Laparoscopic Sterilization
Authors
INTRODUCTION
Laparoscopic sterilization was first performed in the late 1930s by Bösch1 in Switzerland. Independently, two American gynecologists, Powers and Barnes, developed a similar procedure in the United States.2 During the 1940s, female sterilization in the United States was generally performed only for medical indications. Elective sterilizations were subjected to a formula in which age multiplied by parity had to be equal or exceed 120 before the procedure could be considered. This general lack of demand for sterilization coupled with technical difficulties with the early laparoscopic equipment resulted in few American physicians attempting the new procedure. American interest remained dormant until the changing cultural climate of the late 1960s resulted in a demand for a safe, minimally invasive female sterilization procedure.
During this interim period, technical advances in optics and instrumentation pioneered by the Germans, Italians, and French made laparoscopy a much easier and safer procedure. Raoul Palmer of Paris adopted the use of the Trendelenburg position and uterine manipulator to give better access to the fallopian tubes and ovaries.3 He also popularized the use of biopsy forceps and unipolar current for tubal sterilization. After the publication of the first textbook in English on laparoscopy, a resurgence of interest in laparoscopy occurred in the United States.4 Propelled by the increasing demand for elective sterilization, laparoscopy became the most common method of interval sterilization in the United States by the mid 1970s. Conversely, sterilization became the most common indication for laparoscopy.5
Many methods of laparoscopic tubal sterilization have been described. The most commonly used methods today include the use of electrocoagulation, silastic bands, or mechanical clips to achieve occlusion of the fallopian tubes. Other potentially useful but uncommon techniques include endocoagulation and the laparoscopic Pomeroy procedure.
ELECTROCOAGULATION
Laparoscopic electrocoagulation is the oldest technique of laparoscopic sterilization. Electrocoagulation using unipolar current gained widespread popularity during the early years of laparoscopic sterilization but fell into disfavor after reports of increasing numbers of bowel burns resulting from the procedure. Although most bowel injuries were subsequently shown to be trocar injuries and not electrical burns, the majority of laparoscopists abandoned the use of unipolar electric current for sterilization.6 Today, the inherently safer bipolar electric current has essentially replaced unipolar current for tubal sterilization. Because of the widespread tubal destruction associated with electrocoagulation, this method is less affected by tubal thickness and mobility than many other methods. Thus, electrocoagulation may be preferable when the tube is edematous and thickened or cannot be easily mobilized for mechanical device placement. Conversely, the greater tubal damage associated with electrocoagulation makes tubal reversal more difficult should the patient regret her decision. Regardless of the method chosen for tubal occlusion, electrocoagulation should always be readily available during laparoscopic tubal sterilization both as a backup method of sterilization and for control of unexpected bleeding.
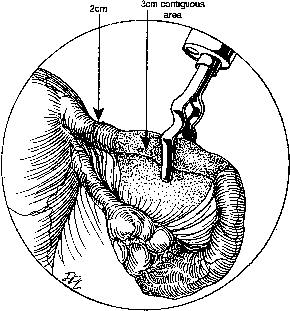
During sterilization with bipolar electrocoagulation, the fallopian tube is identified and grasped at the midisthmus region, approximately 2.5–3 cm from the uterotubal junction, with the bipolar forceps. The tube is tented up to ensure the forceps are not in contact with any other structure, and the current applied until coagulation is complete. Unlike the widespread coagulation seen during unipolar electrocoagulation, tissue destruction with bipolar current is confined to the area between and immediately adjacent to the bipolar paddles.7 Therefore, it is generally necessary to repeat the electrocoagulation an additional two times at immediately adjacent sites to duplicate the same amount of coagulation seen with unipolar current. Destruction of a minimum of 2 cm of tube has been suggested as adequate by some authorities,8 although others, including Kleppinger, advocate coagulation of at least 3 cm to ensure sterilization.9 Data from the CREST study also indicate that coagulation performed with three separate applications of the forceps is associated with a lower failure rate than when fewer applications are made.10
Although electrocoagulation of the tubal ampulla is more likely to produce complete occlusion, it will not achieve the same failure rate as coagulation of the isthmic portion of the tube.11 Conversely, coagulation of the tube too close to the cornu may lead to uteroperitoneal fistula formation. In 1930, Sampson12 described sprouts of endosalpinx growing out of the traumatized mucosa of the tubal stump. McCausland13 suggested that coagulation of the proximal isthmic fallopian tube tends to activate this process, which can then invade the tubal muscularis, penetrate the serosa, and result in a fistula. He named this endosalpingoblastosis. Recannulization frequently results in fistula sufficient to allow passage of sperm but usually not the ovum.14, 15 This may be one explanation of the high ratio of ectopic-to-intrauterine pregnancies after failure of sterilization by electrocoagulation. The correct technique for bipolar electrocoagulation is illustrated in Fig. 1.
