Toxic Shock Syndrome
Authors
INTRODUCTION
An abundance of epidemiologic information regarding TSS has been collected since the 1980 “outbreak” of menses- and tampon-associated TSS.5,6,7,8,9,10 TSS occurs in individuals of all ages but most commonly in previously healthy, young (10 to 30 years old), menstruating, white females. The occurrence of TSS has changed dramatically in the past decade. Early in the 1980s, fully 95% of the cases were in females, whereas 5% occurred in males, who suffered a slightly higher fatality rate.5,6 Of the cases occurring in menstruating females, up to 99% involved the use of vaginal tampons, whereas only a few involved the use of pads or other catamenial products.5 Possibly because of changed menses-related hygienic habits and changes in tampon design, menses-related cases have decreased to 70% of the total. Menstrual TSS causes relatively more cases than TSS in males and nonmenstruating women. Menses-associated cases linked to the use of diaphragms and vaginal sponges are now well described. In one case-control study of 28 patients, it was suggested that diaphragm or contraceptive sponge use was associated with a 10-fold increased risk of TSS. The proportion of nonmenstrual cases is greater in studies in which active case finding techniques have been used.6,7,8,9,10 Probably because of improved recognition and treatment, case-fatality ratios as high as 24% in 1980 dropped to approximately 2.6% from 1983 to 1991.5 However, mortality rates for streptococcal TSS remain at 15% to 30%.4,6
At the height of TSS reporting in 1980, up to 14 cases per 100,000 menstruating women per year were tallied.5 Fewer cases have been reported to the Centers for Disease Control nationally in every succeeding year since. Primarily, it is the occurrence of TSS in menstruating women that has appeared to decrease since 1980.6 Active surveillance studies carried out in 1986 showed only 1 case per 100,000 women. The absolute numbers and proportion of menses-associated cases system suggests that changes in microorganisms or host susceptibility, patient behavior, tampon construction (decreased absorbency), or altered constituents involved in the pathogenesis of TSS have occurred since the peak of reported cases in 1980.
Nonmenstrual TSS occurs in a variety of clinical settings, including puerperal sepsis, infection after cesarean section, mastitis, and staphylococcal wound or skin infection, such as abscesses, furuncles, infected abrasions, and insect bites.11,12 TSS even occurs after nasal packing with “nasal tampons.”13 TSS also has presented as pelvic inflammatory disease, postoperative fever, and cervicitis complicating cervical laser therapy.3,14 Infrequently, the distinction between menstrual- and nonmenstrual-related TSS breaks down, as found in Tack's report of an English plumber who abraded his knee and developed florid TSS after dealing with the “messy job” of clearing a tampon-impacted toilet.15
PATHOGENESIS
The accepted cause of TSS is TSST-1. This toxin has had several names, including staphylococcal enterotoxin F and pyrogenic exotoxin C.16,17 TSST-1 is produced by at least 90% of S. aureus strains recovered from menses-associated cases but only 40% to 80% of non-menses-associated strains.16,17 These observations, combined with the results of animal models, suggest that there may be other TSS toxins or that aspects of microbe-toxin-host interactions, including host genomic susceptibilities, may play yet to be discovered roles in producing TSS.18 Staphylococcal enterotoxins B (SEB), C, E, and possibly others share biologic properties with TSST-1 and are structurally similar to streptococcal exotoxin A (i.e. erythrogenic or scarlet fever toxin).17 Schlievert was the first to observe that up to 78% of non-menses-associated strains of Staphylococcus produced TSST-1, SEB, or both and to suggest that SEB or other exotoxins are important in the pathogenesis of TSS or TSS-like disease.17 Crass and Bergdoll demonstrated that coagulase-negative staphylococci (from S. saprophyticus and S. epidermidis) can produce TSST-1 and other implicated enterotoxins.18,19
These staphylococcal or streptococcal TSS-associated exotoxins are members of a larger family of staphylococcal pyrogenic exotoxins (i.e. serotypes A, B, C, D, E, and G) and streptococcal pyrogenic exotoxins (i.e. scarlet fever toxins, serotypes A to C). Each is antigenically distinct but shares properties of being pyrogenic, powerful mitogenic activity for T cells, inhibitory to immunoglobulin production, and able to increase host susceptibility to lethal endotoxin shock.20 All are potent inducers of tumor necrosis factor production.20 These bacterial toxins are recognized as members of a large family of so-called superantigens. Superantigens have the ability to nonspecifically bind with major histocompatibility complex class II antigens and T-cell receptor complexes.21,22
Human colonization with S. aureus capable of producing TSST-1 is relatively common. In one series of 600 women, 9% had labial or vaginal S. aureus.23 TSST-1 was produced by 10% of the S. aureus strains, or 1% of the women overall produced TSST-1. Anterior nares cultures from 11 of 22 healthy children demonstrated S. aureus, and 4 produced TSST-1.16 Nasal microorganisms are frequently found on hands and are easily spread to other body sites and other individuals.23 Inoculation of microorganisms onto vaginal tampons occurs during tampon handling and placement. Serologic findings show that at least 60% to 88% of individuals older than 10 and 20 years old, respectively, possess antibody to TSST-1.24 These and other similar data17,18 suggest that transient colonization with TSST-1-producing strains is widespread and not a new phenomenon.24 Most genital S. aureus carriers and noncarriers possess anti-TSST-1, with staphylococcal enterotoxin A, B, and C antibody levels exceeding those found in patients with acute or convalescing TSS.17,18,24 These findings suggest that the inability to immunologically respond to TSST-1 and to other staphylococcal toxins places the host at a risk for TSS when faced with a relative abundance of toxin.17,18,24 Similar findings were recognized when streptococcal toxin antibodies were studied.4
How susceptible individuals are challenged with an amount of toxin sufficient to cause disease remains an object of intense interest. Superficial vaginal epithelium changes, including scarification and drying, are common during tampon use and do not appear to specifically predispose to TSS.24 TSST-1 is a small molecule and may be readily absorbed across mucosal membranes and wound surfaces.
