This chapter should be cited as follows:
Langenegger EJ, Hall DR, Glob Libr Women's Med
ISSN: 1756-2228; DOI 10.3843/GLOWM.413753
The Continuous Textbook of Women’s Medicine Series – Obstetrics Module
Volume 9
Principles and practice of obstetric high-dependency and critical care
Volume Editor: Professor Stephen Lapinsky, University of Toronto, Canada

Chapter
Organization of Obstetric Critical Care and Obstetric Critical Care Units (OCCU)
First published: February 2021
Study Assessment Option
By answering four multiple-choice questions (randomly selected) after studying this chapter, readers can qualify for Continuing Professional Development points plus a Study Completion Certificate from GLOWM.
See end of chapter for details.
INTRODUCTION
It has been shown that when patients with severe illnesses are grouped together in the same area and cared for by experienced medical and nursing staff, patient outcomes improve. This principle can also be applied to the management of critically ill obstetric patients.1 Pregnant and postpartum patients pose specific challenges in terms of altered physiology, fetal monitoring and maintaining a fetal-friendly environment. Pregnant patients admitted to an ICU have a greater risk of cesarean section and are especially susceptible to nosocomial infection with drug-resistant organisms.2,3 An obstetric critical care unit (OCCU) system provides the ideal facility for optimizing both maternal and fetal outcomes.4 A specific advantage is that it provides for immediate dedicated obstetric emergency care as well as fetal care and monitoring.5 There is also sufficient space and skill to induce labor and perform normal as well as assisted vaginal deliveries. It is important for the obstetrician and midwife to have appropriate knowledge and skill in the management of obstetric emergencies, resuscitation and critical care management. In an obstetric service, anesthetists are also closely involved with the management of patients with maternal risk factors or when a cesarean section is indicated, while midwives are trained to observe neonates, assist with neonatal resuscitation and can assist mothers with breastfeeding. It is therefore possible for a mother in a stable condition to remain with her baby, thereby reducing maternal anxiety and psychologic trauma resulting from separation from her newborn baby during critical care unit admission.6,7
Owing to the above-mentioned reasons, there are advantages to managing more stable obstetric patients in a specialized OCCU in the labor ward as opposed to management in a general ICU. It is of utmost importance that anesthetists and intensive care specialists are available for consultation and assistance when necessary. It is also important to identify and transfer patients to general intensive care units when indicated. There is little published guidance on how to establish and organize an OCCU. This chapter provides more detailed guidance based on an OCCU central hospital blueprint which has been developed, implemented and tested.2,4,5
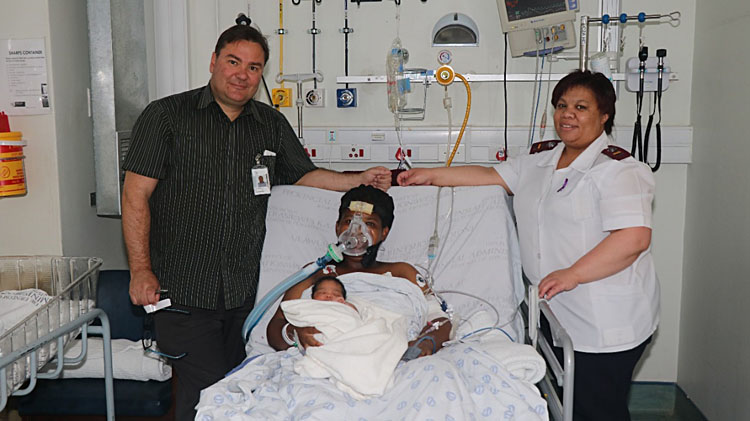
1
Patient on mask respiratory support after delivery in OCCU, South Africa. From right to left (E Langenegger, patient on mask, professional nurse and midwife C Morris) (with permission).
