Hemodynamic Monitoring of the Critically Ill Patient
Authors
INTRODUCTION
In the practice of obstetrics and gynecology, the need for hemodynamic or respiratory resuscitation is fortunately rare; however, all obstetricians and gynecologists encounter the necessity for assessment and monitoring of patients' hemodynamic or respiratory status. This need may occur while managing various complications of pregnancy, such as preterm premature rupture of the membranes or preterm labor complicated by intraamniotic infection and treated with tocolysis and steroids, during peripartum management of preeclampsia or postpartum hemorrhage. The list of possible clinical situations requiring knowledge of the patient's hemodynamic or respiratory status is very long and familiar to those practicing obstetrics and gynecology.
Two basic categories of monitoring are available, invasive and noninvasive. Invasive methods have become the gold standard for monitoring nonpregnant as well as pregnant patients, as their validity and reliability has been established from a large body of evidence. They carry significant risks, and therefore the use of invasive methods of monitoring is recommended for a set of specific indications, when the risks associated with their application are outweighed by benefits of the information they can provide. Therefore, in critically ill patients, the benefits of invasive monitoring are clear. More frequently, however, we are faced with less severe and thus less obvious situations when it would be desirable to assess and monitor the patient's hemodynamic and respiratory status noninvasively.
NONINVASIVE MONITORING
The noninvasive monitoring of the patient's hemodynamics and oxygenation status have two important applications. First, data obtained may help identify patients who will benefit from invasive monitoring. It will aid in establishing indications for invasive monitoring. Second, in a much larger group of patients, the results of noninvasive monitoring will determine that invasive monitoring is not essential, and in these milder situations, noninvasive monitoring will suffice, thereby avoiding the risks of invasive procedures.
Noninvasive monitoring was first established in management of nonpregnant patients under anesthesia and in the intensive care settings. Our published experience with these methods in obstetrics and gynecology is still limited to a few published studies. Nonetheless, there is a fairly large, however uncontrolled, clinical experience. In general, noninvasive methods allow assessment and trend analysis of cardiac output and peripheral tissue perfusion.
Assessment of Cardiac Output
END-TIDAL CARBON DIOXIDE PRESSURE
End-tidal carbon dioxide (ETCO2) pressure measurement is a good predictor of cardiac output. Because of high lipid solubility and the ability to cross the blood–air barrier, change in exhaled CO2 is a function of pulmonary blood flow and thus indirectly of cardiac output. Therefore, the proportion of CO2 in exhaled gases reflects the cardiac output.1, 2 ETCO2 can be measured not only noninvasively, but also very simply, using nasal cannula for oxygen treatment and infrared capnometer, routinely used by anesthesiologists. ETCO2 measurement for estimation of cardiac output has been validated in nonpregnant patients with hypovolemia and during cardiopulmonary resuscitation.3, 4, 5 Comparison with invasive measurement of cardiac output demonstrates high correlation (r2 = 0.82).2 ETCO2 might be especially useful in monitoring patients with postpartum hemorrhage (PPH) during volume resuscitation.
Monitoring the hemodynamic status of the patient during severe PPH is crucial, as estimation of blood loss is often imprecise and monitoring provides objective assessment of the effectiveness of resuscitation. It is important, however, to recognize the limitations of many traditional methods of monitoring. Blood pressure is a simple, but insensitive method of evaluation. Blood pressure may remain normal until 30–40% of the blood volume is lost, and it may be spuriously low when obtained by arm cuff.2 Direct intraarterial recording is preferred in patients with hypovolemia, but access can be problematic. Additional invasive methods of cardiac output monitoring involve measurement of cardiac filling pressures by either central venous or pulmonary wedge pressure. Even so, these measurements demonstrate poor correlation with the extent of blood loss, especially when it is less then 30% of the blood volume.6 Performance of orthostatic maneuvers may improve the sensitivity of cardiac filling pressures in the monitoring of blood loss.7
A decrease in ETCO2 results in an increase of the PaCO2–ETCO2 gradient indicating impaired elimination of CO2. An increased gradient is an early sign of complications such as pulmonary embolism, atelectasis, pneumonia, pulmonary edema, or low cardiac output. Although ETCO2 cannot differentiate between these complications, it can serve, because of its noninvasiveness, as a useful screening tool.
Before we can routinely use ETCO2 measurements in pregnant patients, it is necessary to establish normative data for this population. Currently, studies are being conducted to confirm ETCO2 validity and reliability in pregnant women.
ECHOCARDIOGRAPHY
Unlike ETCO2 measurements, echocardiography for estimation of cardiac output and cardiac filling pressures has been studied in critically ill obstetric patients. Belfort and associates compared cardiac output, right ventricular, right atrial, and pulmonary artery systolic pressures obtained by echocardiography and pulmonary artery catheter in a group of critically ill pregnant patients. They reported no significant differences between the results of the two methods, as well as high correlation of obtained measurements for cardiac output (r2 = 0.98) and cardiac filling pressures (r2 = 0.85 for pulmonary artery systolic pressure).8 The limitation of echocardiography for the purpose of hemodynamic monitoring is that it does not provide continuous measurements. This limitation does not, however, invalidate its usefulness for the intermittent assessment of the patient's hemodynamic status.
Recently, the role of echocardiography (both transthoracic and transesophageal) has grown significantly in the critically ill patient. Transesophageal echo is superior to transthoracic echo in the intensive care unit since imaging in the latter may be compromised by wound dressings, PEEP above 10–15 cmH2O, chest wall edema, and chest tubes.9 Echocardiography is extremely usefull for determining fluid status in patients on mechanical ventilation, since the relationship between filling pressures and filling volumes may not be accurate in this subset of patients. A left ventricular end-diastolic diameter <25 mm and systolic obliteration of the left ventricular cavity are consistent with hypovolemia.
Echocardiography will also provide valuable information in the hemodynamically unstable patient allowing other conditions like valvular anomalies, acute cardiac ischemia, cardiac tamponade, pulmonary embolism, and right ventricular failure to be evaluated.
THORACIC BIOIMPEDENCE
Another promising noninvasive method of cardiac output measurement is thoracic bioimpedence. It relies on the principle that conduction of alternating current applied across the thorax changes proportionally to blood volume in the heart and great vessels. Thus, it is also indirectly proportional to cardiac output. Bioimpedence has been validated in nonpregnant patients. Moreover, Clark and colleagues established its validity in a group of eight normal pregnant women. They compared cardiac index measurements using thoracic bioimpedence and pulmonary artery catheterization and demonstrated high correlation of the results of both methods (r2 = 0.89).10 Correlation was best in the left lateral position.
Tissue Perfusion Assessment
Global oxygen delivery and cardiac output are not synonymous with adequate tissue perfusion in critically ill patients. Therefore any, but especially noninvasive, methods of monitoring tissue perfusion would be very valuable for clinical decision-making and management.