Increased recovery of S. aureus from the lower genital tract during menstruation or the puerperium suggests that vaginal microecologic changes associated with the presence of menstrual fluid or lochia favor growth of S. aureus.20 Wagner suggested that tampon-induced increased oxygen concentrations within the vagina augment TSST-1 production.25 However, studies on the effect of tampon constituents or their breakdown products on S. aureus and TSST-1 production in vitro yield conflicting results.26,27,28 Schlievert documented general suppression of TSST-1 production and bacterial growth by tampon constituents, whereas others claim amplified toxin production.26 Mills and colleagues found an inverse correlation of magnesium concentration with TSST-1 production in vitro and suggested that certain tampon materials (rayon and polyacrylate) that bind magnesium may promote increased TSST-1 production locally within the vagina.28 In vitro models of the vaginal milieu suggest that the addition of blood is important to maximize TSST-1 production.27 These findings remain to be substantiated in humans or in animal models.
Despite the uncertainty regarding precise pathogenic mechanisms, it is apparent that microorganisms capable of producing TSST-1 and similar substances are not rare and may cause disease in susceptible individuals exposed to microenvironmental conditions that promote toxin production and uptake into the systemic circulation. This appears true whether the infection is in the vagina or is nonmenstrual TSS in other superficial body sites such as skin, breast, or other subcutaneous tissues.
CLINICAL PRESENTATION
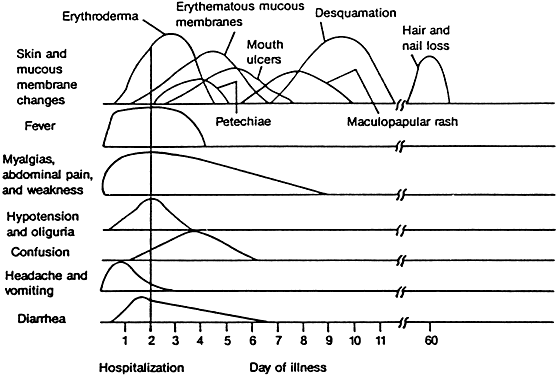
The onset of TSS is usually abrupt, with symptoms of severe disease, including high fever, a sunburn-like diffuse erythema, chills, malaise, headache, sore throat, myalgia, fatigue, vomiting, diarrhea (often with incontinence), abdominal pain, and dizziness or syncope (Fig. 1).1,2 The course of patients with TSS is frequently stormy, marked by dramatic multiorgan dysfunction and possible failure. Altered sensorium with disorientation, somnolence, or agitation is common.28 In some patients, however, onset is gradual, and the characteristic rash is not seen for several days.2 Examination usually reveals a patient with fever, tachycardia, low or unobtainable blood pressure, muscle tenderness (most commonly in the abdominal area), “strawberry” or “beefy” red mucous membranes, and conjunctival hyperemia without a purulent discharge.1,2 Wiesenthal and Todd's “screening” TSS case definition is listed in Table 1.12 In women, erythema and edema may be most prominent in the perineum and inner thighs and can be accompanied by vaginal erythema, edema, and discharge compatible with S. aureus-induced vaginitis in menstrual-associated TSS.2 Menses-associated TSS is frequently associated with signs and symptoms of vaginal inflammation.2
TABLE 1. Diagnostic Criteria for Toxic Shock Syndrome*
Screening TSS Definition
Acute fever (<7 days, 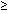 38.5°C or 102°F)
38.5°C or 102°F)
Erythroderma without Nikolsky's sign
Conjunctival hyperemia without purulent exudate
Pharyngeal hyperemia
Case Definition of Toxic Shock Syndrome
Fever (temperature 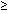 38.9°C or 102°F)
38.9°C or 102°F)
Rash characterized by diffuse macular erythroderma
Desquamation occurring 1–2 weeks after onset of illness
Hypotension (systolic BP 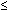 90 mm Hg in adults) or orthostatic syncope
90 mm Hg in adults) or orthostatic syncope
Involvement of three or more of the following:
Gastrointestinal tract (vomiting or diarrhea at onset of illness)
Muscle (myalgia or creatine phosphokinase level twice normal)
Mucous membrane (vaginal, oropharyngeal, or conjunctival hyperemia)
Kidney (BUN or creatinine level twice normal or more, or 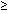 5 WBCs, per high-power field in absence of urinary tract infection)
5 WBCs, per high-power field in absence of urinary tract infection)
Liver (total bilirubin, aspartate transferase [AST], or alanine transferase [ALT] twice normal level)
Blood (platelets 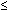 100,000/μl)
100,000/μl)
CNS (disorientation or alterations in consciousness without focal neurologic signs, without fever and hypotension)
Negative throat and cerebrospinal fluid cultures (a positive blood culture for S. aureus does not exclude infection)
Negative serologic tests for Rocky Mountain spotted fever, leptospirosis, rubeola
BP, blood pressure; BUN, blood urea nitrogen; WBCs, white blood cells; CNS, central nervous system.
