Acquired Heart Disease in Pregnancy
Authors
INTRODUCTION
The hemodynamic changes of pregnancy may bring previously undiagnosed heart disease to clinical attention (see Chapter 11 of this subsection Pregnancy in the Woman With Pre-Existing Cardiovascular Disease). In addition, cardiac problems may arise during pregnancy and become complicated by the usual hemodynamic changes of pregnancy which may further complicate the course of the pregnancy. As with any other woman of childbearing age, the pregnant woman is not immune from acquiring cardiac problems, but the health of both the mother and fetus needs to be considered in diagnostic and treatment strategies.
This chapter focuses on common cardiac problems acquired during pregnancy. Although these diseases do not occur frequently, the pregnancy may be affected and specialized treatment strategies must be considered to safeguard maternal and fetal health. Most of the literature concerning cardiac disease arising during pregnancy has been gleaned from anecdotal experience or expanded case reports. In a study of 276 pregnancies in women with cardiac disease, the most common cardiac cause was congenital, but arrhythmias complicated 11% of the pregnancies.1 Acquired heart disease was most often caused by preexisting valvular heart disease. The most common cardiac complications were those of heart failure and arrhythmia. This discussion includes other forms of myocardial disease, coronary artery disease, endocarditis, aortic dissection, and pericarditis. Cardiac complications arising directly related to pregnancy as a result of hypertension or tocolysis are also discussed.
During pregnancy cardiac preload increases with expanded blood volume while afterload decreases because of systemic vasodilatation and the low resistance circuit within the placenta.2 Heart rate and stroke volume increase, and cardiac output nearly doubles. The gravida is hypercoagulable and therefore may also be at increased risk for thromboembolic events. The well-being of the fetus and the effects of medications on the fetal growth and development must also be considered. The cardiovascular effects of pregnancy are summarized in the Table 1. These changes may not completely resolve until 12 weeks' postpartum.3
Table 1. Hemodynamic effects of pregnancy
| Hemodynamic Parameter | Change | Peak Effect | Potential Signs and Symptoms |
| Cardiac output | Increases | 26 weeks | Hyperdynamic; S3; tachycardia |
| Heart rate | Increases | 3rd trimester | Palpitations; tachycardia |
| Stroke volume | Increases | 26 weeks | Edema; nocturia; cardiac chamber enlargement |
| Total peripheral resistance | Decreases | 20 weeks | Hypotension; edema; syncope |
| Erythrocyte volume | Increases but less plasma volume | Term | Physiologic anemia of pregnancy |
| Blood volume | Increases | 32 weeks | Edema; cardiac enlargement |
| Respiratory rate | Increases | 30 weeks | Hyperpnea; dyspnea |
| Coagulation | Increases | 3rd trimester | Thrombotic event |
Many of the symptoms that arise during a normal pregnancy are similar to those that occur in patients with cardiovascular disease. Women typically notice fatigue, chest pain, dyspnea, orthopnea, hyperpnea, palpitations, or vasovagal symptoms. However, it is important to be able to distinguish that which may be abnormal, such as any symptoms occurring at rest, exertional chest pain, exertional or severe dyspnea out of proportion to the activity being performed, progressive orthopnea, paroxysmal nocturnal dyspnea, tachycardia greater than 120 bpm, or a documented arrhythmia. Exertional or rest syncope may be caused by an underlying arrhythmia.4 Any of these symptoms merit further investigation for underlying cardiac or cardiopulmonary cause.
Typically abnormal signs such as neck vein pulsations, a diffuse or displaced apical pulse, splitting of the first heart sound with accentuation of the pulmonic component of the second heart sound due to increased flow, or a third heart sound, may be normal during pregnancy. A systolic murmur of grade 1–2 heard along the upper left sternal border is common in pregnancy and may occur in more than 90% of pregnant woman. There may be a venous hum. Sinus arrhythmia has been documented, and dependent edema in pregnancy has been reported commonly.4 Palpitations and tachycardia are often noticed because of the expected physiologic elevation in heart rate. Alternatively, it may be a result of the relative anemia of pregnancy, the generalized hypermetabolic state, or the deconditioned heart. However, abnormal signs during pregnancy include marked distention of the internal jugular veins. Although the heart is displaced laterally in the chest and the apex may move upward, there should not be cardiomegaly on palpation. A ventricular heave is also abnormal. A very loud pulmonic component of the second heart sound or wide splitting of the second heart is not an expected finding. The presence of a summation gallop requires investigation, as would a loud systolic murmur associated with a thrill located anywhere in the chest. Any diastolic murmur should be evaluated, because it would not be explained by the hemodynamic changes of pregnancy.4 Sustained arrhythmia, supraventricular arrhythmia, or ventricular arrhythmia should be further investigated for cause and treatment. Clubbing and cyanosis is always abnormal and is associated with underlying cyanotic congenital heart disease or a pulmonary process. Positional changes in blood pressure causing lightheadedness or near syncope may occur with compression of the inferior vena cava by the uterus later in pregnancy.5
Diagnostic testing may be affected by changes due to pregnancy. The 12-lead electrocardiogram tracing may be caused by the shift in position of the heart within the thoracic cavity. Because of this shift, there is a shift in the QRS axis and a Q wave may appear in the lead III on a 12-lead electrocardiogram.2 Sinus tachycardia often occurs because of anemia, deconditioning, or the hemodynamic state. Conduction system disease and arrhythmias may be diagnosed by the electrocardiogram. The QT interval may lengthen. Ambulatory electrocardiographic monitoring is indicated to detect arrhythmias occurring daily over a specific period of time (24–48 hours) or for more sporadic symptoms an event monitor can record rhythm changes for several weeks.
In a study of women who presented which heart murmurs during pregnancy, flow murmurs were diagnosed or confirmed by cardiac electrocardiography, which differentiated pathologic murmurs.6 An echocardiogram may appear abnormal during pregnancy because of the changes of pregnancy rather that the underlying pathologic condition. There may be normal or mildly improved left ventricular systolic function, because there is also an increase in systolic and diastolic dimensions. There is an increase in the tricuspid annulus diameter, resulting in a functional tricuspid regurgitation. In an echocardiographic study, valvular regurgitations specifically of the mitral, tricuspid and pulmonic valves were found during pregnancy.7 The most marked change compared with control patients was in the tricuspid valve and in the pulmonic valve, with less significant changes in the degree of mitral regurgitation. Two-dimensional echocardiography may detect chamber enlargement, ventricular dysfunction, or pericardial abnormalities. The Doppler echocardiogram can diagnose valvular hemodynamic abnormalities of regurgitation or stenosis. The velocity of tricuspid regurgitation may permit estimation of pulmonary artery pressure by the modified Bernoulli equation (velocity2 x 4). When combined with limited stress testing of the heart, echocardiography detects wall motion abnormalities caused by myocardial ischemia and assesses functional reserve of the ventricle without exposure to radionuclide isotopes. Transesophageal echocardiography is used to detect intraatrial thrombi, valvular vegetations, or intracardiac abscess in endocarditis. This process may require sedation. Magnetic resonance imaging demonstrates cardiac anatomy well but is best done after 18 weeks' gestation. Cardiac catheterization may be needed to diagnose and treat critical coronary disease but carries risk of radiation and should only be done if clinically indicated.
After the diagnosis of cardiac disease during pregnancy, general medical management may include limitation of physical activity or sodium restriction. The pregnant woman on strict bed rest may require prophylactic anticoagulation to prevent thromboembolic events, depending on the nature of the cardiac lesion. Environmental factors should be controlled by limiting exposure to toxins, irritants, or extremes of temperature. Tachycardia may be caused by an underlying infection, hyperthyroidism, or profound anemia and must be investigated, especially in a woman with impaired ventricular function.