If unipolar electrocoagulation is used, the initial site of coagulation should be chosen to allow any subsequent application to be closer to the uterus. Unipolar current returns to the ground through the path of least resistance. After the initial coagulation of the tube, the desiccated area has increased resistance, thus unipolar current applied distal to this site may flow to the end of the tube instead of through the uterus. If the distal end of the tube should touch bowel, a bowel burn could theoretically occur.
Classically, the fallopian tube was cut and divided after coagulation. A segment of tube can also be removed for histologic evaluation as part of this procedure. Some authorities now believe that division of the tube significantly increases the chance of tuboperitoneal fistula and subsequent ectopic pregnancy.16, 17 The risk of a tear in the mesosalpinx with subsequent hemorrhage is also increased with this technique, and any tissue submitted to pathology is often so distorted that an accurate tissue diagnosis cannot be made. As a result, division of the fallopian tube after electrocoagulation is no longer recommended.
Although gynecologists use electrosurgery almost daily, many are unfamiliar with the physics involved. The unfortunate designation of current as 'cut' and 'coag' is especially confusing as 'cut' current can coagulate and 'coag' current can cut depending on the manner in which it is used. A more appropriate scientific designation is nonmodulated current for 'cut' and modulated current for 'coag'. When used in a contact mode, nonmodulated (cut) current is a far more efficient desiccator of tissue than modulated (coag) current. In a similar situation, modulated current produces a rapid carbonization of the tubal surface that impends deeper electrocoagulation. Thus, nonmodulated current is the most appropriate current to use for tubal sterilization.
Electrosurgical units designed solely for tubal electrocoagulation generate only nonmodulated (cut) bipolar current while 'Bovie'-type electrosurgical generators permit the selection of either modulated (coag) or nonmodulated (cut) current in the bipolar mode. Unfortunately, many surgeons and operating room nurses automatically select the less-powerful 'coag' mode for tubal sterilization. The result may be a tubal lumen that remains viable despite the visual appearance of complete tubal coagulation.18
Many gynecologists also use a 'blanch, swell, and collapse' visual endpoint to determine complete tubal coagulation. However, it is uncertain whether this method is completely reliable.18 Consistent, adequate coagulation is best achieved by using an ammeter to document cessation of current flow rather than depending on a visual endpoint. Alternatively, a timed coagulation period of at least 10 seconds at 25 W of nonmodulated current usually ensures complete tubal occlusion.18, 19
The use of electrosurgical generators with bipolar forceps produced by different manufactures has been suggested as a cause of insufficient tubal coagulation.20 However, subsequent research would seem to indicate that complete coagulation is more dependent on selection of the proper waveform and power setting rather than generator-forceps mismatch.18, 19, 21
The most serious and feared complication occurring with the use of electrocoagulation is thermal injury to the bowel. The use of bipolar current eliminates the majority of risk of this complication. Care to ensure that only the fallopian tube is grasped with the forceps and that the tube is not touching other intra-abdominal structures should further reduce the risk of this complication.