Pending evidence of absence of other possible causes.
Wiesenthal AM, Ress-men M, Caston SA: Toxic shock syndrome. I. Clinical exclusion of other syndromes by strict screening definitions. Am J Epidemiol 122:847, 1985.
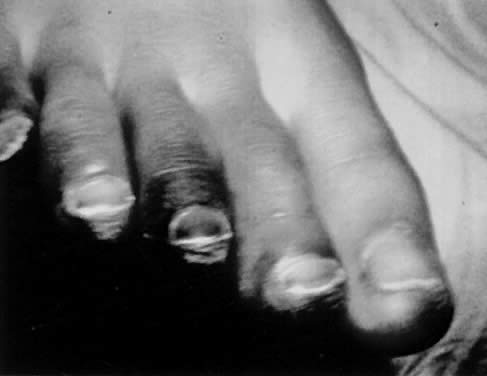
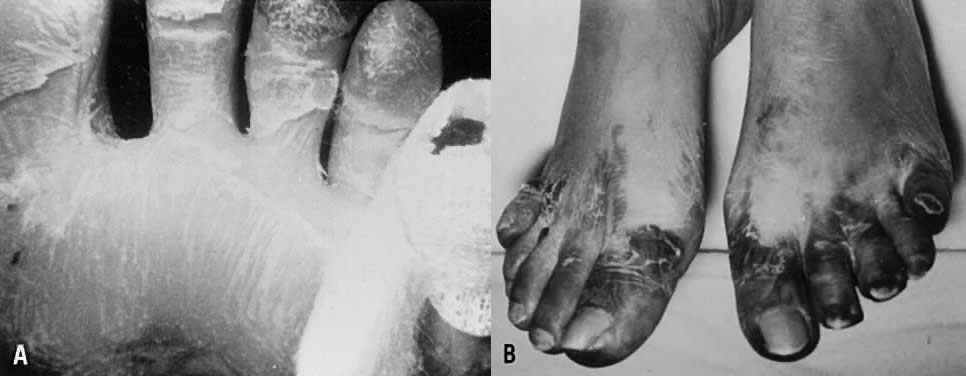
Characteristic delayed manifestations of TSS include oral mucosal ulcerations; a fine, generalized, ashlike desquamation; and peeling of skin at the ends of fingers and toes and on the palms and soles of the hands and feet. These occur in the first and second weeks of illness (Fig. 2). Inadequate perfusion may lead to necrosis and eventual loss of fingers and toes (Fig. 3). The onset and prominence of any of these signs and symptoms may vary (Fig. 1).29
|
|
Mechanisms of death commonly include refractory cardiac arrhythmia, respiratory failure, and disseminated intravascular coagulation. Prolonged sequelae among survivors include chronic renal failure, gangrene of fingers and toes, and loss of hair and nails. Neurologic sequelae, including peripheral neuropathies, impaired memory, and inability to concentrate, have been reported.30
Necropsy findings demonstrate generalized inflammation or necrosis of small vessels, generalized tissue edema, and widespread ulcerated inflamed epithelium, including gastroduodenitis, cholangitis, bronchitis, and bronchiolitis, in addition to acute ulcerative vaginitis in menses-associated cases.31,32 Such cervicovaginal ulcers are not necessarily tampon-induced, because they are also found in women who have never used tampons. In menses-associated cases, paravaginal vasculitis is prominent, suggesting that the vagina is the site of entry for an injurious agent that affects blood vessels and endodermal-derived structures.32
Laboratory test abnormalities reflect multiorgan damage or dysfunction caused by direct toxin effect or secondary organ alterations resulting from vascular changes or hypotension, as well as generalized cytokine release. Most dramatic are the rapid rises in serum creatinine and blood urea nitrogen levels and the yet to be elucidated hypocalcemia and hypophosphatemia. Renal function abnormalities and the presence of casts and sterile pyuria may erroneously suggest pyelonephritis. Other abnormalities include leukocytosis with a left shift, lymphopenia, anemia, thrombocytopenia, and abnormal liver enzyme levels, blood gases, and electrocardiographic findings (Table 2). The differential diagnosis of TSS is extensive (Table 3). The suggested initial evaluation is summarized in Table 4.
