Laparoscopic Sterilization: Clinical Aspects
Authors
INTRODUCTION
The 1990 Bulletin of the World Health Organization (WHO) published data suggesting that approximately 223 million women worldwide rely on surgical sterilization as means of permanent contraception.1 Tubal sterilization was the most common method of contraception used by married and formerly married women in the United States by the year 1988.2 Furthermore by 1990 more women in the United States had undergone tubal ligation than those using oral contraceptive methods.3 By 1995, almost 30% of women in the United States using contraception relied on tubal sterilization.4 However, more recently there has been a reduction in the reliance on tubal sterilization for contraception. In Canada, contraceptive use has changed considerably over the past decade with a linear decline on the reliance on female sterilization (Table 1).5
Table 1. Methods of contraception currently used by Canadian women who have had intercourse.
Method | Percent |
| Oral contraceptives | 32 |
| Barrier | 21 |
| Male sterilization | 15 |
| Female sterilization | 8 |
| other | 11 |
(adapted from Canadian Contraception Consensus. The Society of Obstetricians and Gynecologists of Canada. J Soc Obstet Gynaecol Can. 2004: 26(2); 143-56.)
Laparoscopic tubal ligation provides women access to safe, effective, and dependable methods of tubal sterilization. In well-trained hands, laparoscopic tubal sterilization may be performed under either general or local anesthesia. In the latter case, aside from the need to enter the peritoneal cavity, the procedure is virtually comparable to a vasectomy with respect to ease of performance, safety, and efficacy. More recently, hysteroscopic sterilization has enabled female sterilization without requiring access into the peritoneal cavity. Thus, a couple may choose either the woman or her partner to undergo a sterilization procedure by one of several methods.
Hysteroscopic sterilization offers a further advance in minimal access surgery. It does not require any surgical incisions, does not require access into the peritoneal cavity and commonly does not require a general anesthetic. Furthermore, postoperative pain tends to be minimized and resumption of normal activities is rapid. Development of an effective transcervical method of sterilization has proven elusive until recently. An expanding micro insert placed under hysteroscopic guidance into the proximal portion of the fallopian tube has been developed for occlusion of the fallopian tubes (Essure Permanent Birth Control System, Conceptus Inc.) This method of hysteroscopic sterilization was approved for clinical use by the United States Food and Drug Administration (FDA) in 2002 and currently remains the only method currently approved by the FDA.6, 7 Several other systems are presently undergoing clinical trials and likely will become available for use soon.
While the transcervical offers several advantages, health professionals require special training to perform this technique and women must use additional contraception for at least 3 months before relying on the occlusive effect of this method. Therefore, at the present time laparoscopic sterilization remains the preferred option for most women undergoing permanent contraception. At the same time that we stress the relatively innocuous nature of laparoscopic sterilization, we also stress the seriousness of the decision to undergo sterilization, since for either partner the procedure should be considered a permanent and irreversible one.
WHO?
Any woman requesting sterilization should be given the opportunity to opt for the procedure, provided that she has been adequately counseled and informed preoperatively. She should not, under any circumstances, be coerced or pressured in any way into making such a significant and permanent decision. Of her own accord, she must be convinced and comfortable with her decision. The role of the physician or counselor is, therefore, to ascertain the following:
- Is the patient well informed in all aspects of the procedure, including the risks and benefits?
- Is she making the request and formulating her decision voluntarily and rationally?
- Is the consent form complete and comprehensive, yet easy to understand?
- Does she understand the necessity for continued contraception while awaiting her surgery?
- Does she understand that permanent sterility cannot be guaranteed after any sterilization procedure, and that failures have been reported even up to 10 years after the surgery? The patient must be apprised of the failure rates for the various methods of sterilization. Most importantly, she must be well informed regarding the failure rate for the method of sterilization that she is expecting to undergo.
- Does she understand that all currently employed female sterilization methods are, for all intents and purposes, irreversible? The physician should always keep in mind, however, the relative possibility of reversibility. The procedure that produces the least amount of tissue disruption, and thus lends itself to the greatest degree of reversibility without sacrificing efficacy, should be recommended.
- Is there any underlying gynecologic pathology that would preclude the physician from recommending hysterectomy as a choice for managing both a gynecologic problem as well as the contraceptive requirements? It is essential to stress the concept that tubal sterilization induces sterility but is not a cure for any other gynecologic problems.
A woman's decision to undergo a sterilization procedure should be based on a number of factors irrespective of age and parity. Age should not be a limiting factor in the decision-making process. The use of artificial arithmetic guidelines (age/parity formula) is an obsolete practice. Nulliparity should not necessarily be considered a contraindication to sterilization, because motivation and other patient needs do not parallel the age and parity of the candidate. It is simply not borne out statistically that the younger the woman at the time of sterilization, the greater the chance she will change her mind or regret the procedure. In fact, we have found that the nulliparous woman, regardless of age, who opts for sterilization is often more motivated toward child-free living than her parous counterparts of similar age.
Sterilization of patients with mental disabilities is a controversial subject. It is best if physicians have the support and consent of the patient's family and psychiatrist. Physicians must also be aware of their federal and local regulations regarding informed consent for sterilization of women with mental disabilities. Consultation with the hospital ethics committee is usually advisable. Court approval may be required in some jurisdictions. For example, sterilization of an incompetent, mentally disabled person in Canada is generally illegal.8
There are other methods of contraception that provide not only highly effective contraception, but in the majority of cases, also control of menstrual flow and may even induce long-term amenorrhea (medroxyprogesterone acetate “Depo-Provera”, progestin medicated intra-uterine device "Mirena"). Since the widespread availability of medical therapies, the use of hysterectomy to achieve permanent contraception and to control abnormal menses has become an uncommon practice.
