This chapter should be cited as follows:
Parikh S, Hanna H, et al., Glob Libr Women's Med
ISSN: 1756-2228; DOI 10.3843/GLOWM.420053
The Continuous Textbook of Women’s Medicine Series – Gynecology Module
Volume 8
Gynecological endoscopy
Volume Editors:
Professor Alberto Mattei, Director Maternal and Child Department, USL Toscana Centro, Florence, Italy
Dr Federica Perelli, Obstetrics and Gynecology Unit, Ospedale Santa Maria Annunziata, USL Toscana Centro, Florence, Italy

Chapter
Laparoscopic Entry Techniques
First published: September 2023
Study Assessment Option
By answering four multiple-choice questions (randomly selected) after studying this chapter, readers can qualify for Continuing Professional Development points plus a Study Completion Certificate from GLOWM.
See end of chapter for details.
INTRODUCTION
Initial abdominal entry is essential for the establishment of pneumoperitoneum and performance of laparoscopic procedures. Although many complications related to laparoscopy occur during initial trocar entry, abdominal entry can be accomplished safely by various methods. Currently, there is no consensus regarding the optimal technique to avoid complications. The most serious complications associated with laparoscopic entry include major vascular, bowel and visceral injuries. However, these complications are typically rare, and the literature estimates about 50% of inadvertent laparoscopic injuries to vital organs and vessels occur at the time of entry. The reported incidence of bowel perforation ranges from 0–0.5%, while major vascular injury occurs in approximately 0.01–1.0% of cases.1,2
Entry location depends on the patient’s body habitus, surgical history, surgeon preference, experience with entry techniques and anticipated intra-abdominal pathology. In this chapter, we discuss the most common methods of abdominal entry, including the Veress needle, the open Hasson technique and direct trocar entry.
ENTRY CONSIDERATIONS
Access points
The creation of pneumoperitoneum is critical in performing laparoscopic surgery, and proper technique is mandatory to establish safe laparoscopic entry. As mentioned above, initial trocar entry site is based on surgeon’s preference and comfort, patient’s surgical history and patient anatomy. Common entry sites include the umbilicus, left upper quadrant (Palmer’s point), right upper quadrant, mid-abdomen (Lee–Huang point), vaginal or uterine fundus, and Jain’s point. (Figure 1).
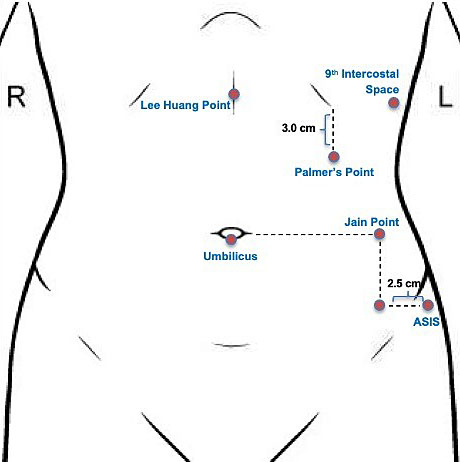
1
Diagram of entry points for initial laparoscopic entry. L, left; R, right.
Initial laparoscopic entry should be performed with the patient lying flat in the supine position. Trendelenburg positioning should be avoided prior to entry, as head-down tilt may decrease the distance between the anterior abdominal wall and major retroperitoneal vessels, thereby increasing the risk of vascular injury during access.