TABLE 2. Laboratory Abnormalities in Toxic Shock Syndrome
Abnormality | Patients Affected (%) |
↓ Serum calcium | 83 |
WBCs in urine | 81 |
↓ Total serum protein | 81 |
↓ Serum albumin | 76 |
Leukocytosis with ↑ bands | 72 |
↑ Serum bilirubin | 88 |
↑ AST, ALT | 65 |
↑ Prothrombin time | 64 |
↑ BUN/creatinine | 61 |
↑ Serum creatinine kinase | 53 |
↓ Hemoglobin/hematocrit | 50 |
↓ Serum phosphorus | 50 |
↓ Platelets | 25 |
WBCs, white blood cells; AST, aspartate transferase; ALT, alanine transferase; BUN, blood urea nitrogen.
Adapted from Tofte RW, Williams DN: Clinical and laboratory manifestations of toxic shock syndrome. Ann Intern Med 96:843, 1982.
TABLE 3. Differential Diagnosis of Toxic Shock Syndrome
Exanthemas
Kawasaki's disease (mucocutaneous lymph node syndrome)*
Streptococcal scarlet fever*
Staphylococcal scarlet fever*
Rubeola and rubella
Meningococcemia and other septicemias*
Rocky Mountain spotted fever*
Leptospirosis*
Erythema multiforme
Stevens-Johnson syndrome
Systemic lupus erythematosus
Legionnaire's disease
Gastrointestinal disorders
Gastroenteritis
Staphylococcal food poisoning
Causes of acute abdomen (e.g. appendicitis)
Other disorders
Acute pyelonephritis*
Septic shock*
Hemolytic uremic syndrome
Rhabdomyolysis
Tick typhus
Tularemia
Pelvic inflammatory disease
Acute rheumatic fever
Kawasaki's disease
* Primary differentials.
TABLE 4. Suggested Initial Evaluation and Treatment of Possible Toxic Shock Syndrome Patients
Evaluation
History and physical examination, including pelvic examination
Remove tampons or other objects from vagina; drain wounds
Strongly consider surgical extrapation of focal abscess or local infection
Laboratory tests
Culture blood, vagina, wound, oropharynx, and cerebrospinal fluid if indicated
Urinalysis
CBC with differential and platelet count
Serum electrolyte, calcium, phosphate, and albumin assessment
Liver enzyme determination
Coagulation tests
Chest radiograph
Blood gases
Electrocardiogram
Store serum for serologic tests
Resuscitation and integrated support of all body systems
Intravenous (IV) fluid administration and monitoring (CVP or Swan-Ganz catheter, Foley catheter)
Fluid administration (up to 12 L/d)
Antibiotics
β-Lactamase---resistant antibiotic adequate for S. aureus
If sepsis possible, broad-spectrum coverage until blood cultures negative
If Rocky Mountain spotted fever possible, ensure tetracycline treatment
If group A streptococcal infection, consider treatment with penicillin and/or clindamycin
Measures in selected patients
Corticosteroids (1 g hydrocortisone IV every 6---8 hours for 3 days)
Vasopressor, dopamine
Calcium supplementation
Blood and/or blood components
Respiratory support for ARDS
Renal dialysis
CBC, complete blood count; CVP, central venous pressure; ARDS, adult respiratory distress syndrome.
TREATMENT
Patients with severe TSS must be aggressively monitored in an intensive care unit setting with integrated support of cardiac, respiratory, renal, hepatic, metabolic, and central nervous system functions.33,34,35,36,37 A meticulous examination should be conducted to identify the site of S. aureus infection, which is frequently not apparent. All wounds and the vagina should be immediately examined, and any tampon or other object in the vaginal vault removed. Possibly infected packing and sutures should also be removed. Immediate treatment (beginning within 2 days of onset) with a short course of pharmacologic doses of corticosteroid appears to hasten clinical improvement and should be strongly considered.34 Vigorous and persistent fluid resuscitation is uniformly required, along with careful monitoring of blood pressure, urine output, and central pressure. Adult respiratory distress syndrome and myocardial failure should be anticipated. Assuming that endogenous endorphin release contributes to hypotension and shock, Cohen and colleagues administered 0.4 mg of naloxone intravenously to a patient with TSS. They observed immediate improvement of blood pressure and sustained the effect with a naloxone infusion of 0.05 mg/kg/hour.36 Optimally, patients with only mild TSS or similar illnesses should be hospitalized. If not admitted, patients should be closely observed as outpatients.
Broad-spectrum antibiotic therapy (including Staphylococcus and group A Streptococcus coverage) is necessary until blood cultures are shown to be negative and septicemia is excluded. TSS with persistent bacteremia is rare.37 Antistaphylococcal antimicrobial treatment is used to reduce the risk of recurrence, which can be expected in up to 30% of menses-associated cases.2,3 Limited anecdotal information suggests improved outcome if antistaphylococcal antimicrobial treatment is specifically provided as initial therapy.34 Irrigation and drainage of infected vaginal or wound surfaces to reduce concentrations of remaining microorganisms and toxin appear reasonable but remain unstudied.
