Premenstrual Syndromes
Authors
INTRODUCTION
The premenstrual syndromes (PMS) are characterized by mood and behavioral changes that occur for several days to 2 weeks before menses, followed by symptom relief in the postmenstrual phase of the cycle. The severity and the regular occurrence of the symptoms in the premenstrual phase are the essential components of the diagnosis. The term PMS as used by clinicians and the public is generic, imprecise, and commonly applied to numerous symptoms that range from the mild and normal physiologic changes of the menstrual cycle to clinically significant symptoms that limit or impair normal functioning. Historically, premenstrual symptoms have been difficult to diagnose and treat because of the lack of diagnostic criteria and any scientific evidence of treatment efficacy. However, in recent years, randomized controlled trials and other well-designed studies have defined diagnostic criteria and identified effective treatments for moderate to severe PMS and/or premenstrual dysphoric disorder (PMDD), a severe form of PMS as defined in the Diagnostic and Statistical Manual of Mental Disorders, 4th Edition (DSM-IV).1
DEFINITIONS
PMS was defined by a National Institute of Mental Health (NIMH) consensus workshop group in 1983 as: “A constellation of mood, behavioral, and/or physical symptoms that have a regular cyclical relationship to the luteal phase of the menstrual cycle, are present in most if not all cycles, and remit by the end of the menstrual flow with a symptom-free interval of at least one week each cycle.”2 The essential characteristic of PMS is the timing of the symptoms, with the severity occurring premenstrually and a symptom-free interval after menses.
The American College of Obstetricians and Gynecologists (ACOG) published a revised practice bulletin in 2000 for the management of premenstrual syndrome.3 The key elements of a PMS diagnosis as identified by ACOG include the following: (1) symptoms consistent with PMS; (2) restriction of the symptoms to the luteal phase of the menstrual cycle; (3) confirmation of the symptom pattern by prospective assessment; (4) the symptoms cause functional impairment; and (5) exclusion of other diagnoses that may better explain the symptoms.
The attempt to provide specific diagnostic criteria for PMS was first made by the American Psychiatric Association. The initial set of criteria was termed late luteal phase dysphoric disorder (LLPDD; same as PMDD) and was described in the third edition (revised) of the Diagnostic and Statistical Manual (DSM-III-R).4 The LLPDD criteria were subsequently slightly revised by adding a symptom (fears of loss of control) and renaming the disorder PMDD, which was included as a diagnosis for further study in DSM-IV.1 By providing diagnostic criteria, PMDD has played an important role in the conduct of clinical trials to determine the efficacy of treatments for the disorder. However, as with other definitions of PMS, the key elements of symptom severity and degree of change over the menstrual cycle are not specifically quantified, and published studies continue to differ in the samples selected on the basis of these criteria.
In this chapter, the term PMS is used to signify clinically significant PMS and includes the severe form of PMDD. The term PMDD is retained when studies clearly used the PMDD diagnosis.
SYMPTOMS
Numerous symptoms have traditionally been associated with PMS (Table 1). The range of symptoms is particularly extensive when there is no clear diagnosis of PMS that distinguishes the disorder from other comorbid conditions that may account for the symptoms. It is underscored that many other disorders, both physical and psychiatric, are exacerbated premenstrually or occur as a comorbid disorder with PMS (see later). However, when a careful diagnosis is made to distinguish PMS from other conditions, a much smaller group of symptoms appears typical of the syndrome, most commonly mood symptoms, accompanied by other specific physical and behavioral symptoms (Table 2).
Table 1. Common signs and symptoms of premenstrual syndrome
| Cognitive | Automatic |
| Loss of interest | Fainting, dizziness, vertigo |
| Indecision | Sweating |
| Difficulty concentrating | Nausea |
| Memory impairment | Vomiting |
| Obsessional thinking | Ringing in ears |
| Confusion | Numbness |
| Feel unreal, like in a dream | Tingling of skin |
| Poor judgment | Trembling |
| Mood | Lightheadedness |
| Mood swings | Palpitations |
| Irritability | Headaches, migraines |
| Anxiety | Gastrointestinal |
| Depression | Increased appetite |
| Cannot cope | Food cravings |
| Feel insecure | Thirst |
| Suicidal thoughts | Nausea |
| Guilty thoughts | Vomiting |
| Feel empty | Abdominal bloating, discomfort |
| Behavioral | Constipation |
| Increased drug and alcohol use | Fluid Retention |
| Increased sensitivity to alcohol | Edema |
| Smoke more | Abdominal bloating, discomfort |
| Impulsive | Puffy hands |
| Increased appetite | Breast tenderness, pain, or swelling |
| Social withdrawal | Leg heaviness |
| Accident prone | Weight gain |
| Clumsiness | Allergic |
| Restlessness (fidgeting, hand-wringing, cannot sit still) | Asthma |
| Breathing difficulties | |
| Lack of self-control, violent behavior | Watery nose, nasal congestion |
| Crying | Red eyes |
| Self-indulgent | Urticaria |
| Change in interest in sex | Pruritus |
| Energy level | Miscellaneous |
| Fatigue | Urinary frequency or retention |
| Malaise | Acne |
| Sleep changes (hypersomnia, insomnia) | Joint and muscle pain |
| Weakness | Backache |
| Frequent naps | Stiffness |
(Gise LH: Premenstrual syndromes. In Lemcke DP, Pattison J, Marshall LA, et al (eds): Primary Care of Women, pp 410–419. Norwalk, Appleton and Lange, 1994.)
Table 2. Predominant symptoms of PMS
| Mood | Behavioral | Physical |
| Irritability | Sleep disturbances | Swelling |
| Mood swings | Appetite changes | Breast tenderness |
| Anxiety/tension | Poor concentration | Aches |
| Depression | Decreased interest | Headache |
| Feeling out of control | Social withdrawal | Bloating/weight gain |
Among women who have been carefully screened for clinically significant PMS, mood symptoms are typically predominant (irritability, anxiety, tension, mood swings, feeling out of control, depression). Almost always accompanying the mood symptoms are behavioral symptoms such as fatigue, decreased interest, food cravings, sleep disturbance, poor concentration, and physical symptoms, most commonly, abdominal swelling and breast tenderness (see Table 2).
The most prevalent premenstrual symptoms as identified in a large, cross-sectional survey are physical symptoms: abdominal bloating, cramps or abdominal pain, and breast tenderness, followed by irritability and mood swings.5 For clinical conditions, it is essential to consider severity of the symptoms, which have been shown to be directly proportional to their duration.6
Some studies suggest that irritability and tension are the cardinal symptoms of the syndrome.7, 8, 9 Although depressive symptoms such as low mood, fatigue, appetite changes, sleep difficulties, and decreased concentration are frequent symptoms of women with PMS, increasing evidence suggests that PMS is not simply a variant of depression but has distinct underlying mechanisms that differ from those of other depressive disorders.10
Premenstrual Exacerbation of Symptoms and Comorbidity
Premenstrual exacerbation of the symptoms of another underlying medical or psychiatric disorder is common. For example, more the 50% of patients experiencing major depression reported a clear-cut premenstrual exacerbation of their symptoms.11 Among the most common medical disorders that may be exacerbated premenstrually include asthma,12, 13 migraine,14 seizure disorders,15 allergies, thyroid disorders, irritable bowel syndrome, and chronic fatigue syndrome.3
The premenstrual phase may represent a vulnerable time for women with mood disorders to have worsening symptoms of severe depression.11 A lifetime history of depression ranges from approximately 20% to 76% in samples of women with PMS or PMDD.16 The premenstrual phase is a risk factor for exacerbations of panic symptoms in women with panic disorder.17, 18 Severe premenstrual symptoms were associated with increased alcohol use premenstrually.19, 20 A family history of alcoholism was related to premenstrual alcohol consumption and the severity of premenstrual symptoms.21 Premenstrual exacerbation of symptoms may occur in other conditions such as schizophrenia.22
Alternatively, the premenstrual symptoms may be distinct from those of the underlying disorder and indicate PMS in conjunction with another diagnosis (comorbidity). The most common comorbid diagnosis with PMS may be dysmenorrhea. There appears to be a strong association among mood disorders that occur with the menstrual cycle, postpartum, and in the perimenopause.23, 24, 25 A history of premenstrual depression is a risk factor for postpartum depression26 and menopausal symptoms.27 There is some preliminary evidence that PMS over time may progress to clinical depression in some women.28, 29, 30
Prevalence
Surveys indicate that PMS is among the most common health problems reported by women of reproductive age,31, 32 and up to 40% of menstruating women experience some difficulty with the symptoms.33, 34
In a population-based survey of 1194 women, classification of the premenstrual symptoms using an empirically derived algorithm showed that 16% had minimal symptoms, 67% had moderate symptoms, 12.6% had severe symptoms, and 4.5% had PMDD.35
In another recent population-based survey, the prevalence of PMDD in the population of reproductive-aged women was estimated at 6%, with an additional 19% identified as near-threshold cases that were highly symptomatic but had four rather than five symptoms as required for the PMDD diagnosis.36 In yet another community-based study, 8% of menstruating women had severe premenstrual symptoms and 14% had moderate premenstrual symptoms that were significantly associated with functional impairment.7 These estimates consistently suggest that approximately 20% of women experience severe premenstrual symptoms and are consistent with the clinical evidence that many women who seek treatment for PMS do not meet the stringent criteria for PMDD.37
Risk Factors
Reports of risk factors for PMS have been inconsistent and contradictory. In a current population-based study, symptom severity decreased with age and with oral contraceptive use.35 Greater symptom severity was associated with comorbidities. Racial differences were observed, with Hispanics reporting greater symptom severity, Asians reporting less symptom severity, and blacks reporting the same symptom severity compared with whites. Symptom severity was not associated with education, employment, marital status, number of children, strenuous exercise, or current smoking.35 Other risk factors that have been suggested include nulliparity,38 earlier age at menarche,39, 40 higher body mass index,10, 39 greater alcohol consumption,39, 41, 42, 43 more caffeine consumption,43 and higher levels of perceived stress.39, 41 Oral contraceptive use38, 44 and regular physical activity45, 46 have been identified as protective factors.
Costs of Premenstrual Syndrome
The morbidity of PMS is caused by its severity, chronicity, and resulting impairment in work, relationships, and activities. PMS appears to be a chronic disorder, with one-quarter to one-half of the nonpregnant reproductive lifespan compromised by disruptive symptoms that return in the luteal phase of each menstrual cycle.
The level of impairment as assessed by standard measures is significantly higher than community norms and is similar to that of major depressive disorder.47 Studies show that women with PMS report the greatest impairment in relationships34, 47, 48 and compromised work levels.34, 47 Moderate to severe PMS/PMDD is associated with increased work absenteeism and less productivity,49 although the limited evidence is not consistent.50, 51 It appears that functioning in PMS/PMDD is impaired, but the impairment is correlated with dysphoric mood symptoms47, 51 and not with decrements in memory or learning.52, 53
Inadequate treatment of mood disorders increases the costs of medical care and lost productivity.54, 55 Reports show that even subsyndromal symptoms of dysphoric mood disorders are associated with increased medical and mental health services.56, 57 A population-based study of PMDD reported that as premenstrual symptom severity increased, the likelihood of health care service use increased for visits to the emergency department, obstetrician/gynecologist, or alternative medicine providers.51
ETIOLOGY
Understanding of the etiology of PMS remains limited. Circulating levels of reproductive hormones are normal,58, 59 although there may be an underlying vulnerability to the normal fluctuations of one or more of these hormones.3, 60 The biochemical changes of PMS are believed to involve central nervous system-mediated interactions of the reproductive steroids with neurotransmitters.60 Serotonergic dysregulation is supported by the most evidence at the present time. There is also evidence of dysregulation of gamma amino butyric acid (GABA) receptor functioning in women's mood disorders.61, 62, 63, 64 Negative mood symptoms in some women may be associated with paradoxical effects of GABA-A modulators.65
Serotonin
Evidence suggests that serotonergic activity plays varying roles in the modulation of PMS. Indications of abnormalities in markers of serotonergic transmission in women with severe PMS include evidence of a lowered platelet imipramine binding (a peripheral marker of serotonin [5-hydroxytryptamine, 5-HT] function) in the luteal phase,62 decreased platelet 5-HT content and 5-HT uptake during the luteal phase,66, 67 and significantly decreased whole blood 5-HT levels premenstrually.68 PMS patients showed a lower 5-HT response to tryptophan (a 5-HT precursor) during the luteal phase compared with the follicular or mid luteal phase.69 Another study found no differences in platelet 5-HT2A receptor binding in PMDD patients compared with controls, but untreated PMDD women had a higher number of [3H]paroxetine binding sites in the follicular phase compared with healthy controls, a difference that disappeared with buserelin treatment, a GnRH agonist.70 These findings contribute to the hypothesis that serotonergic transmission is involved in PMS. Parry provides an extensive review of the role of central serotonergic dysfunction in PMS/PMDD.71
Results of challenge tests and studies to elucidate the mechanisms of PMS also provide evidence of serotonergic involvement in PMS symptoms. Depleting the 5-HT precursor tryptophan provoked PMS symptoms,72 while conversely, tryptophan supplementation relieved PMS symptoms.73, 74 d-Fenfluramine, which releases serotonin and blocks its uptake, blocked food cravings and improved depressed mood in a controlled study of PMS subjects.75 Prolactin responses to buspirone challenge (a partial 5-HT1A receptor agonist) were blunted in the follicular phase of women with late luteal phase disorder but not in healthy controls, suggesting that the subsensitivity of the 5-HT1a receptor may be a trait marker for the disorder.76
m-Chlorophenylpiperazine (m-CPP), a serotonin agonist, decreased symptoms in women with PMDD.77 Women with PMDD who received metergoline (a serotonin receptor antagonist) experienced the return of PMDD symptoms compared with healthy comparisons who did not.78
Animal experiments suggest that serotonin has inhibitory effects on aggression and irritability, which is a predominant symptom of PMS.8 Fluoxetine reduced aggressive behavior that was elicited by administration of estradiol and progesterone to ovariectomized rats.79 Inhibition of serotonin reuptake reduced depression in animal models80 but also reduced sexual receptivity in estrous rats.81 These animal models suggest links between serotonergic transmission and cycle-dependent behaviors associated with steroid hormones.