EVIDENCE FOR OBSTETRIC ADMISSIONS TO A DEDICATED OBSTETRIC CRITICAL CARE UNITS (OCCU)
The volume of research specifically addressing the impact of dedicated obstetric critical care on maternal and perinatal outcomes is limited to descriptive case series, with units reporting generally favorable outcomes and noting the need for mechanical ventilation as the main indication for transfer to general ICU.8,9,10 Two more recent prospective studies2,5 were described by Langenegger et al., which aimed to investigate the outcomes in critically ill obstetric patients managed in a newly established OCCU at a South African Hospital.
In one study, patients with severe maternal morbidity and/or criteria for critical care managed in the labor ward of Tygerberg Academic Hospital, South Africa, were studied over a 3-month period. Immediately thereafter, an OCCU was established within the labor ward of that hospital. Patients admitted and managed in the “after OCCU” group were studied using the same methodology, with 123 patients meeting the inclusion criteria. The data of the “before OCCU” group were compared with the data of the “after OCCU” group. The before and after comparison, demonstrated a decrease in the ratio of mortalities per severe morbidity for patients managed in the OCCU.5 The impact of the intervention was further investigated in a prospective cohort study which described the management and outcome of the initial 302 patients managed in the established OCCU located within the labor ward. Of the admissions, 46% were undelivered, two-thirds of admissions had severe organ dysfunction requiring level 2 obstetric critical care, while one-third developed or had existing indications for level 3 obstetric critical care. The most common reasons for admission were hypertensive disorders (43%), medical disorders (23%), severe sepsis (19%) and massive hemorrhage (11%). Intra-arterial lines were frequently used (91%) to guide resuscitation and administration of vasoactive drug infusions. Mask CPAP (continuous positive airway pressure) was utilized in pre-eclampsia patients with respiratory distress and pulmonary edema first, with the intubation rate being only 12%. Patients with more than one organ system failure or requiring ventilation for more than 24 hours were transferred to general ICU when a bed became available. There were eight deaths (2.6%) in the series.11 The SAMM (severe acute maternal morbidity): mortality rate at the institution prior to the establishment of the OCCU was one death in every five women admitted with severe morbidity, this decreased to one mortality in every 30 patients admitted with severe morbidity afterwards. These studies demonstrated that it was possible to reorganize existing resources to better care for patients with morbidity.
In a review on the provision of critical care services for the obstetric population in the United Kingdom, Sultan et al. emphasized the importance of reducing the incidence of SAMM and mortality.12 They stated that in specific circumstances there may be a role for high dependency care units within labor wards in higher-income countries. Specialist obstetric units show lower rates of maternal transfer to intensive care units and provide continuity of care before and after labor.12 Obstetric patients and critically ill women should receive the same standard of care for both their pregnancy-related and critical care needs provided by relevant professionals whether these are provided in a maternity or general critical care setting.13
Video 1 demonstrates the initiation non-invasive respiratory support provided by a midwife with basic critical care training.
1
Video demonstrating the initiation of mask respiratory support in an OCCU with permission.
WHEN SHOULD A DEDICATED OCCU BE ESTABLISHED?
Obstetricians practicing in large referral central hospitals are increasingly confronted with critically ill patients. Often, doctors and nurses with limited experience in critical care have to care for these patients in labor wards with limited access to ICU resources.14
However, in high-income countries most of the level 2 and 3 intensive care is provided in a general ICU or in a maternity hospital ICU.15 In these circumstances a separate obstetric ICU is not a practical use of resources, based on factors such as appropriateness of population size. In large referral hospitals (which may include those in higher-income countries) and especially in countries with limited ICU resources it is often necessary to provide dedicated level 2 critical care in a labor ward setting. It would then be ideal to have the emergency capacity to upgrade to ICU care which includes short-term ventilation.8,9,10,11
The current FIGO recommendation is based on the central OCCU blueprint described by Langenegger et al., as well as the collective experience of two large OCCUs in South Africa and Columbia.4 To justify a stand alone OCCU, it was estimated that a minimum of four dedicated obstetric critical care beds are required in central hospitals with 45,000–50,000 deliveries per annum when the SAMM incidence is around 1–2%. The requirements and objectives of an OCCU are listed in Table 1.
1
Requirements and objectives of an OCCU.