During labor and delivery, hemodynamic changes of pregnancy interacting with the cardiac disorder must be considered. With each contraction, there is an increase in cardiac output and stroke volume that occurs as a 300–500-ml bolus of blood is ejected into the peripheral circulation. These changes appear to be attentuated when labor is in the left lateral decubitis position. Severe pain may exacerbate tachycardia. Management is determined by functional status. Women of the New York Heart Association (NYHA) functional class I and II are only symptomatic with activity and may require only general management and clinical observation (Table 2). They should have adequate analgesia, because cardiac dysfunction may be exacerbated by pain-induced tachycardia. Volume and blood pressure should be maintained. Women who are NYHA functional class III or IV or who have had pulmonary edema during the pregnancy may require invasive hemodynamic monitoring to assess intracardiac filling pressures and manage fluid status during labor, delivery, and postpartum. These patients may require oxygen administration. If hemodynamic monitoring has been deemed necessary during the pregnancy, it should be continued for at least 24 hours postpartum as fluid shifts occur. Prophylactic anticoagulation for deep venous thrombosis should be prescribed until the patient is ambulatory.
Table 2. New York Heart Association functional class and management of pregnancy
| Class | Definition | Management Issues in Pregnancy |
| I | Asymptomatic with normal activity | Clinical observation and appropriate fluid management |
| II | Symptomatic with physical activity | Clinical observation and appropriate fluid management |
| III | Symptomatic with most activities but asymptomatic at rest | Careful fluid and drug administration; hemodynamic monitoring |
| IV | Symptoms with minimal activity or at rest | Careful fluid and drug administration; hemodynamic monitoring |
Medical therapy choices during pregnancy in the woman with heart disease must consider the maternal and fetal effects. Specific drugs are contraindicated in pregnancy, such as angiotensin-converting enzyme (ACE) inhibitors, but most drugs have been designated category C by the US Food and Drug Administration (FDA). Category C drugs have been defined by animal studies that have revealed adverse effects on the fetus (e.g., teratogenic, embryocidal), but there are no control studies of women, or studies of women and animals are not available. The drug should be given only if the potential benefit justifies a potential risk to the fetus. Specific recommendations regarding drugs are determined by the specific cardiac disease and are discussed later. Ideally, therapy should be initiated after approximately 13 weeks, when organogenesis is complete. The lowest effective dose should be used, and the patient and fetus should be monitored for response and adverse effects.8
MYOCARDIAL DISEASE IN PREGNANCY
The pregnancy woman who develops myocardial disease usually presents in congestive heart failure or ischemia.9, 10 This may be due to previously undiagnosed coronary disease or cardiomyopathy, systemic illness or myocardial dysfunction due to pregnancy. Malignancy or chemotherapy, thyroid disease, hypertension,or alcohol or cocaine abuse may result in congestive heart failure due to the combination of the hemodynamic changes of pregnancy and myocardial dysfunction. There are reports of cardiomyopathy related to pheochromocytoma during pregnancy.11, 12 Women who have had prior doxorubicin or other anthracyclines for a childhood malignancy might have limited cardiac reserve before pregnancy without clinical evidence of impairment.13 Subclinical disease may manifest as the hemodynamic changes of pregnancy occur – specifically as stroke volume increases, resulting in increased preload, which may cause decompensation in the heart lacking functional reserve.
Cardiomyopathy and pulmonary edema
Pulmonary edema may be the initial manifestation of myocardial dysfunction due to systolic or diastolic dysfunction.14, 15, 16 The causes of congestive heart failure during pregnancy are summarized in Table 3. Acquired causes of systolic dysfunction during pregnancy may include viral myocarditis,17, 18 chronic hypertension,19 preeclampsia19, 20 or the use of tocolytic agents.19, 21, 22 Diastolic dysfunction or impaired ventricular compliance may occur with hypertrophic cardiomyopathy,23 chronic hypertension, or preeclampsia.20 Pulmonary edema may occur during a hypertensive crisis.24 In a study of patients presenting with pulmonary edema during pregnancy, 25% had systolic dysfunction, and 75% had diastolic dysfunction. The pulmonary edema occurred antepartum, and in 50% of patients, dexamethasone was a contributing factor.24 The wedge pressure and the central venous pressure may not correlate. When caused by hypertension or preeclampsia, there may be a low capillary wedge pressure found on hemodynamic monitoring.20 Pulmonary edema of pregnancy associated with chronic hypertension and systolic dysfunction on presentation carries a poor prognosis.25
Table 3. Causes of congestive heart failure during pregnancy
| Fluid overload |
| Acute myocarditis (viral) |
| Cardiomyopathy (secondary or idiopathic) |
| Myocardial infarction |
| Peripartum cardiomyopathy |
| Alcohol |
| Mitral stenosis |
| Aortic stenosis |
| Ventricular tachycardia |
| Atrial fibrillation |
| Preeclampsia or toxemia |
The diagnostic criteria for classic peripartum cardiomyopathy require congestive heart failure in the ninth month or within 5 months' postpartum; no evidence of preexisting heart disease; no identifiable cause such as fluid overload, tocolytic therapy, eclampsia or toxemia, or prior cardiac dysfunction documented by echocardiography; and an estimated ejection fraction of less than 45% or fractional shortening less than 30%.26 The end-diastolic dimension should be greater than 2.7 cm. Women present with chest pain, cough, orthopnea, paroxysmal nocturnal dyspnea, edema, or fatigue.27 Examination confirms heart failure with rales, sinus tachycardia, and a third heart sound. The cause of classic peripartum cardiomyopathy is unknown.26 Poor prognostic indicators for peripartum cardiomyopathy include a left ventricular end-diastolic dimension greater than 60 mm, fractional shortening less than 21%, no echocardiographic improvement despite treatment of 6 weeks, or symptoms persisting longer than 2 weeks despite medical therapy. Maternal age greater than 30 may not bode well.19, 27
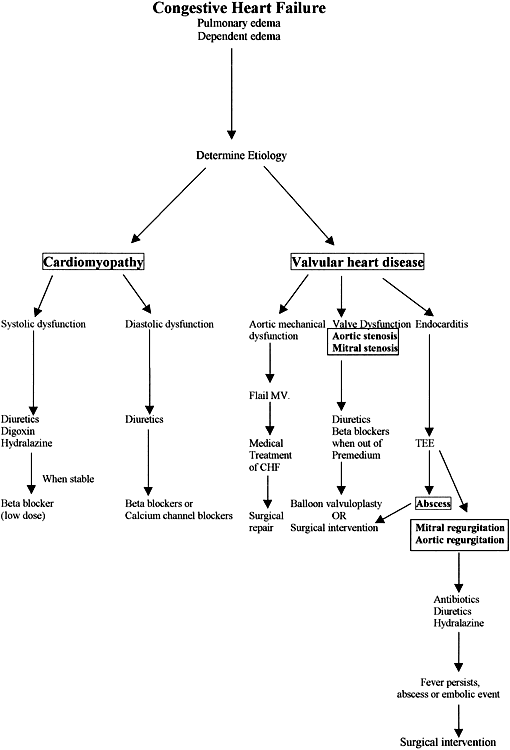
The treatment of pulmonary edema and congestive heart failure depends on the underlying cause (Fig. 1) but generally includes the use of diuretics, digoxin, and afterload reduction. Sodium restriction is effective in the early stages of congestive heart failure. Furosemide or torasemide use during pregnancy has been associated with hypovolemia, hypokalemia, hypomagnesemia, hearing loss, glucose intolerance, and interstitial nephritis. For early signs of mild congestive heart failure, a thiazide diuretic may be effective. Thiazide diuretics cross the placenta and are associated with maternal hypokalemia, volume contraction, pancreatitis, leukopenia, thrombocytopenia, and vasculitis. ACE inhibitors and angiotensin receptor blockers are often used to treat congestive heart failure but are contraindicated during pregnancy.28, 29 Hydralazine is preferred for vasodilation and afterload reduction. Adverse effects of hydralazine may include palpitations, flushing, headache, orthostasis, angina, hypotension with reflex tachycardia, and fetal thrombocytopenia.