The predominant evidence for involvement of the serotonergic (5-HT) system is the clear response of PMS and PMDD patients to serotonergic antidepressants, including fluoxetine,82, 83, 84, 85, 86, 87 sertraline,88, 89, 90, 91, 92 paroxetine,93, 94, 95 citalopram,96 venlafaxine,97, 98and clomipramine.99, 100 The satisfactory response rates in these studies range from 52% to 69%, with placebo improvement ranging from 15% to 47%. Furthermore, the response to serotonin reuptake inhibitor (SSRI) appears to be more rapid in treatment for PMS than is commonly observed for other depressive disorders. The observations of a swift response to SSRIs led to symptom-onset dosing for PMS/PMDD, and preliminary data suggest the feasibility of this approach.101, 102 While treatment response indicates that serotonergic medications can control PMS symptoms, the pharmacologic reasons for this are not known. It is speculated that the mechanism of action in PMS differs from that of other mood disorders or that SSRI treatment corrects an underlying serotonergic dysfunction.
Sex Steroids
Although serotonergic activity appears to modulate PMS symptoms, it is unlikely that it is the causal factor. It is also unlikely that the gonadal steroids are the causal factor, although it appears that PMS requires the sex steroids.60 No consistent differences in progesterone and estradiol levels have been identified between women with PMS and controls. The dominant theoretical view is that the normal gonadal steroid fluctuations of the menstrual cycle trigger an abnormal serotonergic response in vulnerable women.
The strongest evidence of the involvement of the sex hormones is the response of women with PMS and no other comorbid condition to GnRH suppression of ovulation, which consistently relieves PMS symptoms.60, 103, 104, 105, 106, 107, 108, 109 Further strong evidence of a necessary association of the gonadal steroids in PMS is from a controlled study that showed that PMS symptoms were induced with physiologic doses of estradiol and progesterone in PMS subjects but not in asymptomatic controls.60 Manipulation of peripheral levels of ovarian steroids with induction of menses by mifepristone with or without preserving the corpus luteum with human chorionic gonadotropin did not change the premenstrual symptoms in women with carefully diagnosed PMDD.110 This evidence indicated that the hormonal effects associated with PMS may occur before the luteal phase of the cycle.
The progesterone metabolite, allopregnanolone, modulates GABA receptor functioning similar to the barbiturates and benzodiazepines and can mimic the anxiolytic effect of these agents.111, 112 PMS shares clinical features such as comorbidity with panic disorder, panic-type responses to lactate infusion, or carbon dioxide inhalation,113, 114, 115 and moderate response to benzodiazepine therapy with GABA-mediated anxiety disorders.116 Studies suggest that allopregnanolone levels in PMS subjects may be related to symptom severity,117, 118, 119, 120, 121 and that the responsiveness of the GABAa receptor complex may be altered in women with PMS.122 Responses to an intravenous L-tryptophan challenge in women with premenstrual symptoms provided evidence for a possible interaction between the serotonergic system and allopregnanolone.123 There is some evidence that SSRIs increase activity of the enzyme that produces allopregnanolone in human brains,124 but this remains a theoretical possibility in PMS at present.
Progesterone deficiency was long believed to be the cause of PMS. However, there is no consistent evidence of altered progesterone levels in women with PMS,58, 125, 126 and progesterone therapy has clearly been shown to be not better than a placebo.127, 128, 129, 130 The apparent contradiction between the role of gonadal steroids in PMS and the lack of effect of progesterone therapy may be related to the variability in conversion of progesterone to the active metabolite allopregnanolone,61, 131, 132 with a consequent lack of sufficiently high CNS levels of 3 α-reduced metabolites premenstrually in some women.61, 133
Beta-Endorphin
Beta-endorphin was hypothesized to be involved in the etiology of PMS because of its characteristics that include inhibition of gonadotropin release during the luteal phase; modulation of biogenic amine, prostaglandin, vasopressin, and carbohydrate pathways; and influence on mood changes, pain perception, thirst, and appetite. Symptoms of increased beta-endorphin level (anxiety and agitation) and features of opiate withdrawal (dysphoria, mood lability, lethargy, reduced motor activity, and heightened libido) resemble PMS. Halbreich and Endicott hypothesized “that a premenstrual decrease of levels of endorphin may be involved in the pathophysiology of an atypical, depressive premenstrual syndrome, while deregulation of endorphins may be involved in that of an anxious/agitated/depressive syndrome.”134 Administration of the antagonist naloxone in high doses produced PMS-like symptoms in normal women.135 Chuong and associates described a decrease in serum beta-endorphin compared with the follicular phase levels in women with PMS,136 results that were subsequently replicated.137, 138 Administration of naltrexone in the ovulatory days of the cycle to prevent a beta-endorphin peak and consequent luteal phase withdrawal decreased premenstrual symptoms.139
Swelling in the premenstruum is commonly reported by women, but there is no good evidence of differences in sodium or body water in the luteal phase compared with the follicular phase. There is no consistent premenstrual weight gain in women with PMS and no correlation between symptom severity and edema.140, 141 Based on an altered water-to-potassium ratio, it was suggested that fluid redistribution best explained the bloating reported in PMS.141 An analogous model to consider is idiopathic cyclic edema. Patients with cyclic edema have an exaggerated autonomic response to the upright posture that thereby activates both the catecholamine and the renin-angiotensin pathways.142 Renal dopamine, a diuretic and natriuretic that antagonizes the renin-angiotensin-aldosterone system and norepinephrine, is reduced.143 Investigation of dopamine metabolism in women with PMS may reveal value for dopaminergic agents, as has been shown for women with idiopathic edema.144
Prostaglandins
Prostaglandins are ubiquitous, and PMS symptoms touch most organ systems. CNS prostaglandins act as neurotransmitters to modify thirst, appetite, temperature, mood, vascular tone, seizure threshold, and hormones such as vasopressin. The prostaglandin synthetase inhibitor mefenamic acid improved symptoms of fatigue, mood swings, and irritability in women with PMS.145 It is not known whether the prostaglandin inhibition directly reduced these symptoms or whether the improvement resulted from correction of dysmenorrhea, a well-known benefit of nonsteroidal anti-inflammatory drug therapy, which in turn reduced other PMS symptoms. Low serum levels of the essential fatty acid prostaglandin precursor, cis-linoleic acid, were observed in women with PMS.146 However, review of seven placebo-controlled clinical trials of evening primrose oil for the treatment of PMS found no benefits greater than placebo.147
Genetic Factors
Genetic factors may be important in PMS. Study of twins indicated that premenstrual symptoms of depression and anxiety were moderately stable over time and strongly inheritable.148 The researchers concluded that the genetic and environmental risk factors for these premenstrual symptoms were not closely related to the genetic risk factors for lifetime depression. Another study found that the concordance for PMS in monozygotic twins was twice that if the twins were dizygotic twins.149 Preliminary genetic findings suggest that there is a risk association with genetic variation in ESR1, an estrogen receptor alpha gene.150
DIAGNOSIS
Premenstrual syndromes are diagnosed on the basis of the timing of the symptoms, which cross emotional, behavioral, and mood domains. For a diagnosis of PMS, the symptoms must occur during the 2 weeks before menses and subside during the menstrual flow. With remission of the symptoms, a symptom-free period occurs in the follicular phase between menses and ovulation. Clinically significant PMS is determined by the patient's seeking treatment and/or report of impaired functioning in relationships, work, or other activities. For a diagnosis of pure PMS, the symptoms must not be accounted for by other physical or psychiatric disorders. There are no hormonal measures, other laboratory tests, or physiologic measures that identify PMS. Such tests are useful only to identify or rule out other disorders that may be suspected in the diagnostic evaluation.
The most frequently reported symptoms of PMS include irritability, anxiety, nervous tension, mood swings, fatigue, depression, feeling overwhelmed or out of control, physical symptoms of swelling or bloating of the abdomen or extremities, appetite changes and food cravings, aches, and breast tenderness (see Table 2).
The specific symptoms appear to have little importance for the diagnosis. The critical elements are the relationship to menses, severity, and the degree of functional impairment. Women who seek medical treatment usually describe multiple symptoms, with the primary focus and most distressing problems typically focused on the mood and behavioral symptoms. Physical symptoms are widely experienced by women who do not perceive problems with premenstrual distress and are seldom sufficient for a clinical diagnosis of PMS without other mood or behavioral symptoms.
Premenstrual Syndrome
Diagnostic criteria for PMS are presented in the ACOG Practice Bulletin 15 of 2000.3 At least one of the listed affective or somatic symptoms must be experienced during the 5 days before menses in three prior menstrual cycles (Table 3) and relieved with the menstrual flow. The symptoms should be confirmed by two cycles of prospective reports. The symptoms cause identifiable impairment in the patient's functioning and are not accounted for by other physical or emotional disorders.
Table 3. ACOG Diagnosis of Premenstrual Syndrome
| Symptoms consistent with PMS that may include: | |
| Affective symptoms: depression, angry outbursts, irritability, anxiety, confusion, social withdrawal | |
| Somatic symptoms: breast tenderness, abdominal bloating, headache, swelling of extremities | |
| Restriction of these symptoms to the luteal phase of the menstrual cycle assessed prospectively | |
| Impairment of some facet of the woman's life | |
| Exclusion of other diagnoses that may better explain the symptoms |
(American College of Obstetricians and Gynecologists. ACOG Practice Bulletin 15; 2000)
Premenstrual Dysphoric Disorder
The diagnostic criteria for PMDD are listed in the DSM-IV.1 These criteria were intended to diagnose a severe dysphoric form of PMS. The symptoms must be severe premenstrually and minimal or absent after menses. At least five of the 11 listed PMDD symptoms, including one or more of the mood symptoms, must meet these criteria. Physical symptoms, regardless of the number, are counted as a single symptom (Table 4). The symptoms must markedly interfere with functioning and not simply be an exacerbation of another physical or mental disorder. All criteria must be confirmed by prospective daily ratings for at least two menstrual cycles.
Table 4. Symptoms required to diagnose PMDD
| Depressed mood |
| Anxiety/tension |
| Mood swings |
| Irritability |
| Decreased interest |
| Fatigue |
| Concentration difficulties |
| Appetite changes/food cravings |
| Insomnia/hypersomnia |
| Feeling out of control |
| Physical symptoms |
PMDD, premenstrual dysphoric disorder
Five or more symptoms must be severe premenstrually and remit after menses (Adapted from American Psychiatric Association1)
There is no gold standard for operationalizing the premenstrual severity and postmenstrual remission level required for a PMDD diagnosis. The dependence of the diagnosis on subjective report of five specified symptoms without a standard method of determining severe and minimal levels results in marked differences among study samples identified as PMDD. Smith and associates demonstrated that the number of subjects identified by the PMDD criteria varies markedly by the rating scale used for symptom assessment.151 Increasing evidence indicates that approximately 5–8% meet stringent PMDD criteria.35, 36 However, approximately 20% of women may experience severe PMS but not meet the PMDD criteria.35 There is no evidence that treatment response differs between a PMDD or PMS diagnosis in the few studies that have examined this issue.129, 152, 153
Differences Between Premenstrual Syndrome and Premenstrual Dysphoric Disorder
The most obvious difference between the PMS and PMDD diagnosis is the number of symptoms required. PMDD requires five of 11 identified symptoms; the ACOG diagnosis of PMS requires only one severe symptom consistent with PMS. The diagnoses are otherwise identical in their requirements for the menstrually related symptom pattern, confirmation by prospective ratings of the symptoms, impaired functioning and identification of other disorders that could account for the symptoms.