SILASTIC RINGS
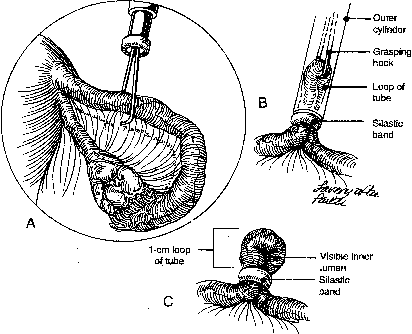
Efforts to replace electric current with a safer means of laparoscopic sterilization lead to the development of silastic rings for tubal occlusion.22 The silastic ring is a nonreactive silicone rubber ring with an inner diameter of 1 mm (Fig. 2). To permit radiographic identification, 5% barium sulfate is incorporated into the ring. The rings are applied with a specialized applicator device consisting of two concentric cylinders, the inner one of which contains grasping prongs at its distal end. The movement of these cylinders is controlled by a single ring grip. The silastic band is stretched over the inner ring using a conical-shaped applicator. Bands should not be loaded on the application until ready for use to prevent possible loss of elastic memory. Applicators are also available that accommodate two rings so that removal for reloading between banding is not required.
The preloaded silastic ring applicator may be introduced either through a second suprapubic puncture or through the operating channel of an operative laparoscope. The grasping forceps are extended and the fallopian tube is grasped approximately 2.5–3 cm distal to the uterotubal junction. The tube is drawn into the inner sleeve by retracting the tongs until resistance is felt. The ring is then pushed off the applicator and onto the tube using the sliding mechanism on the applicator. An adequate knuckle of tube should be approximately 1-cm long with an obvious inner loop (see Fig. 2).
Occasionally, the tubal serosa but not tubal lumen may be pulled into the ring. This knuckle of serosa can closely resemble a truly adequate 'knuckle'. However, close observation shows the absence of the vertical crease formed when an entire loop of tube is included in the ring.
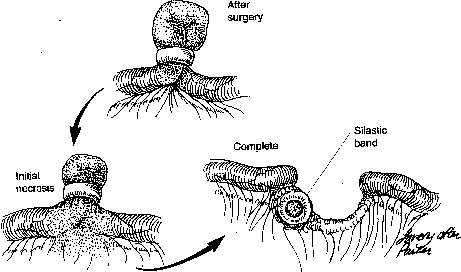
This knuckle of tube then undergoes necrosis from interruption of its blood supply. Complete absorption of the knuckle occurs in 3–6 months, at which time the proximal and distal stumps usually separate completely. The ring itself usually becomes covered with peritoneum and remains near the original occlusion site but may fall free into the abdominal cavity (Fig. 3). Occasionally, this characteristic has resulted in lawsuits when uninformed surgeons, operating for an ectopic pregnancy, have assumed that the absence of a ring on the tube indicated incorrect initial ring placement.
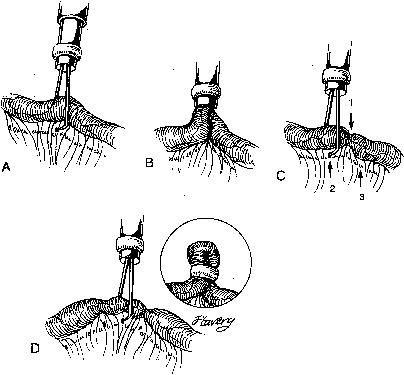
Difficulties with silastic ring placement can occur with thickened or adhesed fallopian tubes. These conditions often hinder complete retraction of the tube into the applicator. The end result is often application of the ring to a knuckle containing only serosa or complete transection of the tube. This complication can generally be prevented by: (1) slow withdrawal of the tube into the sleeve, thus allowing time for the tube to conform to the sleeve diameter; and (2) slightly advancing the entire applicator as the tube is drawn up to avoid counter-traction from the fixed uterine end of the tube. In the case of edematous or thickened tubes, using a 'milking' action with the tongs often allows edematous tubes to be drawn into the sleeve. Alternatively, the 'Yoon three grasp technique' may be used to allow ring placement on edematous tubes (Fig. 4).23 With excessively thick, edematous tubes or scarred tubes, the use of another method such as cautery should be considered as an alternative to attempted mechanical occlusion.