At our institution, we prefer the left upper quadrant entry given our high rate of complex surgical patients. Palmer’s point was described by the French gynecologist, Raoul Palmer, in the early part of the 20th century.3,4,5,6 This technique is generally considered a reliable entry point in patients with previous midline laparotomy, presence of abdominal mesh or umbilical hernia repair, pelvic and abdominal adhesions, and extremes in body mass index (BMI). Prior review of women undergoing laparoscopy after laparotomy shows that more than 50% of women with a midline vertical incision have intra-abdominal adhesions between the anterior abdominal wall and omentum or bowel, and greater than 30% of these women will have severe umbilical adhesions with potential for bowel injury.5,7,8 Patient body habitus affects abdominal entry. In obese women, increased subcutaneous fat can distort the planes around the umbilicus and may cause the umbilicus to shift caudally, making umbilical entry less ideal due to the increased risk of major vascular injury. In contrast, in extremely thin patients, the aortic bifurcation may lie at or just below (1–2 cm) the level of the umbilicus, emphasizing the need for careful entry technique. Additionally, gastric decompression is recommended when using this entry point in the left upper quadrant and may be achieved by placing an oral gastric tube to suction. Relative contraindications to left upper quadrant entry include inability to decompress the stomach, history of splenectomy or gastric surgery, and hepatomegaly.9
ENTRY TECHNIQUES
Closed (Veress)
The term pneumoperitoneum was first popularized by Otto Goetze in the early 20th century. In 1938, Hungarian pulmonologist János Veres introduced an insufflation needle, later adapted for laparoscopic entry.10 The Veress needle continues to be widely used as a safe and effective method for creating pneumoperitoneum.
The Veress is a spring-loaded needle that is available as a reusable or disposable option (Figure 2). The outer sheath is sharp, while the inner sheath contains a dull tip with a spring mechanism that retracts when resistance is encountered. When the Veress needle traverses the abdominal layers and enters the peritoneal cavity, resistance decreases, and the dull tip is exposed to protect intra-abdominal structures from the sharp tip. It is recommended to check the mechanics of the Veress needle prior to insertion, even with the disposable instruments.4
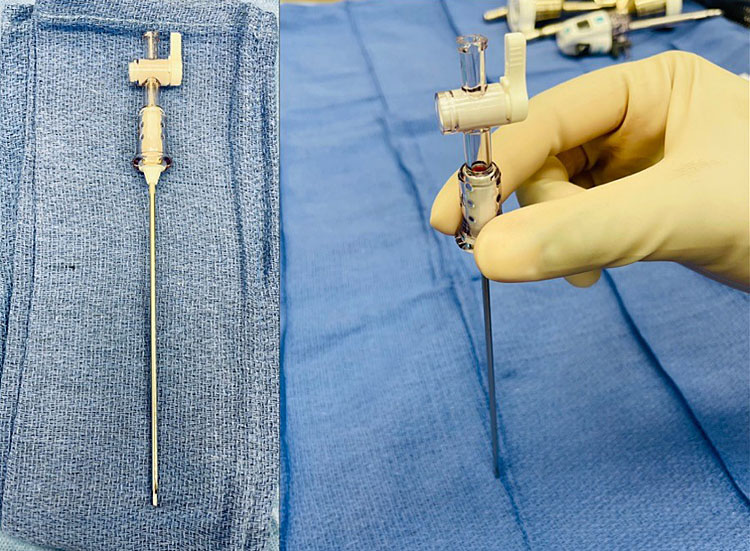
2
Disposable Veress needle.
Entry point for the Veress needle may utilize any of the abovementioned locations, including the umbilicus, left upper quadrant, ninth intercostal space, transuterine, or Jain’s point. Depending on the patient's individual characteristics, such as surgical history and BMI, one entry location may be more suitable than another.4
Left upper quadrant entry
As previously stated, we prefer Palmer’s point at our institution, located in the left midclavicular line 3 cm below the costal margin. After confirming orogastric or nasogastric tube placement to decompress the stomach, a skin incision is made at the desired abdominal entry site and the Veress needle is inserted at a 90° angle to the abdominal wall. In the left upper quadrant, generally three 'pops' are felt as the needle traverses the aponeuroses of the internal and external oblique muscles, transversalis fascia and peritoneum. Gas tubing is attached to the Veress needle and confirmation of intra-abdominal entry with an opening pressure of less than 10 mmHg confirms correct placement. Once the abdomen is insufflated to the predetermined abdominal pressure, an initial 5-mm trocar may be placed either directly or under direct optical guidance. This approach is particularly valuable in morbidly obese patients and is our preferred method in patients with prior abdominal surgery (Figure 3, Video 1).