The diagnosis of PMS and PMDD continues to be made from the patient's report of symptoms on a daily basis for at least two menstrual cycles. Numerous scales for daily symptom rating have been published and are available for use (Table 5). Daily symptom reports may be viewed as difficult to use in the primary care setting, but such reports can also help the busy clinician by swiftly demonstrating the patient's symptoms and indicating whether they are in fact linked to the menstrual cycle in the requisite pattern. Many women who report PMS will not confirm that the symptoms occur only premenstrually in daily symptom reports. Daily symptom reports are also helpful in indicating that there may be other comorbidities when the reports show that symptoms occur randomly or throughout the menstrual cycle. The daily symptom reports are also an important educational tool for the patients. Patients can observe the patterns and severity of their symptoms over the menstrual cycle and gain an increased sense of control.
Table 5. Assessment instruments for PMS/PMDD
| Instrument | Name | # Items | To diagnose | To assess symptoms | Reference | |
| PMS | PMDD | |||||
| COPE | Calendar of premenstrual experiences | 22 | 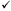 | 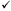 | Mortola et al., 1990154 | |
| DRSP | Daily record of severity of problems | 24 | 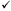 | 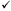 |  | Endicott & Harrison, 1996155 |
| DSR | Penn daily symptom rating | 17 |  |  |  | Freeman et al., 1996156 |
| MDQ | Menstrual distress questionnaire | 48 | 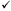 | 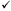 | 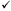 | Moos, 1968157 |
| PAF | Premenstrual assessment form | 96 | 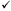 | Halbreich et al., 1982158 | ||
| PMSD | Premenstrual symptom diary | 17 | 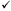 | 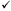 | Thys-Jacobs et al., 1995159 | |
| PMTO | Premenstrual tension scale-observer | 10 | 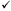 | Steiner et al., 1980160 | ||
| VAS | Visual analogue scales | Open | 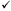 |  |  | Rubinow et al., 1984;161 Steiner et al., 1999162 |
A medical history (with emphasis on reproductive events, mood disorders, and family history of PMS and other mood disorders), complete physical examination, and a gynecologic examination are important for the diagnosis. By definition, PMS occurs with regular ovulatory menstrual cycles in the normal range; irregular cycles require further gynecologic investigation.
Comorbid conditions should be identified, including dysmenorrhea, endometriosis, ovarian cysts, uterine fibroids, pelvic inflammatory disease, seizure disorders, migraine, thyroid disorders, asthma, allergies, diabetes, hepatic dysfunction, cancer, lupus, anemia, and infections. Psychiatric conditions that must be considered include mood disorders, substance abuse, eating disorder, anxiety disorders, and personality disorders (Table 6). It may be difficult to determine whether the symptoms are an exacerbation of a comorbid condition or PMS symptoms superimposed on another condition. In either case, the usual recommendation is to treat the underlying condition first, and then reassess and possibly add treatment for the symptoms that arise premenstrually.
Table 6. Differential Diagnosis of PMS
| Medical disorders | Psychiatric disorders |
Dysmenorrhea Endometriosis Ovarian cysts Uterine fibroids Hypothyroidism Seizure disorders Autoimmune disorders Asthma Allergies Diabetes Anemia | Major depression Dysthymia Bipolar illness Generalized anxiety Panic Substance abuse Eating disorders
|
At least two visits should be considered for the diagnostic evaluation. Evaluating the patient when she is premenstrual usually confirms the severity of the symptoms, but it is difficult to determine their overlap with other conditions. It is diagnostically useful to see the patient after menses when symptoms have abated. If symptoms are absent, it provides convincing evidence for the diagnosis. However, if symptoms are present in the follicular phase, the type and severity of the symptoms provide important diagnostic information for other comorbid conditions.
TREATMENT
Effective treatments demonstrated by randomized placebo-controlled trials are available for PMS and PMDD. Accurate diagnosis is the first step. Support, education, symptom charting, and attention to health behaviors related to diet, exercise, alcohol, nicotine, caffeine, and stress management can be helpful, but if symptoms remain severe and interfere with the patient's usual functioning, pharmacologic treatment should be tried.
Nonpharmacologic Treatment
Numerous nonpharmacologic approaches have been advocated for PMS, but few are supported by solid empirical evidence.47, 163
Nutritional Supplements
CALCIUM
A large multicenter, randomized, double-blind study of calcium supplementation (600 mg twice daily) reduced premenstrual depression, fatigue, edema, and pain significantly more than the placebo in women with PMS.164 This is one of the few nonprescription treatments that has been examined in placebo-controlled study. However, the severity of the dysphoric mood symptoms was not indicated, and further information is required to determine the efficacy of this treatment for PMDD.
VITAMIN B6
The rationale for use of vitamin B6 (pyridoxine) is that its physiologically active form is a cofactor in the synthesis of serotonin, dopamine, and certain prostaglandins. There have been numerous studies of vitamin B6 for PMS treatment, but the results are conflicting and inconclusive. A meta-analysis showed that vitamin B6 was approximately twice as likely as placebo to improve PMS symptoms overall, with an odds ratio for improvement in depressive symptoms of 1.69, but the researchers emphasized that there was very low confidence in the results because of the generally poor quality of the studies.165 There was no significant dose response, indicating that the amount of vitamin B6 was not associated with improvement. The use of megadoses of vitamin B6 (exceeding 100 mg/day) was found to cause peripheral neuropathies, an indication that caution and medical oversight are required with supraphysiologic dosing.
CARBOHYDRATES
Dietary alterations that modify tryptophan levels have been shown to have effects on mood and cognition. Dexfenfluramine, which releases brain serotonin and blocks its reuptake, improved premenstrual dysphoric mood and normalized carbohydrate consumption in women with moderate to severe PMS.75 A study of carbohydrate intake in women with PMS indicated that carbohydrate cravings and subsequent carbohydrate intake significantly improved mood shortly thereafter.166 A formulated carbohydrate-rich beverage, which was known to increase tryptophan levels, improved the mood symptoms of PMS in preliminary studies.167, 168
Health Behaviors
Many women know that healthy behaviors related to diet, exercise, alcohol use, nicotine, caffeine, and stress can reduce symptoms, and improving health behaviors may be therapeutic even if it is not specific for premenstrual symptoms. However, changing health behaviors is difficult, and if behavioral changes are recommended and not followed, both the clinicians and the women may become frustrated. This can be avoided by suggesting that a woman reflect on these health behaviors with the goal of making a selection, rather than making a specific recommendation. This approach also avoids a situation in which the patient feels that the clinician is not taking her problem seriously and offers only behavioral changes rather than medication.
STRESS
Stress aggravates premenstrual symptoms as it does other medical conditions, and there is some evidence that stress response is impaired in women with PMS.39, 122 Many women are quite aware of the sources of stress in their lives and, with little intervention other than the physician's encouragement and permission, are able to make significant changes to reduce the stress. Weekly group follow-up visits may facilitate compliance by offering support.169
Behavioral treatments that reduce stress or facilitate coping reduce PMS symptoms. Behavioral treatments that have helped PMDD include cognitive behavioral therapy,170, 171, 172 training in coping skills,173 and relaxation techniques.174
EXERCISE
Regular aerobic exercise has been found to improve mood and to reduce the severity of premenstrual symptoms,175, 176, 177 possibly by increasing beta-endorphin levels in the brain. Estrogen and progesterone receptors in the brain are closely linked to endorphin function.178 Some studies have identified regular physical exercise as a protective factor for PMS,45, 46 but other epidemiologic studies have not found any significant association between exercise and severity of premenstrual symptoms.35
DIET
Dietary modification is one of the most common treatments for premenstrual syndromes but lacks systematic study to determine its effectiveness. Because premenstrual symptoms mimic hypoglycemia, reduction of the intake of simple carbohydrates and eating healthy snacks at regular intervals to avoid extremes of hunger and satiety was traditionally recommended, but no premenstrual alteration of glucose metabolism has been demonstrated.179 In contrast, a carbohydrate meal without protein raised serotonin levels in the brain, improved mood, and reduced food craving.166 Carbohydrate intake improved mood symptoms of PMS167, 168 (see CARBOHYDRATES section). Caffeine may aggravate premenstrual symptoms, and limiting caffeine intake may be therapeutic. Data suggest that women with premenstrual symptoms may self-medicate with caffeine, consequently exacerbating their symptoms.180 The postulate that there is a relationship between caffeine and premenstrual breast soreness is controversial, but many women report improved symptoms after eliminating xanthine beverages. Significant comorbidity between premenstrual syndromes and alcohol abuse means that this should be addressed in the diagnostic evaluation. Denial of substance abuse is characteristic and may significantly hinder and delay the diagnosis. Nicotine use should also be reviewed. Nicotine causes irritability and clinicians note that many women report improvement in premenstrual symptoms when they stop smoking.
Herbal Treatments
Herbal treatments for PMS are used by increasing numbers of women, but scientific information on their efficacy for this disorder remains limited.163 Agnus castus extract (chaste-tree berry) administered daily has been shown to be significantly better than placebo,181, 182, 183 confirming results of previous uncontrolled studies of this treatment.184, 185 This was shown for women with moderate to severe PMS and the treatment reduced symptoms of negative affect and water retention.182 Hypericum perforatum (St John's Wort) was more effective than placebo186, 187 and also decreased premenstrual symptom scores in an uncontrolled study,188 but the severity of the symptoms differed in these studies as did the symtoms that improved, and further studies are needed to determine the efficacy of this commonly used herbal treatment. Evening primrose oil has historically been a popular treatment for PMS, with at least seven placebo-controlled trials, but the well-controlled studies failed to find any beneficial effects for this treatment.147
Behavioral Therapies
Behavioral treatments that reduce stress or facilitate coping may reduce PMS symptoms. Behavioral treatments that have helped PMDD include cognitive behavioral therapy,170, 171, 172, 173, 189 training in coping skills,173, 190 and relaxation techniques.174 A systematic review of cognitive behavioral therapy concluded that the scientific evidence of its efficacy for PMS was insufficient, and that further rigorous evidence is needed.191
Numerous other complementary and alternative therapies showed no convincing evidence of efficacy for PMS in a review of 27 randomized controlled trials (dietary supplements, 13 trials; herbal medicines, seven trials; biofeedback, two trials; homeopathy, relaxation, massage, reflexology, and chiropractic, one trial each).188 Although it is possible that methodologic issues obscured potential results, the researchers concluded that, based on scientific data, none could be recommended as a treatment for premenstrual syndromes.
Bright Light and Sleep Deprivation Therapy
Chronobiologic disturbances such as lower levels of melatonin and earlier offset of melatonin secretion have been found in women with PMS.192 Both bright light therapy and the dim light that was used as the placebo, administered daily for 1 premenstrual week, significantly reduced depressive symptoms in PMDD patients.193 A therapeutic effect was also reported for total sleep deprivation,194 early and late sleep deprivation in PMDD subjects;195 however, the strength of the responses over placebo treatment remain unclear. These interventions may provide alternative or adjunctive treatments for the management of PMS. The studies also suggest a link between dysphoric PMS and major depressive disorder, which has been shown to respond to bright light therapy and sleep deprivation protocols.196
PHARMACOLOGIC TREATMENTS
Serotonergic Antidepressants
The serotonergic antidepressants, particularly the SSRIs, are the first-line treatment for severe PMS and PMDD at this time. Modulating serotonergic function is consistent with the dominant theoretical view that the normal gonadal steroid fluctuations of the menstrual cycle trigger an abnormal serotonergic response in vulnerable women. (Indications of abnormalities in markers of serotonergic transmission are discussed.) The United States Food and Drug Administration (FDA) has approved three SSRIs, fluoxetine, sertraline, and paroxetine, for the indication of PMDD.