VENOUS BLOOD GASES
Monitoring of venous blood gases is simple and provides valuable information on tissue perfusion. Venous blood gases reflect whole body oxygenation and acid–base status of the tissues better than arterial blood gases. The effectiveness of this approach to organ perfusion monitoring has been demonstrated in patients undergoing cardiopulmonary resuscitation.11 The validity of this method in monitoring of critically ill pregnant patients remains to be established.
ARTERIAL LACTATE
Measurements of blood lactate concentration help to determine whether the oxygen supply is adequate to sustain aerobic metabolism. In patients with septic shock, this parameter has shown to be a superior predictor of outcome, better than hemodynamic parameters or measures of oxygen transport.12 Values of >2 mmol/L and >4 mmol/L predict mortality in 58% and 80% of patients with positive test results, respectively.13 It is important, however, to state that the ability of lactate concentrations to predict mortality is limited to patients with shock. Also, other reasons for increased lactate, such as hepatic and thiamine insufficiency and alkalosis, have to be excluded. It also appears that in patients with sepsis, an increase in lactate concentration is a direct effect of endotoxin, not oxygen deprivation.14 Importantly, the effectiveness in pregnant patients has to be established. The fact that maternal lactate levels normally increase during the second stage of labor further complicates its applicability in the peripartal period.15
GASTRIC TONOMETRY
Venous blood gases and arterial lactate are the measurements of oxygen deficit at the whole body level. Gastric tonometry is based on the observation that splanchnic hypoperfusion is common in critically ill patients and may precede multiple organ failure.16 The instrument is made of a CO2 permeable balloon attached to the end of a nasogastric tube. It measures gastric mucosal partial pressure of CO2. This measurement is then used together with arterial bicarbonate concentration to calculate pH of the gastric mucosa. Gastric acidosis correlates with the onset of anaerobic metabolism in response to hypoxia or sepsis.17 Although gastric tonometry has been successfully used in nonpregnant critically ill patients over the last decade, we do not have at our disposal any studies validating this technique in obstetrics.18
Clearly there is a place and need for noninvasive hemodynamic monitoring in management of women with complicated pregnancies. Several methods of monitoring that are currently successfully used in nonpregnant patients await their validation in pregnancy. However, before the results of such validity studies become available and the best tests in pregnancy are identified, the relative changes in parameters measured by the above-mentioned techniques can serve as an adjunct to deciding if invasive monitoring is indicated or whether the patient can be monitored noninvasively.
INVASIVE HEMODYNAMIC MONITORING
Hemodynamic evaluation of the critically ill patient requires full understanding of cardiovascular structure and function. History taking and physical examination should be carried out efficiently, yet thoroughly. Assessment of maternal vital signs, mental status, urine output, and documentation of fetal well-being provides very important evidence of adequacy of circulation and represents the reference to which patient deterioration or effects of treatment will be compared. When rapid deterioration of cardiovascular status occurs, however, reliance on traditional clinical parameters may not allow for timely intervention. Reliable, continuous information may require the use of invasive monitoring, such as an arterial line (intravascular mean arterial pressure), and/or a pulmonary artery catheter (cardiac output and pulmonary arterial and wedge pressures).
Recent literature has questioned the ability of both central venous and pulmonary artery oclussion pressures to accurately predict volume status in critically ill patients19. Critically ill patients often receive mechanical ventilation. As a result, intrathoracic (and intravascular) pressures increase also. Such an increase in intravascular pressures is not directly related to the actual intravascular volume status. Another frequent situation in the intensive care unit is the presence of ventricular diastolic dysfunction (often seen in patients with severe preeclampsia). In this situation, the ventricular compliance is limited, such that even with small amounts of volume, the ventricles will be unable to dilate and consequently filling pressures on the left side (pulmonary artery oclussion pressure) and right side (central venous pressure) will be elevated despite absolute hypovolemia.
In a recent trial, a low central venous pressure (<8 mmHg) and a low pulmonary artery oclussion pressure (<12 mmHg) predicted volume responsiveness in only 47–54% of patients20
Arterial Line
Blood pressure can be determined, in decreasing order of reliability, by intravascular catheters, digital oscillometers, and sphygmomanometers. Direct recording of intravascular pressure is recommended for all patients in the intensive care unit who require careful continuous monitoring of arterial pressure.21
Fluid-filled tubing transmits the pressure wave from the cannulated artery to the pressure transducer. Systolic, diastolic, and mean arterial pressures are measured. Mean arterial pressure (MAP) represents the driving pressure to the peripheral organs, and it can be either calculated (MAP = diastolic pressure + 1/3 pulse pressure) or measured by integrating the area under the arterial pressure waveform. The latter method is independent of heart rate and the assumption that diastole represents two thirds of the cardiac cycle.21
Some indications for arterial line placement may include: expectation of hemodynamic instability regardless of etiology; need for continuous blood pressure measurement when using vasoactive drugs (e.g., dopamine, nitroprusside); respiratory insufficiency; intubation for more than 4 to 6 hours; and the need for frequent arterial blood sampling. Some anesthesiologists recommend arterial line placement in situations in which the potential for rapid decrease in blood pressure exists. It has also has been recommended for morbidly obese patients for whom appropriate size cuffs are not available.
Cannulation of the radial artery must be preceded by evaluation of arterial supply to the hand by the Allen test.22 Palpate the radial and ulnar pulses. Ask the patient to make a tight fist with her hand in supine position. Occlude both radial and ulnar arteries with your thumbs. Ask the patient to open and close her hand multiple times (this will make the palm pale). Then release your thumb from one of the arteries. The palm should flush in no more than 5 seconds. Persisting pallor of the palm indicates insufficiency or occlusion of the released artery. Repeat the same procedure and test the other artery. Local anesthesia should be used, as it will both decrease the patient's pain and increase your success rate.
Thrombosis, infection, bleeding, vascular or nerve trauma, and accidental injection of intravenous drugs are potential complications.
Pulmonary Artery Catheter
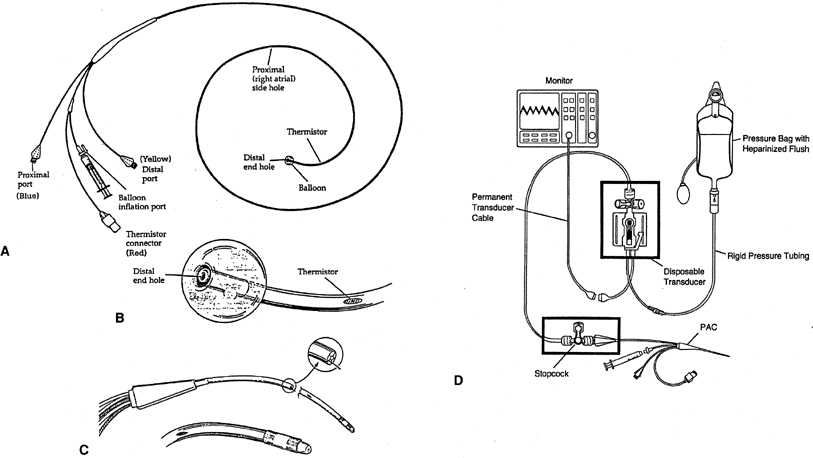
The pulmonary artery catheter (PAC), often called the Swan–Ganz catheter, is a triple lumen, flow-directed, balloon-tipped, thermodilution catheter (Fig. 1). The catheter's length ranges from 60 to 110 cm and is 2.3 mm (7 Fr) in outside diameter. The standard catheter has 3 ports (a proximal infusion port, a distal infusion port, and a balloon inflation port) and the thermistor connector in its proximal end. The catheter's shaft is mainly made of a polyvinyl chloride derivative and is radiopaque.
