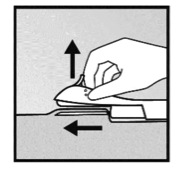
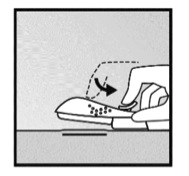
Implantable Contraception
Authors
INTRODUCTION
Contraceptive implants are progestin-based, highly effective, and rapidly reversible methods of contraception that require little of the user and have few side effects. Over the past 35 years they have been approved in more than 60 countries and used by millions of women worldwide.1 Their high efficacy along with ease of use make them a good contraceptive option for women who require progestin-only methods, teens who find adherence to a contraceptive regimen difficult, as well as healthy adult women who desire long-term protection. In most countries, two different contraceptive implants are available: the single rod etonogestrel implant and the two-rod levonogestrel system. The pharmacological profile and physical effects of all the implantable contraceptives are similar. While the etonogestrel implant is the only form of implantable contraception available in the United States, clinicians in other countries may encounter the two rod levonorgestrel (Jadelle®, Sinoplant®) and six capsule (Norplant®) systems.
HISTORY OF IMPLANTABLE CONTRACEPTION
Norplant, a six capsule implantable system containing 216 mg of levonogestrel, was developed by the Population Council and first approved in 1983 in Finland, where it was manufactured. United States’ FDA approved it in 1990, but the distributor withdrew it from the market in 2002. Over one million US women chose Norplant as their contraceptive. Norplant proved highly effective; over a 7-year duration of use, only about 1% of users became pregnant.2 Despite low rates of pregnancy and few serious side effects, limited supplies of the silastic components and unwarranted negative media coverage led to Norplant’s withdrawal from distribution in 2002, leaving no implant alternative for American women.3 Production of Norplant was discontinued worldwide in 2008.
The 15-year experience with Norplant instigated further development and improvements in implant design. A two-rod levonorgestrel (LNG) system (Jadelle) was also developed by the Population Council and manufactured in Finland. Jadelle is effective for 5 years and was first registered for this length of use in the year 2000. Both patients and providers have been shown to prefer Jadelle to Norplant, primarily due to the smaller number of implants.4 Levonorgestrel systems were traditionally inserted with reusable stainless steel trocars. Jadelle’s insertion trocar is now disposable, as the sterilization requirements of reusable trocars were cumbersome to maintain.5 The Sinoplant (II) is a two-rod implant system designed to imitate the performance of Jadelle. It is manufactured in China and is substantially less expensive than Jadelle (US$8 compared with US$23 in some countries).6 This levonorgestrel implant has the potential to improve access to contraceptive implants in resource-poor settings. Sinoplant is not US FDA approved; Jadelle is FDA-approved but is not marketed in the USA. Elcometrine is a single rod nesterone implant registered in Brazil for 6 months of use for the treatment of endometriosis. Nestorone is biologically inactive when given orally due to its rapid first-pass hepatic metabolism and, therefore, is not active in the children of breastfeeding women.7, 8
Implanon, a single rod etonogestrel implant, became widely available for use in 2003. Implanon’s single rod provided great improvements over the previously available six capsule Norplant system in time and ease of insertion.9, 10 The etonogestrel implant inserter is preloaded and disposable. Since only one rod is implanted, there is no chance of moving previously placed capsules out of position with insertion of additional ones. It is not necessary, as it was with Norplant, to create channels under the skin with local anesthetic, which made implants difficult to palpate right after insertion. In addition, ethylene vinyl acetate, the plastic from which Implanon is made, is less likely than Norplant’s silastic to form a fibrous sheath that can prolong removal.11 These differences simplify the insertion and removal technique for the etonogestrel implant. For patients this simplicity means little discomfort at insertion or removal, an unobtrusive implant, and almost no scarring. For clinicians, it means simpler insertion and removal procedures of predictably short duration. The etonogestrel implant has subsequently been modified and marketed as Nexplanon. In December 2012, Merck stopped supplying Implanon to its distributers, whose supply was exhausted in early 2013. Implanon is no longer available for purchase in the United States. Implanon and Nexplanon are bioequivalent, but Nexplanon is radio-opaque and is pre-loaded into a simpler, one-handed, inserter that helps insure subdermal placement.
CANDIDATES FOR IMPLANTABLE CONTRACEPTION
Contraceptive implants are a good choice for women of reproductive age who are sexually active and desire long-term, continuous contraception. Implants should be considered for women who:
1. Desire a highly effective, long-term method of contraception;
2. Experience serious or minor estrogen-related side effects with estrogen-progestin contraception;
3. Prefer a method that does not require repeated adherence;
4. Desire a non-coitus-related method of contraception;
5. Have completed their childbearing but are not yet ready to undergo permanent sterilization;
6. Have a history of anemia with heavy menstrual bleeding;
7. Intend to breastfeed;
8. Have chronic illnesses, in which health will be threatened by pregnancy.
Most women are candidates for implantable contraception; there are few medical disorders where the risk of the method exceeds the benefit (e.g. current breast cancer). For clinicians in the United States, the Centers for Disease Control and Prevention (CDC) has listed these conditions in the table “United States Medical Eligibility Criteria (USMEC) for Contraceptive Use”.12 Standard contraindications to use of hormonal contraceptives are:
1. Known or suspected pregnancy;
2. Current or past history of thrombosis or thromboembolic disorders;
3. Hepatic tumor or active liver disease;
4. Undiagnosed abnormal genital bleeding;
5. Known or suspected breast cancer or history of breast cancer;
6. Hypersensitivity to any component of the method.
Large epidemiologic studies have not identified an increased risk of stroke, myocardial infarction, or venous thromboembolism in users of progestin-only oral contraceptives,13, 14, 15 and none of these events occurred in any of the trials on which approval of implants were based.16 For this reason, the World Health Organization (WHO) and the CDC have indicated progestin-only contraceptives represent a reasonable contraceptive choice for women with risk factors for, or a past history of, venous thromboembolic disease.17, 18 Subsequently published data support this conclusion.19
This recommendation differs from Nexplanon (and Implanon, Jadelle and Sinoplant) package labeling, which lists current or past thrombosis as a contraindication to use. Etonogestrel is the biologically active metabolite of the synthetic progestin desogestrel. Controversy remains as to whether desogestrel or its derivatives may be associated with an increased risk of venous thromboembolism compared with other progestins. Evidence of this increased risk comes from studies of oral contraceptives where desogestrel is administered in combination with ethinyl estradiol, rather than alone as in the implant.20
Women with chronic medical conditions
Implant contraceptives specifically can be a good choice for women with chronic illnesses because, aside from their need for highly effective contraception, there are no clinically significant metabolic changes associated with the sustained, low doses of progestin delivered by the implant. Studies of liver function, blood coagulation, immunoglobulin levels, serum cortisol levels, and blood chemistries have failed to detect changes outside of normal ranges and the etonogestrel implant has not been found to have important clinical effects on the lipoprotein profile, carbohydrate metabolism, thyroid and adrenal function, liver function, or the clotting mechanism.21 A literature review concluded that the etonogestrel implant does not appear to have clinically significant effects on lipid metabolism or liver function, although there may be small changes in laboratory values.22 These findings suggest that implant contraceptives are safe for woman at risk for metabolic, cardiovascular, or thromboembolic disorders.
For diabetics whose disease in well controlled by insulin or diet, implant contraceptives are a good choice. Although it is known that progestins can affect carbohydrate metabolism, most effects are seen with high doses of androgenic progestins, not the low doses found in implants nor with the less-androgenic etonogestrel used in Nexplanon.
Lactating women
As progestin-only methods, the contraceptive implants are a good choice for breastfeeding women because they do not interfere with breast milk production. Studies show no effects on breast milk quality or quantity, and infants of mothers with implants grow normally.23 Implants also seem to be a good choice for immediate postpartum administration. A small study comparing immediate postpartum insertion of the etonogestrel implant to depot medroxyprogesterone acetate at 6 weeks showed no impact on continuation of exclusive breastfeeding at 12 weeks and normal infant weight gain.24 While the WHO guidelines recommend postponing progestin implants until after 6 weeks postpartum, we disagree as the etonogestrel implant does not effect lactogenesis when placed in the immediate postpartum period (within 1–3 days of delivery) compared with delayed insertion (4–8 weeks).18, 25, 26 Immediate placement has also been found to better prevent unintended pregnancies and be more cost-effective when compared with delayed insertion.27
Adolescents
Adolescents are ideal candidates for contraceptive implants, as it is a method that does not require repeated adherence and offers a discrete method of highly effective contraception. Teens most frequently use methods with high failure rates, including condoms, withdrawal and oral contraceptive pills.28 Long acting reversible contraception, including implants and intrauterine devices, has a high uptake among adolescents, with younger teens choosing the implant more commonly.29 The etonogestrel implant is well accepted by postpartum teens as well.30 Women under age 18 years have no medical contraindication to implantable contraception based on age alone and the American College of Obstetricians and Gynecologists recommends offering implants as a first line method for teens seeking contraception.18, 31 Despite the benefits and acceptability of implantable contraception, less than 1% of current contraceptors and only 0.5% of adolescents choose this method.32 Recent studies indicate that use of implantable contraception has been increasing.33
PHARMACOLOGY
Implants are highly effective contraceptives that come in the form of one or more sub-dermally placed rods that slowly release progestin. These sustained-release systems rely on simple diffusion of steroid hormones through semipermeable plastics. The synthetic progestin passes from the plastic into the surrounding tissues and enters the circulatory system through absorption by the local capillary network. The release rate of the progestin depends on the surface area and the density of the plastic (silastic or ethylene vinyl acetate) in which the progestin is contained.