Several meta-analyses of randomized controlled trials of SSRIs in treatment of PMS and PMDD concluded that these drugs were an effective first-line therapy.197, 198 Efficacy has been clearly shown in randomized, placebo-controlled, double-blind trials for fluoxetine,82, 83, 84, 85, 86, 87 sertraline,88, 89, 90, 91, 92 paroxetine,93 citalopram,96 venlafaxine,97 and clomipramine.99, 100
Dosing with Serotonin Reuptake Inhibitor
Effective doses of SSRIs are consistently at the low end of the dose range for depression in all reports of PMS treatment (Table 7). Response is usually swift, with the greatest improvement in the first menstrual cycle of treatment and smaller increments with continued use or dose adjustments in the next one to two cycles.198 In the absence of sufficient response or dose-limiting side-effects, the dose should be increased in the second and/or third cycles of treatment. An adequate trial of a serotonergic antidepressant is at least two menstrual cycles at a dose level known to be effective with a third cycle if there is a partial response. If a patient has an insufficient response or unacceptable side-effects with an initial SSRI, it is reasonable to try another SSRI.199 Although all SSRIs have similar side-effects, an individual patient may respond better to one SSRI than another. No clear predictors of response or side-effects have been identified at this time.
| SSRI | Mean Dose (mg/day) | Reference |
| Citalopram (Celexa®) | 20 | 96 |
| Fluoxetine (Prozac®) | 20 | 82, 83, 84, 85, 86, 87 |
| Paroxetine (Paxil®) | 17 | 93 |
| Paroxetine-CR (Paxil-CR®) | 12.5 | 94, 95 |
| Sertraline (Zoloft®) | 80 | 88, 89, 90, 91, 92 |
| Venlafaxine (Effexor®) | 110 | 97, 98 |
Side-Effects of Serotonin Reuptake Inhibitor
Side-effects are common when treatment is initiated but most are transient and disappear during the first treatment cycle. The most common side-effects include headache, nausea, insomnia, fatigue or lethargy, diarrhea, decreased concentration, dizziness, and decreased libido or delayed orgasm.
It may be difficult to determine whether reports about sexual effects are medication-induced if there is no information about sexual functioning before initiating the drug regimen. Some women report that sexual side-effects diminish with time and adjustment to the medication, while others do not. The incidence of decreased sexual interest or delayed orgasm in the few published reports of PMS patients is approximately 9–16%. This is notably lower than the rates in the population of SSRI users, which were recently reported to be 36–43%.200 The PMS/PMDD reports of sexual side-effects are from acute treatment trials that were not designed to include systematic assessment of sexual function, and they do not represent experience with long-term use of medication. Whether there is a true difference between PMS and major depression, with respect to this side-effect, warrants further study.
Luteal Phase Dosing with Serotonin Reuptake Inhibitors
The use of medication only in the symptomatic luteal phase of the menstrual cycle is of particular interest in PMS because of the cyclic pattern of the symptoms, which include a clear symptom-free interval each month. Based on the rapid response of these patients to SSRIs, a number of preliminary studies examined luteal phase dosing regimens with SSRIs and consistently reported efficacy.88, 90, 91, 92, 96, 100 Two large multicenter trials reported efficacy of fluoxetine201 and sertraline202 administered for the last 2 weeks of the menstrual cycle. A meta-analysis of 15 randomized placebo-controlled trial for PMS or PMDD found no significant difference in symptom reduction between continuous and intermittent dosing.203 Results from one controlled study indicated that once weekly dosing in the two luteal phase weeks with a sustained release formulation of fluoxetine (90 mg, enteric-coated) was also effective.204
Luteal phase dosing is typically initiated 14 days before the expected onset of menstrual bleeding and concluded with the onset or within several days of menstrual bleeding. Several preliminary studies suggest the efficacy of symptom-onset dosing, which for many women with PMS is an even shorter time period than the 2-week luteal phase.101, 102
As with continuous dosing, doses of the SSRI are usually low (at the starting dose indicated for depression or at one dose increase), and the medication is well tolerated. There is some suggestion that there may be fewer side-effects with luteal phase dosing, but this remains an open question. It is also possible that the side-effects of SSRIs that usually diminish with adjustment to the medication do not diminish as swiftly with intermittent dosing. Although luteal-phase dosing entails stopping the medication during each menstrual cycle, discontinuation symptoms have not been reported for this dosing regimen for PMS.
Insufficient Response to Serotonergic Antidepressants
The overall response of PMS patients to SSRIs is approximately 60% in controlled trials. No strong predictors of response have been consistently identified.205 An expert consensus group recommended the common clinical practice of shifting to a second SSRI when patients have an insufficient response or are intolerant to the initial SSRI.199 Augmenting an SSRI with other medications has not been systematically studied in PMS treatment. Switching to another class of medication, such as anxiolytics, is suggested, but there are no data that indicate whether nonresponders to an SSRI will respond to another class of medication. Nonresponse may also be caused by other comorbid disorders. A thorough review of the diagnosis and adjustments of the premenstrual doses of medication for the primary disorder should be considered before pursing other treatments for PMS.
The antidepressant response in PMS and PMDD appears to be associated with potent serotonergic activity and is not a general antidepressant effect. Other antidepressants, which are clearly effective for depressive disorders, such as desipramine (a tricyclic noradrenergic antidepressant),88 bupropion (a weak inhibitor of both serotonin and norepinephrine reuptake),86 and maprotiline (a selective noradrenaline reuptake inhibitor),93 were not more effective than the placebo in PMS treatment.
Alprazolam, a benzodiazepine, and buspirone showed modest efficacy for PMS in some studies,129, 206, 207, 208, 209 but not others.210, 211 The advantage of alprazolam is that it can be taken with the onset of premenstrual symptoms. However, the well-known risk of dependence with alprazolam must be considered, and this medication should be tried only when the patient has symptoms clearly limited to the luteal phase (so that the medication is used for no more than 2 weeks in each cycle) and there is no history of substance abuse. The advantage of buspirone is that it does not have the risk of dependency. Its disadvantage is that its onset of action is not immediate like alprazolam and it must be used daily. These anxiolytic medications offer an alternative to antidepressants, but fewer patients responded, and the extent to which patients who did not respond to antidepressants respond to anxiolytics is not known.
Hormonal treatments for PMS are consistent with the evidence of hormonal involvement in the disorder60 and have been advocated for many years despite limited scientific evidence of their efficacy for PMS. Among the most effective hormonal treatments for symptom suppression are the gonadotropin-releasing hormone agonist (GnRHa), leuprolide, administered by monthly injection in depot form, and intranasal buserelin.105, 106 Both significantly reduced premenstrual symptoms in the absence of ongoing depression.103, 104 However, these medications are of limited use because of the risks associated with low estrogen levels that result from the suppression of ovulation, particularly osteoporosis, and these medications are viewed as appropriate primarily as a diagnostic tool or for patients who do not respond to other treatments. Results of investigations of add-back therapy using low-dose estrogen and progesterone in conjunction with a GnRHa are preliminary and do not yet definitively indicate that this is a safe and effective approach for long-term treatment.107, 212, 213 Limited data indicate that tibolone (a selective estrogen enzyme modulator) administered with a GnRHa in PMS treatment protects against the GnRHa bone loss and does not reduce the therapeutic effect of the agonist.214
Danazol, 100–400 mg/day, improved PMS symptoms,215, 216, 217 but unacceptable side-effects including acne, hirsutism, weight gain, voice change, and vaginal dryness are serious limitations of this medication as a PMS treatment.
Historically, there was no consistent scientific evidence of efficacy of oral contraceptives (OCs) as a treatment for severe PMS or PMDD.218, 219 However, recent clinical trials of an oral contraceptive containing a new progestin, an analog of spironolactone with antimineralocorticoid and antiandrogenic activity and a shortened hormone-free interval, consistently showed efficacy for PMDD220, 221 and confirmed earlier preliminary reports of improvement of both the mood and physical symptoms of PMS.222, 223, 224 The FDA approved the low dose oral contraceptive formulation containing drospirenone 3 mg and ethinyl estradiol 20 μg for the indication of PMDD. Another study of women who experienced symptoms each month during the placebo week of the standard oral contraceptive regimen (21/7 days) established that many women experience premenstrual or withdrawal symptoms during the hormone-free week of OC use and that continuous dosing with the OC alleviated these symptoms.225, 226 In another study of an OC containing 20 μg EE and 100 μg levonorgestrel (LNG), one group used the pills in the standard regimen (21/7 days) and another group used only the active tablets for 168 days. The standard regimen group experienced the usual withdrawal or premenstrual symptoms, while the continuous group had less bloating and menstrual pain.227 Current studies are further investigating the efficacy of continous OC dosing with no hormone-free interval over an extended time period for PMS and PMDD.
From a clinical perspective, OCs overall are widely viewed as both improving and worsening PMS symptoms. Combination OCs have estrogenic and progestational effects that vary considerably among the more than 40 compounds available in the United States. Relative absorption of the hormones, peripheral conversion, the degree of follicular development in the placebo interval, individual susceptibility to monophasic or triphasic formulations, and side-effects have large variations among women and are not well understood in relation to PMS. Moreover, OCs can have side-effects of water retention, bloating, appetite changes, and depressed mood, which are also PMS symptoms. Some studies showed that OC users had fewer PMS symptoms than nonusers overall,228 but other investigations found few symptom differences between OC users and nonusers and no differences with respect to mood changes.229 In summary, there is little empirical support for traditional OCs as a treatment for PMS in contrast to new formulations as noted above or menses-free contraception.
Estrogen therapy with dose regimens sufficient to maintain suppression of ovulation significantly decreased the dysphoric mood and physical symptoms of PMS.230, 231, 232 However, estrogen must be cycled with progesterone to reduce the risk of uterine cancer, and the extent to which exogenous progesterone results in return of PMS symptoms remains unclear. Progesterone treatment of PMS was advocated for many years, but numerous studies, including three large randomized controlled trials127, 128, 129 and a meta-analysis of 14 placebo-controlled trials,130 failed to show improvement significantly greater than placebo for the mood and behavioral symptoms of PMS. In another meta-analysis, the authors reported that only two of 17 trials of progesterone treatment met their inclusion criteria and concluded that progesterone was not effective for PMS but neither had the trials proven that it was not.233
Spironolactone
Fluid retention is a common symptom of women with PMS, but there is no evidence that thiazide diuretics are of benefit for this disorder. Although women commonly report weight gain, objective measurements have found fluid redistribution to account for bloating and swelling, not weight gain.136, 137 Spironolactone, an aldosterone antagonist with antiandrogenic properties, has shown a significant reduction in the somatic and affective symptoms of PMS in some but not all studies.234, 235, 236, 237, 238 The usual dose is 100 mg per day during the 14-day luteal phase.
Nonsteroidal Anti-inflammatory Drugs
Prostagladin inhibitors are effective for dysmenorrhea and may be helpful for mild to moderate PMS symptoms.239, 240, 241 It is essential to clarify that dysmenorrhea is a distinct disorder and not PMS. Many women with PMS also have dysmenorrhea, which may be relieved with the prostaglandin inhibitor. Mefanamic acid was studied in placebo-controlled trials and reduced headache, fatigue, pain, tension, irritability and mood swings administered at 500 mg twice daily.240, 241 There are no studies that compare this class of drugs with SSRIs or other medications shown to be effective for PMS or PMDD.
CLINICAL MANAGEMENT OF PREMENSTRUAL SYNDROME
Management of patients who may have PMS begins with review of the patient's daily symptom report together with a physical examination and evaluation of the mood and behavioral symptoms to determine whether there are other physical or emotional problems that may account for the symptoms. As indicated in the ACOG guidelines (see Table 3), the women should meet standard diagnostic criteria and confirm the timing and menstrual relationship of their symptoms with prospective ratings. It is diagnostically useful to examine the patient in the postmenstrual phase of the cycle when the premenstrual symptoms have subsided. Symptoms or problems that are apparent after menses are not PMS and indicate underlying or concomitant problems that may account for the symptoms.
When a diagnosis of clinically significant PMS is confirmed by prospective ratings (preferably for at least two menstrual cycles), medication may be appropriate. The serotonergic antidepressants are the first-line treatment at present. Antidepressant dosages for PMS usually begin at the standard start level for depression. When an SSRI is initiated, some improvement is usually noted in the first cycle of treatment. In cases in which there is no significant improvement or dose-limiting side-effects, the dose can be increased in the second or third cycle of treatment. As a general guideline, two to three menstrual cycles of treatment at adequate dose levels are sufficient to determine response. If the selected antidepressant is not helpful, another SSRI may be effective.
Oral contraceptives are widely used for PMS, particularly outside the United States, but there is little scientific evidence of the efficacy of traditional OCs for this disorder. An OC containing drospirenone 3 mg and ethinyl estradiol 20 μg demonstrated efficacy for PMDD and has FDA approval for the indication. Patient reports and pilot study suggest that continuous OC dosing with no hormone-free interval may be effective for PMS and PMDD.
