The Bony Pelvis
The pelvis is made of a bony girdle that has a central canal. Its structure must be strong enough to transfer the weight of the body from the spine to the femurs, and yet it must have a large enough opening to allow for a term fetus to be delivered through it.
There are three separate parts to the pelvis: the single midline sacrum and paired innominate bones (os coxae). The line of division between the sacrum and the innominate bones is the sacroiliac joint, while the two innominate bones are separated from one another by the pubic symphysis (Fig.1 and Fig. 2).
|
Each innominate bone is formed from three bones: the ilium, the ischium, and the pubis. These bones have fused into a single unit before reproductive age is reached. Their individual names persist, however, in terms such as the iliac crest, ischial tuberosity, and pubic ramus.
These bony parts are assembled to form a pelvis, which has traditionally been divided into an upper false pelvis and a lower true pelvis, separated from one another by the linea terminalis. The false pelvis forms the lower part of the abdominal cavity. It is bounded laterally by the iliac bones, posteriorly by the lumbar spine, and anteriorly by the abdominal wall. It has little obstetrical significance.
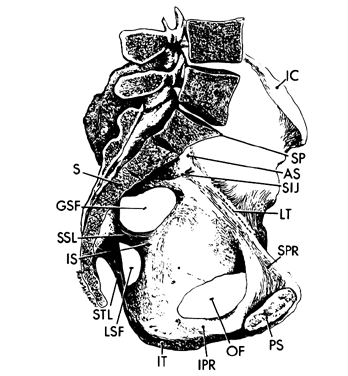
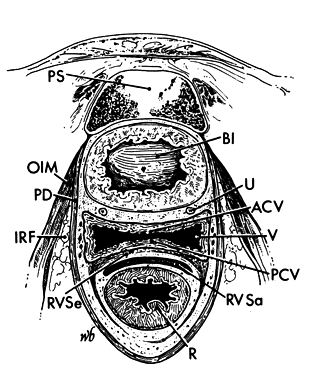
The canal of the true pelvis is bent forward in its lower portion (see Fig. 2) in the curve of Carras. The change in direction of this space is partly due to the curve of the sacrum but is also caused by the muscles of the pelvic floor.
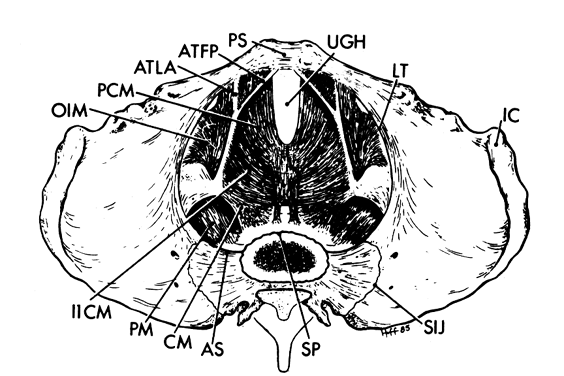
The rim that surrounds the upper opening of the true pelvis is called the inlet and is formed by the promontory and alae of the sacrum posteriorly, by the inner surface of the superior pubic rami anteriorly, and by the linea terminalis laterally (see Fig.1 and Fig. 2). The shape of the inlet as well as the other planes of the pelvis are important to the mechanism of labor and are covered in a later chapter in this volume.
Within the true pelvis the lateral pelvic walls slant toward one another at approximately a 15° angle so that lines drawn down these walls would intersect at the level of the knees. Because of the inward inclination of the walls and protrusion of the ischial spines into the pelvic cavity (without concomitant shortening of the anterior posterior dimension), the middle portion of the pelvic cavity becomes longer in its anterposterior diameter than in the transverse. The level of the midplane is marked on each wall by the ischial spine. It passes through the lower border of the pubic symphysis and the junction of the fourth and fifth sacral vertebrae (see Fig. 2).
