This chapter should be cited as follows:
Francis S, Lau S, Glob Libr Women's Med
ISSN: 1756-2228; DOI 10.3843/GLOWM.413963
The Continuous Textbook of Women’s Medicine Series – Obstetrics Module
Volume 11
Labor and delivery
Volume Editor: Dr Edwin Chandraharan, Director Global Academy of Medical Education and Training, London, UK

Chapter
Immediate Neonatal Care
First published: February 2021
Updated: 2 January 2026
Study Assessment Option
By answering four multiple-choice questions (randomly selected) after studying this chapter, readers can qualify for Continuing Professional Development points plus a Study Completion Certificate from GLOWM.
See end of chapter for details.
INTRODUCTION
The immediate care of the newborn baby is an important first step in allowing term babies to transition safely between intrauterine and newborn life. The majority of babies will make this transition without requiring anything other than basic care. Unfortunately, some babies will be born having been compromised before or during the birthing process; these can sometimes be recognized through intrauterine monitoring, whilst others will be unexpected. Such babies require high-quality resuscitation at birth. The physiological uniqueness of a newborn baby requires a different approach to resuscitation compared with that for adults.
Babies can be born prematurely (before 37 completed weeks of gestation). Management of the preterm baby at birth differs from that of a compromised term neonate, as they are unlikely to require resuscitation and more likely to require stabilization to support transition to extrauterine life. Careful planning and high-quality care can reduce the mortality and morbidity associated with prematurity.
Whether it is the term newborn or the premature one, knowledge of the physiology underlying the transition from intrauterine to extrauterine life is essential to support babies effectively.
PHYSIOLOGY
The newborn baby must transition from having fluid-filled lungs to having lungs filled with air. The fetal circulation, aimed at circulating oxygenated blood from the placenta to the body, needs to switch to one that circulates de-oxygenated blood to the lungs, and pump oxygenated blood to the body.
The preparation for this transition occurs at the onset of labor. The release of endogenous corticosteroids and catecholamines in the fetus switch the fetal pneumocytes from secreting lung fluid to re-absorbing the fluid into the circulation.1 This process is more important than the mechanical forces that push fluid out of the lungs during labor. The initial breaths that the newborn takes further facilitates this. These breaths may generate a negative pressure of between −30 cmH2O and –70 cmH2O, which is significantly greater than that required for a normal breath.2 This higher pressure further drives fluid from the airways into the lymphatic circulation and overcomes the decreased compliance of the fluid-filled lung, thereby enabling the establishment of the functional residual volume. A newborn baby will usually take its first breaths within 1 minute to 90 seconds of obstruction to the umbilical blood flow. The combination of hypoxia resulting from cord obstruction, along with physical stimuli such as changes in temperature, act as a stimulant to start respiration.
The fetal circulation functions by blood flowing through the placenta, which oxygenates the blood, and returns via the right side of the heart to the body. A series of shunts ensures that the majority of the blood bypasses the lungs and goes to the body. At birth, there are three factors that result in drop of pulmonary vascular resistance: a rapid increase in systemic vascular resistance, expansion of the lung and oxygenation of the lung. This combination stops, or greatly reduces, the fetal shunts and establishes the extrauterine circulation. The ductus arteriosus, essential in fetal life to shunt oxygenated blood away from the lungs to the body, closes through muscular spasm stimulated by increased arterial oxygenation.
These mechanisms that enable the transition to extrauterine life can be disrupted under certain conditions. Elective cesarean section, without the onset of labor, prevents the processes that stop the secretion of lung fluid which are regulated through steroid and catecholamine release.3 This can produce lungs that are more fluid-filled than after vaginal birth, resulting in decreased lung compliance and a reduced ability to establish the functional residual capacity. Significant peripartum and intrapartum hypoxia can impede the reduction in pulmonary vascular resistance, leading to persistent pulmonary hypertension and hypoxia.
PATHOPHYSIOLOGY OF PERINATAL ASPHYXIA
The pathophysiology and response to hypoxia are different in a newborn compared to other age groups. Our understanding of how the fetus and newborn responds to hypoxia is gained through animal experiments conducted in the mid 20th century.4 In adults the predominant reason for acute collapse is usually cardiogenic. In newborn babies, it is almost always a respiratory etiology.
As described above, cord occlusion is one the most potent stimuli for the onset of respiration. If the fetus becomes hypoxic in utero, this stimulates breathing movements. However, in utero, these breathing movements will be ineffective in moving air into the lungs, therefore, the hypoxia will not improve. After some time, usually no more than 2–4 minutes, the persisting hypoxia results in cessation of these breathing movements as the respiratory center ceases to function. The resulting period of apnea is called primary apnea.5 During this time, the heart rate initially increases before fetal bradycardia ensues. Peripheral vasoconstriction ensures that blood pressure is better maintained than the heart rate.
