Nutrition Therapy in the Management of Gynecologic Malignancies
Authors
INTRODUCTION
Over the past 50 years, the physiologic stress caused by cancer and the profound metabolic derangements that often result from it have become better understood. It is now accepted that malignant tumors exert their deleterious effects not only by impairing the function of organs or systems, but also by interfering with fundamental mechanisms required to maintain homeostasis.1, 2 Increases in energy and protein requirements related to metabolic demands of a growing cancer can result in loss of healthy body mass. The tumor itself may utilize nutritional substrates preferentially, so that nutritional stores usually adequate to provide energy and protein for normal metabolism can be shunted to the demands of a growing malignancy.3 Compounding the problem, cancer is often associated with anorexia, which can lead to cancer-related malnutrition (cachexia). The resulting deficiency in essential nutrients results in decreased metabolic reserve and impairs the ability to heal wounds, resist infection, and regenerate cells that may be injured by cancer and its treatment.4
The decision to provide nutritional supplementation in a patient with a gynecologic malignancy must be made with a good understanding of the goals of treatment. Judgment based on clinical factors requires an understanding of the natural history of the patient's disease, her prognosis, and her comorbidities. Few would challenge the need to provide all kinds of support, including parenteral nutrition, to a patient with a self-limited condition such as a small bowel fistula resulting from radiation therapy, surgery, or infection. For patients with anorexia and weight loss who have not had potentially curative radical surgery, nutritional augmentation given preoperatively may be of benefit. A more difficult situation is presented by the patient who has a carcinomatous ileus after failure of primary treatment for ovarian carcinoma, or by a patient with radiation enteritis after the diagnosis of lung or bone metastases. Long-term nutritional therapy causes physiologic as well as psychologic stress, and may in fact impair quality of life. Although it may seem intuitive that nutrition should be given to the malnourished, an understanding of the underlying disease process and a careful assessment of potential benefit is required before exposing patients to the discomfort, expense, and risks of nutritional supplementation.
Gynecologic oncologists are uniquely qualified to manage nutritional supplementation in cancer patients. They are well versed in perioperative management of medically compromised patients undergoing radical procedures, and they are trained in medical and surgical management of intestinal tract complications due to disease or therapy. In addition to having an understanding of the metabolic aspects of gynecologic malignancy, these specialists also are trained in radiation and chemotherapy. Because gynecologic oncologists give chemotherapy, they have mechanisms in place for continuous outpatient monitoring for hematologic and metabolic toxicity required for patients receiving peripheral and central alimentation. As trained surgeons, many gynecologic oncologists insert and manage semipermanent implantable central venous catheters (CVCs).
Although an oncologist should be integrally involved in management of malnutrition, nutritional supplementation requires the cooperation of specialists from several disciplines. Dietitians can help determine energy, protein, and nutrient requirements and deficits, and can make useful recommendations for a nutritional prescription. Nutrition pharmacists are trained to develop customized formulations for patients with multiple and complex problems. Many hospitals have developed nutrition care teams to work with clinicians to provide specialized evaluation, prescription of nutritional formulas, maintenance of enteral and intravenous access, metabolic monitoring, and management of complications due to nutritional supplementation. As home care has become an important component of patient management, visiting nurses and other professionals help manage nutrition in conjunction with a patient's family or care giver. Because nutritional support is a rapidly evolving technology, cooperation among specialists can result in a benefit to the patient that is greater than the sum of its parts.
Two factors have arisen in the last decade that limit the use of nutritional therapy in the population of women with gynecologic malignancies. The more significant has been the drive to reduce medical costs by attaching more significance to “evidence-based” clinical care. The accrual of evidence of benefit of nutritional therapy in most situations has been slow and unconvincing. Older evidence described in this chapter leads to the conclusion that supplemental nutrition benefits only a minority of malnourished gynecologic cancer patients. The second most important influence on the utilization of nutritional therapy is the improvement in palliative alternatives such as hospice care and treatment of terminal bowel obstruction by nonsurgical means. Coupled with this improvement in the practice of palliative care has been a new acceptance of the concept of futility in terminal care. More patients, families, and clinicians accept that the best way to maintain quality of life in the final months may be to limit high-tech interventions such as parenteral nutrition.
INDICATIONS FOR NUTRITIONAL SUPPORT IN THE GYNECOLOGIC CANCER PATIENT
Many patients with gynecologic cancer have nutritional problems that would make supplementation advisable even without the diagnosis of malignancy. The generally accepted indications for parenteral nutritional support are summarized in Table 1.5 It is important to distinguish indications that have been validated in controlled clinical trials from those that have not. The most common setting in gynecologic oncology in which patients may benefit from nutritional support is as a preoperative measure before radical and ultraradical surgery in patients with inadequate protein stores. Malnutrition before major surgery presents significant additional risks.6 In theory, preoperative protein deficit results in slower healing, slower return of bowel function, and a greater number of infectious postoperative complications. Perioperative nutritional supplementation is therefore frequently instituted empirically.7
Table 1. Indications for nutritional support
Primary Therapy, Efficacy Shown (by Controlled, Prospective Trials)
Gastrointestinal cutaneous fistula
Renal failure
Short-bowel syndrome
Acute burns
Hepatic failure
Primary Therapy, Efficacy Not Shown
Crohn's disease
Anorexia nervosa
Supportive Therapy, Efficacy Shown
Acute radiation enteritis
Acute chemotherapy toxicity
Prolonged ileus
Weight loss preliminary to major operation
Supportive Therapy, Efficacy Not Shown
Prior to cardiac surgery
Prolonged respiratory support
Large wound losses
Carcinomatous ileus
Metastatic cancer
(Adapted from Fischer JE: Metabolism in surgical patients: Protein, carbohydrate, and fat utilization by oral and parenteral routes. In Sabiston DC (ed): Textbook of Surgery, p 103. Philadelphia, WB Saunders, 1991)
Other patients who benefit from nutritional support are those with self-limited conditions involving impaired oral intake or enteral absorption. Patients with chemotherapy-induced stomatitis or candidal esophagitis impairing the ability to swallow, for example, may be well-served by a course of enteral or parenteral nutrition. Inadequate nutrition related to acute radiation enteritis may be treated by a course of bowel rest with parenteral nutrition. Anorexia or refractory nausea can be a troublesome side effect of many kinds of cancer therapy, and nutritional support may be useful for patients with these conditions.
Other indications for nutritional support for cancer patients may arise out of intra-abdominal metastasis from metastatic gynecologic malignancy. As tumors spread within the peritoneal cavity to external surfaces of the intestinal tract (especially the small bowel mesentery), a carcinomatous ileus may result. This condition, characterized by disordered peristalsis with lack of antegrade transport of chyme, can be caused by direct infiltration of the intestinal wall or by derangement of myenteric nerve conduction. Changes in motility and absorption can disrupt the balance of fluids, exocrine hormones, and nutrients. Intra-abdominal tumor masses may also result in frank intestinal obstruction with severe water, electrolyte, and acid-base disturbances.8 Cancer-related small bowel obstruction or ileus may render the intestine unable to absorb sufficient protein and calories. In this case, parenteral supplementation may be beneficial if coordinated with surgery or other therapy directed at the primary disease process.9 If there is no plan for instituting effective therapy, it may be judicious not to institute nutritional support. It must be emphasized that patients who have ileus or obstruction due to metastatic cancer usually have a terminal prognosis, and nutritional supplementation should not be offered simply as a supportive measure. This is an expensive and unproved modality, and may actually diminish quality of life for a patient with a short life expectancy.10
Cancer patients may present late in the course of their disease with malnutrition related to a variety of coexisting factors. Advancing cancer taxes the body's capacity to grow and regenerate protein and may result in a hypermetabolic state. Liver metastases can seriously impair the metabolism and transport of amino acids, proteins, and other vital nutrients, and may cause derangements in coagulation factors, serum albumin, and liver enzymes. There are both well-characterized and obscure physiologic and psychological factors that may cause nausea and anorexia leading to deficits in dietary protein and energy. Patients with inadequate fat in their diets are deficient in vitamins and minerals, and may have depressed prostaglandin and steroid hormone biosynthesis due to lack of essential precursor fatty acids. Bone metastases and paraneoplastic factors that cause osteoclast activation may cause abdominal cramping and constipation related to hypercalcemia. Frequently used medications such as opioids may also contribute to nausea and constipation which can lead to decreased appetite. The utility of parenteral or enteral feeding in these patients has never been studied, and the recommendation to use nutritional support in a hypermetabolic end-stage cancer patient for whom there is no know effective therapy should await validation in carefully designed and executed clinical trials. There may be no benefit to nutritional support for end-stage cancer patients.11
There have been several studies of parenteral nutrition for patients undergoing chemotherapy for various nongynecologic malignancies.11, 12 Most of these studies have shown no benefit when delivery of chemotherapy, resumption of oral/enteral intake, and disease status have been examined as endpoints. Patients receiving parenteral nutrition as an adjunct to cancer therapy had a high rate of complications related to venous access devices, hyperglycemia, and fluid.13 The conclusion of these studies, summarized in a position statement by the American College of Physicians, was that unless technological advances make the theoretic therapeutic index more favorable, patients should not be exposed to the risk of nutritional supplementation in this setting.13
As a general rule, nutritional support for patients with chemotherapy-induced malnutrition must be considered in the context of the utility of the chemotherapy against the specific disease. A young patient receiving potentially life-saving chemotherapy for a germ cell tumor or high-risk trophoblastic disease should have every supportive modality employed to ensure adequate dose-intensity and timing. The same cannot be said for an elderly patient with refractory epithelial ovarian cancer who is on third-line chemotherapeutic agents. For patients on second- or third-line agents who have nutritional compromise due to anorexia or refractory nausea, nutritional support for the purpose of dosing chemotherapy may not make sense. Perhaps it would be more appropriate to propose a palliative program with the goal of controlling symptoms to maximize quality of life.
ASSESSMENT OF THE GYNECOLOGIC CANCER PATIENT FOR NUTRITIONAL SUPPORT
Although malnutrition has never been carefully studied in patients with gynecologic malignancy, it is probably a significant cause of comorbidity, with a high prevalence in this population. In one estimate of the prevalence of nutritional deficits in patients with breast and other solid tumors, Bruera and MacDonald14 reported that up to 80% of patients with advanced solid tumors met objective criteria for malnutrition. It can therefore be assumed that significant nutritional deficiency is present in the large majority of patients with similarly advanced gynecologic malignancy.15 Determining which of these patients will benefit from nutritional intervention requires the clinical judgment and experience of the oncologist managing the patient's cancer. This must be matched by the skill of the nutrition-care team to define the indications and specific goals for support. In summary, formal nutritional assessment of the cancer patient is performed only if the oncologist, after consideration of these factors, believes that it would be of benefit.