Jadelle
Each Jadelle rod contains 75 mg of levonorgestrel for a total of 150 mg, 66 mg less than that in the six Norplant capsules. The thin, flexible Jadelle rods are wrapped in silastic tubing (the same material used by Norplant), 43 mm in length and 2.5 mm in diameter, thus slightly longer and thicker than Norplant.34 Whereas the levonorgestrel in Norplant is packed into the capsules in crystal form, the core of the Jadelle rod is a mixture of levonorgestrel and an elastic polymer (dimethylsiloxane/methylvinylsiloxane). Long-term clinical trials indicate that the performance and side effects are similar to Norplant.35, 36 Because the release rates with the two levonorgestrel systems are comparable (Table 1) it is reasonable to conclude that clinical studies with Norplant and Jadelle should yield similar results. While Norplant has been more extensively studied, clinicians can assume that the findings apply as well to Jadelle, except that Norplant was shown to be effective for 7 years and Jadelle for 5.
Table 1 Release rate of levonorgestrel in two contraceptive implants
|
| Norplant average release rate | Jadelle average release rate |
| First month | 85 µg levonorgestrel daily | 100 µg levonorgestrel daily |
| After 1 year | 35 µg | 40 µg |
| After 2 years | 30 µg | 30 µg |
From: Speroff L, Darney, PD., 2010. A Clinical Guide for Contraception. 5th edn. Baltimore, MD: Lippencott, Williams & Wilkins.
After insertion of Norplant, plasma levels of levonorgestrel are stable at 0.4–0.5 ng/mL within 24 hours.37, During the first 6–12 months of use, Norplant and Jadelle release a total of about 80 mg of levonorgestrel every 24 hours, giving a plasma concentration of 0.35 ng/mL. After the first year, the release rate gradually declines to a relatively constant rate of 30–35 mg/day. At 5 years, the overall release rate is 25 mg/day, with corresponding levonorgestrel levels of 0.25–0.35 ng/mL. For comparison, progestin-only oral contraceptive pills also deliver about 80 mg of levonorgestrel per day; combined oral contraceptives with levonorgestrel as the active progestin deliver 50–125 mg. Peak serum levels after ingestion of 75 mg of levonorgestrel reach 1.5–2.0 ng/mL; after ingestion of 150 mg of levonorgestrel, serum peaks reach 2.7–4.2 ng/mL. These serum peaks are reached from 30 minutes to 2 hours after ingestion and are followed by a rapid decline, with an average half-life of 10–12 hours.38, This is in contrast to the stable, low serum concentrations of progestin achieved with the sustained-release systems.
Nexplanon
The Nexplanon implant is 40 mm X 2.0 mm and consists of one nonbiodegradable rod of 40% ethylene vinyl acetate and 60% etonogestrel (the 3-keto derivative of desogestrel), covered with a rate-controlling ethylene vinyl acetate membrane 0.06 mm thick. The rod contains 68 mg etonogestrel that is slowly released: initially at 60–70 µg/day, decreasing to 35–45 µg/day at the end of the first year, to 30–40 µg/day at the end of the second year, and then to 25 to 30 µg/day at the end of the third year (Figure 1).39 The high initial rate of absorption is probably due to a significant amount of etonogestrel released from the uncovered ends of the implant. Peak serum concentrations (266 pg/mL) of etonogestrel are achieved within 1 day after insertion, suppressing ovulation, which requires only 90 or more pg/mL.40, 41 Serum concentrations of entonogestrel are adequate to provide contraception for 5 years and WHO data suggest efficacy for that long.
Figure 1 Mean (±SD) serum concentration–time profile of etonogestrel after insertion of Nexplanon during 3 years of use. (With permission from: NEXPLANON® image reproduced with permission of Merck Sharp & Dohme B.V., a subsidiary of Merck & Co., Inc., Whitehouse Station, New Jersey, USA. All rights reserved.)
Etonogestrel is approximately 32% bound to sex hormone binding globulin (SHBG) and 66% bound to albumin in blood. Like other contraceptive steroids, serum levels of etonogestrel are reduced in women taking liver enzyme-inducing drugs such as rifampicin, griseofulvin, phenytoin, and carbamazepine, but are not affected by antibiotics. Steady release of etonogestrel into the circulation avoids first-pass effects on the liver. Bioavailability of etonogestrel remains nearly 100% throughout 2 years of use. The elimination half-life of etonogestrel is 25 hours, compared with 42 hours for Norplant’s levonorgestrel. After implant removal, serum etonogestrel concentrations become undetectable within 1 week. Return of ovulation occurs in 94% of women within 3–6 weeks after method discontinuation.40, 41 Unlike Implanon or the levonorgestrel implants, the Nexplanon rod is radio-opaque so it can be detected by x-ray and thus does not require magnetic resonance imaging (MRI) for locating an impalpable implant.
MECHANISM OF ACTION
Progestin-containing implants have two primary mechanisms of action: inhibition of ovulation and restriction of sperm penetration through cervical mucus.4 Antiestrogenic actions of the progestins affect the cervical mucus, making it viscous, scanty, and impenetrable to sperm thus inhibiting fertilization.42 At high doses, progestins also inhibit gonadotropin secretion, thereby inhibiting follicular maturation and ovulation.43 This dual effect allows contraceptive efficacy to be maintained even though ovulation is not consistently inhibited in etonogestrel implant users toward the end of the 3-year period of use. Even if follicles grow during use of progestin implants, oocytes are not fertilized. If the follicle ruptures, the abnormalities of the ovulatory process prevent release of a viable egg. Although progestins suppress endometrial activity, which makes the endometrium unreceptive to implantation, this is not a contraceptively important effect since the major mechanisms of action prevent fertilization.44 No signs of embryonic development have been found among implant users, indicating that progestin implants have no abortifacient properties. Implants are more effective than other methods because they do not require regular action by the user and because they have multiple modes of action.
EFFICACY
General population
The implant is among the most effective contraceptives available (Table 2), as good or better than sterilization procedures.43 An analysis of 11 clinical trials in which 942 women enrolled for 2–4 years showed the etonogestrel implant was well-tolerated and effective: no pregnancies occurred while women were using this method of contraception.16 Six pregnancies have been reported during the first 14 days after implant removal. The manufacturer cites a Pearl Index of 0.38 pregnancies per 100 women-years of use, which is similar to that of other long-acting methods of contraception. Pregnancy may be intrauterine or extrauterine.45 New data indicate that both the etonogestrel and levonorgestrel implant’s efficacy at pregnancy prevention continues for up to 5 years (Table 3).44, 46 Preliminary data from an ongoing study on prolonged use of the etonogestrel implant indicate that the serum levels of etonogestrel remain well above the 90 pg/mL needed for ovulation suppression.46 An important reason for the both of the implants’ high efficacy in actual use is the nature of the delivery system itself, which requires little effort on the part of the user. Because compliance does not require frequent resupply or instruction in use, as with oral and injectable contraception, the actual or typical use effectiveness is very close to the theoretical (lowest expected) effectiveness.