The proximal infusion port exits 30 cm from the tip of catheter and after correct insertion should be located in the patient's right atria. This port is used to infuse fluids or medications, and when connected to a transducer with a heparinized line, it is used to continuously monitor the right atrial pressure (RAP), which is equivalent to the central venous pressure (CVP).
The distal infusion port exits at the tip of the catheter, and after correct insertion, it should rest in a branch of the patient's pulmonary artery. This port is connected to a transducer with a heparinized pressure line (continuous flush of 3 mL per hour of heparinized solution in a bag at a pressure of 300 mmHg) to maintain the lumen patent and continuously monitor the pulmonary artery pressure (PAP) when the balloon is deflated, and intermittently the pulmonary capillary wedge pressure (PCWP) when the balloon is inflated. Both the proximal and the distal lumina of the catheter may be used to withdraw samples of venous blood for laboratory studies.
The lumen of the balloon's inflation port ends in small latex balloon, located 0.5 cm from the catheter's tip. The balloon is inflated at the time of catheter advancement and when PCWP is needed. The fully inflated balloon (1.5 mL) creates a recess for the tip, preventing the tip from perforating vessels, valves, or chambers as the catheter is advanced.21 While floating the catheter, there is no limit to the duration of inflation; however, once wedged, it should generally not remain inflated for more than 1 minute.
The thermistor is a temperature sensor and transducer, located in the outer surface at 4 cm from the catheter's tip that can be attached to a thermodilution cardiac output computer. When cardiac output measurement is desired, 10 mL of injectate (usually normal saline at room temperature or a known cold temperature) is infused into the proximal port. The thermistor will determine the blood's temperature at the tip of the catheter before and after the injectate infusion, and the computer will calculate the cardiac output.
Conventional PAC measure pressure and flow is appropriate for assessment of left ventricular function, but right ventricular function, which is more dependent on volume than pressure, is not assessed.23 The standard PAC has been modified to accomplish other functions. The oxymetric PAC, in conjunction with a bedside microprocessor, provides continuous determination of mixed venous blood's hemoglobin oxygen saturation (SvO2), which allows continuous calculation of oxygen consumption (VO2). Another enhanced PAC can measure right ventricular end-diastolic volume and ejection fraction through a combination of electrode sensing and thermodilution.24 Right ventricular ejection fraction catheters allow recognition of right and left ventricle interdependence.25 New thermodilution catheters (with a thermal filament) can measure cardiac output continuously.26 These modified catheters are 7.5 Fr and require an 8.0-Fr introducer. There are other catheters with additional ports that exit 14 cm from the tip through which medication can be given or for passing temporary pacemaker leads into the right ventricle. However, the small size of these ports renders them ineffective for resuscitation with infusion of large volumes of fluid or blood.
INDICATIONS FOR PAC PLACEMENT IN OBSTETRIC PATIENTS
Currently, the PAC is used in obstetrics in the management of critically ill patients or those at risk for sudden decompensation and in clinical investigations that attempt to define the pathophysiology of various disease processes or evaluate therapy of a specific condition.
A list of obstetric conditions for which invasive hemodynamic monitoring may assist in their management was published by the American College of Obstetrics and Gynecology (ACOG) in 1992.27 Invasive monitoring is not needed in every patient with one of these conditions, nor is this an all-inclusive list. This list can be divided into:
- Obstetric patients with acute critical condition or whose condition is subject to rapid deterioration:
- Sepsis with refractory hypotension or oliguria (septic shock);
- Unexplained or refractory pulmonary edema, heart failure, or oliguria;
- Severe preeclampsia with pulmonary edema or persistent oliguria;
- Intrapartum or intraoperative sudden cardiovascular decompensation (i.e., amniotic fluid embolism);
- Severe hypovolemic shock (massive hemorrhage);
- Adult respiratory distress syndrome;
- Shock of undefined etiology.
- Sepsis with refractory hypotension or oliguria (septic shock);
- Obstetric patients with chronic cardiovascular or metabolic diseases:
- New York Heart Association class III and IV cardiac disease*;
- Cardiomyopathy irrespective of etiology;
- Uncontrolled hyperthyroidism or pheochromocytoma;
- Unstable coronary artery disease.
- New York Heart Association class III and IV cardiac disease*;
*Particularly dangerous structural or physiologic disturbances include primary pulmonary hypertension, Eisenmenger's physiology, aortic coarctation, and mitral stenosis. More precise assessment of their base line condition, both early in pregnancy to assess the risk of continuing the pregnancy and during labor and delivery, as well as prompt evaluation of complications and subsequent therapeutic decisions, should favorably affect both management and outcome.27
CONTRAINDICATIONS FOR PAC PLACEMENT
In general, contraindications are28:
- Right heart valvular disease: Tricuspid or pulmonary valvular stenosis or prosthetic valves.
- Right-to-left shunt: By definition, pulmonary blood flow is reduced, and the balloon-tipped catheter is more likely “to be floated” into the systemic side of the shunt. Even if placed in the pulmonary artery, the inflated balloon can significantly increase the shunt.
- Previous pneumonectomy: Balloon inflation may precipitate an unacceptable rise in pulmonary vascular resistance, and although a rare complication, pulmonary artery rupture in such a patient would almost certainly be fatal.
- Latex allergy: Unless latex-free catheter is available.
- Anticoagulation or severe coagulopathy: This is a relative contraindication that can be bypassed by avoiding percutaneous venepuncture and cannulation. In these cases, venous cut down of the left basilic vein is recommended.
- Patient at risk of severe arrhythmias: Although not common, complete AV block can occur in patients with preexisting left bundle branch block. In these cases, the appropriate transthoracic pacing equipment must be available.
Central Venous Access
The two most common vascular approaches are, in order of preference:
- Right internal jugular vein: Provides a nearly straight access to right atria and ventricle, and offers a low risk of creating a pneumothorax.
- Left subclavian vein: Provides a more direct access to the vena cava and offers less risk of thoracic duct damage, as compared with the left internal jugular vein.