A preliminary step should be a determination of the patient's desire to be supported in this way. Many patients do not want “tube feedings” or parenteral nutrition, especially if they associate nutritional support with futility and loss of autonomy at the end of life. Many times these patients simply need a discussion of short-term and long-term goals of nutritional support. If a long-term program is contemplated, the possibility of home therapy should be explored. An investigation of the patient's insurance benefits is required before recommending this extremely expensive modality. If nutritional therapy is prescribed before this step is taken, many families without coverage will empty savings accounts or sell possessions in order to comply with their doctor's recommendations. Occasionally, home-care companies donate services to patients without coverage, but this practice may become less common as insurance reimbursements decrease.
In general, if the malnutrition is based on low oral intake due to a temporary condition such as recent uncomplicated intestinal surgery, simple observation for recovery may be the most reasonable approach. Most patients will be able to meet their nutritional needs orally within a few days of resumption of their diet, and can be supplemented with commercially available formulas if necessary. Aggressive nutritional support is probably indicated in patients with marginal status before surgery, complicated or radical procedures, major small bowel resections, or no sign of bowel recovery after 5–7 days without protein intake. Healing in these patients will be compromised by inadequate substrate for formation of structural protein and enzymes required for body processes.
Evaluation of the malnourished gynecologic cancer patient begins with a careful history and physical examination to look for signs of metastatic disease or other conditions that would make nutritional support unnecessary. A general oncologic history may elicit reasons for malnutrition, including multiple surgical procedures, courses of emetogenic chemotherapy, and limitations due to cancer or therapy. It is important to have some idea about baseline weight and nutritional status. A patient who has been not been able to maintain body weight without supplementation may benefit from earlier institution of nutritional therapy than a patient who has never had such a difficulty. The time course of nutritional compromise is important. If a patient has been malnourished for several weeks, it is much more difficult to reestablish protein anabolism. These patients may require more aggressive nutritional supplementation than those with short-term nutritional compromise.
In the initial history, a correctable cause of decreased intake may be found. In patients with anorexia caused by nausea, pain, or psychological depression, it may be worth treating these conditions with medical therapy before instituting nutritional supplementation. Depending on the patient's ability to recall personal information, it may be useful to ask about premorbid weight and recent dietary changes. A malnourished patient who may be able to modify components of the diet may be able to avoid artificial nutritional supplementation. History and physical examination may also identify factors that would help determine whether the gastrointestinal tract should be used for nutritional support. Patients with a history of radiation therapy to a large fraction of the small intestine, or those with multiple bowel resections, fistulas, refractory diarrhea or emesis, or bowel obstruction are obviously unsuited to enteral feeding. These patients must be treated with parenteral nutritional support. Conversely, patients with poorly controlled diabetes may be difficult to manage with high-calorie infusions. In addition, patients with frequent episodes of fluid imbalance related to congestive heart failure, cirrhosis, or renal disease may not be well suited to intravenous nutrition.
The decision to provide nutritional support preoperatively begins with an assessment of recent weight loss. A baseline weight can frequently be found in the medical records. The recorded weight from the patient's first office visit may be able to provide this information. If this information is unavailable, anesthesia records from prior surgery usually include body weight. If the patient has documented loss of weight of 6% below baseline, the need for nutritional therapy should be assessed. These patients probably have sufficient nutritional reserves to withstand all but the severe stresses of ultraradical surgery. For patients with a documented weight loss of 6–12% below baseline, other factors from the evaluation may be used to determine the need for nutritional supplementation. If a major operation is planned, however, these patients may benefit from intervention. If weight loss exceeds 10–12% below baseline, there is a high likelihood of malnutrition-related complications, and preoperative nutritional support is probably indicated.11, 16
Nutrient deficiencies and syndromes of malnutrition
It is important to direct the history and physical examination toward documentation of dietary intake and determination of nutrient deficiencies. Patients who have had long periods of decreased oral intake or who have underlying eating disorders (e.g., anorexia, bulimia) may have multiple vitamin deficiencies, but other patients are also at risk. Patients with food intolerance (e.g., to lactose-containing dairy products) may need to have their dietary supplements adjusted accordingly. Many patients who have diarrhea precipitated by fatty foods may have a malabsorption syndrome that predisposes them to lipid-soluble vitamin and essential fatty acid deficiencies. The clinician must not assume that the North American diet is sufficiently balanced to provide adequate nutrition for all. Patients who have been on weight-loss programs or special diets may also have specific deficiencies. It is important to consult a dietitian when considering nutritional intervention at the time of assessment, as certain important issues may not be evident to the oncologist.
Changes in bowel function, such as diarrhea, constipation, melena, or emesis, obviously relate to the utility of enteral feeding, and should be elicited in a directed history and physical examination. Patients with radiation enteritis may have food intolerance due to the lack of absorptive surfaces in the injured bowel. They may have dysmotility or partial obstruction, especially in the terminal ileum, which is more susceptible to radiation injury. Internal bypass procedures can change the characteristics of the intestinal flora by isolating loops of intestine from the fecal stream. This so-called blind loop syndrome may cause malabsorption of fat-soluble vitamins, essential fatty acids, bile salts, and other important nutrients. These patients may benefit from changing the commensal bacterial environment within the intestine by selective use of antibiotics, or they may require surgery. In any case, parenteral supplementation may be beneficial. Many gynecologic cancer patients have a portion of their small or large bowel resected as part of their initial surgical debulking. These patients may have rapid intestinal transit coupled with loss of specialized absorptive surfaces in the ileum, precipitating short-bowel syndrome. Although nutrition can be successfully given enterally with less than 40 cm of remaining small bowel if the duodenum and distal ileum are preserved, most patients left with less than 100 cm of small intestine require nutritional support.17
In addition to the patient's cancer diagnosis, other conditions may have an influence on planning for nutritional support. Patients with renal, hepatic, or pulmonary disease may require adjustments in components of the nutritional formulas. In patients with inadequate cardiac reserve to handle large volumes of fluid, concentrated formulations may be necessary. Patients with diabetes, hypercholesterolemia, or divalent cation-wasting syndromes related to cisplatin chemotherapy must be carefully monitored during nutritional supplementation.
An assessment of protein stores can be made on physical examination to identify characteristics of the nutritional deficiency known as kwashiorkor. Patients with ankle or periorbital edema, ascites, or tight skin turgor may have insufficient capillary oncotic pressure due to protein deficit. It is important to assess renal function because protein wasting due to albuminuria is also a cardinal feature of nephrotic syndrome. Another kind of malnutrition is the deficiency in energy stores, which is a general wasting syndrome characterized by loss of extremity muscle mass, temporal atrophy, and a scaphoid abdomen with prominent skeletal contours. This more chronic deficiency is related to pan-starvation and is frequently called marasmus. Neurologic, musculoskeletal, and skin examinations may demonstrate important signs of energy, protein, vitamin, and mineral deficiencies. Cutaneous sores, especially stomatitis and xerostomia, are often the result of malnutrition caused by vitamin B deficiencies.
Objective measures of malnutrition
Although it may be obvious from a history and physical examination that a patient is malnourished, it frequently is not. Even if it is clinically apparent, objective measures of malnutrition are helpful in determining the indication for nutritional support and for monitoring its effectiveness. In addition to the physical examination findings noted above, other objective measurements of malnutrition should be made. For preoperative patients, these are summarized in Table 2. Research nutritionists use sophisticated circulating markers of nutritional status, and specialty laboratories can provide the results of these blood tests. Other measures of nutritional status, such as calorimetry, may aid in the management of the malnourished patient. Nitrogen balance is performed by measuring urinary nitrogen excretion and adding a factor for respiratory and fecal loss. These measurements are more useful for determining how much nutritional support is required than for indicating whether or not to administer nutritional support at all.
Table 2. Objective criteria for perioperative nutritional support
Mild to Moderate Malnutrition
(May proceed with operation, but consider postoperative nutrition)
- Recent weight loss of 6–12% of usual body weight
- Serum albumin >3.5 g/dL
- Transferrin >200 mg/dL
- Leukocyte count >1500/mm3
Severe Malnutrition
(Preoperative and postoperative intervention may be necessary)
- Recent weight loss >12% of usual body weight
- Serum albumin <3.5 g/dL
- Transferrin <200 mg/dL
- Leukocyte count <1500/mm3
In practice, only a few blood tests are clinically useful. These include serum albumin and transferrin concentrations and a standard complete blood count. Circulating serum transport proteins reflect the synthetic capacity of the liver, and can be used as markers of nutritional deficit. Other proteins, such as thyroxine-binding prealbumin and retinol-binding protein have half-lives of 2 days and 12 hours, respectively, but are not measured at most clinical laboratories within a time frame useful for management of nutrition. The half-lives of these special proteins may be used as approximate indicators of the duration of a patient's nutritional compromise and can be helpful for monitoring recovery of protein synthetic function. Serum albumin is the most frequently used assay for determining whether a patient is in a state of nutritional deficiency. The half-life of albumin is approximately 19 days,14 and deficits reflect the duration of the inability of the liver to produce this important protein. Because of the relatively long half-life of albumin, its concentration is not often used as a marker of recovery. A normal albumin level is usually considered to be greater than 3.5 g/dL, and patients with an albumin level less than 3 g/dL are severely malnourished. Immune reactivity tests, such as the intracutaneous injection of tuberculin or mumps antigen, are also sometimes used as an index of malnutrition. In a cancer patient, however, anemia, leukopenia, and cutaneous anergy are often due to other cancer-related factors that can cause bone marrow suppression or impair cell-mediated immunity. More often, a history and physical examination combined with readily available blood tests can help determine which patients will benefit from nutritional support.
In the cancer patient, nutritional requirements can change dramatically. While estimates from population-based studies may be adequate for determining the need for protein and energy requirements in patients with diseases other than cancer, they may be grossly inaccurate in a woman with gynecologic malignancy. It is important to determine a precise number of kilocalories and the number of grams of nitrogen used in the maintenance of lean body mass. The stresses related to disease and therapy may accelerate protein wasting and may result in essential nutrient and vitamin deficiencies. These components should be replaced in the proper proportions to avoid excess carbohydrate and nitrogen intake. Many patients with gynecologic malignancy may be able to take some food by mouth, and in this case, a count of calories and grams of protein should be undertaken to determine how much of the requirement for these nutrients would be met without intervention. An assessment of nutritional deficits allows tailoring supplementation to the individual patient according to her needs.
DETERMINING NUTRITIONAL REQUIREMENTS
Energy requirements
Although population-based nutritional estimates are sometimes grossly inadequate, they do allow a reasonable starting point for determining a patient's needs. It is known from many studies, for example, that 1 g of protein and 3–4 kcal are required to maintain 1 kg of lean body mass. These maintenance figures are calculated with the addition of factors related to specific stresses or deficits resulting from suboptimal oral intake. The Harris-Benedict Equation is a well-known population-based formula for estimating daily energy requirements for men and women. The utility of this cumbersome gross estimate is hampered by the fact that it derives the number of calories required to maintain homeostasis on the basis of a healthy person at bed rest, and it must therefore be adapted to patients with underlying diseases or energy requirements for protein turnover. Multiplicative factors must be used to determine specific energy requirements associated with mild, moderate, and severe activity within the normal range, besides the major stress associated with malignancy combined with recovery from surgery. The Harris-Benedict Equation is given on the Magee-Womens Hospital order sheets (Fig. 1 and Fig. 2). In meeting energy requirements, carbohydrates such as glucose (dextrose) and lipids, which store energy more efficiently, are the best substrates. Dextrose provides 3.4 kcal for every 1 g metabolized. Proteolysis can also supply energy, and after carbohydrate and lipid stores are depleted, amino acid metabolites are shunted to biochemical pathways to fulfill unmet calorie requirements.