A consent document that is clearly understandable for the patient must be signed. It is often recommended that the sterilization procedure be performed a few weeks after the initial consultation to allow more time for consideration of the choice of sterilization. Written information in the patient's first language, that can be taken home to read, may be useful.
WHEN?
Laparoscopic sterilization as an outpatient procedure may be performed (1) concomitantly with a pregnancy termination or uterine evacuation for spontaneous abortion, (2) in the postpartum period, or (3) as an interval procedure (most common).9 When the patient is in good health and her psychological status is stable (i.e., she is not experiencing any stressful situation), the decision-making process can be considered a rational one. In some jurisdictions, a waiting period of 30 days is mandatory between consultation and performance of a sterilization procedure, to ensure that the woman has had adequate time to reconsider her decision.
Immediate postpartum sterilization is reasonable, provided the discussion and the decision to undergo the procedure was made before delivery.10 Indeed, during labor or emergency cesarean section, it is not deemed appropriate for health-care providers to initiate discussion regarding elective puerperal sterilization. Generally, the subject of postpartum tubal ligation should be discussed with the patient during her antenatal visits and documented in the patient's chart prior to labor and delivery. If the patient, however, initiates the discussion and the entire consent process during early labor, one might consider that the patient is still capable of making an informed and valid consent to undergo sterilization.
The major advantage of immediate postpartum sterilization is the fact that the woman is already hospitalized. Conversely, the disadvantage is that the frequently encountered state of postpartum depression may produce increased stress that, when combined with the sterilization procedure, can result in deeper depression. Furthermore, the fate of the newborn is not certain in the early neonatal period. Statistically, regret is more frequent when the decision to undergo sterilization has been made immediately postpartum.
Lastly, any intra-abdominal surgical procedure may present an occasion for concomitant tubal sterilization. For example, a woman undergoing surgery, for management of an ectopic pregnancy or some nongynecologic procedure such as cholecystectomy, may undergo concomitant sterilization.
HOW?
The equipment, procedures, and hazards of laparoscopic sterilization have been dealt with elsewhere. The following is a review of the various approaches to tubal occlusion, along with a discussion of their specific advantages and disadvantages. These techniques are presented in chronologic order of their introduction in the medical literature.
Electrocoagulation
Unipolar
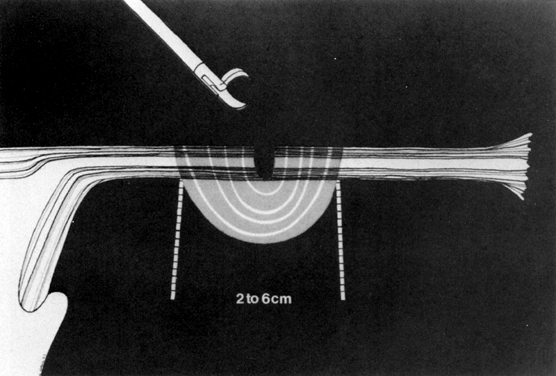
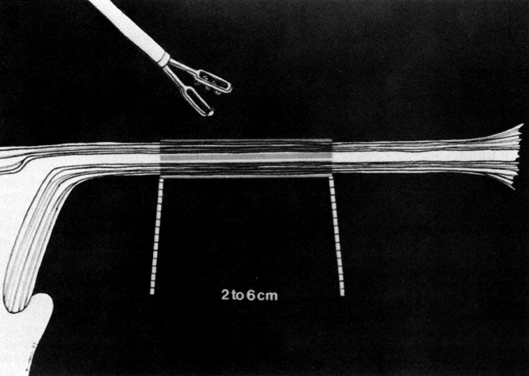
Although gynecologic laparoscopy was flourishing in Europe (only gastroenterologists were using the technique in North America), it was Anderson,11 an American, who in 1937 proposed laparoscopic electrocoagulation of the fallopian tubes to achieve female sterilization. However, it is Palmer12 of France who is credited with describing the modern technique of laparoscopic tubal electrocoagulation in 1962. The first instrument employed for this purpose was the Palmer biopsy forceps, because it was already adapted for electrosurgical capabilities. Powerful, grounded, high-voltage generators producing unipolar electric current were employed. Under such circumstances, the electrical energy is concentrated at the site where the fallopian tube is grasped by the jaws of the forceps. Once current is applied, it then has to travel through the patient's body, from whence it exits and is collected by a ground plate or return electrode to complete the electrical circuit. The original technique involved electrocoagulation of the tubal isthmus, followed by tubal transection and recoagulation of the cut edges (Fig. 1).13
|
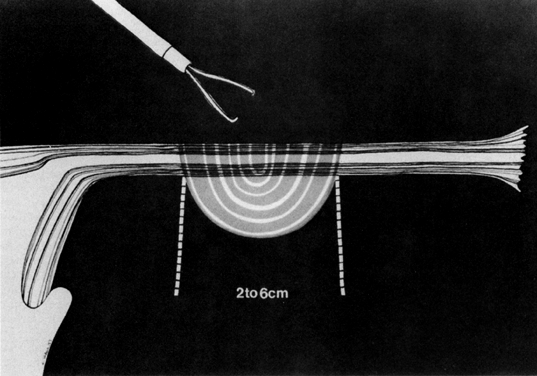
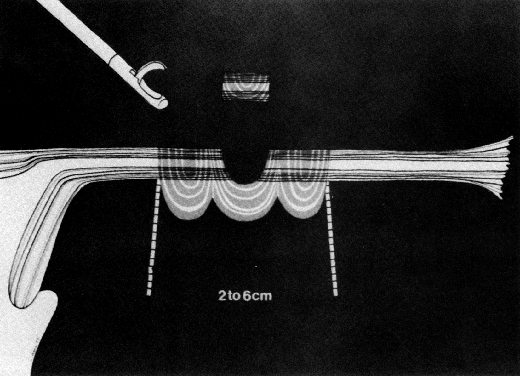
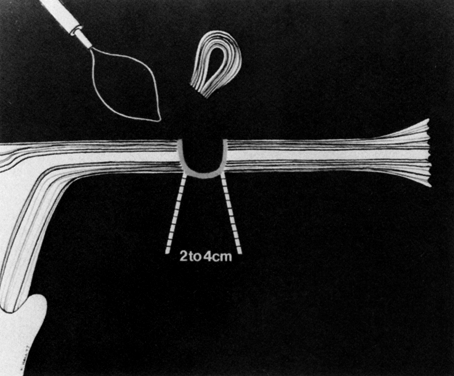
Some authors subsequently indicated that coagulation alone without tubal transection is equally effective, provided the surgeon is experienced and confident that the coagulation is complete (Fig. 2).14 Others recommended that a specimen of the tube be excised for pathologic confirmation.15 This step appears to have evolved as much for medicolegal reasons as for scientific ones. Unfortunately, the frequently charred tissue specimen cannot be identified as originating from the fallopian tube, thus defeating the primary purpose of the biopsy (Fig. 3). With this in mind, Soderstrom and Smith described a technique whereby a loop of tube could be passed through an electrified polyp snare.16 As the snare is squeezed tightly, current is applied; a loop of tube is mechanically excised and the tissue bed concomitantly coagulated. The excised segment, structurally unaltered, can then be evaluated pathologically as well as bacteriologically if indicated (Fig. 4). This method is technically complex and requires the use of an operating laparoscope as well as a second suprapubic puncture.
