negligible due to inherited androgen insensitivity, and the estrogens produced by the gonads are necessary for physiologic pubertal changes. In all other instances in which a Y chromosome is present, gonadectomy should be performed before puberty to prevent virilization and masculinization after puberty, which may be biologically and psychosocially very distressing to a person raised as a female. Surgical correction of the external genitalia to provide functional and socially acceptable genitalia should be undertaken when feasible and required by the patient.
When amenorrhea is due to hypothalamic or pituitary disorders and the ovaries and genital organs are normal, the prognosis for childbearing is excellent. Estrogen replacement therapy will stimulate maturation and development of the secondary sexual characteristics. When pregnancy is desired, ovulation can be induced by gonadotropin therapy or, in hyperprolactinemic states, by bromocriptine.
Advances in in vitro fertilization-embryo transfer (IVF-ET) have expanded the reproductive alternatives for the woman with gonadal dysgenesis or müllerian agenesis. Ovum donation has allowed patients with Turner's syndrome to undergo IVF-ET with partner's sperm and their own uterus. Patients with müllerian agenesis may be candidates for a surrogate uterus. As there appears to be an increased prevalence of chromosomal aberrations in these patients,22 one should consider karyotyping them before an oocyte retrieval for an embryo transfer to a surrogate uterus.