Protein requirements
Protein requirements are even more difficult to predict. Nitrogen balance can be estimated by collecting a 24-hour urine specimen and measuring urine urea nitrogen excretion. Because nitrogen is also excreted in feces, across the skin, and in exhalation, a factor must also be added to account for these losses. The relatively constant proportion of molecular nitrogen in essential amino acids is exploited in the determination of protein requirements. For every 1 mol of excreted nitrogen, 6.25 mol of protein is required to maintain balance. It follows that for every 1 g of nitrogen excreted, 6 g protein is added to the nutritional formula. One important goal of nutritional therapy is to provide enough carbohydrate and lipid substrate to preserve lean body mass. Protein is given in nutritional therapy to provide essential and nonessential amino acids for anabolism of structural and metabolic proteins. In the process, protein provides approximately 4.1 kcal/g substrate.
Lipid requirements
Dietary lipids, in addition to being an efficient means of energy storage, are also a source of essential nutrients. Linoleic and linolenic acids, which cannot be synthesized, are major precursors of necessary steroids and arachidonic acid. Although steroid biosynthesis can proceed without these fatty acids, prostaglandin synthesis requires arachidonic acid. This precursor is essential to chemical reactions required to maintain skin, nerve, hair, and mucosal cells. Lipids are also the most concentrated source of energy per gram: 1 mL of a 20% lipid solution provides approximately 2 kcal, which is approximately 9 kcal/g enteral lipid substrate. Glycerol as an emulsifying agent adds another 1 cal/g in intravenous lipid solutions. Complications associated with delivering large amounts of energy as dextrose can often be avoided by using lipid infusions as a source of calories.
Vitamin and trace metal requirements
Vitamins and trace metals act as cofactors for these essential chemical reactions. The quantities of vitamins and trace metals required for daily metabolism in a healthy person are given on the order sheets (see Fig. 1 and Fig. 2). These minimum daily requirements are easily met by patients with an intact gastrointestinal tract and a reasonably balanced diet. Several situations encountered in gynecologic oncology, however, make enteral absorption of vitamins problematic. Most commonly, metabolism of vitamin B12 is impaired in patients who have had either surgical ileal resection or bypass, or functional malabsorption related to radiation enteritis or blind loop syndrome. Intrinsic factor, which is produced by the parietal cells of the stomach, allows absorption of dietary vitamin B12 from the distal ileum. Failure to absorb this nutrient can result in permanent neurologic deficits and macrocytic anemia. For patients with malnutrition not based on the short-bowel or blind loop syndromes, enteral formulations contain adequate amounts of these nutrients. For practical purposes, one need only add vitamins and trace metals to dietary supplements in the appropriate concentrations. A more difficult situation is encountered in the patient who has a malabsorption syndrome coupled with deficiencies of all fat-soluble vitamins. These patients usually require intravenous or intramuscular administration of vitamins and trace metals.18
Summary
Nutritional support should be given to supply sufficient energy (usually in the form of carbohydrates), an amino acid substrate for the formation of protein, essential lipids, vitamins, and trace metals. In addition, fluid and electrolytes must be given in the proper proportion to maintain cellular metabolism, provide osmotic balance, and counteract urinary and insensible losses. Practical considerations in the administration of nutritional therapy are addressed in the next section.
INSTITUTING NUTRITIONAL THERAPY
Nutritional supplementation can be divided into two broad categories based on the route of administration: enteral and parenteral. In general, enteral feeding is considered more desirable because it is more physiologic, safer, and less costly. Most gynecologic oncology patients who require support, however, receive parenteral nutrition. Parenteral feeding is preferred in this group because (1) their nutritional depletion is based on primary gastrointestinal dysfunction due to metastatic tumor, radiation, or surgery; (2) semipermanent access to the stomach and small intestine for tube feedings may be difficult because of peritoneal disease or ascites; and (3) parenteral nutrition may deliver more calories and protein per day than enteral feeding in some patients.
Parenteral nutritional support is further divided into two categories: peripheral parenteral nutrition (PPN) and total parenteral nutrition (TPN; also known as central venous hyperalimentation).
Historically, high-concentration PPN has been associated with an unacceptable rate of complications related to peripheral venous thrombophlebitis (PVT). For that reason, PPN is considered a stopgap measure in which some nutrients are infused to allow time to decide whether longer term therapy might be indicated. The distinction between these types of parenteral nutrition is becoming less important as techniques of minimizing PVT have allowed higher osmolarity solutions to be administered through noncentral venous catheters.19 In addition, peripherally implanted semipermanent long-line and percutaneous brachiocephalic CVCs currently under study may eliminate some of the mechanical complications related to CVCs.
Enteral feeding
The most physiologic way to meet the nutritional needs of a malnourished patient is to exploit the intestinal tract as a vehicle for nutrients. It is therefore accepted that if a patient has a viable intestinal tract, it should be used before resorting to the “artificial intestine” approach of parenteral nutrition. Depending on the indication for support, physiologically intact portions of the gastrointestinal tract can usually be counted on to absorb nutrients and to process wastes. Besides this advantage, enteral feeding is safer and less expensive than intravenous feeding, although serious complications can occur regardless of the route of administration.
GASTRIC FEEDING
Patients with a problem localized to any segment of the alimentary tract proximal to the gastroesophageal junction may be able to achieve full nutritional support by artificial bypass of the diseased segment. Patients with dysfunction of the mouth and esophagus due to head or neck tumor, or those who have stomatitis or esophagitis related to therapy or infection, may be well served by simply instilling pureed regular food or commercial nutritional supplements directly into the stomach. This can be accomplished in many patients with a temporary 16-gauge flexible polyethylene nasogastric tube. The traditional rigid nasogastric sump used for decompression is not suitable for feeding because it is uncomfortable and can predispose patients to aspiration. The use of newer nasogastric feeding tubes made of flexible materials prevents rhinitis, pharyngitis, and pulmonary complications related to impaired coughing due to rigid tubes. In selected ambulatory patients, the technique of placing a nasogastric tube can be taught to care givers. The obvious benefit is that the patient is allowed to leave a skilled-care facility earlier and to have a normal appearance and level of activity when not feeding. Patients can also be taught self-intubation by swallowing a flexible tube inserted with its tip in the oropharynx or nasopharynx. These innovations have made long-term nasogastric feeding an acceptable alternative to percutaneous abdominal access routes.
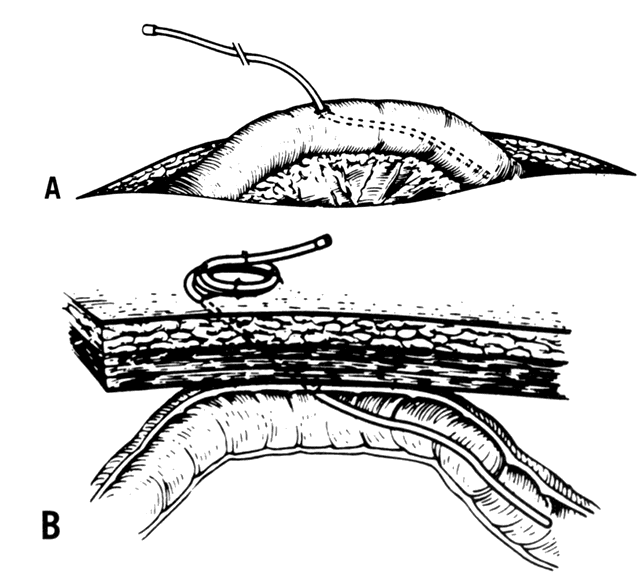
In many circumstances, however, the placement of a gastrostomy catheter for tube feeding may be necessary or desirable. Gastrostomy tubes must have significant rigidity and caliber to accommodate some constriction and excursion at the abdominal wall insertion site without becoming occluded. It is helpful to be able to irrigate the gastrostomy tube to release mucus and other particulates that may render it nonfunctional. Any semirigid flexible plastic feeding tube can be used for this purpose, including standard urinary Foley catheters. Feeding gastrostomy tubes may be placed at the time of laparotomy or at a separate minilaparotomy by techniques familiar to gynecologic oncologists, or they can be placed percutaneously under gastroscopic or fluoroscopic guidance at any time. Feeding gastrostomy placed at the time of surgery is inserted through a stab wound in the anterior wall of the stomach and stabilized by two concentric silk purse-string sutures. The gastrostomy channel is then brought close to the peritoneum and attached to the anterior abdominal wall without tension at three or four sites around the tube. Catheters placed in this manner can be removed at the bedside or on an outpatient basis without risk of spilling gastric contents into the peritoneum. The hole in the stomach will seal without sequelae in 1 or 2 days.17
The major risk of gastric feeding by either route is aspiration pneumonitis, which can be fatal. For this reason, it is important that gastric feeding be used only in those patients who have an intact sensorium, have normal airway reflexes, or are endotracheally intubated. In any event, observation for aspiration is imperative, and gastric volume should be monitored frequently to lessen the risk. To allow adaptation to gastric feeding, the rate of instillation of nutritional formula and the concentration of the solution should be increased slowly. Initially, normal saline is given through the catheter as a test to assess gastric emptying. Residual volumes should be less than 50% of the infused volume after 1 hour of infusion. If the patient reports symptoms attributable to gastroesophageal reflux, has abdominal cramping, or has diarrhea unrelated to other causes, the rate or concentration should be decreased. Monitoring for metabolic complications should be done as described later in the section on parenteral feeding.
DUODENAL AND JEJUNAL FEEDING
Many advocate direct intubation of the duodenum or jejunum in order to minimize the risk of aspiration. Certainly nasogastric or gastrostomy feeding may be problematic for patients who cannot protect their airway or who have a history of gastroparesis. If a patient has a problem related to upper gastrointestinal obstruction, then a bypass of the obstructed segment may be reasonable. The instillation of nutritional solutions distal to the pylorus or duodenum requires pharmacologically prepared solutions to adapt the chyme to the environment of the small intestine. Formulas must simulate the mechanical and enzymatic actions on the bolus normally provided by the mouth, stomach, and duodenum, including hydrolysis of fats and breakdown of proteins into oligopeptides. In patients whose gastrointestinal tract has not been used for 3–4 weeks, these formulations are usually given as “elemental diets” in that they exist in forms that are easily absorbed and produce little waste, although they are more expensive than standard oral or gastric “nonelemental” supplements. After allowing for recovery of intestinal function, the transition to these polymeric supplements should proceed. Nasoenteral feeding is possible with tubes that can bypass the pylorus, but feeding by transcutaneous jejunostomy tube is more comfortable for the patient and easier to administer.