Table 2 Percentage of women experiencing an unintended pregnancy during the first year of typical use and the first year of perfect use of contraception and the percentage continuing use at the end of the first year. Adapted from Trussell 201182
|
| Percentage of women experiencing an unintended pregnancy within the first year of use | Percentage of women continuing use at 1 yeara | |
|
| Typical useb | Perfect usec | |
| Method |
|
|
|
| No methodd | 85 | 85 | — |
| Spermicidese | 28 | 18 | 42 |
| Fertility awareness-based methodsf | 24 | 0.4–5 | 47 |
| Withdrawal | 22 | 4 | 46 |
| Sponge |
|
| 36 |
| Parous women | 24 | 20 |
|
| Nulliparous women | 12 | 9 |
|
| Male condomg | 21 | 5 | 41 |
| Female condomg | 18 | 2 | 43 |
| Diaphragm | 12 | 6 | 57 |
| Combined pill and progestin-only pill | 9 | 0.3 | 67 |
| Combined patch | 9 | 0.3 | 67 |
| Combined ring | 9 | 0.3 | 67 |
| Depot medroxyprogesterone acetate | 6 | 0.2 | 56 |
| Copper IUD | 0.8 | 0.6 | 78 |
| Levonorgestrel IUD | 0.2 | 0.2 | 80 |
| Etonogestrel implant | 0.05 | 0.05 | 84 |
| Female sterilization | 0.5 | 0.5 | 100 |
| Male sterilization | 0.15 | 0.1 | 100 |
a. Among couples attempting to avoid pregnancy, the percentage who continue to use a method for 1 year.
b. Among typical couples who initiate use of a method (not necessarily for the first time), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.
c. Among couples who initiate use of a method (not necessarily for the first time) and who use it perfectly (both consistently and correctly), the percentage who experience an accidental pregnancy during the first year if they do not stop use for any other reason.
d. The percentages becoming pregnant are based on data from populations where contraception is not used and from women who cease using contraception in order to become pregnant. Among such populations, about 89% become pregnant within 1 year. This estimate was lowered slightly (to 85%) to represent the percentage who would become pregnant within 1 year among women now relying on reversible methods of contraception if they abandoned contraception altogether.
e. Foams, creams, gels, vaginal suppositories and vaginal film.
f. Includes the Ovulation, TwoDay, Standard Days and Symptothermal methods.
g. Without spermicides.
h. With spermicidal cream or jelly.
Table 3 Efficacy of implantable contraception at 36, 48 and 60 months. Adapted from Bahamondes44
|
| Levongestrel implant | Etonogestrel implant | ||
| Time from device insertion (months) | At risk/events (cum) | Rate (95% CI) | At risk/events (cum) | Rate (95% CI) |
| 0 | 997/0 | 0.0 | 995/0 | 0.0 |
| 36 | 682/3 | 0.41 (0.13–1.28) | 640/3 | 0.41 (0.13–1.28) |
| 48 | 507/3 | 0.41 (0.13–1.28) | 372/3 | 0.41 (0.13–1.28) |
| 60 | 449/3 | 0.41 (0.13–1.28) | 276/3 | 0.41 (0.13–1.28) |
Overweight and obese women
Contraceptive implants are not contraindicated in obese women. Although the effectiveness of the implant has not been adequately studied in women more than 130% of their ideal body weight (body mass index [BMI] greater than 30 kg/m2), available data show no decrease in contraceptive efficacy even though etonogestrel concentration is affected by weight. Etonogestrel concentrations do not decline below contraceptive levels as body weight increases, nor is there an increased risk of difficult insertions or removals with increasing BMI.47
Drug interactions compromising efficacy
Contraceptive efficacy may be decreased in women taking medications that affect the metabolism of etonogestrel. One case report of contraceptive failure occurred in a woman on carbamazepine for a seizure disorder who had had an etonogestrel implant in place for 25 months.48 There have been seven cases of contraceptive failure (two in one woman) in human immunodeficiency virus (HIV)-positive women using the etonogestrel implant and on efavirenz-based antiretroviral therapy.49, 50, 51, 52 All implants appeared to be correctly positioned and there was no obvious reason for the contraceptive failures other than a possible decrease of etonogestrel efficacy related to administration of efavirenz, a hepatic enzyme-inducing antiretroviral medication. One pharmacokinetic study of the etonogestrel implant in women on antiretroviral medications showed substantial decreases in the bioavailability of etonogestrel in women on a efavirenz-based regimen, whereas women on a lopivanir-based regimen had increased bioavailability of etonogestrel.53
Emerging evidence also suggests that efavirenz-based antiretroviral regimens affect levonorgestrel levels more profoundly, resulting in higher contraceptive failure rates.54, 55 In one retrospective study of HIV-positive women with the levonorgestrel implant, one of the 221 women on nevirapine or lopinavir/ritonavir-based regimens became pregnant, whereas 15 of the 121 women on efavirenz became pregnant.55 Neither nevirapine-based regimens nor tenofovir disoproxil fumarate-emtricitabine have been shown to alter levonorgestrel levels.54, 56
Although it is not currently possible to assess the magnitude of the risk of contraceptive failure in this setting, prospective users taking antiretrovirals should be informed that efavirenz use accelerates etonogestrel and levonorgestrel metabolism and greatly increases implant failure rates. From the available evidence on the etonogestrel implant in women taking efavirenz, it appears that the contraceptive failures occur later within the 3 years that the device is efficacious, possibly due to a more rapid depletion of etonogestrel levels. Some experts have suggested replacing the levonorgestrel implants early or placing more than one implant for women on efavirenz due to the decreased levonorgestrel levels, but these practices haven not been studied. The accelerated metabolism of progestin does not preclude use of implants, which remains highly effective for most women on antiretroviral and antiseizure drugs. Furthermore, HIV-positive women are typically advised to use condoms to protect against transmission of HIV and other sexually transmitted infections, thus they typically have back-up contraceptive protection.
COUNSELING
Irregular bleeding
Unscheduled bleeding is a common side effect, which may or may not decrease with continued use. Because implants allow for follicular development but not ovulation, endogenous estrogen production is nearly normal, and unlike the combined estrogen-progestin contraceptives, progestin is not regularly withdrawn to allow endometrial sloughing. Consequently, the endometrium sheds at unpredictable intervals and menstrual bleeding patterns can be highly variable among users of implant contraception. Changes include alterations in the interval between bleeding, the duration and volume of menstrual flow, and spotting.
In the analysis of 11 clinical trials, unscheduled bleeding was the primary reason for discontinuation, with a rate of 14.8% in the United States and Europe, but only 3.7% in Southeast Asia, Chile, and Russia.16 United States users were more likely to discontinue because of prolonged or heavy bleeding than women from other countries (7.0 versus 4.3%). The mean number of bleeding and spotting days per 90-day reference period was 7.3 and 10.4 days, respectively. One third of 90-day reference periods had fewer than three bleeding/spotting episodes; one fifth had no bleeding/spotting (amenorrhea); 17% had a bleeding episode that lasted more than 14 days, and 6% had more than five bleeding/spotting episodes. The number of unscheduled bleeding days was highest in the first 3 months of use, decreased during the first year of use, and then plateaued for the second and third years of use. However, this decrease may have resulted from patients discontinuing as a result of a bleeding irregularity, leaving for analysis those less likely to experience bleeding. Although amenorrhea occurs in approximately 20% of women in the first year of use, the rates of amenorrhea actually decline with duration of use to 13% by year 3.57
Women who experienced more days of bleeding were more likely to discontinue, especially if the bleeding was prolonged. For example, the mean number of bleeding/spotting days in women who discontinued and who continued implant use during a 90-day reference period was 45.2 and 16.5 days, respectively. Frequent or prolonged bleeding/spotting was reported in about 90% of women who discontinued the implant but in only 22% of those who continued its use.58
Management of irregular bleeding
Treatment of unscheduled bleeding is not necessary, but since bleeding disturbances are the principal cause of discontinuation, several approaches to their treatment have been used. For women who have no contraindications to estrogen, prolonged bleeding may be treated with a short course of oral estrogen: conjugated estrogens, 1.25 mg, or estradiol, 2 mg, administered daily for 7 days.59 An alternative approach is to administer an estrogen-progestin oral contraceptive for 1–3 months. Studies have also show some benefit with mifepristone, doxycycline and NSAIDs but estrogen is probably the most effective treatment. A pragmatic approach to the management of unscheduled bleeding is outlined in Table 4.58
Table 4 A pragmatic approach to manage unscheduled bleeding in women using implantable contraception. Adapted from Mansour et al.58 and Abdel-Aleem et al.59
Other side effects
The most common adverse events besides unscheduled bleeding that were deemed possibly, probably, or definitely related to the etonogestrel implant included headache (16%), weight gain (12%), acne (12%), breast tenderness (10%), emotional lability (6%) and abdominal pain (5%).16
The etonogestrel implant does not induce bone loss. In contrast, depot medroxyprogesterone acetate (DMPA), another progestin-only contraceptive that reduces estrogen levels, can decrease bone mineral density.
There is conflicting evidence about whether or not DMPA increases the risk of human immunodeficiency virus (HIV) acquisition and transmission compared to noncontraceptive users.60, 61 There is no evidence that other contraceptive progestins at lower doses, such as the etonogestrel implant, have similar effects.
A large epidemiologic study using registry data from Denmark did not find an increased risk of arterial events among 24,954 implant users compared with over 9 million nonusers of hormonal contraception.19 For thrombotic stroke, there were three events among users, incidence 12/100,000 person years, RR 0.88, 95% CI 0.28–2.72; for myocardial infarction, there were three events among users, incidence 12/100,000 person years, RR 2.14, 95% CI 0.69–6.65.