Digoxin is recommended for treatment of congestive heart failure due to systolic dysfunction and has been used safely in pregnancy.29 Digoxin may slow the heart rate and cause conduction system disease. Anticoagulation with heparin may be indicated for the treatment of thromboembolic events, unstable angina, cardiomyopathy, or atrial fibrillation. It can be administered twice or three times daily.
The low-molecular-weight heparins may obviate the need for continuous blood testing, but their use for cardiac disorders has not been extensively reported.30, 31 With standard heparin therapy, there is an associated risk of bleeding, osteoporosis, and thrombocytopenia. Coumadin use has been contraindicated during pregnancy because of teratogenicity.
The prognosis for postpartum cardiomyopathy varies widely.32, 33 Strictly defined peripartum cardiomyopathy may not improve, and the patient may eventually require cardiac transplantation or, although clinically improved, may experience recurrence with subsequent pregnancies. Other causes may be associated with a better prognosis. Decisions regarding subsequent pregnancies should be made only after full recovery.34
Coronary artery disease
The older gravida at risk for coronary artery disease may first develop angina with pregnancy, although this is fortunately rare.34 Risk factors for coronary artery disease most often identified in this population are smoking and hypertension, but homocystinuria and diabetes may also be the cause.35, 36 Theoretically, women with anticardiolipin antibodies may be at risk for thrombotic events.37 Complications of anomalous coronary arteries may first arise during pregnancy.38
The evaluation and treatment of chest pain during pregnancy should proceed as during the nonpregnant state. The differential diagnosis includes aortic dissection, esophageal spasm, and a pulmonary process.39 Early in pregnancy, stress testing to a predetermined heart rate (140–150 bpm) may confirm coronary artery disease, especially when combined with echocardiography. Echocardiography to detect wall motion abnormalities induced by ischemia is preferred over nuclear imaging during exercise, because the radioisotope is excreted by the kidneys and may concentrate in the bladder. If indicated, cardiac catheterization may be done with abdominal shielding. Beta blockers and aspirin are the initial treatment choice.29 Additional antianginal medical therapy may include nitrates and calcium channel blockers. These drugs have had limited use during pregnancy for angina, but calcium channel blockers such as diltiazem and verapamil have been used more often for treatment of arrhythmia. Although aspirin (81 mg) has been associated with bleeding and premature ductal closure, it has been used for other indications during pregnancy.
Acute myocardial infarction occurs rarely during pregnancy and has a reported incidence of 1 case in 10,000.40, 41, 42, 43, 44 Coronary vasospasm in the setting of normal coronary arteries has been described as a cause of an infarct during pregnancy.42 In a review of women who had myocardial infarction during pregnancy, the average maternal age was 32 years.45 Infarction most often occurred in the third trimester. On review of the clinical factors, the women who had infarcts were most often multiparous. The anterior walls of the heart were most often involved, and when the women underwent cardiac catheterization, nearly one third had normal coronary arteries. Maternal mortality was approximately 21%, with a 13% fetal mortality. It was hypothesized that the infarcts resulted from vasospasm or localized dissection.45, 46 Dissecting aneurysm of a coronary artery has been reported.47
The treatment of a myocardial infarction during pregnancy should follow guidelines for the nonpregnant patient with the use of nitrates, beta blockers, and aspirin.29 Nitrates may cause hypotension. Aspirin should be used in low doses, because there is a risk of bleeding. There are case reports in the literature on the use of thrombolytic therapy for the treatment of myocardial infarction during pregnancy.48, 49 Reports have included the use of streptokinase, urokinase, or tissue plasminogen activator.48, 49 The agent has been administered at any time from 9 to 38 weeks. There has been no evidence of teratogenic effects. However, maternal complications have included hemorrhage, preterm delivery, fetal loss, spontaneous abortion, and uterine hemorrhage. Primary angioplasty for acute myocardial infarction has been reported and may be preferred over aggressive thrombolytic therapy.50, 51, 52, 53, 54 Angioplasty and stent implantation has been used for treatment of acute myocardial infarction. This procedure required periprocedure and subsequent use of the antiplatelet agents abciximab and ticlodipine in addition to aspirin.52, 54 Ticlodipine may cause neutropenia and thrombocytopenia. Cardiac surgery during pregnancy has been reported.55, 56 Most reports are of surgery for valvular heart disease. Cardiac surgery requiring generalized hypothermia may precipitate uterine contractions resulting in preterm labor. Normothermic conditions are recommended with continuous fetal monitoring.55, 56
ARRHYTHMIAS
Supraventricular arrhythmias
Atrial premature beats are common during pregnancy, and woman present with palpitations.57 Palpitations may be caused by an inappropriate sinus tachycardia, atrial premature beats, supraventricular tachycardia, or atrial fibrillation. The causes and treatment strategies vary and are summarized in Table 4. Holter monitoring has demonstrated that atrial premature beats are common, and patients may be equally symptomatic or asymptomatic.58 Thirty-day event monitoring may diagnose arrhythmias that do not occur daily.
Table 4. Treatment of supraventricular arrhythmias
Arrhythmia | Common Etiologies | Treatment |
Sinus tachycardia | Anemia | Iron supplementation |
Hyperthyroidism | Medical therapy | |
| Deconditioning | |
Relative volume depletion | Fluids | |
Hypoxemia | Determine etiology: oxygen | |
Caffeine | Avoidance | |
Sympathomimetics | Avoidance | |
Tocolytics | Use with adequate hydration | |
Uterine compression of IVC | Change position (left lateral decubitus) | |
Heart failure | Diagnose and treat medically | |
Atrial premature beats or paroxysmal supraventricular tachycardia | Hyperthyroidism | Medical therapy |
Caffeine | Avoidance | |
Sympathomimetics | Avoidance | |
| Valvular heart disease | Diagnose; medical therapy |
Idiopathic | ||
Atrial flutter or fibrillation | Mitral stenosis/regurgitation | Beta-blockade; digoxin, anticoagulation |
Hypertension | Beta-blockade; calcium channel blocker | |
Pericardial disease | Nonsteroidal medication | |
Pulmonary embolism | Anticoagulation | |
Heart failure | Medical therapy; cardioversion | |
Atrial enlargement | Determine etiology | |
Hyperthyroidism | Medical therapy |
IVC, inferior vena cava.