Tube feeding should be initiated at an iso-osmolar concentration of 20–30 mL/h, based on clinical assessment of motility and tolerance. The rate should be increased by 20–30 mL/h at 12–24-hour intervals until the daily requirements of fluids, electrolytes, and nutrition intended by the enteral therapy are reached. If patients experience high residual volume, reflux symptoms, or abdominal cramping, the rate should remain constant for a day or be increased by only 10–20 mL every 12–24 hours. If patients are monitored clinically and advanced in this fashion, there is little need to use half-strength feeding to improve tolerance.
Permanent and temporary jejunostomy tubes can be placed by several well-described techniques. The Witzel technique is most commonly used during laparotomy.17 To fashion a jejunostomy, a stab incision is made separate from the primary abdominal incision, through which a 14-French red rubber catheter is brought into the abdomen. A small antimesenteric incision is made in a segment of proximal jejunum 15–20 cm from the ligament of Treitz. The catheter is inserted and advanced distally. A purse-string suture is placed to secure the catheter, and a serosal tunnel is constructed by forming a sleeve of antimesenteric jejunum. The serosa is stabilized with silk sutures for a distance of 5–6 cm proximally. The adjacent bowel is brought to the anterior abdominal wall with silk sutures, and to the skin with nylon sutures. This catheter can be removed at the bedside without the risk of fistula formation.
Ballon20 described the use of needle-catheter jejunostomy in gynecologic oncology patients (Fig. 3). In this technique, a submucosally tunneled jejunostomy is created at the time of laparotomy with a 14-gauge needle-catheter system (e.g., Insyte, Becton Dickinson Vascular Access, Sandy, UT) through which a 16-gauge plastic catheter is inserted into the jejunum. According to several investigators,21, 22 enteral feeding can be safely started early in the postoperative period, without the risk of prolonging ileus or precipitating malabsorption syndromes. In Ballon's study, elemental feeding was begun in the recovery room. This technique is a safe and cost-effective means of providing nutritional support in the first few postoperative days, as well as positive nitrogen balance. Parenteral nutrition may also be used during this period, and may be associated with fewer complications in patients who have had intestinal surgery.23
Parenteral feeding
Dudrick and associates24 are credited with showing that nutritional needs could be met by infusing a nutrient formula directly into the venous circulation. In a classic study,6 beagle puppies were given a solution containing glucose, fibrin hydrolysate, vitamins, and minerals into the superior vena cava. Weight gain was superior to matched controls, and development was normal in the experimental group. Over the past 30 years, the techniques first described by Dudrick and his group have been refined so that patients with nutritional needs that cannot be met by oral/enteral feeding are maintained on cycled TPN indefinitely.25 Innovations in permanent venous access have allowed patients to manage their own nutritional therapy at home with a minimum of impact on their quality of life. In gynecologic oncology, patients with nutritional impairment may benefit from intravenous hyperalimentation in conjunction with surgery, or for longer periods of time as necessary for management of short-bowel syndrome and radiation enteritis.
PERIPHERAL PARENTERAL NUTRITION
Payne-James and associates19 reviewed the indications for using peripheral veins for administration of supplementary nutritional formulas, and suggested that this route may be underutilized. Historically, because of the high concentrations of glucose infused, peripheral veins were susceptible to thrombophlebitis. It is now thought that this complication can be minimized by meticulous attention to atraumatic sterile technique of venipuncture and cannula care. Large-bore (16-gauge) flexible catheters are associated with a significantly higher rate of PVT than newer small (23-gauge) elastomer cannulas. The rate of PVT may also be related to cannula length, insertion site, size of the peripheral vein, and duration of infusion. Other factors that may cause an unacceptably high rate of venous complications include the osmolarity and pH of the solution and particulates within the formula.
Prophylaxis against PVT includes using appropriate pH buffers to allow a more physiologic solution. The addition of 1% sodium bicarbonate in one study reduced the incidence of PVT over control solutions by approximately 50%.26 Another way to mix peripheral nutritional formulas so as to minimize the risk of PVT is to use glycerol instead of glucose as an energy source. Glycerol has a lower osmolarity and does not irritate the veins as much as an equivalent calorie-dose of dextrose. Heparin, steroids, and lipids can also protect the peripheral veins by topical action on the endothelium. Nonsteroidal anti-inflammatory drugs have been administered in gels to the skin around the catheter insertion site, and they have also been shown to reduce the risk of PVT. In general, taking extra precautions to reduce inflammation at catheter sites may reduce the rate of venous complications. Payne-James and co-workers19 suggested that an experienced, dedicated nutrition-support team can reduce the incidence of PPN failure and prevent the need for central catheterization in most cases. This can be accomplished by establishing hospital protocols for insertion of fine-bore catheters for infusion of nutritional formulas, stabilizing intravenous lines to flat surfaces of the extremities, and providing meticulous cannula care. To replace the more cumbersome CVCs, these protocols should be as rigorously applied as current protocols for subclavian and jugular lines.
Peripheral nutrient infusion should be an all-in-one mixture, so that changes in the fluid are kept to a minimum. An in-line filter can prevent infusion of particulate matter. Every attempt should be made to prepare the formula so that it will not irritate the vein by using a low-osmolarity solution with a bicarbonate buffer, alternative energy substrates, and topical nonsteroidal medications, if available. Intravenous lipids can actually protect the endothelium and should be used as a source of calories in every PPN formulation. An important component of catheter care in PPN is vigilance for early signs of PVT. The patient should be advised to tell the staff if the cannula should become irritated, so that it can be removed at the first sign of phlebitis. If all of these measures are taken, PPN can be given without complications for several days and can prevent the complications associated with CVCs.19
In summary, PPN should be given when there is a likelihood that nutritional support will be necessary for less than 2 weeks. It can be used as a stopgap measure to provide calories and protein for the patient who is not taking adequate nutrients orally while decisions are made about the appropriateness of other kinds of nutritional support. It can also be used as an adjunct to enteral feeding in the patient with uncertain gastrointestinal function or an inadequate oral diet. If it appears that TPN will be required, a CVC can always be placed. PPN should be the first line of treatment in patients in whom CVC is contraindicated or who have had thrombosis or occlusion of central veins due to catheterization.19
TOTAL PARENTERAL NUTRITION
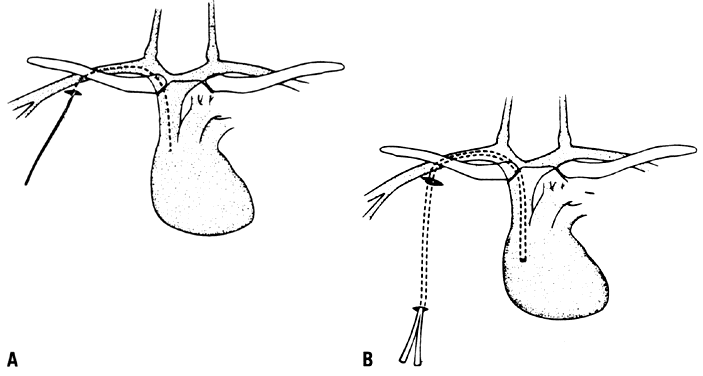
Infusion of hypertonic solutions for longer than 3 or 4 days is best done with a large-bore catheter placed into the lumen of the superior vena cava. The subclavian, internal jugular, or external jugular vein can be catheterized percutaneously by a modified Seldinger technique or by venous cutdown (Fig. 4 and Fig. 5). The use of femoral catheters is associated with an unacceptable rate of infections, and their use should be discouraged.27 There are advocates for each site of approach to the superior vena cava based on ease of insertion, patient comfort, and risk of complications. The insertion of CVCs is safe in experienced hands, and complications should occur in fewer than 1% of procedures. Life-threatening complications of insertion can occur, such as pneumothorax, hemothorax, hemorrhage, catheter and air embolus, and venous thrombosis. A semipermanent tunneled catheter or intravenous port should be used for long-term hyperalimentation. These devices allow delivery of nutritional support outside the hospital, and in many areas of North America, home infusion is possible. Semipermanent implantable flexible catheters have been used for more than 20 years in oncology in an effort to protect peripheral veins and extremities from vesicant injury and extravasation. These CVCs usually do not require skilled nursing care and can be accessed by patients and family members. For the purposes of TPN, the port can remain accessed or it can be removed at intervals between infusions. With attention to sterile technique by the personnel who access these devices, it is not uncommon to be able to maintain a CVC dedicated to hyperalimentation for years.28
Semipermanent CVC insertion is a minor surgical procedure, and as such, it is important to discuss the risks with the patient. The patient should be informed that access devices can become infected or malfunction at any time, and that removing the catheter requires another minor procedure. My current preference is to cannulate the superior vena cava through the right internal jugular vein because of the extremely low risk of pneumothorax and the easy accessibility at this site for management of vascular complications such as arterial laceration.
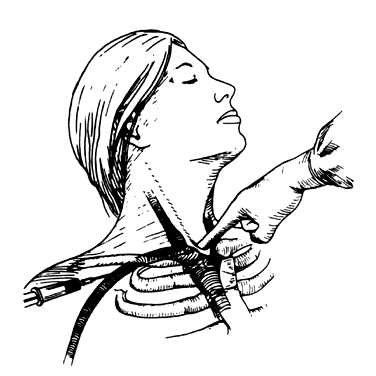
The vein is approached percutaneously just behind the anterior sternocleidomastoid muscle with a 2-cm, 25-gauge finder needle. The needle enters the skin at an angle approximately 90° to the trachea and approximately 2 cm cephalad and parallel to the clavicle. A flexible-tip J-wire is then inserted into the vena cava through an 18-gauge needle. For insertion of permanent or implantable CVCs, fluoroscopy is used or an x-ray is taken with the wire or catheter in the vena cava to ensure that the catheter is positioned above the junction of the right atrium and the superior vena cava. After the position of the guide wire is seen radiographically, a CVC can be inserted over the wire for percutaneous insertion or under direct visualization at cutdown. Implantable percutaneous CVC kits often contain a dilator and peel-away sheath, which are inserted through the subcutaneous tract, and a Groshong-tip silicone antithrombotic catheter is placed to 13–17 cm, based on the distance from the insertion site to the right atrium. Many surgeons prefer the subclavian approach because a tunneled catheter is more comfortable and cosmetic when stabilized to the skin in this area, although the risk of insertion complications is higher (see Fig. 4).
The implanted subcutaneous “port” is placed into a pocket created in the tissue beneath the skin of the infraclavicular fossa or in the apical aspect of the breast. A tunnel is created between this pouch and the needle insertion site at the subclavian or jugular vein (see Fig. 5). The catheter is tunneled from the vein to the pouch and attached firmly to a special nipple on the port. The port has an anterior silicone diaphragm through which special noncoring needles are used to access the vein. The port is stabilized to the superficial fascia of the anterior thorax with permanent sutures, and the skin is closed in layers. Care must be taken to avoid placing the port where a brassiere strap may become a source of discomfort, skin irritation, or infection. A common mistake is to place the port too superficially: with repeated accessing, the skin anterior to the port will erode. After several months, the port can extrude itself through the skin and will need to be removed. To prevent this complication, at least 1 cm of subcutaneous tissue should be placed between the port diaphragm and the needle insertion site in the skin.