Objectives of an OCCU
|
GUIDANCE FOR THE ESTABLISHMENT AND ORGANIZATION OF AN OCCU
Based on the experience gained from the establishment of a four-bedded dedicated OCCU in South Africa there is now detailed guidance describing exactly how to establish a new OCCU with minimal changes in labor ward infrastructure and human resources. In the conceptualization and planning of an OCCU, it is important to combine common standards of care applicable to a general ICU and apply them in an OCCU. In this regard, an urgent need exists for a detailed blueprint describing the establishment of an OCCU located within a labor ward. This blueprint should provide sufficient detail to be used by lead clinicians, nursing managers, builders and clinical engineers. Another integrated essential aspect is the planning of an educational blueprint to train the midwives and doctors who will provide care in the OCCU. The model for a central hospital OCCU described here was recommended by the FIGO Safe Motherhood committee.4
WHO SHOULD BE ADMITTED TO AN OCCU?
Combining general critical care definitions and SAMM, the following definition is proposed for obstetric critical care: “A critically ill obstetric patient can be defined as an antenatal, intrapartum or postpartum (42 days) woman with impending, developing or established significant organ dysfunction, which may lead to long-term morbidity or death”.16,17 The indications for admission and the levels of obstetric critical care requirements are described in Tables 2 and 3.
2
Criteria for admission to an OCCU.
|
3
Requirements for different levels of care in an OCCU.
OCCU (level 2) | OCCU (level 3) | |
Monitoring | Arterial-line, central venous pressure catheter (CVP), ECG, SaO2 | Cardiac output assessment, CVP, ECG, SaO2 |
CVS support | IV infusion antihypertensives, IV nitrates | IV infusion antihypertensives, IV nitrates, inotropes |
Respiratory support | Non-invasive respiratory support | Emergency intubation and ventilation capacity (short term), refer to general ICU |
Renal support | Dialysis done by renal team in renal unit | Dialysis done by renal team in OCCU |
Organ system support | Single organ system failure | Single organ system failure and another organ system dysfunction |
MANAGEMENT MODELS OF CRITICAL CARE UNITS
There are two management models for general critical care, namely open and closed units. In the closed unit the patient is transferred to the specific ICU. The dedicated ICU team takes over responsibility of the patient, while members of the multidisciplinary specialties are consulted when necessary. In the open unit a surgeon, physician, obstetrician, anesthetist or pediatrician admit their patient into an open ICU. The admitting doctor maintains responsibility for the management of patient. The closed unit has the advantage of a clinical director managing the unit.. Clinical care is provided by an intensivist or fellow on a 24-hour basis. Closed models have been shown to have improved clinical outcomes with lower morbidity and mortality and shortened length of hospital stay.3,18 A hybrid of the closed ICU system may be possible for an OCCU in South Africa with limited resources. During normal working hours the medical director or obstetrician with an interest in Maternal Medicine will triage, admit and decide on patient management. Outside normal working hours the on call obstetric consultant and registrar will be primarily responsible for patient management. Critical care support when needed may be provided by the labor ward theater anesthetic registrar. Involving anesthetists in obstetric critical care patient management may improve maternal outcomes in obstetric critical care. It is valuable when critically ill women or women at risk of critical illness can be assessed in the antenatal period in order to formulate an anesthetic and combined critical care plan.4
HOW TO PLAN, DESIGN AND ESTABLISH AN OCCU
Unit design and site location
The unit should be located in close proximity to the labor ward. It is also important that the unit must be located close to the obstetric admissions area, obstetric theaters, neonatal resuscitation station and postoperative recovery room. The location of an OCCU must allow for access to existing infrastructure such as gas pipelines, emergency power supply and ventilation shafts, which can be extended to the OCCU site.