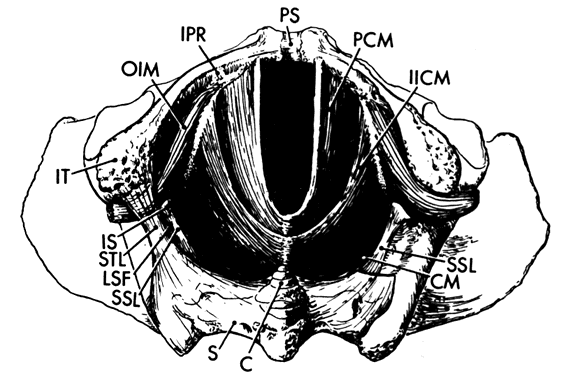
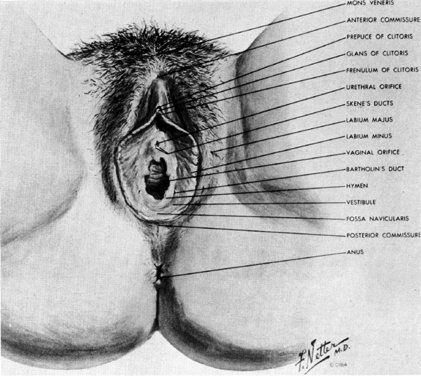
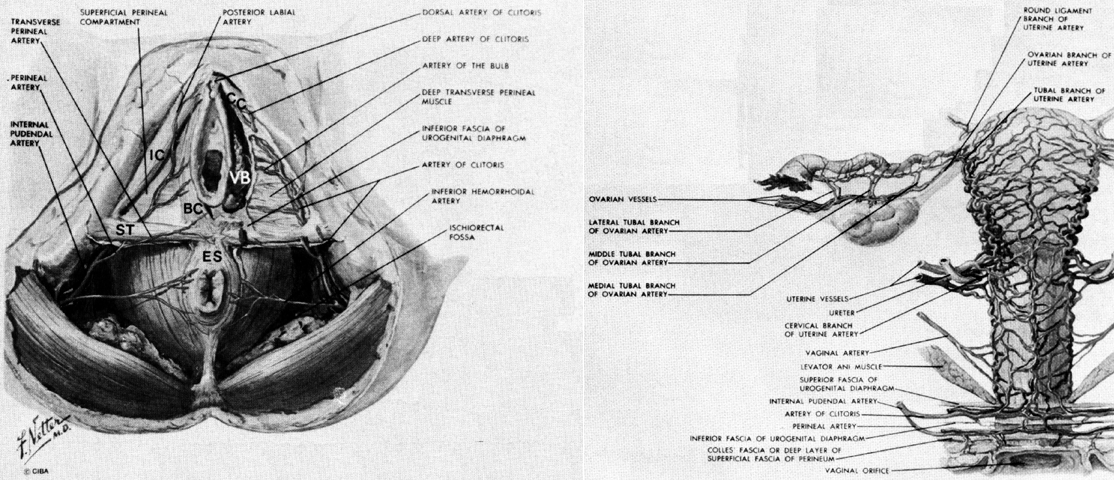
The pelvic outlet (Fig. 3) is formed by two triangles fitted base to base to form a diamond. The anterior (urogenital) triangle has its corners at the lower end of the pubic symphysis and the inner aspects of the ischial tuberosities. It is bounded laterally by the inferior ischiopubic rami. The posterior (anal) triangle has its apex at the tip of the sacrum and shares its base with the anterior triangle. The lateral borders of the posterior triangle are the sacrotuberous ligaments.
|
The pelvis has three joints: two sacroiliac joints and the pubic symphysis. The sacroiliac joints are true synovial joints, but the symphysis is a synchrondrosis, without a synovial space. Although immobile during most of life, these joints do display some movement during pregnancy. 1,2
Each hemipelvis contains three lateral openings in its wall. These are the obturator foramen and the greater and lesser sciatic foramina (see Fig. 2). The sacrospinous ligament separates the two sciatic foramina and has a broad attachment to the lateral surfaces of the lower sacrum and coccyx and an apical insertion into the ischial spine. It is covered on its pelvic surface by the coccygeus muscle (Fig.2 and Fig. 3). At the bottom of the lesser sciatic foramen is the sacrotuberous ligament. It arises from the posterior iliac spines and the back and side of the lower sacrum and coccyx and ends at the ischial tuberosity. These ligaments help to stabilize the pelvis and probably undergo the same softening that the ligaments around the pelvic articulations experience.