Supraventricular tachycardia has an estimated onset in pregnancy of approximately 4%, or there may be exacerbation of a previously diagnosed arrhythmia.59, 60 The exacerbating or precipitating factors that have been proposed include adrenergic sensitivity to circulating estrogen, increased plasma volume, atrial dilatation, stress or anxiety, and hyperthyroidism. Systemic illnesses such as hyperthyroidism and anemia need to be identified. Caffeine or sympathomimetics may also be a cause as well.61 Women may present with preexcitation syndrome such as Wolff-Parkinson-White syndrome for the first time during pregnancy because of the hemodynamic changes that occur.59, 62 One study suggested arrhythmias may be more common during labor.60 These were predominantly atrial arrhythmias or isolated ventricular premature beats.60
Paroxysmal supraventricular tachycardia arising during pregnancy may be treated acutely with adenosine.63, 64, 65 Adenosine has a half-life of approximately 10 seconds.66 It can cause transient asystole or heart block, but it has been used in pregnancy to terminate paroxysmal supraventricular tachycardia.63, 64, 65 Digoxin is another alternative and has been used for atrial arrhythmia during pregnancy. It crosses the placenta and is secreted in breast milk. Higher doses may be required during pregnancy, when the volume of distribution of digoxin is altered, and drug assays may be misleading. Intravenous verapamil, a calcium channel blocker, has also been used to terminate paroxysmal supraventricular tachycardia during pregnancy.67 Verapamil also crosses the placenta and is found in breast milk. Beta blockers have been used for atrial and ventricular arrhythmias. Beta blockers cross the placenta, and adverse affects have been described predominantly in literature concerning women with hypertension and include fetal bradycardia, fetal hypoglycemia, fetal hyperbilirubinemia, and intrauterine growth retardation.68 Cardioselective agents such as metoprolol or atenolol would be preferred in this setting, because the uterus has beta receptors, and a nonspecific agent such as propranolol may affect uterine function.
Atrial fibrillation usually is caused by underlying structural heart disease. It is usually associated with valvular heart disease, such as mitral disease, that may have been previously undiagnosed. It is associated with long-standing hypertension in the general population, and it may be associated with hypertension exacerbation during pregnancy in the woman who had preexisting hypertension. Other causes may include hyperthyroidism, pulmonary embolism, and pericardial disease. These causes also apply to atrial flutter as well, although this arrhythmia is less common during pregnancy. Initial treatment with digoxin, a beta blocker, or the calcium channel blocker diltiazem may control rate. If hemodynamic compromise is evident, emergent cardioversion should be considered.69 If the precise timing of onset of atrial fibrillation is not clear, the patient should be therapeutically anticoagulated with heparin before chemical or electrical cardioversion. Anticoagulation should be continued for several weeks after cardioversion. Antiarrhythmics that have been used in pregnancy for conversion of atrial fibrillation include procainamide, disopyramide,70 amiodarone,62 sotalol,71 and propafenone.72 Amiodarone is the most commonly used agent because of its efficacy at low doses for atrial fibrillation and ventricular tachycardia. There are maternal risks of thyroid dysfunction, skin discoloration, pulmonary fibrosis, and a proarrhythmic effect.73 There may be drug interactions with digoxin. All antiarrhythmic drugs are associated with a proarrhythmic risk, identified by prolongation of the QT interval on the 12-lead electrocardiogram.
Ventricular arrhythmias
Ventricular arrhythmias appear to increase during pregnancy, and frequent ventricular premature beats may occur with or without symptoms on Holter monitoring58, 60, 73 (Table 5). Women experience palpitations, lightheadedness, or syncope if the arrhythmia is sustained. The possible precipitating factors may be adrenergic sensitivity to estrogen, undiagnosed myocardial disease, stress and anxiety, caffeine, cocaine, or over-the-counter decongestant medications that are sympathomimetics. The over-the-counter sympathomimetics such as phenylpropanolamine and pseudoephedrine may cause ventricular arrhythmias.61 Caffeine has also been identified as a cause. Premature ventricular beats and ventricular tachycardia may occur temporally related to terbutaline administration.74 Less common causes of ventricular tachycardia may include myocardial ischemia due to underlying coronary disease or an anomalous coronary artery, hypomagnesemia,75 therapeutic doses of theophylline, cocaine use, hypoxemia, right ventricular dysplasia,76 or as the first sign of subclinical cardiomyopathy.
Table 5. Treatment of ventricular arrhythmia
Arrhythmia | Etiology | Treatment |
Ventricular premature beats | Caffeine | Avoidance |
Sympathomimetics | Avoidance if symptoms | |
Hypomagnesemia | Replete electrolytes | |
Drug induced | Identify and change medications | |
Hypoxemia | Identify etiology; supplemental oxygen | |
Endogenous cathecholamine | Identify and avoid | |
Myocardial fibrosis/scan | Medical therapy; defibrillation | |
Myocardial ischemia/infarction | Identify and treat | |
Cardiomyopathy | Beat-blockade | |
Ventricular tachycardia | Sympathomimetics | Avoidance |
Hypoxemia | Identify etiology | |
Cardiomyopathy | Medical therapy; defibrillator | |
Myocardial ischemia | Medical/interventional therapy |
Ventricular arrhythmias may be the result of a long QT syndrome, which may be idiopathic or a familial syndrome.77 A prolonged QT interval on the 12-lead electrocardiogram may be associated with antiarrhythmic therapy, cardiomyopathy, intracranial hemorrhage, hypocalcemia, or hypomagnesemia. In addition to antiarrhythmic agents, phenothiazine, tricyclic antidepressants, and lithium all prolong the QT interval. Prolonged QT interval is defined as a corrected (for heart rate) interval of greater than 0.44 seconds on the 12-lead electrocardiogram. This abnormal prolongation and risk arises when the QT interval is prolonged, but the QRS is normal, and bundle branch block is not present. A variant ventricular tachycardia, torsades de pointe, is associated with the long QT syndrome.77 Beta-blocker therapy is recommended to decrease QT interval and risk of torsades de pointe.77
The evaluation of ventricular tachycardia should proceed as in the nonpregnant patient with a search for cause (Table 5), which includes ambulatory monitoring, or if symptoms occur less frequently than on a daily basis, event monitoring for 30 days may help define the arrhythmia. The echocardiogram establishes the presence or absence of structural heart disease. The 12-lead electrocardiogram may confirm the long QT syndrome. Limited stress testing may be indicated for inducing an arrhythmia. Electrophysiologic testing may be performed if clinically indicated with abdominal shielding.
