Preventing cervical cancer
Cervical cancer and cervical screening
An educational
initiative
supported by

Written by experienced doctors, midwives and other medical professionals – and approved by a specialist Editorial Board
Enhancing the Welfare of Women
Expert Health Information for Women








(or HPV).







































The authors of this PREVENTING CERVICAL CANCER program are:
- Dr Catherine Howell
Calderdale and Huddersfield NHS Foundation Trust, Halifax, UK - Dr Veena Kaul
The Mid Yorkshire Teaching Hospitals NHS Trust, Wakefield, UK
The Welfare of Women program has been created under the General Editorship of Dr Kate Lightly, University of Liverpool, UK and is overseen by an expert International Editorial Board
The cost of producing this resource has been partly funded by an educational grant from GSK
Thank you for watching this Welfare of Women video. We would welcome your views and feedback. Please complete this short questionnaire.
Cervical cancer is one of the most common causes of cancer death in women worldwide. Most of these deaths could be avoided because this cancer can be prevented by vaccination and screening.
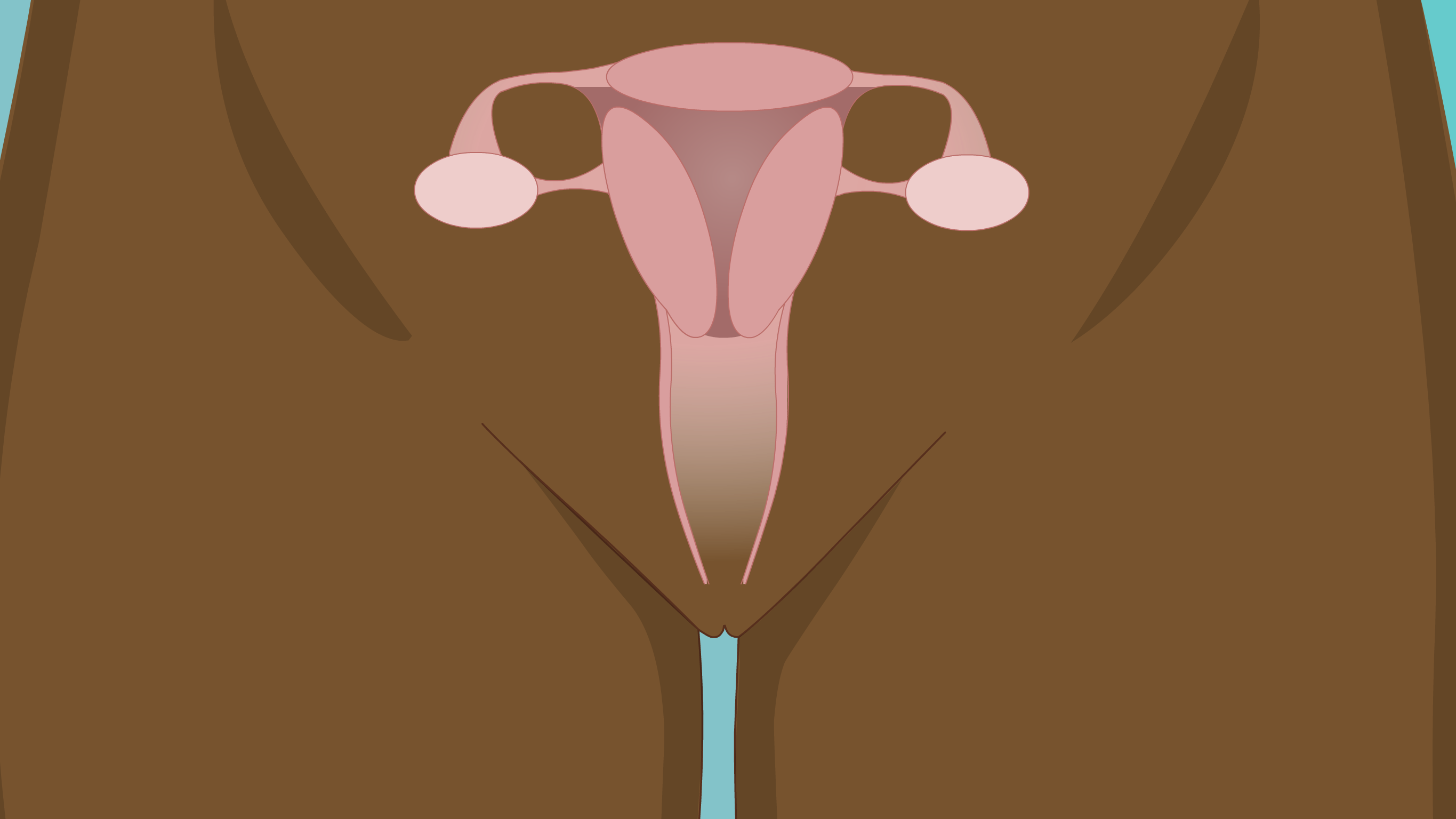
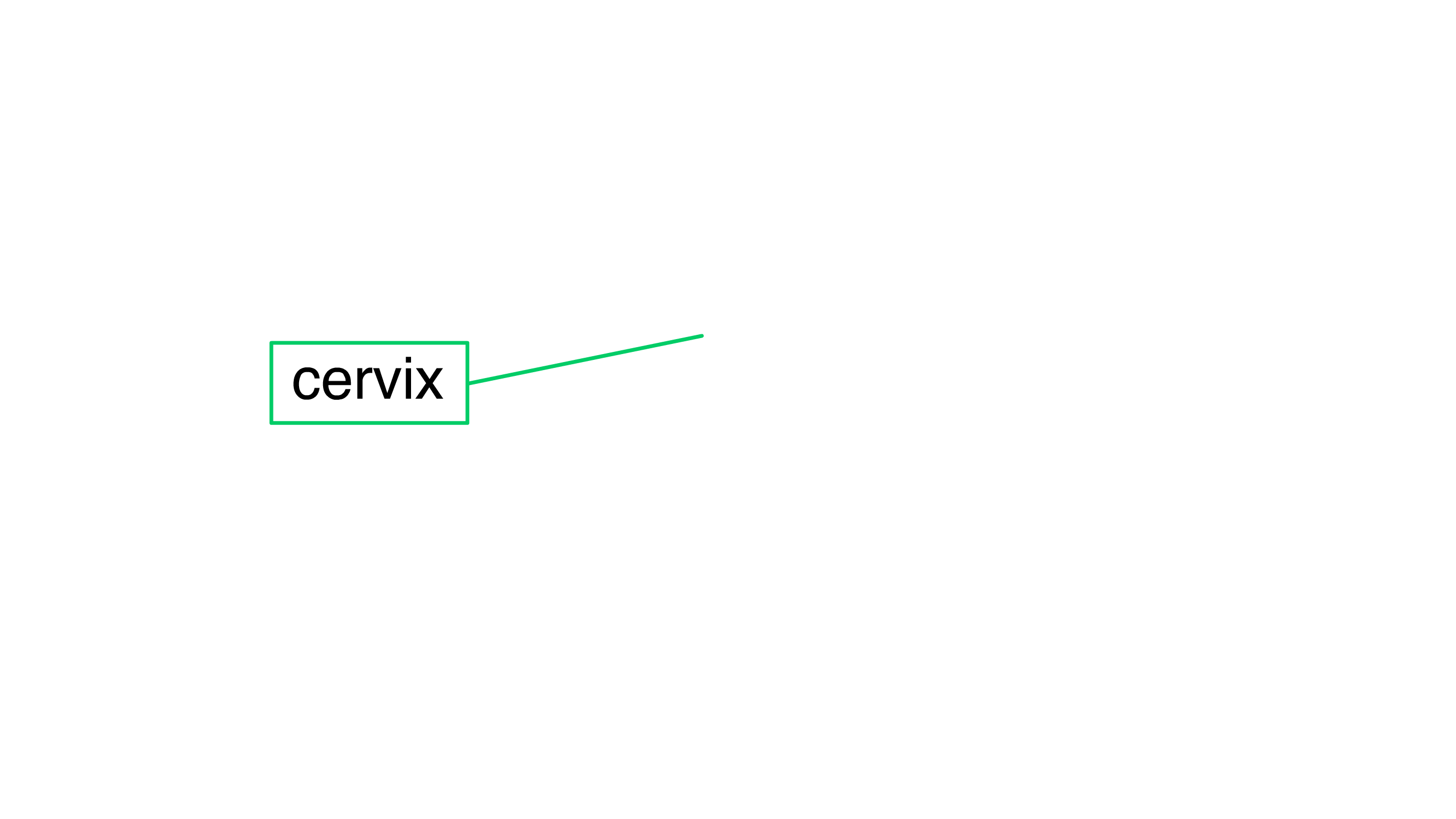
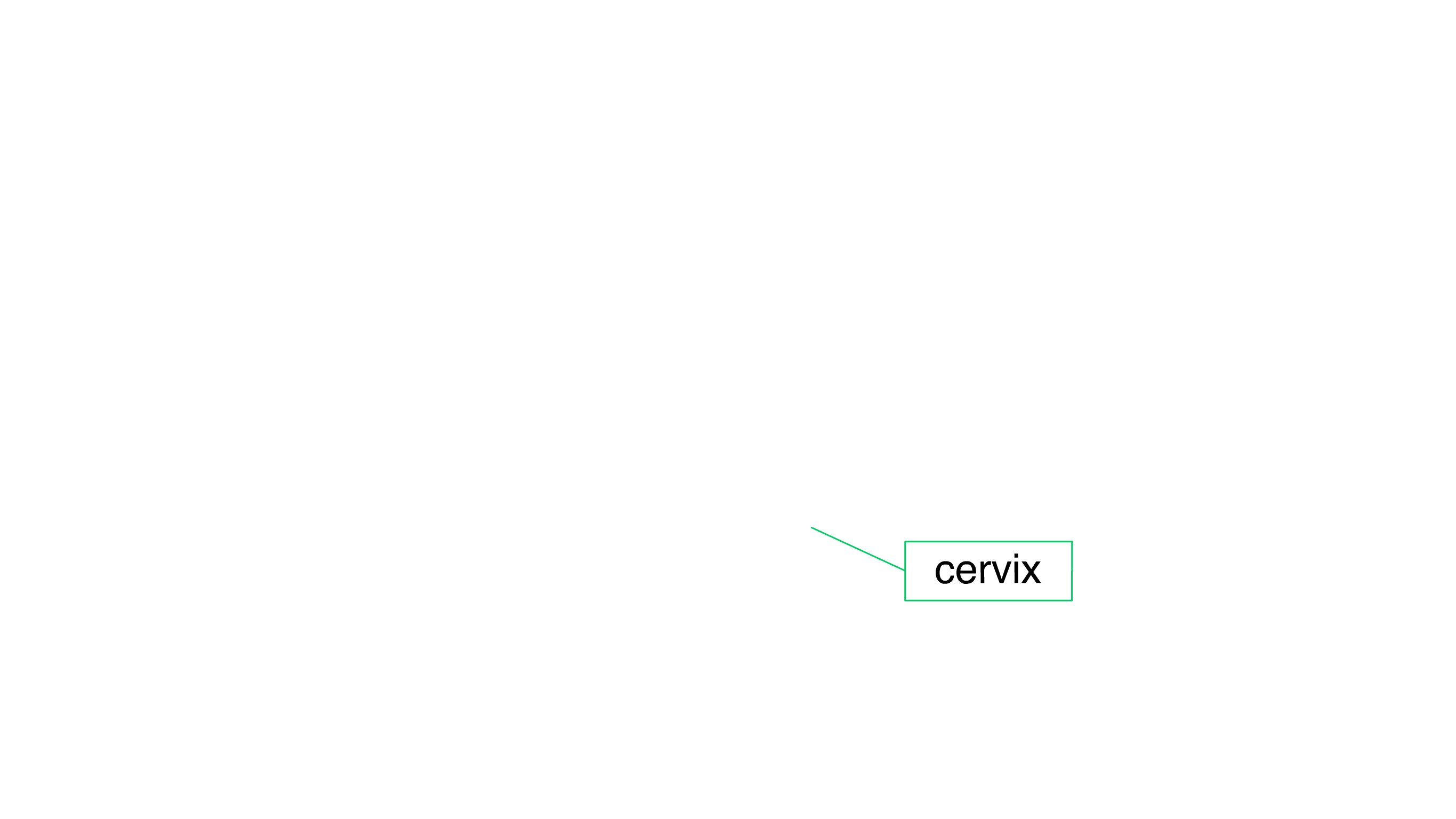
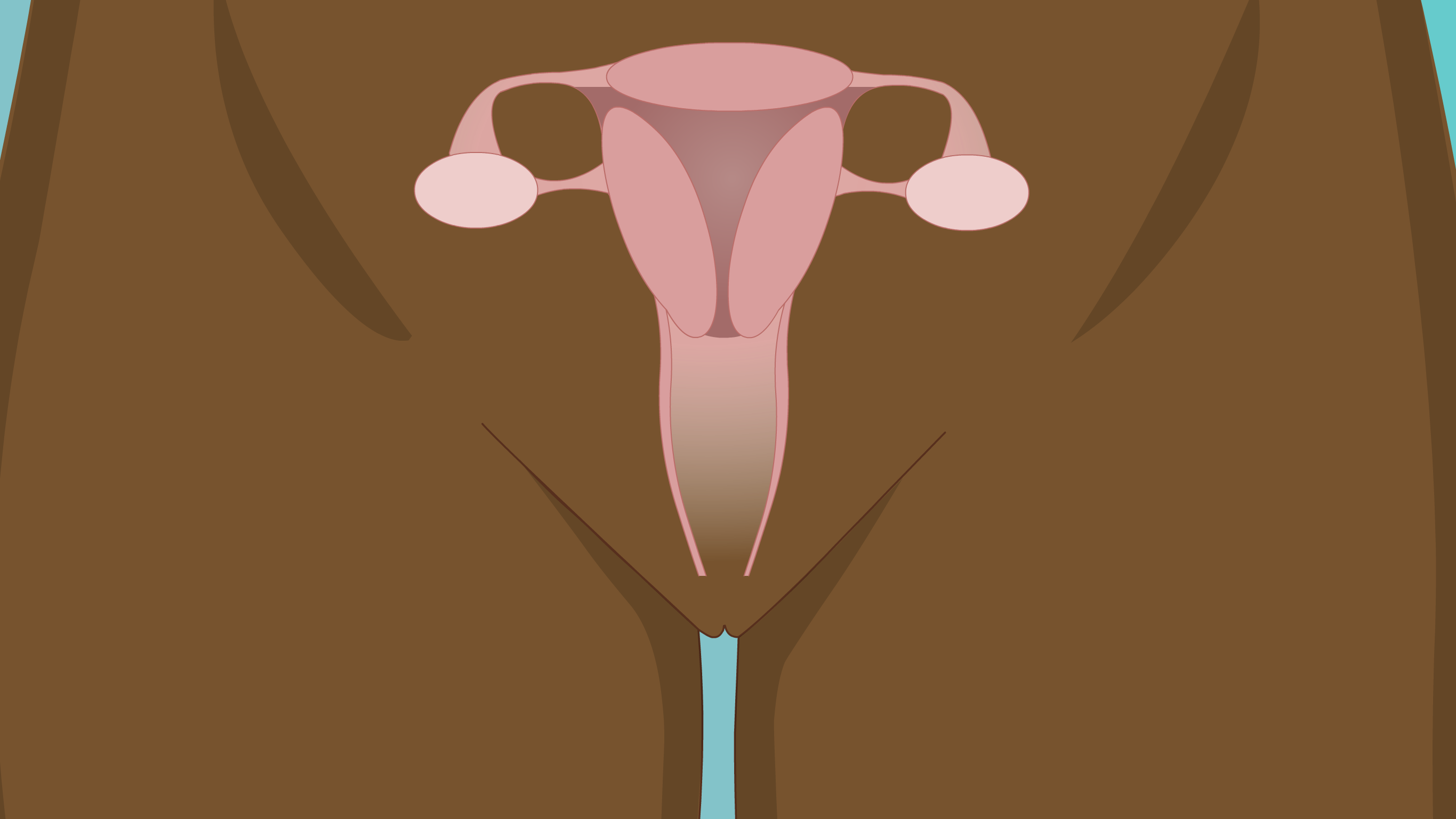
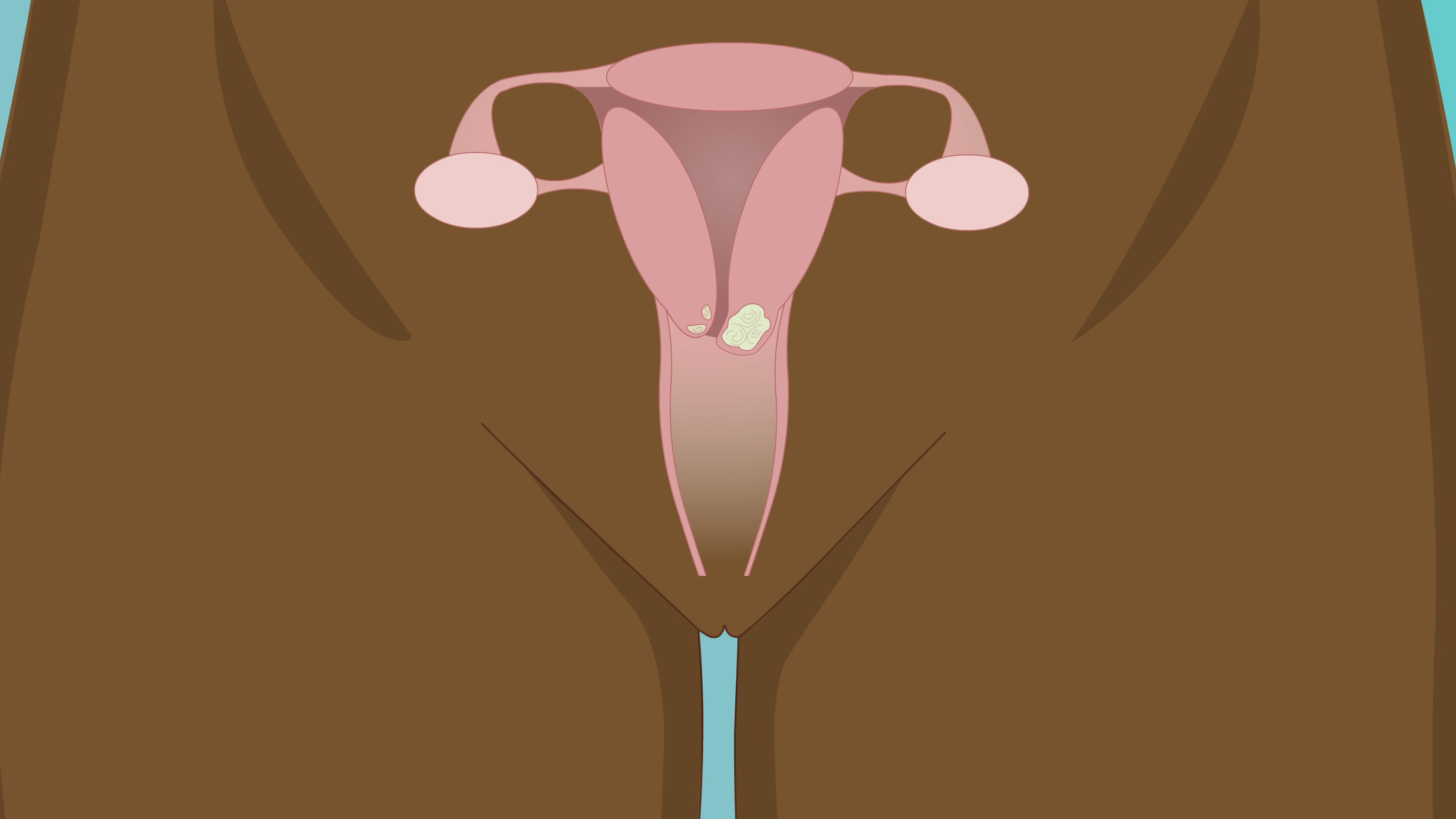
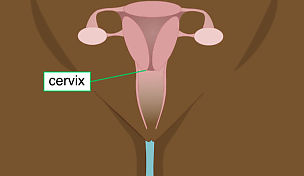
What is the cervix?