- The femoral and antecubital veins are used less frequently because of greater difficulty in positioning the catheter. Additionally, use of the inguinal area in obstetrics may limit access to and manipulation of the catheter at critical times such as during delivery.29
INSERTION TECHNIQUE
- Set up. At the time of publication, a video is available at this address:http://www.manbit.com/PAC/videos/video1.wmv
- Check patient's allergies record (especially iodine and latex).
- Patient must be monitored with continuous EKG (V2 is recommended) and EFM.
- The catheter's proximal and distal lumina should be flushed and purged of air and the balloon checked for symmetrical inflation, absence of an air leak, and ease of spontaneous deflation.
- Check all tubing, stopcocks, and transducer connections for a tight fit. Supervise establishment of zero reference point, flushing of pressure tubing, and calibration of pressure transducer.
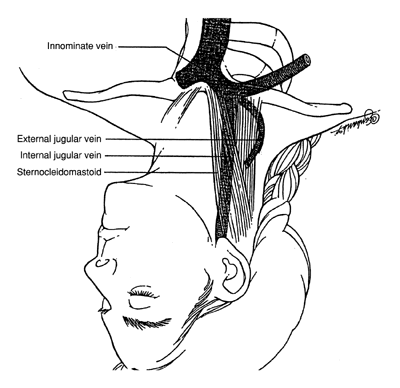
- If the internal jugular approach is selected, the patient is positioned in slight Trendelenburg position (head tilted below the horizontal) with a wedge under the ipsilateral hip and asked to turn her head to the side opposite the vessel selected for cannulation.
- The selected insertion site is then prepared and draped in a sterile fashion. If a povidone-iodine preparation (Betadine) is used, it should be left in contact with the skin at least 2 minutes.
- The operator should be gowned and gloved.
- A resuscitation cart should be available at the bedside.
- Check patient's allergies record (especially iodine and latex).
- Central vein percutaneous cannulation: Catheter-over-guidewire modified technique. At the time of publication, a video is available at this address:http://www.manbit.com/PAC/videos/video2.wmv
- Inject the skin and make a wheal made over the carotid artery (Fig. 2) with 1% Xylocaine and a 21- or 22-gauge 5-cm needle.
- The needle (“finder needle”) is then directed into the patient's neck and toward the ipsilateral nipple at a 45° angle, aspirating for blood as a tract toward the vessel is anesthetized. Often the vein walls will be collapsed, one against the other, by the pressure of the needle, and the vessel is completely traversed without blood return. Accordingly, if a tract of the entire length of the needle has been anesthetized and no blood has returned, the operator should slowly withdraw the needle, maintaining a small amount of negative pressure on the syringe. Failure to achieve blood return merits repositioning the patient and further attempts, each time redirecting the angle by approximately 5° medial or lateral to the prior attempt.
- Once the vessel is located (free-flowing blood returns), the finder needle is left free in the patient's neck to serve as a guide for recannulation of the vessel with an 18-gauge needle (“insertion needle”), following which a vascular J-tipped guidewire is passed into the vessel. The wire should pass freely and without resistance and should never be withdrawn through the cutting edge of the needle for fear of severing the wire.
- After the wire is passed into the vessel, the needle is withdrawn over the wire.
- A scalpel is used to make a 3- to 4-mm cut about the wire, following which the larger 7.5- or 8-Fr vascular access catheter is passed, with the assistance of a vein dilator, over the wire.
- The wire and dilator are then withdrawn and ready withdrawal of blood through the catheter introducer should be achieved. If there is any doubt as to whether the blood is arterial or venous, blood gas analysis can be performed.
- Inject the skin and make a wheal made over the carotid artery (Fig. 2) with 1% Xylocaine and a 21- or 22-gauge 5-cm needle.
- Intracardiac passage and intrapulmonary positioning. At the time of publication, a video is available at this address:http://www.manbit.com/PAC/videos/video4.wmv
- Connect the distal port of the catheter to the pressure transducer and oscilloscope monitor.
- The catheter is next advanced through an introducer at the venous access site.
- Fully inflate the balloon (1.5 mL of air) after the tip enters the vessel. This will be marked by the appearance of oscillations in the monitor reflecting the pressure in the vein (normal jugular, subclavian, and superior vena cava pressure is 1–6 mmHg). In an average size individual, this is obtained after insertion of approximately 15 cm of the catheter. If resistance to balloon inflation is encountered, the catheter should be advanced further into the vessel and a repeat attempt made at inflation. This will usually be successful, as the caliber of the vessels increases as the catheter is advanced centrally.
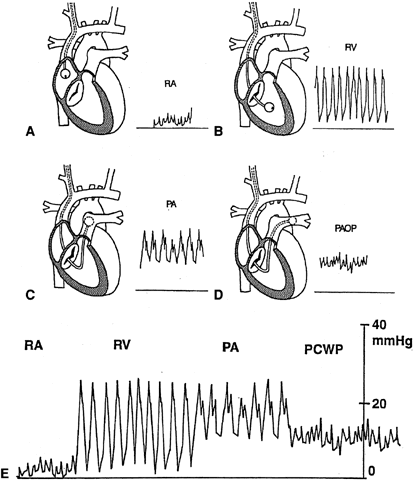
- Monitor continuously the pressure tracings to determine tip location (Fig. 3). By slowly advancing the balloon-tipped catheter, it will be carried along and directed into position by venous blood flow.21, 28, 29
- The pressure tracing in the superior vena cava, its tributaries, and the right atria is the same. It is a low-amplitude pressure tracing that varies with the respiratory cycle (i.e., pressure falls with inspiration and rises with expiration).
- Continued advancement of the catheter tip across the tricuspid valve into the right ventricle results in a spiking waveform, representative of the pulsatile systolic pressure (normal right ventricular systolic pressure is 15–30 mmHg). The pressure in the right ventricle during diastole should be the same as the pressure in the right atrium.
- Subsequently, as the pulmonary artery is entered, another spiking waveform of lower amplitude is identifiable, measuring now diastolic pressures above 0 mmHg (normal pulmonary artery diastolic pressure is 6–12 mmHg), whereas the systolic pressure, in normal conditions, should be equal to the right ventricular systolic pressure.
- The next waveform obtained, a damped tracing with respiratory variation, is the pulmonary capillary wedge pressure. If the balloon is deflated, a pulmonary artery tracing reappears. The wedge pressure is the same as the diastolic pressure in the pulmonary artery, unless there is pulmonary hypertension. A true pulmonary capillary wedge pressure is verified by: conversion of a pulmonary artery pressure tracing to a pulmonary capillary wedge pressure tracing when the balloon is inflated; the presence of respiratory variation in the pressure tracing; and a calculated mean pulmonary artery pressure higher than the pulmonary capillary wedge pressure.
- The pressure tracing in the superior vena cava, its tributaries, and the right atria is the same. It is a low-amplitude pressure tracing that varies with the respiratory cycle (i.e., pressure falls with inspiration and rises with expiration).