Most women who seek medical treatment for PMS can be helped with some form of treatment. If symptom relief does not occur with the initial treatment, another approach should be tried. Calcium supplementation has reported efficacy for PMS.156 Dietary alterations, exercise, or stress reduction programs are often helpful, particularly for women with less severe symptoms or in combination with medication. Based on evidence of efficacy, second-line treatments include anxiolytics, spironolactone, oral contraceptives, cognitive behavioral therapies, nutritional supplements, and bright light therapy. GnRHa is highly effective but has limited use for PMS because of the risks of a prolonged hypoestrogenic status. Further treatment recommendations based on levels of evidence are offered in the ACOG Practice Bulletin.3
Long-Term Treatment of Premenstrual Syndrome
Nearly all published studies of treatment efficacy for PMS or PMDD are based on acute treatment of 2–3 months' duration. A number of anecdotal reports and several small pilot investigations suggest that PMS symptoms return within several months if medication is stopped.242, 243, 244, 245 A randomized, placebo-controlled study estimated the time to relapse, comparing short-term and long-term treatment with an SSRI.246 The relapse rate was high in both groups and significantly greater after short-term treatment (4 months) compared with long-term treatment (12 months). The women with severe symptoms prior to treatment were the most likely to relapse. Women's reports suggest that untreated PMS symptoms do not resolve spontaneously, as may occur in depression, but continue for many years. Information from clinical trials indicates that the duration of the disorder before treatment is in the range of 8–10 years. These observations of chronic symptoms and the swift return of symptoms after stopping medication suggest that long-term maintenance treatment maybe appropriate for patients with clinically significant PMS.
Placebo Response
The placebo response is reliable, ubiquitous, and can be substantial and prolonged.247 Large, multicenter, randomized, double-blind treatment trials reported placebo responses up to 48%.89, 201, 202
Although placebo effects are the bane of clinical trials, which must demonstrate that the studied treatment effect significantly exceeds the nonspecific effects in improvement of the treated condition, the nonspecific effects of medical treatment can also positively influence and enhance patient outcomes.248, 249 In a study of characteristics of placebo responses in medical treatment of PMS, 20% of placebo-treated subjects showed sustained improvement for the 4-month duration of the investigation.250 Another 42% showed partial improvement with placebo treatment, while 39% were clearly unimproved in the 4 months of treatment. It appeared that some patients with severe PMS experienced significant and sustained improvement in response to the placebo, indicating the importance of nondrug factors in clinical care. Patients who sustained improvement for at least 2 consecutive months were more likely to remain improved. However, it is underscored that most PMS patients reported only partial or no improvement with placebo treatment and that effective pharmacologic treatment is also needed.
SUMMARY
Emerging from a long history with little understanding and many treatments of doubtful effect, clinically significant PMS is now recognized as a chronic disorder that impairs psychosocial functioning for a sizable number of women. Serotonergic antidepressants are the first-line treatment at this time. Using these medications only in the symptomatic luteal phase is effective for women with a diagnosis of clinically significant PMS or PMDD without other comorbid disorders. Recent evidence of efficacy of a new low-dose oral contraceptive formulation and altered dosing regimens of the OCs that reduce the hormone-free interval offer another class of medication for PMS treatment, particularly for women who also want contraception.
Beyond the efficacy of treatments that are demonstrated in short-term clinical trials, the cost-benefit issues of long-term maintenance of medication remain unanswered. While clinical experience dictates the use of augmentation strategies for patients who experience no response or a partial response to medications, there are no systematic studies that provide guidance for such approaches. There are also no studies of treatment strategies for premenstrual exacerbation of other disorders, a condition that may be more common than pure PMS. Finally, neuroendocrine studies to identify pathways that link the gonadal and serotonergic systems to the symptoms manifested in PMS and PMDD remain an important area for identifying the etiology of the disorder.
REFERENCES
American Psychiatric Association: Diagnostic and Statistical Manual of Mental Disorders. p 350, 4th ed. Washington, DC, American Psychiatric Association, 1994 |
|
Hamilton JA, Parry BL, Alagna S: Premenstrual mood changes: A guide to evaluation and treatment. Psychiatr Ann 14:426, 1984 |
|
ACOG Practice Bulletin: Premenstrual Syndrome. Int J Gynecol Obstet 73:183, 2001 |
|
American Psychiatric Association: Diagnostic and Statistical Manual of Mental Disorders. 3rd ed revised. Washington, DC, American Psychiatric Association, 1987 |
|
Dennerstein L, Lehert P, Backstrom TC et al: Premenstrual symptoms -- severity, duration and typology: an international Menopause Int. 2009 Sep;15(3):120-6. |
|
Dennerstein L, Lehert P, Keung LS et al: A population-based survey of Asian women's experience of premenstrual symptoms. Menopause Int. 2010 Dec;16(4):139-45. |
|
Angst J, Sellaro R, Stolar M et al: The epidemiology of perimenstrual psychological symptoms. Acta Psychiatr Scand 104:110, 2001 |
|
Eriksson E: Serotonin reuptake inhibitors for the treatment of premenstrual dysphoria. Int Clin Psychopharmacol 14:(S2):527, 1999 |
|
Eriksson E, Andersch B, Ho HP et al: Premenstrual dysphoria: An illustrative example of how serotonin modulates sex-steroid-related behavior. CNS Spectr 6:141, 2001 |
|
Endicott J, Amsterdam J, Eriksson E et al: Is premenstrual dysphoric disorder a distinct clinical entity? J Womens Health Gend Based Med 8:663, 1999 |
|
Endicott J: The menstrual cycle and mood disorders. J Affect Disord 29:193, 1993 |
|
Ensom MH, Chong E, Carter D: Premenstrual symptoms in women with premenstrual asthma. Pharmacotherapy 19:374, 1999 |
|
Chandler MH, Schuldheisz S, Phillips BA et al: Premenstrual asthma: The effect of estrogen on symptoms, pulmonary function, and beta Z-receptors. Pharmacotherapy 17:224, 1997 |
|
Silbertstein SD: Hormone-related headache. Med Clin North Am 85:1017, 2001 |
|
Rosciszewska D: Analysis of seizure dispersion during menstrual cycle in women with epilepsy. Monogr Neural Sci 5:280, 1980 |
|
Yonkers KA: The association between premenstrual dysphoric disorder and other mood disorders. J Clin Psychiatry 58:(S15):19, 1997 |
|
Kaspi SP, Otto MW, Pollack MH et al: Premenstrual exacerbation of symptoms in women with panic disorder. J Anxiety Disord 8:131, 1994 |
|
Fava M, Pedrazzi F, Guaraldi GP et al: Comorbid anxiety and depression among patients with late luteal phase dysphoric disorder. J Anxiety Disord 6:325, 1992 |
|
Tobin MB, Schmidt PJ, Rubinow DR: Reported alcohol use in women with premenstrual syndrome. Am J Psych 151:1503, 1994 |
|
Mello NK, Mendelson JH, Lex BW: Alcohol use and premenstrual symptoms in social drinkers. Psychopharmacology 101:448, 1990 |
|
McLeod DR, Foster GV, Hoehn SR et al: Family history of alcoholism in women with generalized anxiety disorder who have premenstrual syndrome: Patient reports of premenstrual alcohol consumption and symptoms of anxiety. Alcohol Clin Exp Res 18:664, 1994 |
|
Choi SH, Kang SB, Joe SH: Changes in premenstrual symptoms in women with schizophrenia: A prospective study. Psychosom Med 63:820, 2001 |
|
Pearlstein TB, Frank E, Rivera-Tovar A et al: Prevalence of axis I and axis II disorders in women with late luteal phase dysphoric disorder. J Affective Disord 20:129, 1990 |
|
Stewart DE, Boydell KM: Psychologic distress during menopause: Associations across the reproductive life cycle. Int J Psych Med 23:157, 1993 |
|
Warner P, Bancroft J, Dixson A et al: The relationship between perimenstrual depressive mood and depressive illness. J Affect Disord 23:9, 1991 |
|
O'Hara MW, Schlechte JA, Lewis DA et al: Prospective study of postpartum blues. Arch Gen Psychiatry 48:801, 1991 |
|
Dennerstein L, Smith AM, Morse C et al: Menopausal symptoms in Australian women. Med J Aust 159:232, 1993 |
|
Endicott J, Halbreich U: Clinical significance of premenstrual dysphoric changes. J Clin Psych 49:486, 1988 |
|
Endicott J: The menstrual cycle and mood disorders. J Affect Disord 29:193, 1993 |
|
Graze KK, Nee J, Endicott J: Premenstrual depression predicts future major depressive disorder. Acta Psychiatr Scand 81:201, 1990 |
|
Brown WJ, Doran FM: Women's health: Consumer views for planning local health promotion and health care priorities. Aust N Z J Public Health 20:149, 1996 |
|
Corney RH, Stanton R: A survey of 658 women who report symptoms of premenstrual syndrome. J Psychosom Res 35:471, 1991 |
|
Singh BB, Berman BM, Simpson RL: et al: Incidence of premenstrual syndrome and remedy usage: A national probability sample study. Altern Ther Health Med 4:75, 1998 |
|
Campbell EM, Peterkin D, O'Grady K et al: Premenstrual symptoms in general practice patients: Prevalence and treatment. J Reprod Med 42:637, 1997 |
|
Sternfeld B, Swindle R, Chawla A et al: Severity of premenstrual symptoms in a health maintenance organization population. Obstet Gynecol 99:1014, 2002 |
|
Wittchen H-U, Becker E, Lieb R et al: Prevalence, incidence and stability of premenstrual dysphoric disorder in the community. Psychol Med 32:119, 2002 |
|
Steiner M, Born L: Advances in the diagnosis and treatment of premenstrual dysphoria. CNS Drugs 13:287, 2000 |
|
Woods NF, Most A, Dery GK: Prevalence of perimenstrual symptoms. Am J Public Health 72:1257, 1982 |
|
Deuster PA, Adera T, South-Paul J: Biological, social and behavioral factors associated with premenstrual syndrome. Arch Fam Med 8:122, 1999 |
|
Huerta-Franco MR, Malacara JM: Association of physical and emotional symptoms with the menstrual cycle and life-style. J Reprod Med 38:448, 1993 |
|
Ramcharan S, Love EJ, Fick GH et al: The epidemiology of premenstrual symptoms in a population-based sample of 2650 urban women: Attributable risk and risk factors. J Clin Epidemiol 45:377, 1992 |
|
Tobin MB, Schmidt PJ, Rubinow DR: Reported alcohol use in women with premenstrual syndrome. Am J Psychiatry 151:1503, 1994 |
|
Caan B, Duncan D, Hiatt RA et al: Association between alcoholic and caffeinated beverages and premenstrual syndrome. J Reprod Med 38:630, 1993 |
|
Johnson SR, McChesney C, Bean JA: Epidemiology of premenstrual symptoms in a nonclinical sample. I. Prevalence, natural history and help-seeking behavior J Reprod Med 33:340, 1988 |
|
Gannon L, Luchetta T, Pardie L et al: Perimenstrual symptoms: Relationships with chronic stress and selected lifestyle variables. Behav Med 15:149, 1989 |
|
Choi PYL, Salmon P: Symptom changes across the menstrual cycle in competitive sportswomen, exercisers and sedentary women. Br J Clin Psychol 34:447, 1995 |
|