Muscles of the Pelvis
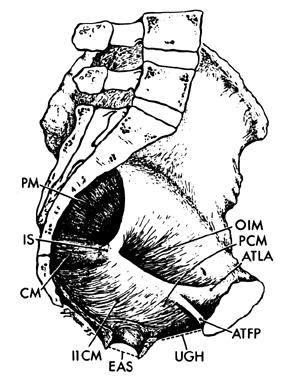
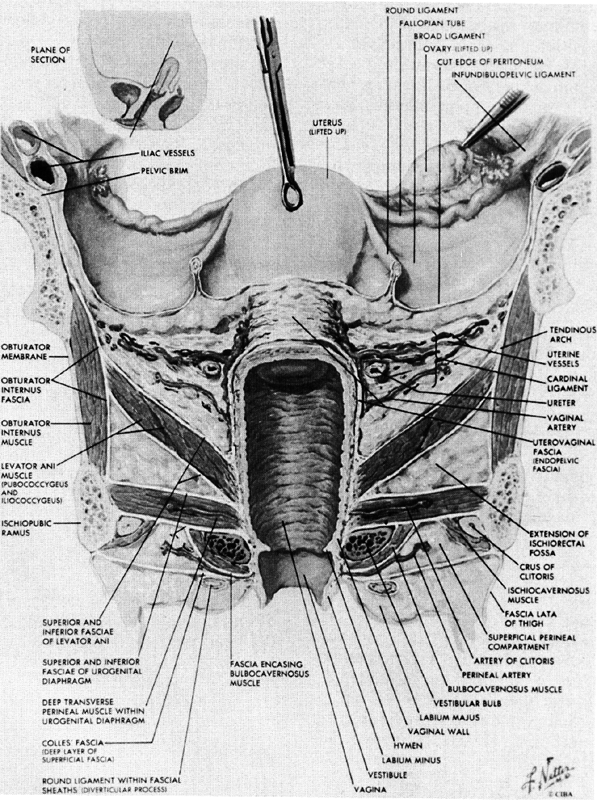
When a bony pelvis and model of a fetal head are used to demonstrate forceps delivery or mechanisms of labor there exists an obvious space between the fetal head and the osseous structures that is so large that the head can easily fall through the pelvic canal. This space is filled by the soft tissues of the pelvis. There are two components to these tissues. The first includes the muscles of the pelvic wall (Fig. 4), a series of muscles that cover the inner surfaces of the bony pelvis, following its shape and exerting their action on the hip. The second component is the pelvic floor, which supports the abdominal and pelvic viscera and whose resistance must be overcome by the presenting part during delivery. The pelvic floor consists of the pelvic diaphragm, which stretches across the entire pelvic cavity at the level of the midplane, and the urogenital diaphragm and external genital muscles, which span the anterior portion of the pelvic outlet.
|
MUSCLES OF THE PELVIC WALL.
Arising from the inner surface of the obturator foramen and membrane, the obturator internus muscle leaves the pelvis through the lesser sciatic foramen to insert into the medial surface of the greater trochanter. The piriformis muscle arises from the anterior aspect of the sacrum. It passes through the greater sciatic foramen and inserts into the upper border of the greater trochanter. The obturator internus muscle is innervated by the obturator nerve and the piriformis muscle is innervated by a branch from the sacral plexus. Both muscles are lateral rotators and abductors of the thigh.
MUSCLES OF THE PELVIC DIAPHRAGM.
The muscles of the pelvic wall do little to close off the opening in the pelvis. A fetal head would still fall through the pelvic opening were it not closed off by the pelvic diaphragm. There are three muscles in the pelvic diaphragm: the pubococcygeus, the iliococcygeus, and the coccygeus. The pubococcygeus muscle arises from the inner surface of each pubic bone to pass posteriorly on either side of the urethra, vagina, and rectum. Behind the rectum some fibers bend back anteriorly to join the muscle on the other side, thereby forming a sling. Other fibers insert into the sacrum and coccyx. Some of the most medial fibers within this group attach to the walls of the vagina and rectum.