Sexually transmitted infections
Sexually active women are exposed to the risk of pregnancy as well as to the risk of sexually transmitted infections (STIs), such as HIV, hepatitis B, human papillomavirus, Chlamydia trachomatis, syphilis, and gonorrhea the sequelae of which may be life-threatening. Implantable contraceptives neither increase the risk of nor offer protection against STIs.62 Women counseled about contraception should also be informed about the risks of STIs. They should be advised that use of condoms concomitantly with an effective method of pregnancy prevention is the best means of protection against unintended pregnancy and STIs. It seems likely that the etonogestrel implant, like oral contraceptive pills and DMPA, reduces the risk of pelvic upper tract infection (PID), probably because of progestin effects on cervical mucus.
INITIATION
For healthy women, no physical examination or laboratory tests are indicated before insertion of a progestin implant.63 Although some medical conditions represent contraindications to hormone use,18 the low prevalence of these conditions in asymptomatic reproductive age women does not warrant screening for these conditions by physical examination or laboratory testing for the safe initiation of implants.
The possibility of early pregnancy can generally be assessed by review of the woman’s menstrual, sexual, and contraceptive history. The absence of pregnancy can be reasonably inferred if she meets any of the criteria in (Box 1). An appropriately timed pregnancy test (at least 2 weeks after the last episode of sex) can be obtained if pregnancy is uncertain. There is no evidence that the etonogestrel implant or other hormonal contraceptives have caused abnormal fetal development. Most of the few pregnancies reported among etonogestrel implant users were present before insertion. If these pregnancies are continued, implants should be removed, but if they are terminated implants can remain.
Box 1. How to be Reasonably Certain that a Woman is not Pregnant (Centers for Disease Control and Prevention US Selected Practice Recommendations for Contraceptive Use, 2013. Adapted from the World health Organization Selected practice Recomendations for Contraceptive Use, 2nd edn. MMWR;62(RR05):1-46. http://www.cdc.gov/mmwr/pdf/rr/rr62e0614.pdf (Accessed on September 23, 2014).)
The implant can be inserted at any time as long as the clinician is reasonably certain that the patient is not pregnant. Women who are postabortion (either medical or surgical) or postpartum can have the implant inserted immediately after termination of pregnancy or delivery.18
Back-up contraception
Abstinence or back-up contraception is suggested for the first 7 days after insertion if the implant is inserted more than 5 days since the beginning of the patient’s last menstrual period,64 although data to support this need are lacking.65 This conservative approach is recommended because changes in cervical mucus occur rapidly and are probably complete within 36 hours of insertion. Options for back-up contraception include use of condoms or continued use of the woman’s previous method of contraception. For women who are postpartum, not exclusively breastfeeding, and have not resumed menses, back-up contraception is suggested for those who are more than 3 weeks postpartum. For women who are postpartum, exclusively breastfeeding, and have not resumed menses, back-up contraception is suggested for those who are more than 6 months postpartum. For women who are postabortion, back-up contraception is suggested if the implant is not placed on the day of the abortion.
If the woman has been using an intrauterine device (IUD) and is switching to the implant, she may have residual sperm in her reproductive tract, which could result in fertilization and implantation if the IUD is removed. Options include:
- Advise the woman to retain the IUD for at least 7 days after the implant is inserted and then return for IUD removal.
- Advise the woman to abstain from sexual intercourse or use barrier contraception for 7 days before removing the IUD and switching to the implant. Back-up contraception is suggested if the implant is inserted more than 5 days since the beginning of the patient’s last menstrual period
- Advise the woman to use emergency contraception at the time of IUD removal and use back-up contraception if the implant is inserted more than 5 days since the beginning of the patient’s last menstrual period.
INSERTION
Insertion of contraceptive implants is a brief office procedure performed under local anesthesia. A clinician who has been trained in the technique can do it in less than 1 minute for Nexplanon66 and 2 minutes for Jadelle.36 The US Food and Drug Administration (FDA) and Nexplanon's maker, Merck, agreed that Implanon and Nexplanon would be distributed in the USA only to clinicians who have received 3 hours of training in patient selection, counseling, insertion, and removal. Those already trained for Implanon can take an online course to qualify for use of Nexplanon (www.nexplanon-usa.com). Questions regarding training can be answered at 1-877-467-5266 (USA). An FDA-mandated reporting system for adverse events has not revealed any unexpected problems with insertion or removal of Implanon or Nexplanon.
Required equipment for implant insertion
- A 25-gauge needle (1.5 inches in length) attached to a 2–5 mL syringe
- 1% chloroprocaine or lidocaine without epinephrine
- Antiseptic solution (e.g. povidone iodine, chlorhexidine gluconate, isopropyl alcohol)
- An adhesive strip for closure of the puncture site
- Elastic pressure bandage (e.g. "Kerlex")
- Surgical gloves (sterile for Jadelle, non-sterile for Nexplanon)
- Sterile drape
- For Nexplanon: Sterile, preloaded Nexplanon applicator
- For Jadelle: Sterile, disposible Jadelle trocar with the obturator in place and two Jadelle implants
Positioning the patient
Positioning the patient is the same when inserting Nexplanon and Jadelle or Sinoplant. The patient is placed in a supine position with the full length of her arm exposed. The manufacturer suggests positioning the upper inner arm by bending the elbow to 90 degrees and rotating the arm out. Some providers find the procedure is easier when the arm is extended, allowing full exposure of the insertion site at the crease between the biceps and triceps muscles. Adequate support under the arm should be provided to ensure comfort with, e.g., a thick book. An insertion site approximately four fingerbreadths superior and lateral to the medial epicondyle of the humerus is identified. The site should be at least 6 cm and no more than 10 cm from the medial epicondyle (Figure 2). The optimum site depends upon an individual woman’s anatomy, such as the length of the upper arm (avoid placing the end of the implant too near the axilla) and the area where the crease between the biceps and triceps muscles is clearest.
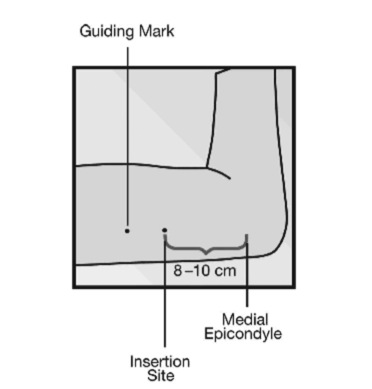 Figure 2 Insertion site in medial aspect of upper, nondominant, arm. (With permission from: NEXPLANON® image reproduced with permission of Merck Sharp & Dohme B.V., a subsidiary of Merck & Co., Inc., Whitehouse Station, New Jersey, USA. All rights reserved.)
Figure 2 Insertion site in medial aspect of upper, nondominant, arm. (With permission from: NEXPLANON® image reproduced with permission of Merck Sharp & Dohme B.V., a subsidiary of Merck & Co., Inc., Whitehouse Station, New Jersey, USA. All rights reserved.)
To minimize the risk of infection, strict aseptic technique should be maintained throughout the procedure, e.g. do not touch the trocar containing the implant. A sterile drape is placed under the arm, and the insertion site on the arm is cleaned with an antiseptic such as povidone-iodine.
Some clinicians mark the skin to help guide insertion. One mark is made where the rod(s) will be inserted and a second mark is made a few centimeters proximal to the first mark to serve as a direction guide during insertion. However, insertion directly through the marked skin should be avoided as it can result in "tattooing." Use of skin marks is at the clinician’s discretion.
Anesthesia
For Nexplanon, local anesthesia for the incision is obtained by raising a wheal of 1% chloroprocaine or lidocaine using a 1 ½ inch 25-gauge needle and injecting 1–3 mL under the skin along the track of the implant insertion needle. For Jadelle, infiltrate the skin with 2–4 mL 1% lidocaine with 1:100,000 epinephrine, ensuring it is placed just beneath the dermis in a “V” shape, creating two subdermal channels to aid in placement of the implants. A burning sensation is common during injection of the local anesthetic. This effect can be eliminated for most patients by adding 1 mEq of sodium bicarbonate to each 10 mL of anesthetic (however, this buffering shortens shelf life to 24 hours).67 A few minutes should be allowed for local anesthesia to take effect, and the insertion site should be tested prior to beginning the procedure to ensure that the patient is comfortable.
Insert implant
The operator should be seated and should view the insertion site from the side, not from above the device. Most women feel no more than a pressure sensation during the insertion procedure. The sharp, beveled trocar for both Nexplanon and Jadelle easily penetrates the skin, making a separate scalpel incision unnecessary.