|
|
|
All of the laparoscopic procedures described up to this point employ the two-puncture technique (i.e., a viewing laparoscope usually introduced at the umbilicus, and an operating instrument most often introduced through a second, suprapubic puncture in the midline). In 1972, Wheeless17 adapted this method to the operating laparoscope, thus obviating the need for a second puncture. The one-puncture technique appears to be particularly suitable for use in conjunction with local anesthesia and requires few instruments with less surgical assistance.
Whether one or two punctures are employed, and regardless of the coagulation technique used (i.e., coagulation only, coagulation combined with tubal transection, or resection), it was discovered that the unipolar electrical system was associated with some inherent dangers. As early as 1973, Thompson and Wheeless18 reported 11 cases of bowel burns secondary to accidental electrical injury during the process of tubal electrocoagulation. Other reports followed, further emphasizing the fact that a potentially dangerous situation existed with the use of unipolar current.19 There generally was no rational explanation for such accidents and, as a consequence, it was difficult if not impossible to avoid them. We now know that some cases were simply secondary to faulty technique, but most were related to the inherent danger associated with high-voltage, grounded generators. Some of these units, when set in the coagulation mode, were capable of producing thousands of volts and hundreds of amperes of current. As the tubal tissue was being dehydrated, the tissue resistance increased, and the generator produced more current in an attempt to overcome this resistance. Today, more sophisticated generators are available; these are generally of solid-state construction, producing low-voltage, high-frequency current; they are not grounded, but rather isolated from ground. Although these have turned out to be much safer, some bowel burns unfortunately still occur.
Another and most logical theory to account for the bowel burns when a single puncture technique was employed is the role played by capacitative induced current. As we have seen, Wheeless popularized the use of the operating laparoscope for sterilization. If one adds to that the appearance of fiberglass sheaths through which the laparoscope is passed, one has all of the elements necessary to create an electrical capacitor. When high-frequency current is passed through the coagulating instrument within the operating channel of the laparoscope, up to 50% of the current is transferred or leaks to the laparoscope itself, despite the fact that the instrument is insulated. If a metal sheath is used rather than an insulating or fiberglass sheath, this current is dispersed within the abdominal wall, which is a much larger surface, and thus will cause no harm. However, if the fiberglass sheath or a metal sheath surrounded by a plastic anchor is used, the current will not be allowed to leak out and will instead charge the laparoscope, which now becomes a capacitor. This current can be discharged to a loop of bowel or other structure, should it come into contact with the laparoscope during the procedure without the knowledge of the operator.
Bipolar
In 1973, after scattered reports of electrosurgical injury in the medial literature, Rioux and Cloutier20 devised the bipolar technique for tubal electrocoagulation. This method differed from the conventional unipolar system in that the operating forceps carried both the active and the return electrode.21
By completely isolating the two jaws of the forceps from one another, high-frequency current can be passed through one jaw and retrieved and returned to the generator through the other. The current thus passes selectively through the tissue grasped between the jaws of the forceps. Although high-frequency current is employed, it is required to travel only a short distance: that is, the thickness of the tube that is grasped within the jaws (1 to 2 mm). The bipolar procedure appears to be safer than the unipolar system, since the dangers of sparking are eliminated. Capacitative current is not produced because of a “canceling out” of the electric waves (i.e. the current enters and exits via the same instrument). Inadvertent electrosurgical injury to the bowel with bipolar forceps can, therefore, only occur if the bowel is grasped directly with the forceps. If such a situation were to occur, the complication would obviously be a result of surgical error as opposed to instrument failure. A further advantage of bipolar electrocoagulation is that the resulting burn is discrete and localized, selectively destroying only the tube that is in the grasp of the forceps jaws, leaving most of the mesosalpinx unaffected (Fig. 5).
|
At this point, a word of caution is essential: Bipolar instruments should be employed only with compatible electrosurgical units as recommended by the manufacturers, or with a generator possessing both limited output and isolated circuitry.
The complication rate for laparoscopy is directly proportional to the experience of the operator and his or her attention to the appropriate safety guidelines. Soderstrom and Butler22 achieved a significant reduction in the complication rate, from 13% to 3% within 1 year, after the introduction and implementation of an organized operative protocol. Electrosurgical complications have become considerably less frequent since the advent of the bipolar technique, as well as with the use of low-voltage, high-frequency generators. Furthermore, education and familiarization of physicians and operating-room personnel with electrosurgical instruments have resulted in fewer complications. Of further interest is the fact that Soderstrom and Butler22 demonstrated that many suspected bowel burns were actually the result of sharp trocar injuries, rather than electrical injuries.