- Routine chest radiography to verify catheter positioning is not necessary if the insertion was uncomplicated and the surgeon is certain the chest cavity was not entered. Verification of proper positioning of the pulmonary artery catheter is dependent on obtaining a high quality and appropriate pressure tracing, not by chest radiograph.
- Connect the distal port of the catheter to the pressure transducer and oscilloscope monitor.
The ability to obtain accurate tracings over prolonged periods can be enhanced by the use of two devices, which are particularly useful in situations that mandate catheter repositioning. A catheter introducer system containing a one-way valve allows a malfunctioning catheter to be advanced, withdrawn, or changed without loss of the venous access. Additionally, sheaths are available that fit over the catheter itself and attach to the introducer port. The sheaths maintain sterility of a segment of the pulmonary artery catheter, allowing its advancement or withdrawal as necessary to obtain accurate pressure tracings.
DATA COLLECTION
The hemodynamic parameters can be subdivided in the cardiovascular and pulmonary profiles (Table 1).
Table 1. Hemodynamic parameters
Hemodynamic Parameters | Abbreviation | Formula | Units |
Cardiovascular |
|
|
|
Central venous pressure | CVP | CVP = RAP = RVEDP | mmHg |
Pulmonary capillary wedge pressure | PCWP | PCWP = LAP = LVEDP | mmHg |
Cardiac output | CO | measured by thermodilution | L/min |
Cardiac index | CI | CI = CO/body surface area | L/min/m2 |
Stroke volume | SV | SV = CO/heart rate | mL/beat |
Mean arterial pressure | MAP | MAP = diastolic + (1/3)(systolic - diastolic) | mmHg |
Left ventricular stroke work | LVSW | LVSW = (MAP – PCWP) × SV × (0.0136) | g × m |
Right ventricular stroke work | RVSW | RVSW = (PAP – CVP) × SV × (0.0136) | g × m |
Systemic vascular resistance | SVR | SVR = (MAP – RAP) × 80/CO | dynes × sec × m2/cm5 |
Pulmonary vascular resistance | PVR | PVR = (PAP – PCWP) × 80/CO | dynes × sec × m2/cm5 |
Pulmonary |
|
|
|
Arterial O2 content | CaO2 | CaO2 = (PaO2 × 0.003) + (Hb × 1.36) × Sao2 | mL O2/dL blood |
Mixed venous O2 content | CvO2 | CvO2 = (PvO2 × 0.003) + (Hb × 1.36) × SvO2 | mL O2/dL blood |
Arterial – mixed venous dfference in O2 content | avDO2 | avDO2 = CaO2 – CvO2 | mL O2/dL blood |
Oxygen delivery | DO2 | DO2 = (CaO2) × CO × 10 | mL/min |
Oxygen consumption or uptake | VO2 | VO2 = (CaO2 – CvO2) × CO × 10 | mL/min |
Oxygen extraction ratio | ERO2 | O2 ER = VO2/DO2(×100) | % |
Mixed venous oxygen saturation | SvO2 | SvO2 | % |
Cardiovascular Profile
In the ICU, blood pressure (BP) and mean arterial pressure (MAP) are obtained through an arterial line; heart rate and rhythm are monitored by continuous electrocardiography. Hemodynamic parameters are either directly measured or calculated (by formula) continuously or intermittently from data obtained with the PAC.
- Central venous pressure (CVP) is equal to the right atrial pressure (RAP) and should be equal to the right ventricular end-diastolic pressure (RVEDP) in the absence of tricuspid pathology.
- Pulmonary capillary wedge pressure (PCWP) is intermittently obtained from the transducer connected to the distal port. The PCWP is equal to the left atrial pressure (LAP) and should be equal to the left ventricular end-diastolic pressure in the absence of mitral pathology. PCWP is also known as pulmonary artery occlusion pressure (PAOP) and pulmonary artery wedge pressure (PAWP).
- Cardiac output (CO) measures the amount of blood ejected by the ventricle each minute. It is intermittently measured by the thermodilution method.
- Cardiac index (CI) is the CO divided by the patient's body surface area (BSA). Indexed parameters refer to values divided by the patient's body surface area (nomogram or formula). Indexed values are used in obstetrics despite the fact that specific nomograms for pregnant patients have not been developed.
- Stroke volume is the amount of blood pumped by the ventricle per systole. It can be calculated indirectly by CO divided by the HR. The stroke volume index (SVI) is the CO divided by the BSA.
- Left ventricular stroke work index (LVSWI) is the work performed by the left ventricle to pump blood into the aorta (systemic circulation).
- Right ventricular stroke work index (RVSWI) is the work performed by the right ventricle to pump blood into the pulmonary circulation.
- Systemic vascular resistance index is the resistance to flow from the left ventricle.
- Pulmonary vascular resistance index is the resistance to flow from the right ventricle.
NORMAL HEMODYNAMIC PARAMETERS DURING PREGNANCY
Clark and colleagues studied 10 healthy primiparous volunteers, younger than 26 years of age, carrying a single normal vertex fetus between 36 and 38 weeks confirmed by ultrasonography. Recordings were done in the left lateral recumbent position.30 Each patient served as her own control between 11 and 13 weeks postpartum (surrogate for the nonpregnant state). In summary, they reported a mean rise in cardiac output of 43%, as a result of increase in heart rate (17%) and stroke volume (27%), a significant fall in systemic vascular resistance (21%), and a greater decrease in pulmonary vascular resistance. No significant difference was found in left ventricular stroke work index nor PCWP (Table 2).
Table 2. Hemodynamic parameters in pregnancy
| Nonpregnant* | Pregnant |
Cardiac output (l/min) | 4.3 ± 0.9 | 6.2 ± 1.0 |
Heart rate (beats/min) | 71 ± 10 | 83 ± 10 |
Systemic vascular resistance (dyne × cm × sec–5) | 1530 ± 520 | 1210 ± 266 |
Pulmonary vascular resistance (dyne × cm × sec–5) | 119 ± 47 | 78 ± 22 |
Colloid oncolic pressure (mmHg) | 20.8 ± 1.0 | 18.0 ± 1.5 |
Colloid oncolic pressure – pulmonary capillary wedge pressure (mmHg) | 14.5 ± 2.5 | 10.5 ± 2.7 |
Mean arterial pressure (mmHg) | 86.4 ± 7.5 | 90.3 ± 5.8 |
Pulmonary capillary wedge pressure (mmHg) | 6.3 ± 2.1 | 7.5 ± 1.8 |
Central venous pressure (mmHg) | 3.7 ± 2.6 | 3.6 ± 2.5 |
Left ventricular stroke work index (g x m x m–2) | 41 ± 8 | 48 ± 6 |
*Nonpregnant represents the measurements obtained between 11 and 13 weeks postpartum.