For Nexplanon, grasp the applicator above the needle cap on its textured surface between thumb and forefinger. Remove the clear plastic needle cover. Place the needle against the insertion site holding the applicator at an angle 30 degrees to the skin (Figure 3). While applying counter traction to the skin around the insertion site, puncture the skin with the needle tip. Lower the applicator so that it is parallel to the skin and advance the needle in the subdermal connective tissue while lifting the skin with the tip of the needle. Advance the needle to its full length. If the needle is not fully advanced under the skin, the implant will not be correctly inserted. Unlock the slider with downward finger pressure on the lever, then move the slider fully backward (distally) and withdraw the needle.
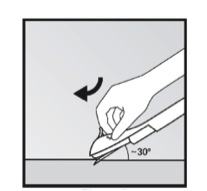 Figure 3 a Nexplanon one-handed, subdermal, pre-loaded inserter puncturing skin surface. (With permission from: NEXPLANON® image reproduced with permission of Merck Sharp & Dohme B.V., a subsidiary of Merck & Co., Inc., Whitehouse Station, New Jersey, USA. All rights reserved.)
Figure 3 a Nexplanon one-handed, subdermal, pre-loaded inserter puncturing skin surface. (With permission from: NEXPLANON® image reproduced with permission of Merck Sharp & Dohme B.V., a subsidiary of Merck & Co., Inc., Whitehouse Station, New Jersey, USA. All rights reserved.)
For Jadelle, pull apart the films of the pouch to drop the two implants on a sterile cloth. Jadelle implants should always be handled with sterile gloves or forceps. The trocar has two marks along the length of the barrel to guide the placement of the implants. The first mark is close to the bevel and indicates how far the trocar should be retracted before redirecting it for placement of the second implant. The second mark is close to the hub and indicates the distance the trocar must be inserted under the dermis before loading the implants for placement. Insert the trocar with the obturator in place, bevel side up, to the second mark by pointing slightly upwards, tenting the skin to stay in the subdermal plan. Remove the obturator and load the implant into the trocar (with either sterile forceps or sterile gloves), then gently replace the obturator until resistance is felt. Retract the trocar to the first mark while holding the obturator stationary to deposit the implant in the subdermal space the proper distance from the insertion site. Redirect the trocar at an angle 15 degrees from the first implant and repeat this procedure for placement the second implant to form a “V” shape. After removing the trocar, place a finger over the incision and gently palpate the implants to document their location and ensure that their tips are at least 5 mm from the incision site. A video of Jadelle insertion can be seen at: https://www.k4health.org/sites/default/files/Animation%20Intro_1.mp4
Verify placement
Immediately after insertion, palpate the skin to verify correct placement of the rod; both ends of the implant(s) should be palpable. Ask the patient to feel her implant(s), then place an adhesive closure on the insertion puncture and wrap the site with a pressure bandage to minimize bruising. If you cannot feel the implant(s), check the applicator to make sure the implant is no longer in the applicator. The Nexplanon applicator obturator is purple, while the implant is white. If there is doubt about the presence of the implant(s), use sonography or an x-ray to determine its presence. Magnetic resonance imaging (MRI) is not required.
Postinsertion care and follow-up
Complete the Patient Chart Label for the patient's medical record and the User Card, which must be given to the patient. The woman may remove the pressure bandage in 24 hours and the skin closure in 3 days. Most women do not experience pain after insertion, but if it occurs, aspirin, acetaminophen, or nonsteroidal anti-inflammatory agents usually provide relief. The patient may be discharged immediately after the procedure. A routine follow-up visit is not necessary.68 She should call the provider if she develops pain, discharge, or swelling at the insertion site, fever, or other concerns. She should also contact her provider if she has a change in her health status that could affect safe and effective use of this method, or when she wants to switch contraception methods, remove the implant to attempt pregnancy, or replace the implant when efficacy wanes.
Complications of insertion
Complications are rare, reported in 0.3–1% of insertions and 0.2–1.7% of removals.69, 70 Potential complications include infection, hematoma formation, local irritation or rash, expulsion, and allergic reactions. The implant may migrate a short distance (less than 2 cm) over time.71 The incidence of complications is minimized by clinician training and experience, and the use of strict aseptic technique. Nerve injury can result in impaired sensibility, severe localized pain, or the formation of painful neuroma. There are two case reports of neurologic symptoms during etonogestrel implant insertion in the literature: nerve injury to branches of the medial antebrachial cutaneous nerve during placement 72 and neuropathy due to contact of the implant with the medial antebrachial cutaneous nerve.73
REMOVAL
The rod can be removed at any time, but should be removed when efficacy begins to decline (3 years after insertion according to the package insert; 5 years according to WHO studies). The hormonal effects end promptly after removal; circulating levels of etonogestrel are undetectable within 1 week. Return of ovulation occurs in 94% of women within 3–6 weeks after method discontinuation.40, 41, If the implant is not removed at 3 years, contraceptive effects persist for at least an additional 2 years.44
Implant removal is an office procedure requiring only local anesthesia. Equipment is the same as that listed above for insertion, except the applicator is replaced by sterile mosquito forceps (curved and straight) and a #11 scalpel. For removing deeply inserted implants, modified (<2 mm diameter ring) vasectomy forceps can be useful. Removal time averages 4.5 minutes for Jadelle, 4 minutes for Implanon36, 74 and 2 minutes for Nexplanon.75 Fibrous tissue surrounding Nexplanon is rare (4%) but increases removal time.74, 75 We recommend viewing an instructional video (one for Nexplanon may be found via the up to date article “Etonogestrel contraceptive implant” and one for Jadelle at https://www.k4health.org/sites/default/files/Animation%20Removal_1.mp4 ),76 and practicing removal on a model arm before attempting the procedure on a patient. A removal kit containing a model arm and a manual and compact disc illustrating basic technique is available at no charge from Merck (by calling 877-467-5266). The patient should read and sign an informed consent, which should be filed in her medical record. We suggest that the patient also be given a copy.
Procedure
Position the patient and prepare the implant site as described above for rod insertion. We prefer to have the patient extend her arm for the insertion procedure but bend her arm for implant removal.
Palpate the distal tip of the rod (the end closest to the elbow). If it is not palpable, then removal should be postponed until the rod can be localized with sonography or x-ray imaging. Push down on the proximal end of the rod (the end closest to the axilla) and inject no more than 0.5 mL of buffered lidocaine with epinephrine into the dermis immediately under the elevated distal tip of the rod, raising a wheal about 5 mm in diameter. Too much anesthetic, especially if it is injected on top of the rod, makes it difficult to palpate the tip of the rod. Massage this area to disperse the anesthetic.
Use your fingers to again apply pressure on the proximal (axillary) end of the rod so that the distal (elbow) end pushes up against the skin. As the rod is pushed against the skin, the blade of a #11 scalpel is positioned so that the point is immediately available to incise the sheath without releasing pressure on the rod. It is best to keep the scalpel in one hand with thumb and index finger while manipulating the rod with the rest of the fingers of both hands. Pushing the rod against the incision with finger pressure is critical for success with this "Pop Out" technique because, if pressure is released, the rod will slip back into its sheath in the subdermal tissue.
Make a 2–3 mm longitudinal incision through the skin over the end of the rod. Deepen the incision until you feel a rubbery sensation against the point of the #11 scalpel blade; this is the rod encased in its fibrous sheath. Nick the fibrous sheath covering the end of the rod with the tip of the scalpel blade. It may take several nicks in different directions to fully open the sheath.
The end of the rod will come into view as the sheath is opened. Continue to exert finger pressure on the proximal (axillary) end of the rod to push the distal (elbow) end through the incision until it can be grasped with mosquito forceps and pulled out. Confirm that all 40 mm of the rod have been removed. For the two-implant and six-implant systems, repeat as necessary through the same incision. Close the incision with an adhesive strip (e.g. butterfly bandage or “Steri Strip”) and cover with a pressure bandage to minimize bruising.
Alternatively, a “fingers only” technique can be used to remove both the one-implant (Nexplanon) and two-implant (Jadelle) systems. After positioning the patient’s arm and creating a sterile field as described previously, inject no more than 0.5 mL of local anesthetic directly at the tip of the implant. Make a 2–3-mm incision directly at the proximal tip of the most centrally located implants. Manipulate the implant tip into the incision with finger pressure until the fibrous sheath is visible. Maintaining this finger pressure on the implant with one hand to keep its tip visible in the incision, nick the sheath at the tip of the capsule with a No. 11 scalpel. Once the sheath is opened, simply squeeze out the implant. For the two-implant system, repeat this procedure to remove the second implant through the single incision. For six implants, a combination of fingers and instruments is often most efficient. A video demonstrating fingers only removal is available at: http://www.screenr.com/MS7N.
Difficult removals
If the rod will not move toward the incision with finger pressure, it can be grasped with a hemostat or modified (filed down to a 2 mm diameter grasping ring) vasectomy forceps, but the incision will usually have to be lengthened in order to admit the clamp (Figure 4). It may be necessary to inject more local anesthetic, and to dissect around the rod with a straight mosquito clamp. The disadvantage of instrument removal is that it can be more painful, cause more bleeding, require a larger incision, and increase the risk of breaking the rod.