The acute treatment of ventricular tachycardia requires intravenous lidocaine or defibrillation if there is hemodynamic compromise.78, 79 Lidocaine crosses the placenta and, at toxic doses, may result in fetal acidosis, with central nervous system and cardiovascular depression in the neonate.78 Uterine artery constriction also has been reported. Lidocaine is secreted in breast milk.80 Intravenous amiodarone may be used for ventricular tachycardia, and then the patient is converted to oral dosing. Amiodarone has been used also to treat fetal arrhythmias by maternal administration. The iodine in the metabolites of amiodarone does cross the placenta. Adverse effects have been described and include transient fetal bradycardia, prolonged maternal QT interval on the electrocardiogram, and neonatal thyroid disorders.62 Sotalol is an FDA class D antiarrhythmic drug that has been used in ventricular arrhythmias.71 It may result in QT interval prolongation and subsequent torsades de pointe. It has a half-life of approximately 10–20 hours. Adverse effects have included fatigue, depression, dyspnea, chest pain, palpitations, and proarrhythmia. It crosses the placenta and is secreted in breast milk. Other antiarrhythmic agents such as propafenone,72 mexiletine,81 and flecainide76 have had limited use in pregnancy. There are reports of pregnancies in women with implanted defibrillators, and if indicated clinically, a defibrillator should be placed by transvenous approach with abdominal radiation shielding.82
Cardiac arrest during pregnancy is rare.83 It occurs in approximately 1 of 30,000 deliveries. The causes may include amniotic fluid embolism, pulmonary embolism, eclampsia, drug toxicity, trauma, severe hemorrhage, epidural anesthesia, and recreational drug use, specifically cocaine.79, 83 Cardiac arrest may occur as a result of congestive heart failure or cardiomyopathy. Aortic dissection may result in cardiac arrest with electromechanical dissociation. During the setting of cardiac arrest, prompt attention should be given for performing a cesarean section.81, 83 It is always important to check for aortocaval compression by the uterus in the supine position, which may markedly decrease blood return to the heart and be the cause of the arrest or exacerbate hypotension. The resuscitation should best occur in the left lateral decubitus position in the pregnant woman.79
Conduction system disease
Syncope or near-syncope may result from marked bradycardia or advanced conduction system disease, such as atrioventricular dissociation or complete heart block. Marked bradycardia is rare in pregnancy but may be seen in any setting with high vagal tone associated with hyperemesis or severe nausea. The cause of conduction system disease in this population is usually congenital and may first come to medical attention during pregnancy.84 Acquired heart block may result from acute myocarditis, after cardiac surgery (i.e., valve replacement or congenital defect repair) hyperkalemia, drug toxicity, systemic illness, or spinal cord injury. Drugs that may cause conduction system disease include digoxin, quinidine, phenothiazines, and tricyclic antidepressants. It may be seen with sarcoidosis, systemic lupus erythematosus or thyroid disease. Heart block may also be a complication of Lyme disease or after endocarditis. The electrocardiogram may diagnose significant chronic heart block, but if it is intermittent, ambulatory monitoring may be required. Patients with symptomatic profound bradycardia and those with symptomatic or asymptomatic advanced conduction system disease require placement of a permanent pacemaker.85
PERICARDIAL DISEASE
The pregnant woman may develop acute pericarditis due to the same etiologies as in the nonpregnant patient (Table 6).18 It has been suggested that her immune system may be suppressed during pregnancy and that she may be at increased risk for infectious disease. The most common cause of acute pericarditis during pregnancy is a viral infection. Secondary bacterial or fungal infections may occur including tuberculosis.86 The most common viruses implicated are Coxsackie A or B, echovirus, adenovirus, Epstein-Barr, varicella, hepatitis B, and human immunodeficiency virus (HIV). Other, less common causes may include rubella or mycoplasma. In a woman of childbearing age who has received irradiation for a childhood malignancy, this might have resulted in a chronic pericarditis or pericardial constriction.87 Pericardial involvement is also commonly seen in this age group with collagen vascular diseases such as rheumatic fever or systemic lupus erythematosus.86 A pericardial effusion may be present.86
Table 6. Common causes of acute pericarditis during pregnancy
| Idiopathic causes |
| Trauma |
| Viral |
| Bacterial |
| Fungal |
| Tuberculosis |
| Radiation |
| Amyloidosis |
| Neoplasm |
| Systemic lupus erythematosus |
| Rheumatoid arthritis |
| Vasculitis |
| Idiopathic thrombocytopenia purpura |
| Endocarditis |
Pericarditis is often recognized clinically by pleuritic chest pain that worsens in the supine position.18 There may be fever or tachycardia, and, classically, a pericardial friction rub is auscultated. The four stages of electrocardiographic changes that occur with acute pericarditis are summarized in Table 7. An early subtle change may be PR segment depression, ST elevation, peaking of the T wave, and then T-wave inversion. Initially, in stage I, there is diffuse elevation of the ST segment with reciprocal depression in leads aVR and aVL. There is also PR depression that can occur within hours to days. The second phase is the isoelectric phase, during which the electrocardiogram may appear normal. The third phase reveals inversion of the T wave in multiple leads, and in the fourth stage, the electrocardiogram returns to normal. The echocardiogram may reveal a pericardial effusion or evidence of cardiac tamponade88, 89 (Table 7).
Table 7. Diagnostic features of pericardial disease
| Electrocardiographic Changes of Pericarditis |
| Diffuse ST segment elevation and ST segment depression in leads a VR and V1 with -R segment depression |
| Isoelectric phase – return to baseline |
| Inversion of T waves diffusely |
| Reverts to normal |
| Echocardiographic Features |
| Effusion |
| Tamponade |
| Right ventricular compression/collapse |
| Right atrial compression |
| Posterior motion of interventricular septum |
Pericardial effusion may occur during a normal pregnancy.88, 90 Other causes of a pathologic pericardial effusion associated with acute pericarditis include neoplasm, irradiation, trauma, and collagen vascular disease.89 Cardiac tamponade occurs acutely as a result of trauma or cardiovascular rupture. Subacute tamponade is seen with pericarditis, neoplasm, or uremia.89 It is a medical urgency or, if there are signs of hemodynamic compromise, an emergency requiring catheter drainage. Hemodynamic compromise may manifest by tachycardia proceeding to hypotension. A pulsus paradoxus of greater than 20 mmHg is diagnostic. Pericardial constriction is rare in pregnancy and may be the sequela of prior infection or radiation.91 Women who present with marked edema may require pericardiectomy.92
ENDOCARDITIS
Infective endocarditis is rare occurs rarely during pregnancy. There is underlying valvular or congenital heart disease that may not have been previously diagnosed.93 Changes in immunologic status and exposure to infection may predispose the gravida to endocarditis during pregnancy. The most common organisms that cause endocarditis during pregnancy remain Streptococcus viridans and Staphylococcus aureus.93 S. viridans is a commonly acquired mouth organism. Endocarditis should be treated the same as in the nonpregnant state. The choice of antibiotics to be used should be the same as in the nonpregnant state, with careful monitoring for toxicity. The mother should receive the full course of treatment. If valve function worsens and congestive heart failure ensues, additional medical therapy to treat heart failure may be required. If heart failure is intractable or the infection is not eradicated by standard therapy, surgical intervention may be necessary.94, 95
Transesophageal echocardiography may reveal an intracardiac abscess requiring surgical attention. Even in the setting of a prominent vegetation, if the woman responds to antibiotic therapy and defervesces, she may continue antibiotic therapy for the standard prescribed course. Once having had endocarditis, the woman is at increased risk for future episodes of endocarditis and should receive antibiotic prophylaxis during labor and delivery.96
AORTIC DISSECTION DURING PREGNANCY
Any woman entering the third trimester may have an increased risk of aortic dissection because of hormonally mediated changes within the aortic wall.97 Women with Marfan or Turner syndrome may be at increased risk, as are those with hypertension or an uncorrected coarctation of the aorta.98, 99 Aortic dissection has been associated with cocaine use.100 It is usually a type A dissection, beginning in the ascending aorta and extending proximally to the aortic valve ring or the coronary artery ostia or distally to involve the neck vessels. When the dissection involves the ostium of a coronary artery, there may be evidence of ischemia clinically as on the electrocardiogram. The chest pain of aortic dissection is sharp and severe, and it usually radiates to the back. Aortic insufficiency may occur if the dissection involves the valve ring. There is often loss of distal extremity pulses. During pregnancy, one of the best modalities to diagnose this disorder is transesophageal echocardiography, avoiding ionizing radiation if possible.
Initial treatment of an aortic dissection is beta blockade and nitroprusside (see Table 8). Nitroprusside must be used carefully to avoid cyanide toxicity.101, 102 Intravenous labetalol has also been used to provide alpha and beta blockade. According to one study, it was recommended that aortic dissection occurring before 28 weeks should be considered for primary aortic repair, but after 32 weeks, a primary cesarean section should be followed by aortic repair.97 Cardiopulmonary bypass during surgery should be high flow, high pressure, and normothermic.55, 56, 97 Hypothermia may result in uterine contractions and precipitate an early delivery.