(Clark SL, Cotton DB, Lee W, et al: Central hemodynamic assessment of normal term pregnancy. Am J Obstet Gynecol 161:1439 1989)
No longitudinal hemodynamic studies have been done during the first and second trimesters. Longitudinal studies using thoracic electrical bioimpedance31 and two-dimensional and M-mode echocardiography32 33 have reported changes in hemodynamics during normal pregnancy.
Pulmonary Profile
The next parameters are calculated based on PAC data, arterial and mixed venous blood gas analysis, hemoglobin levels, and the patient's fraction of inspired oxygen (FIO2).
- Arterial O2 content (CaO2) represents the total amount of oxygen in arterial blood, including that bound and transported by hemoglobin and the dissolved in plasma.
- Mixed venous O2 content (CvO2) represents the total amount of oxygen in mixed venous blood, including that bound and transported by hemoglobin and that dissolved in plasma.
- Arterial–mixed venous difference in O2 content (avDO2 = CaO2 – CvO2) represents the amount of oxygen extracted from the blood by peripheral organs/tissue/cells.
- Oxygen delivery (DO2) is the rate of oxygen transport in arterial blood per minute. This depends directly on CO and CaO2.
- Oxygen consumption or uptake (VO2) represents the tissue extraction of oxygen. This depends directly on CO and avDO2.
- Oxygen extraction ratio is the fractional uptake of oxygen from the systemic microcirculation. It is equivalent to the ratio between DO2 and VO2.
- Mixed venous oxygen saturation (SvO2): Mixed venous blood is the blood obtained from the distal port of the PAC. Oxygen's partial pressure (PvO2) and saturation in mixed venous blood (SvO2) can be determined intermittently by blood gas analysis and continuously monitored and plotted by oxymetric PACs. A low SvO2 could be caused either by a high VO2 or a low CO2, SaO2, or hemoglobin concentration.
The advantages of continuous monitoring of mixed venous blood saturation, as opposed to arterial blood saturation, are many. First, arterial blood samples will almost always have a saturation of 90% or greater, corresponding to a pO2 of 60–100 mmHg or greater. Because of the shape of the hemoglobin dissociation curve, fluctuations at these higher levels of oxygen tension are reflected by very small corresponding changes in saturation. Conversely, at the lower levels of oxygen present in venous blood, a linear relationship exists between saturation and tension, making it a sensitive test for detection of physiologic instability. Second, although an arterial blood analysis provides useful information concerning pulmonary oxygen exchange, ventilation, and shunt, it provides little information regarding the overall adequacy of oxygen delivery to peripheral tissues. Because the mixed venous gas reflects the end product of supply and demand, it is superior in this respect. Finally, the addition of a thermodilution cardiac output, in conjunction with a mixed venous gas, can support or refute clinical assumptions made based on the mixed venous oxygen saturation. For example, improvement of mixed venous oxygen saturation with a stable cardiac output is a good prognostic sign and heralds clinical improvement. If, however, the same change in the mixed venous oxygen saturation is accompanied by a 100% increase in cardiac output, it may simply be the first sign of sepsis.29 Continuous monitoring of SvO2 has been advocated for titration of vasoactive and inotropic drugs, adjustment of positive end-expiratory pressure, evaluation of fluid therapy, routine patient care, and an early warning system for changes in cardiorespiratory status.34 Few data are available on the use of this technology in pregnant women. Normal SvO2 values during pregnancy have not been determined yet. Nonpregnant normal SvO2 values are 75–85%, persistent SvO2 below 60% being abnormally low.29
DATA INTERPRETATION
One of the main objectives of critical/intensive care monitoring and intervention is to prevent or treat circulatory failure. Circulatory failure is defined as the inability of the cardiovascular system to oxygenate and extract waste material adequately from cells, tissues, or organs. Circulation depends on intact vascular system, adequate oxygen exchange, and cardiac function. Cardiac output is determined by stroke volume and heart rate. Stroke volume is determined by four variables: preload, myocardial contractility, afterload, and heart rate.
Preload is the pressure in the ventricles determined by the amount of blood that returns to heart and the ventricular wall compliance. The measurement for the right ventricular preload is the CVP or RAP. The measurement for the left ventricular preload is the PCWP. The “Frank-Starling law of the heart” describes that an increase in preload stretches the myocardial fiber and causes more forceful contraction up to a point of stretch beyond which the heart fails to contract (dissociation of the actin-myosin complex). The preload can be increased by the administration of crystalloid, colloid, or blood and can be decreased by the use of a diuretic, a vasodilator, or by phlebotomy.
Afterload is the resistance against which blood is pumped. The SVR and PVR are the afterloads to the left and right ventricles, respectively. Increased afterload during heart failure deteriorates cardiac output. Pure α-adrenergic drugs, such as phenylephrine, are used to increase afterload. Decreases in afterload or systemic vascular resistance can be achieved by numerous agents (e.g., hydralazine, labetalol, sodium nitroprusside). In cases of pulmonary hypertension, short-term treatment with epoprostenol may have a role in decompensated heart failure.35
Contractility is the inotropic state (“inherent strength”). RVSWI and LVSWI reflect the performance of the right and left ventricle, respectively. In low-output cardiac failure, both preload and afterload should be optimized first. If this fails to restore the CO to an acceptable level, attention should be directed to improving myocardial contractility. Digitalis and β-sympathomimetics, such as dopamine and dobutamine, are effective in improving myocardial contractility.
Cardiac output can be affected by either very fast or very slow heart rates. The pathophysiologic basis of tachycardia should be determined and corrected (fever, hypovolemia, pain, hypothyroidism). Sustained tachycardia can lead to heart failure from shortened systolic ejection and diastolic filling times or increased myocardial oxygen consumption (ischemia). Fast rate arrhythmias can be treated with adenosine,36 propranolol, digoxin, or a calcium channel blocker such as verapamil.
COMPLICATIONS
Pulmonary artery catheterization is invasive and, as such, can never be entirely free of complications, but the rate of complications is low, and the technique has become a routine procedure in virtually all ICUs (Table 3).37, 38 Data misinterpretation is an important complication because a monitoring technique can only be as good as the interpretation of the data it provides and the clinical application of this interpretation.39
Table 3. Common complications from pulmonary artery catheter insertion and use
Complication | Frequency (%) |
After placement | |
Pneumothorax | 2 |
Arterial puncture | 2–15 |
Hemorrhage | 2 |
Transient dysrhythmia | 11–87 |
Ventricular fibrillation | 2 |
After use | |
Mural thrombus | 14–91 |
Infection | 5–45 |
Pulmonary infarction | 1–7 |
Pulmonary artery rupture | 0.06–2.0 |
(Van Hook JW, Hankins GDV: Invasive hemodynamic monitoring. Prim Care Update Ob/Gyns 4:39, 1997)
DOES PULMONARY ARTERY CATHETERIZATION IMPROVE OUTCOME?