Figure 4 Removal of contraceptive implant by grasping its tip with mosquito clamp and exposing implant by moving handle of clamp toward patient’s shoulder. (With permission from: Speroff L, Darney, PD., 2010. A Clinical Guide for Contraception. 5th edn. Baltimore, MD: Lippincott, Williams & Wilkins.)
Once a rod is damaged, it can fracture with further attempts to grasp it with clamps. To decrease this risk, the rod should be grasped by its end whenever possible and with as little traction as possible for exposure and removal.
If it is not possible to grasp and push up on the end of a deeply implanted rod to open the fibrous sheath, use a scalpel to cut longitudinally, not across, the sheath covering the rod. Rarely, removal of a cut or broken rod will require an additional incision at the proximal end of the rod so that the remaining piece can be extracted. When the rod must be grasped around its diameter, rather than at the end, the vasectomy forceps are particularly useful.
Rods too deeply placed cannot be palpated under the skin, but can be seen with imaging studies (Implanon can be identified with high resolution sonography or magnetic resonance imaging [MRI]; Nexplanon can be identified with high resolution sonography, plain X-ray, computed tomography, or MRI). Such "lost" rods should be located with a high frequency (10–15 mHz), short focus, linear ultrasound transducer prior to attempting the removal, as their locations may vary.77, 78, 79, 80 Use a transverse orientation to identify an acoustic shadow (the rod itself is more difficult to see), measure the depth, and draw a line representing the rod location on the surface of the skin. A thin wire (e.g. an opened paper clip), held under the transducer may be used to help mark the skin surface in relation to the impalpable rod. If the rod is very deep (>1.5–2 cm), sonography should be used during the removal procedure because movement of the patient’s arm may change the location of skin marks in relation to the underlying implant.
Patients with “very” (>2 cm) deep implants (as determined sonographically) should be referred to a clinician experienced in challenging implant removals. The contraceptive specialist can then work with interventional radiologists to remove the implant under direct imaging and controlled conditions. A case series of implant removal with a hook-wire marker method used in breast tumor surgery has been proposed.81
Removal of contraceptive implants is never an emergency; there is no evidence that their presence adversely affects pregnancies or other conditions. Therefore, we suggest waiting until removal can be performed by someone with expertise in removal of difficult contraceptive implants. Consultation with an orthopedic or plastic surgeon without specific expertise managing this problem is rarely required and not advised.
REINSERTION
If the patient wants to continue to use implant contraception, a new rod can be inserted immediately through the same incision that was used to remove the old rod. Alternatively, the new implant can be placed in the other arm.
SUMMARY
Implants offer women a highly effective, long-term and easy to use method of contraception. They may be used in most women, including women with contraindications to estrogen, adolescents, women with chronic illnesses and breastfeeding women. Implantable contraception is safe and cost-effective immediately postabortion and postpartum. Providers interested in placing and removing implants should undergo appropriate training, but all providers counseling women about contraception should offer implantable contraception as a highly-effective, first-line method.
REFERENCES
MEIRIK, O., FRASER, I.S., D'ARCANGUES, C. and WHO CONSULTATION ON IMPLANTABLE CONTRACEPTIVES FOR WOMEN, 2003. Implantable contraceptives for women. Human reproduction update, 9(1), pp. 49-59. |
|
SIVIN, I., MISHELL, D.R.,Jr, DARNEY, P., WAN, L. and CHRIST, M., 1998. Levonorgestrel capsule implants in the United States: a 5-year study. Obstetrics and gynecology, 92(3), pp. 337-344. |
|
KUIPER, H., MILLER, S., MARTINEZ, E., LOEB, L. and DARNEY, P., 1997. Urban adolescent females' views on the implant and contraceptive decision-making: a double paradox. Family planning perspectives, 29(4), pp. 167-172. |
|
BRACHE, V., FAUNDES, A., ALVAREZ, F. and GARCIA, A.G., 2006. Transition from Norplant to Jadelle in a clinic with extensive experience providing contraceptive implants. Contraception, 73(4), pp. 364-367. |
|
STEINER, M.J., BOLER, T., OBHAI, G. and HUBACHER, D., 2010. Assessment of a disposable trocar for insertion of contraceptive implants. Contraception, 81(2), pp. 140-142. |
|
STEINER, M.J., LOPEZ, L.M., GRIMES, D.A., CHENG, L., SHELTON, J., TRUSSELL, J., FARLEY, T.M. and DORFLINGER, L., 2010. Sino-implant (II)--a levonorgestrel-releasing two-rod implant: systematic review of the randomized controlled trials. Contraception, 81(3), pp. 197-201. |
|
HEIKINHEIMO, O., RANTA, S., MOO-YOUNG, A., LAHTEENMAKI, P. and GORDON, K., 1999. Parenteral administration of progestin Nestorone to lactating cynomolgus monkeys: an ideal hormonal contraceptive at lactation? Human reproduction (Oxford, England), 14(8), pp. 1993-1997. |
|
LAHTEENMAKI, P.L., DIAZ, S., MIRANDA, P., CROXATTO, H. and LAHTEENMAKI, P., 1990. Milk and plasma concentrations of the progestin ST-1435 in women treated parenterally with ST-1435. Contraception, 42(5), pp. 555-562. |
|
SIVIN, I., MISHELL, D.R.,Jr, DIAZ, S., BISWAS, A., ALVAREZ, F., DARNEY, P., HOLMA, P., WAN, L., BRACHE, V., KIRIWAT, O., ABDALLA, K., CAMPODONICO, I., PASQUALE, S., PAVEZ, M. and SCHECHTER, J., 2000. Prolonged effectiveness of Norplant(R) capsule implants: a 7-year study. Contraception, 61(3), pp. 187-194. |
|
DUNSON, T.R., AMATYA, R.N. and KRUEGER, S.L., 1995. Complications and risk factors associated with the removal of Norplant implants. Obstetrics and gynecology, 85(4), pp. 543-548. |
|
MECKSTROTH, K.R. and DARNEY, P.D., 2001. Implant contraception. Seminars in reproductive medicine, 19(4), pp. 339-354. |
|
United States Medical Eligibility Criteria (US MEC) for Contraceptive Use, 2010. Available: http://www.cdc.gov/reproductivehealth/unintendedpregnancy/USMEC.htm [July 3, 2013]. |
|
HEINEMANN, L.A., ASSMANN, A., DOMINH, T. and GARBE, E., 1999. Oral progestogen-only contraceptives and cardiovascular risk: results from the Transnational Study on Oral Contraceptives and the Health of Young Women. The European journal of contraception & reproductive health care : the official journal of the European Society of Contraception, 4(2), pp. 67-73. |
|
GOMES, M.P. and DEITCHER, S.R., 2004. Risk of venous thromboembolic disease associated with hormonal contraceptives and hormone replacement therapy: a clinical review. Archives of Internal Medicine, 164(18), pp. 1965-1976. |
|
Cardiovascular disease and use of oral and injectable progestogen-only contraceptives and combined injectable contraceptives. Results of an international, multicenter, case-control study. World Health Organization Collaborative Study of Cardiovascular Disease and Steroid Hormone Contraception. 1998. Contraception, 57(5), pp. 315-324. |
|
DARNEY, P., PATEL, A., ROSEN, K., SHAPIRO, L.S. and KAUNITZ, A.M., 2009. Safety and efficacy of a single-rod etonogestrel implant (Implanon): results from 11 international clinical trials. Fertility and sterility, 91(5), pp. 1646-1653. |
|
ACOG COMMITTEE ON PRACTICE BULLETINS-GYNECOLOGY, 2006. ACOG practice bulletin. No. 73: Use of hormonal contraception in women with coexisting medical conditions. Obstetrics and gynecology, 107(6), pp. 1453-1472. |