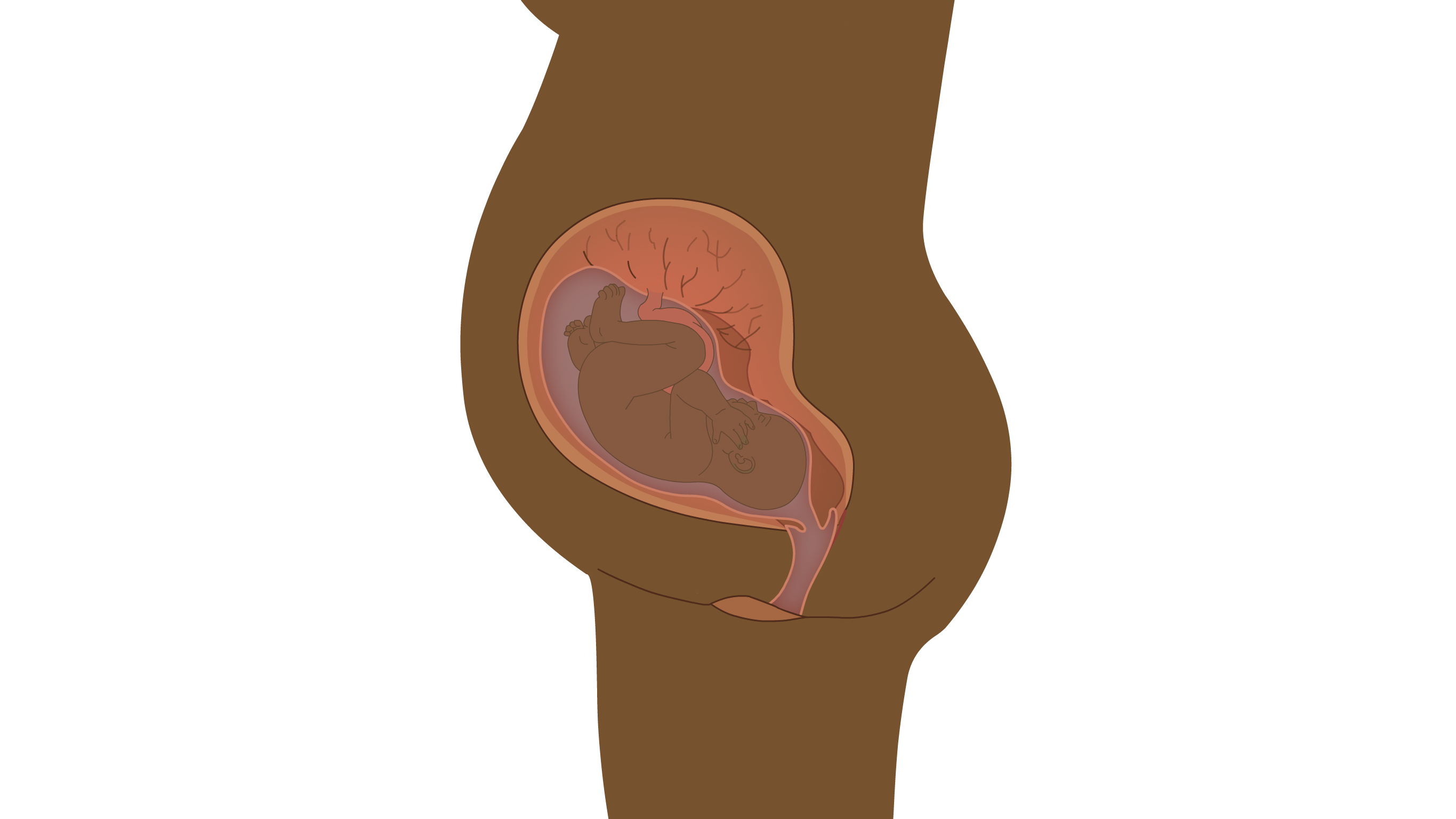
The cervix is the lower region of the womb (uterus) that opens into the birth canal (vagina). It is sometimes called the 'neck' of the womb. During childbirth, the cervix opens to allow passage of the baby.
What is cervical cancer?