If the tube is transected, silastic rings may be placed proximal and distal to the transection, interrupting blood supply to the rent. Electrocoagulation of the free ends also may be used to achieve both hemostasis and tubal occlusion.
MECHANICAL CLIPS
Sterilization by mechanical clips is potentially the most reversible of all the laparoscopic methods. Originally, mechanical clips for tubal occlusion were essentially identical to the hemostatic clips used to occlude small bleeding vessels during surgery. These original clips had an unacceptably high failure rate. Such failures occurred when necrosis of the tubal muscularis beneath the clip eliminated the pressure on the deeper endosalpinx and allowed the tubal lumen to reopen. To prevent this complication, modern clips are designed to maintain a constant pressure as the tube undergoes necrosis. When properly placed, only 4 mm of tube and virtually none of the tubal blood supply are destroyed. Thus, elective tubal reanastomosis is more easily accomplished after mechanical clip tubal occlusion.24 The disadvantage of this limited destruction is that precise and accurate placement is required to achieve acceptable failure rates.
Today, there are primarily two mechanical clips in widespread use: the Hulka-Clemens clip and the Filshie clip.25, 26 The Hulka-Clemens clip consists of two toothed jaws of Lexan plastic joined by a metal hinge pin. The lower jaw possesses a distal hook. The stainless-steel pin (gold plated to reduce peritoneal irritation) maintains the clip in an open position. When completely advanced, the spring closes and locks the jaws. The Hulka applicator is 7 mm in diameter with a three-ring configuration at the handle. A fixed distal lower jaw cradles the clip while the mobile upper jaw opens and closes the clip. A center piston, when advanced, locks the clip closed. The Filshie clip is made of titanium and silicone. It is technically a simpler device than the Hulka-Clemens clip. A thick silicone coating instead of a metal spring is used to provide constant pressure on the tube.
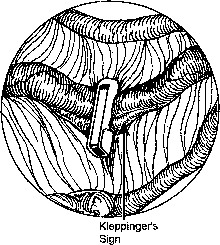
The loaded clip applicator is introduced with the clip in the closed position and the clip opened after the applicator is intra-abdominal. The clip is placed perpendicular to the tube at a site 1–2 cm from the uterotubal junction. With correct application, the mesosalpinx on the surface of the tube is pulled upward to resemble the flat triangle shape of an envelope flap (Kleppinger's 'envelope' sign) (Fig. 5). A grasper inserted through another abdominal port or the operating laparoscope can be used to place the tube on tension before clip application. This decreases the likelihood that the lumen will roll out of the clip during application. With Filshie clips, the distal tip of the applicator can generally be seen through the mesosalpinx when the clip is properly position completely around the tube. The clip may be repeatedly opened and repositioned until ideal position is achieved. The clip is then locked in place and the applicator withdrawn, leaving the clip in place on the tube.
ENDOCOAGULATION
A technique of laparoscopic sterilization using true cautery to coagulate the fallopian tubes has been developed by Semm.27 This system uses direct electric current to heat grasping forceps to 100–120°C. Coagulation occurs as a result of heat transfer from the forceps and not by heat generated from the effect of current passing through the tissue. This method, although rarely used in the United States, is popular in many parts of Europe. Proponents believe that endocoagulation is less likely than high-frequency electrocoagulation to stimulate tubal recannulization.
During endocoagulation as described by Semm, the tube is grasped 1–3 cm from the uterotubal junction. The tube is then coagulation in two adjacent areas. Semm continues to recommend transection of the tube after endocoagulation.
LAPAROSCOPIC POMEROY
One of the disadvantages of most laparoscopic sterilization techniques is the lack of a tissue specimen to document sterilization. Methods such as the Soderstrom snare technique, which can provide such a specimen, have not gained widespread acceptance.28 Recently, a laparoscopic version of the Pomeroy tubal ligation has been advocated27, 29 (Fig. 6). The laparoscopic Pomeroy may be performed using either two lower abdominal operating ports, or one midline suprapubic port and an umbilical operating laparoscope.