Renal impairment is a common finding in TSS, and hemodialysis or peritoneal dialysis may be required.38,39 Despite frequent thrombocytopenia and coagulation disorders, frank hemorrhage is uncommon.38,40 Vitamin K should be given for hypoprothrombinemia in cases of severe hepatic derangement.38 If uncontrolled bleeding occurs, transfusion of fresh frozen plasma, platelets, and fresh whole blood may be undertaken.39,40,41 Plasma exchange was helpful in a patient presenting with TSS and thrombolytic thrombocytopenia.41 Exchange transfusion to remove presumed toxin has been attempted on occasion without success, but it needs systematic evaluation.
Death may occur despite intensive care. More specific treatment awaits further understanding of the pathogenesis. Chesney's suggestion that an antitoxin with specific activity against the responsible toxin would be of use but remains to be evaluated,29 as does the possibility of active vaccination with the TSST-1 antigen. Polyvalent immunization against TSST-1 and the related staphylococcal and streptococcal exotoxins would appear ideal. Use of anti-group A streptococcal antibody has also been suggested. Factors effective against superantigen-induced cytokines and possibly against endotoxin doubtless be evaluated in the future.
TOXIC SHOCK AND REPRODUCTIVE CARE
Health care professionals providing reproductive care must be familiar with TSS for several reasons:
- Their patients are often the young, menstruating women who are at greatest risk.
- They are frequently sources of information regarding menses-related problems and catamenial products.
- They provide contraception, obstetric, and surgical services that may be complicated by TSS (Table 5).
TABLE 5. Toxic Shock Syndrome in Obstetric and Gynecologic Settings
Obstetric settings
Postpartum: after vaginal or cesarean section delivery
Mother-newborn transmission
Mastitis
Gynecologic settings
Postoperative: any procedure with frequently occult superficial infection
Vaginitis or vaginal discharge
Pelvic inflammatory disease
Use of vaginal tampons; anecdotal association with diaphragm and various sponges
Possible sexual transmission
Many cases of TSS occur in menstruating females, and most of these are associated with tampon use.5 Rare cases are associated with diaphragm, vaginal contraceptive, or catamenial sponge use.6,7,8,9,10 The use of any contraceptive method is associated with an overall decreased risk of TSS.42,43,44 Oral contraceptives reduce the amount and duration of menstrual blood and have been recommended as the contraceptive of choice in women with recurrent TSS.45 However, barrier methods of contraception (i.e. vaginal sponge and diaphragm) have been associated with reports of TSS.46,47,48,49 Analogies between the use of barrier contraceptives and another foreign body applied to a mucus membrane (e.g. tampons) support a common pathophysiology of TSS. Notable features of these cases were prolonged retention for 24 hours or more and difficult removal.49,50 Most of these patients were not menstruating; some were lactating, and a few noticed an abnormal vaginal discharge before using the sponge or diaphragm. Rates of S. aureus colonization are increased in diaphragm users compared with other contraceptive users, presumably because of autoinoculation during diaphragm insertion.51,52 The risk of TSS in sponge users was estimated to be extremely low at 9 cases per 16 million sponges, or 0.28 cases per 1 million nonmenstrual days.50 The sponge has been withdrawn from the market for other reasons. Diaphragm users should limit retention and not use the diaphragm with an undiagnosed abnormal vaginal discharge.
TSS has not been associated with cervical cap use. None of the epidemiologic studies found an increase risk of TSS attributable to the intrauterine device (IUD),44 although IUD users have increased rates of S. aureus colonization.52
More than 30 cases of TSS are reported in postpartum women, which is not surprising considering that 1% of women carry TSST-1-producing strains of S. aureus in the lower genital tract.3,5,53 TSS may complicate postpartum endometritis and infection after cesarean section and gynecologic and surgical operations.3,6 The newborn is also colonized with genital tract microflora at birth, and the simultaneous onset of maternal-neonatal TSS has been reported.53 S. aureus is the most common cause of mastitis, and TSS may complicate this common infection.3 Although never surgically documented, clinical findings suggestive of pelvic inflammatory disease are often associated with menstrual TSS.3 This suggests that endometrial and fallopian tube inflammation may occur because of the presence of S. aureus or TSST-1. The simultaneous onset of TSS in a married couple suggests that sexual transmission occurs and that susceptible sexual partners may be at risk.
An inapparent wound infection with toxin-producing S. aureus may cause TSS.53,54,55 TSS has occurred after laparoscopy, ovarian cystectomy, and hysterectomy. This situation is reminiscent of tetanus, in which clinically uninflamed Clostridium tetani-infected wounds may prove lethal. Postoperative or postpartum onset of high fever, rash, and hypotension should prompt an immediate search for a wound site infection and the consideration of TSS. Any surgical packing or vaginal tampon must be removed. Prompt physician response may be lifesaving.