Mechanical Techniques
Clip
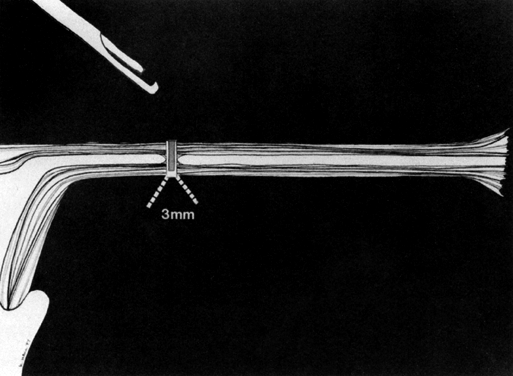
Two nonelectrical (mechanical) laparoscopic tubal occlusive techniques have become popular in the past few years. Hulka and colleagues23 developed the spring-loaded clip. Aware of the high failure rate associated with the use of a previously developed tantalum clip (up to 27% according to Wheeless24), yet still fascinated by the simplicity of the concept, Hulka and associates spent years developing a clip of Lexan (Richard Wolf Instrument Corp., Rosemont, IL) plastic jaws held in place by a gold-plated stainless steel spring, which is thought to reduce peritoneal reaction. The basic principle involved in this technique is that the plastic jaws with interlocking teeth leave no spaces. The maximal pressure on the tube is applied over a period of time, thus lessening the acute crushing effect that could result in fistula formation (Fig. 6). This plastic clip, as opposed to the tantalum clip, supposedly leaves no room for recanalization.
The original clip applicator was subsequently adapted to the operating laparoscope for single-puncture application. Later, Lieberman and co-workers,25 favoring the two-puncture technique, devised an appropriate applicator.
Another clip, devised by Filshie and colleagues26 and introduced into the United States in 1997 (more than 10 years after its introduction into Canada and many other countries), is made up of titanium jaws lined with silicone. Locking of the device is achieved by a flattening effect of the upper jaw, which locks into the lower hooked jaw. This locking occurs through the mesosalpinx and is easily visualized at the time of application and enclosure of the clip. This confirms that the entire diameter of the tube has been included within the jaws. Visualization of the hooked end of the lower jaw can actually be confirmed before locking. When locked in place, the clip leaves no space at all between the jaws, thus achieving complete tubal occlusion. Compared to the Hulka clip, the Filshie clip appears to be easier to position properly before closure. In addition, because of its length, the Filshie clip can be placed on almost any fallopian tube, regardless of thickness or shape, including postpartum tubes.
Falope Ring
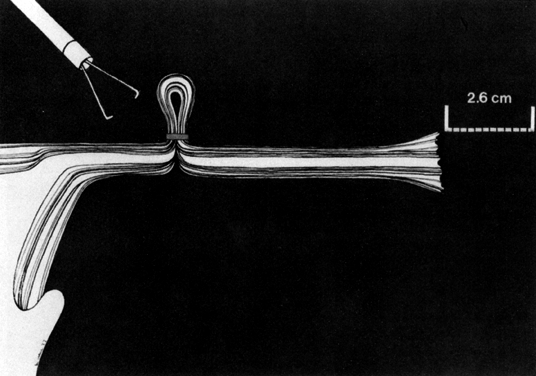
The Falope ring, devised by Yoon and King,27 is ingeniously simple. A loop of tube is drawn into the central hollow cylinder of the ring applicator forceps (single- or double-puncture technique) by gentle squeezing of the applicator handle. The loaded Silastic band is then forced down over the loop of tube by the forward action of an outer cylinder by a further squeezing of the applicator handle. This results in the release of the band from the applicator onto the loop of tube, thus achieving tubal occlusion. The portion of the tube encircled by the ring gradually becomes sclerosed, and the proximal and distal segments of tube become occluded (Fig. 7).
|
When the tubes are slender and lie free (i.e., are not involved in an adhesive or old inflammatory process), they are easily drawn up within the inner cylinder. When a thick or edematous tube is encountered, however, a slow “milking up” of the tube by means of a to-and-fro motion of the applicator handles is usually necessary in order to draw the tube into the hollow central cylinder. In doing so, the serosa may be damaged, or the tube may be totally transected (“click sign” of Levinson), thus increasing the risk of fistula formation, as with the Madlener technique. In addition, there is also the potential for bleeding from the transected tube.
INDICATIONS FOR VARIOUS STERILIZATION TECHNIQUES
Should one be familiar with and have the capacity to perform more than one technique? Is it possible to tailor the sterilization technique to the individual patient? Is any one sterilization technique better suited for outpatient surgery? Which single technique is most universally applicable?
It is difficult, if not impossible, to answer these questions definitively. It is important, however, to have a backup form of sterilization for any routine technique that is chosen, in the event of equipment failure.
We believe the two-puncture approach is the most versatile: (1) it allows the surgeon to choose any of the previously described techniques; and (2) it permits the best working angle, best visibility, and best maneuverability of instruments. Our approach is as follows: After we obtain an adequate pneumoperitoneum, we introduce a small, 180° forward optic laparoscope. After a short, but complete, observation of the entire abdominal cavity, we introduce the second trocar under direct vision, thus eliminating a second blind abdominal puncture. We make sure a complete variety of instruments is available, and are thus able to chose the method that appears best suited for the patient or the clinical situation. For example, the decision to use the Falope ring may have been reached preoperatively during discussions between the patient and surgeon. However, exploration may reveal the presence of an edematous fallopian tube, with or without some degree of subclinical inflammation, precluding the use of the ring. Under such circumstances, one would require the backup of an alternate technique, such as electrocoagulation or a clip, to achieve the sterilization. In contrast, with the one-puncture technique, the operator may be restricted to a technique that is applicable to the operating laparoscope.