CARDIOVASCULAR EFFECTS OF HYPERTENSION
Four recognized types of hypertension occur during pregnancy: gestational hypertension with or without proteinuria; exacerbation of preexisting hypertension; preeclampsia; and toxemia.103, 104 Pulmonary edema may be a complication of severe hypertension, particularly preeclampsia and toxemia, and is probably caused by an acute lung injury syndrome, which results in a noncardiogenic pulmonary edema.15 In an echocardiographic study of women with pulmonary edema associated with hypertension, 25% demonstrated impaired systolic function, which is usually transient.24 Predisposing factors for the development of pulmonary edema related to hypertension in pregnancy can include prior dexamethasone treatment,24 diabetes mellitus, or amniotic fluid embolism.15 Preeclampsia has been defined as a generalized endothelial dysfunction with release of cytokines and toxins, vasoconstriction, and platelet activation.103 This may play a role in the development of noncardiogenic pulmonary edema. Noncardiogenic pulmonary edema may also be associated with premature labor, tocolytic administration,21 infection, hypertension, aspiration, and abruptio placentae. The pulmonary edema that usually accompanies the exacerbation of a hypertensive disorder during pregnancy is usually transient and responds to control of blood pressure and diuresis. When hemodynamic monitoring is used, there are usually low cardiac filling pressures after the hypertension is controlled. Pulmonary edema may be associated with the preeclampsia syndrome, but an investigation for an underlying cardiac cause should occur. Treatment of pregnancy-induced hypertension may prevent maternal cardiovascular complications.103, 104 Hydralazine, labetalol, nifedipine or sodium nitroprusside may be used during pregnancy for acute and/or severe hypertension and are summarized in Table 8.
Table 8. Medical therapy for hypertension during pregnancy
| Drug | FDA Class | Adverse Effects in Pregnancy | May be Used for Chronic Therapy |
| Hydralazine | C | Flushing; tachycardia | Yes |
| Labetalol | C | Flushing; nausea | Yes |
| Nifedipine | C | Flushing; early labor; lower extremity edema; tachycardia | Yes |
| Sodium nitroprusside | C | Cyanide toxicity for mother and fetus – monitor levels | No |
(Adapted from Frishman WH, Schlocker SJ, Awan K et al: Pathophysiology and medical management of systemic hypertension in pregnancy. Cardiology in Review. 13: 274–284, 2005.)
CARDIOVASCULAR EFFECTS OF TOCOLYTICS
Tocolysis may result in cardiac effects during pregnancy. Betamimetic drugs such as ritodrine or terbutaline, when given intravenously, decrease peripheral vascular resistance, increase cardiac output, and have a positive inotropic effect. There have been reports of pulmonary edema and coronary spasm causing myocardial ischemia and myocardial injury.21, 22, 105 The electrocardiogram may reveal ST segment depression, T-wave flattening or inversion, and prolongation of the QT interval, which may be transient.74 Arrhythmias and conduction system disease have been observed as well.74, 105
The estimated incidence of pulmonary edema is 1–5%, and the edema is usually associated with excessive volume retention.74 Persistent left ventricular dysfunction often is caused by a previously unrecognized cardiomyopathy unmasked by betamimetic therapy.21 These complications have been reported with ritodrine (oral or subcutaneous administration). Use of betamimetics in women with known cardiac disease may carry further risk and is specifically contraindicated in the gravida with pulmonary hypertension, right-to-left shunting, valvular stenosis, hypertrophic cardiomyopathy, or coarctation of the aorta.74 Women with a history of arrhythmias may experience an exacerbation of the arrhythmia. Magnesium or calcium channel blockers may be better alternatives in these patients, along with careful monitoring for the development of hypotension.
CONCLUSIONS
Acquired heart disease may complicate pregnancy and may require immediate intervention that is often similar to the non-pregnant state. Treatment should not be withheld but rather modified to consider both the mother and fetus. Clinically indicated medications should be administered in the lowest effective dose, and, if possible, blood levels monitored. One of the major issues of any illness complicating pregnancy is the effect on long-term prognosis – whether the mother will return to her previous functional level and whether future pregnancies are possible. The mother often requires complete cardiovascular evaluation after pregnancy. Because the hemodynamic changes of pregnancy may linger, evaluation should not occur until at least 12 weeks after delivery.3 Before another conception, she should undergo a complete evaluation with cardiac imaging, stress testing, and, if clinically indicated, invasive studies. Correcting an underlying cardiac problem may facilitate future pregnancies in certain cases.
ACKNOWLEDGMENTS
The author gratefully acknowledges the secretarial assistance of Joan Draves.
REFERENCES
Sermer M, Colamn J, Siu S: Pregnancy complicated by heart disease: a review of Canadian experience. Obstet Gynecol 23: 540–544, 2003 |
|
Warnes C: Pregnancy and Heart Disease. In Libby P, Bonow RO, Mann DL, Zipes DP (eds), Braunwald's Heart Disease. 8th ed. Philadelphia: WB Saunders, 2008 |
|
Capeless EL, Clapp JF: When do cardiovascular parameters return to their preconception values? Am J Obstet Gynecol 1165: 883–886, 1991 |
|
Mendelson M: Pregnancy in the woman with preexisting cardiovascular disease. Gynecol Obstet 1: 17, 1998 |
|
Kerr MG: The mechanic effects of the gravid uterus in late pregnancy. J Obstet Gynaecol Br Commonw 72: 513–529, 1965 |
|
Sadaniantz A, Kocheril AG, Emaus SP et al: Cardiovascular changes in pregnancy evaluated by two-dimensional and Doppler echocardiography. Am J Soc Echocard 5: 258, 1992 |
|
Campos O, Andrade JL, Bocanegra J et al: Physiologic multivalvular regurgitation during pregnancy: A longitudinal Doppler echocardiographic study. Int J Cardiol 40: 265, 1993 |
|
Widerhorn J, Rubin J, Frishman W: Cardiovascular drugs in pregnancy. Cardiol Clin 5: 651–674, 1987 |
|
Davies GA, Herbert WN: Ischemic heart disease and cardiomyopathy in pregnancy. J Obstet Gynecol Can 29: 575–579, 2007 |
|
Sliwa K, Forster O, Libhaber E et al: Peripartum cardiomyopathy: inflammatory markers as predictors of outcome in 100 prospectively studied patients. Eur Heart J 27: 441–446, 2006 |
|
Kim HJ, Kim DK, Lee SC et al: Pheochromocytoma complicated with cardiomyopathy after delivery: a case report and literature review. Korean J Intern Med 13: 117–122, 1998 |
|
Nanda AS, Feldman A, Liang CS: Acute reversal of pheochromocytoma-induced catecholamine cardiomyopathy. Clin Cardiol 18: 421–423, 1995 |