After the fallopian tube has been identified, a ligature of #0 plain gut with a pre-tied Roeder knot is inserted through one of the lower abdominal ports. The laparoscopic forceps are inserted through the opposite lower abdominal port or alternatively through the operating channel of an operating laparoscope. The forceps are passed through the endoloop, and the isthmic portion of the tube is grasped and elevated through the loop. The loop is secured around the knuckle of the tube and the suture tail cut with scissors and removed. A second loop may be placed to double ligate the knuckle as described in the initial report of the Pomeroy procedure.30 Alternatively, sutures may be placed and secured using extracorporal knot-tying techniques. The ligated segment is excised with scissors and submitted for pathologic examination. This method of sterilization is more complicated than other methods of laparoscopic sterilization and requires more operative laparoscopic skill. However, because this technique uses many of the basic skills required for more complex operative laparoscopy, it has been advocated as a training step in preparation for these more complicated procedures.31
APPLICATION OF LOCAL ANESTHESIA
The use of mechanical devices for tubal occlusion is often associated with more postoperative discomfort than with electrocoagulation.32,33 Electrocoagulation destroys the neural innervation, thus rendering the tube anesthetic. Conversely, mechanical occlusion of the tube may be considered occlusion of a small hollow viscus and produces a similar crampy abdominal pain. Postoperative nausea and vomiting also are reported to be increased with these methods. These side effects can be minimized or eliminated, however, if the fallopian tubes are first anesthetized with a local anesthetic.32,33,34
Because of its high protein binding and long duration of action, 0.5% bupivacaine is an excellent choice as the local anesthetic. For best results, the local anesthetic should be applied to each tube before and not after occlusion. Five milliliters of 0.5% bupivacaine per tube provides prolonged tubal anesthesia. An aspiration cannula can be used to flow the bupivacaine over all surfaces of the tube. Topical application of bupivacaine has been shown to be equal to tubal injection and is technically much simpler.
CONCLUSION
The laparoscopic techniques and methods presented in this chapter should enable the practitioner to choose an appropriate technique for female laparoscopic tubal sterilization and to use these techniques in a manner that minimizes morbidity and maximizes success.
REFERENCES
Bosch PF: Laparoskopie. Scheiz Z Krankenhaus-u Anstaltsw 6: 62, 1936 |
|
Powers FH, Barnes AC: Sterilization by means of peritonoscopic tubal fulguration: Preliminary report. Am J Obstet Gynecol 41: 1038, 1941 |
|
Palmer R: Essai de sterilization tubaire celioscopique par electrocoagulation isthique. Bull Fed Gynecol Obstet Lang Fr 14: 298, 1962 |
|
Steptoe PC: Laparoscopy in gynaecology. Edinburg, E&S Livingston, 1967 |
|
Phillips J, Hulka B, Hulka J et al: Laparoscopic procedures: The American Association of Gynecologic Laparoscopists' Membership Survey for 1975. J Reprod Med 18: 227, 1977 |
|
Levy BS, Soderstrom RM, Dail DH: Bowel injuries during laparoscopy. Gross anatomy and histology. J Reprod Med 30: 168, 1985 |
|
Ryder RM, Hulka JF: Bladder and bowel injury after electrodesiccation with Kleppinger bipolar forceps. A clinicopathologic study. J Reprod Med 38: 595, 1993 |
|
Soderstrom RM: Sterilization failures and their causes. Am J Obstet Gynecol 152: 395, 1985 |
|
Kleppinger RK: Laparoscopic tubal sterilization. In Garcia CR, Mikuta JJ (eds): Current Therapy in Surgical Gynecology, pp 80–86. Philadelphia, BC Decker, 1987 |