Size and infrastructure construction
The optimum size for the unit is set at four beds in an open area. The open floor area should be 80–120 m2 in order to allow for at least 20 m2 floor area for each bed as well as 2.5 m of unobstructed corridor space between the beds. Partitions should be used to ensure privacy during labor and delivery.4 Critical care units with less than four beds pose clinical management challenges in terms of staffing ratios and may not be cost-effective due to scales of economy. Units larger than eight beds on the other hand present problems with regards to unit management. The doorways of the area have to be wide enough to allow easy passage for a bed and movable equipment. Clinical aspects of addressing adequate size in terms of the number of beds needed should be based on general intensive care guidelines. An OCCU should ideally have the capacity to accept 95% of all patient referrals with an indication for admission.4
Bedside layout taking fetal monitoring into consideration
The practical bed head-to-wall layout is the recommended option (Figure 2). The unit must be furnished with four critical care beds with bedside rails and adjustable height as well as positions (head up, head down, elevate or lower bed). It is useful, but not essential, to have access to a delivery bed in the event of vaginal delivery; however, the majority of deliveries can safely be performed on the ICU bed. In the case of a unexpected emergency such as shoulder dystocia, the patient can be turned sideways with support to facilitate the delivery. Delivery beds are more expensive and most of the available labor ward delivery beds do not have bedside railings; most delivery beds can only be used for a vaginal delivery when the patient is stable and fully conscious with no risk of falling off the bed. There must be suitable screening between each bed. The ideal is a ceiling to floor partition, however, material curtains hung from ceiling suspended curtain railings can also be used. The walls must be strong enough to support equipment fixed from them such as monitors. A rail with a load capacity of 20 kg must be mounted to the wall for equipment.19,20,21 The monitors can be fixed to the wall using monitor mountings (Figure 2).
Adjustable examination lights should ideally be suspended from the ceiling. A framed mobile light can also be used. Sufficient lighting is essential to conduct a vaginal delivery or a clinical procedure such as inserting a central venous catheter. Storage as well as a bedside light must be available next to each patient’s bed. Every bed must have a mobile trolley with adjustable height for meals, patient files and observation charts. The key requirement for the layout of the bed area is that it must provide for easy access to the patients. Infrastructure and equipment must be mounted in such a way that it will not impede basic nursing care (Figure 2).
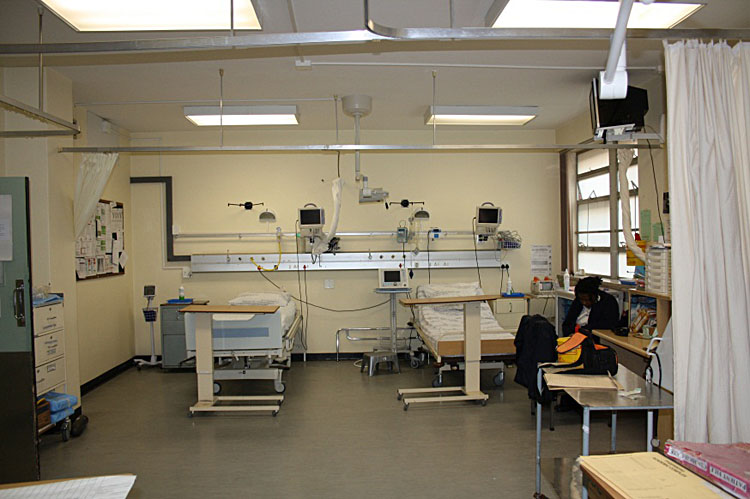
2
OCCU infrastructure and equipment.
The advantage of an OCCU situated in close proximity to the labor ward is access to storage space within the labor ward store room with a dedicated storage area for OCCU. It is essential to have storage space within OCCU to store essential items listed in Table 4
4
Essential items in the OCCU cupboard space.
Circulation: infusion lines, intra-arterial lines, central venous catheters, pulmonary artery catheter Airway: oxygen mask, ambu bag, ventilator circuits and filters Breathing: additional oxygen cylinder Cables for monitors Fridge: blood and necessary drugs for cold storage Other drugs in glass cabinet Scheduled drugs (e.g. opioids) in a lockable cabinet Blood gas analyser on cupboard surface Environment: gloves, masks, soap, sterile swabs Disposables Small capital items, e.g. ophthalmoscope, reflex hammer |
Central nursing station
The central nursing station should be sited where direct visual contact with all four patients and their monitors is possible, and close enough to patients to enable the staff to hear any alarms. There should be storage shelves behind the nursing station desk to store management booklets, files, forms (e.g. laboratory and blood bank forms) and stationery.