We believe that the technique chosen should be tailored to the individual patient's needs, discussed with the patient preoperatively and be a technique that the physician has training and experience with. We believe that, because we are in an era in which consideration of reversibility is so important, sterilization methods resulting in the least tissue destruction should be favored As mentioned previously, alternative options should be available for cases when the clinical findings preclude the application of the primary technique. This possibility should also be mentioned to the patient in the preoperative counseling. If a secondary technique is required then the patient should be informed post-operatively.
Therefore, to preserve a relatively high rate of reversibility, and to destroy the least amount of tissue, the clip appears to be ideal because it destroys only 3 mm of tubal tissue and little, if any, of the blood supply. We prefer the Filshie clip because of its ease of application and apparent improved efficacy. The Falope ring, which destroys approximately 2.6 cm of fallopian tube and involves only a small amount of its vascularity, should be considered as the next least destructive method. Electrocoagulation destroys the largest amount of tubal tissue, even more than is apparent at the time of the procedure. This is more pronounced when unipolar current is employed, as opposed to bipolar. Thus, electrosurgical methods, should be reserved for older women whose future fertility is not desired under any circumstance.
ANESTHESIA
Any of the occlusive techniques discussed can be performed using either local or general anesthesia. In practice, however, local anesthesia is combined with an intravenous injection of an analgesic and/or neuroleptic (e.g., meperidine, fentanyl, droperidol) to reduce the patient's level of pain and anxiety.
It appears that the mechanical methods of tubal occlusion are better suited to local anesthesia, if for no other reason than the fact that the procedure may be performed more quickly.
FAILURE RATES ASSOCIATED WITH STERILIZATION PROCEDURES
In 1996 the risk of pregnancy after tubal sterilization: findings from the US collaborative review of sterilization (CREST study) was published. This review is the most widely referenced study regarding both short and long term failure rates associated with tubal sterilization. This was a prospective study involving over 10,00 women undergoing tubal sterilization at 9 medical centers in the United States. The authors do comment that most of the participants were enrolled from teaching institutions and that there was substantial difference noted in the failure rates from different institutions, possibly a reflection on the degree of experience of use at each center. They do state that their results may only be generalized to tubal sterilizations occurring in similar settings. Patients were followed by annual telephone follow-up and true sterilization failures were determined by consensus of two of the CDC investigators. Much to the surprise of many clinicians, early reported failure rates were only part of the overall failure picture. Failures were still being reported up to 10 years after the initial procedure and at 10 years post-surgery, the overall rate rises to 1.8%. Definite differences in long-term failure rates have been demonstrated among various methods and are presented in Tables 2 and 3.28, 29, 30, 31
Table 2. Probabilities of pregnancy - CREST study 1996, ectopic pregnancy rate - AAGL survey 1995
Method Sterilization | Number of cases in CREST study (n)28 | Cumulative probability of pregnancy (per 1000) (10 yrs)28 | Ectopic pregnancy rate (%)29 |
| Postpartum partial salpingectomy | 1637 | 7.5 | 26 |
| Laparoscopic: | |||
| Unipolar | 1432 | 7.5 | 22 |
| Bipolar | 2267 | 24.8 | 53 |
| Falope ring | 3329 | 17.7 | 41 |
| Hulka clip | 1595 | 36.5 | 47 |
Table 3. Probability of pregnancy and ectopic pregnancy following laparoscopic tubal sterilization with Filshie clips
| Number (n) | Probability of pregnancy (per 1000)(up to 15 yrs follow up) | Ectopic pregnancy rate(AAGL survey 1995)(%)29 |
| Kovacs GT, Krins AJ30 | 30,000 | 2.4 | 0.02 |
| Penfield AJ31 | 434 | 2.3 | 0.02 |
With multivariant analysis the CREST study demonstrated that age at sterilization, race-ethnicity, study site and sterilization method were all independent significant factors affecting failure rate. The highest failure rates were reported for women undergoing sterilization prior to age 28 with either bipolar electrocoagulation or spring-loaded clip. The authors comment that all methods require proper application to maximize effectiveness. Thus they include the following recommendations. The spring-loaded clip should be applied after the fallopian tube is placed on stretch. The clip should be placed on the proximal segment of the isthmus perpendicular to the long axis of the fallopian tube. Prior to closure of the jaws of the clip, the clip should be advanced over the width of the tube until the tube reaches the hinge of the clip. Thus when closed the clip will include a small portion of the mesosalpinx. With regards to the bipolar tubal electrocoagulation they cite the recommendations of Soderstrom32 who suggested the following strategies for reducing failure rates:
1. 25 watts of non-modulated (cutting) waveform,
2. in-line current meter, and
3. coagulation of at least 3 contiguous segments of the isthmus.
PROBLEMS ENCOUNTERED DURING THE PROCEDURE AND THEIR MANAGEMENT
The more experienced and skillful the surgeon is with a particular technique, the lower the complication rate. Most experienced laparoscopists favor a specific technique and therefore become more proficient in it compared to the other techniques. As a result, the data are biased regarding complication rates, and it is impossible to apply surgeon-specific data to all physicians.
The unipolar electrocoagulation method is probably the most efficient method of laparoscopic sterilization to perform, because the tube is well grasped by the electrocoagulating forceps. The tube can then be lifted and mobilized to ensure that it is not in close proximity to any surrounding structures while the current is being applied. A more than adequate segment of tubal occlusion can be obtained as well with a single, properly placed grasp, as long as the current is applied for an adequate length of time. Unfortunately, as discussed earlier, this technique is also associated with the highest risk of electrosurgical complication. If electrosurgical bowel injury is recognized at the time of the procedure, immediate segmental resection of the bowel at the site of the injury should be performed. For most operators this would require immediate laparotomy, but some may perform the same surgery by laparoscopic access. It is not sufficient to oversew the burned area, since electrical burns notoriously destroy more tissue than is actually evident. Wide segmental resection is required.