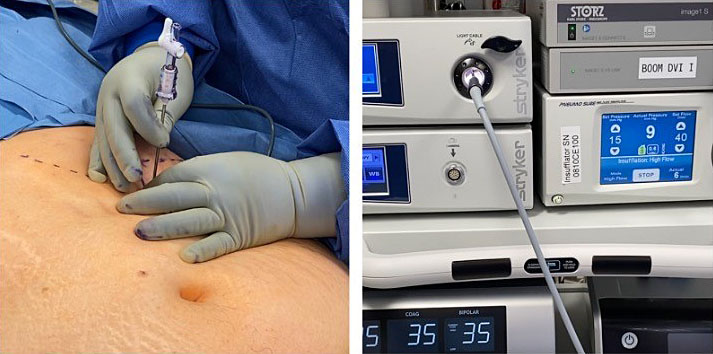
3
Veress needle entry technique in a morbidly obese patient with a history of two prior cesarean sections. Peritoneal entry was confirmed by a decrease in resistance and an intra-abdominal pressure <10 mmHg.
1
Veress technique.
Safety tests that can be used to confirm Veress needle placement include irrigation or aspiration test, hanging drop test, and gas insufflation. Observational studies suggest that an initial intra-abdominal pressure <10 mmHg is the most reliable indicator of correct needle placement.9 At our institution, we confirm Veress needle entry using this opening pressure. In agreement with the Middlesborough consensus document,11 we temporarily insufflate with carbon dioxide to an intra-abdominal pressure of 25 mmHg to establish sufficient pneumoperitoneum. At this pressure, the distance between the abdominal wall and underlying structures is about 10 cm, which minimizes the risk of vascular and visceral injury, even when additional force is required for trocar placement in challenging cases.7
Numerous publications have reported that the Veress technique is a popular entry method among gynecologists around the world.1 A 2019 Cochrane review of laparoscopic entry techniques reported that there is insufficient and low-quality evidence to show any differences in vascular, visceral or solid organ injury with direct versus Veress or open entry technique.1 However, following the Cochrane review, Raimondo et al. reviewed 25 randomized controlled studies and reported preference for the direct trocar method over the Veress needle or open entry techniques owing to a lower risk of omental injury, failed entry, extraperitoneal insufflation and infection at the trocar site.2 Common reasons for Veress entry failure include underestimation of preperitoneal fat, tracking, insufflation of preperitoneal space, unexpected adhesions, and advancing the needle too deep under the omentum. The rate of complications increases with each subsequent attempt. It is recommended that no more than three attempts should be made with any of the entry methods and an alternative entry option should be utilized in these cases.5
Direct
Direct trocar entry is a safe alternative method for initial abdominal entry in laparoscopic surgery. While the Veress needle requires three blind steps in entry (insertion, insufflation, trocar placement), direct entry is initiated with only one blind step i.e. trocar insertion.12 To perform this technique, a small infraumbilical incision is made to the diameter of desired trocar/cannula system. The abdominal wall is lifted with the non-dominant hand, and the trocar is carefully inserted into the abdominal cavity through this incision with a twisting motion, aiming towards the pelvis until there is a loss of resistance. The angle in thin and normal-sized patients should be 45° with respect to the patient’s abdominal wall at the level of the umbilicus, while, in obese patients, an angle of 90° to the abdominal wall is used during entry. To confirm intra-abdominal entry, insufflation tubing should be attached to the trocar and a laparoscope introduced.