Temporary CVCs are usually placed percutaneously at the bedside, and are more likely to be multipurpose, semirigid, triple-lumen catheters. The technique for insertion into the superior vena cava through the subclavian or jugular approach is identical to the procedure described above, although because of their rigidity, temporary lines are much more comfortable if placed through the subclavian vein. The catheters are stabilized to the skin with silk or nylon sutures, and occlusive dressings are applied. In addition to providing good access for instillation of fluids, the lines can be used for monitoring central venous pressure and drawing blood. If these short-term CVCs are used for parenteral nutrition, they should be used for that purpose only, not for other medicines such as chemotherapy or symptomatic drugs.
Late complications
Late complications associated with long-term CVCs are common, occurring in up to 10% of cancer patients who have these devices.28 These problems can be related to mechanical effects (i.e., changes due to deposition of proteinaceous debris such as blood clots) or infection. Port migration or catheter dislodgment and extrusion through the skin are relatively unusual, but can render the access device unusable. More common are mechanical problems, whereby clots or fibrin deposits encase the catheter in a sleeve and impair the ability to draw blood or infuse fluids. Urokinase (5000–10,000 units) administered through an occluded catheter generally degrades fibrin and protein deposits if left in the catheter for more than 1 hour. Catheter-associated thrombus formation is a significant cause of vascular occlusion and a difficult management problem in hypercoagulable cancer patients. These patients may benefit from low-dose chronic warfarin administration (1 mg/day), although intravenous vitamin K is often included in hyperalimentation formulas.28
Infection is probably the most common complication of indwelling venous catheters. Cancer patients may have a special tendency to acquire port or CVC infections because of the immunosuppressive effects of their primary disease process or neutropenia related to chemotherapy. Most of these infections are caused by cutaneous Gram-positive bacteria, and this is thought to be related to breakdown of the natural skin barrier by repeated access. The rates of catheter-related infection vary from 2.7% to 60%,29 and can involve the catheter itself, the line between the external access site and the venous puncture (tunnel infection), or the pocket created for reservoirs or ports. Localized cutaneous infections can become systemic if a port is accessed through an infected pouch. If the port is already accessed, then blood specimens can be drawn and antibiotics should be infused through the port. Local infections should be treated with oral antibiotics that cover cutaneous flora, but infections of deeper structures require intravenous antibiotics. Isolation of resistant organisms (e.g., Staphylococcus aureus) usually requires port removal. It is not uncommon for a cellulitis at a port site to clear with a course of antibiotics delivered intravenously into the port or by mouth, but infections that do not clear after 1 or 2 days should be treated by removing the port and catheter.28
A unique port complication that occurs with the administration of TPN is calcium-phosphorus precipitation. This can be caused by TPN that is more than a few days old, and can be prevented by careful inspection of TPN solutions before infusing them. If incompatible solutions are to be run through the catheter consecutively, 10 mL of a neutral flush should be used to avoid this complication.28 Extravasation of TPN is not usually a serious problem, but can cause symptomatic phlebitis. The infusions should be stopped and a reason for the extravasation should be determined before using the port again. In most cases a dislodged needle delivers a bolus of solution outside of the port or reservoir. This can be prevented by using an appropriate-sized needle and anchoring it carefully after the port is accessed.
DETERMINING THE NUTRITIONAL PRESCRIPTION
A careful account of nutritional requirements is a prerequisite for producing any artificial nutritional formula. This is true whether the support is to be administered by enteral or parenteral route. An important preliminary point is to establish clinical endpoints, which should be used to determine when enteral feeding, PPN, or TPN should be stopped. As has already been emphasized, this therapy should not be administered in the cancer patient without understanding that it carries with it substantial risks as well as benefits. It is a source of frustration to the nutrition-care team and is certainly not in the patient's interest for a complication to arise from a therapy that is no longer indicated, and but for a lack of forethought should have already been stopped. This is especially important to keep in mind when administering TPN for an uncertain period of time in a patient in whom lean body mass is compromised due to progression of disease.
Appropriate clinical endpoints for cessation of artificial nutrition should always include resumption of oral/enteral intake that is adequate for absorption of energy and protein. Patients whose condition has improved to the point where oral nutrition can resume are the most likely to benefit from a short course of support. In a setting where nitrogen excretion can be measured, maintenance of positive nitrogen balance is a good clinical endpoint. If a patient is taking in more nitrogen than she excretes in urine, feces, skin, and exhaled air, one can assume the nitrogen is being “fixed” in new protein. If this patient can maintain nitrogen balance without the nutritional intervention, as determined by clinical and laboratory indices, it should be stopped.
It must be emphasized that a particular patient's nutritional requirements will be the same regardless of the route of absorption. In order to heal, all patients need energy-producing molecules, essential nutrients for anabolism and body processes, water, and electrolytes. Providing these ingredients in the proper quantities and proportions is the goal of a successful nutritional prescription. Some patients have specific problems that make fulfilling their nutritional requirements more challenging. Patients with large burns or wounds, complex enteric fistulas, and renal or hepatic failure require a different protein composition and perhaps vitamins and trace metals added to their formulas. Patients on respirators and those with chronic obstructive pulmonary disease need to have special attention paid to endogenous production of respiratory CO2. This can be adjusted by changing the proportion of energy derived from glucose, which is metabolized to CO2. The oncologist would be well advised to consult with critical-care and nutrition specialists when devising a formulation for patients with new or preexisting major organ-system insufficiency.
Most hospitals use preprinted nutritional prescription forms for inpatient therapy. This practice allows nutrition pharmacists to standardize the preparation of enteral and parenteral solutions. Additives such as heparin and insulin are included on the forms, and the ordering physicians are reminded to include trace metals and vitamins on the appropriate schedule. These forms not only facilitate preparation of the patient's formula, but also provide guidance to clinicians about nutritional requirements. At Magee-Womens Hospital, formulas required for the calculation of nutritional requirements are provided on the back of the prescription form. These forms (see Fig. 1 and Fig. 2) are currently used in the pharmacy and on the gynecologic oncology unit.
Energy requirements
Preparing the nutritional prescription begins with determining a daily energy requirement. The number of calories required to maintain homeostasis is provided in the form of proteins, carbohydrates, and lipids. Patients with cancer who require nutritional support have a wide range of activity levels, and therefore have widely disparate energy substrate requirements. To maintain lean body mass, energy as measured by calories must be provided for anabolism to proceed and for body processes to continue. Patients with weight loss due to inadequate ingestion of calories should have some assessment of their basal metabolic rate. As mentioned previously, there are several means for accomplishing this, depending on the degree of precision required. In patients with pulmonary artery catheters, this information can be derived from oxygen utilization in a formula that uses cardiac output and mixed venous and arterial oxygen saturation. A more common means of estimating nutritional requirements is the Harris-Benedict formula. A patient with a severe injury, however, must have her calorie requirement adjusted by the addition or another 50–100% over the value derived from the Harris-Benedict equation. Determination of standard energy requirements in gynecologic oncology is severely limited by a paucity of data in this population. For a patient with a significant metabolic burden attributable to a gynecologic malignancy, one can only assume an increase in energy requirements and make adjustments accordingly.
A practical approach to energy delivery assumes that there is a given number of kilocalories required to maintain 1 kg of lean body mass in 1 day. This number is adjusted based on a clinical impression of the level of metabolic stress and on consideration of the patient's list of current problems. Patients who require nutritional support, but who have had minor procedures, small surgical wounds, and no significant confounding metabolic stress, are probably well served by 30 kcal/kg/day. This should be considered the average protein requirement for patients with primary malnutrition (i.e., nutritional support is indicated for malnutrition alone). For patients with secondary malnutrition, such as those with ongoing severe metabolic stresses related to surgical wounds, infections, cancer, or burns, approximately 35–40 kcal/kg/day is probably required.
Patients with morbid obesity, defined as more than 100 lb over ideal body weight, should have their energy supplementation based on 25 kcal/kg/day to exploit the endogenous energy derived from adipose reserves. In addition, this level of carbohydrate and lipid infusion helps prevent complications due to insulin resistance seen frequently in obese patients. Calorie counts can be calculated from hospital tray surveys or patients' nutritional diaries to determine whether needs are being met by oral intake. If not, consideration should be given to starting enteral feeding. If there is a reason to supplement parenterally, PPN or TPN should be instituted.
CARBOHYDRATE REQUIREMENTS
In the nutritional prescription, the largest proportion of energy is generally delivered as glucose (dextrose), because it is very inexpensive and easy to mix. These solutions are available in any concentration up to 70% (D70), and can be easily diluted to fulfill any osmolarity or fluid requirement. Because glucose is water soluble, dextrose solutions can also be mixed easily with electrolytes and water, facilitating determination of osmolarity. Because glucose infusions are mixed by weight, it is simple to calculate energy delivered by a certain volume. For example, there are 150 g glucose for every 1 L D15, resulting in a calorie delivery of 450 g of glucose for every daily infusion of 3 L fluid. Because every 1 g glucose provides 3.4 kcal, 1530 cal dextrose is delivered in 3000 mL D15 each day. Dextrose infusions can also be mixed with commercial amino acid formulas, making this source of energy the most convenient way to deliver calories.
There is, however, a physiologic limit to the amount of glucose that can be used as a source of energy by peripheral tissues. Limitations of cellular glucose transport mechanisms and the effects of insulin can cause excess glucose to remain in the circulation until it is excreted. Excess glucose can cause serious toxicities, including osmotic diuresis resulting in dehydration, fatty infiltration of the liver, and hyperglycemic nonketotic coma. Overinfusion of carbohydrate energy substrate should be avoided by careful monitoring of urine for glucose, as well as by serial blood measurements of glucose level. Even with the administration of insulin during nutritional support, the peripheral cell transport mechanisms may be overwhelmed, and excess glucose can become toxic. A daily infusion of approximately 7 mg/kg/min results in fatty infiltration of the liver and excess production of CO2. This latter toxicity is especially important in the respirator-dependent patient receiving nutritional support. Excess CO2 can be more difficult to clear through impaired lungs, and endogenous production can compromise respiratory function. While administering nutritional support, one must be cognizant of potential complications related to carbohydrate infusion. Too much carbohydrate can complicate the healing process, negating the presumed benefit of nutritional supplementation. Carbohydrates are required, however, because the highly metabolic central nervous system cannot derive energy from lipids; rather, it will use 50–150 g dextrose each day, and this vital nutrient cannot be withheld from nutritional support formulas.