Pearlstein TB, Halbreich U, Batzar ED et al: Psychosocial functioning in women with premenstrual dysphoric disorder before and after treatment with sertraline or placebo. J Clin Psychiatry 61:101, 2000 |
|
Kuczmierczyk AR, Labrum AH, Johnson CC: Perceptions of family and work environments in women with premenstrual syndrome. J Psychosom Res 36:787, 1992 |
|
Heinemann LA, Minh TD, Filonenko A et al: Explorative evaluation of the impact of severe premenstrual disorders on workabsenteeism and productivity. Womens Health Issues. 2010 Jan-Feb;20(1):58-65. |
|
Hallman J, Georgiev N: The premenstrual syndrome and absence from work due to illness. J Psychosom Obstet Gynaecol 6:111, 1987 |
|
Chawla A, Swindle R, Long S: Premenstrual dysphoric disorder: Is there an economic burden of illness? Med Care 40:1101, 2002 |
|
Morgan M, Rapkin AJ, D'Ella L et al: Cognitive functioning in premenstrual syndrome. Obstet Gynecol 88:961, 1996 |
|
Resnick A, Perry W, Parry B et al: Neuropsychological performance across the menstrual cycle in women with and without premenstrual dysphoric disorder. Psychiatry Res 77:147, 1998 |
|
Hall RCW, Wise MG: The clinical and financial burden of mood disorders--cost and outcome. Psychosom 36:S11, 1995 |
|
Simon GE, Vonkorff M, Barlow W: Health-care costs of primary-care patients with recognized depression. Arch Gen Psychiatry 52:850, 1995 |
|
Johnson J, Weissman MM, Klerman GL: Service utilization and social morbidity associated with depressive symptoms in the community. JAMA 267:1478, 1992 |
|
Horwath E, Johnson J, Klerman GL et al: Depressive symptoms as relative and attributable risk factors for first-onset major depression. Arch Gen Psychiatry 49:817, 1992 |
|
Rubinow DR, Hoban MC, Grover GN et al: Changes in plasma hormones across the menstrual cycle in patients with menstrually related mood disorder and in control subjects. Am J Obstet Gynecol 158:5, 1988 |
|
Steiner M, Hasket RF, Carroll BJ: Circadian hormone secretory profiles in women with severe premenstrual tension syndrome. Br J Obstet Gynecol 91:466, 1984 |
|
Schmidt PJ, Nieman LK, Danaceau MA et al: Differential behavioral effects of gonadal steroids in women with and in those without premenstrual syndrome. N Engl J Med 338:209, 1998 |
|
Rapkin AJ: Progesterone, GABA and mood disorders in women. Arch Womens Ment Health 2:97, 1999 |
|
Rojansky N, Halbreich U, Zander K et al: Imipramine receptor binding and serotonin uptake in platelets of women with premenstrual changes. Gynecol Obstet Invest 31:146, 1991 |
|
Amin Z, Mason GF, Cavus I et al: The interaction of neuroactive steroids and GABA in the development of neuropsychiatric disorders in women. Pharmacol Biochem Behav 2006;84(4):635-43. Epub 2006 Jul 24. |
|
N-Wihlbäck AC, Sundström-Poromaa I, Bäckström T: Action by and sensitivity to neuroactive steroids in menstrual cycle related CNS disorders. Psychopharmacology (Berl) 2006;186(3):388-401. Epub 2005 Dec 15. |
|
Backstrom T, Haage D, Lofgren M et al: Paradoxical effects of GABA-A modulators may explain sex steroid induced negativemood symptoms in some persons.Neuroscience. 2011 May 13. |
|
Ashby CR Jr, Carr LA, Cook CL et al: Alteration of 5-HT uptake by plasma fractions in the premenstrual syndrome. J Neural Transm (Gen Sect) 79:41, 1990 |
|
Taylor DL, Matthew RJ, Ho BT et al: Serotonin levels and platelet uptake during premenstrual tension. Neuropsychobiology 12:16, 1984 |
|
Rapkin AJ, Edelmuth E, Change LC et al: Whole-blood serotonin in premenstrual syndrome. Obstet Gynecol 70:533, 1987 |
|
Rapkin AJ, Chang LC, Reading AE: Tryptophan loading test in premenstrual syndrome. J Obstet Gynecol 10:140, 1989 |
|
Bixo M, Allard P, Bäckström T et al: Binding of [3H] paroxetine to serotonin uptake sites and of [3H] lysergic acid diethylamide to 5-HT2A receptors in platelets from women with premenstrual dysphoric disorder during gonadotropin releasing hormone treatment. Psychoneuroendocrinology 26:551, 2001 |
|
Parry BL: The role of central serotonergic dysfunction in the aetiology of premenstrual dysphoric disorder: therapeutic implications. CNS Drugs 15:277, 2001 |
|
Menkes DB, Coates DC, Fawcett JP: Acute tryptophan depletion aggravates premenstrual syndrome. J Affect Disorder 32:37, 1994 |
|
Steinberg S, Annable L, Young SN et al: Tryptophan in the treatment of late luteal phase dysphoric disorder: A pilot study. J Psychiatry Neurosci 19:114, 1994 |
|
Steinberg S, Annable L, Young SN et al: A placebo-controlled clinical trial of L-tryptophan in premenstrual dysphoria. Biol Psychiatry 45:313, 1999 |
|
Brzezinski AA, Wurtman JJ, Wurtman RJ et al: d-Fenfluramine suppresses the increased calorie and carbohydrate intakes and improves mood of women with premenstrual depression. Obstet Gynecol 76:296, 1990 |
|
Yatham LN: Is 5HT1A receptor subsensitivity a trait marker for late luteal phase dysphoric disorder? A pilot study Can J Psych 38:662, 1993 |
|
Su T-P, Schmidt PJ, Danaceau M et al: Effect of menstrual cycle phase on neuroendocrine and behavioral responses to the serotonin agonist m-chlorophenylpiperazine in women with premenstrual syndrome and controls. J Clin Endocrinol Metab 82:1220, 1997 |
|
Roca CA, Schmidt PJ, Smith MJ et al: Effects of metergoline on symptoms in women with premenstrual dysphoric disorder. Am J Psych 159:1876, 2002 |
|
Ho H-P, Olsson M, Westberg L et al: The serotonin reuptake inhibitor fluoxetine reduces sex steroid-related aggression in female rats: An animal model of premenstrual irritability? Neuropsychopharmacology 24:502, 2001 |
|
Marvan ML, Chavez-Chavez L, Santana S: Clomipramine modifies fluctuations of forced swimming immobility in different phases of the rat estrus cycle. Arch Med Res 27:83, 1996 |
|
Matuszczyk JV, Larsson K, Eriksson E: Subchronic administration of fluoxetine impairs estrus behavior in intact female rats. Neuropsychopharmacology 19:492, 1998 |
|
Steiner M, Steinberg S, Stewart D et al: Fluoxetine in the treatment of premenstrual dysphoria. N Engl J Med 332:1529, 1995 |
|
Wood SH, Mortola JF, Chan YF et al: Treatment of premenstrual syndrome with fluoxetine: A double-blind, placebo-controlled, crossover study. Obstet Gynecol 80:339, 1992 |
|
Menkes DB, Taghavi E, Mason PA: Fluoxetine treatment of severe premenstrual syndrome. Br Med J 305:346, 1992 |
|
Ozeren S, Corakci A, Yucesoy I et al: Fluoxetine in the treatment of premenstrual syndrome. Eur J Obstet Gynecol Reprod Biol 73:167, 1997 |
|
Pearlstein TB, Stone AB, Lund SA: Comparison of fluoxetine, bupropion, and placebo in the treatment of premenstrual dysphoric disorder. J Clin Psychopharmacol 17:261, 1997 |
|
Su TP, Schmidt PJ, Danaceau MA et al: Fluoxetine in the treatment of premenstrual dysphoria. Neuropsychopharmacol 16:346, 1997 |
|
Freeman EW, Rickels K, Arredondo F et al: Full or half-cycle treatment of severe premenstrual syndrome with a serotonergic antidepressant. J Clin Psychopharmacol 19:3, 1999 |
|
Yonkers KA, Halbreich U, Freeman E et al: Symptomatic improvement of premenstrual dysphoric disorder with sertraline treatment. A randomized controlled trial JAMA 278:983, 1997 |
|
Young SA, Hurt PH, Benedek DM et al: Treatment of premenstrual dysphoric disorder with sertraline during the luteal phase: a randomized, double-blind, placebo-controlled crossover trial. J Clin Psych 59:76, 1998 |
|
Jermain DM, Preece CK, Sykes RL et al: Luteal phase sertraline treatment for premenstrual dysphoric disorder. Results of a double-blind, placebo-controlled, crossover study Arch Fam Med 8:328, 1999 |
|
Halbreich U, Smoller JW: Intermittent luteal phase sertraline treatment of dysphoric premenstrual syndrome. J Clin Psych 58:399, 1997 |
|
Eriksson E, Hedberg A, Andersch B et al: The SRI paroxetine is superior to the noradrenaline reuptake inhibitor maprotiline in the treatment of premenstrual syndrome: A placebo-controlled trial. Neuropsychopharmacol 12:167, 1995 |
|
Steiner M, Hirschberg AL, Bergeron R et al: Luteal phase dosing with paroxetine controlled release (CR) in the treatment of premenstrual dysphoric disorder. Am J Obstet Gynecol 2005;193(2):352-60. |
|
Cohen LS, Soares CN, Yonkers KA et al: Paroxetine controlled release for premenstrual dysphoric disorder: a double-blind, placebo-controlled trial. Psychosom Med 2004;66(5):707-13. |
|
Wikander I, Sundblad C, Andersch B et al: Citalopram in premenstrual dysphoria: is intermittent treatment during luteal phases more effective than continuous medication throughout the menstrual cycle? J Clin Psychopharmacol 18:390, 1998 |
|
Freeman EW, Rickels K, Yonkers KA et al: Venlafaxine in the treatment of premenstrual dysphoric disorder. Obstet Gynecol 98:737, 2001 |
|
Cohen LS, Soares CN, Lyster A et al: Efficacy and tolerability of premenstrual use of venlafaxine (flexible dose) in the treatment of premenstrual dysphoric disorder. J Clin Psychopharmacol 2004;24(5):540-3. |
|
Sundblad C, Modigh K, Andersch B et al: Clomipramine effectively reduces premenstrual irritability and dysphoria: A placebo-controlled trial. Acta Psychiatr Scand 85:39, 1992 |
|
Sundblad C, Hedberg M, Eriksson E: Clomipramine administered during the luteal phase reduces the symptoms of premenstrual syndrome: A placebo controlled trial. Neuropsychopharmacology 9:133, 1993 |
|
Freeman EW, Sondheimer SJ, Sammel MD, Ferdousi T, Lin H. A preliminary study of luteal phase versus symptom-onset dosing with escitalopram for premenstrual dysphoric disorder. J Clin Psychiatry 2005;66(6):769-73. |
|
Yonkers KA, Holthausen GA, Poschman K, Howell HB. Symptom-onset treatment for women with premenstrual dysphoric disorder. J Clin Psychopharmacol 2006;26(2):198-202. |
|
Brown CS, Ling FW, Andersen RN et al: Efficacy of depot leuprolide in premenstrual syndrome: Effect of symptom severity and type in a controlled trial. Obstet Gynecol 84:779, 1994 |
|
Freeman EW, Sondheimer SJ, Rickels K: Gonadotropin-releasing hormone agonist in treatment of premenstrual symptoms with and without ongoing dysphoria: A controlled study. Psychopharmacol Bull 33:303, 1997 |
|
Hammarback S, Backstrom T: Induced anovulation as treatment of premenstrual tension syndrome: A double-blind cross-over study with GnRH-agonist versus placebo. Acta Obstet Gynecol Scand 67:159, 1988 |
|
Hussain SY, Massil JH, Matta WH et al: Buserelin in premenstrual syndrome. Gynecol Endocrinol 6:57, 1992 |
|
Leather AT, Studd JW, Watson NR et al: The treatment of severe premenstrual syndrome with goserelin with and without “add-back” estrogen therapy: A placebo-controlled study. Gynecol Endocrinol 13:48, 1999 |
|
Muse KN, Cetel NS, Futterman LA et al: The premenstrual syndrome: Effects of “medical ovariectomy. ” N Engl J Med 311:1345, 1984 |
|
Sundstrom I, Nyberg S, Bixo M et al: Treatment of premenstrual syndrome with gonadotropin-releasing hormone agonist in a low dose regimen. Acta Obstet Gynecol Scand 78:891, 1999 |
|
Schmidt PJ, Nieman LK, Grover GN et al: Lack of effect of induced menses on symptoms in women with premenstrual syndrome. N Engl J Med 324:1174, 1991 |
|
Majewska MD, Harrison NL, Schwartz RD et al: Steroid hormone metabolites are barbiturate-like modulators of the GABA receptor. Science 232:1004, 1986 |
|
Bitran D, Hilvers RJ, Kellogg CK: Anxiolytic effects of 3 alpha-hydroxy-5 alpha[beta]-pregnan-20-one: endogenous metabolites of progesterone that are active at the GABAA receptor. Brain Res 561:157, 1991 |
|
Gorman JM, Kent J, Martinez J et al: Physiological changes during carbon dioxide inhalation in patients with panic disorder major depression, and premenstrual dysphoric disorder. Arch Gen Psych 58:125, 2001 |