If the burned area is not recognized at the time of the surgery, the patient generally will present emergently within 2–8 days postoperatively with signs and symptoms of peritonitis. For this reason, every patient should be instructed to contact her physician if excessive pain or fever occurs 48 hours or more postoperatively. Increasing abdominal pain, greater than 48 hours after laparoscopy, should always raise the concern of bowel injury until proven otherwise. In some cases, if another physician is consulted in the face of such signs and symptoms, he or she may not immediately relate them to the possibility of a bowel burn, with its associated fecal peritonitis (secondary to the perforation); thus, the morbidity rate is increased. The bowel injury in such cases is usually located in the terminal ileum, approximately 20 to 37.5 cm from the cecum. If the surgeon is unaware of the electrosurgical nature of the injury and simply oversews it, there is often a secondary breakdown of the site and recurrent peritonitis, with an even greater risk of morbidity and mortality. If adequate steps are undertaken initially, and wide segmental resection is performed, healing generally occurs with minimal morbidity to the patient.
The problem with bipolar electrocoagulation is that none of the commonly available forceps allows for as good a grasp of the fallopian tube as does the unipolar forceps. This occurs because the jaws of the bipolar forceps cannot, by virtue of their construction, touch each other. The tube can then slip out of the jaws, making it more difficult to elevate the tube and to mobilize it away from surrounding structures. However, the bipolar technique is so much safer that this inconvenience is still considered to be a minor one.
Based on statistical evidence, we believe that it is unnecessary to transect the tube after adequate electrocoagulation as long as adequate tubal destruction is achieved. What constitutes adequate electrocoagulation? Only experience enables the surgeon to formulate this judgment. Generally, when the tissue held within the grasper stops showing visible signs of conducting electricity then that segment is fully electrocoagulated. A final word of caution: It is not necessary to electrocoagulate the entire tube to achieve foolproof occlusion. We believe that adequate electrocoagulation of a 2 to 3 cm segment in the isthmic portion of the fallopian tube is sufficient to achieve permanent sterility.
There is no replacement for expertise in applying clips properly, an absolute necessity for obtaining low failure rates. The major problem encountered in developing a sound technique for the Hulka clip application is the difficulty in enclosing the entire tube well within the jaws of the clip to ensure complete tubal occlusion. Because the tube is quite mobile, this can be difficult at times, but once the technique of application is mastered, it becomes quite simple. To achieve predictable occlusion, the clip should be applied at right angles to the fallopian tubes. Because these clips contain small teeth in both jaws, care must be taken to avoid tearing of tubal serosa or the mesosalpinx during clip application. With the development of the second-puncture clip applicator, application of the clip has become simpler. With a second puncture technique, manipulation of the clip applicator is independent of movements of the telescope. The Filshie clip is easier to apply than the Hulka clip because it is longer, and because of the grasping effect of the upper jaw. We personally have never encountered a situation where the Filshie clips could not be applied during an interval sterilization procedure. Clips should be applied at the isthmic portion of the tube, 1 to 2 cm distal to the cornua, to permit a future isthmic-isthmic reanastomosis, should the need to restore fertility arise.
The Falope ring is a simple and efficient technique considered by some to be the simplest when the tubes are thin and mobile. In the presence of adhesions or tubal edema, however, it may be impossible to elevate a knuckle of tube adequately to carry out the procedure without difficulty. Furthermore, when the tube is large or edematous, it may be virtually impossible to pull the tubal knuckle into the inner sheath of the instrument. Overzealous attempts at this step may result in tubal transection. Should such a transection inadvertently occur, the complication may be managed in one of two ways. The first method is to apply separate rings to each of the cut ends of the fallopian tube to achieve both hemostasis and tubal occlusion. A second alternative is to introduce a 5-mm reducer into either the 8-mm second-puncture cannula or the operating channel of the one-puncture instrument and to introduce a 5-mm bipolar electrocoagulating forceps. The cut ends of the fallopian tube and, if necessary, the mesosalpinx (if actively bleeding) can then be electrocoagulated for the purpose of both hemostasis and tubal occlusion.
The authors consider it highly advisable for all surgeons who employ the Falope ring technique to have electrocoagulation potential available in the operating theater and a 5-mm reducer to reduce the diameter of the 8-mm Falope ring sheath to accommodate an electrocoagulating instrument.
COMPLICATIONS AND THEIR MANAGEMENT
Complications are uncommon with laparoscopic sterilization. However, the operator should be familiar with those that may occur, the mechanism involved and the method of management.
Pain
Postoperative pain is usually limited to the immediate postoperative period (6–48 hours). With electrocoagulation, it appears that nerve endings in the fallopian tube are destroyed, and very little, if any, postoperative pain occurs secondary to the electrocoagulation itself. Because of their crushing effect, the mechanical occlusive techniques (Falope ring and clips) tend to produce a crampy type of lower abdominal pain, which may last up to 48 hours. Whether or not this is related to the release of prostaglandins due to tissue ischemia and necrosis is unproven, but suspected. In any case, a minor form of analgesic, either a prostaglandin synthetase inhibitor or one containing 5–30 mg of codeine, may be administered as needed.
When local anesthesia is given along with mechanical occlusive techniques, a local anesthetic agent (e.g., bupivacaine) may be applied directly to the tube before application of the ring or clip. This theoretically reduces the resultant pain from the occlusive procedure.33 It is difficult to substantiate any long-term relationship between laparoscopic tubal sterilization and pelvic pain.