Protein requirements
During periods of limitation of nutritional intake, the first priority is to maintain homeostasis, and this requires a constant supply of energy. When a patient is starved, as happens after 5–7 days of zero oral/enteral energy intake, the carbohydrate and lipid stores are depleted. In this situation, energy for body processes must be derived from endogenous protein, which results in the so-called catabolic state. Protein stored in lean muscle and other tissues is shunted to biochemical pathways that turn amino acids into energy in the form of glucose. Homeostasis is therefore maintained at the expense of the formation of structural and other proteins required for recovery. This impairment of protein anabolism, which includes the formation of structural as well as vital metabolic proteins in the form of antibodies, clotting factors, cytokines, and enzymes, probably results in a greater susceptibility to complications. These include failure of primary healing, delayed respiratory competence, slow return of bowel function, renal failure, and impaired humoral and cell-mediated immunity.4, 30, 31 The objective of protein and energy support is therefore to minimize the complications related to acceleration of protein catabolism in the starved state.
In addition to maintaining homeostasis during the superimposed stresses of recovery from surgery, patients with underlying metabolic derangements require large amounts of protein-building substrate. Whereas the average healthy person requires 0.8 g protein daily for maintenance of every 1 kg lean body mass, an increased protein requirement is seen in patients with cancer or other metabolic stressors. Critically ill patients, such as those with a large tumor burden, a systemic inflammatory response such as sepsis, or large surface area burns may require up to 2 g protein/kg/day.32 Most malnourished cancer patients benefit from 90 to 120 g of amino acids, which are commercially prepared as a standard solution mixed with other parenteral components by volume. The normal ratio of nitrogen to calories is 1:150, which is the proportion of carbohydrates and proteins characteristic of most standard enteral formulas. This ratio must be adjusted in patients with altered protein metabolism due to renal or hepatic failure.
Protein is adjusted on the basis of nitrogen balance. The usual starting protein formula includes 1 g/kg/day. For a 60-kg woman, 60 g of amino acids per day would be administered, which converts to approximately 10 g nitrogen (1 mole nitrogen per mole of amino acid). The patient whose protein requirement is not met by this estimate will continue to excrete more nitrogen than she takes in, and she will not be able to build structural and metabolic proteins. For example, if a 60-kg patient was under greater catabolic stress than clinically suspected, she may require 1.5 g protein/kg/day. This would correspond to 90 g of amino acids per day, or 15 g nitrogen. The amount of nitrogen excreted in her urine will give an estimate of the amount of nitrogen retained. When the nitrogen given is equal to the nitrogen excreted, then homeostatic requirements are met, but not exceeded. Obviously, if a patient must heal a wound or deal with metabolic stress, nitrogen must be retained in quantities sufficient to synthesize structural proteins, cytokines, growth factors, enzymes, and immunoglobulins. This nitrogen retention is considered a positive nitrogen balance and is prerequisite for healing and weight gain.
Determination of nitrogen loss in the urine can therefore be a clinically useful measure in determining the adequacy of protein anabolism. Using a standard laboratory assay for urea, urinary nitrogen can be measured in a 24-hour specimen. The number of grams of urine urea nitrogen can be converted to a gross estimate of the amount of excreted nitrogen by adding 20% for respiration and loss through the skin and feces. The goal of nutritional supplementation is met when “nitrogen in,” as calculated from the number of grams of amino acid divided by 6.25, is greater than “nitrogen out.” In this way, endogenous protein production can be monitored, and the effect of the nutritional supplementation can be gauged. This information can also be useful in deciding when to stop nutritional therapy.5, 7, 24, 32, 33
Although most standard protein formulas are composed of relatively equal proportions of essential and nonessential amino acids, there may be some benefit to varying the composition of the amino acids, especially in enteral feeding. Recent investigation has shown that specific amino acids and precursors may be better suited to certain injuries and indications.34 For example, a high concentration of glutamine in enteral and parenteral feeding may enable more rapid recovery of the intestine. This substrate is used as fuel directly by the small intestine, aiding its growth and function. Arginine, a “semiessential” amino acid, may be especially useful in patients with cancer due to poorly characterized immunomodulatory effects.32 Branched-chain amino acids (leucine, isoleucine, and valine) are considered better suited to trauma patients. There are more than 30 different amino acid preparations available.35 Amino acid proportions vary with different commercial enteral and parenteral products.36 Oncologists should seek the advice of consultants who use nutritional therapy more frequently.
As already mentioned, the metabolism of protein also results in an energy dividend of approximately 4 kcal/g. The number of grams of protein may be calculated from the energy requirement in grams of nitrogen, with 1 g nitrogen (or 6.25 g protein) for every 150 cal of energy. This estimates the amount of energy required to utilize each gram of protein for anabolism. Although this formula may seem cumbersome, it allows calculation of calorie and protein needs based on excreted nitrogen, and it can be clinically useful if nitrogen balance is measured by the support team.
Lipid requirements
Modern nutritional supplementation includes a large proportion of the daily energy needs supplied in the form of lipid infusion. Because approximately 9 kcal/g infused is provided, the most efficient way to deliver energy is to use lipid emulsions. There are three principal reasons to use lipids in nutritional support:
- Energy requirements can exceed the glucose threshold, and lipids are therefore given as a source of energy.
- Essential fatty acids are required to produce prostaglandins and steroid hormones.
- Patients with a fluid restriction can receive more calories per volume of lipid emulsion than by any other means; this is especially important in patients with a history of congestive heart failure or kidney disease.
Lipid emulsions provide linoleic and linolenic acids, which are essential nutrients. Without an oral/enteral source of linoleic and linolenic acids, body stores of these essential nutrients will be depleted in 4–6 weeks.37 In addition, energy requirements are best met by using a mixed fuel system that supplies 30–50% of nonprotein calories in lipid form. Lipids can be added to the prescription as separate infusions given intermittently or as slower infusions given with the entire nutritional formula. The maximum recommended lipid dose is 60% of total calorie requirements. Larger proportions may be associated with a detrimental effect on immune function.38 Because lipid emulsions are isotonic with serum, they can be infused through a peripheral vein, providing a large number of calories without complications attributable to CVCs. At least 10 different commercial lipid preparations are available for developing the nutritional prescription.35
Vitamin and trace metal requirements
Supplementation of vitamins and trace metals is required to provide cofactors to enzymatic processes necessary for growth and healing. For most patients, a standard multivitamin supplement (e.g., MVI-12) is added to the prescription as 10 mL per each 24 hours. Other patients with specific deficiencies may require specific supplementation. In gynecologic oncology, many patients have deficiencies based on injury or removal of the terminal ileum due to radiation and/or surgery. This portion of the intestine is important for enterohepatic circulation and the absorption of vitamin B12 and fat-soluble vitamins. Because deep vein thrombosis is common in this population, vitamin K is often iatrogenically antagonized by warfarin. In patients who require specific replacement of vitamins, these special circumstances must be considered, and care must be taken not to induce a further thrombosis.
Most patients will not require vitamin supplementation while in negative nitrogen balance because their protein and energy requirements do not exceed their vitamin stores. Only after the substrates for active metabolism are provided will deficiencies become manifest. MVI-12 contains water-soluble and fat-soluble vitamins, which can be administered intravenously in patients receiving either enteral or parenteral nutrition. The body excretes water-soluble vitamins supplied in excess, but some fat-soluble vitamins (A, D, and E) must be titrated more carefully to avoid toxicity. Vitamin K replacement is required to prevent coagulopathy, and vitamin B12 is necessary to prevent macrocytic anemia and nerve damage. These vitamins are usually given as periodic intramuscular injections, although vitamin B12 is frequently added to the MVI-12. Chronic anemias from effects of chemotherapy and radiation on the bone marrow can be exacerbated by nutritional iron deficiency. As protein is supplemented, anabolic activity may be limited by iron stores, and intramuscular iron supplementation may be necessary.
Trace metals such as zinc, molybdenum, selenium, chromium, manganese, copper, and cobalt are given daily to prevent myriad complications from their deficiency. Zinc deserves specific mention, as it is a nutrient required for wound healing; it becomes especially important in the setting of high-output enterocutaneous fistulas or diarrhea. Zinc supplements may need to be increased in patients at bowel rest for this specific problem, which is seen not infrequently in the gynecologic oncology population.39
Insulin and other additives
Patients who have been in a catabolic state due to malnutrition may not be prepared to adapt to a sudden infusion of glucose and other nutrients. Insulin, which is required for glucose metabolism in the cell and lipolysis for energy production, may not be present in sufficient quantities to begin to use the essential nutrients. Recombinant insulin is now routinely added to intravenous nutritional supplements. A sliding scale of subcutaneous insulin based on urinary glucose concentration is often included in enteral feeding orders to prevent hyperglycemia.
Patients on nutritional supplementation may have derangements in exocrine and endocrine pathways that can result in gastric hyperacidity. Stimulation of the duodenum and ileum may cause the gastric parietal cells to produce acid by reflex. For this reason, histamine receptor (H2) blockers are an important adjunct to enteral nutrition. Changes in the intestinal mucosa can also arise after prolonged periods of parenteral feeding. Intravenous histamine receptor blockers may be valuable in preventing hyperacidity in patients receiving parenteral nutrition as well.
Heparin is also frequently added to nutritional solutions to prevent catheter occlusion or thrombosis. It is administered either by adding 1000 units/L alimentation fluid or by flushing the catheter three times daily with 1000 units. Care must be taken to avoid exacerbating a coagulopathy in a patient with already compromised liver function.
Electrolyte, acid–base, and fluid balance
During the early clinical trials of parenteral nutrition, dehydration and fluid overload were significant problems. Over the ensuing years, management of fluid and electrolytes has been identified as an important component in successful nutritional supplementation. During the initial administration of parenteral or enteral nutrition, it is essential to monitor fluid intake and output. Oral, enteral, and intravenous fluids must be balanced against urinary, oral, nasogastric, fistulous, and fecal outputs, as well as an appropriate adjustment for insensible losses. The estimate of insensible loss must be increased by 10–50% for patients with open wounds, fever, hyperventilation, or burns. Gastrointestinal losses may need to be supplemented separately by a peripheral intravenous line. A good rule of thumb is that specific electrolyte derangements related to underlying conditions, such as excess gastrointestinal or renal losses, should be replaced separate from the nutritional prescription. In this way, nutritional requirements can be gauged periodically and changes made less frequently. As has already been mentioned for patients with TPN, the intravenous access line dedicated to nutritional support should be used only for that purpose. Because electrolyte requirements tend to change frequently, water and specific mineral deficiencies can be adjusted several times a day by using a separate infusion.