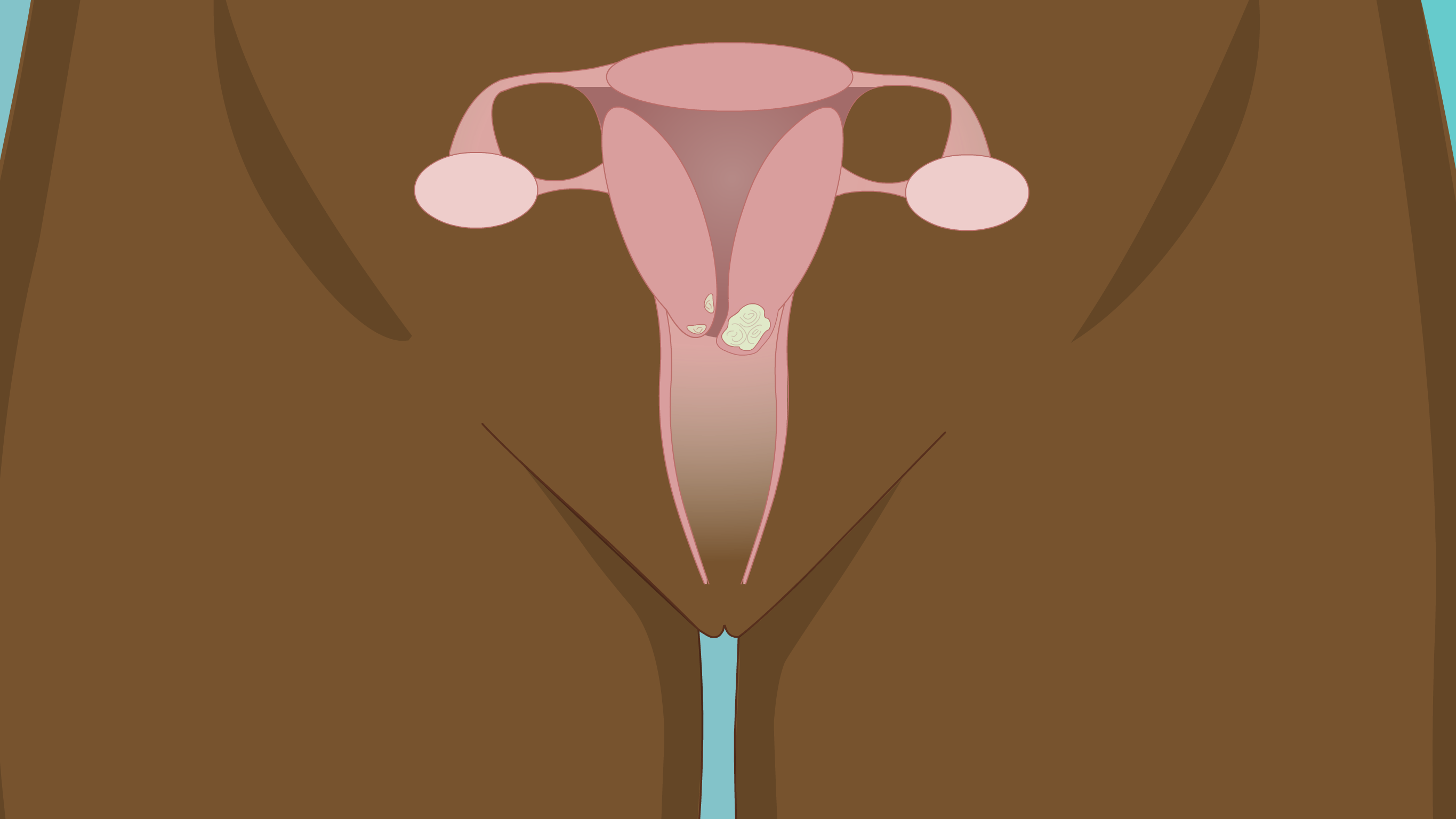
Cervical cancer is cancer that is found to have started anywhere in the cervix. Cervical cancer is a common cause of cancer death in women worldwide.
Anyone with a cervix can get cervical cancer, and almost all cervical cancers are caused by human papilloma virus (HPV). HPV is a virus which is sexually transmitted (passed from one person to another during any kind of sexual contact). HPV is a very common virus, which comes and goes for most people during their lifetime. Certain types of the HPV virus are 'high risk' for causing cervical cancer. HPV viruses are very common and most people will get some type of HPV during their life. Like the flu, if a woman comes into contact with the virus, her body's immune system (a system which protects the body against disease) is usually able to stop the virus.
However, some women will not be able to get rid of the virus. When this happens, the virus can sometimes infect the cervix and cause changes to the cells (the basic building blocks of all living things). Over time, these infected cells can begin to act differently, and can change to become precancerous. Precancerous cells can become cancer cells if they are not found early and treated.
HPV is the main cause of cervical cancer. Other major risk factors for cervical cancer include human immunodeficiency virus (HIV), smoking tobacco, and having other sexually transmitted infections, such as chlamydia, alongside HPV.
HPV is a very common virus, do not be ashamed if you test positive for the virus. If you have previously tested negative for HPV, but have a positive result this time, it does not mean that your partner has had sex with someone else, it is possible to have HPV even if you have not had sexual contact for many years.
What is cervical screening?
Cervical screening is a special test which is performed to look for precancerous cells, in order to prevent a woman from developing cervical cancer or from dying of cervical cancer. Cervical screening is not a test for cancer but it can help prevent cervical cancer.
Cervical screening usually starts around a woman's 30th birthday. Screening may start at 25 years in some countries or if a woman has HIV. She is encouraged to attend a health center for screening regularly. The World Health Organization recommends that women should be screened every 5 years, but it is performed more frequently than this in some countries. Women with HIV usually have screening more often than women who do not have HIV.
At the health center
The woman will be asked about any medical problems she has, if she has any children, if she has had cervical screening in the past, and what the result of that screening was. The screening test is then explained. She is then asked to give her consent (permission) to have the test.
The test usually takes a few minutes.