Between 1945 and 1970, pulmonary artery catheterization was performed exclusively in the cardiac catheterization laboratory by few cardiologists, using semi-rigid catheters under fluoroscopic guidance.40 At that time, their purpose was to diagnose congenital heart diseases, select candidates for surgical correction, and improve understanding of pathophysiology. Swan, Ganz, Forrester, Marcus, Diamond, and Chonette, in 1970, reported pulmonary artery catheterization at the patient's bedside using a flexible flow-directed balloon-tipped catheter, without fluoroscopic guidance.41
Shortly thereafter, the catheter was commercially available, and intensive care unit and operative room physicians used the pulmonary artery catheter (PAC) to determine, monitor, and modify therapy in critically ill and/or hemodynamically unstable patients with a broad spectrum of conditions, accepting its benefits without randomized clinical trials.
In 1996, based on three retrospective observational studies,39, 40, 41 experts in critical care medicine called for either a moratorium on the use of PAC for the management of critically ill patients or randomized clinical trials to demonstrate its benefit.42 The first two studies reported that mortality in patients with acute myocardial infarction complicated by congestive heart failure was significantly increased in those who underwent pulmonary artery catheterization. The mortality in patients with acute myocardial infarction complicated by cardiogenic shock was essentially the same with or without PAC. The third study was a multicenter, nonrandomized observational study in which 2184 of 5735 critically ill patients admitted to the medical ICU with nine disease categories underwent pulmonary artery catheterization. Each case was paired to a control with a comparable diagnosis. The results of this paired analysis, in which differences in severity of illness was statistically adjusted, reported increased mortality and cost in patients with PAC.43
In response to the debate, The National Heart, Lung and Blood Institute and the United States Food and Drug Administration in conjunction with several professional societies convened a consensus conference. The proceedings were published in 1997,44 and recommendations were published in 2000.45 This workshop developed four recommendations. Its highest priority recommendation was for implementation of educational programs for training, certification, and quality improvement for physicians and nurses using the PAC. The second set of recommendations included conducting clinical trials investigating pulmonary artery catheterization safety and effectiveness in the following conditions: persistent/refractory congestive heart failure (class IV NYHA), low-risk coronary artery bypass graft surgery, hypoxic lung syndromes, mainly the acute respiratory distress syndrome (ARDS), and severe sepsis/septic shock, conditions for which equipoise existed as to its benefit.
Randomized trials of patients undergoing high risk surgery, patients with congestive heart failure, and patients with general critical illness have failed to show a benefit from the use of the PAC 46, 47, 48. In a recent randomized trial patients with acute lung injury/ARDS were randomized to receive hemodynamic management with a conventional central venous line versus a pulmonary artery catheter. There was no difference in mortality between both groups and there were more complications in the PAC group.49
To date, the evidence dictates that the PAC does not improve outcomes in patients with ALI/ARDS, congestive heart failure, high risk surgical patients, and in the general critically ill. Still, data is needed on patients with pulmonary hypertension, COPD, and patients undergoing dialysis.
Essentially, PAC is a diagnostic tool that will improve outcome, only if it permits timely diagnosis and management of conditions for which proven treatment exists. Conversely, use of the PAC will unlikely improve outcome if utilized “late” (i.e., when organ failure and irreversible oxygen debt has already occurred) and/or in conditions for which no therapeutic intervention exists.47, 48, 49 To maximize patient outcome, placement of the PAC, acquisition and interpretation of data, and intervention must be performed by trained critical care providers.50, 51
The use of the “Swan-Ganz” catheter in obstetrics was first reported in 1977, and it was used to evaluate hemodynamic parameters at 12 and 36 hours postpartum in a case of toxemia complicated by pulmonary edema.52 This PAC was introduced through the femoral artery after a cesarean section. Since then, obstetricians have become more interested and formally trained in the care of the critically ill obstetric population, which in its majority is composed by relatively young and healthy patients acutely affected by conditions unique to pregnancy or by preexisting disorders affected by the pregnancy itself. ACOG published a technical bulletin on invasive hemodynamic monitoring, with emphasis on its indications and data interpretation in 1992.27 It should be noted that the Pulmonary Artery Catheterization and Clinical Outcomes Workshop did not include the participation of ACOG nor the Society for Maternal-Fetal Medicine and did not address the use of PAC in the critically ill obstetric patient.53, 54
REFERENCES
Weil MH, Bisera J, Trevino RP et al: Cardiac output and end-tidal carbon dioxide. Crit Care Med 13: 907, 1985 |
|
Shibutani K, Muraoka M, Shirasaki S et al: Do changes in end tidal PCO2 quantitatively reflect changes in cardiac output? Anesth Analg 79: 829, 1994 |
|
Falk JL, Rackow EC, Weil MH: End-tidal carbon dioxide concentration during cardiopulmonary resuscitation. N Engl J Med 318: 607, 1988 |
|
Sanders AB, Kern KB, Otto CW et al: End-tidal carbon dioxide monitoring during cardiopulmonary resuscitation: A prognostic indicator for survival. JAMA 262: 1347, 1989 |
|
Falk JL, O'Brien JF, Kerr R: Fluid resuscitation in traumatic hemorrhagic shock. Crit Care Clin 8: 323, 1992 |
|
Shippy CR, Appel PL, Shoemaker WC: Reliability of clinical monitoring to assess blood volume in critically ill patients. Crit Care Med 12: 107, 1984 |
|
Amoroso P, Greenwood RN: Posture and central venous pressure measurement in circulatory volume depletion. Lancet 2: 258, 1989 |
|
Belfort MA, Rokey R, Saade GR et al: Rapid echocardiographic assessment of left and right heart hemodynamics in critically ill obstetric patients. Am J Obstet Gynecol 171: 884, 1994 |
|
Balachundhar S, Talmor D. Echocardiography for management of hypotension in the intensive care unit. Crit Care Med 2007; 35(8): S401-S407. |
|
Clark SL, Southwick J, Pivarnik JM et al: A comparison of cardiac index in normal term pregnancy using thoracic electrical bio-impedance and oxygen extraction (Fick) techniques. Obstet Gynecol 83: 669, 1994 |