During the period of primary apnea, the primitive spinal centers start to function, as the suppression of these centers is mediated by the respiratory centers in the brain.6 The resulting respiratory movements are irregular and deep, involving all the accessory respiratory muscles. These are best described as 'gasping breaths'. If these breaths also fail to aerate the lungs, the continued hypoxia leads to cessation of these gasping breaths. The ensuing period of apnea is called terminal apnea. It is only during terminal apnea that complete circulatory failure occurs. Until then, the circulation is maintained through the presence of glycogen reserves in the heart and a normal circulation will be re-established if the lungs are aerated. This entire process, terminating in the final apneic phase (terminal apnea), takes longer in the neonate than in other age groups. It can be up to 20 minutes before terminal apnea sets in and circulatory failure ensues.5 Until then, a newborn provided with a patent airway and air will be able to aerate its lungs and restart the circulation. The difficulty is often in understanding where a particular neonate exhibiting signs of compromise is along this process.
As discussed above, a newborn baby can be born in one of four basic states as detailed below.
State 1
The majority of newborn infants fall into this category. They have a heart rate greater than 100 beats per minute and either cry and establish effective spontaneous respiration immediately after birth, or do so shortly thereafter (within about 60–90 seconds). These infants do not require resuscitative interventions and need only routine postnatal care, as discussed later in this chapter.
State 2
A newborn who has experienced a period of hypoxia before birth (for example, due to umbilical cord occlusion) may enter primary apnea. At birth, it can be difficult to distinguish between primary apnea and the early phase of secondary (terminal) apnea. An infant in primary apnea will, after a period of stimulation and with a patent airway, typically resume gasping respirations, with a corresponding increase in heart rate, and may require no further resuscitative intervention.
State 3
A newborn who has entered secondary (terminal) apnea will make no spontaneous respiratory effort and is therefore unable to aerate the lungs. Effective lung aeration using face-mask intermittent positive pressure ventilation (IPPV) is required. In the early phase of secondary apnea, cardiac activity is usually still present, and effective ventilation can improve oxygen delivery to the myocardium, resulting in an increase in heart rate toward normal values. Following successful ventilation, the infant typically passes through a period of gasping respirations before establishing regular spontaneous breathing, and will require more prolonged respiratory support than the infant described in State 2.7
State 4
This infant has experienced prolonged hypoxia and has progressed beyond secondary (terminal) apnea. As a consequence, the heart rate is severely depressed (less than 60 beats per minute) and cardiac output is inadequate. Despite effective ventilation, the heart rate fails to improve, necessitating advanced resuscitative measures. Coordinated chest compressions are required to provide circulatory support while ventilation corrects hypoxia and improves myocardial oxygen delivery. Depending on the severity and duration of hypoxia, the infant may also require pharmacological support and prolonged resuscitation.
This chapter documents the steps in assessing and resuscitating babies born at the different stages. It also discusses special circumstances and the stabilization and immediate care of the premature newborn, all of which need a common degree of preparation and equipment. These should be present in any environment where babies are delivered.
All newborn infants, including those who do not require resuscitation, have basic care requirements in the delivery area. Although some fetuses can be identified antenatally or intrapartum as being compromised, allowing the need for resuscitation to be anticipated, many infants who require resuscitative intervention are unexpected. Consequently, all delivery areas should have facilities and equipment necessary to provide neonatal resuscitation.
ROOM PREPARATION
Temperature
Babies get cold quickly due to their increased surface area–to–body weight ratio. Heat loss occurs through a number of physical mechanisms (Table 1).2 Cold babies respond less well to resuscitation and temperature has been shown to be an independent risk factor for mortality and morbidity.8
1
Mechanisms of heat loss in newborn babies.
Mechanism of heat loss | Ways to prevent heat loss |
Evaporation: Babies are wet when delivered. As the liquid on babies’ skin evaporates, heat is lost | Dry the baby as soon as it has been fully delivered to remove the amniotic fluid from the skin. Premature babies less than 29 weeks' gestation or under 1 kg should not be dried, but instead placed in an occlusive wrap or plastic bag. This is described in more detail later in this chapter9 |
Conduction: Heat is lost through conduction when a warm object touches a cooler surface. As the newborn tends to be warmer than the surfaces on which it is placed, conductive heat loss can occur | All surfaces that come into contact with the baby should be warmed wherever possible. This includes towels used to dry the baby and the surface on which the baby is placed. Conductive heat loss can be easily minimized by placing the well-dried neonate directly onto the mother’s skin (skin-to-skin) and covering the baby and mother with a warmed towel or blanket. For preterm babies, the use of a warming mattress should be considered. |
Convection: Heat is lost to the surrounding air through convection. This is greater if the temperature differential between the baby and the surrounding environment is high. It is made worse by draughts that move the warmer air immediately around the baby and replace it with cooler air. | Ensure that all rooms used for deliveries are draught free. If fans or other devices are used to keep the mother cool, ensure these are switched off when the baby is delivered. Reduce movement of people near the baby by ensuring that the resuscitation surface is away from doorways or other movement corridors. The room should be kept as warm as possible, ideally above 25⁰C for preterm babies. |
Radiation: This is the loss of heat to cooler objects that are not in direct contact with the baby. This can occur if there are cooler objects close to the baby. | This can be reduced by ensuring the baby is covered as soon as it is dried. The use of an overhead radiant warmer will also assist with this as well as ensure that the surfaces near the baby are warm. |
Equipment
The equipment required for neonatal resuscitation and stabilization differs from that used for adults and older children. In addition to obvious differences in size, neonatal cardiorespiratory collapse is most commonly respiratory in origin, with secondary cardiovascular compromise; consequently, resuscitation equipment is primarily focused on airway management and ventilation. Ventilation circuits and devices therefore differ from those used in other age groups, while equipment commonly found on adult resuscitation trolleys, such as defibrillators, is rarely required in neonatal resuscitation.