|
Peterson HB, Xia Z, Wilcox LS et al: Pregnancy after tubal sterilization with bipolar electrocoagulation. U.S. Collaborative Review of Sterilization Working Group. Obstet Gynecol 94: 163, 1999 |
|
Cheng MC, Wong YM, Rochat RW et al: Sterilization failures in Singapore: An examination of ligation techniques and failure rates. Stud Fam Plann 8: 109, 1977 |
|
Sampson JA: Postsalpingectomy endometriosis (endosalpingiosis). Am J Obstet Gynecol 20: 443, 1930 |
|
McCausland A: Endosalpingosis (“endosalpingoblastosis”) following laparoscopic tubal coagulation as an etiologic factor of ectopic pregnancy. Am J Obstet Gynecol 143: 12, 1982 |
|
Makar AP, Vanderheyden JS, Schatteman EA et al: Female sterilization failure after bipolar electrocoagulation: A 6 year retrospective study. Eur J Obstet Gynecol Reprod Biol 37: 237, 1990 |
|
Metz KG, Mastroianni L, Jr: Tubal pregnancy subsequent to transperitoneal migration of spermatozoa. Obstet Gynecol Surv 34: 554, 1979 |
|
Cunanan RG Jr, Courey NG, Lippes J: Complications of laparoscopic tubal sterilization. Obstet Gynecol 55: 501, 1980 |
|
Shah A, Courey NG, Cunanan RG, Jr: Pregnancy following laparoscopic tubal electrocoagulation and division. Am J Obstet Gynecol 129: 459, 1977 |
|
Soderstrom RM, Levy BS, Engel T: Reducing bipolar sterilization failures. Obstet Gynecol 74: 60, 1989 |
|
Tucker RD, Benda JA, Mardan A et al: The interaction of electrosurgical bipolar forceps and generators on an animal model of fallopian tube sterilization. Am J Obstet Gynecol 165: 443, 1991 |
|
Soderstrom RM, Levy BS: Bipolar systems—do they perform? Obstet Gynecol 69: 425, 1987 |
|
Tucker RD, Benda JA, Sievert CE et al: The effect of bipolar electrosurgical coagulation waveform on a rat uterine model of fallopian tube sterilization. J Gynecol Surg 8: 235, 1992 |
|
Yoon IB, Wheeless CR, Jr, King TM: A preliminary report on a new laparoscopic sterilization approach: the silicone rubber band technique. Am J Obstet Gynecol 120: 132, 1974 |
|
Yoon IB, King TM: A preliminary and intermediate report on a new laparoscopic tubal ring procedure. J Reprod Med 15: 54, 1975 |
|
Hulka JF, Noble AD, Letchworth AT et al: Reversibility of clip sterilizations. Lancet 2: 927, 1982 |
|
Hulka JF, Fishburne JI, Mercer JP et al: Laparoscopic sterilization with a spring clip: A report of the first fifty cases. Am J Obstet Gynecol 116: 715, 1973 |
|
Filshie GM, Casey D, Pogmore JR et al: The titanium/silicone rubber clip for female sterilization. Br J Obstet Gynaecol 88: 655, 1981 |
|
Semm K: Course of endoscopic abdominal surgery. In Freidrich ER (ed): Operative Manual for Endoscopic Abdominal Surgery. Chicago, Year Book Publishers, 1987 |
|
Soderstrom RM, Smith MR: Tubal sterilization. A new laparoscopic method. Obstet Gynecol 38: 152, 1971 |
|
Murray JE, Hibbert ML, Heth SR et al: A technique for laparoscopic Pomeroy tubal ligation with endoloop sutures. Obstet Gynecol 80: 1053, 1992 |
|
Bishop E, Nelms WF: A simpler method of tubal sterilization. NY State J Med 30: 214, 1903 |
|
Parsons MT, Hill DA: The benefits of using the loop ligature (Endoloop) laparoscopic sterilization procedure in a residency program. J Gynecol Surg 10: 15, 1994 |
|
Koetsawang S, Srisupandit S, Apimas SJ et al: A comparative study of topical anesthesia for laparoscopic sterilization with the use of the tubal ring. Am J Obstet Gynecol 150: 931, 1984 |
|
Borgatta L, Guss L, Barad D et al: Randomized trial of local anesthetic application for the relief of postoperative pain after tubal sterilization with Falope rings. Am J Gynecol Health 5: 11, 1991 |
|
Lipscomb GH, Stovall TG, Ramanathan JA et al: Comparison of silastic rings and electrocoagulation for laparoscopic tubal ligation under local anesthesia. Obstet Gynecol 80: 645, 1992 |