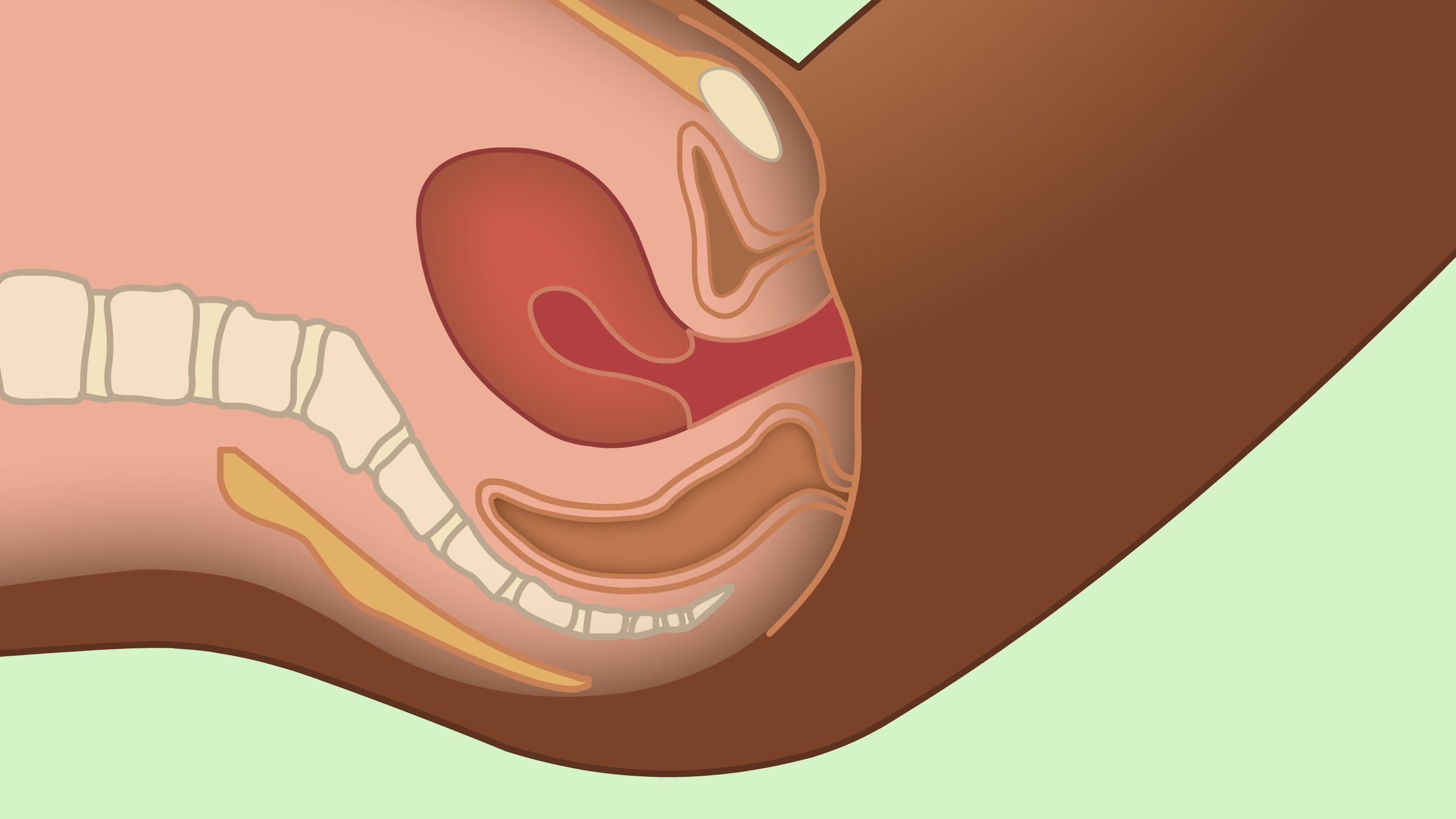
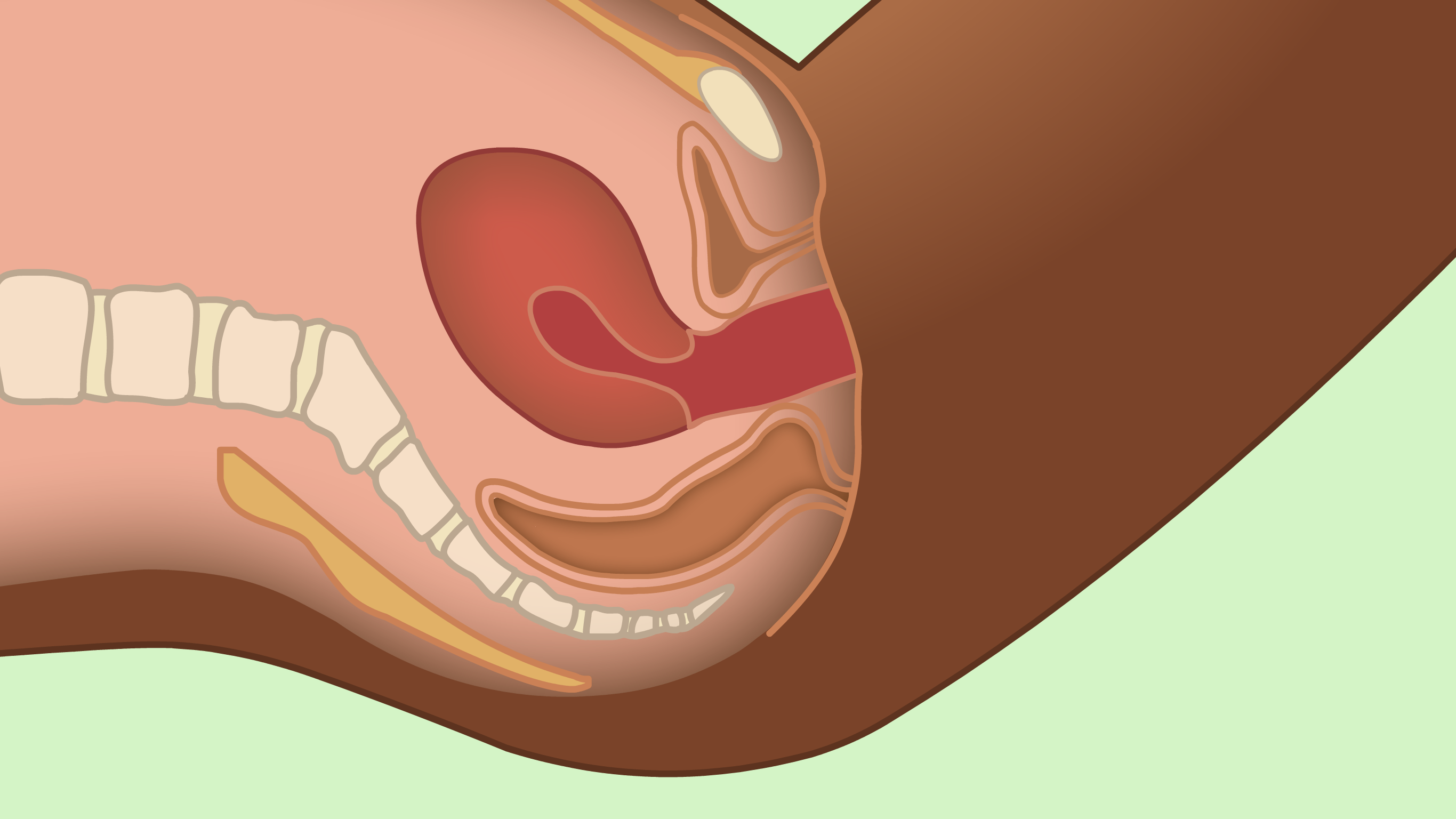
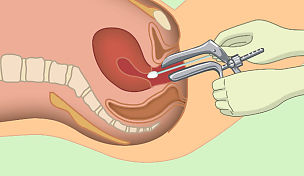
She is then asked to undress from the waist downwards and lie on an examination couch. A speculum (a plastic or metal tube) is then passed into the vagina to allow the healthcare provider to see the cervix. They will take a good look at the cervix to see if it appears healthy. The next part of the examination will depend on which test the health center provides.