Direct visual entry
The direct optical access technique can be performed either after pneumoperitoneum is established or without prior insufflation. This technique requires an optical trocar. When performed without prior pneumoperitoneum, a 5–10-mm skin incision is made at the intended primary port site. As with direct trocar entry, the abdominal wall is gently lifted with the non-dominant hand, and an optical trocar with a 5–10-mm laparoscope is carefully advanced through the abdominal layers using gentle rotation until the peritoneal cavity is entered and underlying structures are visualized. The trocar sheath is removed, and the laparoscope is reinserted to confirm peritoneal entry. The same technique can be applied after pneumoperitoneum is established with the Veress needle. Entry is typically confirmed by visualization of a dark circular space at the tip of the trocar, often accompanied by a rush of gas from the peritoneal cavity, indicating that the appropriate depth has been reached.9,4
As with all other techniques, it is important to assess the entry point for any vascular or visceral injury. The advantage of using direct trocar entry is that it is faster than the Veress needle or open techniques. There is also less gas leak around the primary port compared to open Hasson approach and reduced risk of inadvertent injury with optical entry compared to closed technique.13 The 2019 Cochrane review on laparoscopic entry techniques concluded that there is moderate-quality evidence to show that there is a reduction in failed abdominal entry by direct entry compared to Veress (OR 0.24, 95% CI 0.17–0.34).1 However, this approach does require knowledge of the abdominal wall layers and ability to distinguish between preperitoneal and omental fat.5
Open (Hasson)
The open entry technique was first developed and described by Dr Harrith Hasson in 1971.14 This technique has become widely accepted and is constantly being modified to improve its practice. Open entry is generally preferred in patients with a history of previous surgery and intra-abdominal adhesions as well as in cases in which other entry methods have failed.7 This technique can be used in any quadrant of the abdomen, but it is most used at the central umbilical site.
Ports used for open entry differ from standard laparoscopic ports, typically being blunt and lacking sharp or bladed trocars. A well-known example is the Hasson port (Figure 4), which consists of a blunt-tipped trocar with a sleeve system that allows the abdominal fascia to be sutured to the port to stabilize it and maintain pneumoperitoneum. Some open-entry ports also use a balloon mechanism for stabilization and pneumoperitoneum maintenance.
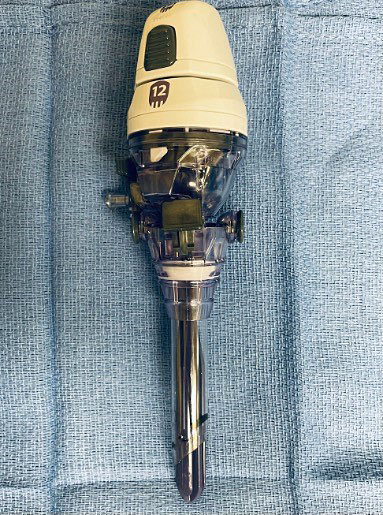
4
Hasson trocar for open technique for laparoscopic entry.
The following describes the technical aspects of the open entry technique (Video 2):
2
Open Hasson technique.
- Skin incision is made at desired entry point;
- Subcutaneous fat is bluntly dissected using a S retractor;
- Once fascia is identified, Kocher clamps are used to grasp the fascia or umbilical stalk if entry is through umbilicus;
- Fascia is incised and tagged with stay sutures which will be used to secure the port;
- The preperitoneal fat is bluntly dissected and the peritoneum is tented up using a clamp. The peritoneum is sharply dissected to enter the abdominal cavity;
- The underside of the abdominal wall should be swept with index finger to clear omentum or bowels and confirm the absence of adhesions;
- A blunt-ended or Hasson trocar is placed through the incision into the abdominal cavity and secured with stay sutures;
- Insufflation tubing is attached to the port;
- At the end of the procedure, stay sutures are cut or detached to remove the port.