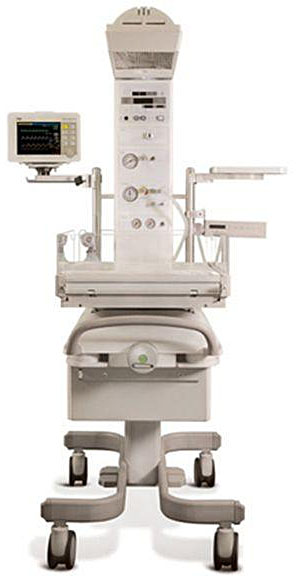
A warm, flat surface is essential for stabilization and resuscitation. This can be provided by any flat surface, ideally with an overhead heat source. A resuscitaire is an ideal piece of equipment to use, and should be available in all modern delivery rooms (Figure 1).
1
A modern resuscitaire has integrated heating, suction and equipment for positive pressure ventilation.
Equipment required for immediate basic neonatal care should be present in the storage baskets of the resuscitaire. These should include at a minimum:
- Back-up air and oxygen cylinders. Ideally, the resuscitaire should be plugged into wall medical gas supplies;
- Disposable gloves;
- Cord clamp;
- Scissors;
- Self inflating resuscitation bag, such as an Ambu Bag;
- Circuits that can be used on the pressure limiting ventilation device of the resuscitaire;
- Face masks of at least three different sizes (00, 0 and 1);
- Suction catheters, ideally a Yankauer suction catheter and flexible catheters of at least 12 Fr size;
- Stethoscope;
- Oropharyngeal (Guedel) airways;
- Laryngoscopes with straight blades, size 0 and 1;
- Plastic bag for preterm babies.
It is important that equipment for more advanced resuscitation, including drugs, is readily available. In a large delivery suite, it can be impractical to have the advanced equipment in every delivery room as the time required to check it daily can be prohibitive. It can be more practical to have a number of advanced neonatal resuscitation trolleys that can be checked and restocked following use. A suggested stock and equipment list is provided in Table 2.
2
Checklist for neonatal resuscitation trolley.
Drawer ALaryngoscopes × 2 each 00, 0, 1 ET Introducers × 1 box – Sterile Individually sealed (size 2.0) ET Tubes – Sizes 2.0, 2.5, 3.0, 3.5 (× 3 each size) ETT Clamps – Sizes 2.5, 3.0, 3.5 (× 3 each size) ET Tubes – 4.0, 4.5 (× 1 each) ETT Clamps – 4.0, 4.5 (× 1 each size) (Portex) Sterile Scissors × 2 Sterile Needle Holders × 2 Mersilk Sutures × 4 PEEP Valve for Tom Thumb × 2 End Tidal CO2 Detector (Neo-StatCO2) × 2 Elastoplast (2.5 cm) × 1 roll Transpore Tape × 1 roll
| Drawer DAdrenaline 1 : 10,000 × 3 Sodium Bicarbonate 4.2% × 3 10% Dextrose (500 ml bag) × 1 0.9% Sodium Chloride (500 ml bag) × 1 Water for Injection 10 ml × 5 Yellow Drug Labels × 2 Named Drugs Labels – Normal Saline Adrenaline Sodium Bicarbonate 4.2% 1 ml IV Syringes × 5 2 ml IV Syringes × 5 5 ml IV Syringes × 5 10 ml IV Syringes × 5 20 ml IV Syringes × 5 50 ml IV Syringes × 2 Needles – Green × 5 Blue × 5 Red Filter × 5 Sanicloths × 5 Blood Filter Set × 2 Blue Spike × 2 (for fluids)
| ||
IV Cannula – | Size 24Fg | – Neoflon × 5 | Clinical Waste Bags (× 1 roll – small) Plastic Trays – Blue, Yellow, Red × 1 each Opsite Spray × 1 Batteries AA × 4 Safety Goggles × 2
|
– Jelco × 5 | |||
Size 26Fg Size 20Fg | – Abocath × 2 – Abocath × 2 | ||
T-Piece Extension × 3 Transpore Tape × 1 roll Blue Bionectors × 2 Splints Small & Large × 1 each Sterile gauze × 2 Tape Measure × 1 IV Syringes – 10 ml, 20 ml × 2 each Intraosseous Needle × 1 | |||
ASSESSMENT OF THE BABY AT BIRTH
In order to provide a systematic approach to resuscitation, the following assessments should be made:
1) Respiration
It is important to differentiate effective spontaneous respirations from ineffective, irregular or absent breathing. Most newborns will establish regular breathing within the first 3 minutes, with a heart rate above 100 bpm, good color and normal tone. If respirations are absent, gasping or irregular, respiratory support will need to be provided until regular effective breathing is established.