Typical fluid and electrolyte requirements for patients receiving TPN are shown in Table 3. These general guidelines are useful as a starting point, but electrolyte supplementation depends on individual patient characteristics and changes over time. For example, patients with underlying renal or cardiac insufficiency may require less sodium than others; patients with magnesium and calcium wasting syndromes related to cisplatin nephrotoxicity may require extra supplementation with these minerals. Patients with renal failure must be given potassium judiciously. In addition, acid-base balance may be disturbed by a variety of respiratory, renal, and gastrointestinal mechanisms that are exacerbated by cancer. In cases of underlying acidosis due to sepsis or cancer, the indication may be for anions to be delivered as acetate salts. This provides a better acid-base buffer than chloride or phosphate. Sodium bicarbonate can be given in background fluids to help regain control of physiologic pH, but patients with acid-base derangements of this magnitude due to cancer commonly require monitoring by critical-care specialists or nephrologists. Of the important physiologic cations, sodium and potassium can be delivered as phosphate, acetate, or chloride salts. In this way, anions can be manipulated to provide extra acid-base buffers as necessary. Commercial amino acid preparations can contain significant electrolyte doses, and it is important to consider this when making calculations.39
Table 3. Calculating minimum fluid requirements
Calculating Fluid Requirement for 24 Hours
24-hour fluid requirement = 100 mL/kg for the second 10 kg
+ 50 mL/kg for the second 10 kg
+ 20 mL/kg for each remaining kg
Example (for a 60-kg patient):
24-hour requirement = (100 mL  10) + (50 mL
10) + (50 mL  10) + (20 mL
10) + (20 mL  40)
40)
= 1000 mL + 500 mL + 800 mL
= 2300 mL
(Adapted from Mann WJ Jr: Nutritional Complications. In Orr JW, Shingleton HM (eds): Complications in Gynecologic Surgery: Prevention, Recognition, and Management. Philadelphia, JB Lippincott, 1994)
METABOLIC COMPLICATIONS OF INTRAVENOUS NUTRITIONAL SUPPLEMENTATION
Patients receiving nutritional supplementation require careful metabolic monitoring until their response to the nutritional prescription reaches a steady state. Vital signs, urine dipstick tests for glucose and ketones, and intake and output should be measured at least three times a day in all patients receiving enteral or parenteral nutrition. Patients who have glucose metabolism problems should have 5–60 units of insulin added to each bag of parenteral nutritional fluid or given subcutaneously according to a sliding scale to be reordered daily. Fluids and electrolytes should be adjusted of the basis of blood tests and urine output. Blood urea nitrogen may be spuriously elevated as a result of the nitrogen content of TPN, and should not result in clinical uremia unless it is greater than 100 mg/dL and urine output is decreased. Weekly or biweekly blood tests should include liver injury indices (transaminase, bilirubin fraction and alkaline phosphatase levels), magnesium, calcium, phosphorus, bilirubin, iron storage protein, prothrombin time, triglyceride levels, and complete blood count. After several normal values have been obtained, these blood tests can be ordered less frequently. Patients who have been stable on home nutritional therapy should have their blood chemistries measured at least weekly; a more complete set of blood chemistries should be evaluated monthly.
Metabolic complications attributable to nutritional therapy are very common, and should be minimized by frequent monitoring and adjustment of nutritional additives. Despite meticulous attention to a particular patient's metabolic requirements, the most common problems result from iatrogenic deficiencies and excesses of the components of the prescription. Imbalances of glucose, calcium, phosphate, magnesium, potassium, sodium, and chloride should be recognized early by careful monitoring and should be corrected. Other problems, such as CO2 retention, hyperammonemia, and deficiencies in essential fatty acids, vitamins, or trace metals, may be harder to recognize.18 Some of these can result in serious injury or death in the already compromised cancer patient.
A well-characterized but poorly understood metabolic complication of nutritional therapy is the “refeeding syndrome.” In patients with chronic malnutrition, the action of bolus infusion of protein, energy, and electrolytes may cause profound disruption of metabolic pathways. In theory, homeostasis in the chronically malnourished host is maintained by a series of tenuous adaptive mechanisms. In these patients, providing energy and protein substrate may saturate low concentrations of downregulated enzymes, receptor sites, and transport mechanisms. Patients may rapidly develop fluid and electrolyte-wasting syndromes with osmotic diuresis and acidosis. This can be avoided by slowly infusing enteric and intravenous nutritional solutions for the first 24–48 hours to allow upregulation of deficient enzymes before instituting full-strength solutions.
Electrolyte deficiencies can be avoided by careful monitoring. Blood levels of calcium, phosphate, magnesium, potassium, and sodium should be measured at least twice weekly until they are normal for 2 weeks. They may then be monitored weekly. The consequences of electrolyte imbalances are significant, but replacement of deficiencies within the hyperalimentation fluid may result in needless inconvenience and expense. Commercial preparations are balanced in salt concentrations and osmolarity, and the addition of extra electrolytes may disrupt the balance. For this reason, it is recommended to provide electrolyte supplements through a separate infusion unless only minor changes are required. It is important to consult with a nutrition pharmacist before adding concentrations of electrolytes to the nutritional formula to correct deficits.
A significant problem can occur if insulin reserves are depleted or glucose transport proteins are saturated in a patient with a high-concentration dextrose infusion. Hyperglycemic hyperosmolar nonketotic coma is characterized by dehydration due to osmotic diuresis, in combination with lethargy, stupor, and disorientation. Blood glucose levels can approach 1 g/dL, and serum osmolarity may be as high as 350 mOsm/L. The treatment of this life-threatening condition is to stop the intravenous infusion, administer insulin at 10–20 units/h, give bicarbonate to reverse acid–base disturbances, and monitor vital functions intensively. These patients are managed much as patients with diabetic ketoacidosis. The most important considerations are (1) correcting dehydration and acid-base and electrolyte disturbances, and (2) managing underlying medical conditions. The current practice of adding insulin to hyperalimentation and delivering a larger proportion of nonprotein calories as lipid has made hyperglycemic nonketotic coma a rare complication of intravenous nutrition.
Hypoglycemia can be a problem as hyperalimentation is weaned or turned off. The normal pancreas produces insulin in relation to the amount of absorbed dietary glucose. When the dextrose infusion is decreased or rapidly stopped, the pancreas continues to secrete insulin, resulting in hypoglycemia. Left untreated, decreased blood sugar can give rise to seizures, and it should be suspected if the patient exhibits mental status changes, excessive sweating, or thirst. In the past this complication was managed by slowly tapering hyperalimentation over a 3–4-day period. The current recommendation is to taper the hyperalimentation over a 24-hour period by reducing the dextrose infusion rapidly to a 10% solution before discontinuing hyperalimentation altogether.40 This strategy does not seem to result in an increased frequency of hypoglycemia.
Other problems that need to be considered in the patient on hyperalimentation include hepatic steatosis due to excess carbohydrate infusion, which can result in biliary stasis and hyperbilirubinemia.41 Fatty infiltration of the liver begins with mild elevations of liver injury indices, usually within the first week of treatment. Alkaline phosphatase and bilirubin elevations reflect progression to biliary stasis. Gallstone formation and jaundice may also occur. Usually these problems are self-limited, but the theoretic risk of progression to cirrhosis in patients with significant biliary stasis or fatty infiltration should mandate a reassessment of calorie compositions and adjustment of carbohydrate fractions. Of course, other causes of hepatic injury should be investigated as well. A cancer patient with liver enzyme elevations should be evaluated for hepatic metastases, infectious hepatitis, or hepatic injury from chemotherapy.
HOME PARENTERAL NUTRITION
Ambulatory home nutrition has been well employed for patients with nonmalignant conditions such as short-bowel syndrome, congenital malabsorption syndromes, inflammatory bowel disease, and anorexia nervosa.24 The remarkable successes achieved in maintaining many of these patients who would otherwise die without benefit of they “artificial intestine” has spurred interest in applying these technologies in patients with terminal diseases. Cancer diagnoses account for the largest proportion of patients starting home nutritional therapy in the United States, and the number of patients receiving this therapy is growing by approximately 25% per year.10 Yet, nutrition therapy has never been validated in the cancer patient either as an adjunct to cancer-directed therapy or as a means of prolonging survival.42, 43, 44 Klein and Koretz30 reviewed more than 70 prospective, randomized, controlled trials and concluded that small improvements in some clinical outcomes could be achieved with the use of nutritional therapy in cancer patients, but complications were significantly increased.
The best theoretic indication for home nutritional therapy in the gynecologic cancer patient is posthospital rehabilitation after potentially curative therapy directed at the malignancy. Nutritional support is indicated, for example, in the patient who has undergone total pelvic exenteration for recurrent cervical cancer. This ultraradical surgery can result in nutritional morbidity in the acute postoperative phase, and prolonged bowel rest followed by anorexia due to a combination of factors may impair healing. A course of intravenous nutrition may allow such a patient to heal bowel and urinary anastomoses, fight infection, and allow slow resumption of normal diet. In this example, 1–2 months of nutritional support can be followed by outpatient weaning, as protein stores are maintained and normal diet resumes. Another example is the patient with malabsorption or dysmotility caused by radiation bowel injury, who is found to be malnourished before contemplated corrective surgery to the intestine. This patient may not be nutritionally fit to undergo the extensive lysis of adhesions and bowel bypass required to solve her problem. Therefore, a target nutritional status (e.g., serum albumin level) may be reached by administering parenteral nutrition at home before performing potentially curative surgery.
Unfortunately, most patients who receive parenteral nutritional support have metastatic disease, and their nutritional compromise is based on progressive cancer. In these patients, the goals of nutritional therapy are usually to provide supportive care in the terminal phase. A great deal of controversy exists regarding the role of nutritional support in patients with terminal cancer, because no prospective trials looking at quality-of-life outcomes have been concluded. Most studies are limited by inadequate sample sizes, poorly defined outcome variables, differences in cancer-related comorbidities, different diseases and treatment regimens, and variable clinical practice patterns. King and associates43 reviewed a diverse group of gynecologic cancer patients treated with home nutritional therapy at the University of Minnesota. No clinically significant improvement was seen in retrospectively applied quality-of-life parameters and performance status. The conclusion of this and other studies was that judicious application of this high-cost technology should be based on better evidence. Until data are available, instituting home nutritional therapy is based on treatment philosophy derived from individual experience, intuition, and anecdote. Further research should determine objective criteria for the use of home nutrition in this population.
DEVELOPMENTS IN NUTRITION THERAPY FOR GYNECOLOGIC CANCER PATIENTS
The prevalence of malnutrition in gynecologic oncology patients remains high. Santoso and coworkers45 studied nutritional parameters in 67 consecutive gynecologic oncology patients at Parkland Memorial Hospital using standardized criteria. The study included indigent patients with tumors from various primary sites (58% had cervical cancer) and early as well as advanced stages of disease; the prevalence of malnutrition was 54% overall. The analysis of the effects of malnutrition showed that the adverse effects of malnutrition were limited to women who were admitted for surgery. The effects were independent of age, extent of disease, or primary tumor. Malnourished women had a 50% longer length of hospital stay (6 versus 9 days). Serum albumin levels correlated well with clinical malnutrition and were inversely correlated with length of hospital stay.