|
Katz A, Goldenberg I, Maoz C et al: Peripartum cardiomyopathy occurring in a patient previously treated with doxorubicin. Am J Med Sci 314: 399–400, 1997 |
|
Curtis SL, Marsden-Williams J, Sullivan C et al: Current trends in the management of heart disease in pregnancy. Int J Cardiol 2008 [Epub ahead of print] |
|
Karetzky M, Ramirez M: Acute respiratory failure in pregnancy: An analysis of 19 cases. Medicine (Baltimore) 77: 41–49, 1998 |
|
Abboud J, Murad Y, Chen-Scarabelli C, Saravolatz L et al: Peripartum cardiomyopathy: a comprehensive review. Int J Cardiol 127: 295–303, 2007 |
|
Lamparter S, Pankuweit S, Maisch B. Clinical and immunologic characteristics in peripartum cardiomyopathy. Int J Cardiol 118: 14–20, 2007 |
|
Oakley C. Myocarditis, pericarditis and other pericardial diseases. Heart 84: 449–454, 2000. |
|
Elkayam U, Akhter MW, Singh H et al: Pregnancy-Associated cardiomyopathy. Clinical characteristics and a comparison between early and late presentation. Circulation. 111: 2050–2055, 2005 |
|
Lang RM, Pridjian G, Feldman et al: Left ventricular mechanics in preeclampsia. Am Heart J 121: 1768–1775, 1991 |
|
Lampert MB, Hibbard J, Weinert L et al: Peripartum heart failure associated with prolonged tocolytic therapy. Am J Obstet Gynecol 168: 493–495, 1993 |
|
Tatara T, Morisaki H, Shimada M et al: Pulmonary edema after long-term beta-adrenergic therapy and cesarean section. Anesth Analg 81: 417–418, 1995 |
|
Sasson Z, Rakowski H, Wigle ED: Hypertrophic cardiomyopathy. Cardiol Clin 6: 233–288, 1988 |
|
Desai DK, Moodley J, Naidoo DP, Bhorat I: Cardiac abnormalities in pulmonary edema associated with hypertensive crises in pregnancy. Br J Obstet Gynaecol 103: 523–528, 1996 |
|
Witlin AG, Mabie WC, Sibai BM: Peripartum cardiomyopathy: A longitudinal echocardiographic study. Am J Obstet Gynecol 177: 1129–1132, 1997 |
|
Lang RM, Lampert MB, Poppas A et al: Peripartal cardiomyopathy. In Elkayam U, Gleicher N (eds): Cardiac Problems in Pregnancy, pp 87–100. 3rd ed. New York: Wiley-Liss, 1998 |
|
Brown CS, Bertolet BD: Peripartum cardiomyopathy: A comprehensive review. Am J Obstet Gynecol 178: 409–414, 1998 |
|
Qasqas SA, McPherson C, Firshman WH et al: Cardiovascular pharmacotherapeutic considerations during pregnancy and lactation. Cardiol Rev 12: 240–261, 2004 |
|
Qasqas SA, McPherson C, Frishman WH et al: Cardiovascular pharmacotherapeutic considerations during pregnancy and lactation. Cardiol Rev 12: 201–221, 2004 |
|
Hirsh J, Warkentin TE, Raschke R et al: Heparin and low-molecular-weight heparin: Mechanisms of action, pharmacokinetics, dosing considerations, monitoring, efficacy, and safety. Chest 114: 489S– 510S, 1998 |
|
Schneider DM, von Tempelhoff GJ, Heilmann L: Retrospective evaluation of the safety and efficacy of low molecular-weight heparin as thromboprophylaxis during pregnancy. Am J Obstet Gynecol 177: 1567–1568, 1997 |
|
St John Sutton M, Cole P, Plappert M et al: Effects of subsequent pregnancy on left ventricular function in peripartum cardiomyopathy. Am Heart J 121: 1776–1778, 1991 |
|
Carvalho AM, Brandao A, Martinez EE et al: Prognosis in peripartum cardiomyopathy. Am J Cardiol 64: 540–542, 1989 |
|
Reece EA, Egan JFX, Coustan DR: Coronary artery disease in diabetic pregnancies. Am J Obstet Gynecol 154: 150–151, 1986 |
|
Hagay Z, Weissman A: Management of diabetic pregnancy complicated by coronary artery disease and neuropathy. Obstet Gynecol 23: 205–220, 1996 |
|
Rutherford JD: Coronary artery disease in pregnancy. In Elkayam U, Gleicher N (eds): Cardiac Problems in Pregnancy, pp 121–130. New York: Wiley-Liss, 1998 |
|
Hughes JR, Davies JA: Anticardiolipin antibodies in clinical conditions associated with a risk of thrombotic events. Thromb Res 89: 101–106, 1998 |
|
Daniels C, Bacon J, Fontana ME et al: Anomalous origin of the left main coronary artery from the pulmonary trunk masquerading as peripartum cardiomyopathy. Am J Cardiol 79: 1307–1308, 1997 |
|
Mabie WC, Freire CM: Sudden chest pain and cardiac emergencies in the obstetric patient. Obstet Gynecol Clin North Am 22: 19–37, 1995 |
|
Donnelly S, McKenna P, McGing P, Sugrue D: Myocardial infarction during pregnancy. Br J Obstet Gynaecol 100: 781–782, 1993 |
|
Hankins GDV, Wendel GD Jr, Leveno KF: Myocardial infarction during pregnancy: A review. Obstet Gynecol 65: 13–146, 1985 |
|
Iadanza A, Del Pasqua A, Barbati R et al: Acute ST elevation myocardial infarction in pregnancy due to coronary vasospasm: A case report and review of literature. Int J Cardiol 115: 81–85, 2007 |
|
Garry D, Leikin E, Fleisher AG: Acute myocardial infarction in pregnancy with subsequent medical and surgical management. Obstet Gynecol 87: 802–804, 1996 |
|
Roth A, Elkayam U: Acute myocardial infarction associated with pregnancy. Ann Intern Med 125: 751–762, 1996 |
|
Badui E, Enciso R: Acute myocardial infarction during pregnancy and puerperium: A review. Angiology 47: 739–756, 1996 |
|
Klutstein MW, Tzivoni D, Bitran D et al: Treatment of spontaneous coronary artery dissection: Report of three cases. Cathet Cardiovasc Diagn 40: 372–376, 1997 |
|
Koul AK, Hollander G, Moskovits N et al: Coronary artery dissection during pregnancy and the postpartum period: Two case reports and review of literature. Cathet Cardiovasc Intervent 52: 88–94, 2001 |
|
Webber MD, Halligan RE, Schumacher JA: Acute infarction, intracoronary thrombolysis, and primary PTCA in pregnancy. Cathet Cardiovasc Diagn 42: 38–43, 1997 |
|
Leonhardt G, Gaul C, NIetsch HH et al: Thromboytic therapy in pregnancy. J Thrombolysis. 21: 271–276, 2006 |
|
Ascarelli MH, Grider AR, Hsu HW: Acute myocardial infarction during pregnancy managed with immediate percutaneous transluminal coronary angioplasty. Obstet Gynecol 88: 655–657, 1996 |
|
Cowan NC, deBelder MA, Rothman MT: Coronary angioplasty in pregnancy. Br Heart J 59: 588– 592, 1988 |
|
Balmain S, McCullough CT, Love C et al: Acute myocardial infarction during pregnancy successfully treated with primary percutaneous coronary intervention. Int J Cardiol 116: e85–e87, 2007 |
|
Boztosun B, Olcay A, Avci A et al: Treatment of acute myocardial infarction in pregnancy with coronary artery balloon angioplasty and stenting. Use of tirofiban and clopidogrel. Int J Cardiol 127: 413–416, 2008 |
|
Ladner HE, Danielsen B, Gilbert WM. Acute myocardial infarction in pregnancy and the puerperium: A population-based study. Am Coll Obstet Gynecol. 105: 480–484, 2005 |
|
Becker RM: Intracardiac surgery in pregnant women. Ann Thorac Surg 36: 453–458, 1983 |
|
Weiss BM, von Segesser LK, Alon E et al: Outcome of cardiovascular surgery and pregnancy: A systematic review of the period 1984-1996. Am J Obstet Gynecol 179: 1643–1653, 1998 |
|