PREVENTION
Recommendations for prevention of menstrual-associated TSS remain speculative until the pathogenesis of the disease is better understood. However, presumptive recommendations may be made on the basis of current knowledge.29,56 Continual use of tampons through menses and use of highly absorbent tampons should be avoided.57 Tampons with the greatest amount of absorbency have been removed from the market by manufacturers. Limiting tampon use to the days of heaviest menstrual flow and switching to napkins or pads while sleeping appears appropriate. Tampons for midcycle bleeding, symptomatic discharge, or leukorrhea can be avoided with the alternative use of minipads and appropriate medical care. The fingers and vulva are colonized by S. aureus and careful handwashing before handling a fresh tampon and the separation of the vulva during gentle tampon insertion can be recommended.58 Vulvar skin and hand cleansing before the insertion of any tampon or contraceptive device can decrease the inoculation of microorganisms into the vagina.59 Tampons and vaginal contraceptives probably should be avoided in the presence of S. aureus infection elsewhere in the body, including boils, paronychia, or other pyodermas. Handwashing should become customary after handling used tampons.
Communicability of TSS-associated strains of S. aureus or other bacteria remains poorly studied. Family members are commonly colonized with TSST-1-producing S. aureus.20 Reports of coincident TSS in a mother-newborn pair53 and among sexual partners54 suggest that transmission and disease may occur in susceptible individuals. Newborns of mothers with postpartum TSST or similar syndromes should be given a full course of antistaphylococcal antibiotics, because they have not received anti-TSST-1 antibody transplacentally. Spread of TSST-1-producing, non-coagulase-producing staphylococci and streptococci remains unstudied. Patients, medical care providers, and others should exercise caution and cleanliness in handling used tampons and possibly infectious secretions.58 Use of oral contraceptives or use of condoms along with nonoxynol-9-based spermicides appears to be epidemiologically associated with a decreased risk in some studies.60 Although prolonged use of tampons is not specifically associated with TSS, women who “lose” tampons or vaginal devices should be seen promptly, so that the object may be recovered and bacterial overgrowth avoided.59,61 Proof of the efficacy of any of these recommendations await further study. Other reviews have become available.62,63,64,65
CONCLUSIONS
TSS is a multisystem, potentially lethal (2% to 5%) illness that primarily affects women (70% to 90%). The disease is characterized by sudden onset of fever, hypotension, scarlatiniform (sunburn-like) rash, involvement of three main organ systems, and delayed desquamation, most prominently of the palms and soles. The syndrome may recur in up to 30% of menses-associated cases. Menses-associated TSS accounts for at least 90% of TSS in postpubertal females. TSS also occurs in males and nonmenstruating females of any age.
TSS is the result of in vivo production of a toxin at the site of localized, often asymptomatic infection with enterotoxin-producing strains of S. aureus, non-coagulase-producing staphylococci, and various streptococci.66 Staphylococci produce a variety of substances, most important of which is TSST-1. TSST-1 is implicated in 90% of menstrual TSS cases and 40% to 60% of nonmenstrual TSS cases. TSS-like diseases are also associated with exotoxins produced by staphylococci and streptococci: staphylococcal enterotoxins B and C1 and the streptococcal pyrogenic exotoxin A.
TSS should be considered strongly in any menstruating women with fever and in any individual with fever and shock. Screening diagnostic criteria include scarlatiniform erythroderma, pharyngitis, nonpurulent conjunctivitis, and fever. In women, initial assessment and treatment must include a pelvic examination with removal of any vaginal objects, drainage of any abscesses or wound infections, and appropriate cultures and other laboratory tests. Treatment consists of aggressive, integrated support of all organ systems. Treatment with antistaphylococcal antimicrobials may lessen mortality and reduces the risk of recurrence. Prompt administration of steroids ameliorates TSS.