2) Heart Rate
The heart rate is one of the most important physiological parameters in neonatal resuscitation. A good heart rate (defined as over 100 bpm) is reassuring. A heart rate that is increasing is the earliest sign of adequate aeration of the lungs and establishment of an effective circulation. The heart rate is best ascertained by direct auscultation at the cardiac apex in the initial stages. As soon as practically possible, a pulse oximeter should be applied to the right hand to measure preductal oxygen saturation. This will often provide a saturation and heart rate trace within a minute or two of application. However, in circumstances of very poor perfusion, it may fail to pick up and this will usually correlate with severe bradycardia or asystole on auscultation. Evidence shows that it can be practically possible to assess the heart rate using a three-lead ECG on bedside monitoring.10,11 Palpation of peripheral or central pulses is of limited use and should not be used during neonatal resuscitation.
3) Color
The central color of a baby can be useful to guage response to resuscitation. Peripheral duskiness is quite common in the first few postnatal hours. However, color alone cannot be used reliably to assess the effectiveness of oxygenation. A newborn who remains pale despite adequate resuscitative measures may have experienced significant blood loss, which should be suspected from the clinical history and examination.
4) Tone
A well newborn will have a flexed posture and will have active movements. A floppy baby with no active movements has usually undergone some degree of compromise. Improvements in tone usually lag behind improvements in the heart rate and respiration by many minutes, especially in the more compromised newborn.
5) Saturation
Preductal saturation measurements should be obtained as soon as possible and used to guide ventilation. It should be borne in mind that normal saturation levels in the first few postnatal minutes differ from those that are acceptable later.
Approximate target preductal SpO₂ levels in the first 10 minutes after birth are:
2 minutes 60%;
3 minutes 70%;
4 minutes 80%;
5 minutes 85%;
10 minutes 90%.5
A well baby, and one who has started respiratory movements due to late intrapartum hypoxia, is easy to identify. These babies will be breathing soon after delivery, have a good heart rate and tone, and will change color to a central pink color. They require no resuscitation, but care should still be taken to reduce heat loss by drying the baby as described above. These babies should be given to their mothers for skin-to-skin contact and to initiate the first breastfeed.
Babies in the later phases of terminal apnea are also relatively easy to identify. They will be born with no respiratory effort, and have a heart rate that is <60 bpm or be asystolic. The color will be pale and there will be a loss of the normal tone. Babies who are in primary apnea and those in the early phase of terminal apnea can be very difficult to differentiate.
There is a significant body of evidence that demonstrates advantages to both the baby and the mother from early skin-to-skin contact and breastfeeding. These include both short-term benefits for the baby such as better thermoregulation and reduction in stress hormones, and longer-term benefits to both the baby and the mother from higher rates of breastfeeding initiation and maintenance.
RESUSCITATION PROCESS
A standardized process to resuscitation will allow for babies to receive the resuscitation they require without over intervention.
It is important to note the time of birth for all deliveries. Most modern resuscitaires will have a digital timer that can be switched on easily. This should be done regardless of the condition of the baby at delivery. Irrespective of how unwell the baby looks, the first step is to dry the baby and ensure that the radiant heater is on and also that towels are available in which to wrap the baby to minimize heat loss. While doing this, more help should be summoned.
After the initial assessment and common actions described above, resuscitation should use the following structure:
- Airway;
- Breathing;
- Circulation;
- Drugs (rarely used).
Airway
Unlike in older children and adults, the airway of the newborn can be occluded both by extension and flexion. The head should therefore be placed in a neutral position with the face parallel to the surface on which the baby is lying. In a floppy baby, the loss of pharyngeal tone and a relatively large tongue can result in physical airway obstruction. Jaw thrust should be provided if the baby is floppy. Lose secretions do not usually cause any airway obstruction and are often best left alone. If there are copious amounts or if there are visible blood clots or thick mucus, this should be suctioned under direct vision using a Yankauer suction catheter. Over-vigorous and deep suction can cause vagal induced bradycardia. Suction should be set to about 90–100 mmHg.
Breathing
If the baby fails to establish spontaneous respiration following measures to open and maintain the airway, then breathing support should be provided. This should ideally be provided using a pressure-limiting device that provides 30 cmH2O in term babies for the initial breaths. For preterm babies, the pressure should be set lower, possibly no more than 25 cmH2O. If a pressure-limiting device is not available, a self-inflating bag with a 'blow-off' valve set at 30–40 cmH2O can be used. Bags with a volume under 500 ml should not be used as rapid depression can lead to significantly higher pressures than those recommended above.
The initial breaths provided need to artificially produce the functional residual capacity the baby would otherwise have established spontaneously. These should be provided over 2–3 seconds through a close-fitting soft mask that covers the nose and mouth. Five such breaths should be provided and evidence of chest rise during each breath should be observed. There may not be chest rise in the first 2 or 3 breaths, but inflation can be considered to be achieved if the chest moves during the final 2 or 3 breaths in conjunction with an increasing heart rate. If the heart rate has not increased and/or the chest is not seen to move, the head should be repositioned into neutral position, the mask on the face should be re-secured and inflation breaths provided again. The commonest reason for failed inflation breaths are poor position of the head. A small, rolled towel (not more than 2 cm thick) can be placed under the neck and shoulders to help position the head. It can also be easier to perform a jaw thrust if there are two people present: one to hold the mask firmly on the face with a bilateral jaw thrust, while the other provides the breaths through the breathing circuit or self-inflating bag.