The following nursing station communication facilities are regarded as essential:
- a computer terminal connected to the hospital intranet service
- an internet link to laboratories and radiology
- two telephone extensions: one internal and one external.
Accommodation
Accommodation such as rooms for dirty linen and tearoom should be incorporated into the existing labor ward accommodation where possible in order to save on cost and decrease construction time. It is, however, important to have a separate office for the nursing manager. The essential accommodation that could be shared with the existing labor ward is listed in Table 5.
5
Accommodation that could be shared with existing labor ward.
Reception area Patient areas Staff tearoom Lavatories, showers and cloakrooms Kitchen facilities Storage area for case notes Secretary’s office Doctors sleeping room Linen rooms Dirty utility rooms Clinical waste disposal holding area |
Bedside layout of engineering services and specifications
Recommendations of the International Federation of Gynaecology and Obstetrics,4 European Society of Critical Care Medicine,22 United Kingdom Health Building Note 27,23 and the South African Policy on Defining Critical Care24 were followed to compile a blueprint for bedside engineering services such as the specifications for oxygen pipelines, central vacuum pipelines, electricity, water and basins, unit ventilation requirements, infection control requirements (Table 6), climate control, heating, lighting, safety and security requirements.
6
Infection control requirements.
Antibiotic policy guided by the department of microbiology Infection control guidance on clothing of staff and visitors Guidance on hand washing methods Sterilization of equipment Aseptic precautions for invasive procedures such as placement of a central venous catheter Disposable items Changing of catheters, humidifiers, ventilator filters, tubing and other equipment Isolation of patients with an infective disease Barrier nursing Temperature control |
Equipment in OCCU: maternal, fetal and neonatal
The correct equipment is essential to provide an appropriate level of critical care. Patient physiological variables need to be monitored. Effective respiratory and hemodynamic support equipment are key functions in critical care and may be life-saving. The monitor screens in the unit have to be clearly visible to the medical and nursing personnel. Detailed standards for critical care unit equipment are listed in Tables 7 and 8. A neonatal resuscitair should be available to the unit with the recommended temperature settings, oxygen and suction connections. In the case of twin deliveries, a neonatal resuscitair crib in the delivery room next to the unit was used. The baby was placed in a standard cot next to the mother in OCCU when both mother and baby was stable. Skin contact and breastfeeding were encouraged and maintained when the mother was stable.
7
Equipment needed in an OCCU.
Large capital items | Indication |
Resuscitation trolley Adult & neonatal | Maternal resuscitation, neonatal resuscitation Elective and emergency intubation |
Defibrillator | Resuscitation |
Neonatal “Mecacrib” | Maintain neonatal temperature and infrastructure for neonatal resuscitation |
Monitors | Monitor vitals: blood pressure, SaO2, ECG, respiration, cardiac output |
Respiratory support equipment | Bi-PAP/CPAP machine, Ventilator |
Circulatory support equipment | Volumetric infusion pumps Syringe drivers for IV drug infusions |
Electric warming blanket | Maintain adequate temperature during critical illness or resuscitation |
Small fridge | Drug storage for specific drugs requiring cold storage, emergency blood products |
Cardiotocograph (CTG) | Monitor fetal heart and contractions |
Blood gas analyser (preferable) | Frequent blood gas analysis |
Lockable cupboard | Morphine and other scheduled drugs |
Procedure trolley | Insertion of arterial lines, central venous pressure catheters (CVP) |
Sterile procedure pack | CVPs, arterial lines, epidural |
Sterile delivery pack | Delivery of baby |
Ultrasound machine | Fetal ultrasound and ultrasound guided procedures, non-invasive CVP |
CPAP, continuous positive airway pressure; Bi-PAP, Bi level positive airway pressure.
8
Smaller capital items necessary in an OCCU.