|
Kent JM, Papp LA, Martinez JM et al: Specificity of panic response to CO2 inhalation in panic disorder: A comparison with major depression and premenstrual dysphoric disorder. Am J Psych 158:58, 2001 |
|
Sandberg D, Endicott J, Harrison W et al: Sodium lactate infusion in late luteal phase dysphoric disorder. Psych Res 46:79, 1993 |
|
Facchinetti F, Tarabusi M, Nappi G: Premenstrual syndrome and anxiety disorders: A psychobiological link. Psychother Psychosom 67:57, 1998 |
|
Wang M, Seippel L, Purdy RH et al: Relationship between symptom severity and steroid variation in women with premenstrual syndrome: study on serum pregnenolone sulfate, 5-pregnan-3, 20-dione and 3-hydroxy-5-pregnan-20-one. J Clin Endocrinol Metab 81:1076, 1996 |
|
Rapkin AJ, Morgan M, Goldman L et al: Progesterone metabolite allopregnanolone in women with premenstrual syndrome. Obstet Gynecol 90:709, 1997 |
|
Bicikova M, Dibbelt L, Hill M et al: Allopregnanolone in women with premenstrual syndrome. Horm Metab Res 30:227, 1998 |
|
Monteleone P, Luisi S, Tonetti A et al: Allopregnanolone concentrations and premenstrual syndrome. Eur J Endocrinol 142:269, 2000 |
|
Freeman EW, Frye CA, Rickels K et al: Allopregnanolone levels and symptom improvement in severe premenstrual syndrome. J Clin Psychopharmacol 22:516, 2002 |
|
Girdler SS, Straneva PA, Light KC et al: Allopregnanolone levels and reactivity to mental stress in premenstrual dysphoric disorder. Biol Psychiatry 49:788, 2001 |
|
Rasgon N, Serra M, Biggio G et al: Neuroactive steroid-serotonergic interaction: Responses to an intravenous L-tryptophan challenge in women with premenstrual syndrome. Eur J Endocrinol 145:25, 2001 |
|
Griffin LD, Mellon SH: Selective serotonin reuptake inhibitors directly alter activity of neurosteroidogenic enzymes. Proc Natl Acad Sci 96:13512, 1999 |
|
Hammarback S, Damber JE, Backstrom T: Relationship between symptom severity and hormone changes in women with premenstrual syndrome. J Clin Endocrinol Metab 68:125, 1989 |
|
Watts JF, Butt WR, Logan Edwards R et al: Hormonal studies in women with premenstrual tension. Br J Obstet Gynaecol 92:247, 1985 |
|
Maddocks S, Hahn P, Moller F et al: A double-blind placebo-controlled trial of progesterone vaginal suppositories in the treatment of premenstrual syndromeAm J Obstet Gynecol 154:573, 1986 |
|
Freeman E, Rickels K, Sondheimer SJ et al: Ineffectiveness of progesterone suppository treatment for premenstrual syndrome. JAMA 264:349, 1990 |
|
Freeman EW, Rickels K, Sondheimer SJ et al: A double-blind trial of oral progesterone, alprazolam and placebo in treatment of severe premenstrual syndrome. JAMA 274:51, 1995 |
|
Wyatt K, Dimmock P, Jones P et al: Efficacy of progesterone and progestogens in management of premenstrual syndrome: systematic review. Br Med J 323:776, 2001 |
|
Arafat ES, Hargrove JT, Maxson WS et al: Sedative and hypnotic effects of oral administration of micronized progesterone may be mediated through its metabolites. Am J Obstet Gynecol 159:1203, 1988 |
|
Freeman EW, Purdy RH, Coutifaris C: Anxiolytic metabolites of progesterone: Correlation with mood and performance measures following oral progesterone administration to healthy female volunteers. Neuroendocrinology 58:478, 1993 |
|
Myers ER, Sondheimer SJ, Freeman EW et al: Serum progesterone levels following vaginal administration of progesterone during the luteal phase. Fertil Steril 47:71, 1987 |
|
Halbreich U, Endicott J: Possible involvement of endorphin withdrawal or imbalance in specific premenstrual syndromes and postpartum depression. Med Hypotheses 7:1045, 1981 |
|
Cohen MR, Cohen RM, Pickar D et al: Behavioral effects after high dose naloxone administration to normal volunteers (letter). Lancet 2:1110, 1981 |
|
Chuong CJ, Coulam CB, Kao PC et al: Neuropeptide levels in premenstrual syndrome. Fertil Steril 44:760, 1985 |
|
Tulenheimo A, Laafikainen T, Salminen K: Plasma b-endorphin immunoreactivity in premenstrual tension. Br J Obstet Gynecol 94:26, 1987 |
|
Facchinetti F, Martignoni E, Petraglia F et al: Premenstrual fall of plasma, b-endorphin in patients with premenstrual syndrome. Fertil Steril 47:570, 1987 |
|
Chuong CJ, Coulam CB, Bergstralh EJ et al: Clinical trial of naltrexone in premenstrual syndrome. Obstet Gynecol 72:332, 1988 |
|
Bruce J, Russell GFM: Premenstrual tension: A study of weight changes and balances of water, sodium and potassium. Lancet 2:267, 1962 |
|
Andersch B, Hahn L, Andersson M et al: Body water and weight in patients with premenstrual tension. Br J Obstet Gynecol 85:546, 1978 |
|
Kuchel O, Horky K, Gregorova I et al: Inappropriate response to upright posture: A precipitating factor in the pathogenesis of idiopathic edema. Ann Intern Med 73:245, 1970 |
|
Kuchel O, Cuche JL, Buu NT et al: Catecholamine excretion in “idiopathic” edema: Decreased dopamine excretion, a pathogenic factor? J Clin Endocrinol Metab 44:639, 1977 |
|
Norbiato G, Bevilacqua M, Raggi U et al: Effect of metoclopramide, a dopaminergic inhibitor, on renin and 1aldosterone in idiopathic edema: Possible therapeutic approach with levodopa and carbidopa. J Clin Endocrinol Metab 48:37, 1979 |
|
Mira M, McNeil D, Fraser I et al: Mefenamic acid in the treatment of premenstrual syndrome. Obstet Gynecol 68:395, 1986 |
|
Brush MG, Watson SJ, Horrobin DF et al: Abnormal essential fatty acid levels in plasma of women with premenstrual syndrome. Am J Obstet Gynecol 150:363, 1984 |
|
Budeiri D, Li Wan Po A, Dornan JC: Is evening primrose oil of value in the treatment of premenstrual syndrome? Controlled Clin Trials 17:60, 1996 |
|
Kendler KS, Karkowski LM, Corey LA et al: Longitudinal population-based twin study of retrospectively reported premenstrual symptoms and lifetime major depression. Am J Psych 155:1234, 1998 |
|
Condon JT: The premenstrual syndrome: A twin study. Br J Psychi 162:481, 1993 |
|
Huo L, Straub RE, Roca C, Schmidt PJ et al: Risk for premenstrual dysphoric disorder is associated with genetic variation in ESR1, the estrogen receptor alpha gene. Biol Psychiatry 2007;62(8):925-33. Epub 2007 Jun 27. |
|
Smith MJ, Schmidt PJ, Rubinow DR: Operationalizing DSM-IV criteria for PMDD: Selecting symptomatic and asymptomatic cycles for research. J Psychiatr Res 37:75, 2003 |
|
Freeman EW, Rickels K, Sondheimer SJ et al: Differential response to antidepressants in women with premenstrual syndrome/premenstrual dysphoric disorder: A randomized controlled trial. Arch Gen Psych 56:932, 1999 |
|
Freeman EW, Rickels K, Sondheimer SJ et al: Continuous or intermittent dosing with sertraline for patients with severe premenstrual syndrome or premenstrual dysphoric disorder. Am J Psychiatry 2004;161(2):343-51. |
|
Mortola JF, Girton L, Beck L, Yen SS. Diagnosis of premenstrual syndrome by a simple, prospective, and reliable instrument: the calendar of premenstrual experiences. Obstet Gynecol. 1990 Aug;76(2):302-7. |
|
Endicott J, Nee J, Harrison W. Daily Record of Severity of Problems (DRSP): reliability and validity. Arch Womens Ment Health. 2006 Jan;9(1):41-9 |
|
Freeman EW, DeRubeis RJ, Rickels K. Reliability and validity of a daily diary for premenstrual syndrome. Psychiatry Res. 1996 Nov 15;65(2):97-106. |
|
Moos RH. The development of a menstrual distress questionnaire. Psychosom Med. 1968 Nov-Dec;30(6):853-67. |
|
Halbreich U, Endicott J, Schacht S, Nee J. The diversity of premenstrual changes as reflected in the Premenstrual Assessment Form. Acta Psychiatr Scand. 1982 Jan;65(1):46-65. |
|
Thys-Jacobs S, Alvir JM, Fratarcangelo P. Comparative analysis of three PMS assessment instruments--the identification of premenstrual syndrome with core symptoms. Psychopharmacol Bull. 1995;31(2):389-96. |
|
Steiner M, Haskett RF, Carroll BJ.Premenstrual tension syndrome: the development of research diagnostic criteria and new rating scales. Acta Psychiatr Scand. 1980 Aug;62(2):177-90. |
|
Rubinow DR, Roy-Byrne P, Hoban MC, Gold PW, Post RM. Prospective assessment of menstrually related mood disorders. Am J Psychiatry. 1984 May;141(5):684-6. |
|
Steiner M, Streiner DL, Steinberg S, Stewart D, Carter D, Berger C, Reid R, Grover D.The measurement of premenstrual mood symptoms. J Affect Disord. 1999 Jun;53(3):269-73. |
|
Fugh-Berman A, Kronenberg F: Complementary and alternative medicine (CAM) in reproductive-age women: a review of randomized controlled trials. Reprod Toxicol 17:137, 2003 |
|
Thys-Jacobs S, Starkey P, Bernstein D et al: Calcium carbonate and the premenstrual syndrome: Effects on premenstrual and menstrual symptoms. Am J Obstet Gynecol 179:444, 1998 |
|
Wyatt KM, Dimmock PW, Jones PW et al: Efficacy of vitamin B-6 in the treatment of premenstrual syndrome: Systematic review. Br Med J 318:1375, 1999 |
|
Wurtman JJ, Brzezinski A, Wurtman RJ et al: Effect of nutrient intake on premenstrual depression. Am J Obstet Gynecol 161:1228, 1989. |
|
Sayegh R, Schiff I, Wurtman J et al: The effect of a carbohydrate-rich beverage on mood, appetite, and cognitive function in women with premenstrual syndrome. Obstet Gynecol 86:520, 1995. |
|
Freeman EW, Stout AL, Endicott J et al: Treatment of premenstrual syndrome with a carbohydrate-rich beverage. Int J Gynaecol Obstet 77:253, 2002 |
|
Gise LH: Group approaches to the diagnosis and treatment of the premenstrual syndromes. In Halperin DA (ed): (ed): Group Psychodynamics: New Paradigms and New Perspectives. pp 139, Chicago, Yearbook Medical Publishers, 1989 |
|
Hunter MS, Ussher J, Browne SJ et al: A randomized comparison of psychological (cognitive behavior therapy), medical (fluoxetine) and combined treatment for women with premenstrual dysphoric disorder. J Psychosom Obstet Gynaecol 23:193, 2002 |
|
Hunter MS, Ussher JM, Cariss M et al: Medical (fluoxetine) and psychological (cognitive-behavioural therapy) treatment for premenstrual dysphoric disorder: A study of treatment processes. J Psychosom Res 53:811, 2002 |
|
Blake F, Salkovskis P, Gath D et al: Cognitive therapy for premenstrual syndrome: A controlled trial. J Psychosom Res 45:307, 1998 |
|
Morse CA, Dennerstein L, Farrell E et al: A comparison of hormone therapy, coping skills training and relaxation for the relief of premenstrual syndrome. J Behav Med 14:469, 1991 |
|
Goodale IL, Domar AD, Benson H: Alleviation of premenstrual syndrome symptoms with the relaxation response. Obstet Gynecol 75:649, 1990 |
|
Aganoff JA, Boyle GJ: Aerobic exercise, mood states and menstrual cycle symptoms. J Psychosom Res 38:183, 1994 |
|
Steege JF, Blumenthal JA: The effects of aerobic exercise on premenstrual symptoms in middle-aged women: A preliminary study. J Psychosom Res 37:127, 1993 |
|
Prior JC, Vigna Y: Conditioning exercise and premenstrual symptoms. J Reprod Med 32:423, 1987 |
|
McEwen BS: Basic research perspective: ovarian hormone influence on brain neurochemical functions. In Gise LH (ed): (ed): The Premenstrual Syndromes. pp 21, New York, Churchill Livingstone, 1988 |
|
Dennicoff KD, Hoban CG, Grover GN et al: Glucose tolerance testing in women with premenstrual syndrome. Am J Psych 147:447, 1990 |
|
Rossignol AM, Bonnlander H, Song L et al: Do women with premenstrual symptoms self-medicate with caffeine? Epidemiology 2:403, 1991 |
|
Schellenberg R: Treatment for the premenstrual syndrome with agnus castus fruit extract: prospective, randomized, placebo controlled study. Br Med J 322:134, 2001 |