If the heart rate has responded and chest movement is seen, then shorter ventilation breaths at a rate of 30 per minute should be provided until regular respiration is seen. These should be provided at a lower pressure than the inflation breaths. Usually, no more than 16–20 cmH2O is required. The best way to assess this is to provide adequate pressure to be able to just see chest rise with each breath.
There is strong evidence that room air is adequate and safest for neonatal resuscitation.3 The use of supplemental oxygen should be guided by the expected saturations as described above.
Circulation
If the heart rate remains slow (<60 bpm) or absent despite the provision of adequate ventilation breaths for 30 seconds, then chest compressions should be started. The purpose of chest compressions in the newborn is to move oxygenated blood from the lungs, back to the myocardium through the coronary arteries. There is therefore no purpose in performing chest compressions until the lungs are adequately aerated.
Chest compressions can be provided by compressing the sternum at a point approximately one finger width below the inter-nipple line and compressing the chest by one-third of its depth. The most effective and efficient way of doing this is to encircle the chest with both hands such that both thumbs are on the sternum at the compression position, then press down firmly and quickly, with three compressions provided for each breath. Re-assess the baby’s response to chest compressions after 30 seconds. Most babies will have responded with a rise in the heart rate after 1–2 cycles of chest compressions and ventilation breaths. If this has not occurred, drug administration may be considered. The outcomes for babies in whom drugs are required is more guarded, and experienced support should be sought by this point, if not done so already.
Drugs
Drugs used in neonatal resuscitation are ideally delivered centrally. The easiest and fastest central access can be obtained through the umbilical vein. Catheterization of this is relatively easily done using specific umbilical catheters. In the absence of these, nasogastric tubes of 5–6 Fr size can be used but medications will need to be drawn up using an IV syringe and transferred into an enteral syringe before administration. When a line is inserted (peripheral or central), blood should be taken at the very least for a blood gas analysis and blood glucose level. Many point-of-care blood gas analysers will provide a blood glucose and lactate level.
All resuscitation drugs, as with most neonatal dosing, are based on weight. Endotracheal tube size, length of insertion and umbilical line insertion depths are also based on weight. Although some newer resuscitaires have inbuilt weighing scales that provide an immediate weight, these have fairly low penetration in most services. Therefore weights are often guessed based on gestation and appearance. It is better to estimate in 500 g increments to ensure simplification of calculations.
Adrenaline
Adrenaline increases coronary artery perfusion enhancing oxygen delivery to the heart. In the presence of refractory bradycardia or asystole, 10 μg/kg (0.1 ml/kg 1 : 10,000) adrenaline may be given intravenously. If there is no response, further doses of 10–30 μg/kg (0.1–0.3 ml 1 : 10,000) may be given at 3–5-minutes. If there is no response to 2–3 doses of adrenaline despite good chest inflation and effective chest compressions, further doses are likely to be futile.
Bicarbonate
A baby who is in terminal apnea will have significant metabolic acidosis, which can impair cardiac function and the response to catecholamines. The use of bicarbonate has not been proven to be beneficial but is used in situations in which asystole has persisted, despite effective resuscitation. A dose of 1–2 mmol/kg (2–4 ml/kg of 4.2% solution) is typically used.
Glucose
Ideally the glucose level should be checked before administration of glucose. However, as asphyxiated newborns are at risk of hypoglycemia, the administration of glucose can be beneficial. A single dose of 2.5 ml/kg of 10% glucose is advisable. This should be followed up with maintenance glucose infusion as detailed below.
Volume expansion
Most asphyxiated newborns are euvolemic. The use of multiple fluid boluses, especially hyperchloremic ones, can worsen acidosis and postresuscitation recovery. A single bolus of 0.9% saline may be used but further fluid boluses should be avoided, unless there is evidence of blood loss from the history or appearance. Emergency O-negative blood at 10–20 ml/kg should be used in preference to any other type of fluid.
Other drugs
No other drugs have been shown to be useful in resuscitating the asphyxiated newborn. There are specific circumstances in which certain drugs may be beneficial. A baby who has severe respiratory depression secondary to the use of systemic opiates in the mother shortly before delivery may benefit from naloxone. However, naloxone has a shorter half-life than commonly used opiates and so the baby may suffer further respiratory depression as the effect of the naloxone wears off. A baby given naloxone should be observed and monitored in a suitable high-care environment until the effects of the opiates have worn off. Ultra-short acting opiates like remifentanil have an extremely short half-life and would not usually cause respiratory depression in the newborn.
Tracheal intubation
The critical step in newborn resuscitation is establishing an airway and aerating the lungs. This can be effectively achieved with intubation. Usually, this is the only measure that is required in the majority of term newborns. There will be some babies in whom an adequate airway cannot be established with mask ventilation. In the majority of cases, this will be due to poor airway and mask positioning and can be rectified with repositioning. Occasionally, the use of an oropharyngeal airway is helpful. Often the most effective method is the use of a two-person jaw thrust.