|
WHO Medical eligibility criteria for contraceptive use. Fourth edition, 2009. Available at http://whqlibdoc.who.int/publications/2010/9789241563888_eng.pdf. |
|
LIDEGAARD, O., LOKKEGAARD, E., JENSEN, A., SKOVLUND, C.W. and KEIDING, N., 2012. Thrombotic stroke and myocardial infarction with hormonal contraception. The New England journal of medicine, 366(24), pp. 2257-2266. |
|
HENNESSY, S., BERLIN, J.A., KINMAN, J.L., MARGOLIS, D.J., MARCUS, S.M. and STROM, B.L., 2001. Risk of venous thromboembolism from oral contraceptives containing gestodene and desogestrel versus levonorgestrel: a meta-analysis and formal sensitivity analysis. Contraception, 64(2), pp. 125-133. |
|
DORFLINGER, L.J., 2002. Metabolic effects of implantable steroid contraceptives for women. Contraception, 65(1), pp. 47-62. |
|
SUHERMAN, S.K., AFFANDI, B. and KORVER, T., 1999. The effects of Implanon on lipid metabolism in comparison with Norplant. Contraception, 60(5), pp. 281-287. |
|
REINPRAYOON, D., TANEEPANICHSKUL, S., BUNYAVEJCHEVIN, S., THAITHUMYANON, P., PUNNAHITANANDA, S., TOSUKHOWONG, P., MACHIELSEN, C. and VAN BEEK, A., 2000. Effects of the etonogestrel-releasing contraceptive implant (Implanon on parameters of breastfeeding compared to those of an intrauterine device. Contraception, 62(5), pp. 239-246. |
|
BRITO, M.B., FERRIANI, R.A., QUINTANA, S.M., YAZLLE, M.E., SILVA DE SA, M.F. and VIEIRA, C.S., 2009. Safety of the etonogestrel-releasing implant during the immediate postpartum period: a pilot study. Contraception, 80(6), pp. 519-526. |
|
GURTCHEFF, S.E., TUROK, D.K., STODDARD, G., MURPHY, P.A., GIBSON, M. and JONES, K.P., 2011. Lactogenesis after early postpartum use of the contraceptive implant: a randomized controlled trial. Obstetrics and gynecology, 117(5), pp. 1114-1121. |
|
LOPEZ, L.M., GREY, T.W., STUEBE, A.M., CHEN, M., TRUITT, S.T. and GALLO, M.F., 2015. Combined hormonal versus nonhormonal versus progestin-only contraception in lactation. The Cochrane database of systematic reviews, 3, pp. CD003988. |
|
HAN, L., TEAL, S.B., SHEEDER, J. and TOCCE, K., 2014. Preventing repeat pregnancy in adolescents: is immediate postpartum insertion of the contraceptive implant cost effective? American Journal of Obstetrics and Gynecology, 211(1), pp. 24.e1-24.e7. |
|
ABMA, J.C., MARTINEZ, G.M. and COPEN, C.E., 2010. Teenagers in the United States: sexual activity, contraceptive use, and childbearing, national survey of family growth 2006-2008. Vital and health statistics.Series 23, Data from the National Survey of Family Growth, (30)(30), pp. 1-47. |
|
MESTAD, R., SECURA, G., ALLSWORTH, J.E., MADDEN, T., ZHAO, Q. and PEIPERT, J.F., 2011. Acceptance of long-acting reversible contraceptive methods by adolescent participants in the Contraceptive CHOICE Project. Elsevier. |
|
GUAZZELLI, C.A., DE QUEIROZ, F.T., BARBIERI, M., TORLONI, M.R. and DE ARAUJO, F.F., 2010. Etonogestrel implant in postpartum adolescents: bleeding pattern, efficacy and discontinuation rate. Contraception, 82(3), pp. 256-259. |
|
COMMITTEE ON ADOLESCENT HEALTH CARE LONG-ACTING REVERSIBLE CONTRACEPTION WORKING GROUP, THE AMERICAN COLLEGE OF OBSTETRICIANS AND GYNECOLOGISTS, 2012. Committee opinion no. 539: adolescents and long-acting reversible contraception: implants and intrauterine devices. Obstetrics and gynecology, 120(4), pp. 983-988. |
|
MOSHER, W.D. and JONES, J., 2010. Use of contraception in the United States: 1982-2008. Vital and health statistics.Series 23, Data from the National Survey of Family Growth, (29)(29), pp. 1-44. |
|
FINER, L.B., JERMAN, J. and KAVANAUGH, M.L., 2012. Changes in use of long-acting contraceptive methods in the United States, 2007-2009. Fertility and sterility, 98(4), pp. 893-897. |
|
SIVIN, I., LAHTEENMAKI, P., RANTA, S., DARNEY, P., KLAISLE, C., WAN, L., MISHELL, D.R.,Jr, LACARRA, M., VIEGAS, O.A., BILHAREUS, P., KOETSAWANG, S., PIYA-ANANT, M., DIAZ, S., PAVEZ, M., ALVAREZ, F., BRACHE, V., LAGUARDIA, K., NASH, H. and STERN, J., 1997. Levonorgestrel concentrations during use of levonorgestrel rod (LNG ROD) implants. Contraception, 55(2), pp. 81-85. |
|
SIVIN, I., ALVAREZ, F., MISHELL, D.R.,Jr, DARNEY, P., WAN, L., BRACHE, V., LACARRA, M., KLAISLE, C. and STERN, J., 1998. Contraception with two levonorgestrel rod implants. A 5-year study in the United States and Dominican Republic. Contraception, 58(5), pp. 275-282. |
|
WAN, L.S., STIBER, A. and LAM, L.Y., 2003. The levonorgestrel two-rod implant for long-acting contraception: 10 years of clinical experience. Obstetrics and gynecology, 102(1), pp. 24-26. |
|
ROBERTSON, D.N., SIVIN, I., NASH, H.A., BRAUN, J. and DINH, J., 1983. Release rates of levonorgestrel from Silastic capsules, homogeneous rods and covered rods in humans. Contraception, 27(5), pp. 483-495. |
|
ORME, M.L., BACK, D.J. and BRECKENRIDGE, A.M., 1983. Clinical pharmacokinetics of oral contraceptive steroids. Clinical pharmacokinetics, 8(2), pp. 95-136. |
|
WENZL, R., VAN BEEK, A., SCHNABEL, P. and HUBER, J., 1998. Pharmacokinetics of etonogestrel released from the contraceptive implant Implanon. Contraception, 58(5), pp. 283-288. |
|
MAKARAINEN, L., VAN BEEK, A., TUOMIVAARA, L., ASPLUND, B. and COELINGH BENNINK, H., 1998. Ovarian function during the use of a single contraceptive implant: Implanon compared with Norplant. Fertility and sterility, 69(4), pp. 714-721. |
|
CROXATTO, H.B. and MAKARAINEN, L., 1998. The pharmacodynamics and efficacy of Implanon. An overview of the data. Contraception, 58(6 Suppl), pp. 91S-97S. |
|
VARMA, R. and MASCARENHAS, L., 2001. Endometrial effects of etonogestrel (Implanon) contraceptive implant. Current opinion in obstetrics & gynecology, 13(3), pp. 335-341. |
|
TRUSSELL, J., 2011. Contraceptive failure in the United States. Contraception, 83(5), pp. 397-404. |
|
BAHAMONDES, L., 2014. Three years follow up: Multicentre randomised clinical trial of two implantable contraceptives for women, Jadelle and Implanon. |
|
BOUQUIER, J., FULDA, V., BATS, A.S., LECURU, F. and HUCHON, C., 2012. A life-threatening ectopic pregnancy with etonogestrel implant. Contraception, 85(2), pp. 215-217. |
|
MCNICHOLAS, C., MADDIPATI, R., ZHAO, Q., SWOR, E. and PEIPERT, J.F., 2015. Use of the Etonogestrel Implant and Levonorgestrel Intrauterine Device Beyond the U.S. Food and Drug Administration's Approved Duration. Obstetrics & Gynecology, 125(3),. |
|
LEVINE, J.P., SINOFSKY, F.E., CHRIST, M.F. and IMPLANON US STUDY GROUP, 2008. Assessment of Implanon insertion and removal. Contraception, 78(5), pp. 409-417. |
|
LANGE, J., TEAL, S. and TOCCE, K., 2014. Decreased efficacy of an etonogestrel implant in a woman on antiepileptic medications: a case report. Journal of medical case reports, 8, pp. 43-1947-8-43. |
|
LETICEE, N., VIARD, J.P., YAMGNANE, A., KARMOCHKINE, M. and BENACHI, A., 2012. Contraceptive failure of etonogestrel implant in patients treated with antiretrovirals including efavirenz. Contraception, 85(4), pp. 425-427. |
|
LAKHI, N. and GOVIND, A., 2010. Implanon failure in patients on antiretroviral medication: the importance of disclosure. The journal of family planning and reproductive health care / Faculty of Family Planning & Reproductive Health Care, Royal College of Obstetricians & Gynaecologists, 36(3), pp. 181-182. |
|
MATILUKO, A.A., SOUNDARARJAN, L. and HOGSTON, P., 2007. Early contraceptive failure of Implanon in an HIV-seropositive patient on triple antiretroviral therapy with zidovudine, lamivudine and efavirenz. The journal of family planning and reproductive health care / Faculty of Family Planning & Reproductive Health Care, Royal College of Obstetricians & Gynaecologists, 33(4), pp. 277-278. |