Ferrero S, Colombo BM, Ragni N. Maternal arrhythmias during pregnancy. Arch Gynecol Obstet 269: 244–253, 2004 |
|
Shotan A, Ostrzega E, Mehra A et al: Incidence of arrhythmias in normal pregnancy and relation to palpitations, dizziness and syncope. Am J Cardiol 79: 1061–1064, 1997 |
|
Tawan M, Levine S, Mendelson M et al: The effect of pregnancy on paroxysmal supraventricular tachycardia. Am J Cardiol 72: 838–840, 1993 |
|
Romem A, Romem Y, Katz M et al: Incidence and characteristics of maternal cardiac arrhythmias during labor. Am J Cardiol 93: 931–933, 2004 |
|
Onuigbo M, Alikham M: Over-the-counter sympathomimetics: A risk factor for cardiac arrhythmias in pregnancy. South Med J 91: 1153–1155, 1998 |
|
Plomp TA, Vulsma T, deVijlder JJM: Use of amiodarone during pregnancy. Eur J Obstet Gynecol 43: 201–207, 1992 |
|
Mason BA, Ricci-Goddman J, Koos BJ: Adenosine in the treatment of maternal paroxysmal supraventricular tachycardia. Obstet Gynecol 80: 478–480, 1992 |
|
Harrison KJ, Greenfield RA, Wharton MJ: Acute termination of supraventricular tachycardia by adenosine during pregnancy. Am Heart J 123: 1386–1388, 1992 |
|
Elkayam U, Goodwin TM: Adenosine therapy for supraventricular tachycardia during pregnancy. Am J Cardiol 75: 521–523, 1995 |
|
Wilbur SL, Marchlinski FE: Adenosine as an antiarrhythmic agent. Am J Cardiol 79: 30–37, 1997 |
|
Byerly WG, Hartman A, Foster DE: Verapamil in the treatment of maternal paroxysmal supraventricular tachycardia. Ann Emerg Med 20: 552–554, 1991 |
|
Hurst AK, Shotan A, Hoffman K et al: Pharmacokinetic and pharmacodynamic evaluation of atenolol during and after pregnancy. Pharmacotherapy 18: 840–846, 1998 |
|
Schroeder JS, Harrison DC: Repeated cardioversion during pregnancy. Am J Cardiol 27: 445–446, 1971 |
|
Tadmor OP, Keren A, Rosenak D: The effect of disopyramide on uterine contractions during pregnancy. Am J Obstet Gynecol 162: 482–486, 1990 |
|
MacNeil DJ: The side effect profile of class III antiarrhythmic drugs: focus on D,L-sotalol. Am J Cardiol 80: 90G–98G, 1997 |
|
Capucci A, Boriani G: Propafenone in the treatment of cardiac arrhythmias: A risk-benefit appraisal. Drug Safety 12: 55–72, 1995 |
|
Brodsky M, Doria R, Allen B: New-onset ventricular tachycardia during pregnancy. Am Heart J 123: 933–941, 1992 |
|
Goodwin TM: Tocolytic therapy in the cardiac patient. In Elkayam U, Gleicher N (eds): Cardiac Problems in Pregnancy, pp 437–444. 3rd ed. New York: Wiley-Liss, 1998 |
|
Varon ME, Sherer DM, Abamowicz JS: Maternal ventricular tachycardia associated with hypomagnesemia. Am J Obstet Gynecol 167: 1352–1355, 1992 |
|
Villanova C, Muriago M, Nava F: Arrhythmogenic right ventricular dysplasia: pregnancy under flecainide treatment. J Ital Cardiol 28: 691–693, 1998 |
|
Rashba EJ, Zareba W, Moss AJ et al: Influence of pregnancy on the risk for cardiac events in patients with hereditary long QT syndrome: LQTS investigators. Circulation 97: 451–456, 1998 |
|
Cox JL, Gardner MJ: Treatment of cardiac arrhythmias during pregnancy. Prog Cardiovasc Dis 36: 137–178, 1993 |
|
Lee RV, Rodgers BD, White LM: Cardiopulmonary resuscitation of pregnancy women. Am J Med 81: 311–318, 1986 |
|
Chow T, Galvin J, McGovern B: Antiarrhythmic drug therapy in pregnancy and lactation. Am J Cardiol 82: 581–621, 1998 |
|
Gregg AR, Tomich PG: Mexilitene use in pregnancy. J Perinatol 8: 33–35, 1988 |
|
Natale A, Davidson T, Geiger JM, Newby K: Implantable cardioverter-defibrillators and pregnancy. Circulation 96: 2808–2812, 1997 |
|
Kloeck W, Cummins RO, Chamberlain D: Special resuscitation situations: An advisory statement from the International Liaison Committee on Resuscitation. Circulation 95: 2196–2110, 1997 |
|
Dalvi BV, Chaudhuri A, Kulkarni HL: Therapeutic guidelines for congenital complete heart block presenting in pregnancy. Obstet Gynecol 79: 802–804, 1992 |
|
Jaffe R, Gruber A, Fejgin M: Pregnancy with an artificial pacemaker. Obstet Gynecol 42: 137–139, 1987 |
|
Seferovic AD, Seferovic PM, Ljubic A et al: Pericardial disease in pregnancy. Herz 28: 209–215, 2003 |
|
Bakri YN, Martan A, Amri A, Amri M: Pregnancy complicating irradiation-induced constrictive pericarditis. Acta Obstet Gynecol Scand 71: 143–144, 1992 |
|
Enein M, Zina AAA, Kassem M et al: Echocardiography of the pericardium in pregnancy. Obstet Gynecol 69: 851, 1987 |
|
Hagley MT, Shaub TF: Acute pericarditis with a symptomatic pericardial effusion complicating pregnancy. Reprod Med 38: 813–814, 1993 |
|
Abduljabbar HSO, Marzouki KMH, Zawawi TH, Kahn AS: Pericardial effusion in normal pregnancy in women. Acta Obstet Gynecol Scand 70: 291–294, 1991 |
|
Blake S, Bonar F, McDonald D: Pregnancy with constrictive pericarditis: Case reports. Br J Obstet Gynaecol 91: 404–406, 1984 |
|
Richardson PM, LeRoux BT, Rogers MA: Pericardiectomy in pregnancy. Thorax 25: 627–630, 1970 |
|
Campuzano K, Roque H, Bolnick et al: Bacterial endocarditis complicating pregnancy: case report and systematic review of the literature. Arch Gynecol Obstet 268: 251–255, 2003 |
|
Burstein H: Gonococcal endocarditis during pregnancy: Simultaneous cesarean section and aortic valve surgery. Obstet Gynecol 66: 48S–51S, 1985 |
|
Westaby S: Reoperation for prosthetic valve endocarditis in the third trimester of pregnancy. Ann Thorac Surg 53: 263–265, 1992 |
|
Wilson W, Taubert KA, Gewitz M et al: Prevention of infective endocarditis. Guidelines from the American Heart Association. Circulation. 116: 1736–1754, 2007 |
|
Zeebregts CJ, Schepens MA, Hameeteman TM et al: Acute aortic dissection complicating pregnancy. Ann Thorac Surg 65: 1511–1512, 1998 |
|
Garvey P, Elovitz M, Landsberger EJ: Aortic dissection and myocardial infarction in a pregnant patient with Turner syndrome. Obstet Gynecol 91: 864, 1998 |
|
Dizon-Townson D, Magee KP, Twickler DM: Coarctation of the abdominal aorta in pregnancy: Diagnosis by magnetic resonance imaging. Obstet Gynecol 85: 817–819, 1995 |
|
Roth A, Elkayam U. Acute myocardial infarction associated with pregnancy. J Am Coll Cardiol 52: 171–180, 2008 |
|
Naulty J, Cefalo RC, Lewis PE: Fetal toxicity of nitroprusside in the pregnancy ewe. Am J Obstet Gynecol 139: 708–711, 1981 |
|
Shoemaker CT, Meyers M: Sodium nitroprusside for control of severe hypertensive disease of pregnancy: A case report and discussion of potential toxicity. Am J Obstet Gynecol 149: 171–173, 1984 |
|
Menzies J, Magee LA, Li J et al: Instituting surveillance guidelines and adverse outcomes in preeclampsia. Obstet Gynecol. 110: 121–127, 2007 |
|
Frishman WH, Schlocker SJ, Awan K et al: Pathophysiology and medical management of systemic hypertension in pregnancy. Cardiol Rev 13: 274–284, 2005 |
|
Perry KG, Morrison JC, Rust OA et al: Incidence of adverse cardiopulmonary effects with low-dose continuous terbutaline infusion. Am J Obstet Gynecol 173: 1273–1277, 1995 |