Where airway position has not established an adequate airway or resuscitation is required over a prolonged period, tracheal intubation can lead to more efficient CPR and also ensures more stable management of the airway. Most term newborns require a size 3.0–3.5 endotracheal tube. Larger newborns (over 4 kg) may benefit from a large tube such as a size 4.0. Endotracheal intubation in a newborn uses a very similar technique to that in adults and older children. The relatively large tongue, smaller mouth and anterior airway means a straight miller direct laryngoscopy blade is usually better suited to neonatal intubation. Successful placement should be confirmed using a colorimetric carbon dioxide detector, as well as through auscultation of the chest and visual confirmation of chest rise with breaths.
If intubation is not possible, due to either lack of expertise or a difficult airway, the use of a suitably sized laryngeal mask can also be used until more help is available.
SPECIAL CIRCUMSTANCES
Meconium
Thin, loose meconium is not uncommon, particularly in post-term infants, and is rarely associated with respiratory compromise. Thick particulate meconium is more often associated with fetal compromise, commonly in the context of hypoxia. Hypoxia may trigger fetal gasping or respiratory movements, which can result in in-utero aspiration of meconium. However, meconium aspiration is uncommon, and the majority of infants born through thick meconium-stained amniotic fluid do not develop meconium aspiration syndrome.
Due to the aspiration usually having occurred prior to delivery, there is no value in suctioning the oropharynx or nares when the head is on the perineum. Similarly with a vigorous neonate, there is no value in suctioning the trachea. Suctioning the trachea in a vigorous baby can lead to injury to the airway and/or oropharyngeal structures or vagal stimulation. If a baby is floppy, with no respiratory effort, then suctioning any visible meconium in the oropharynx and pharynx under direct vision may be useful. If this will take time due to lack of equipment or expertise, it should not delay positioning of the airway and respiratory support.
Prematurity
Premature babies differ from term babies in their needs at birth. Most term babies will not require any help other than being dried and kept warm. When they do require help, it is usually because of ante- or peripartum hypoxia as described above. Prematurity may occur as a consequence of catastrophic intrauterine events such as abruption of the placenta, other hemorrhagic events, placental failure or infection. Often though, the preterm baby is born due to factors that do not cause the baby to be acutely hypoxic or physiologically compromised in the way that a term baby needing resuscitation does. For this reason, what many premature babies need is not resuscitation, but support to adapt to extrauterine life.
When managing a preterm baby, there are three main focuses: maintaining a good temperature, recognizing respiratory support requirements including the need for surfactant and early feeding.
Thermoregulation for premature babies
Premature infants are prone to hypothermia because of minimal subcutaneous fat and immature heat-generating mechanisms.12 Hypothermia can increase mortality and also cause significant morbidity, including worsening pulmonary insufficiency and intraventricular hemorrhage.13 For this reason, premature and smaller babies (under 1.5 kg) need specific measures to maintain body temperature.
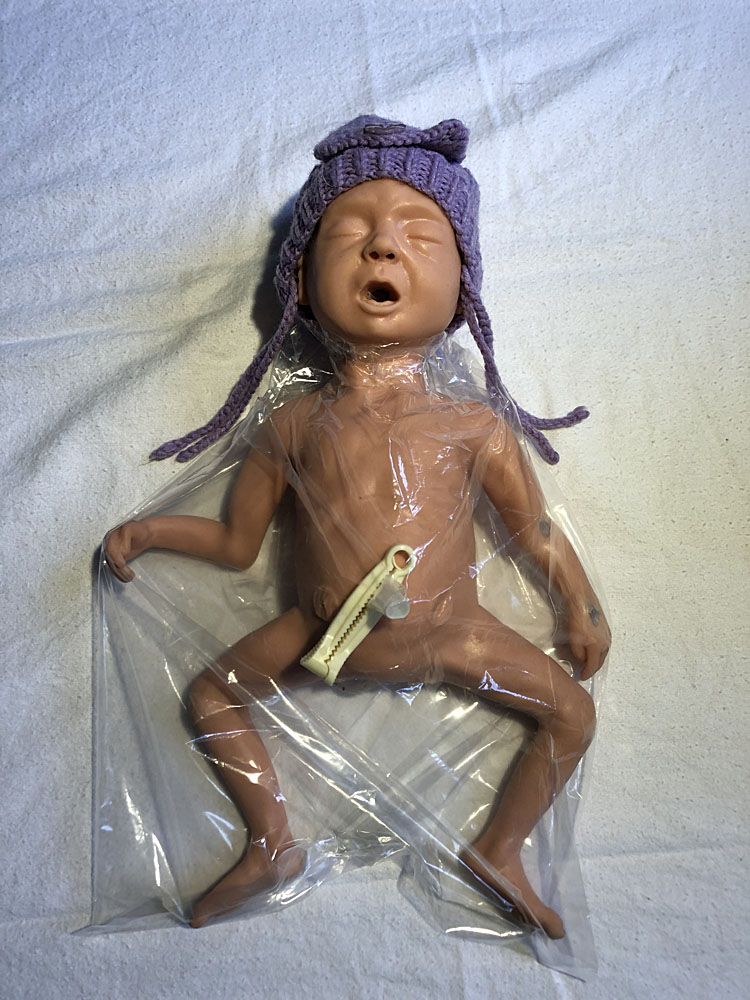
Babies under 1 kg or under 29 weeks should be covered in an occlusive plastic covering to reduce heat loss (Figure 2).14 This can be achieved through the use of occlusive plastic wraps or by placing into a plastic bag, such as a large plastic sandwich bag. These do not need to be sterile, but should be stored in a clean, dust free area. Babies need to be placed, feet first, in the occlusive cover as soon as they are born, without being dried. The plastic cover should be brought up to the neck and any excess opening should be lightly closed using tape. The head should be dried and covered with a hat, leaving the face as the only part of the baby that is exposed. The plastic-bag covered baby should not be covered with blankets. They should be placed under the overhead heat source, which should initially be set to the highest heat output. This allows the water on the baby to create a warm, humid environment that reduces heat loss. Babies under 800 g, and/or under 27 weeks may require additional warmth through the use of thermal mattresses such as the Transwarmer mattress. Premature babies can also get overheated easily if the above measures are applied rigorously. For this reason, continuous temperature monitoring during stabilization or resuscitation is recommended.