Durable items | Non-durable items |
Diagnostic ophthalmoscope Wright’s spirometer Low temperature thermometer Oxygen bed rack for transport of patients on a ventilator Fiberoptic laryngoscope & blades | Pressure bags for arterial lines Normal and large sized blood pressure cuffs Pressure air mattress Nasal CPAP mask sets Full face mask CPAP sets Ambu bags (manual resuscitators) |
CPAP, continuous positive airway pressure.
The construction of the unit and purchasing of equipment should be performed as a parallel process. The admission guidelines, unit management model, recruiting and allocation of required human resources are described in the following section.
ADMISSION AND DISCHARGE GUIDELINES
It is important to decide on appropriate admission guidelines in order to ensure that the resources are used appropriately. The medical and nursing staff as well as infrastructure must be planned carefully in order to provide the effective care required by the patients admitted to the OCCU. The proposed admission criteria are described in Table 2.
HUMAN RESOURCES AND OPERATIONAL RECOMMENDATIONS
In the blueprint described in this chapter, the OCCU level 2/3 human resource management plan was based on a hybrid of the closed general ICU system. This required the appointment of an obstetrician with an interest in critical care, and the ability to lead and manage the process of establishing the OCCU. The director of OCCU should be a specialist obstetrician with an interest in high-risk obstetrics and a prior 3-month rotation in a general ICU. Additional support from cardiology, nephrology, and the medical and the surgical ICUs should be mobilized by the identified head of the OCCU. The duties of the head of the unit are listed in Table 9.
9
Duties and responsibilities of the head of the OCCU.
Manage the unit establishment process Function as multidisciplinary team leader Establish and monitor admission and discharge criteria Establish policies and protocols Quality assurance Coordinate education and, if possible, research Manage the unit budget Manage staff requirements |
After identification of the clinical head, the next important step was to appoint a suitable, dedicated nursing manager for the OCCU. The recommended requirements for the nursing manager are knowledge and skill in critical care and obstetrics. Together, the clinical head and nursing manager proceeded with communicating the vision and care benefits for complicated cases previously managed in a labor ward but now in an OCCU. The nursing manager was responsible for the nursing program including delegation of roles and responsibilities of the nursing staff. Other functions performed by her were the implementation of policies and procedures, quality assurance, provision of supplies and equipment and staff education and training.
Day-to-day care in the OCCU
Day-to-day care should be provided by a dedicated registrar (resident) and a dedicated medical officer under the guidance of a specialist/consultant with experience in obstetric critical care. Although the OCCU should be managed by the clinical head, this person will also have other clinical responsibilities. For this reason, additional consultant cover during office hours and out of hours should also be provided by the other specialists/consultants in the department. The obstetric registrars (residents) or a dedicated senior medical officer can provide daytime clinical patient management. Senior residents or experienced medical officers should cover the unit after hours. The anesthetist registrar on call for the labor ward should be available for preoperative assessment, critical care advice and to assist with procedures such as intubation and ventilation. The duties of the obstetric doctors working in the unit are listed 10.
10
Clinical duties of the doctor working in the OCCU.
Resuscitation of unstable patients Assess labor ward patient referrals Admit patients with, or at risk of organ disfunction or failure Do a systematic evaluation Discuss admissions with the on call consultant Consult relevant disciplines Treat the underlying cause Administrative duties |
Professional nurses
The nurse functioning in the critical care environment should monitor patients closely, make decisions based on clinical and monitoring assessment, and act accordingly.6 Midwives and professional nurses working in an OCCU, must be trained in and understand basic obstetric critical care principles as well as midwifery. The nursing staff required for the four-bedded unit include were, one unit-nursing manager, ten professional nurses and five enrolled nursing assistants. The planned work pattern was a 12-hour shift in order to provide two nurses in the OCCU on each shift. Ideally, an experienced midwife with critical care knowledge and one general nurse with experience in critical care were placed together on a shift. The duties of the professional nurse and midwife are listed in Table 11. Ancillary nursing staff play a very important role in the OCCU patient management through supporting the professional nurse in her duties under supervision. However, they are not able to replace a trained professional nurse and midwife (in South Africa this is one person).