|
Ma L, Lin S, Chen R et al: Treatment of moderate to severe premenstrual syndrome with Vitex agnus castus(BNO 1095) in Chinese women. Gynecol Endocrinol. 2010 Aug;26(8):612-6. |
|
He Z, Chen R, Zhou Y et al: Treatment for premenstrual syndrome with Vitex agnus castus: A prospective, Maturitas. 2009 May 20;63(1):99-103. Epub 2009 Mar 9. |
|
Berger D, Schaffner W, Schrader E et al: Efficacy of vitex agnus castus L extract Ze 440 in patients with premenstrual syndrome (PMS). Arch Gynecol Obstet 264:150, 2000 |
|
Loch EG, Selle H, Boblitz N: Treatment of premenstrual syndrome with a phytopharmaceutical formulation containing vitex agnus castus. J Womens Health Gend Based Med 9:315, 2000 |
|
Canning s, Waterman M, Orsi N et al. The efficacy of hypericum perforatum (St John's Wort) for the treatment of premenstrual syndrome. CNS Drugs 24: 207, 2010. |
|
Ghazanfarpour M, Kaviani M, Asadi N et al. Hypericum perforatum for the treament of premenstrual syndrome. Int J Gynecol Obstet 84, 2011 |
|
Stevinson C, Ernst E: A pilot study of hypericum perforatum for the treatment of premenstrual syndrome. Br J Obstet Gynecol 107:870, 2000 |
|
Christensen AP, Oei TP: The efficacy of cognitive behaviour therapy in treating premenstrual dysphoric changes. J Affect Disord 33:57, 1995 |
|
Kirkby RJ: Changes in premenstrual symptoms and irrational thinking following cognitive-behavioral coping skills training. J Consult Clin Psychol 62:1026, 1994 |
|
Lustyk MK, Gerrish WG, Shaver S et al: Cognitive-behavioral therapy for premenstrual syndrome and premenstrual dysphoricdisorder: a systematic review. Arch Womens Ment Health. 2009 Apr;12(2):85-96. Epub 2009 Feb 27. |
|
Parry BL, Berga SL, Kripke DF et al: Altered waveform of nocturnal melatonin secretion in premenstrual depression. Arch Gen Psychiatry 47:1139, 1990 |
|
Parry BL, Mahan AM, Mostofi N et al: Light therapy of late luteal phase dysphoric disorder: an extended study. Am J Psych 150:1417, 1993 |
|
Parry BL, Wehr TA: Therapeutic effect of sleep deprivation in patients with premenstrual syndrome. Am J Psych 144:808, 1987 |
|
Parry BL, Cover H, Mostofi N et al: Early versus late partial sleep deprivation in patients with premenstrual dysphoric disorder and normal comparison subjects. Am J Psych 152:404, 1995. |
|
Parry BL, Javeed S, Laughlin GA et al: Cortisol circadian rhythms during the menstrual cycle and with sleep deprivation in premenstrual dysphoric disorder and normal control subjects. Biol Psychiatry 48:920, 2000 |
|
Brown J, O' Brien PM, Marjoribanks J et al: Selective serotonin reuptake inhibitors for premenstrual syndrome. Cochrane Database Syst Rev. 2009 Apr 15;(2):CD001396. |
|
Shah NR, Jones JB, Aperi J et al: Selective serotonin reuptake inhibitors for premenstrual syndrome and Obstet Gynecol. 2008 May;111(5):1175-82. |
|
Altshuler LL, Cohen LS, Moline ML et al: The Expert Consensus Guideline Series: Treatment of depression in women, 2001. Postgrad Med March 1, 2001 |
|
Clayton AH, Pradko JF, Croft HA et al: Prevalence of sexual dysfunction among newer antidepressants. J Clin Psych 63:357, 2002 |
|
Cohen LS, Miner C, Brown E et al: Premenstrual daily fluoxetine for premenstrual dysphoric disorder: A placebo-controlled, clinical trial using computerized diaries. Obstet Gynecol 100:435, 2002 |
|
Halbreich U, Bergeron R, Yonkers KA et al: Efficacy of intermittent, luteal phase sertraline treatment of premenstrual dysphoric disorder. Obstet Gynecol 100:1219, 2002 |
|
Dimmock PW, Wyatt KM, Jones PW et al: Efficacy of selective serotonin-reuptake inhibitors in premenstrual syndrome: a systematic review. Lancet 256:1131, 2000 |
|
Miner C, Brown E, McCray S et al: Weekly luteal-phase dosing with enteric-coated fluoxetine 90 mg in premenstrual dysphoric disorder: A randomized, double-blind, placebo-controlled clinical trial. Clin Ther 24:417, 2002 |
|
Freeman EW, Sondheimer SJ, Polansky M et al: Predictors of response to sertraline treatment of severe premenstrual syndromes. J Clin Psych 61:579, 2000 |
|
Berger CP, Presser B: Alprazolam in the treatment of two subsamples of patients with late luteal phase dysphoric disorder: A double-blind, placebo-controlled crossover study. Obstet Gynecol 84:379, 1994 |
|
Harrison WM, Endicott J, Nee J: Treatment of premenstrual dysphoria with alprazolam: A controlled study. Arch Gen Psych 47:270, 1990 |
|
Smith S, Rinehart JS, Ruddock VE et al: Treatment of premenstrual syndrome with alprazolam: Results of a double-blind, placebo-controlled, randomized crossover clinical trial. Obstet Gynecol 70:37, 1987 |
|
Rickels K, Freeman EW, Sondheimer SJ: Buspirone in treatment of premenstrual syndrome. Lancet 1:777, 1989 |
|
Schmidt PJ, Grover GN, Rubinow DR: Alprazolam in the treatment of premenstrual syndrome: A double-blind, placebo-controlled trial. Arch Gen Psychiatry 50:467, 1993 |
|
Dennerstein L, Morse C, Burrows G et al: Alprazolam in the treatment of premenstrual syndrome. In Dennerstein L, Fraser I (eds): Hormones and Behavior. p 175, New York, Elsevier Science Publishing, 1986 |
|
Mortola JF, Girton L, Fischer U: Successful treatment of severe premenstrual syndrome by combined use of gonadotropin-releasing hormone agonist and estrogen/progestin. J Clin Endocrinol Metab 71:252, 1991 |
|
Mezrow G, Shoupe D, Spicer D et al: Depot leuprolide acetate with estrogen and progestin add-back for long-term treatment of premenstrual syndrome. Fertil Steril 62:932, 1994 |
|
Di Carlo C, Palomba S, Tommaselli GA et al: Use of leuprolide acetate plus tibolone in the treatment of severe premenstrual syndrome. Fertil Steril 75:380, 2001 |
|
Watts JW, Butt WR, Edwards RL: A clinical trial using danazol for the treatment of premenstrual tension. Br J Obstet Gynecol 94:30, 1987 |
|
Gilmore DH, Hawthorn RJS, Hart DM: Danazol for premenstrual syndrome: A preliminary report of a placebo-controlled double-blind study. J Intern Med Res 13:129, 1985 |
|
Sarno AP, Miller EJ, Lundblad EG: Premenstrual syndrome: Beneficial effects of periodic, low-dose danazol. Obstet Gynecol 70:33, 1987 |
|
Graham CA, Sherwin BB: A prospective treatment study of premenstrual symptoms using a triphasic oral contraceptive. J Psychosom Res 36:257, 1992 |
|
Bäckström T, Hansson-Malmström Y, Lindhe BA et al: Oral contraceptives in premenstrual syndrome: A randomized comparison of triphasic and monophasic preparations. Contraception 46:253, 1992 |
|
Pearlstein TB, Bachmann GA, Zacur HA, Yonkers KA. Treatment of premenstrual dysphoric disorder with a new drospirenone-containing oral contraceptive formulation. Contraception 2005;72(6):414-21. Epub 2005 Nov 2. |
|
Yonkers KA, Brown C, Pearlstein TB et al: Efficacy of a new low-dose oral contraceptive with drospirenone in premenstrual dysphoric disorder. Obstet Gynecol 2005;106(3):492-501. |
|
Freeman EW, Kroll R, Rapkin A et al: Evaluation of a unique oral contraceptive in the treatment of premenstrual dysphoric disorder. J Womens Health Gend Based Med 10:561, 2001 |
|
Parsey KS, Pong A: An open-label, multicenter study to evaluate Yasmin, a low-dose combination oral contraceptive containing drospirenone, a new progestogen. Contraception 64:51, 2001 |
|
Borenstein J, Yu H-T, Wade S et al: Effect of an oral contraceptive containing ethinyl estradiol and drospirenone on premenstrual symptomatology and health-related quality of life. J Reprod Med 48:79, 2003 |
|
Sulak PJ, Scow RD, Preece C et al: Hormone withdrawal symptoms in oral contraceptive users. Obstet Gynecol 95:261, 2000 |
|
Sulak PJ, Kuehl TJ, Ortiz M et al: Acceptance of altering the standard 21-day/7-day oral contraceptive regimen to delay menses and reduce hormone withdrawal symptoms. Am J Obstet Gynecol 186:1142, 2002 |
|
Kwiecien M, Edelman A, Nichols MD et al: Bleeding patterns and patient acceptability of standard or continuous dosing regimens of a low-dose oral contraceptive: A randomized trial. Contraception 67:9, 2003 |
|
Walker A, Bancroft J: Relationship between premenstrual symptoms and oral contraceptive use: A controlled study. Psychosom Med 52:86, 1990 |
|
Sveindòttir H, Bäckström T: Prevalence of menstrual cycle symptom cyclicity and premenstrual dysphoric disorder in a random sample of women using and not using oral contraceptives. Acta Obstet Gynecol Scand 405, 2000 |
|
Magos AL, Brincat M, Studd JWW: Treatment of the premenstrual syndrome by subcutaneous oestradiol implants and cyclical oral norethisterone: placebo-controlled study. Br Med J 292:1629, 1986 |
|
Watson NR, Savvas M, Studd JWW et al: Treatment of severe premenstrual syndrome with oestradiol patches and cyclical oral norethisterone. Lancet 2:730, 1989 |
|
Smith RNJ, Studd JWW, Zamblera D et al: A randomised comparison over 8 months of 100 μg and 200 μg twice weekly doses of transdermal oestradiol in the treatment of severe premenstrual syndrome. Br J Obstet Gynaecol 102:475, 1995 |
|
Ford O, Lethaby A, Roberts H et al: Progesterone for premenstrual syndrome. Cochrane Database Syst Rev. 2009 Apr 15;(2):CD003415. |
|
O'Brien PM, Craven D, Selby C: Treatment of premenstrual syndrome by spironolactone. Br J Obstet Gynaecol 86: 142, 1979 |
|
Vellacott ID, Shroff NE, Pearce MY et al: A double-blind, placebo-controlled evaluation of spironolactone in the premenstrual syndrome. Curr Med Res Opin 10:450,1987 |
|
Wang M, Hammarback S, Lindhe BA et al: Treatment of premenstrual syndrome by spironolactone: A double-blind, placebo-controlled study. Acta Obstet Gynecol Scand 74:803, 1995 |
|
Burnet RB, Radden HS, Easterbrook EG et al: Premenstrual syndrome and spironolactone. Aust N Z J Obstet Gynaecol 31:366, 1991 |
|
Hellberg D, Claesson B, Nilsson S: Premenstrual tension: A placebo-controlled efficacy study with spironolactone and medroxyprogesterone acetate. Int J Gynaecol Obstet 34 :243, 1991 |
|
Budoff PW: Use of prostaglandin inhibitors in the treatment of PMS. Clin Obstet Gynecol 30:453,1987 |
|
Mira M, McNeil D, Fraser IS et al: Mefenamic acid in the treatment of premenstrual syndrome. Obstet Gynecol 68:395,1986 |
|
Wood C, Jakubowicz D: The treatment of premenstrual symptoms with mefenamic acid. Br J Obstet Gynecol 87:627, 1980 |
|
Yon ers KA, Barnett LK, Carmody T et al: Serial discontinuation of SSRI treatment for PMDD. Biol Psychiatry 43: 1s, 1998 |
|
Pearlstein TB, Stone AB: Long-term fluoxetine treatment of late luteal phase dysphoric disorder. J Clin Psych 55:332,1994 |
|
Elks ML: Open trial of fluoxetine therapy for premenstrual syndromeSouth Med J 86: 503, 1993 |
|
Freeman EW, Rickels K, Sondheimer SJ: Course of premenstrual syndrome symptom severity after treatment. Am J Psych 149:531, 1992 |
|
Freeman EW, Rickels K, Sammel MD, Lin H, Sondheimer SJ. Time to relapse after short- or long-term treatment of severe premenstrual syndrome with sertraline. Arch Gen Psychiatry. 2009 May;66(5):537-44 |
|
Parlee MB: Commentary of the literature review. In Gold JH, Severino SK (eds): Premenstrual Dysphorias: Myths and Realities. p 157, Washington, DC, American Psychiatric Press, 1994 |
|
Straus JL, von Ammon Cavanaugh S: Placebo effects: Issues for clinical practice in psychiatry and medicine. Psychsomatics 37:315,1996 |
|
Schmidt PJ, Rubinow DR: Placebo effect--how powerful? (letter) Fertil Steril 59: 1144, 1993 |
|
Freeman EW, Rickels K: Characteristics of placebo responses in medical treatment of premenstrual syndrome. Am J Psych 156:1403, 1999 |