2
Model of preterm baby placed, feet first, into plastic bag to reduce heat loss.
Respiratory support for premature babies
The amount of respiratory support required is determined by the gestation of the neonate. The majority of preterm babies will only require positive end expiratory pressure between 4 and 5 cmH2O. Preterm lungs are much more susceptible to damage from overdistension, therefore if inflation breaths are required, the pressure used should be reduced to 25 cmH2O and increased only if there is difficulty achieving chest movement or improvement of heart rate. The preterm lung is compliant, so obvious chest movement suggests excessive tidal volumes. More detail is provided below. Cells in the alveolar epithelium naturally secrete surfactant the effect of which is to reduce alveolar surface tension which prevents collapse of the alveolus in expiration. There is a natural surge in surfactant production between 30 and 34 weeks' gestation as well as at birth.5 Preterm babies who are less than 32 weeks are more likely to be surfactant deficient and may require administration of artificial surfactant to prevent prolonged respiratory distress and increasing oxygen requirement. Production of surfactant is greatly inhibited by hypothermia and acidosis, highlighting the importance of achieving normothermia in preterm neonates.
Premature babies are more susceptible to the toxic effects of hyperoxia with evidence of adverse long-term effects. Respiratory resuscitation should always be undertaken in air and increased only if there is significant resuscitation need or inability to achieve the recommended saturation thresholds provided above.5
Continuous pulse oximetry should be used during the stabilization of a preterm baby as this allows for monitoring of heart rate and saturation and determines when, if any, additional respiratory support is required.
Other factors
Preterm babies lack glycogen and fat stores, have increased metabolic demand and reduced ability to mount a counter regulatory response to low blood glucose levels. They are, therefore, are at increased risk of hypoglycemia within the first few hours of postnatal life.15 Preterm neonates near 34 weeks’ gestation can be managed on the postnatal ward with the mother, but with increased vigilance to poor feeding and hypoglycemia. Three-hourly feeding and monitoring of blood glucose level is paramount with a low threshold to escalate support, if concerned. There is an increased risk of jaundice due to liver immaturity and inability to get rid of bilirubin, so close monitoring for jaundice is also important.
Babies born close to term can often be supported in the same manner as non-compromised term babies. Those born earlier should be managed with additional measures:
Management at 34–36 weeks' gestation
These babies can often be managed in the same way as a term baby. Provided that they are well grown and have had no significant antenatal problems, these babies would be able to adapt to extrauterine life in a similar way to a term baby. They should be able to stay with their mothers after delivery, albeit with additional monitoring and care for temperature regulation and feeding.
Thermoregulation
Babies at this gestation are more prone to hypothermia than term infants; therefore, extra care should be taken during procedures that may cause heat loss, such as weighing and physical examination. Immediate skin-to-skin contact with the mother is appropriate for clinically stable infants, together with maintaining a warm delivery and ward environment, avoiding draughts and ensuring careful temperature monitoring.
Respiratory support
Often, babies born at this gestation do not require additional respiratory support. If they do, care should be taken to reduce the inflation pressures to around 25 cmH2O. If there is some degree of respiratory distress, providing 5–6 cmH2O of positive end expiratory pressure for the spontaneously breathing baby is often beneficial and may be the only support required. If additional support is needed, it is provided in a similar way to a term baby.
Management at 32–34 weeks' gestation
Babies born at this gestation will need additional support after birth and admission for neonatal care.
Thermoregulation
These newborns are very likely to get hypothermia without active measures to reduce heat loss. This is particularly true if the cause for premature birth is related to poor intrauterine growth.
Respiratory
Most babies will only require airway positioning to maintain patency and a degree of positive end expiratory pressure to establish and maintain the functional residual capacity of the lung.
Management at 28–32 weeks' gestation
At these gestations, babies have significant immaturity and need to be supported by professionals experienced in providing neonatal care.
Thermoregulation
These babies need significant active measures to avoid hypothermia. This will include occlusive wrapping, increased room temperatures and frequent temperature monitoring.
Respiratory support
Almost all babies will need positive end expiratory pressure and some will need surfactant in the delivery room. The more immature the gestation, the more likely they are to need invasive respiratory support, including in some cases intubation and mechanical ventilation.