Types of cervical screening test
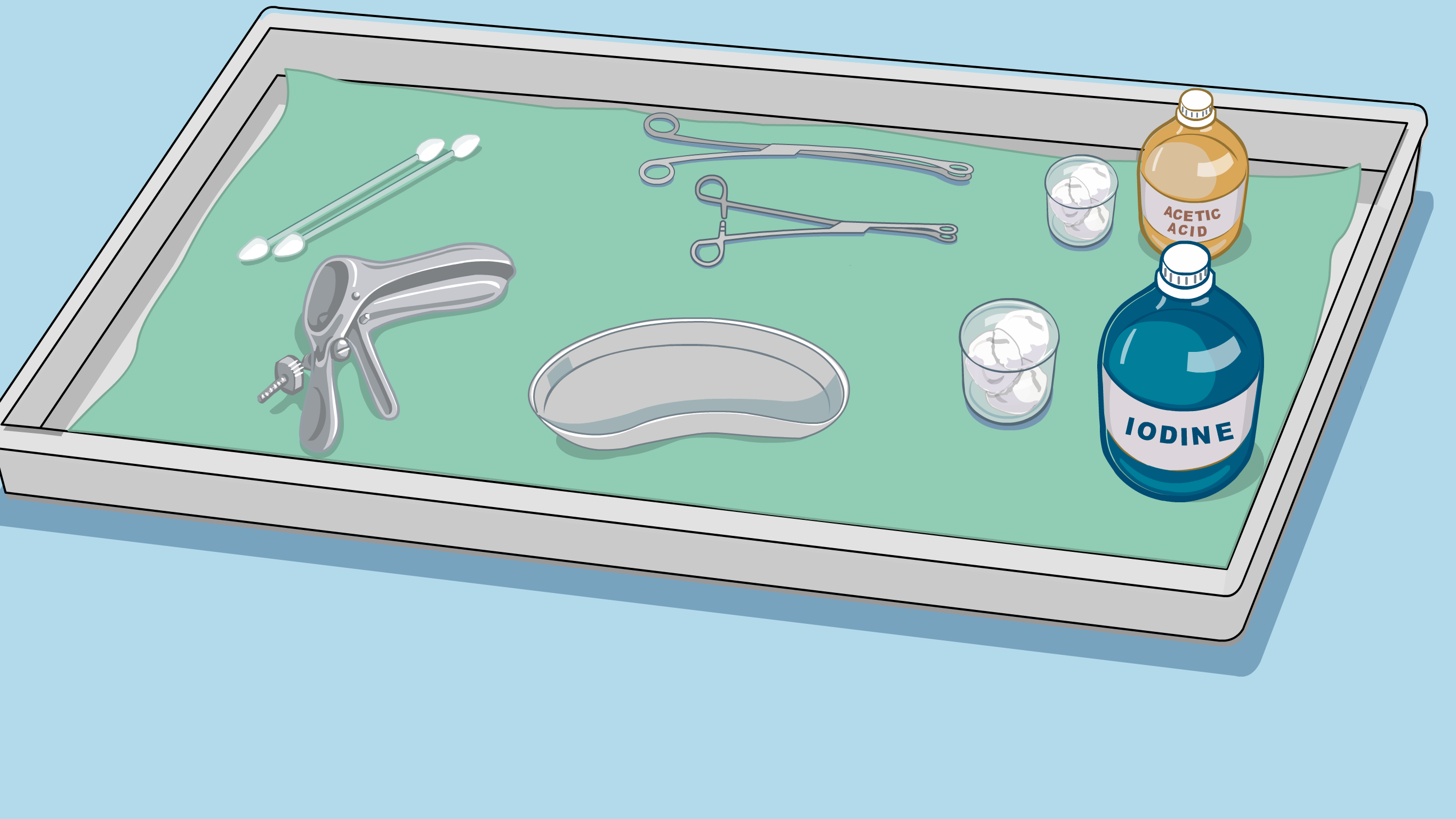
- Visual inspection with acetic acid (VIA)
The cervix is cleaned using water and then a liquid is gently applied onto the cervix. Iodine, a brown solution, may also be applied to the cervix. Abnormal areas of the cervix will change color. If this occurs, the healthcare provider may need to take a biopsy (a small sample which is sent for testing at a medical laboratory) to check the cells for precancer or cancer and the woman is referred on to a colposcopy unit (a special clinic usually in a hospital). If the abnormal area is small, the healthcare provider may ask for consent to treat the area straightaway (screen-and-treat method), by removing the area. - Cervical cytology (also known as the Pap smear test)
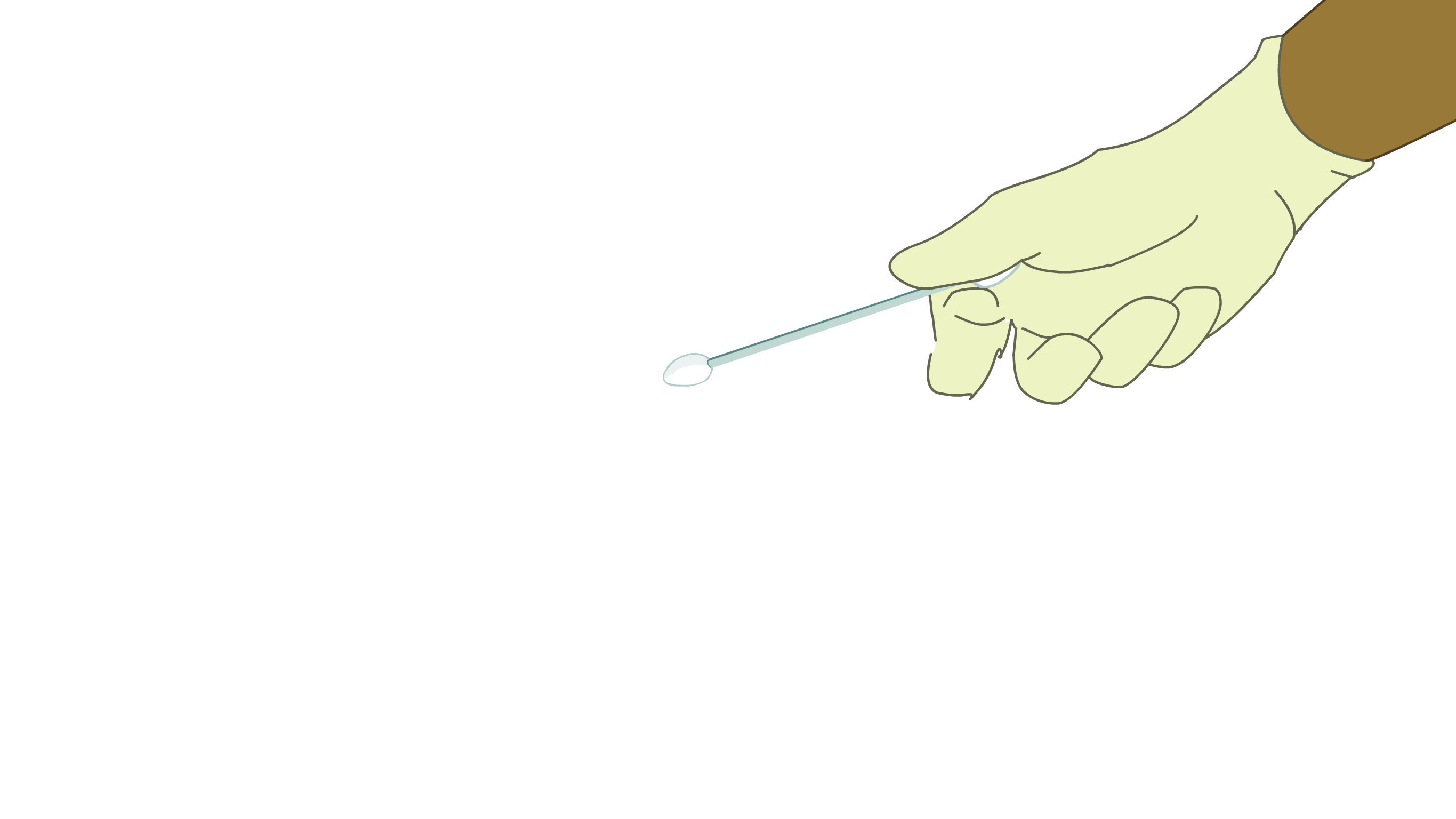
In some countries, a soft plastic brush or spatula is used to collect cells from the cervix. The brush is placed in a liquid and the cells are shaken into the liquid, or the cells collected by the spatula are smeared onto a glass slide. The sample is then sent to a laboratory where the cells are checked under a microscope (a special magnifying-glass tool) in a laboratory looking for precancerous cells. In many countries, this method is now used in combination with HPV testing. - HPV test
In some parts of the world, cervical screening involves checking for the HPV virus first before any other test. The sample might be taken by the healthcare provider at the same time as doing VIA or cervical cytology. If the 'high risk' types of HPV are found, the sample is then checked for any changes in the cells of the cervix. If the cells are normal, it is likely that there is no precancer or cancer, and the woman will be offered another test in the future to check that the virus has been cleared. If the virus is not detected, there is a very low chance of a woman having precancer or cancer of the cervix, and no further testing needs to be done at this stage.
HPV testing is now recommended by the World Health Organization as it is more accurate than are other methods. In some low-income countries, if the HPV test is positive, VIA and treatment if needed may be offered straightaway, rather than the cells being checked as above.
Risks
You may experience some spotting or light bleeding after the test. If the bleeding is heavy, you should seek help from a healthcare worker.
Remember, you are still at risk of cervical cancer if:
- You have had the HPV vaccine
- You have only had one sexual partner
- You are a lesbian or bisexual – any sexual contact, with a man or a woman, can put a person at risk
- You are a trans man with a cervix
- You have had a subtotal hysterectomy in which the cervix was left in place
Did you know?
Cervical screening can prevent cervical cancer. Make sure you are checked regularly.