|
MCCARTY, E.J., KEANE, H., QUINN, K. and QUAH, S., 2011. Implanon(R) failure in an HIV-positive woman on antiretroviral therapy resulting in two ectopic pregnancies. International Journal of STD & AIDS, 22(7), pp. 413-414. |
|
VIEIRA, C.S., BAHAMONDES, M.V., DE SOUZA, R.M., BRITO, M.B., ROCHA PRANDINI, T.R., AMARAL, E., BAHAMONDES, L., DUARTE, G., QUINTANA, S.M., SCARANARI, C. and FERRIANI, R.A., 2014. Effect of antiretroviral therapy including lopinavir/ritonavir or efavirenz on etonogestrel-releasing implant pharmacokinetics in HIV-positive women. Journal of acquired immune deficiency syndromes (1999), 66(4), pp. 378-385. |
|
SCARSI, K., LAMORDE, M., DARIN, K., PENCHALA, S.D., ELSE, L., NAKALEMA, S., BYAKIKA-KIBWIKA, P., KHOO, S., COHN, S., MERRY, C. and BACK, D., 2014. Efavirenz- but not nevirapine-based antiretroviral therapy decreases exposure to the levonorgestrel released from a sub-dermal contraceptive implant. Journal of the International AIDS Society, 17(4 Suppl 3), pp. 19484. |
|
PERRY, S.H., SWAMY, P., PREIDIS, G.A., MWANYUMBA, A., MOTSA, N. and SARERO, H.N., 2014. Implementing the Jadelle implant for women living with HIV in a resource-limited setting: concerns for drug interactions leading to unintended pregnancies. AIDS (London, England), 28(5), pp. 791-793. |
|
TODD, C.S., DEESE, J., WANG, M., HUBACHER, D., STEINER, M.J., OTUNGA, S., VAN DAMME, L. and FEM-PREP STUDY GROUP, 2015. Sino-implant (II)(R) continuation and effect of concomitant tenofovir disoproxil fumarate-emtricitabine use on plasma levonorgestrel concentrations among women in Bondo, Kenya. Contraception, 91(3), pp. 248-252. |
|
ADAMS, K. and BEAL, M.W., 2009. Implanon: a review of the literature with recommendations for clinical management. Journal of midwifery & women's health, 54(2), pp. 142-149. |
|
MANSOUR, D., BAHAMONDES, L., CRITCHLEY, H., DARNEY, P. and FRASER, I.S., 2011. The management of unacceptable bleeding patterns in etonogestrel-releasing contraceptive implant users. Contraception, 83(3), pp. 202-210. |
|
ABDEL-ALEEM, H., D'ARCANGUES, C., VOGELSONG, K.M., GAFFIELD, M.L. and GULMEZOGLU, A.M., 2013. Treatment of vaginal bleeding irregularities induced by progestin only contraceptives. The Cochrane database of systematic reviews, 10, pp. CD003449. |
|
HEFFRON, R., DONNELL, D., REES, H., CELUM, C., MUGO, N., WERE, E., DE BRUYN, G., NAKKU-JOLOBA, E., NGURE, K., KIARIE, J., COOMBS, R.W., BAETEN, J.M. and PARTNERS IN PREVENTION HSV/HIV TRANSMISSION STUDY TEAM, 2012. Use of hormonal contraceptives and risk of HIV-1 transmission: a prospective cohort study. The Lancet.Infectious diseases, 12(1), pp. 19-26. |
|
WHO technical statement: Hormonal Contraception and HIV. February 16, 2012. Available: http://www.who.int/reproductivehealth/publications/family_planning/rhr_12_8/en/. |
|
DARNEY, P.D., CALLEGARI, L.S., SWIFT, A., ATKINSON, E.S. and ROBERT, A.M., 1999. Condom practices of urban teens using Norplant contraceptive implants, oral contraceptives, and condoms for contraception. American Journal of Obstetrics and Gynecology, 180(4), pp. 929-937. |
|
US Selected Practice Recommendations for Contraceptive Use, 2013. http://www.cdc.gov/mmwr/pdf/rr/rr62e0614.pdf (Accessed on March 23, 201 |
|
(United States Medical Eligibility Criteria (US MEC) for Contraceptive Use, 2010, US Selected Practice Recommendations for Contraceptive Use, 2013. http://www.cdc.gov/mmwr/pdf/rr/rr62e0614.pdf (Accessed on March 23, 2015) |
|
FOLGER, S.G., JAMIESON, D.J., GODFREY, E.M., ZAPATA, L.B. and CURTIS, K.M., 2013. Evidence-based guidance on selected practice recommendations for contraceptive use: identification of research gaps. Elsevier. |
|
MANSOUR, D., MOMMERS, E., TEEDE, H., SOLLIE-ERIKSEN, B., GRAESSLIN, O., AHRENDT, H.J. and GEMZELL-DANIELSSON, K., 2010. Clinician satisfaction and insertion characteristics of a new applicator to insert radiopaque Implanon: an open-label, noncontrolled, multicenter trial. Contraception, 82(3), pp. 243-249. |
|
NELSON, A.L., 1995. Neutralizing pH of lidocaine reduces pain during Norplant system insertion procedure. Contraception, 51(5), pp. 299-301. |
|
(US Selected Practice Recommendations for Contraceptive Use, 2013. http://www.cdc.gov/mmwr/pdf/rr/rr62e0614.pdf (Accessed on March 23, 2015) |
|
BENSOUDA-GRIMALDI, L., JONVILLE-BERA, A.P., BEAU-SALINAS, F., LLABRES, S., AUTRET-LECA, E. and LE RESEAU DES CENTRES REGIONAUX DE PHARMACOVIGILANCE, 2005. Insertion problems, removal problems, and contraception failures with Implanon. Gynecologie, obstetrique & fertilite, 33(12), pp. 986-990. |
|
MASCARENHAS, L., 2000. Insertion and removal of Implanon: practical considerations. The European journal of contraception & reproductive health care : the official journal of the European Society of Contraception, 5 Suppl 2, pp. 29-34. |
|
ISMAIL, H., MANSOUR, D. and SINGH, M., 2006. Migration of Implanon. The journal of family planning and reproductive health care / Faculty of Family Planning & Reproductive Health Care, Royal College of Obstetricians & Gynaecologists, 32(3), pp. 157-159. |
|
WECHSELBERGER, G., WOLFRAM, D., PULZL, P., SOELDER, E. and SCHOELLER, T., 2006. Nerve injury caused by removal of an implantable hormonal contraceptive. American Journal of Obstetrics and Gynecology, 195(1), pp. 323-326. |
|
BROWN, M. and BRITTON, J., 2012. Neuropathy associated with etonogestrel implant insertion. Elsevier. |
|
LEVINE, J.P., SINOFSKY, F.E., CHRIST, M.F. and IMPLANON US STUDY GROUP, 2008. Assessment of Implanon insertion and removal. Contraception, 78(5), pp. 409-417. |
|
MOMMERS, E., BLUM, G.F., GENT, T.G., PETERS, K.P., SORDAL, T.S. and MARINTCHEVA-PETROVA, M., 2012. Nexplanon, a radiopaque etonogestrel implant in combination with a next-generation applicator: 3-year results of a noncomparative multicenter trial. American Journal of Obstetrics and Gynecology, 207(5), pp. 388.e1-388.e6. |
|
DARNEY, P., Etonogestrel contraceptive implant. In UpToDate, Post TW (Ed), UpToDate, Waltham, MA. (Accessed on September 13, 2014.). |
|
SINGH, M., MANSOUR, D. and RICHARDSON, D., 2006. Location and removal of non-palpable Implanon implants with the aid of ultrasound guidance. The journal of family planning and reproductive health care / Faculty of Family Planning & Reproductive Health Care, Royal College of Obstetricians & Gynaecologists, 32(3), pp. 153-156. |
|
JAMES, P. and TRENERY, J., 2006. Ultrasound localisation and removal of non-palpable Implanon implants. The Australian & New Zealand Journal of Obstetrics & Gynaecology, 46(3), pp. 225-228. |
|
SINGH, M., MANSOUR, D. and RICHARDSON, D., 2006. Location and removal of non-palpable Implanon implants with the aid of ultrasound guidance. The journal of family planning and reproductive health care / Faculty of Family Planning & Reproductive Health Care, Royal College of Obstetricians & Gynaecologists, 32(3), pp. 153-156. |
|
BUITRON-GARCIA-F, R., OROPEZA-RECHY, G., GONZALEZ-DE LA CRUZ, J. and LARA-RICALDE, R., 2014. Complex location of a single rod contraceptive implant. Ginecologia y obstetricia de Mexico, 82(10), pp. 666-671. |
|
NOURI, K., PINKER-DOMENIG, K., OTT, J., FRASER, I. and EGARTER, C., 2013. Removal of non-palpable Implanon(R) with the aid of a hook-wire marker. Contraception, 88(4), pp. 577-580. |
|
TRUSSELL, J., 2011. Contraceptive failure in the United States. Contraception, 83(5), pp. 397-404. |