11
Duties of the professional bedside nurse and midwife.
Provide compassionate and holistic care Collect and interpret vital data Repeated clinical assessments Communicate relevant findings to the doctor Interact with family members Provide patient health care education |
Other ancillary staff must be available for consultation when necessary. These include physiotherapists, social workers, nutritionists, radiographers, clinical engineers and critical care technicians when available. The daily program of the OCCU model is shown in Table 12.
12
Day to day program of care in the OCCU model.
Prior to the consultant morning round:
|
At the consultant morning ward round:
|
Afternoon consultant ward round:
|
After hours care:
|
Quality assurance and ongoing training
The recommended quality indicators must be used to measure the effectiveness and safety of critical obstetric care services. These should include number of admissions as level 3, number of admissions as level 2, readmissions, length of hospital stay, referrals, maternal morbidity and mortality, patient outcomes, communication and availability of staff with competencies for critical care management.4,13
Ongoing training is essential to ensure quality care. Simulation is the preferred strategy that makes it easier for teams to practice in a safe environment and eliminates the possibility of harm to patients. Medical staff working in the obstetric critical care unit must also receive ongoing training in monitoring to ensure correct interpretation and management.
CONCLUSION
Models of obstetric critical care vary widely, depending on health system characteristics and, in particular, the degree of development of each country. One of the options to provide a dedicated obstetric critical care service is to establishment an obstetric critical care unit. The discipline of obstetric critical care must be expanded wherever possible. The OCCU blueprint adapted for local requirements and conditions can be implemented in central or tertiary level hospitals in both low- and middle-income countries.
ACKNOWLEDGEMENTS
The Tygerberg OCCU’s nursing manager, Charmaine de Villiers played a central role in the establishment and organization of the unit. She provided invaluable in service critical care skills training for midwives working in the unit.
PRACTICE RECOMMENDATIONS
- Obstetric patients at risk of organ dysfunction or with established organ dysfunction must receive emergency critical care management as soon as possible.
- Obstetric critical care (OCC) is described as the specialized management of critically ill obstetric patients via an interdisciplinary approach in which the optimization of the clinical variables of pregnant women should be approximated to the maternal–fetal unit needs as a whole.21
- One pragmatic solution is to establish OCCUs in the labor wards of central hospitals with the recommended infrastructure, equipment and human resources required.4
- An OCCU must be able to provide the following clinical services:
- Provide clear admission, discharge guidelines and operational procedures;
- Early identification and resuscitation of patients with maternal complications and organ dysfunction;
- The ability to offer short-term ventilation and full intensive care prior to transfer to a general ICU or if no such bed is available;
- Monitor the mother and fetus in a critical care environment;
- Induce and monitor labor, safe delivery of the baby;
- Rooming-in of healthy newborn babies when the mother is stable.
CONFLICTS OF INTEREST
The author(s) of this chapter declare that they have no interests that conflict with the contents of the chapter.
Feedback
Publishers’ note: We are constantly trying to update and enhance chapters in this Series. So if you have any constructive comments about this chapter please provide them to us by selecting the "Your Feedback" link in the left-hand column.