|
Weil MH, Rackow EC, Trevino R et al: Difference in acid-base state between venous and arterial blood during cardiopulmonary resuscitation. N Engl J Med 315: 153, 1986 |
|
Bakker J, Coffernils M, Leon M et al: Blood lactate levels are superior to oxygen-derived variables in predicting outcome in human septic shock. Chest 99: 956, 1991 |
|
Aduen J, Bernstein WK, Khastgir T et al: The use and clinical importance of a substrate-specific electrode for rapid determination of blood lactate concentrations. JAMA 272: 1678, 1994 |
|
Curtis SE, Cain SM: Regional and systemic oxygen delivery/uptake relations and lactate flux in hyperdynamic, endotoxin-treated dogs. Am Rev Respir Dis 145: 348, 1992 |
|
Nordstrom L, Achanna S, Naka K et al: Fetal and maternal lactate increase during active second stage of labour. Br J Obstet Gynecol 108: 263, 2001 |
|
Fiddian-Green RG: Tonometry: Theory and applications. Intensive Care World 9: 60, 1992 |
|
Fiddian-Green RG: Tonometry: II. Clinical use and cost implications. Intensive Care World 9: 130, 1992 |
|
Marik PE: Gastric intramucosal pH: A better predictor of multiorgan dysfunction syndrome and death than oxygen-derived variables in patients with sepsis. Chest 104: 225, 1993 |
|
Bendjelid K, Romand JA. Fluid responsiveness in mechanically ventilated patients: A review of indices used in intensive care. Intensive Care Med 2003; 29: 352-360. |
|
Osman D, Ridel C, Ray P, et al. Cardiac filling pressures are not appropiate to predict hemodynamic response to volume challenge. Crit Care Med 2007; 35(1): 64-68. |
|
Marino PL: The ICU Book, 2nd ed. Baltimore, Williams & Wilkins, 1998 |
|
Bates B: A Pocket Guide to Physical Examination and History Taking, 2nd ed, p 61. Philadelphia, JB Lippincott, 1995 |
|
Barie PS: Advances in critical care monitoring. Arch Surg 132: 734, 1997 |
|
Cockroft S, Withington PS: The measurement of right ventricular ejection fraction by thermodilution: A comparison of values using differing injectate ports. Anaesthesia 48: 312, 1993 |
|
Mihm FG, Gettinger A, Hanson CW III et al: A multicenter evaluation of a new continuous cardiac output pulmonary artery catheter system. Crit Care Med 26: 1346, 1998 |
|
Dhainaut JF, Brunet F, Monsallier JF et al. Bedside evaluation of right ventricular performance using a rapid computerized thermodilution method. Crit Care Med 15:148, 1987 |
|
The American College of Obstetricians and Gynecologists. Invasive Hemodynamic in Obstetrics and Gynecology. ACOG Technical Bulletin No. 175. In 2001 Compendium of Selected Publications, pp 567–572. Washington, DC, ACOG, 2001 |
|
Pybus A: The “St. George” Guide to Pulmonary Artery Catheterization. http://www.manbit.com/PAC/chapters/ PAC.cfm. |
|
Hankins GDV: Invasive hemodynamic monitoring in obstetrics. In Winn HN, Hobbins JC (eds): Clinical Maternal-Fetal Medicine, pp 157–165. New York, Parthenon Publishing, 2000 |
|
Clark SL, Cotton DB, Lee W et al: Central hemodynamics of normal term pregnancy. Am J Obstet Gynecol 161: 1439, 1989 |
|
van Oppen AC, van der Tweel I, Alsbach GP et al: A longitudinal study of maternal hemodynamics during normal pregnancy. Obstet Gynecol 88: 40, 1996 |
|
Gilson GJ, Samaan S, Crawford MH et al: Changes in hemodynamics, ventricular remodeling, and ventricular contractility during normal pregnancy: A longitudinal study. Obstet Gynecol 89: 957, 1997 |
|
Mabie WC, DiSessa TG, Crocker LG et al: A longitudinal study of cardiac output in normal human pregnancy. Am J Obstet Gynecol 170: 849, 1994 |
|
Divertie MG, McMichan JC: Continuous monitoring of mixed venous oxygen saturation. Chest 85: 423, 1984 |
|
Haywood GA, Adams KF Jr, Gheorghiade M et al: Is there a role for epoprostenol in the management of heart failure? Am J Cardiol 75: 44, 1995 |
|
Elkayam U, Goodwin TM Jr: Adenosine therapy for supraventricular tachycardia during pregnancy. Am J Cardiol 75: 521, 1995 |
|
Vincent JL: Complications associated with pulmonary artery catheterization. Crit Care Med 26: 1283, 1998 |
|
Matthay MA, Chatterjee K: Bedside catheterization of the pulmonary artery: Risks compared with benefits. Ann Intern Med 109: 826, 1988 |
|
Tuman KJ, Carroll GC, Ivakovich AD: Pitfalls in interpretation of pulmonary artery catheter data. J Cardiothorac Anesth 3: 625, 1989 |
|
Dexter L, Haynes FW, Burwell CS et al: Studies of congenital heart disease. J Clin Invest 26: 547, 1947 |
|
Swan HJC, Ganz W, Forrester J et al: Catheterization of the heart in man with use of a flow-directed balloon tipped catheter. N Engl J Med 283: 447, 1970 |
|
Dalen JE, Bone RC: Is it time to pull the pulmonary artery catheter? [editorial]. JAMA 276: 916, 1996 |
|
Connors AF, Speroff T, Dawson NV et al: The effectiveness of right-heart catheterization in the initial care of critically ill patients. JAMA 276: 889, 1996 |
|
Pulmonary Artery Catheter Consensus Conference Participants: Pulmonary Artery Catheter Consensus Conference. Crit Care Med 25:910, 1997 |
|
Pulmonary Artery Catheterization and Clinical Outcomes: National Heart, Lung and Blood Institute and Food and Drug Administration Workshop Report [consensus statements]. JAMA 283:2568, 2000 |
|
Binanay C, Califf RM, Hasselblad V, et al. Evaluation study of congestive heart failure and pulmonary artery catheterization effectiveness: the ESCAPE trial. JAMA 2005; 294: 1625-1633. |
|
Rhodes A, Cusack RJ, Newman PI, et al. A randomized controlled trial of the pulmonary artery catheter in critically ill patients. Intensive Care Med 2002; 28: 256-264. |
|
Sandham JD, Hull RD, Brant RF, et al. A randomized controlled trial of the use of pulmonary artery catheters in high risk surgical patients. N Engl J Med 2003; 348: 5-14. |
|
The National Heart, Lung, and Blood Institute Acute Respiratory Distress Syndrome (ARDS) Clinical Trials Network. Pulmonary-artery versus central venous catheter to guide treatment af acute lung injury. N Engl J Med 2006; 354: 2213-2224. |
|
Reynolds HN, Haupt MT, Thill-Baharozian MC et al: Impact of critical care physician staffing on patients with septic shock in a university hospital intensive care unit. JAMA 260: 3446, 1988 |
|
Brown JJ, Sullivan G: Effect on ICU mortality of a full-time critical care specialist. Chest 96: 127, 1989 |
|
Freund U, French W, Carlson RW et al: Hemodynamic and metabolic studies of a case of toxemia of pregnancy. Am J Obstet Gynecol 127: 206, 1977 |
|
Bowdle TA, Freund PR, Rooke GA: Cardiac Output. Redmond, WA: SpaceLabs Medical Inc, 1993 |
|
Baumgartner RG: Invasive hemodynamic monitoring in the critically ill or high-risk obstetric patient. In Harvey CJ (ed): Critical Care Obstetrical Nursing, pp 35–48. Gaithersburg, MD, Aspen, 1991 |