The iliococcygeus muscle arises from a series of tendon-like fibers that attach to the fascia of the obturator internus muscle (the arcus tendineus levator ani). From these broad origins the fibers of the iliococcygeus insert into the anococcygeal raphe and the coccyx. The coccygeus arises from the ischial spine and the sacrospinous ligament to insert into the borders of the coccyx and the lowest segment of the sacrum.
These muscles are covered on their superior and inferior surfaces by the superior and inferior fasciae of the pelvic diaphragm. These fasciae arise from the obturator internus fascia and also in certain areas from the pubic bones. They fuse at the urogenital hiatus with the urogenital diaphragm and vagina.
The iliococcygeus and coccygeus muscles receive their innervation from an anterior branch of the ventral rami of the third and fourth sacral nerves while the pubococcygeus muscle is supplied by the pudendal nerve.
The muscle fibers of the pelvic diaphragm form a “U” with the open end directed anteriorly. The open area within the “U” through which the urethra, vagina, and rectum pass is called the urogenital hiatus. The normal tone of these muscles keep the base of the “U” pressed against the back of the pubic bones, squeezing the urethra, vagina, and rectum closed. During labor, this sling pulls the presenting part anteriorly once it has passed the midplane to assist in rotation.
Blood Vessels of the Pelvic Wall
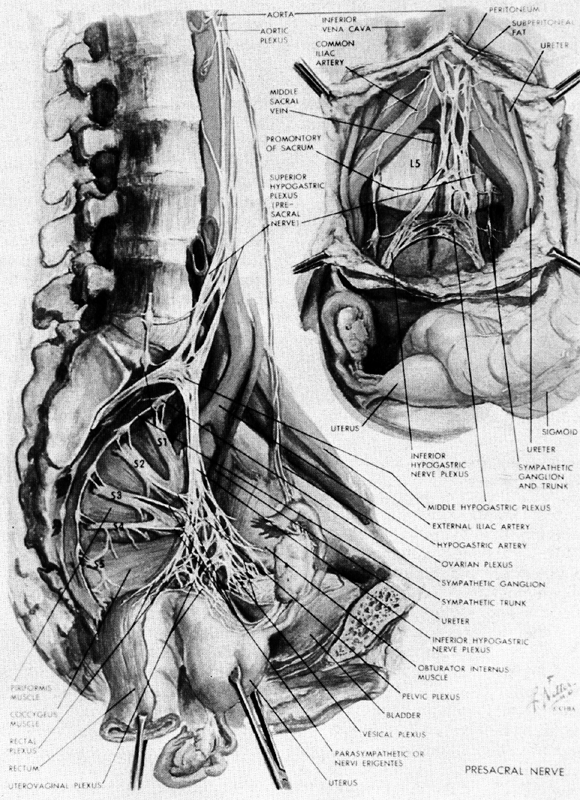
The aorta lies on the lumbar spine slightly to the left of the vena cava, which it overlies (Fig. 5). Both the aorta and vena cava are subject to compression by the uterus in this location when a patient is supine. At the level of the fourth lumbar vertebra (on a line between the tops of the iliac crests) the aorta bifurcates into the left and right common iliac arteries. After about 5 cm the common iliac arteries give off the internal lilac artery from their medial side and continue toward the inguinal ligament as the external iliac artery. This division occurs in the area of the sacroiliac joint.
The branching pattern of the internal iliac arteries and veins is extremely variable.3 A description of a common variant will be included here. The internal iliac artery supplies the viscera 9f the pelvis as well as many of the muscles of the pelvic wall and gluteal region. It usually divides into an anterior and posterior division 3 cm to 4 cm after leaving the common iliac artery. The vessels of the posterior division (the iliolumbar, lateral sacral, and superior gluteal) leave the internal iliac artery from its lateral surface to provide some of the blood supply to the pelvic wall and gluteal muscles. Trauma to these hidden vessels should be avoided during internal iliac artery ligation.