The greatest advantage of the open entry technique is that it allows for precise, controlled entry into the intra-abdominal cavity. However, the open Hasson technique can be challenging in obese patients as it is difficult to gain abdominal entry through a small, 3-cm skin incision due to depth of subcutaneous fat. As previously mentioned, initial trocar insertion is perhaps the most important and dangerous step in minimally invasive surgery. Champault et al. showed that 83% of vascular injuries, 75% of bowel injuries and 50% of local hemorrhage injuries during laparoscopy were caused during primary trocar insertion.15
vNOTES
Vaginal natural orifice transluminal endoscopic surgery (vNOTES) is an emerging minimally invasive surgical approach in which the vagina is used as a 'natural orifice' or entry point into the peritoneal cavity for single-port laparoscopy.16 The American College of Obstetricians and Gynecologists recommends the vaginal route as the gold standard approach to hysterectomy as there is evidence of fewer complications, decreased operative time and cost, and shorter hospital stay in comparison to laparoscopic and abdominal hysterectomies.17 vNOTES can be used to broaden the feasibility of vaginal hysterectomy or other gynecologic procedures in patients with narrow vaginal opening, high BMI, prior abdominal surgery, history of cesarean section, or large uterus18 and can offer better visualization of the pelvic anatomy. A randomized controlled trial of 70 women comparing traditional laparoscopic hysterectomy to vNOTES hysterectomy showed non-inferiority in successfully completing the surgery without conversion.19 However, subgroup meta-analysis comparing vNOTES to multi-port traditional laparoscopy could not be undertaken given the paucity of the studies meeting eligibility.20 Other advantages of this approach include shorter operative time, reduced length of hospital stay, and less postoperative pain compared with traditional laparoscopy. However, this technique requires an experienced surgeon, as technical challenges such as limited triangulation and instrument crowding may be encountered with this approach. Thus, further larger randomized controlled trials are needed.
CONCLUSION
The entry technique is the most important step in performing laparoscopy. The most common entry techniques include Veress, open Hasson, and direct entry as described in this chapter. Complications related to laparoscopy are relatively low, and most adverse events are associated initial trocar entry. A large Cochrane review of laparoscopic techniques does not provide sufficient evidence to support one method over another or differences in visceral or vascular complications.1 Thus, choice of entry technique and initial trocar placement is dependent on surgeon experience and patient characteristics and pathology.
PRACTICE RECOMMENDATIONS
- When performing laparoscopy, there is no consensus on the optimal method for initial abdominal entry. The choice of technique should be determined by the surgeon’s experience and the patient’s individual characteristics, including prior surgical history.
- Left upper quadrant entry (Palmer’s technique) should be considered in patients with previous abdominal surgery, adhesive disease or extremes in body mass index.
- Initial entry is performed with the patient supine, avoiding head-down (Trendelenburg) tilt prior to peritoneal access, as such positioning may decrease the distance to major vessels and increase the risk of injury.
- Temporarily insufflating the abdomen to 25 mmHg prior to initial trocar insertion can increase the distance between the abdominal wall and underlying structures, which may reduce the risk of vascular and visceral injury.
- Direct entry may be preferable to the Veress needle in cases of failed peritoneal access.
CONFLICTS OF INTEREST
The author(s) of this chapter declare that they have no interests that conflict with the contents of the chapter.
Feedback
Publishers’ note: We are constantly trying to update and enhance chapters in this Series. So if you have any constructive comments about this chapter please provide them to us by selecting the "Your Feedback" link in the left-hand column.
REFERENCES
Ahmad G, Baker J, Finnerty J, et al. Laparoscopic entry techniques. Cochrane Database Syst Rev 2019;1(1):CD006583. doi: 10.1002/14651858.CD006583.pub5. PMID: 30657163. | |