Wound Infection
When laparoscopic sterilization is performed in an operating theater under sterile conditions, wound infection is rarely a problem. Occasionally, however, superficial wound infection of the upper or lower abdominal punctures can occur and, if present, generally can be managed easily by means of hot compresses with or without the concomitant use of topical antibiotics.
Peritoneal Infection
Septic peritonitis associated with laparoscopy is rare. We have never personally experienced this complication.
Intra-peritoneal Bleeding
Mesosalpingeal tears with resultant bleeding may result from ring or clip application. If recognized at the time of initial procedure this should be managed as described in the previous section. If recognized later, return to the operating room for laparoscopy, and possible laparotomy, may be required to control the bleeding.
Uterine Perforation
This may occur with the uterine manipulator. It often does not require further surgery, but may require laparoscopic suturing if there is ongoing bleeding.
Organ Injury
Injury to blood vessels, intestines, or other organs has been reported to occur with an incidence of 0.6 per 1000 cases.34 Morbidity is reduced if recognized and managed immediately, either by operative laparoscopy or if necessary laparotomy. Management of electrosurgical bowel injury is discussed in the previous section.
Hernia
Hernias at the site of the umbilical or lower abdominal incisions have been reported. Ideally, the best management of such problems is to prevent them. Use of the Z insertion technique theoretically prevents such complications. In addition, the use of the smallest instrument and smallest trocar cannula system applicable to the procedure is preferable. Careful removal of the upper and lower puncture sheaths so that no omental tissue is entrapped is also important. Laparoscopic tubal sterilization is usually performed with incisions less than 10mm in length. However, incisions equal to or greater than 10mm in length, or those that have been inadvertently stretched to a similar length, should be subjected to fascial suture closure employing a delayed absorbable suture.
Abnormal Uterine Bleeding
Numerous physicians have suggested, on the basis of clinical impression, that a long-term sequela of tubal sterilization is the development of abnormal uterine bleeding. This has been named the "post-tubal ligation syndrome". However, there is no supportive evidence to suggest that menstrual bleeding changes as a result of tubal ligation. In fact, several reports have been unable to demonstrate differences in either hormone levels or menstrual bleeding patterns in women who have previously been sterilized when compared to non-sterilized control women.35, 36, 37, 38, 39
Several factors must be considered. A major one is the fact that many women electing to undergo tubal sterilization have previously used some form of contraception, the most popular of which is the oral contraceptive, for varying numbers of years before the sterilization procedure. Considering that oral contraceptives are classically associated with a reduction in menstrual flow, one might well expect an increase in the amount of bleeding associated with discontinuation of this medication after sterilization. Therefore, most physicians do not believe that the "post-tubal ligation syndrome" exists.40
Ectopic Pregnancy
Ectopic pregnancy should be suspected whenever a woman who has previously undergone tubal sterilization. The rate of ectopic pregnancy among sterilized women ranges from 4–73% of pregnancies, depending on the method of sterilization.41 There is an approximately 3-fold greater incidence of ectopic pregnancies after electrocoagulation compared to falope rings.42 Ectopic pregnancy has most often been associated with: utero-peritoneal fistula after unipolar electrocoagulation; inadequate electrocoagulation or recanalization after bipolar procedures; recanalization or fistula formation after partial segmental resection, falope ring, or clip procedures.41 The CREST study demonstrated a 10-year cumulative probability of ectopic pregnancy of 7.3 per 1000 women for all methods combined.28
CONCLUSION
Laparoscopic sterilization has become the most popular method of interval female sterilization in North America. This procedure has the advantage of providing a visual survey of the upper abdomen and entire pelvic cavity, as well as much of the superficial bowel content. There are very few situations in which laparoscopy is impossible to perform. It is a sophisticated procedure with an array of highly technical and, in some cases, expensive instruments. Therefore, it seems ideally suited for the more developed countries. In lesser developed nations, however, the relative ease of the procedure and the lack of disfigurement may also act as motivating factors. For a country with a well-established family-planning infrastructure and motivated, skillful surgeons, the introduction of female laparoscopic sterilization can provide the necessary impetus to foster voluntary sterilization.
REFERENCES
Bulletin of the World Health Organization, ISSN 0042-9686 |
|
Mosher WD, Pratt WF. Contraceptive use in the United States, 1973-1988. Hyattsville, Maryland: National Center for Health Statistics, 1990; advance data from vital and health statistics no. 182. |
|
Peterson LS. Contraceptive use in the United States: 1982-90. Hyattsville, Maryland: National Center for Health Statistics, 1995; advance data from vital and health statistics of the Centers for Disease Control and Prevention/National Center for Health Statistics, no. 260. |
|