REFERENCES
Todd J, Fishaut M, Kapral F, Welch T: Toxic-shock syndrome associated with phage-group-I staphylococci. Lancet 2: 1116, 1978 |
|
Chesney PJ, Bergdoll MS, Davis JP, Vergeront JM: The disease spectrum, epidemiology and etiology of toxic shock syndrome. Annu Rev Microbiol 38: 315, 1984 |
|
Wager GP: Toxic shock syndrome: a review. Am J Obstet Gynecol 146: 93, 1983 |
|
Davies HD, McGeer A, Schwartz B, et al: Invasive group A streptococcal infections in Ontario, Canada. N Engl J Med 335: 547, 1996 |
|
Reingold AL: Epidemiology of toxic-shock syndrome, United States, 1980–1984. MMWR Morb Mortal Wkly Rep 33:19SS, 1984 |
|
Broome CV: Epidemiology of toxic shock syndrome in the United States: overview. Rev Infect Dis 11 (Suppl): S14, 1989 |
|
Gaventa S, Reingold AL, Hightower AW et al: Active surveillance of toxic shock syndrome in the United States, 1986. Rev Infect Dis 11 (Suppl): S28, 1989 |
|
Petitti DB, Reingold AL: Update through 1985 on the incidence of toxic shock syndrome amongmembers of a prepaid health plan. Rev Infect Dis 11 (Suppl): S22, 1989 |
|
Schwartz B, Gaventa S, Broome CV et al: Nonmenstrual toxic shock syndrome associated with barrier contraceptives: report of a case-control study. Rev Infect Dis 11 (Suppl): S48, 1989 |
|
Reingold AL, Broome CV, Gaventa S, Hightower AW: Risk factors for menstrual toxin shock syndrome: results of a multistate case-control study. Rev Infect Dis 11 (Suppl): S35, 1989 |
|
Petitti D, D'Agustino RB, Oldman MJ: Nonmenstrual toxic shock syndrome: methodologic problems in estimating incidence and delineating risk factors. J Reprod Med 32: 10, 1987 |
|
Todd JK, Wiesenthal AM, Ressman M et al: Toxic-shock syndrome. II. Estimated occurrence in Colorado as influenced by case ascertainment methods. Am J Epidemiol 122: 857, 1985 |
|
Barbour SD, Shlaes DM, Guertin SR: Toxic-shock syndrome associated with nasal packing: analogy to tampon-associated illness. Pediatrics 73: 163, 1984 |
|
Bowen LW, Sand PK, Ustergard DR: Toxic shock syndrome following carbon dioxide laser treatment of genital tract condyloma acuminatum. Am J Obstet Gynecol 154: 145, 1986 |
|
Tack KJ: Possible tampon-associated illness. Pediatrics 73: 163, 1984 |
|
Garbe PL, Arko RJ, Reingold AL et al: Staphylococcus aureus isolates from patients with nonmenstrual toxic shock syndrome: evidence for additional toxins. JAMA 253: 2538, 1985 |
|
Schlievert PM: Staphylococcal enterotoxinB and toxic shock syndrome toxin-1 are significantly associated with non-menstrual TSS. Lancet 1: 1149, 1986 |
|
Crass BA, Bergdoll MS: Toxin involvement in toxic shock syndrome. J Infect Dis 153: 918, 1986 |
|
Crass BA, Bergdoll MS: Involvement of coagulase-negative staphylococci in toxic shock syndrome. J Clin Microbiol 23: 43, 1986 |
|
Fast DJ, Schlievert PM, Nelson RD: Toxic shock syndrome-associated staphylococcal and streptococcal pyrogenic toxins are potent inducers of tumor necrosis factor production. Infect Immun 57: 291, 1989 |
|
Schlievert PM: Role of superantigens in human disease. J Infect Dis 167: 997, 1993 |
|
Johnson HM, Torres BA, Soos JM: Superantigens: structure and relevance to human disease. Proc Soc Exp Biol Med 212: 99, 1996 |
|
Linnemann CC, Staneck JL, Hornstein S et al: The epidemiology of genital colonization with Staphylococcus aureus. Ann Intern Med 96: 940, 1982 |
|
Bonaventure PF, Linnemann C, Weckbach LS et al: Antibody responses to toxic shock syndrome (TSS) toxin by patients with TSS and by healthy staphylococcal carriers. J Infect Dis 150: 662, 1984 |
|
Wagner G, Bohr L, Wagner P, Petern LN: Tampon-induced changes in vaginal oxygen and carbon dioxide tensions. Am J Obstet Gynecol 148: 147, 1984 |
|
Schlievert PM, Shands KN, Dann BB et al: Identification and characterization of an endotoxin from Staphylococcus aureus associated with toxic shock syndrome. J Infect Dis 143: 509, 1981 |
|
Kirkland JJ, Ryan CA, Kohrman KA, Danneman PJ: Growth of Staphylococcus aureus and synthesis of toxic shock syndrome toxins in different in vitro systems. Rev Infect Dis 11(Suppl):SI88, 1989 |
|
Mills JT, Parsonnet J, Tsai YC et al: Control of production of toxic-shock-syndrome toxin-1 (TSST-1) by magnesium ion. J Infect Dis 151: 1158, 1985 |
|
Chesney PJ, Crass B, Polyak MB et al: Toxic shock syndrome: management and long term sequelae. Ann Intern Med 96: 847, 1982 |
|
Rosene KA, Copass MK, Kastner LS et al: Persistent neuropsychological sequelae of toxic shock syndrome. Ann Intern Med 96 (Part 2):865, 1982 |
|
Blair JD, Livingston DG, Vongsnichakul R: Tampon related toxic shock syndrome: histopathologic and clinical findings in a fatal case. Hum Pathol 12: 16, 1981 |