If you have HIV or certain other medical conditions, you may be recommended to have cervical screening more frequently, as you are at increased risk of having HPV and cervical cancer.
Simple ways to lower your risk of cervical cancer

- Get the HPV vaccination if you are eligible
- Attend cervical screening regularly
- Use condoms – they can provide some protection against HPV and other sexually transmitted infections such as chlamydia and gonorrhea
- Quit smoking – this will strengthen your immune system
- Eat healthily – to support your immune system
- See a healthcare worker if you have abnormal bleeding especially after sex or in between periods, unusual discharge or pain
Don't delay getting tested, your health is really important!
The authors of this PREVENTING CERVICAL CANCER program are:
- Dr Catherine Howell, Calderdale and Huddersfield NHS Foundation Trust, Halifax, UK
- Dr Veena Kaul, The Mid Yorkshire Teaching Hospitals NHS Trust, Wakefield, UK
The Welfare of Women program has been created under the General Editorship of Dr Kate Lightly, University of Liverpool, UK and is overseen by an expert International Editorial Board
The publishing reference for this program is: DOI 10.3843/GLOWM.w10073
The Welfare of Women information program is an attempt to provide women everywhere with access to reliable information about key health issues that may be relevant to them. Information is offered at three separate levels which women may select according to their preferences; firstly, short video animations with voice commentary, secondly, more detailed text-based descriptions, and thirdly, links to recommended further reading. With the animated videos, women can also select the images that they feel most comfortable in viewing from a short range of very generalized and non-specific ethnicity options. Because of the special programming used, both the videos and the text information can – when authorized – be translated into any language in a simple and rapid manner.
Recommended links for more comprehensive and detailed reading
The following websites provide more comprehensive and extensive information on this topic, which is both reliable and strongly recommended for readers who want to learn more than the details provided above:
World Health Organization Cervical Cancer Factsheet
https://www.who.int/news-room/fact-sheets/detail/cervical-cancer
NHS Conditions: Cervical screening
https://www.nhs.uk/conditions/cervical-screening/
Resources the author(s) used in preparing this guidance
World Health Organization
https://www.who.int/publications/i/item/9789240014107
Global strategy to accelerate the elimination of cervical cancer as a public health problem
World Health Organization Cervical Cancer Factsheet
https://www.who.int/news-room/fact-sheets/detail/cervical-cancer
World Health Organization Comprehensive Cervical Cancer Control
https://www.who.int/publications/i/item/9789241548953
NHS Conditions: Cervical screening
https://www.nhs.uk/conditions/cervical-screening/