REFERENCES
Scott J, Foley M. Organizing an Obstetric Critical Care Unit. In: Belfort M. (ed.) Critical Care Obstetrics, 5th edn. Blackwell Science Publications, 2010:11–5. | |
Langenegger EJ. Establishing an obstetric critical care unit in a South African tertiary hospital, PhD thesis 2016. <http://scholar.sun.ac.za> Faculty of Medicine and Health Sciences, Department of Obstetrics and Gynaecology and Tygerberg Hospital. | |
Critical Care in pregnancy. ACOG Practice Bulletin No. 100: American College of Obstetricians and Gynecologists. Obstet Gynecol 2009;113:443–50. | |
Langenegger EJ, Theron GB, Hall DR, et al. A blueprint to establish a four-bed obstetric critical care unit in the labor ward of a central hospital. International journal of gynaecology and obstetrics: the official organ of the International Federation of Gynaecology and Obstetrics. 2019;146:29-35 | |
Langenegger EJ, Hall DR, Mattheyse F, et al. The impact of an obstetrician-led, labor ward critical care unit: A prospective comparison of outcomes before and after. Obstetric Medicine 2019;1–5. Available at: https://doi.org/10.1177/1753495X19838193. | |
McMurphy Baird S, Troiano N. Critical Care Obstetric Nursing. In: Belfort M, Saade GR, Foley MR, Phelan JP, Dildy GA. (eds.) Critical Care Obstetrics, 5th edn. Oxford: Blackwell Publishing, 2010:16–29. | |
Hinton L, Locock L, Knight M. Maternal critical care: what can we learn from patient experience? A qualitative study. BMJ Open 2015;5:e006676. doi: 10.1136/bmjopen-2014–006676. | |
Johanson R, Anthony J, Dommisse J. Obstetric Critical Care at Groote Schuur Hospital, Cape Town. J Obstet Gynecol 1995;15(3):174–178. | |
Mabie W, Sibai B. Treatment in an obstetric intensive care unit. Am J Obstet Gynecol 1990;162:1–4. | |
Zeeman G, Wendel G, Cunningham F. A blueprint for obstetric critical care. Am J Obstet Gynecol 2003;188:532–536. | |
Langenegger EJ, Hall DR, Mattheyse F. Management and outcome of the first 302 patients admitted to a new South African Obstetric Critical Care Unit (OCCU) within the labour ward: a prospective case series. BJOG 124(Suppl 1):143. | |
Sultan P, Arulkumaran N, Rhodes A. Provision of critical care services for the obstetric population. Best Pract Res Clin Obstet Gynaecol 2013; 27(6):803–9. | |
The Maternal Critical Care Working Group. Providing equity of critical and maternity care for the critically ill pregnant or recently pregnant woman. London Royal College of Obstetricians and Gynecologists. Available at: http://www.rcog.org.uk/files/rcog-corp/Prov_Eq_ MatandCritCare.pdf. | |
Mathivha L. ICUs worldwide: An overview of critical care medicine in South Africa. Crit Care 2002;6(1):22–23. | |
Lapinsky S, Kruczynski K, Seaward G, et al. Critical care management of the obstetric patient. Can J Anaesth 1997; 44:325–29. | |
Mantel G, Buchmann E, Rees H. Severe acute maternal morbidity: A pilot study of a definition for a near-miss. BJOG 1998;105:985–90. | |
Ananth C, Smulian J. Epidemiology of Critical Illness in Pregnancy. In: Belfort M, Saade GR, Foley MR, Phelan JP, Dildy GA. (eds.) Critical Care Obstetrics, 5th edn. Oxford: Blackwell Publishing, 2010:1–10. | |
Valentin A, Ferdinande P, ESICM Working Group on Quality Improvement. Recommendations on basic requirements for intensive care units: structural and organizational aspects. Intensive Care Med 2011;37(10):1575–87. | |
Society of Critical Care Medicine. Recommendations for critical care unit design. Task force on guidelines. Crit Care Med 1988;16:796–806. | |
Health Building Note 27: Intensive Therapy Unit. NHS Estates. HMSO Department of Health and Social Security. United Kingdom, 1992. | |
Royal College of Anaesthetists. Care of the critically ill woman in childbirth; enhanced maternal care, 2018. https://www.rcoa.ac.uk/system/files/EMC-Guidelines2018.pdf. Accessed April 23, 2019. | |
European Society of Critical Care Medicine | |
United Kingdom Health Building Note 27 | |
South African Policy on Defining Critical Care |
Online Study Assessment Option
All readers who are qualified doctors or allied medical professionals can automatically receive 2 Continuing Professional Development points plus a Study Completion Certificate from GLOWM for successfully answering four multiple-choice questions (randomly selected) based on the study of this chapter. Medical students can receive the Study Completion Certificate only.
(To find out more about the Continuing Professional Development awards program CLICK HERE)