Westoff C, Davis A. Tubal sterilization: focus on the U.S. experience. Fertil Steril 2000; 73:913-22. |
|
The Society of Obstetricians and Gynecologists of Canada. Canadian Contraception Consensus. J Soc Obstet Gynaecol Can. 2004: 26(2); 143-56. |
|
CDRH, FDA, U.S. Food and Drug Administration, Center for Device andRadiological Health. EssureTM System- P020014. (Online) November 04, 2002. Cited: September 22, 2007) http://www.fda.gov/cdrh/pdf2/2p020014.html. |
|
Cooper JM, Carignan CS, Cher D, Kerin JF and Group. Selective Tubal Occlusion Procedure 2000 Investigators, Microinser nonincisional hysteroscopic sterilization. Obstet Gynecol., Jul 2003, vol 102(1), pp.59-67. |
|
The Society of Obstetricians and Gynecologists of Canada. Canadian Contraception Consensus. J Soc Obstet Gynaecol Can. 2004: 26(4); 327-87. |
|
Rioux JE, Yuzpe AA: Evaluation of female sterilization procedures. Curr Probl Obstet Gynecol 11(9): 1979 |
|
Keith L, Houser K, Webster A et al: Postpartum laparoscopy for sterilization. J Int Fed Obstet Gynecol 8: 145, 1970 |
|
Anderson ET: Peritoneoscopy. Am J Surg 35: 136, 1937 |
|
Palmer MR: Essais de stérilisation tubaire coelioscopique par électrocoagulation isthmique. Bull Fed Soc Gynecol Obstet Lang Fr 14: 298, 1962 |
|
Steptoe PC: Laparoscopy in Gynaecology. Edinburgh, E & S Livingstone, 1967 |
|
Yuzpe AA, Rioux JE, Loffer FD et al: Laparoscopic tubal sterilization by the “burn only” technique. Obstet Gynecol 49: 106, 1977 |
|
Wheeless CR Jr, Thompson BH: Laparoscopic sterilization: Review of 3,600 cases. Obstet Gynecol 42: 751, 1973 |
|
Soderstrom RM, Smith MR: Tubal sterilization: New laparoscopic method. Obstet Gynecol 38: 152, 1972 |
|
Wheeless CR Jr: Elimination of second incision in laparoscopic sterilization. Obstet Gynecol 39: 134, 1972 |
|
Thompson BH, Wheeless CR Jr: Gastrointestinal complications of laparoscopy sterilization. Obstet Gynecol 41: 669, 1973 |
|
Rioux JE, Quesnel G, Blanchet J et al: Laparoscopie: Stérilisation tubaire: Étude de 1,000 cas et évaluation globale de la méthode. Union Med Can 102: 1865, 1973 |
|
Rioux JE, Cloutier D: Laparoscopic tubal sterilization: Sparking and its control. Vie Med Can Franç 2: 760, 1973 |
|
Rioux JE, Cloutier D: A new bipolar instrument for laparoscopic tubal sterilization. Am J Obstet Gynecol 119: 737, 1974 |
|
Soderstrom RM, Butler JC: A critical evaluation of complications in laparoscopy. J Reprod Med 10: 245, 1973 |
|
Hulka JF, Fishburne JI, Mercer JP et al: Laparoscopic sterilization with a spring-clip: A report of the first fifty cases. Am J Obstet Gynecol 116: 715, 1973 |
|
Wheeless CR Jr: Where we've been, what we've tried and where we are going in the use of laparoscope in female sterilization. In Sciarra JJ, Droegemueller W, Speidel JJ (eds): Advances in Female Sterilization Technology. Hagerstown, MD, Harper & Row, 1976 |
|
Lieberman BA, Gordon AG, Bostock JF et al: Laparoscopic sterilization with spring-loaded clips: Double puncture technique. J Reprod Med 18: 241, 1977 |
|
Filshie GM, Casey D, Pogmore JR et al: The titanium/silicone rubber clip for female sterilization. Br J Obstet Gynaecol 88: 655, 1981 |
|
Yoon IB, King TM: A preliminary and intermediate report on a new laparoscopic tubal ring procedure. J Reprod Med 15: 54, 1975 |
|
Peterson HB, Xia Z, Hugues JM et al: The risk of pregnancy after tubal sterilization: Findings from the U.S. Collaborative Review of Sterilization. Am J Obstet Gynecol 174: 1161, 1996 |
|
Hulka JF, Phillips JM, Peterson HB, Surrey MW: Laparoscopic sterilization: American Association of Gynecologic Laparoscopists' 1993 membership survey. J Am Assoc Gynecol Laparosc 2: 137, 1995 |
|
Kovacs GT, Krins AJ. Female sterilizations with Filshie clips: what is the risk of failure? A retrospective survey of 30,000 applications. J Fam Plan and Repr Health Care. 2002: 28(1);34-5. |
|
Penfield AJ. The Filshie clip for female sterilization: a review of world experience. Am J Obstet Gynecol. 2000: 182(3): 485-9. |
|
Soderstrom RM, Levy BS, Engel T. Reducing bipolar sterilization failures. Obstet Gynecol. 1989;74:60. |
|
Tool AL, Kammerer-Doak DN, Nguyen CM et al: Postoperative pain relief following laparoscopic tubal sterilization with Silastic bands. Obstet Gynecol 90: 731, 1997 |
|
Lam A, Rosen DMB. Laparoscopic bowel and vascular complications: should the veress needle and cannula be replaced? J Am Assoc Gynecol Laparosc 1996;3:524. |
|
Geber S, Caetano JP. Doppler colourflow analysis of uterine and ovarian arteries prior to and after surgery for tubal sterilization: a prospective study. Hum Reprod 1996;11(6):1195-8. |
|
Taner CE, Hakverdi KU, Erden AC, Satici O. Menstrual disorders and pelvic pain after sterilization. Adv Contracept 1995; 11(4):309-15. |
|
Ruifang W, ZhenhaiW, Lichang L, Fenger Z, Xinglin G. Relationship between prostaglandin in peritoneal fluid and pelvic venous congestion. Prostaglandins 1996;51(2):161-7. |
|
Hakverdi KU, Taner CE, Erden AC, Satici O. Changes in ovarian function after tubal sterilization. Adv Contracept 1994;10:51-6. |
|
Pati S, Cullins V. Female Sterilization: Evidence. Obstet Gynecol Clin North Am 2000;27(4);859-99. |
|
Rioux JE. Uterine bleeding following tubal occlusion in gynecology. In Kieth Berger GS et al (eds): The Safety of Fertility Control, Chap 29, pp267-280, Springer, 1980. |
|
The Society of Obstetricians and Gynecologists of Canada. The Canadian Consensus Conference on Contraception. J Soc Obstet Gynaecol Can. 1998; 20(7), part 4: 58-63. |
|
Sitko D, Commenges-Ducos M, Roland P, Papaxanthos-Roche A, Horovitz J, Dallay D. IVF following impossible or failed surgical reversal of tubal sterilization. Hum Reprod 2001;16(4):683-5. |