|
Abdul-Karim FW, Lederman MM, Carter JR et al: Toxic shock syndrome: clinicopathologic findings in a fatal case. Hum Pathol 12: 16, 1981 |
|
Todd JK: Therapy of toxic shock syndrome. Drugs 39: 856, 1990 |
|
Todd JK, Ressman M, Caston SA et al: Corticosteroid therapy for patients with toxic shock syndrome. JAMA 252: 3399, 1984 |
|
Vanderhyden JS, Renard JM, Dehaem M, Bal J: Nonmenstrual toxic shock syndrome: a case report and a review of non-menstrual toxic shock syndrome in Western Europe. Eur J Obstet Gynecol Reprod Biol 22: 243, 1986 |
|
Cohen KR, Emmons KM, Goldstein MF: Naloxone treatment of toxic shock syndrome. Arch Intern Med 143: 1072, 1983 |
|
Crowther MA, Ralph ED: Menstrual toxic shock syndrome complicated by persistent bacteremia: case report and review. Clin Infect Dis 16: 288, 1993 |
|
Clark JDA, Tan LB, Edwards OM: Toxic shock: clinical presentation and management II. Postgrad Med J 61 (Suppl 1): 27, 1985 |
|
Thomas D, Withington PS: Toxic shock syndrome: a review of the literature. Ann R Coll Surg Engl 67: 156, 1985 |
|
Jespersen J, Rasmussen NR, Toftgaard C: Observation during the treatment with antithrombin-Ill concentrate of a case of tampon-related toxic shock syndrome and disseminated intravascular coagulation: discrepancies between function and immunologic determination of antithrombins. Thromb Res 26: 457, 1982 |
|
Toffelmire EB, Clark WF, Cordy PE et al: Plasma exchange in thrombotic thrombocytopenia puerpera. Can Med Assoc J 131: 1371, 1987 |
|
Davis JP, Chesney J, Wand PJ et al: Toxic shock syndrome: epidemiologic features, recurrence, risk factors, and prevention. N Engl J Med 303: 1429, 1980 |
|
Toxic shock syndrome—United States. MMWR Morb Mortal Wkly Rep 29:229, 1980 |
|
Shands KN, Schmid GF, Dan BB et al: Toxic shock syndrome in menstruating women: association with tampon use and Staphylococcus aureus and clinical features in 52 cases. N Engl J Med 303: 1436, 1980 |
|
Melvor ME, Lewis ML: Treatment of recurrent toxic shock syndrome with oral contraceptive agents. Md St Med J 31: 56, 1982 |
|
Baehler EA, Dillon WP, Cumbo TJ et al: Prolonged use of a diaphragm and toxic shock syndrome. Fertil Steril 38: 248, 1982 |
|
Loomis L, Feder HM: Toxic shock syndrome associated with diaphragm use [Letter]. N Engl J Med 305: 1585, 1981 |
|
Jaffe R: Toxic shock syndrome associated with diaphragm use [Letter]. N Engl J Med 305: 1585, 1981 |
|
Toxic shock syndrome and the vaginal contraceptive sponge. MMWR Morb Mortal Wkly Rep 33:43, 1984 |
|
Faich G, Pearson K, Fleming D et al: Toxic shock syndrome and the vaginal contraceptive sponge. JAMA 255: 216, 1986 |
|
Lansdell LW, Taplin D, Aldrich TE: Recovery of Staphylococcus aureus from multiple body sites in menstruating women. J Clin Microbiol 20: 307, 1984 |
|
Guinan ME, Dan BB, Guidoth RJ, et al: Vaginal colonization with Staphylococcus aureus in healthy women. Ann Intern Med 96: 944, 1982 |
|
Green SL, LaPeter KS: Evidence of postpartum toxic shock syndrome in a mother-infant pair. Am J Med 72: 169, 1982 |
|
Brawley RL, Harrison WO: Sexual transmission of toxic shock syndrome. N Engl J Med 306: 750, 1982 |
|
Bartlett P. Reingold AL, Graham DR et al: Toxic shock syndrome associated with surgical wound infection. JAMA 247: 1448, 1982 |
|
Gleckman RA, Roth RM: Fever following abdominal surgery: unusual infectious causes. Postgrad Med 79: 287, 1986 |
|
Schuchat A. Broome CV: Toxic shock syndrome and tampons. Epidemiol Rev 13: 99, 1991 |
|
Berkley AS, Micha JP, Freedman KS, Hirsch JC: The potential of digitally inserted tampons to induce vaginal lesions. Obstet Gynecol 60: 31, 1985 |
|
Shelley WB: Preventing tampon-associated toxic shock. Lancet 1: 21, 1982 |
|
Shelton JD. Higgins JE: Contraception and toxic shock syndrome: a reanalysis. Contraception 24: 631, 1981 |
|
Friedrich EG Jr: Tampon effects on vaginal health. Clin Obstet Gynecol 24: 395, 1981 |
|
Reingold AL: Toxic shock syndrome: an update. Am J Obstet Gynecol 165: 1236, 1991 |
|
Parsonnet J: Non-menstrual toxic shock syndrome: new insights into diagnosis, pathogenesis and treatment. Curr Clin Top Infect Dis 16: 1, 1996 |
|
Stevens DL. The toxic shock syndromes. Infect Dis North Am 10:727, 1996 |
|
Stevens DL. Streptococcal toxic-shock syndrome: spectrum of disease, pathogenesis and new concepts in treatment. Emerg Infect Dis 1: 69, 1995 |
|
Breiman R, Davis J, Flockam R: Defining the group A streptococcal toxic shock syndrome: rationale and consensus of definition. JAMA 269: 390, 1993 |