Management at under 28 weeks' gestation
These are the most vulnerable and fragile neonates. Every effort should be made for these babies to be delivered in centers with expertise in caring for babies at this gestation.
Thermoregulation
Occlusive wrapping and a warm room are essential in managing babies at these gestations. Many will also need additional heat sources such as heated mattresses and continuous temperature monitoring.
Respiratory support
While many babies at the higher end of this gestational age range may only need positive end expiratory pressure, many are likely to need surfactant administration along with non-invasive respiratory support. At younger gestations, the need for invasive ventilation support is greater.
SUMMARY
In summary, all babies, regardless of gestation, require support at birth to transition from intrauterine to extrauterine life. Ensuring that adequate equipment is available and using a standardized approach to delivery-room management facilitates a smooth transition. Maintaining normothermia, providing respiratory support tailored to the individual infant, and recognizing the need for early escalation of care in high-risk deliveries are the mainstays of management.
PRACTICE RECOMMENDATIONS
- Newborn babies undergo specific physiological changes at birth that necessitate a different approach to resuscitation compared to that in older children and adults.
- The process of labor initiates a cascade of hormonal changes in the fetus that reduces the amount of lung fluid. Further stimulation of the baby at birth, and clamping of the umbilical cord, results in a drop in pulmonary vascular resistance and the establishment of the extrauterine circulation.
- Most newborn babies do not require resuscitation at birth. However, attention needs to be paid to maintaining the baby’s body temperature and immediate skin-to-skin contact with the mother and breastfeeding.
- Hypoxia in utero leads to a predictable pattern of physiological responses. Knowledge of these is essential in undertaking resuscitation.
- The equipment required for advanced resuscitation of a newborn is not complex, or expensive. All delivery suites need to have this equipment available to facilitate resuscitation.
- Preterm babies often do not require resuscitation, but rather support to adapt to extrauterine life. However, the smallest and most immature babies will need considerable support and should be delivered in centers with expertise in providing this.
CONFLICTS OF INTEREST
The author(s) of this chapter declare that they have no interests that conflict with the contents of the chapter.
Feedback
Publishers’ note: We are constantly trying to update and enhance chapters in this Series. So if you have any constructive comments about this chapter please provide them to us by selecting the "Your Feedback" link in the left-hand column.
REFERENCES
te Pas A, Davis P, Hooper S, et al. From Liquid to Air: Breathing after Birth. The Journal of Pediatrics 2008;152(5):607–11. | |
Wyllie J, Ainsworth S, Tinnion R, et al. Newborn life support, 4th edn. Resuscitation Council (UK), 2016. | |
Ramachandrappa A, Jain L. Elective Cesarean Section: Its Impact on Neonatal Respiratory Outcome. Clinics in Perinatology 2008;35(2):373–93. | |
Dawes GS. Foetal and Neonatal Physiology. Chicago: Year Book Medical Publishers (1968). | |
Katheria A, Arnell K, Brown M, et al. A pilot randomized controlled trial of EKG for neonatal resuscitation. PLOS ONE 2017;12(11):e0187730. | |
Davis P, Tan A, O'Donnell C, et al. Resuscitation of newborn infants with 100% oxygen or air: a systematic review and meta-analysis. The Lancet 2004;364(9442):1329–33. | |
Johanson R, Spencer S, Rolfe P, et al. Effect of post-delivery care on neonatal body temperature. Acta Paediatrica 1992;81(11):859–63. | |
Freeman B, Berger J. Anesthesiology Core Review. McGraw Hill, 2016. | |
Koos B, Rajaee A. Fetal Breathing Movements and Changes at Birth. Advances in Fetal and Neonatal Physiology 2014;89–101. | |
Moore E, Bergman N, Anderson G, et al. Early skin-to-skin contact for mothers and their healthy newborn infants. Cochrane Database of Systematic Reviews 2016. | |
Mizumoto H, Tomotaki S, Shibata H, et al. Electrocardiogram shows reliable heart rates much earlier than pulse oximetry during neonatal resuscitation. PediatrInt 2012;54:205–7 | |
Knobel R, Holditch‐Davis D. Thermoregulation and Heat Loss Prevention After Birth and During Neonatal Intensive‐Care Unit Stabilization of Extremely Low‐Birthweight Infants. Journal of Obstetric, Gynecologic & Neonatal Nursing 2007;36(3):280–7. | |
Lyu Y, Shah PS, Ye XY, et al. Association Between Admission Temperature and Mortality and Major Morbidity in Preterm Infants Born at Fewer Than 33 Weeks’ Gestation. JAMA Pediatr 2015;169(4):e150277. doi:10.1001/jamapediatrics.2015.0277 | |
Vohra S, Frent G, Campbell V, et al. Effect of polyethylene occlusive skin wrapping on heat loss in very low birth weight infants at delivery: A randomized trial. The Journal of Pediatrics 1999;134(5):547–51. |
Online Study Assessment Option
All readers who are qualified doctors or allied medical professionals can automatically receive 2 Continuing Professional Development points plus a Study Completion Certificate from GLOWM for successfully answering four multiple-choice questions (randomly selected) based on the study of this chapter. Medical students can receive the Study Completion Certificate only.
(To find out more about the Continuing Professional Development awards program CLICK HERE)