Raimondo D, Raffone A, Travaglino A, et al. Laparoscopic entry techniques: Which should you prefer? Int J Gynaecol Obstet 2022. doi: 10.1002/ijgo.14412. PMID: 35980870. | |
Palmer R. Instrumentation et technique de la coelioscopie gynécologique [Instrumentation and technique of gynecological laparoscopy]. Gynecol Obstet (Paris). 1947;46(4):420-31. French. PMID: 18917806. | |
Lang T, Pasic RP. Creation of Pneumoperitoneum and Trocar Insertion Techniques. Practical Manual of Minimally Invasive Gynecologic and Robotic Surgery: A Clinical Cook Book 2018;3:43–54. | |
Recknagel JD, Goodman LR. Clinical Perspective Concerning Abdominal Entry Techniques. J Minim Invasive Gynecol 2021;28(3):467–74. doi:10.1016/j.jmig.2020.07.010. PMID: 32712324. | |
Jain N, Sareen S, Kanawa S, et al. Jain point: A new safe portal for laparoscopic entry in previous surgery cases. J Hum Reprod Sci 2016;9(1):9–17. doi: 10.4103/0974-1208.178637. PMID: 27110072. | |
Ahmad G, Duffy JM, Watson AJ. Laparoscopic entry techniques and complications. Int J Gynaecol Obstet 2008;99(1):52–5. doi: 10.1016/j.ijgo.2007.04.042. PMID: 17628561. | |
Audebart A, Gomel V. Role of microlaparoscopy in the diagnosis of peritoneal and visceral adhesions and in the prevention of bowel injury associated with blind trocar insertion. Fertility and Sterility 2000;3(3):631–5. | |
Thepsuwan J, Huang K-G, Wilamarta M, et al. Principles of safe abdominal entry in laparoscopic gynecologic surgery. Gynecology and Minimally Invasive Therapy 2013;2(4):105–7. https://doi.org/10.1016/j.gmit.2013.07.003. | |
Alkatout I, Mechler U, Mettler L, et al. The Development of Laparoscopy-A Historical Overview. Front Surg 2021;8:799442. doi: 10.3389/fsurg.2021.799442. PMID: 34977146. | |
A consensus document concerning laparoscopic entry techniques: Middlesbrough, March 19–20 1999. Gynaecological Endoscopy 1999. 8: 403-406. https://doi.org/10.1046/j.1365-2508.1999.00309.x | |
Theodoropoulou K, Lethaby DR, Bradpiece HA, et al. Direct trocar insertion technique: an alternative for creation of pneumoperitoneum. JSL 2008;12(2):156–8. PMID: 18435888. | |
Aust TR, Kayani SI, Rowlands DJ. Direct optical entry through Palmer’s point: a new technique for those at risk of entry-related trauma at laparoscopy. Gynecol Surg 2010:315–7. https://doi.org/10.1007/s10397-009-0500-8. | |
Hasson HM. A modified instrument and method for laparoscopy. Am J Obstet Gynecol 1971;110(6):886–7. | |
Champault G, Cazacu F, Taffinder N. Serious trocar accidents in laparoscopic surgery: a French survey of 103,852 operations. Surg Laparosc Endosc 1996;6(5):367–70. | |
Thigpen B, Sun J, Guan X. Robotic transvaiginal NOTES: A step-by-step approach to surgical technique. Intelligent Surgery 2022;4:1–8. https://doi.org/10.1016/j.isurg.2022.06.002. | |
American College of Obstetricians and Gynecologists. Choosing the Route of Hysterectomy for Benign Disease. Committee Opinion No. 701. Obstet Gynecol. 2017. | |
Nulens K, Bosteels J, De Rop C, et al. vNOTES HYsterectomy for Large Uteri: A retrospective cohort study of 114 patients. J Minim Invasive Gynecol 2020;28(7):1351–6. https://doi.org/10.1016/j.jmig.2020.10.003. | |
Baekelandt JF, De Mulder PA, Le Roy I, Mathieu C, Laenen A, Enzlin P, Weyers S, Mol B, Bosteels J. Hysterectomy by transvaginal natural orifice transluminal endoscopic surgery versus laparoscopy as a day-care procedure: a randomised controlled trial. BJOG. 2019 Jan;126(1):105-113. doi: 10.1111/1471-0528.15504. PMID: 30325565. | |
Michener CM, Lampert E, Yao M, et al. Meta-analysis of Laparoendoscopic Single-site and Vaginal Natural Orifice Transluminal Endoscopic Hysterectomy Compared with Multiport Hysterectomy: Real Benefits or Diminishing Returns? J Minim Invasive Gynecol 2021;28(3):698–709. doi: 10.1016/j.jmig.2020.11.029. PMID: 33346073. |
Online Study Assessment Option
All readers who are qualified doctors or allied medical professionals can automatically receive 2 Continuing Professional Development points plus a Study Completion Certificate from GLOWM for successfully answering four multiple-choice questions (randomly selected) based on the study of this chapter. Medical students can receive the Study Completion Certificate only.
(To find out more about the Continuing Professional Development awards program CLICK HERE)