The anterior division has both parietal and visceral branches. The obturator, internal pudendal, and inferior gluteal vessels primarily supply muscles, while the uterine, superior vesical, vaginal (inferior vesical), and middle rectal vessels supply the pelvic organs. The internal iliac veins begin lateral and posterior to the arteries and have a much more plexiform arrangement.
Although the external iliac vein lies above the pelvic brim, the internal iliac vein crosses the linea terminalis. During obstructed labor, the internal iliac vein may be compressed for long periods of time, giving rise to the vulvar and pelvic soft tissue swelling seen in this situation. The legs, however, remain relatively uninvolved because of the external lilac vein's position above the true pelvis.
Ligation of the internal iliac artery has proven to be helpful in the management of postpartum hemorrhage. Burchell's arteriographic studies have demonstrated that physiologically active anastomoses were immediately patent following ligation of the internal iliac artery and connected the following arteries of the internal iliac system with systemic blood vessels4:
Internal iliac--Systemic
Iliolumbar  Lumbar
Lumbar
Lateral Sacral  Middle sacral
Middle sacral
Middle hemorrhoidal  Superior hemorrhoidal
Superior hemorrhoidal
(These were quite different than the anastomoses that had previously been hypothesized on purely anatomical grounds.) The lumbar arteries arise directly from the aorta; the middle sacral, again from the aorta; and the superior hemorrhoidal, from the inferior mesenteric.
Further detailed anatomy of the internal iliac artery and its surgical exposure are covered in the first volume of this series (see Volume 1, Chapter 73, Surgical Management of Intractable Pelvic Hemorrhage).
Nerves of the Pelvic Wall
There are instances in which paralysis and numbness of the lower extremity occur following difficult vaginal delivery, which in some cases may be explained by nerve compression in the pelvis.
As the lumbar and sacral nerves exit from the intervertebral foramina, they form the lumbar and sacral plexuses (see Fig. 5). The lumbar nerves and plexus lie deep within the psoas muscle on either side of the spine. The sacral plexus lies on the piriformis muscle, and its major branch, the sciatic nerve, leaves the pelvis through the lower part of the greater sciatic foramen. The sacral plexus supplies nerves to the muscles of the hip, pelvic diaphragm, and perineum, as well as to the lower leg (through the sciatic nerve). The femoral nerve from the lumbar plexus is primarily involved in supplying the muscles of the thigh.
In the interval between these two plexuses lies the lumbosacral trunk, which is composed of fibers from the fourth and fifth lumbar nerves. It curves in an exposed location over the brim of the pelvis at the sacroiliac articulation to join in the formation of the sacral plexus. In this position it lies directly on the bone of the pelvic inlet. Its fibers are destined to join in the formation of the sciatic nerve and eventually to form the common peroneal nerve and the tibial nerve.
After difficult labor and/or delivery, weakness and numbness in the distribution of the peroneal nerve develops in a manner suggesting compression of the lumbosacral trunk against the ala of the sacrum.5 In this way, dorsiflexion of the foot is impaired, along with sensation of the skin on the dorsum of the foot and lateral aspect of the lower leg. In some cases these signs may be secondary to herniation of an intervertebral disk.6
Posterior Abdominal Wall
After the viscera of the abdomen and pelvis have been removed from a cadaver the general shape and contour of the posterior abdominal wall may be appreciated. There is a prominent midline ridge formed by the lumbar spine. The psoas muscles produce ridges that extend downward from the spine on either side of the pelvic inlet.
The prominence of the lumbar spine forces the pregnant uterus to choose either the left or right gutter in which to lie. Because of the bulk of the sigmoid colon on the left side of the abdomen and pelvis, the uterus is found more frequently in the right gutter in a “dextrorotated” position.
The psoas ridges become important during external cephalic version. As the fetal head is moved downward toward the pelvis, some resistance is often encountered as attempts are made to push the head over the inlet and past the psoas ridge. Gentle upward pressure on the head through the flank can be used at this point to lift the head over this ridge and position it over the pelvic inlet.