The concept of prolonged bowel rest with nasogastric suction following extensive abdominal surgery has been challenged by general and intestinal surgeons. A meta-analysis published by Cheatham and associates46 demonstrated that nasogastric suction was useful only for a tiny minority of patients. In addition, several well-executed studies are looking at groups of women undergoing gynecologic cancer surgery.47,48 The result of this change in philosophy is that patients are resuming oral calorie intake sooner. The change in utilization of nasogastric suction has been one influence on the observed decrease in hospital stay. It has also undoubtedly reduced the indication for parenteral nutrition owing to prolonged bowel rest. Schilder and colleagues47 reported that reductions in hospital stay were seen, with no significant increase in gastrointestinal complications. In fact, as noted by Kelly and Stanhope,48 many gastrointestinal surgeons place needle catheter jejunostomies as (described previously) for postoperative feeding beginning immediately postoperatively.
Peripherally inserted central venous catheters have gained acceptance in centers in which interventional radiologists are skilled in implanting them. The advantages are fewer complications at insertion, lower cost, and improved cosmetic result. These catheters can be used for blood and chemotherapy infusions and have achieved a degree of acceptance in the gynecologic oncology community.49
CONCLUSION
The possibility of serious complications such as those mentioned in the previous sections requires a frequent reassessment of calorie and protein requirements with an eye toward stopping support as soon as it is no longer needed. For patients with malnutrition due to a progressive disease such as gynecologic cancer, the lack of objective criteria for stopping nutritional support makes avoidance of complications even more important. Philosophic questions related to terminal care must be raised before instituting this costly and potentially dangerous modality. Especially in patients for whom significant prolongation of life with existing treatments is not ensured, nutritional support must be avoided or used to accomplish well-defined short-term goals. Quality of life must be preserved, and although nutritional support may seem to be indicated intuitively, it may not provide the intended result. Careful judgment is required before instituting such an aggressive modality for a patient with a terminal disease. A clear understanding of the patient's circumstances, her disease process, and her prognosis will allow the gynecologic oncologist to confront the difficult decisions about whether to institute, continue, or withdraw nutritional support. The assistance provided by a multidisciplinary team with a good understanding of this evolving technology is required to allow the gynecologic cancer patient to derive maximum benefit from it.
Nutritional therapy remains controversial in the context of treatment of gynecologic cancer. Evidence-based criteria exist for only a small subset of patients. As in the noncancer population, treatment is most effective for patients with self-limited nutritional problems. Nutritional therapy can also be justified when chronic pre-existing nutritional problems render curative therapy difficult. In addition, some patients will suffer intestinal injuries, such as fistulas or obstruction from radiation and surgery, and may have an indication for nutritional support for that reason as an adjunct to effective repair. Supplementation is not generally useful as a palliative component of terminal care.
ACKNOWLEDGMENT
The author acknowledges the assistance of Lisa Sunyecz, PharmD, who critically reviewed the manuscript.
REFERENCES
Rivlin RS, Shils ME, Sherlock P: Nutrition and cancer. Am J Med 75: 843, 1983 |
|
Espat NJ, Moldawer LL, Copeland EM: Cytokine-mediated alterations in host metabolism prevent nutritional repletion in cachectic cancer patients. J Surg Oncol 58: 77, 1995 |
|
Torosian MH: Stimulation of tumor growth by nutrition support. JPEN 16 (suppl): 72S, 1992 |
|
McMillan DC, Preston T, Watson WS et al: Relationship between weight loss, reduction of body cell mass and inflammatory response in patients with cancer. Br J Surg 81: 1011, 1994 |
|
Fischer JE: Metabolism in surgical patients: Protein, carbohydrate, and fat utilization by oral and parenteral routes. In Sabiston DC (ed): Textbook of Surgery, p 103. Philadelphia, WB Saunders, 1991 |
|
Smale BF, Mullen JL, Buzby GP, Rosato EF: The efficacy of nutritional assessment and support in cancer surgery. Cancer 47: 2375, 1981 |
|
Buzby GP: The Veterans Affairs Total Parenteral Nutrition Cooperative Study Group: Perioperative total parenteral nutrition in surgical patients. N Engl J Med 325: 525, 1991 |
|
Clarke-Pearson DL, Rodriguez G, Boente M: Palliative surgery for epithelial ovarian cancer. In Rubin S, Sutton G (eds): Ovarian Cancer, p 351. New York, McGraw-Hill, 1993 |
|
August DA, Thorn D, Fisher RL, Welchek CM: Home parenteral nutrition for patients with inoperable malignant bowel obstruction [see comments]. JPEN 15: 323, 1991 |
|
Howard L: Home parenteral and enteral nutrition in cancer patients. Cancer 72: 3531, 1993 |
|
Tchekmedyian NS: Clinical approaches to nutritional support in cancer. Curr Opin Oncol 5: 633, 1993 |
|
Parnes HL, Aisner J: Protein calorie malnutrition and cancer therapy. Drug Safety 7: 404, 1992 |
|
McGreer AJ, Detsky AS, O'Rourke K: Parenteral nutrition in patients receiving cancer chemotherapy. Ann Intern Med 110: 734, 1989 |
|
Bruera E, MacDonald RN: Nutrition in cancer patients: An update and review of our experience, part 3. J Pain Symptom Manage 3: 133, 1988 |
|
Tchekmedyian NS, Zahyna D, Halpert C, Heber D: Assessment and maintenance of nutrition in older cancer patients. Oncology 6: 105, 1992 |
|
Buzby GP: Overview of randomized clinical trials of total parenteral nutrition for malnourished surgical patients. World J Surg 17: 173, 1993 |
|
Hautamaki RD, Souba WW: Principles and techniques of nutritional support in the patient with cancer. In Bland KI, Karakousis CP, Copeland EM (eds): Atlas of Surgical Oncology, p 741. Philadelphia, WB Saunders, 1995 |
|
Baumgartner TG: Trace elements in clinical nutrition. Nutr Clin Pract 8: 251, 1993 |
|
Payne-James JJ, Khawaja HT: First choice for total parenteral nutrition: The peripheral route. JPEN 17: 468, 1993 |
|
Ballon SC: Effective early postoperative nutrition by defined formula diet via needle-catheter jejunostomy. Gynecol Oncol 14: 23, 1982 |
|
Wells C, Rawlinson K, Tinckler L et al: Postoperative gastrointestinal motility. Lancet 1: 4, 1964 |
|
Nachlas MM, Younis MT, Rada CP, Wityk JJ: Gastrointestinal motility studies as a guide to postoperative management. Ann Surg 175: 510, 1972 |
|
Muggia-Sullam M, Bower RH, Murphy RF et al: Postoperative enteral versus parenteral nutritional support in gastrointestinal surgery. Am J Surg 149: 106, 1985 |
|
Dudrick SJ, Wilmore DW, Vars HM, Rhoads JE: Long-term parenteral nutrition with growth, development, and positive nitrogen balance. Surgery 64: 134, 1968 |
|
Dudrick SJ, O'Donnell JJ, Englert DM et al: 100 patient-years of ambulatory home total parenteral nutrition. Ann Surg 199: 770, 1984 |
|
Fujiwara T, Kawarasaki H, Fonkalsrud EW: Reduction of post-infusion venous endothelial injury with Intralipid. Surg Gynecol Obstet 158: 57, 1984 |
|
Harden JL, Kemp L, Mirtallo J: Femoral catheters increase risk of infection in total parenteral nutrition patients. Nutr Clin Pract 10: 60, 1995 |
|
Wickham R, Purl S, Welker D: Long-term central venous catheters: Issues for care. Semin Oncol Nurs 8: 133, 1992 |
|
Groeger JS, Lucas AB, Coit D: Venous access in the cancer patient. PPO Updates 5: 1, 1991 |
|
Klein S, Koretz RL: Nutrition support in patients with cancer: What do the data really show? Nutr Clin Pract 9: 91, 1994 |
|
Priest BP: Trauma and the septic state: Pathophysiological mechanisms and the role for parenteral nutrition. Trauma Q 7: 12, 1991 |
|
Rombeau JL, Rolandelli RH, Wilmore DW: Nutritional support. In Wilmore DW (ed): Scientific American Surgery, p 1. New York, Scientific American, 1994 |
|
Mullen JL, Buzby GP, Matthews DC et al: Reduction of operative morbidity and mortality by combined preoperative and postoperative nutritional support. Ann Surg 192: 604, 1980 |
|
Pisters PW, Pearlstone DB: Protein and amino acid metabolism in cancer cachexia: Investigative techniques and therapeutic interventions. Crit Rev Clin Lab Sci 30: 223, 1993 |
|
Mann Jr WJ: Nutritional complications. In Orr JW Jr, Shingleton HM (eds): Complications in Gynecologic Surgery: Prevention, Recognition, and Management, p 260. Philadelphia, JB Lippincott, 1994 |
|
Furst P, Albers S, Stehle P: Evidence for a nutritional need for glutamine in catabolic patients. Kidney Intl Suppl 27: S87, 1989 |
|
Heber D, Byerley LO, Chi J et al: Pathophysiology of malnutrition in the adult cancer patient. Cancer 58: 1867, 1986 |
|
Gottschlich MM: Selection of optimal lipid sources in enteral and parenteral nutrition. Nutr Clin Pract 7: 152, 1992 |
|
Seltzer V, Sall S: Nutritional support in patients with gynecologic malignancies. In Sciarra JJ (ed): Gynecology and Obstetrics, p 1. Philadelphia, JB Lippincott, 1987 |
|
Wagman LD, Miller KB, Thomas RB et al: The effect of acute discontinuation of total parenteral nutrition. Ann Surg 204: 524, 1986 |
|
Hager LA: Hepatic complications associated with total parenteral nutrition. Support Line 16: 1, 1994 |
|
Russel DM, Shike M, Marliss EB et al: Effects of total parenteral nutrition and chemotherapy on the metabolic derangements in small cell lung cancer. Cancer Res 44: 1706, 1984 |
|
King LA, Carson LF, Konstantinides N et al: Outcome assessment of home parenteral nutrition in patients with gynecologic malignancies: What have we learned in a decade of experience? Gynecol Oncol 51: 377, 1993 |
|
Nixon DW, Moffitt S, Lawson DH et al: Total parenteral nutrition as an adjunct to chemotherapy of metastatic colorectal cancer. Cancer Treat Rep 65: 121, 1981 |
|
Santoso JT, Canada T, Latson B, et al: Prognostic nutritional index in relation to hospital stay in women with gynecologic cancer. Obstet Gynecol 95:844, 2000 |
|
Cheatham ML, Chapman WC, Key SP, et al: A meta-analysis of selective versus routine nasogastric decompression after elective laparotomy. Ann Surg 221:469, 1995 |
|
Schilder JM, Hurteau JA, Look KY, et al: A prospective controlled trial of early postoperative oral intake following major abdominal gynecologic surgery. Gynecol Oncol 67:235, 1997 |
|
Kelly DG, Stanhope CR: Postoperative enteral feeding: Myth or fact? Gynecol Oncol 67:233, 1997 |
|
Deppe G, Kahn ML, Malviya VK, et al: Experience with the P.A.S.-PORT venous access device in patients with gynecologic malignancies Gynecol Oncol 62:340, 1996 |